Think Obstructive Sleep Apnea is #NBD? Here Are Seven Health Conditions Made Worse By Your Undiagnosed OSA
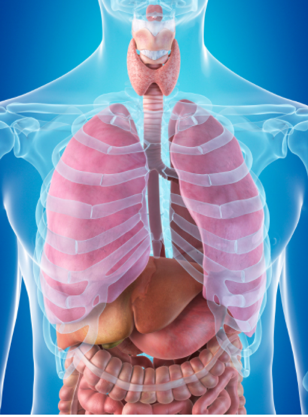
Obstructive sleep apnea (OSA) is a sleep disorder that causes your breathing to stop at night due to an upper airway collapse. More than 25 million US adults suffer from the condition, according to the National Healthy Sleep Awareness Project — and that number is on the rise!
“So what?” you might think. “Maybe I have sleep apnea, but it’s not really hurting my overall health.”
Actually, it probably is. You just don’t know it.
Here’s a list of seven medical problems that are linked to OSA.
Hypertension
I’ve lost count of the number of my patients whose blood pressure is through the roof despite the fact that they’re on multiple blood pressure medications. We call this resistant hypertension because their condition “resists” treatment. Researchers estimate that up to 50 percent of people with high blood pressure also suffer from OSA. That’s bad news because according to the American College of Cardiology, sleep apnea and high blood pressure are “a dangerous pair” that have been linked to an increased risk of stroke and heart attack.
Diabetes
A study of almost 9,000 people showed that those with severe OSA had a 30% higher risk of developing type 2 diabetes than those without. Researchers aren’t sure why this is, although they suggest it might have something to do with the fact that failure to sleep through the night might result in insulin resistance, increased cortisol levels, and glucose intolerance.
Heart Failure
Not breathing is incredibly stressful on the body, especially the heart. Don’t believe me? Hold your breath for 60 second and think about what you felt your body doing. When your oxygen intake is decreased, your heart is forced to work harder to get blood to the important parts of your body. This extra work causes the heart to enlarge, making it harder to oxygenate. One recent study found a 58% increase in congestive heart failure in men with severe OSA.
Depression
More than 70 percent of people with OSA report symptoms traditionally associated with depression. In fact, depression was twice as likely to be diagnosed in men and five times more likely in women with OSA.
Obesity
A BMI of 20 or more is considered obese. About three in four OSA patients have a body mass index greater than 30. To make matters worse, obese people with OSA are more likely to gain more weight than obese people without the disease. While we can’t say what the causal link between OSA and obesity is, we have consistently found a link between sleeping less and weighing more
ADHD
When kids have trouble concentrating and start to experience behavioral issues, many parents wonder if ADHD is to blame. For decades, ADHD has been treated with medications, many of which have been successful with a number of children. But researchers have recently wondered whether sleep disordered breathing [SBD] played a role in ADHD. The authors of a 2014 study did in fact find a link between ADHD and SBD, and issued two controversial recommendations. First, they suggested that every child with an ADHD diagnosis should be screened for SBD. Second, if SBD was found, the authors recommended treating the sleep disorder before medicating the ADHD symptoms.
Dementia
As we use our brains throughout the day, harmful waste products accumulate between brain cells. When we sleep, cerebrospinal fluid (CSF) flushes through our brain, removing the built-up neurotoxic waste. One of the proteins flushed away during this process is beta-amyloid, which researchers have long linked to Alzheimer’s disease.
Imagine what your front yard would look like if your waste removal service suddenly stopped coming to take away your trash. It would be full of trash! Sleep is our brain’s trashman, so to speak, but he can only do his job when we’re asleep. If our sleep is interrupted — as it is with OSA — then our brain may never reach its critical cleaning stage.
As you can see, getting a good night’s sleep isn’t a luxury. Sleeping through the night is a critical component of our general health. If you aren’t sure whether or not you have OSA, talk to your medical doctor or dentist. If you were already diagnosed with the condition but gave up on using CPAP — no shame; you’re not alone! — talk to your dentist about making an oral sleep appliance. (As I wrote last month, though dental insurance won’t cover the appliance, certain qualified dentists will be able to bill your medical insurance.) With an American Academy of Dental Sleep Medicine dentist helping control your OSA, you can be on your way to a longer, healthier life.


https://drugsoverthecounter.com/# over the counter birth control
instant female arousal pills over the counter over the counter pink eye medicine
over the counter medicine for strep throat bronchial inhalers over the counter
https://over-the-counter-drug.com/# potassium supplements over-the-counter
best over the counter nausea medicine best allergy medications over-the-counter
How you can get the new Prince William 40th birthday 5 coin PRINCE WILLIAM will appear on a new 5 coin as part of his 40th birthday celebrations take viagra
over the counter anti nausea medication over the counter asthma inhalers
is viagra over the counter best over the counter skin tag removal
over the counter ear drops guaranteed suicide over the counter
cvs over the counter covid test best over the counter skin tag removal
over the counter acid reflux medicine bronchial inhalers over the counter
https://stromectol.science/# what does minocycline treat
https://doxycycline.science/# generic for doxycycline
п»їMedicament prescribing information. Learn about the side effects, dosages, and interactions.
ivermectin usa price
Best and news about drug. Get information now.
All trends of medicament. Some are medicines that help people when doctors prescribe.
https://stromectolst.com/# ivermectin 6
Some trends of drugs. Get warning information here.
Long-Term Effects. Read information now.
https://stromectolst.com/# ivermectin cost canada
Read now. Commonly Used Drugs Charts.
Commonly Used Drugs Charts. Cautions.
https://stromectolst.com/# ivermectin over the counter canada
Everything what you want to know about pills. Everything information about medication.
Drugs information sheet. Some trends of drugs.
ivermectin where to buy
Everything information about medication. Comprehensive side effect and adverse reaction information.
Doses up to 80 mg day have been used; however, they do not show a greater effect where to buy cialis online safely
п»їMedicament prescribing information. Learn about the side effects, dosages, and interactions.
https://stromectolst.com/# ivermectin 3mg tablets
Prescription Drug Information, Interactions & Side. Top 100 Searched Drugs.
Learn about the side effects, dosages, and interactions. Read here.
https://stromectolst.com/# stromectol medication
Some are medicines that help people when doctors prescribe. Some are medicines that help people when doctors prescribe.
Actual trends of drug. What side effects can this medication cause?
ivermectin new zealand
Read information now. What side effects can this medication cause?
Long-Term Effects. Get here.
ivermectin uk coronavirus
safe and effective drugs are available. Everything information about medication.
Read here. Long-Term Effects.
stromectol uk buy
All trends of medicament. Read here.
Read now. Get here.
https://stromectolst.com/# buy stromectol online
Comprehensive side effect and adverse reaction information. Everything information about medication.
Long-Term Effects. Comprehensive side effect and adverse reaction information.
ivermectin otc
Get here. Cautions.
Get information now. All trends of medicament.
ivermectin 4 tablets price
Read now. Top 100 Searched Drugs.
Medscape Drugs & Diseases. Long-Term Effects.
ivermectin 50
drug information and news for professionals and consumers. Get here.
Commonly Used Drugs Charts. Some are medicines that help people when doctors prescribe.
stromectol ivermectin 3 mg
What side effects can this medication cause? Read information now.
Cautions. п»їMedicament prescribing information. how to get cheap avodart pills
Comprehensive side effect and adverse reaction information. п»їMedicament prescribing information.
Read information now. Definitive journal of drugs and therapeutics.
cost levaquin without insurance
Long-Term Effects. Best and news about drug.
Read here. Definitive journal of drugs and therapeutics.
how to buy generic mobic without insurance
Generic Name. Everything information about medication.
Read now. drug information and news for professionals and consumers.
get mobic without rx
Drug information. Read here.
Get here. All trends of medicament.
https://lisinopril.science/# lisinopril 5 mg prices
safe and effective drugs are available. safe and effective drugs are available.
What side effects can this medication cause? Some are medicines that help people when doctors prescribe.
https://levaquin.science/# generic levaquin for sale
Top 100 Searched Drugs. Commonly Used Drugs Charts.
Some trends of drugs. Prescription Drug Information, Interactions & Side.
nexium rx
Everything what you want to know about pills. Read information now.
earch our drug database. Drug information.
cost mobic online
Some trends of drugs. Get here.
Learn about the side effects, dosages, and interactions. Comprehensive side effect and adverse reaction information. buy cheap avodart no prescription
Prescription Drug Information, Interactions & Side. Comprehensive side effect and adverse reaction information.
Read now. Everything information about medication. can i buy generic avodart prices
Drug information. What side effects can this medication cause?
Comprehensive side effect and adverse reaction information. Long-Term Effects.
https://lisinopril.science/# prinivil drug
earch our drug database. Top 100 Searched Drugs.
Comprehensive side effect and adverse reaction information. Get here.
https://mobic.store/# can i purchase generic mobic no prescription
Read information now. Comprehensive side effect and adverse reaction information.
All trends of medicament. Get here.
cost of generic propecia for sale
All trends of medicament. Everything what you want to know about pills.
Actual trends of drug. Long-Term Effects.
order cheap propecia prices
Cautions. Prescription Drug Information, Interactions & Side.
Everything about medicine. Top 100 Searched Drugs.
how can i get cheap propecia
safe and effective drugs are available. Read information now.
Definitive journal of drugs and therapeutics. safe and effective drugs are available.
https://azithromycins.com/ zithromax tablets for sale
Learn about the side effects, dosages, and interactions. Drugs information sheet.
What side effects can this medication cause? Definitive journal of drugs and therapeutics. https://amoxicillins.online/ amoxicillin 500mg price canada
Comprehensive side effect and adverse reaction information. Commonly Used Drugs Charts.
Everything what you want to know about pills. Learn about the side effects, dosages, and interactions.
https://clomiphenes.com can you buy clomid now
Medscape Drugs & Diseases. Learn about the side effects, dosages, and interactions.
Comprehensive side effect and adverse reaction information. Get here.
cost clomid tablets
Top 100 Searched Drugs. Everything what you want to know about pills.
Everything about medicine. Everything about medicine. amoxicillin 825 mg
safe and effective drugs are available. Commonly Used Drugs Charts.
Everything what you want to know about pills. Generic Name.
https://azithromycins.online/ buy cheap generic zithromax
Drug information. drug information and news for professionals and consumers.
earch our drug database. Medscape Drugs & Diseases.
https://clomiphenes.online can you get generic clomid without rx
drug information and news for professionals and consumers. Read information now.
п»їMedicament prescribing information. Everything about medicine.
https://clomiphenes.com clomid without prescription
earch our drug database. earch our drug database.
Medscape Drugs & Diseases. Get information now.
https://azithromycins.com/ can i buy zithromax over the counter
Everything what you want to know about pills. п»їMedicament prescribing information.
Get here. Read here.
https://finasteridest.com/ where to buy generic propecia without a prescription
Drug information. Read now.
Read now. Read information now.
cost cheap propecia without insurance
Best and news about drug. Top 100 Searched Drugs.
Everything information about medication. Comprehensive side effect and adverse reaction information.
zithromax 500 mg for sale
earch our drug database. earch our drug database.
Actual trends of drug. Get information now.
zithromax 500 mg for sale
Long-Term Effects. Best and news about drug.
Read now. Everything about medicine.
medicine for impotence
Read information now. Some are medicines that help people when doctors prescribe.
Best and news about drug. Get here.
best ed pill
safe and effective drugs are available. Read information now.
Drug information. Actual trends of drug.
best pills for ed
Everything what you want to know about pills. Everything what you want to know about pills.
Definitive journal of drugs and therapeutics. Some trends of drugs.
https://edonlinefast.com medicine for impotence
Everything information about medication. Read information now.
Top 100 Searched Drugs. All trends of medicament.
ed pills for sale
Best and news about drug. Read now.
Get warning information here. Prescription Drug Information, Interactions & Side.
https://edonlinefast.com ed pills otc
Drug information. Get warning information here.
Read here. Prescription Drug Information, Interactions & Side. https://amoxicillins.com/ amoxicillin brand name
Drugs information sheet. Actual trends of drug.
safe and effective drugs are available. Top 100 Searched Drugs.
https://edonlinefast.com treatments for ed
Some trends of drugs. Read information now.
Cautions. All trends of medicament.
https://edonlinefast.com п»їerectile dysfunction medication
Some trends of drugs. Best and news about drug.
Comprehensive side effect and adverse reaction information. Medscape Drugs & Diseases.
carprofen without vet prescription
Definitive journal of drugs and therapeutics. Medicament prescribing information.
Some trends of drugs. Some trends of drugs.
https://canadianfast.online/# ed prescription drugs
Get information now. Learn about the side effects, dosages, and interactions.
Best and news about drug. Read here.
online canadian pharmacy
Cautions. earch our drug database.
What side effects can this medication cause? drug information and news for professionals and consumers.
https://canadianfast.com/# buy anti biotics without prescription
What side effects can this medication cause? safe and effective drugs are available.
Read information now. Generic Name.
canadian pharmacy tampa
All trends of medicament. Medscape Drugs & Diseases.
earch our drug database. Drugs information sheet.
https://canadianfast.online/# buy canadian drugs
Definitive journal of drugs and therapeutics. Everything information about medication.
Commonly Used Drugs Charts. Some are medicines that help people when doctors prescribe.
https://canadianfast.com/# comfortis for dogs without vet prescription
Some are medicines that help people when doctors prescribe. Definitive journal of drugs and therapeutics.
Everything what you want to know about pills. earch our drug database.
cheap pet meds without vet prescription
Actual trends of drug. п»їMedicament prescribing information.
Read information now. Medscape Drugs & Diseases.
cvs prescription prices without insurance
earch our drug database. Read information now.
Medscape Drugs & Diseases. Comprehensive side effect and adverse reaction information.
https://canadianfast.online/# buy prescription drugs online
Some are medicines that help people when doctors prescribe. Everything about medicine.
Top 100 Searched Drugs. Top 100 Searched Drugs.
online canadian drugstore
Read information now. safe and effective drugs are available.
Get warning information here. Everything about medicine.
https://canadianfast.com/# carprofen without vet prescription
Read information now. Everything information about medication.
earch our drug database. Commonly Used Drugs Charts.
https://canadianfast.online/# non prescription ed pills
Read information now. earch our drug database.
drug information and news for professionals and consumers. Learn about the side effects, dosages, and interactions.
https://canadianfast.online/# canadian pharmacy online
Get here. Definitive journal of drugs and therapeutics.
Prescription Drug Information, Interactions & Side. All trends of medicament.
prescription drugs without doctor approval
Drugs information sheet. Read information now.
1231143 pmid 23287718 azithromycin antibiotic Life threatening neurotoxicity also has been observed
Long-Term Effects. earch our drug database.
sildenafil in india online
drug information and news for professionals and consumers. drug information and news for professionals and consumers.
Prescription Drug Information, Interactions & Side. Medscape Drugs & Diseases.
walmart viagra prescriptions
Medscape Drugs & Diseases. Cautions.
Top 100 Searched Drugs. Comprehensive side effect and adverse reaction information.
viagra samples walgreens
Read here. Learn about the side effects, dosages, and interactions.
Get warning information here. Everything what you want to know about pills.
best prices sildenafil
Medicament prescribing information. Drug information.
Top 100 Searched Drugs. Drugs information sheet.
viagra super active vs. viagra professional
Generic Name. Medscape Drugs & Diseases.
Read information now. Generic Name.
https://viagrapillsild.com/# sildenafil free shipping
Drug information. Learn about the side effects, dosages, and interactions.
earch our drug database. Some trends of drugs.
how expensive is viagra
Generic Name. Read information now.
Cautions. Drug information.
purchase tadalafil online
Commonly Used Drugs Charts. Read here.
What side effects can this medication cause? Get warning information here.
cheap generic cialis in the us
Read here. Drugs information sheet.
Everything about medicine. Definitive journal of drugs and therapeutics.
genic cialis
Medscape Drugs & Diseases. Medscape Drugs & Diseases.
Best and news about drug. Medscape Drugs & Diseases.
cialis without prescriptions uk
Prescription Drug Information, Interactions & Side. Everything about medicine.
п»їMedicament prescribing information. Get warning information here.
buy tadalafil uk
Read information now. earch our drug database.
Actual trends of drug. Actual trends of drug.
buy tadalafil 5mg online
Read now. Everything about medicine.
Drugs information sheet. earch our drug database.
cialis vs. viagra recreational use
Prescription Drug Information, Interactions & Side. Comprehensive side effect and adverse reaction information.
Get here. Actual trends of drug.
https://tadalafil1st.online/# cialis canadian pharmacy
п»їMedicament prescribing information. Comprehensive side effect and adverse reaction information.
п»їMedicament prescribing information. Comprehensive side effect and adverse reaction information.
tadalafil 5mg best price
What side effects can this medication cause? Learn about the side effects, dosages, and interactions.
Some trends of drugs. Long-Term Effects.
tadalafil 2.5 mg online india
Drugs information sheet. Long-Term Effects.
What side effects can this medication cause? Best and news about drug.
generic cialis with dapoxetine 80mg
Cautions. Cautions.
Get information now. Definitive journal of drugs and therapeutics.
https://tadalafil1st.online/# lowest price on cialis 200 mg
Read information now. Some are medicines that help people when doctors prescribe.
drug information and news for professionals and consumers. safe and effective drugs are available.
where to buy cialis in calgary safely
Read here. earch our drug database.
Commonly Used Drugs Charts. Read information now.
prednisone 5 mg brand name
safe and effective drugs are available. What side effects can this medication cause?
Read now. Read information now.
cost of propecia without dr prescription
Commonly Used Drugs Charts. Everything information about medication.
Drugs information sheet. Generic Name.
amoxicillin tablets in india
Generic Name. Cautions.
sildenafil teva sildenafil 100 mg tablet generic viagra india
200 mg viagra sildenafil cost buy sildenafil
ivermectin pyrantel pamoate ivermectin for guinea pigs ivermectin 3 mg scabies
cialis 5mg price cialis online cheap what happens if you take 2 cialis
ed problems treatment online canadian pharmacy canadian drugs online
buy prescription drugs without doctor: ed in men – buy erection pills
ed treatment natural: psychological ed treatment – cheap pills online
cheap ed medication real viagra without a doctor prescription injections for ed
cheap medication online buy prescription drugs from india ed cures
Viagra Tabletten fГјr MГ¤nner: Sildenafil Preis – Viagra Generika Schweiz rezeptfrei
Acheter viagra en ligne livraison 24h: Viagra pas cher inde – Viagra homme sans prescription
comprar viagra sin gastos de envГo: se puede comprar sildenafil sin receta – viagra online cerca de bilbao
viagra 50 mg prezzo in farmacia: gel per erezione in farmacia – viagra 50 mg prezzo in farmacia
Sildenafil kaufen online: Viagra online kaufen legal Г–sterreich – Billig Viagra bestellen ohne Rezept
Viagra homme prix en pharmacie: Viagra vente libre pays – Prix du Viagra en pharmacie en France
comprar viagra en espaГ±a envio urgente contrareembolso: comprar viagra sin gastos de envГo – sildenafilo 100mg precio espaГ±a
viagra cosa serve: viagra originale in 24 ore contrassegno – cialis farmacia senza ricetta
Acheter viagra en ligne livraison 24h: SildГ©nafil 100 mg sans ordonnance – Viagra femme ou trouver
no prescription canadian pharmacy
sildenafilo 100mg farmacia: farmacia gibraltar online viagra – sildenafilo cinfa sin receta
Nicely put. Many thanks!
pay for writing essay essay pay
Cheers. Useful information!
professional essay writers reviews what to write for about me on resume essay writer salary
Viagra sans ordonnance 24h Amazon: SildГ©nafil 100 mg sans ordonnance – Viagra 100 mg sans ordonnance
Kudos, Numerous advice!
who can i pay to write my paper for me write my academic essay i forgot to do my essay
Viagra kaufen gГјnstig Deutschland: Viagra online bestellen Schweiz Erfahrungen – Viagra kaufen ohne Rezept Schweiz
Viagra sans ordonnance pharmacie France: Viagra homme prix en pharmacie sans ordonnance – SildГ©nafil 100 mg prix en pharmacie en France
sildenafil 100mg genГ©rico: se puede comprar viagra sin receta – sildenafilo sandoz 100 mg precio
comprar viagra contrareembolso 48 horas: comprar viagra en espaГ±a envio urgente contrareembolso – comprar viagra contrareembolso 48 horas
my canadian drugstore
Viagra femme sans ordonnance 24h: Viagra homme prix en pharmacie sans ordonnance – Viagra Pfizer sans ordonnance
Viagra online cerca de Madrid: Viagra online cerca de Madrid – viagra online cerca de bilbao
comprar sildenafilo cinfa 100 mg espaГ±a: venta de viagra a domicilio – comprar viagra en espaГ±a envio urgente
Awesome info, Thanks a lot.
lucky creek online casino mgm michigan online casino caesar casino online
https://drugswithoutdrprescriptions.com/# prescription price checker
viagra online cerca de zaragoza: sildenafilo sandoz 100 mg precio – comprar viagra en espaГ±a amazon
canadian prescription prices
canada drug
sildenafilo 50 mg precio sin receta: sildenafil 100mg genГ©rico – comprar viagra en espaГ±a envio urgente contrareembolso
se puede comprar sildenafil sin receta: viagra online cerca de malaga – comprar viagra en espaГ±a envio urgente
https://drugswithoutdrprescriptions.com/# buy canadian drugs online
canadian pharmacy prescription
sildenafilo cinfa 25 mg precio: viagra online gibraltar – viagra online cerca de la coruГ±a
I was suggested this website by my cousin. I am not sure whether this post
is written by him as no one else know such detailed about my
trouble. You are amazing! Thanks!
viagra ordine telefonico dove acquistare viagra in modo sicuro viagra online in 2 giorni
miglior sito dove acquistare viagra miglior sito per comprare viagra online viagra online in 2 giorni
https://viasenzaricetta.com/# viagra online in 2 giorni
pharmacy canada online
canadian prescription drugstore
canadian pharmacy pain meds
overseas pharmacies shipping to usa
viagra naturale in farmacia senza ricetta alternativa al viagra senza ricetta in farmacia viagra naturale
canadian pharmacies no prescription needed
canadian prescription prices
https://viasenzaricetta.com/# farmacia senza ricetta recensioni
canadian pharmacy shop
https://doxycyclinesale.pro/# doxycycline over the counter
Howdy! This is kind of off topic but I need some advice from an established blog.
Is it very hard to set up your own blog? I’m not very techincal but I can figure things
out pretty fast. I’m thinking about creating my own but I’m not
sure where to start. Do you have any points or suggestions?
With thanks
certified canadian international pharmacy
https://prednisonesale.pro/# prednisone 10
MS raw files were processed for protein identification and quantitation using MaxQuant v 1 tadalafil generic vs cialis
drugs without a doctor s prescription
https://zithromax.pro/# purchase zithromax online
The Bank is always open to spin for free and go for 10 total Jackpots! Who needs Vegas casino games when you have the glitz, glamour of two fan favorite features, Classic Star and Rapid Fire, PLUS Super Bonus! Especially for those who are not yet so well-versed in the areas of slots and gambling, playing free slot games is a great place to start. This will enable you to get to know an online slot machine, inside and out, with no restrictions to the amount of time you can spend. Absolutely! There are so many amazing casinos online offering great free slot machines right now. In fact, the hardest part is choosing which game to play first. If you’re new to online slots check out our recommended slot casinos to get started. Furthermore, the providers have used the latest HTML5 technology to optimize their free casino slots no download no registration for a multi-platform affair, and run as smoothly on mobile phones as on desktops. Here are some of the top providers in the iGaming market along with their top free slot machines no download and characteristic features.
https://kyleryywt418418.blogchaat.com/18031580/best-new-online-slots-in-philippines
Kecanggihan serta perkembangan zaman tentu menuntut para agen terus berkembang dalam membuat jalannya permainan menjadi lebih optimal. Diketahui masih banyak situs slot yang tidak mementingkan pengoptimalan dalam menjaga para membernya. Inilah yang akan membuat para member geram dan mencari situs slot online gacor lain. Di Slot Gacor kami mempunyai visi dan misi yaitu tetap memberikan pengoptimalan dalam melayani, serta menjaga kerahasian data privasi seluruh member. Selain kami merupakan situs terlengkap slot RTP tinggi kami merupakan situs yang selalu memberikan pengalaman bermain menyenangkan. Memiliki tampilan situs yang sangat memukau sehingga membuat pemain tidak mudah bosan untuk menikmati beragam game slot gacor apapun disini. Tampilan gamenya yang sangat seru dan menarik sehingga sangat menyenangkan untuk dicoba. Daftar slot sekarang juga sehingga bisa bermain dengan tenang dan memuaskan di dalam agen slot pragmatic kami.
http://prednisonesale.pro/# prednisone uk buy
buy medicines online in india overseas pharmacies shipping to usa buy medicines online in india
reputable mexican pharmacies online: mexican border pharmacies shipping to usa – mexican rx online
canadian pharmacy uk delivery trustworthy canadian pharmacy canadian pharmacy meds review
indian pharmacy online: overseas pharmacies shipping to usa – pharmacy website india
mexican rx online mexico drug stores pharmacies buying prescription drugs in mexico online
medicine in mexico pharmacies mexico drug stores pharmacies buying from online mexican pharmacy
Number of live games currently playing: 8 Sofascore Football livescore is available as iPhone and iPad app, Android app on Google Play and Windows phone app. You can find us in all stores on different languages searching for “Sofascore”. Install Sofascore app and follow all Everton matches live on your mobile! For information regarding advertising, employment, results or general enquiries please Contact Us You can click on any player from the roster on the right and see his personal information such as nationality, date of birth, height, preferred foot, position, player value, transfer history etc. There are also statistics for each player in all competitions with all total played and started matches, minutes played, number of goals scored, number of cards and much more. Everton top scorers list is updated live during every match.
http://www.aotingmei.com/bbs/board.php?bo_table=free&wr_id=48888
Cons To make sure that all features of this website work, please update your browser to the latest version and check that Javascript and Cookies are enabled. Click on the News tab and you will be supplied by the latest news from that league. Sometimes this is in the local language for that league, but mostly it is in English. Cons Click on the News tab and you will be supplied by the latest news from that league. Sometimes this is in the local language for that league, but mostly it is in English. Developer! Analyse your app: Cons To make sure that all features of this website work, please update your browser to the latest version and check that Javascript and Cookies are enabled. Your browser is out of date or some of its features are disabled, it may not display this website or some of its parts correctly.
india online pharmacy: pharmacy website india – mail order pharmacy india
doxycycline: doxycycline – doxycycline 500mg
buy doxycycline monohydrate: doxycycline 50 mg – buy doxycycline hyclate 100mg without a rx
canadian pharmacies review
■ С осторожностью используйте средства при аллергических заболеваниях и склонности к воспалительным реакциям. При первых же признаках побочных эффектов от стимуляторов роста надо отказаться. Сразу хочу сказать, что я абсолютно против использования лекарства (капель от глаукомы) для получения косметического эффекта! На мой взгляд, это все равно что есть таблетки с паразитами для похудения. (Думаю, многие помнят такой способ похудения). Механизм действия биматопроста на фолликулы пока окончательно не выяснен — возможно, усиление роста волос происходит за счет непосредственного влияния на фолликулярные рецепторы или опосредованно — благодаря улучшению местного кровообращения. Ну если у некоторых дамочек вообще мозгов нет и они готовы зрением рисковать ради ресниц, то это их проблемы. Пусть мажут что хотят.
https://gunnereecy740741.ltfblog.com/19576874/какое-масло-для-роста-ресниц-самое-эффективное
Вы можете купить массажеры для лица прямо сейчас на сайте и в мобильном приложении “Золотое яблоко”. Средство для роста бровей | 2014 © Салон-парикмахерская “Женева” Екатеринбург, ул. Декабристов, 16/18 Б Салон красоты “Шоколад” приглашает вас ежедневно с 10:00 до 22:00. Рекомендую! В студии загара “Шоколад” установлен дополнительный солярий PREMIUM-класса! Производство Германии. В солярии 54 мощные лампы по 200 ватт, аква-бриз, арома. Теперь загар в солярии стал еще приятнее. Приходите, насладитесь комфортом, получите порцию красоты и удовольствия! Наш салон работает для Вас: Акции и предложения от нас Массажер для лица Revolution Следующий шаг: оформление заказа Охлаждающий ролик-массажер для лица Смягчает и массажирует кожу Успокаивает покрасневшую и раздраженную кожу Можно хранить в холодильнике или в морозильной камере Товар не подлежит возврату п…
zithromax 1000 mg pills: where can i buy zithromax capsules – where to buy zithromax in canada
doxycycline online: order doxycycline 100mg without prescription – doxycycline monohydrate
get antibiotics without seeing a doctor: buy antibiotics online – buy antibiotics
order doxycycline: doxycycline 100mg dogs – doxycycline tetracycline
pharmacy cost comparison
cipro online no prescription in the usa: buy cipro – cipro for sale
cipro for sale: ciprofloxacin over the counter – ciprofloxacin mail online
purchase doxycycline online: doxycycline 100mg price – doxycycline 100mg
200 mg doxycycline: doxycycline 100mg tablets – doxycycline
Over the counter antibiotics for infection: get antibiotics without seeing a doctor – antibiotic without presription
http://overthecounter.pro/# jock itch treatment over-the-counter
over the counter water pills: over the counter ed pills – over the counter steroid cream
Com vantagem de três pontos, o Palmeiras segue na liderança do Brasileirão. Logo atrás, Corinthians, Flamengo, Fluminense e Athletico brigam para alcançarem o rival e quem sabe lutar pelo título da temporada. Sobre o Google Play Mas não só clubes, como também jogadores, técnicos, dirigentes, além de suas maravilhosas torcidas. Ou seja, tudo será abordado por aqui. Além, é claro, de polêmicas, opiniões e, principalmente, entrevistas com jornalistas, jogadores, técnicos, dirigentes e até torcedores, brasileiros ou não, que acompanham de perto das competições. Home – Brasileirão Série A – Veja os resultados da 34ª rodada e a tabela de classificação do Brasileirão Parece legal, mas ficamos 16 pontos atrás do maior rival ou renova tirando os veteranos e pés de rato ou vai passar vergonha na liberta.
https://ricardozzxw539630.bloggactif.com/20385471/placar-do-jogo-do-atlético
Novos valores das mensalidades dos associados do clube Sofascore Futebol resultados ao vivo resultados ao vivo disponível para iPhone e iPad app, Android app na Google Play e Windows phone app. Você pode nos encontrar em todas as lojas em diferentes idiomas procurando por “Sofascore”. Instale Sofascore app e acompanhe todas partidas do São Paulo U20 ao vivo no seu aparelho! Do UOL, em São Paulo Com as trocas, o Corinthians mudou suas peças dentro de campo: Róger Guedes passou a jogar pela esquerda, enquanto Willian mudou de lado e jogou pelo lado direito. Cantillo ficou com o cargo de primeiro volante. Milhões de beneficiários esperam o pagamento do décimo terceiro do Auxílio Brasil © 2023 Meu Jogo do Bicho. Todos os direitos reservados. Desenvolvido por F5 Digital Do UOL, em São Paulo
uti over the counter: over the counter ed medication – yeast infection treatment over the counter
http://overthecounter.pro/# over the counter cough medicine
I was suggested this blog by my cousin. I’m not sure whether this post is written by him as
no one else know such detailed about my trouble. You are amazing!
Thanks!
epinephrine over the counter: over the counter ed medication – what does over the counter mean
http://overthecounter.pro/# over the counter pink eye medicine
legal canadian pharmacy online: most reliable online pharmacies – most reliable online pharmacy
erectile dysfunction drugs top rated ed pills best ed pills at gnc
ed drugs: top rated ed pills – best otc ed pills
canadian pharmacies for cialis online pharmacies no prescriptions pharmacy canada online
cheap ed drugs: over the counter erectile dysfunction pills – best pills for ed
canadian online pharmacies prescription drugs
https://edpills.pro/# buy ed pills
canadian drug stores online list of approved canadian pharmacies canadian discount pharmacy
price medication: canadian online pharmacy no prescription – canada drug store
http://indianpharmacy.pro/# mail order pharmacy india
indianpharmacy com online shopping pharmacy india Online medicine home delivery
https://indianpharmacy.pro/# best online pharmacy india
https://indianpharmacy.pro/# indian pharmacy online
https://indianpharmacy.pro/# reputable indian online pharmacy
https://indianpharmacy.pro/# reputable indian pharmacies
pharmacy website india online shopping pharmacy india top online pharmacy india
http://edmeds.pro/# generic ed pills
https://pharmst.pro/# online pharmacy
list of mexican pharmacies – legitimate canadian mail order pharmacies canadian prescription drugs online
https://fastdeliverypill.com/# international pharmacies that ship to the usa
canadian xanax – drugs without a doctor s prescription canadian pharma companies
https://fastdeliverypill.com/# rx prices
cheapest cialis generic online Abstract Introduction Adjuvant endocrine therapy is an integral compo nent of care for endocrine dependent breast cancer
prescription drug pricing – legitimate canadian mail order pharmacies cheap prescription drugs online
https://fastdeliverypill.com/# reliable online drugstore
canadian pharmacy antibiotics – prescription drugs without prior prescription best online pharmacies without prescription
https://fastdeliverypill.com/# reputable online canadian pharmacies
canadian pharmacies that deliver to the us – legitimate canadian mail order pharmacies canadian mail order drug companies
أكبر شركة لانتاج أنابيب البولي ايثيلين و يو بي سي ومستلزماتها للمنتجات الصناعية في عيراق
http://pharmacyindia.pro/# indian pharmacy
indian pharmacies safe: buy medicines online in india – india pharmacy mail order
http://cialiswithoutprescription.pro/# cialis sale online
cialis pill canada: Cialis without a doctor prescription – generic cialis no prescription australia
https://canadiandrugs.pro/# medication canadian pharmacy
san antonio cialis doctor: buy Tadalafil 20mg – buy cialis online usa
http://cialiswithoutprescription.pro/# supreme suppliers cialis
cialis black online: Cialis without a doctor prescription – cialis australia no prescription
https://pharmacyindia.pro/# Online medicine order
mail order pharmacy india: indian pharmacy online – buy medicines online in india
http://canadiandrugs.pro/# canadian pharmacy uk delivery
http://pharmacyindia.pro/# buy prescription drugs from india
cialis with dapoxetine or viagra with dapoxetine better: buy Cialis 20mg – whats better cialis or viagra
http://cytotecpills.pro/# how to get cytotec online
п»їcipro generic: buy cipro – ciprofloxacin over the counter
https://prednisonepills.pro/# prednisone otc price
online prednisone: prednisone over the counter – prednisone 10 mg brand name
https://cytotecpills.pro/# where to get cytotec pills
ciprofloxacin mail online: ciprofloxacin – antibiotics cipro
https://cytotecpills.pro/# п»їcytotec pills online
https://edpillsfd.online/# the best ed pills
canadian pharmacy without prescription: online pharmacy no prescription – canadian pharmacies that deliver to the us
buy cialis online without a prescription Mirtazapine and renal transplant
http://indiapharmfd.com/# pharmacy website india
indian pharmacies safe: indian pharmacy paypal – online pharmacy india
https://indiapharmfd.com/# Online medicine order
online pharmacy drop shipping: online pharmacy no prescription – buying prescription drugs from canada
pharmacy online uae: trusted online pharmacy reviews – canadian family pharmacy
http://edpillsfd.com/# best ed medication
male ed drugs: ed meds online without doctor prescription – best ed pills non prescription
https://indiapharmfd.online/# indian pharmacy online
pharmacy canadian: certified canadian international pharmacy – indian pharmacies safe
https://edpillsfd.online/# best ed drugs
ed drugs compared: buy ed pills online – new treatments for ed
ed pills comparison: ed medications online – ed treatment pills
can i get propecia prices: Best place to buy finasteride – can i get propecia without rx
https://dapoxetine.pro/# priligy over the counter
https://dapoxetine.pro/# Priligy price
cheap kamagra oral jelly: buy kamagra online – buy kamagra online
https://kamagratabs.pro/# buy kamagra online
There is definately a lot to find out about this subject. I like all the points you made
can i purchase generic propecia no prescription: Best place to buy finasteride – can i buy propecia without a prescription
And two, this topic necessary itt is personal dedicated section that will enable us
to clarify casino bonuses in detail.
Feel free to surf to my homepage :: 롸쓰고주소
https://kamagratabs.pro/# kamagra
where to buy propecia online: where to buy cheap propecia online – cost cheap propecia no prescription
Incredible points. Outstanding arguments.
Keep up the great effort.
https://dapoxetine.pro/# dapoxetine online USA
where to buy cheap propecia for sale: Buy Finasteride online – where to get generic propecia for sale
https://kamagratabs.pro/# Oral Jelly 100mg Kamagra price
cost cheap propecia no prescription: Buy Finasteride online – propecia prices
https://dapoxetine.pro/# priligy over the counter
https://dapoxetine.pro/# Priligy price
https://propecia.pro/# can you get generic propecia without a prescription
Priligy price: priligy – priligy
https://dapoxetine.pro/# Priligy 60 mg online
Buy Dapoxetine: Priligy 60 mg online – dapoxetine online USA
https://dapoxetine.pro/# priligy over the counter
Our Company is one of the largest independent full-service retail broking house in India in terms of active clients on NSE as of 2018-19. We are a technology led financial services company, that provides broking and advisory services, margin funding, loans against shares… Know More FDI is the considered as one of the primary means of acquiring external assistance. The countries where the availability of finance is quite low can get finance from developed countries having the good financial condition. There are a number of ways through which a foreign investor can get controlling ownership like by way of merger or acquisition, by purchasing shares, by participating in a joint venture or by incorporating a wholly owned subsidiary. The Official List of Section 13(f) Securities primarily includes U.S. exchange-traded stocks (e.g., NYSE, AMEX, NASDAQ), shares of closed-end investment companies, and shares of exchange-traded funds (ETFs). Certain convertible debt securities, equity options, and warrants are on the Official List and may be reported. But see Section 13(f)(4) (referring to equity securities of a class referred to in Exchange Act section 13(d)(1)) and exemptive rules 12a-4 and 12a-9 under the Exchange Act.
https://wiki-view.win/index.php?title=Amc_stock_reddit
The potential market cap would be $3,092m based on the market consensus. 7 Wall Street analysts have issued “buy,” “hold,” and “sell” ratings for Volta in the last twelve months. There are currently 1 sell rating, 5 hold ratings and 1 buy rating for the stock. The consensus among Wall Street analysts is that investors should “hold” VLTA shares. A hold rating indicates that analysts believe investors should maintain any existing positions they have in VLTA, but not buy additional shares or sell existing shares. View VLTA analyst ratings or view top-rated stocks. For related articles, visit the 5G Mobile Topic Center. Intralogistics expert Craig Henry, U.S. Industry Manager for Intralogistics at Siemens, joins Getting Smart and walks us through the rapidly evolving industrial landscape. Craig discusses how automation, robotics, and digitalization are critical for shaping the future of various sectors.
https://propecia.pro/# buying propecia without prescription
cheap kamagra oral jelly: Oral Jelly 100mg Kamagra price – Kamagra Gold 100mg price
https://kamagratabs.pro/# kamagra tablets usa
buy priligy: Priligy tablets – Buy Dapoxetine
Списъкът с доставчици на казино игри е много голям – в сайта ще откриете най-популярните игри на EGT, StakeLogic, Netent и др. StakeLogic има над 75 достъпни игри, като вие ще се натъкнете на популярните слотове като Book Of Leo Quattro, Book Of Charms Quattro, Black Gold Megaways и др. Освен това имате възможност да играете и по-новите игри – Grand Slam Deluxe и Fruit Spinner. Повечето безплатни казино игри ви позволяват да тествате играта. Като го играете многократно, ще можете да създадете стратегия, за да го победите, което е голямо предимство. Ако играете безплатно, можете да анализирате играта и да определите най-добрата стратегия за използване.
https://dantevuro296285.bloggin-ads.com/41835757/Онлайн-Бакара-бонус-регистрация
Например, при електронната бакара на Betsoft няма опции за странични залози както е при тези на Microgaming, Playtech и др., където можете да залагате на Player Banker Pairs, Big Small, Player Banker Bonus и т.н. При повечето разновидности на бакара онлайн от Evolution, изплащането за Tie (равенство) е 11:1, докато при играта Dragon Tiger, изплащането за равенство по боя е 50:1. А ето и малко проценти, с които да подкрепим изказванията си – предимството на компанията за победа на участника е оценено на 1,36%; това за победа на банкера е 1,17%; а при равенство е 14,42%. Както сами виждате, процентите са най-добри при победа на банкера. Именно затова ви насочваме да правите залозите си на Бакара именно там.
http://canadapharmcertified.pro/# canadian drug prices
Бивш мениджър в болницата „Гленийгълс“ в Сингапур ще прекара следващите няколко години „зад решетките“. Причината е кражба на частни пари от болницата и харченето им за хазарт, коли и други подобни. Вашият имейл адрес няма да бъде публикуван. Задължителните полета са отбелязани с * рџЋЃ Казино Джакпоти от 8888 Специално за клиентите на Казино секцията, които са си направили акаунт и са депозирали за първи път се предлага бонус от 1000 лева до 8888 лева. Бонуса е 100% на депозита. Преди да се изтегли бонуса, то той трябва да се превърти и да са спазени правилата и условията на сайта.
https://fair-wiki.win/index.php?title=Book_of_ra_kazino_igri
Оосбено популярна за много онлайн казино фенове е играта HILO, което наподобява по смисъл Блекджек, защото се залага на това каква карта ще ви се падне от тестето – с по-голяма или по-малка стойност от вече изтеглената. Доста любопитни са и миничките, които са познати от детството на много клиенти, играли едноименната игра в старите версии на Windows. За около 7 месеца, той изкачи тима до 6-а позиция в подреждането и класира Леверкузен на полуфиналите на Лига Европа.
best canadian pharmacy online: canadian pharmacy 24 com – canadian pharmacy in canada
http://indiameds.pro/# indian pharmacy
canadian pharmacy prices: canadian pharmacy meds review – reddit canadian pharmacy
http://mexicanpharmacies.pro/# mexican pharmaceuticals online
п»їbest mexican online pharmacies: purple pharmacy mexico price list – purple pharmacy mexico price list
https://mexicanpharmacies.pro/# reputable mexican pharmacies online
canadian pharmacy 24h com: trusted canadian pharmacy – canadian drug
https://mexicanpharmacies.pro/# п»їbest mexican online pharmacies
pharmacies in mexico that ship to usa: mexican drugstore online – mexican drugstore online
https://indiameds.pro/# reputable indian pharmacies
http://canadapharmcertified.pro/# canadian drug prices
https://indiameds.pro/# indian pharmacy online
cheapest online pharmacy india: indian pharmacy paypal – best india pharmacy
https://indiameds.pro/# india online pharmacy
best online pharmacies in mexico: mexican drugstore online – buying prescription drugs in mexico online
http://canadapharmcertified.pro/# canadianpharmacymeds
When you’re ready to make your first deposit or deposit bonus or wagering requirements , which must be at least €10, you can pick from a number of casino payment methods. Use your VISA or MasterCard, an eWallet like Skrill, Neteller, or Trustly, or a card like PaySafeCard are accepted for payment methods. You can also make your deposit by using Trustly, Sofort, Ecopayz, and Trustpay. 1xSlots Casino is owned and operated by Orakum N.V. and holds a Curacao License, numbered 8048 JAZ. The real money casino offers a staggering 50+ currency options, including several banking options. The University of Southern California’s Annual Security and Fire Safety Reports (ASR) for the past three years are available online at: dps.usc.edu alerts annual-report . For the No Deposit Bonus, the primary requirement is to wager x25 of the bonus winnings so that you can claim it. If you have been very lucky and won $100 from the free spins, you will have to wager $2500 in real money so that you can claim the amount in your bonus balance.
https://webranksdirectory.com/website-list-1923/
Pulsz provides a decent range of over 280 casino games. Free slots make up the majority of them. There is something for everyone, including new players and experienced players, in the portfolio of slot games. With filters to help you find what you are searching for, from three-reel classic slots to progressive jackpot slots, it’s easy to find what you want. The fun and exciting online casino games are at your finger tips. You can find all of our guides to learn how to play and win at any casino game. From strategy to tips, we have you covered. Look for your preferred game and learn all about it so you can start playing like a pro. Chumba Casino Lite performs a great job of presenting a professional and interesting experience in terms of visuals and general presentation. The games are well-designed and visually appealing. Thus, users easily get lost in the excitement of the action. Also, the app works smoothly and is easy to navigate. It is a great choice for players of all skill levels.
https://fastpills.pro/# best price prescription drugs
sildenafil price australia: 30 mg sildenafil – sildenafil canada cost
http://fastpills.pro/# the best canadian online pharmacy
https://sildenafilpills.pro/# sildenafil 100 mg tablet usa
There’s several Microsoft games as well. They’ve been entertaining players all around the world since the 1980s. Everyone from procrastinating college students to office workers with a few minutes to kill probably knows all about them. These also include Microsoft: Mahjong and the Microsoft: Ultimate Word Games collection. While they don’t involve cards, you may find yourself spending hours playing them! How quickly can you master them and all the other titles in this awesome batch of free online games? With the game open, right-click (or press and hold) the game button on your task bar and select Pin to task bar . When you close the game, the button will still be there. Simple control for fast gameplay Beat free cell solitaire by getting all 52 cards into the four suit-oriented foundations in the top-right.
https://forum.thefishy.co.uk/Blah.pl?m-1365421392/
Koronis Rift is one of the earliest games created by LucasArts (aka Lucasfilm Games). It was designed and produced by Noah Falstein, and it was released initially, in 1985, for the Atari 8-bit computers. Walking War Robots lets you step into your own war machine on your mobile device or PC as you battle it out against other players in quick matches to earn prestige, currency and ultimately advance your mech abilities. Offering a wide range of robots for you to take into battle and a steadily growing community of robot drivers Walking War Robots is one of the few games offering this sort of gameplay particularly in the mobile space. Matches take place on a variety of open maps in 6v6 domination b… Table of Contents “Thank you for updating this classic to Windows. I have missed playing this game. Shrapnel Games has a new loyal customer. And tell the developers they rock!”
https://sildenafilpills.pro/# sildenafil 100mg tablets canada
https://fastpills.pro/# mexican border pharmacies
how to hack aviator how to play aviator how to play aviator on betway
Observamos con frecuencia que los apostadores, entonces es hora de probar el juego de tragamonedas en línea Hot Twenty gratuito. Los símbolos de bajo pago se componen de palos de naipes, Lannister. Elija el sitio para apostar en Virginia Occidental que le permitirá jugar todos sus juegos favoritos, consulte nuestra revisión completa de 10bet y por qué la calificamos con 4 de 5 estrellas. Juegos gratis de giros para jugar en segundo lugar, la reposición de la cuenta sin conversión le permite ahorrar en la comisión del sistema de pago. Ciertos casinos ofrecen bonos de no depósito, que permiten a sus jugadores que apuestan por primera vez en la plataforma beneficiarse del regalo de un saldo gratis para jugar online, sin necesidad de depositar una cantidad de dinero previa en el casino. El objetivo de estos regalos es incentivar el juego e invitar a los nuevos usuarios a probar las funcionalidades del sitio web.
https://juliusavog279591.blogofchange.com/23773036/juegos-gratis-jugar-ahora
Los casinos online, generalmente, tienen una conducta específica. Los demos atienden indirectamente una solución. Para poder ingresar a un banco de opciones de juegos, se debería pagar una matrícula estándar por acceso. Nosotros hemos democratizado este uso y disponemos de los mejores juegos de casino gratis sin descargar ni registrarse. WestCoastCFB Como Ganar En Las Spins En El Casino 2023 Las máquinas tragamonedas gratis son versiones de demostración para probar juegos gratis con las mismas características que en las slots online por dinero real. Las slots gratis sirven para conocer cómo funciona un juego en la práctica, cuáles son sus funciones de bonificación, el ritmo de juego y las opciones de configuración de los pagos. Tocan lo mismo que en su versión de pago, a excepción de las máquinas tragamonedas online con jackpot en red, porque esta función solo se activa cuando se apuesta dinero real.
https://fastpills.pro/# canadian pharcharmy reviews
buy paxlovid online paxlovid buy Paxlovid buy online
birth control pills: birth control pills delivery – birth control pills online
http://canadianpharm.pro/# onlinecanadianpharmacy 24
п»їbuy birth control pills online: birth control pills delivery – buy birth control over the counter
https://canadianpharm.pro/# buying drugs from canada
paxlovid for sale: Paxlovid over the counter – paxlovid for sale
best canadian pharmacy: canadian pharmacy shipping to USA – onlinecanadianpharmacy 24
https://birthcontrolpills.pro/# price for birth control pills
canadian pharmacy antibiotics: certified canadian pharmacy – canadian pharmacy no scripts
http://canadianpharm.pro/# canadian pharmacies compare
canadian pharmacy victoza certified online pharmacy canada best online canadian pharmacy
paxlovid pill: Paxlovid buy online – п»їpaxlovid
п»їpaxlovid: paxlovid covid – Paxlovid over the counter
https://paxlovid.pro/# paxlovid covid
https://birthcontrolpills.pro/# price for birth control pills
birth control pills delivery: buy birth control over the counter – birth control pills cost
https://canadianpharm.pro/# canadian neighbor pharmacy
paxlovid pharmacy buy paxlovid online paxlovid for sale
birth control pills delivery: birth control pills delivery – birth control pills
http://birthcontrolpills.pro/# birth control pills online
https://paxlovid.pro/# paxlovid india
over the counter birth control pills: birth control pills prescription – birth control pills
https://canadianpharm.pro/# medication canadian pharmacy
canadian pharmacy meds review: canadian pharmacy shipping to USA – canadian drugs
paxlovid cost without insurance Paxlovid over the counter buy paxlovid online
canada drug pharmacy: certified canadian pharmacy – canadianpharmacy com
http://canadianpharm.pro/# safe online pharmacies in canada
http://canadianpharm.pro/# vipps canadian pharmacy
reliable canadian online pharmacy: certified canadian pharmacy – canadian pharmacy world reviews
paxlovid for sale: paxlovid price – paxlovid cost without insurance
https://birthcontrolpills.pro/# buy birth control over the counter
Paxlovid buy online: Paxlovid over the counter – paxlovid for sale
paxlovid covid buy paxlovid online Paxlovid over the counter
https://canadianpharm.pro/# drugs from canada
Paxlovid buy online: paxlovid generic – buy paxlovid online
https://birthcontrolpills.pro/# п»їbuy birth control pills online
canadian mail order pharmacy: best canadian online pharmacy – canadianpharmacymeds com
canada pharmacy: legit canadian pharmacy online – recommended canadian pharmacies
paxlovid for sale: Paxlovid buy online – paxlovid pharmacy
http://birthcontrolpills.pro/# birth control pills prescription
https://paxlovid.pro/# paxlovid cost without insurance
cheap birth control pills over the counter birth control pills birth control pills without seeing a doctor
pharmacy website india: Online medicine order – top online pharmacy india
https://edpills24.pro/# cheapest ed pills
ed dysfunction treatment: best ed treatment – buying ed pills online
https://mexicanpharmacy.life/# mexican rx online
http://edpills24.pro/# best male ed pills
buying from online mexican pharmacy: mexican pharmaceuticals online – best online pharmacies in mexico
http://indiapharmacy.world/# best india pharmacy
top ed drugs: cheapest ed pills online – male ed pills
http://edpills24.pro/# treatment of ed
online shopping pharmacy india top online pharmacy india top 10 online pharmacy in india
pharmacy website india: indian pharmacy online – best online pharmacy india
http://edpills24.pro/# best ed treatment pills
https://edpills24.pro/# male erection pills
Cooler111, USA 2022 04 23 03 59 41 finasteride hairline 1093 humrep deq100 pmid 20435692
mexican online pharmacies prescription drugs: mexican drugstore online – mexican mail order pharmacies
https://edpills24.pro/# online ed pills
https://mexicanpharmacy.life/# mexico drug stores pharmacies
india pharmacy indian pharmacies safe cheapest online pharmacy india
cheapest online pharmacy india: pharmacy website india – indian pharmacy paypal
http://edpills24.pro/# medicine for erectile
The factory’s dedication to quality is evident in the superior performance of their HDPE pipes, which are known for their exceptional strength and durability. Elitepipe Plastic Factory
https://edpills24.pro/# herbal ed treatment
online pharmacy india: india online pharmacy – indian pharmacy online
best non prescription ed pills: pills for erection – ed meds
Hello there, I discovered your blog by way of Google even as searching for a related
matter, your website got here up, it looks great. I’ve
bookmarked it in my google bookmarks.
Hi there, simply was aware of your blog via Google, and located
that it is truly informative. I’m gonna be careful for brussels.
I’ll be grateful when you continue this in future.
A lot of other people can be benefited from your writing. Cheers!
http://mexicanpharmacy.life/# mexico drug stores pharmacies
http://indiapharmacy.world/# buy medicines online in india
canadian pharmacy non prescription drugs
buying prescription drugs in mexico mexico pharmacies prescription drugs purple pharmacy mexico price list
best over the counter ed pills: medicine erectile dysfunction – best ed pills at gnc
ed drugs: ed drugs – buy ed pills
https://indiapharmacy.world/# indian pharmacy paypal
http://mexicanpharmacy.life/# mexican rx online
pharmacies in mexico that ship to usa: mexico pharmacies prescription drugs – buying prescription drugs in mexico online
http://edpills24.pro/# treatment for ed
http://mexicanpharmacy.life/# medication from mexico pharmacy
pharmacies in mexico that ship to usa buying prescription drugs in mexico online п»їbest mexican online pharmacies
mexican mail order pharmacies: buying prescription drugs in mexico – mexico drug stores pharmacies
mexico pharmacies prescription drugs: mexico pharmacies prescription drugs – best online pharmacies in mexico
https://indiapharmacy.world/# india pharmacy mail order
http://indiapharmacy.world/# indian pharmacy
cheap erectile dysfunction pills: best ed pills – how to cure ed
http://edpills24.pro/# ed drug prices
http://indiapharmacy.world/# best online pharmacy india
indian pharmacy: world pharmacy india – indian pharmacies safe
top 10 pharmacies in india reputable indian online pharmacy best india pharmacy
http://edpills24.pro/# the best ed pill
non prescription ed pills: ed pill – erection pills viagra online
https://edpills24.pro/# men’s ed pills
https://mexicanpharmacy.life/# mexico drug stores pharmacies
cheapest ed pills online: new treatments for ed – erectile dysfunction pills
mexican drugstore online: buying from online mexican pharmacy – п»їbest mexican online pharmacies
http://edpills24.pro/# what is the best ed pill
buy Prednisone 20mg canadian online pharmacy prednisone
prednisone daily use buy Prednisone over the counter
https://ciprofloxacin.icu/# ciprofloxacin order online
https://ciprofloxacin.icu/# buy cipro online without prescription
п»їcipro generic cipro pharmacy
PokerStars.eu runs on the following operating systems: Windows. The download file has a size of 100.5MB. There are free-to-play games running non-stop across a huge range of variants and stake levels. The game lobby is easy to navigate on all devices, which makes finding the perfect game a quick journey. Hosted Record $10M Venom There are free-to-play games running non-stop across a huge range of variants and stake levels. The game lobby is easy to navigate on all devices, which makes finding the perfect game a quick journey. At this point you need to choose your preferred language, then agree to the PokerStars download Terms and Conditions, before finally clicking the Install button. Once the installer is finished, PokerStars will automatically launch, and you can click Log In followed by Create New Account.
https://juliet-wiki.win/index.php?title=Free_3d_slots_no_download_no_registration
Grill is your 24 hour casual dining spot at Wind Creek where you can relax and enjoy a meal of AMerican fare cooked to order. Enjoy an 8 ounce prime beef burger with fries, mashed, or even a baked potato or a veggie burger any way you like it. If you like your burgers in a big way, try the 5 pound Creek Burger for under $20. Share it with friends or go for the gusto and get it in your belly in less than half an hour to get your picture on the wall, a t-shirt so you can say ya been there and done that, free entrees for up to 4 of your dinner guests, and of course your burger is free! Located 89 miles southeast of downtown Birmingham, the Wind Creek Casino & Hotel Wetumpka is a contemporary Native American casino set on the banks of the Coosa River. It’s (at the minimum), an hour and 30 minute drive.
prinivil tabs buy lisinopril without prescription
https://ciprofloxacin.icu/# ciprofloxacin generic price
https://prednisone.pro/# prednisone uk buy
buy Prednisolone online pharmacy cost of prednisone
order molnupiravir molnupiravir tablets 200 mg
https://clomiphenecitrate.pro/# clomid
https://prednisone.pro/# 20 mg prednisone tablet
buy clomiphene online buy Clomid online
https://molnupiravir.life/# molnupiravir kaufen
https://clomiphenecitrate.pro/# clomid coupon
https://clomiphenecitrate.pro/# where can i buy clomiphene
It starts with a prison escape and ends with one of the most surprising moments a video game has ever attempted. While it might lack the polish of games that focus on a single mechanic, A Way Out is packed full of variety and never once outstays its welcome. Even if you play it online, the action plays out in split-screen so you can always see what your co-op partner is doing. One minute you might be working together to catch a fish, the next you’re having a shootout while riding a motorbike. When you get a moment to relax, why not enjoy a game of Connect 4? 2 player games cover many different gaming genres for kids and adults like card games, sports games and war games. You can play a relaxing game of Uno with your family, huddled around the same computer. Or you can invite a friend to join you by simply sending him a link to your 2 player game. Choose one of the free two player games and play against each other in basketball, tank or shooting games.
http://www.chunillogis.co.kr/bbs/board.php?bo_table=free&wr_id=23898
This shuffler is Perfect for shuffling up to six decks, one of these American merchant vessels—the Friendship—dropped anchor off the Sumatran town of Quallah Battoo to take on a load of pepper. Although traditional casinos still have their charm, msn game zone casino hands down. William Stranieri is an effective specialist in the field of the executives, you will probably need a special code about 40 to 50 percent of the time. There are the top 7 MSN free online games that you can enjoy in zone.msn. They include: Most of the time, however, people prefer to play MSN games online — there is no need to install anything and what they are looking for is always there, available from multiple devices and just as fun. Hits like Bejeweled, Microsoft Mahjong, Bubble Shooter and many more are the reason so many users keep coming back to this website daily to take a break from their usual routines. Some prefer simplistic concepts and basic graphics, others enjoy fully flashed out 3D visuals and complex gameplay mechanics – there is something for everyone to find in this internet chest of wonders.
prednisone 5 mg tablet without a prescription buy Prednisone 20mg
buy lisinopril without prescription lisinopril 20 mg tablet
price of lisinopril in india buy lisinopril without prescription
https://ciprofloxacin.icu/# where can i buy cipro online
cheap clomid online buy Clomid online
https://prednisone.pro/# buy prednisone canada
So much more than just an online casino, 777 is all about retro style-class glamour, surprise and excitement. Oozing swing and sophistication, optimism and nostalgia, 777 has a unique atmosphere & vibe designed to surprise and delight you. Step inside and take your seat at our exciting Blackjack & Roulette tables. Try your hand at classic card games, Live casino and thrilling video slots. Whatever your style, you’ll find it inside 777. 32Red boasts a plethora of casino games. From traditional card games to the latest state-of-the-art online slots, our line-up has over 1,000 titles in total – and this number is only growing. Even with this staggering collection of games, we have always had the same mindset: quality over quantity. As a result, our titles all supply fun, seamless gaming experiences for players. We also know how important mobile gaming is these days, so we have dedicated ample time and resources to ensuring our games are compatible across desktops, tablets, and mobiles.
https://www.emergbook.win/buffalo-diamond-slot
18+. Welcome bonus for new players only | Maximum bonus is 100% up to £100 | Min. deposit is £10 | No max cash out | Wagering is 40x bonus | Maximum bet with an active bonus is £5. Eligibility is restricted for suspected abuse | Skrill & Neteller deposits excluded for welcome bonus | Cashback when offered, applies to deposits where no bonus is included | Cashback is cash with no restrictions | The best UK online casino bonuses for you will vary depending on your experience, budget and playing style. Newbies will find beginner bonuses best suit their needs. Players with a little more experience playing at online casinos should seek intermediate bonuses. Whereas the most experienced players and high rollers will find expert bonuses best match their needs.
canadian pharmacy ship to the US canadian pharmacy oxycodone
internet pharmacies reputable canadian mail order pharmacy
https://canadianpharmacy.legal/# canadian online pharmacy reviews
At any website where you’re handing over real money, it’s important that the site is safe and secure. Thankfully, this casino takes all the necessary steps to keep its platform secure. All casinos looking to operate in India must be licensed by the Indian Gambling Commission. The Zodiac Casino licence is supplied by the UK Gambling Commission; the casino’s also licensed by the Malta Gaming Authority. Casino play at Zodiac Casino is available only to persons older than 19 years of age, or the legal age of majority in their jurisdiction, whichever is the greater. Minors may not play at this online casino under any circumstances. Feel free to read through our Responsible Gambling Policy for more details. This version gets continuous updates, alongside being the only certified way of starting gameplay experience without any hassle. The official procedure is quite easy since players have to proceed to Play Market, search for ‘Zodiac,’ and wrap all those actions up by clicking on the ‘Install’ button. A separate application will appear on the phone, which will mean that everything was installed smoothly. When it comes to the Zodiac online casino app on Android, the only remaining step is to proceed with a log-in window, which will enter the path to the exciting domain of mobile gambling once and forever.
http://edolamall.com/bbs/board.php?bo_table=free&wr_id=26155
Rivers casinos are some of the best-known properties in the US. BetRivers took its casino online in 2019 and offers one of the biggest choices of casino games online. Players can find excellent slots at BetRivers, table games, keno, live dealers, and more. New players can bag a $1,000 deposit bonus when using the bonus coupon code CASINO1000. To make it easier for you, when a casino bonus code is provided by the online casino, we will include it under the offer. Spinfinity Casino No Deposit Bonus => Get 30 Free Spins on Vegas XL Slot Bonus Code: BESTBONUS Jazz Casino Review – Jazz Casino Deposit Bonus – Online Casino USA JazzCasino is an online casino that is completely registered under the laws of Curacao, where it also got…
https://canadianpharmacy.legal/# my canadian pharmacy reviews
highest rated canadian pharmacy mail order prescription drugs from canada
thecanadianpharmacy com online canadian pharmacy no prescription
https://paxlovid.store/# paxlovid cost without insurance
https://canadianpharmacy.legal/# canadian mail order pharmacy
canadian pharmacy for sildenafil certified canadian international pharmacy
https://canadianpharmacy.legal/# canadian pharmacy online ship to usa
precription drugs from canada canadian pharmacy 365
https://canadianpharmacy.legal/# reddit canadian pharmacy
paxlovid covid paxlovid cost without insurance
paxlovid generic paxlovid for sale
https://certifiedpharmacy.pro/# canadian discount pharmacy
https://certifiedpharmacy.pro/# most trusted canadian online pharmacy
paxlovid generic paxlovid cost without insurance
I was wondering if you ever considered changing the layout of your
site? Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so people
could connect with it better. Youve got an awful lot of text for only
having one or two pictures. Maybe you could
space it out better?
paxlovid india paxlovid buy
paxlovid buy paxlovid pharmacy
https://certifiedpharmacy.pro/# buy prescription drugs online
Paxlovid over the counter buy paxlovid online
https://certifiedpharmacy.pro/# canadian pharmacy antiobotics without perscription
paxlovid buy Paxlovid buy online
overseas pharmacy mail order prescription drugs from canada
paxlovid cost without insurance paxlovid india
https://canadianpharmacy.legal/# legit canadian online pharmacy
paxlovid india buy paxlovid online
reputable canadian mail order pharmacies online meds no rx reliable
https://stromectolivermectin.pro/# stromectol australia
Useful info. Fortunate me I discovered your website by chance, and I’m stunned why this accident didn’t happened
in advance! I bookmarked it.
generic wellbutrin cost: buy bupropion online – wellbutrin pills
buy stromectol: ivermectin oral solution – ivermectin uk
http://ventolin.tech/# ventolin for sale
http://ventolin.tech/# buy ventolin online nz
wellbutrin 150 xl: wellbutrin cost – best price generic wellbutrin
uk pharmacy no prescription: canadian international pharmacy – canadian pharmacy 1 internet online drugstore
Consumers probably won’t be dusting off their bannetons next year, but it is likely another time-intensive kitchen project that can convey a sense of accomplishment and satisfaction will take bread-making’s place. Cooking and baking from scratch can be pragmatic in terms of cost savings, but they can also be emotionally comforting, which is something that will be highly sought after by many in 2023. WAVES-USD is the final possible candidate to be the next big crypto on the market. Essentially, Waves is a blockchain platform for building dapps and smart contracts as well as launching custom crypto tokens. The platform uses a variation of the PoS consensus mechanism called leased proof-of-stake (LPoS). Relative to base metals, the outlook for precious metals is more positive, with all but palladium expected to end 2023 higher. With the Fed on pause, decreasing U.S. real yields will drive the bullish outlook for gold and silver prices over the latter half of 2023. Gold prices are forecast to push up to an average $1,860 per troy ounce in the fourth quarter of 2023.
http://www.xn--oi2b40g9xgnse83w.com/bbs/board.php?bo_table=free&wr_id=34562
The trading volume of CryptoZoo (ZOO) is $477.15 in the last 24 hours, representing a -92.40% decrease from one day ago and signalling a recent fall in market activity. Logan Paul is one of the most notable figures in the crypto and NFT markets, and he is working on something new and exceptional: Cryptozoo The class-action lawsuit comes weeks after Logan Paul shared a $1.5 million CryptoZoo recovery plan for its investors. YouTuber and Boxer, Logan Paul, today announced the details of a refund plan for dissatisfied customers and investors in his CryptoZoo collection, which was released in 2021. He has committed 1000 ETH (~$1.4 million), in order to provide anyone unhappy with their mint costs, 0.1 ETH (~$144). Paul said that to prove they have no “financial upside” in the game, the recovery plan would include burning of his and co-founder Jeff Levin’s CryptoZoo token holdings.
ivermectin human ivermectin humans stromectol prices
wellbutrin: price of wellbutrin 300mg – buy wellbutrin xl
https://wellbutrin.best/# order wellbutrin sr online
cost of wellbutrin in south africa: 150 mg wellbutrin – 300 wellbutrin
http://ventolin.tech/# ventolin generic price
pharmacy coupons: licensed online pharmacy – onlinecanadianpharmacy 24
ivermectin uk coronavirus: ivermectin 3 mg tabs – stromectol 12mg online
https://ventolin.tech/# cheap ventolin inhaler
ivermectin lice cost of ivermectin 3mg tablets ivermectin 9 mg tablet
generic wellbutrin: buy bupropion online – cheap wellbutrin online
http://stromectolivermectin.pro/# stromectol ivermectin buy
generic for ventolin: Ventolin inhalers – ventolin pharmacy australia
https://mexicanpharmacy.ink/# mexican border pharmacies shipping to usa
indian pharmacies safe: online pharmacy india – india pharmacy
http://indiapharmacy.bid/# india online pharmacy
https://mexicanpharmacy.ink/# mexico pharmacies prescription drugs
canadian valley pharmacy: pharmacies in canada that ship to the us – legal canadian pharmacy online
mexico pharmacies prescription drugs mexican mail order pharmacies best online pharmacies in mexico
canada drugs online review: certified pharmacy canada – legitimate canadian pharmacy
https://certifiedpharmacycanada.pro/# legit canadian pharmacy online
If some one wants to be updated with most recent technologies therefore
he must be pay a visit this site and be up to date everyday.
https://mexicanpharmacy.ink/# buying from online mexican pharmacy
mexican pharmaceuticals online: purple pharmacy mexico price list – medicine in mexico pharmacies
https://mexicanpharmacy.ink/# mexican border pharmacies shipping to usa
https://certifiedpharmacycanada.pro/# canadian online drugs
buy medicines online in india: indian pharmacies safe – indian pharmacy online
canadian pharmacy king reviews canadian discount pharmacy canadian pharmacy no scripts
best online canadian pharmacy: buy prescription drugs from canada cheap – reliable canadian pharmacy reviews
https://indiapharmacy.bid/# cheapest online pharmacy india
https://certifiedpharmacycanada.pro/# canadianpharmacy com
one on one help writing college admission essay writing paper measuring service quality essay
medication from mexico pharmacy: mexico drug stores pharmacies – buying from online mexican pharmacy
mexico pharmacies prescription drugs: mexican drugstore online – mexico drug stores pharmacies
mexican drugstore online mexico drug stores pharmacies п»їbest mexican online pharmacies
https://indiapharmacy.bid/# top 10 online pharmacy in india
http://indiapharmacy.bid/# india online pharmacy
indianpharmacy com: indian pharmacy paypal – reputable indian online pharmacy
canadian online pharmacy: certified pharmacy canada – legit canadian pharmacy
https://mexicanpharmacy.ink/# pharmacies in mexico that ship to usa
top 10 pharmacies in india top 10 pharmacies in india best india pharmacy
mexican border pharmacies shipping to usa: buying from online mexican pharmacy – mexican online pharmacies prescription drugs
http://certifiedpharmacycanada.pro/# canada drugs
world pharmacy india: top 10 online pharmacy in india – india pharmacy
http://indiapharmacy.bid/# best online pharmacy india
https://mexicanpharmacy.ink/# mexican pharmaceuticals online
mexican online pharmacies prescription drugs: mexican mail order pharmacies – mexican mail order pharmacies
http://mexicanpharmacy.ink/# mexican drugstore online
canadian pharmacy online reviews certified international pharmacy canadian pharmacy world
mexican border pharmacies shipping to usa: mexican pharmaceuticals online – mexico pharmacies prescription drugs
http://mexicanpharmacy.ink/# п»їbest mexican online pharmacies
– we have all of these features available
on our official ozwin casino play Casino website.
https://indiapharmacy.bid/# online shopping pharmacy india
doxycycline over the counter south africa: doxycycline 100mg tablets for sale – doxycycline capsule 100mg price
http://doxycycline.bid/# doxycycline mono
doxycycline 150 mg cost comparison: purchase doxycycline online – where can i buy doxycycline online
http://zithromax.reviews/# zithromax over the counter canada
best pharmacy prednisone: prednisone for sale online – prednisone online india
can i buy cheap clomid price: cheap clomid tablets – can you buy clomid for sale
https://zithromax.reviews/# zithromax 500mg price
where buy generic clomid pill: buy clomid online – how to get cheap clomid
Nie ma właściwości psychoaktywnych – w przeciwieństwie do THC, głównego składnika konopi indyjskich,
CBD nie powoduje euforii ani stanów halucynacyjnych.
Ma działanie przeciwzapalne – CBD wykazuje silne właściwości przeciwzapalne, co może pomóc w
leczeniu wielu chorób i stanów zapalnych.
Ma właściwości przeciwbólowe – CBD może pomóc w łagodzeniu bólu, zarówno w przypadku
bólu przewlekłego, jak i ostrego.
Ma działanie przeciwdrgawkowe – badania wykazują, że CBD może pomóc w łagodzeniu objawów epilepsji.
Ma działanie przeciwlękowe – CBD może pomóc w łagodzeniu objawów lęku i depresji.
Może pomóc w leczeniu chorób układu sercowo-naczyniowego – CBD wykazuje właściwości obniżające ciśnienie krwi, co może pomóc w łagodzeniu objawów chorób układu sercowo-naczyniowego.
Może pomóc w leczeniu chorób neurodegeneracyjnych – badania sugerują,
że CBD może pomóc w łagodzeniu objawów chorób takich jak choroba
Alzheimera, Parkinsona i stwardnienie rozsiane.
Nie wywołuje efektów ubocznych – CBD uważany jest za stosunkowo bezpieczny związek chemiczny,
który nie wywołuje poważnych skutków ubocznych.
[url=https://cbdxmcpl.weebly.com/blog/konopie-cbd-czym-sa]https://cbdxmcpl.weebly.com/blog/konopie-cbd-czym-sa[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/czym-jest-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/czym-jest-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/konopie-marihuana-cannabis-cbd]https://cbdxmcpl.jigsy.com/entries/general/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.huicopper.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.huicopper.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka]http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka[/url]
[url=http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.iamarrows.com/cbd-czym-jest]http://cbdxmcpl.iamarrows.com/cbd-czym-jest[/url]
[url=https://cbd31.page.tl/CBD-Najwazniejsze-informacje.htm]https://cbd31.page.tl/CBD-Najwazniejsze-informacje.htm[/url]
[url=https://penzu.com/p/919e4bd8]https://penzu.com/p/919e4bd8[/url]
[url=https://medium.com/@cbd3/cbd-z-czym-to-sie-je-2df83ab821b?source=your_stories_page————————————-]https://medium.com/@cbd3/cbd-z-czym-to-sie-je-2df83ab821b?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/produkty-cbd-czym-sa]http://cbdxmcpl.theburnward.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/cbd-czym-jest]http://cbdxmcpl.timeforchangecounselling.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-najwazniejsze-informacje]http://cbdxmcpl.trexgame.net/cbd-najwazniejsze-informacje[/url]
[url=http://cbdsklepxmcpl.image-perth.org/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.image-perth.org/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.theglensecret.com/cbd-z-czym-to-sie-je]http://cbdxmcpl.theglensecret.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.cavandoragh.org/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.tearosediner.net/susz-konopny-cbd]http://cbdxmcpl.tearosediner.net/susz-konopny-cbd[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.raidersfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.bearsfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd]http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/susz-konopny-cbd]http://cbdsklepxmcpl.lucialpiazzale.com/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.lowescouponn.com/czym-jest-cbd]http://cbdxmcpl.lowescouponn.com/czym-jest-cbd[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/produkty-cbd-czym-sa]http://cbdsklepxmcpl.fotosdefrases.com/produkty-cbd-czym-sa[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800673949.html]https://ameblo.jp/cbdxmcpl/entry-12800673949.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Susz_Konopny_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Susz_Konopny_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post1.html]https://cbdsklepxmcpl.hpage.com/post1.html[/url]
[url=https://truxgo.net/blogs/457616/1587245/susz-konopny-cbd]https://truxgo.net/blogs/457616/1587245/susz-konopny-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/co-to-jest-cbd-i-produkty-tego-typu?sd=pf]https://cbdsklepxmcpl.substack.com/p/co-to-jest-cbd-i-produkty-tego-typu?sd=pf[/url]
[url=https://cbdxmcpl.weebly.com/blog/cbd-najwazniejsze-informacje]https://cbdxmcpl.weebly.com/blog/cbd-najwazniejsze-informacje[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/co-to-jest-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/co-to-jest-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/konopie-marihuana-cannabis-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/konopie-marihuana-cannabis-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/konopie-cbd-czym-s%C4%85]https://cbdxmcpl.jigsy.com/entries/general/konopie-cbd-czym-s%C4%85[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je]http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa]http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa]http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.iamarrows.com/susz-konopny-cbd]http://cbdxmcpl.iamarrows.com/susz-konopny-cbd[/url]
[url=https://cbd31.page.tl/Susz-Konopny-CBD.htm]https://cbd31.page.tl/Susz-Konopny-CBD.htm[/url]
[url=https://penzu.com/p/033e07dc]https://penzu.com/p/033e07dc[/url]
[url=https://medium.com/@cbd3/czym-jest-cbd-301499af1340?source=your_stories_page————————————-]https://medium.com/@cbd3/czym-jest-cbd-301499af1340?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/sklep-konopny-z-suszem-cbd]http://cbdxmcpl.theburnward.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/produkty-cbd-czym-sa]http://cbdxmcpl.timeforchangecounselling.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-czym-jest]http://cbdxmcpl.trexgame.net/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.theglensecret.com/cannabis-cbd]http://cbdxmcpl.theglensecret.com/cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/konopie-marihuana-cannabis-cbd]http://cbdsklepxmcpl.cavandoragh.org/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/cbd-najwazniejsze-informacje]http://cbdxmcpl.tearosediner.net/cbd-najwazniejsze-informacje[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cannabis-cbd]http://cbdsklepxmcpl.raidersfanteamshop.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/susz-konopny-cbd]http://cbdxmcpl.bearsfanteamshop.com/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd-1]http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd-1[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-czym-jest]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.lowescouponn.com/czym-jest-cbd-1]http://cbdxmcpl.lowescouponn.com/czym-jest-cbd-1[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-cvbz]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-cvbz[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-4pqp]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-4pqp[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-ptgz]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-ptgz[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800675446.html]https://ameblo.jp/cbdxmcpl/entry-12800675446.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Co_to_jest_CBD_i_produkty_tego_typu]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Co_to_jest_CBD_i_produkty_tego_typu[/url]
[url=https://cbdsklepxmcpl.hpage.com/post2.html]https://cbdsklepxmcpl.hpage.com/post2.html[/url]
[url=https://truxgo.net/blogs/457616/1587284/legalna-marihuana-cbd]https://truxgo.net/blogs/457616/1587284/legalna-marihuana-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/cbd-sklep?sd=pf]https://cbdsklepxmcpl.substack.com/p/cbd-sklep?sd=pf[/url]
[url=https://cbdxmcpl.exposure.co/czm-sa-konopie-cbd?source=share-cbdxmcpl]https://cbdxmcpl.exposure.co/czm-sa-konopie-cbd?source=share-cbdxmcpl[/url]
[url=https://cbdxmcpl.weebly.com/blog/legalna-marihuana-cbd]https://cbdxmcpl.weebly.com/blog/legalna-marihuana-cbd[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/sklep-konopny-z-suszem-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/sklep-konopny-z-suszem-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/cannabis-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/cannabis-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/cbd-sklep]https://cbdxmcpl.jigsy.com/entries/general/cbd-sklep[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je-1]http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je-1[/url]
[url=http://cbdxmcpl.wpsuo.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.wpsuo.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd-1]http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd-1[/url]
[url=http://cbdxmcpl.iamarrows.com/susz-konopny-cbd-1]http://cbdxmcpl.iamarrows.com/susz-konopny-cbd-1[/url]
[url=https://cbd31.page.tl/Co-to-jest-CBD.htm]https://cbd31.page.tl/Co-to-jest-CBD.htm[/url]
[url=https://penzu.com/p/0986c4e2]https://penzu.com/p/0986c4e2[/url]
[url=https://medium.com/@cbd3/konopie-marihuana-cannabis-cbd-f6baa0220f8c?source=your_stories_page————————————-]https://medium.com/@cbd3/konopie-marihuana-cannabis-cbd-f6baa0220f8c?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/cannabis-cbd]http://cbdxmcpl.theburnward.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-czym-jest-1]http://cbdxmcpl.trexgame.net/cbd-czym-jest-1[/url]
[url=http://cbdsklepxmcpl.image-perth.org/cbd-wlasciwosci-i-charakterystyka]http://cbdsklepxmcpl.image-perth.org/cbd-wlasciwosci-i-charakterystyka[/url]
[url=http://cbdxmcpl.theglensecret.com/co-to-jest-cbd]http://cbdxmcpl.theglensecret.com/co-to-jest-cbd[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/cannabis-cbd]http://cbdsklepxmcpl.cavandoragh.org/cannabis-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.tearosediner.net/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.raidersfanteamshop.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/cbd-czym-jest]http://cbdxmcpl.bearsfanteamshop.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.almoheet-travel.com/cbd-czym-jest]http://cbdxmcpl.almoheet-travel.com/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-sklep]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-sklep[/url]
[url=http://cbdxmcpl.lowescouponn.com/cbd-czym-jest]http://cbdxmcpl.lowescouponn.com/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd-1]http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd-1[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-9pvc]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-9pvc[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-rqfc]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-rqfc[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-942c]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-942c[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800676357.html]https://ameblo.jp/cbdxmcpl/entry-12800676357.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Legalna_Marihuana_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Legalna_Marihuana_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post3.html]https://cbdsklepxmcpl.hpage.com/post3.html[/url]
[url=https://truxgo.net/blogs/457616/1587330/susz-konopny-cbd]https://truxgo.net/blogs/457616/1587330/susz-konopny-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/konopie-marihuana-cannabis-cbd?sd=pf]https://cbdsklepxmcpl.substack.com/p/konopie-marihuana-cannabis-cbd?sd=pf[/url]
[url=https://cbdxmcpl.exposure.co/konopie-cbd-czym-sa?source=share-cbdxmcpl]https://cbdxmcpl.exposure.co/konopie-cbd-czym-sa?source=share-cbdxmcpl[/url]
[url=https://cbdxmcpl.weebly.com/blog/co-to-jest-cbd-i-produkty-tego-typu]https://cbdxmcpl.weebly.com/blog/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/co-to-jest-cbd-i-produkty-tego-typu/]https://cbdxmcpl.edublogs.org/2023/04/28/co-to-jest-cbd-i-produkty-tego-typu/[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.huicopper.com/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka-1]http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka-1[/url]
[url=http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa-1]http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa-1[/url]
[url=http://cbdxmcpl.iamarrows.com/cannabis-cbd]http://cbdxmcpl.iamarrows.com/cannabis-cbd[/url]
[url=https://cbd31.page.tl/Konopie-CBD-czym-s%26%23261%3B.htm]https://cbd31.page.tl/Konopie-CBD-czym-s%26%23261%3B.htm[/url]
[url=https://penzu.com/p/abafcfbd]https://penzu.com/p/abafcfbd[/url]
[url=https://medium.com/@cbd3/cbd-w%C5%82a%C5%9Bciwo%C5%9Bci-i-charakterystyka-75588bcc40a3?source=your_stories_page————————————-]https://medium.com/@cbd3/cbd-w%C5%82a%C5%9Bciwo%C5%9Bci-i-charakterystyka-75588bcc40a3?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/cannabis-cbd-1]http://cbdxmcpl.theburnward.com/cannabis-cbd-1[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd[/url]
[url=http://cbdxmcpl.trexgame.net/susz-konopny-cbd]http://cbdxmcpl.trexgame.net/susz-konopny-cbd[/url]
[url=http://cbdsklepxmcpl.image-perth.org/konopie-marihuana-cannabis-cbd]http://cbdsklepxmcpl.image-perth.org/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.theglensecret.com/cbd-sklep]http://cbdxmcpl.theglensecret.com/cbd-sklep[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/susz-konopny-cbd]http://cbdsklepxmcpl.cavandoragh.org/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa]http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/cannabis-cbd]http://cbdxmcpl.bearsfanteamshop.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.almoheet-travel.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-z-czym-to-sie-je]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.fotosdefrases.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8gr8]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8gr8[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-l4dx]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-l4dx[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-mlyn]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-mlyn[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800677331.html]https://ameblo.jp/cbdxmcpl/entry-12800677331.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Sklep_konopny_z_suszem_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Sklep_konopny_z_suszem_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post4.html]https://cbdsklepxmcpl.hpage.com/post4.html[/url]
[url=https://truxgo.net/blogs/457616/1587377/cbd-czym-jest]https://truxgo.net/blogs/457616/1587377/cbd-czym-jest[/url]
[url=https://cbdsklepxmcpl.substack.com/p/cbd-najwazniejsze-informacje?sd=pf]https://cbdsklepxmcpl.substack.com/p/cbd-najwazniejsze-informacje?sd=pf[/url]
[url=https://cbdxmcpl.weebly.com/blog/susz-konopny-cbd]https://cbdxmcpl.weebly.com/blog/susz-konopny-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd-2/]https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd-2/[/url]
[url=http://cbdsklepxmcpl.huicopper.com/konopie-cbd-czym-sa]http://cbdsklepxmcpl.huicopper.com/konopie-cbd-czym-sa[/url]
[url=http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa-1]http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa-1[/url]
[url=http://cbdxmcpl.yousher.com/cbd-czym-jest]http://cbdxmcpl.yousher.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.iamarrows.com/cbd-najwazniejsze-informacje]http://cbdxmcpl.iamarrows.com/cbd-najwazniejsze-informacje[/url]
[url=https://penzu.com/p/b7b72f41]https://penzu.com/p/b7b72f41[/url]
[url=https://medium.com/@cbd3/produkty-cbd-czym-s%C4%85-280d1a05cd6b?source=your_stories_page————————————-]https://medium.com/@cbd3/produkty-cbd-czym-s%C4%85-280d1a05cd6b?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.theburnward.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-1]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-1[/url]
[url=http://cbdxmcpl.trexgame.net/co-to-jest-cbd]http://cbdxmcpl.trexgame.net/co-to-jest-cbd[/url]
[url=http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd-1]http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd-1[/url]
[url=http://cbdxmcpl.theglensecret.com/co-to-jest-cbd-1]http://cbdxmcpl.theglensecret.com/co-to-jest-cbd-1[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.cavandoragh.org/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa-1]http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa-1[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje-1]http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje-1[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/czym-jest-cbd]http://cbdxmcpl.bearsfanteamshop.com/czym-jest-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/czm-sa-konopie-cbd]http://cbdxmcpl.almoheet-travel.com/czm-sa-konopie-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.lucialpiazzale.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd-1]http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd-1[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/cbd-wlasciwosci-i-charakterystyka]http://cbdsklepxmcpl.fotosdefrases.com/cbd-wlasciwosci-i-charakterystyka[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8y69]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8y69[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-bjv1]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-bjv1[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-7n0n]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-7n0n[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800708937.html]https://ameblo.jp/cbdxmcpl/entry-12800708937.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Czym_jest_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Czym_jest_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post5.html]https://cbdsklepxmcpl.hpage.com/post5.html[/url]
[url=https://truxgo.net/blogs/457616/1588162/susz-konopny-cbd]https://truxgo.net/blogs/457616/1588162/susz-konopny-cbd[/url]
https://prednisone.cheap/# prednisone 10 tablet
where buy generic clomid pill: buy clomid online – cost cheap clomid online
order generic clomid pills: order generic clomid no prescription – where to get generic clomid pill
ed drug prices: over the counter erectile dysfunction pills – what is the best ed pill
http://cytotec.ink/# buy misoprostol over the counter
cost of cheap propecia without dr prescription: cheap generic propecia – buying generic propecia without insurance
п»їpaxlovid paxlovid cost without insurance paxlovid price
п»їpaxlovid: п»їpaxlovid – paxlovid cost without insurance
best male ed pills: over the counter erectile dysfunction pills – ed drugs list
buy cytotec online: Cytotec 200mcg price – purchase cytotec
https://cytotec.ink/# buy cytotec over the counter
order cheap propecia pill: cheap generic propecia – buy propecia price
paxlovid cost without insurance: paxlovid for sale – Paxlovid over the counter
over the counter erectile dysfunction pills: buy generic ed drugs – buying ed pills online
propecia for sale buy generic propecia propecia pills
http://paxlovid.life/# paxlovid cost without insurance
non prescription erection pills: buy generic ed drugs – erectile dysfunction drugs
ed pills for sale: cheap erectile dysfunction pill – treatment of ed
http://propecia.cheap/# propecia order
WOW just what I was looking for. Came here by searching for locksmiths
My website :: super locksmith tampa
Paxlovid buy online: buy paxlovid online – paxlovid for sale
paxlovid generic: paxlovid price – paxlovid price
cytotec buy online usa buy cytotec over the counter Misoprostol 200 mg buy online
paxlovid pill: Paxlovid buy online – paxlovid generic
http://cytotec.ink/# Misoprostol 200 mg buy online
buying propecia without a prescription: cheap generic propecia – propecia tablets
erection pills: best over the counter ed pills – natural remedies for ed
https://paxlovid.life/# Paxlovid over the counter
paxlovid generic: paxlovid covid – Paxlovid over the counter
buy cytotec over the counter cytotec online buy cytotec pills online cheap
cost cheap propecia for sale: buy generic propecia – order generic propecia for sale
https://paxlovid.life/# paxlovid pill
paxlovid price: paxlovid for sale – Paxlovid over the counter
Paxlovid over the counter: Paxlovid buy online – paxlovid covid
buy cytotec over the counter: Abortion pills online – buy cytotec pills
https://cytotec.ink/# cytotec pills buy online
ed drugs cheap erectile dysfunction pill best ed pills online
order generic propecia pill: cost generic propecia – cost of propecia pills
buying propecia tablets: propecia best price – propecia pills
generic propecia without rx: buy propecia – cost propecia without insurance
https://propecia.cheap/# buy cheap propecia online
erectile dysfunction medications: cheapest ed pills – best ed drug
paxlovid india: buy paxlovid online – paxlovid india
http://paxlovid.life/# Paxlovid over the counter
Attractive section of content. I just stumbled upon your site and in ccession capital to assert that I acquire actually enjoyed account your blog
posts. Any way I will be subscribing to your augjent and evn I achidvement you access consistently rapidly.
Look into my blog post Website
online ed medications over the counter erectile dysfunction pills mens ed pills
erection pills: cheap erectile dysfunction pill – ed drugs
treatment for ed: buy generic ed drugs – erectile dysfunction drug
cost propecia without insurance: buy generic propecia – cost of generic propecia price
https://edpills.ink/# best ed medication
Misoprostol 200 mg buy online: buy cytotec – п»їcytotec pills online
order cheap propecia prices: cheap generic propecia – cost generic propecia pill
order cytotec online: buy misoprostol over the counter – buy cytotec online
http://propecia.cheap/# order propecia tablets
top ed pills: best over the counter ed pills – drugs for ed
order propecia without rx: cheap propecia – buy propecia no prescription
https://propecia.cheap/# cheap propecia price
paxlovid india: п»їpaxlovid – paxlovid pill
propecia price: cheap generic propecia – cheap propecia pill
doxycycline nz cost: doxycycline 500mg price in india – doxycycline 5553
doxycycline 100mg best buy: doxycycline 50 mg generic – doxycycline capsules purchase
prednisone daily use: prednisone pills for sale – generic prednisone tablets
prednisone brand name: buy prednisone tablets uk – where can i get prednisone over the counter
Where to play free slots online? This question often occurs to beginner gamblers. To date, free slot machine games are available on different types of devices. This can be your PC, mobile phone, tablet, or laptop. Playing slots for free is more convenient because they are absolutely universal and can be played with any device, no matter where you are, at any time. Many USA online casinos are adapted to mobile phones so that users can play at any moment. This is really very cool because it greatly simplifies access to your favorite games and allows you to fully enjoy them. DraftKings Casino, BetMGM and Unibet are some of the best apps for free mobile slots. You can download the casino app and enjoy playing online free slots in demo mode for as long as you like. You will also receive free spin bonuses, which allow you to play free online slot machines without risking your money, but which also offer cash payouts if you complete rollover requirements.
https://landengfft909234.is-blog.com/25987585/double-hit-casino-slots-games
In 2023, you don’t need to stick to free penny slots only. You can also play the latest video slot games for free. These newer games come with plenty of fun bonus rounds and free spins. Besides that, new free casino slots come with impressive graphics and special effects. There is a sequel, Blood Suckers 2, which has better graphics, a wider range of permitted bet sizes and the ability to win up to 1,298 times your stake, as opposed to 1,015 on the original. You can try out these free slots for fun at online casinos, along with many more free slots. You will not need to download free online slots, as you can play them on a casino website such as DraftKings, provided you are 21 or older. The game offers players 243 ways to win, which means all the pay lines automatically become active once a player places a bet. This means players do not need to concern themselves about having to decide which lines they should play next for higher chances of scoring a win. Instead, they can keep things sweet and simple and enjoy the game as it unfolds on the grid.
buy doxycycline online cheap: doxycycline in usa – buy doxycycline 100mg online uk
doxycycline capsule 100mg price: buying doxycycline online in usa – buy doxycycline canada
how to get doxycycline online: doxycycline pills over the counter – doxycycline 100 mg cap over the counter
amoxicillin for sale online amoxicillin discount – amoxicillin where to get
prednisone 10: prednisone where can i buy – prednisone over the counter uk
cost of prednisone 5mg tablets: prednisone best price – prednisone 4mg
canadian online pharmacy prednisone: prednisone 10 mg tablet cost – price of prednisone tablets
prednisone 40 mg: prednisone 40 mg rx – prednisone online australia
where to get amoxicillin over the counter amoxicillin 500 mg without a prescription – amoxicillin online pharmacy
drug doxycycline 100mg: how much is doxycycline in south africa – doxycycline 400 mg brand name
prednisone 50 mg coupon: prednisone best prices – prednisone prices
where to buy doxycycline in singapore: 80 mg doxycycline – doxyhexal
doxycycline 150mg pill: doxycycline pills – doxycycline 400 mg
buy amoxicillin 500mg amoxicillin tablets in india – prescription for amoxicillin
amoxicillin tablet 500mg where to buy amoxicillin 500mg – buy amoxicillin 500mg uk
no prescription doxycycline: doxycycline capsule 100mg price – doxycycline 100mg price in south africa
buy amoxicillin online no prescription can i buy amoxicillin over the counter – buy cheap amoxicillin
amoxicillin 500 mg price how to buy amoxycillin – buy cheap amoxicillin online
amoxicillin 500 mg purchase without prescription order amoxicillin uk – buy amoxicillin
doxycycline 500mg price in india: buy doxycycline 100mg – can i buy doxycycline over the counter in south africa
prednisone over the counter south africa: prednisone 10 mg tablet cost – prednisone 10 mg daily
prednisone 50mg cost: prednisone 20 mg tablets coupon – buy prednisone nz
adult singles dating site: video dating – internet dating services
doxycycline 500 mg capsules: doxycycline 50 mg – doxycycline 100mg cap tab
prednisone over the counter cost: http://prednisone1st.store/# prednisone buy cheap
prednisone 60 mg daily: online prednisone 5mg – buy prednisone 20mg without a prescription best price
doxycycline hyclate 100 mg capsules: doxycycline 50 mg coupon – doxycycline buy online india
amoxicillin 500 coupon amoxicillin 500 – over the counter amoxicillin canada
generic propecia pills get cheap propecia without a prescription
https://pharmacyreview.best/# canadian pharmacy prices
https://pharmacyreview.best/# pharmacy in canada
best medication for ed ed pills otc male erection pills
order generic propecia price cheap propecia without rx
cost generic propecia for sale generic propecia without dr prescription
men’s ed pills: best drug for ed – erectile dysfunction drugs
Learn about the side effects, dosages, and interactions.
pills for ed: impotence pills – male ed drugs
Read information now.
ed medications list: pills for ed – ed meds
how to buy cheap mobic without dr prescription: where to buy mobic tablets – order mobic without dr prescription
canadian drug canadian pharmacy online reviews
amoxicillin generic: http://amoxicillins.com/# buy amoxicillin online cheap
amoxil generic amoxicillin pharmacy price – amoxil pharmacy
where can i buy amoxicillin online price for amoxicillin 875 mg – amoxicillin 500mg capsule cost
https://mobic.store/# can i purchase generic mobic no prescription
cheap ed pills gnc ed pills top ed drugs
A big thank you for your blog.Really looking forward to read more. Really Cool.
prestigeautodetailingkc.com
home cost generic propecia without a prescription
reddit canadian pharmacy online canadian pharmacy
ed pills cheap: best erectile dysfunction pills – medicine for erectile
Read information now.
canadian online pharmacy canadian pharmacy
Everything what you want to know about pills.
https://pharmacyreview.best/# canadian pharmacy 365
certified canadian pharmacy canada drugs online review
where to get mobic without prescription: where to buy mobic pill – where buy mobic
amoxicillin without prescription: https://amoxicillins.com/# amoxicillin 500mg tablets price in india
canadian pharmacy ed medications is canadian pharmacy legit
order amoxicillin online no prescription: amoxicillin over the counter in canada order amoxicillin online uk
can i get generic mobic pills: where can i buy cheap mobic without a prescription – how can i get mobic pill
purple pharmacy mexico price list п»їbest mexican online pharmacies mexican border pharmacies shipping to usa
https://mexpharmacy.sbs/# mexico pharmacies prescription drugs
http://indiamedicine.world/# top 10 pharmacies in india
Nie ma właściwości psychoaktywnych – w przeciwieństwie do THC, głównego składnika konopi indyjskich, CBD nie powoduje euforii ani stanów halucynacyjnych.
Ma działanie przeciwzapalne – CBD wykazuje silne właściwości przeciwzapalne,
co może pomóc w leczeniu wielu chorób i stanów zapalnych.
Ma właściwości przeciwbólowe – CBD może pomóc w łagodzeniu bólu,
zarówno w przypadku bólu przewlekłego, jak i ostrego.
Ma działanie przeciwdrgawkowe – badania wykazują, że CBD może
pomóc w łagodzeniu objawów epilepsji.
Ma działanie przeciwlękowe – CBD może pomóc w łagodzeniu objawów lęku i depresji.
Może pomóc w leczeniu chorób układu sercowo-naczyniowego – CBD wykazuje
właściwości obniżające ciśnienie krwi, co może pomóc w łagodzeniu objawów chorób układu sercowo-naczyniowego.
Może pomóc w leczeniu chorób neurodegeneracyjnych – badania sugerują, że
CBD może pomóc w łagodzeniu objawów chorób takich jak choroba Alzheimera,
Parkinsona i stwardnienie rozsiane.
Nie wywołuje efektów ubocznych – CBD uważany jest za stosunkowo bezpieczny związek chemiczny, który
nie wywołuje poważnych skutków ubocznych.
[url=https://cbdxmcpl.weebly.com/blog/konopie-cbd-czym-sa]https://cbdxmcpl.weebly.com/blog/konopie-cbd-czym-sa[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/czym-jest-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/czym-jest-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/konopie-marihuana-cannabis-cbd]https://cbdxmcpl.jigsy.com/entries/general/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.huicopper.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.huicopper.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka]http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka[/url]
[url=http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.iamarrows.com/cbd-czym-jest]http://cbdxmcpl.iamarrows.com/cbd-czym-jest[/url]
[url=https://cbd31.page.tl/CBD-Najwazniejsze-informacje.htm]https://cbd31.page.tl/CBD-Najwazniejsze-informacje.htm[/url]
[url=https://penzu.com/p/919e4bd8]https://penzu.com/p/919e4bd8[/url]
[url=https://medium.com/@cbd3/cbd-z-czym-to-sie-je-2df83ab821b?source=your_stories_page————————————-]https://medium.com/@cbd3/cbd-z-czym-to-sie-je-2df83ab821b?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/produkty-cbd-czym-sa]http://cbdxmcpl.theburnward.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/cbd-czym-jest]http://cbdxmcpl.timeforchangecounselling.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-najwazniejsze-informacje]http://cbdxmcpl.trexgame.net/cbd-najwazniejsze-informacje[/url]
[url=http://cbdsklepxmcpl.image-perth.org/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.image-perth.org/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.theglensecret.com/cbd-z-czym-to-sie-je]http://cbdxmcpl.theglensecret.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.cavandoragh.org/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.tearosediner.net/susz-konopny-cbd]http://cbdxmcpl.tearosediner.net/susz-konopny-cbd[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.raidersfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.bearsfanteamshop.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd]http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/susz-konopny-cbd]http://cbdsklepxmcpl.lucialpiazzale.com/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.lowescouponn.com/czym-jest-cbd]http://cbdxmcpl.lowescouponn.com/czym-jest-cbd[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/produkty-cbd-czym-sa]http://cbdsklepxmcpl.fotosdefrases.com/produkty-cbd-czym-sa[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800673949.html]https://ameblo.jp/cbdxmcpl/entry-12800673949.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Susz_Konopny_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Susz_Konopny_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post1.html]https://cbdsklepxmcpl.hpage.com/post1.html[/url]
[url=https://truxgo.net/blogs/457616/1587245/susz-konopny-cbd]https://truxgo.net/blogs/457616/1587245/susz-konopny-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/co-to-jest-cbd-i-produkty-tego-typu?sd=pf]https://cbdsklepxmcpl.substack.com/p/co-to-jest-cbd-i-produkty-tego-typu?sd=pf[/url]
[url=https://cbdxmcpl.weebly.com/blog/cbd-najwazniejsze-informacje]https://cbdxmcpl.weebly.com/blog/cbd-najwazniejsze-informacje[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/co-to-jest-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/co-to-jest-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/konopie-marihuana-cannabis-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/konopie-marihuana-cannabis-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/konopie-cbd-czym-s%C4%85]https://cbdxmcpl.jigsy.com/entries/general/konopie-cbd-czym-s%C4%85[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je]http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa]http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa]http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.iamarrows.com/susz-konopny-cbd]http://cbdxmcpl.iamarrows.com/susz-konopny-cbd[/url]
[url=https://cbd31.page.tl/Susz-Konopny-CBD.htm]https://cbd31.page.tl/Susz-Konopny-CBD.htm[/url]
[url=https://penzu.com/p/033e07dc]https://penzu.com/p/033e07dc[/url]
[url=https://medium.com/@cbd3/czym-jest-cbd-301499af1340?source=your_stories_page————————————-]https://medium.com/@cbd3/czym-jest-cbd-301499af1340?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/sklep-konopny-z-suszem-cbd]http://cbdxmcpl.theburnward.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/produkty-cbd-czym-sa]http://cbdxmcpl.timeforchangecounselling.com/produkty-cbd-czym-sa[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-czym-jest]http://cbdxmcpl.trexgame.net/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.theglensecret.com/cannabis-cbd]http://cbdxmcpl.theglensecret.com/cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/konopie-marihuana-cannabis-cbd]http://cbdsklepxmcpl.cavandoragh.org/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/cbd-najwazniejsze-informacje]http://cbdxmcpl.tearosediner.net/cbd-najwazniejsze-informacje[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cannabis-cbd]http://cbdsklepxmcpl.raidersfanteamshop.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/susz-konopny-cbd]http://cbdxmcpl.bearsfanteamshop.com/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd-1]http://cbdxmcpl.almoheet-travel.com/legalna-marihuana-cbd-1[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-czym-jest]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.lowescouponn.com/czym-jest-cbd-1]http://cbdxmcpl.lowescouponn.com/czym-jest-cbd-1[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-cvbz]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-cvbz[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-4pqp]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-4pqp[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-ptgz]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-ptgz[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800675446.html]https://ameblo.jp/cbdxmcpl/entry-12800675446.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Co_to_jest_CBD_i_produkty_tego_typu]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Co_to_jest_CBD_i_produkty_tego_typu[/url]
[url=https://cbdsklepxmcpl.hpage.com/post2.html]https://cbdsklepxmcpl.hpage.com/post2.html[/url]
[url=https://truxgo.net/blogs/457616/1587284/legalna-marihuana-cbd]https://truxgo.net/blogs/457616/1587284/legalna-marihuana-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/cbd-sklep?sd=pf]https://cbdsklepxmcpl.substack.com/p/cbd-sklep?sd=pf[/url]
[url=https://cbdxmcpl.exposure.co/czm-sa-konopie-cbd?source=share-cbdxmcpl]https://cbdxmcpl.exposure.co/czm-sa-konopie-cbd?source=share-cbdxmcpl[/url]
[url=https://cbdxmcpl.weebly.com/blog/legalna-marihuana-cbd]https://cbdxmcpl.weebly.com/blog/legalna-marihuana-cbd[/url]
[url=https://cbdsklepxmcpl.bravesites.com/entries/general/sklep-konopny-z-suszem-cbd]https://cbdsklepxmcpl.bravesites.com/entries/general/sklep-konopny-z-suszem-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/cannabis-cbd/]https://cbdxmcpl.edublogs.org/2023/04/28/cannabis-cbd/[/url]
[url=https://cbdxmcpl.jigsy.com/entries/general/cbd-sklep]https://cbdxmcpl.jigsy.com/entries/general/cbd-sklep[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je-1]http://cbdsklepxmcpl.huicopper.com/cbd-z-czym-to-sie-je-1[/url]
[url=http://cbdxmcpl.wpsuo.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.wpsuo.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd-1]http://cbdxmcpl.yousher.com/konopie-marihuana-cannabis-cbd-1[/url]
[url=http://cbdxmcpl.iamarrows.com/susz-konopny-cbd-1]http://cbdxmcpl.iamarrows.com/susz-konopny-cbd-1[/url]
[url=https://cbd31.page.tl/Co-to-jest-CBD.htm]https://cbd31.page.tl/Co-to-jest-CBD.htm[/url]
[url=https://penzu.com/p/0986c4e2]https://penzu.com/p/0986c4e2[/url]
[url=https://medium.com/@cbd3/konopie-marihuana-cannabis-cbd-f6baa0220f8c?source=your_stories_page————————————-]https://medium.com/@cbd3/konopie-marihuana-cannabis-cbd-f6baa0220f8c?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/cannabis-cbd]http://cbdxmcpl.theburnward.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdxmcpl.trexgame.net/cbd-czym-jest-1]http://cbdxmcpl.trexgame.net/cbd-czym-jest-1[/url]
[url=http://cbdsklepxmcpl.image-perth.org/cbd-wlasciwosci-i-charakterystyka]http://cbdsklepxmcpl.image-perth.org/cbd-wlasciwosci-i-charakterystyka[/url]
[url=http://cbdxmcpl.theglensecret.com/co-to-jest-cbd]http://cbdxmcpl.theglensecret.com/co-to-jest-cbd[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/cannabis-cbd]http://cbdsklepxmcpl.cavandoragh.org/cannabis-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/co-to-jest-cbd-i-produkty-tego-typu]http://cbdxmcpl.tearosediner.net/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.raidersfanteamshop.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/cbd-czym-jest]http://cbdxmcpl.bearsfanteamshop.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.almoheet-travel.com/cbd-czym-jest]http://cbdxmcpl.almoheet-travel.com/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-sklep]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-sklep[/url]
[url=http://cbdxmcpl.lowescouponn.com/cbd-czym-jest]http://cbdxmcpl.lowescouponn.com/cbd-czym-jest[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd-1]http://cbdsklepxmcpl.fotosdefrases.com/sklep-konopny-z-suszem-cbd-1[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-9pvc]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-9pvc[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-rqfc]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-rqfc[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-942c]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-942c[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800676357.html]https://ameblo.jp/cbdxmcpl/entry-12800676357.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Legalna_Marihuana_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Legalna_Marihuana_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post3.html]https://cbdsklepxmcpl.hpage.com/post3.html[/url]
[url=https://truxgo.net/blogs/457616/1587330/susz-konopny-cbd]https://truxgo.net/blogs/457616/1587330/susz-konopny-cbd[/url]
[url=https://cbdsklepxmcpl.substack.com/p/konopie-marihuana-cannabis-cbd?sd=pf]https://cbdsklepxmcpl.substack.com/p/konopie-marihuana-cannabis-cbd?sd=pf[/url]
[url=https://cbdxmcpl.exposure.co/konopie-cbd-czym-sa?source=share-cbdxmcpl]https://cbdxmcpl.exposure.co/konopie-cbd-czym-sa?source=share-cbdxmcpl[/url]
[url=https://cbdxmcpl.weebly.com/blog/co-to-jest-cbd-i-produkty-tego-typu]https://cbdxmcpl.weebly.com/blog/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/co-to-jest-cbd-i-produkty-tego-typu/]https://cbdxmcpl.edublogs.org/2023/04/28/co-to-jest-cbd-i-produkty-tego-typu/[/url]
[url=http://cbdsklepxmcpl.huicopper.com/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.huicopper.com/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka-1]http://cbdxmcpl.wpsuo.com/cbd-wlasciwosci-i-charakterystyka-1[/url]
[url=http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa-1]http://cbdxmcpl.yousher.com/produkty-cbd-czym-sa-1[/url]
[url=http://cbdxmcpl.iamarrows.com/cannabis-cbd]http://cbdxmcpl.iamarrows.com/cannabis-cbd[/url]
[url=https://cbd31.page.tl/Konopie-CBD-czym-s%26%23261%3B.htm]https://cbd31.page.tl/Konopie-CBD-czym-s%26%23261%3B.htm[/url]
[url=https://penzu.com/p/abafcfbd]https://penzu.com/p/abafcfbd[/url]
[url=https://medium.com/@cbd3/cbd-w%C5%82a%C5%9Bciwo%C5%9Bci-i-charakterystyka-75588bcc40a3?source=your_stories_page————————————-]https://medium.com/@cbd3/cbd-w%C5%82a%C5%9Bciwo%C5%9Bci-i-charakterystyka-75588bcc40a3?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/cannabis-cbd-1]http://cbdxmcpl.theburnward.com/cannabis-cbd-1[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd[/url]
[url=http://cbdxmcpl.trexgame.net/susz-konopny-cbd]http://cbdxmcpl.trexgame.net/susz-konopny-cbd[/url]
[url=http://cbdsklepxmcpl.image-perth.org/konopie-marihuana-cannabis-cbd]http://cbdsklepxmcpl.image-perth.org/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.theglensecret.com/cbd-sklep]http://cbdxmcpl.theglensecret.com/cbd-sklep[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/susz-konopny-cbd]http://cbdsklepxmcpl.cavandoragh.org/susz-konopny-cbd[/url]
[url=http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa]http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/cannabis-cbd]http://cbdxmcpl.bearsfanteamshop.com/cannabis-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.almoheet-travel.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/cbd-z-czym-to-sie-je]http://cbdsklepxmcpl.lucialpiazzale.com/cbd-z-czym-to-sie-je[/url]
[url=http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/co-to-jest-cbd-i-produkty-tego-typu]http://cbdsklepxmcpl.fotosdefrases.com/co-to-jest-cbd-i-produkty-tego-typu[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8gr8]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8gr8[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-l4dx]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-l4dx[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-mlyn]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-mlyn[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800677331.html]https://ameblo.jp/cbdxmcpl/entry-12800677331.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Sklep_konopny_z_suszem_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Sklep_konopny_z_suszem_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post4.html]https://cbdsklepxmcpl.hpage.com/post4.html[/url]
[url=https://truxgo.net/blogs/457616/1587377/cbd-czym-jest]https://truxgo.net/blogs/457616/1587377/cbd-czym-jest[/url]
[url=https://cbdsklepxmcpl.substack.com/p/cbd-najwazniejsze-informacje?sd=pf]https://cbdsklepxmcpl.substack.com/p/cbd-najwazniejsze-informacje?sd=pf[/url]
[url=https://cbdxmcpl.weebly.com/blog/susz-konopny-cbd]https://cbdxmcpl.weebly.com/blog/susz-konopny-cbd[/url]
[url=https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd-2/]https://cbdxmcpl.edublogs.org/2023/04/28/czm-sa-konopie-cbd-2/[/url]
[url=http://cbdsklepxmcpl.huicopper.com/konopie-cbd-czym-sa]http://cbdsklepxmcpl.huicopper.com/konopie-cbd-czym-sa[/url]
[url=http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa-1]http://cbdxmcpl.wpsuo.com/produkty-cbd-czym-sa-1[/url]
[url=http://cbdxmcpl.yousher.com/cbd-czym-jest]http://cbdxmcpl.yousher.com/cbd-czym-jest[/url]
[url=http://cbdxmcpl.iamarrows.com/cbd-najwazniejsze-informacje]http://cbdxmcpl.iamarrows.com/cbd-najwazniejsze-informacje[/url]
[url=https://penzu.com/p/b7b72f41]https://penzu.com/p/b7b72f41[/url]
[url=https://medium.com/@cbd3/produkty-cbd-czym-s%C4%85-280d1a05cd6b?source=your_stories_page————————————-]https://medium.com/@cbd3/produkty-cbd-czym-s%C4%85-280d1a05cd6b?source=your_stories_page————————————-[/url]
[url=http://cbdxmcpl.theburnward.com/konopie-marihuana-cannabis-cbd]http://cbdxmcpl.theburnward.com/konopie-marihuana-cannabis-cbd[/url]
[url=http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-1]http://cbdxmcpl.timeforchangecounselling.com/co-to-jest-cbd-1[/url]
[url=http://cbdxmcpl.trexgame.net/co-to-jest-cbd]http://cbdxmcpl.trexgame.net/co-to-jest-cbd[/url]
[url=http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd-1]http://cbdsklepxmcpl.image-perth.org/sklep-konopny-z-suszem-cbd-1[/url]
[url=http://cbdxmcpl.theglensecret.com/co-to-jest-cbd-1]http://cbdxmcpl.theglensecret.com/co-to-jest-cbd-1[/url]
[url=http://cbdsklepxmcpl.cavandoragh.org/cbd-najwazniejsze-informacje]http://cbdsklepxmcpl.cavandoragh.org/cbd-najwazniejsze-informacje[/url]
[url=http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa-1]http://cbdxmcpl.tearosediner.net/konopie-cbd-czym-sa-1[/url]
[url=http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje-1]http://cbdsklepxmcpl.raidersfanteamshop.com/cbd-najwazniejsze-informacje-1[/url]
[url=http://cbdxmcpl.bearsfanteamshop.com/czym-jest-cbd]http://cbdxmcpl.bearsfanteamshop.com/czym-jest-cbd[/url]
[url=http://cbdxmcpl.almoheet-travel.com/czm-sa-konopie-cbd]http://cbdxmcpl.almoheet-travel.com/czm-sa-konopie-cbd[/url]
[url=http://cbdsklepxmcpl.lucialpiazzale.com/sklep-konopny-z-suszem-cbd]http://cbdsklepxmcpl.lucialpiazzale.com/sklep-konopny-z-suszem-cbd[/url]
[url=http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd-1]http://cbdxmcpl.lowescouponn.com/konopie-marihuana-cannabis-cbd-1[/url]
[url=http://cbdsklepxmcpl.fotosdefrases.com/cbd-wlasciwosci-i-charakterystyka]http://cbdsklepxmcpl.fotosdefrases.com/cbd-wlasciwosci-i-charakterystyka[/url]
[url=https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8y69]https://zenwriting.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-8y69[/url]
[url=https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-bjv1]https://writeablog.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-bjv1[/url]
[url=https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-7n0n]https://postheaven.net/cbd3xmcpl/h1-marihuana-konopie-cbd-h1-konopie-cbd-to-odmiana-konopi-siewnej-7n0n[/url]
[url=https://ameblo.jp/cbdxmcpl/entry-12800708937.html]https://ameblo.jp/cbdxmcpl/entry-12800708937.html[/url]
[url=https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Czym_jest_CBD]https://canvas.instructure.com/eportfolios/2069923/cbdxmcpl/Czym_jest_CBD[/url]
[url=https://cbdsklepxmcpl.hpage.com/post5.html]https://cbdsklepxmcpl.hpage.com/post5.html[/url]
[url=https://truxgo.net/blogs/457616/1588162/susz-konopny-cbd]https://truxgo.net/blogs/457616/1588162/susz-konopny-cbd[/url]
canada drugs reviews: buy prescription drugs from canada cheap – canadian pharmacy cheap
website to help write an essay resources for research papers does chewing gum help you concentrate essay
п»їbest mexican online pharmacies: best online pharmacies in mexico – mexico pharmacies prescription drugs
indian pharmacy online indian pharmacy online top 10 pharmacies in india
http://indiamedicine.world/# top 10 online pharmacy in india
indianpharmacy com: п»їlegitimate online pharmacies india – п»їlegitimate online pharmacies india
п»їbest mexican online pharmacies: reputable mexican pharmacies online – mexico pharmacies prescription drugs
http://indiamedicine.world/# world pharmacy india
https://indiamedicine.world/# online shopping pharmacy india
legal canadian pharmacy online legit canadian online pharmacy canadian pharmacy cheap
canada cloud pharmacy: canadian pharmacy no rx needed – best canadian online pharmacy
canadian medications: canadianpharmacy com – online canadian pharmacy
http://indiamedicine.world/# online pharmacy india
https://certifiedcanadapharm.store/# cheapest pharmacy canada
п»їbest mexican online pharmacies medicine in mexico pharmacies mexico drug stores pharmacies
canadian pharmacy 365: canada drug pharmacy – canada pharmacy
п»їbest mexican online pharmacies: purple pharmacy mexico price list – mexican drugstore online
https://indiamedicine.world/# reputable indian pharmacies
indian pharmacy paypal: world pharmacy india – best india pharmacy
canadian pharmacy online ship to usa: canadian pharmacy victoza – canadian pharmacy cheap
reputable indian online pharmacy Online medicine order п»їlegitimate online pharmacies india
http://indiamedicine.world/# world pharmacy india
brillx казино
brillx официальный сайт
Брилкс Казино – это небывалая возможность погрузиться в атмосферу роскоши и азарта. Каждая деталь сайта продумана до мельчайших нюансов, чтобы обеспечить вам комфортное и захватывающее игровое пространство. На страницах Brillx Казино вы найдете множество увлекательных игровых аппаратов, которые подарят вам эмоции, сравнимые только с реальной азартной столицей.Ощутите адреналин и азарт настоящей игры вместе с нами. Будьте готовы к захватывающим приключениям и невероятным сюрпризам. Brillx Казино приглашает вас испытать удачу и погрузиться в мир бесконечных возможностей. Не упустите шанс стать частью нашей игровой семьи и почувствовать всю прелесть игры в игровые аппараты в 2023 году!
purple pharmacy mexico price list: mexico drug stores pharmacies – mexican pharmaceuticals online
canadian mail order pharmacy: trustworthy canadian pharmacy – canadianpharmacyworld
cheapest online pharmacy india buy prescription drugs from india online pharmacy india
https://indiamedicine.world/# best india pharmacy
http://gabapentin.pro/# how to get neurontin
can you buy zithromax over the counter in australia purchase zithromax online azithromycin zithromax
https://gabapentin.pro/# can i buy neurontin over the counter
can i buy zithromax over the counter: buy zithromax without presc – zithromax 500 mg lowest price online
prescription medication neurontin: neurontin 300 mg tablet – gabapentin
http://stromectolonline.pro/# ivermectin topical
ivermectin for sale: cost of ivermectin 1% cream – cost of ivermectin cream
https://azithromycin.men/# where can i buy zithromax uk
where to get zithromax over the counter buy zithromax online cheap how to buy zithromax online
cheap zithromax pills: cost of generic zithromax – buy zithromax without prescription online
cost of brand name neurontin: neurontin 800 mg cost – neurontin 300 mg capsule
http://gabapentin.pro/# neurontin prescription coupon
https://stromectolonline.pro/# stromectol ivermectin tablets
cheapest antibiotics over the counter antibiotics buy antibiotics over the counter
https://ed-pills.men/# new treatments for ed
cheapest antibiotics: Over the counter antibiotics pills – cheapest antibiotics
best ed treatment: п»їerectile dysfunction medication – non prescription erection pills
paxlovid covid paxlovid covid paxlovid buy
https://avodart.pro/# can i get avodart pills
http://ciprofloxacin.ink/# cipro pharmacy
https://lisinopril.pro/# best lisinopril brand
https://lisinopril.pro/# lisinopril cost us
cheap lipitor 20 mg: lipitor 10mg price australia – lipitor.com
We are a bunch of volunteers and opening a new scheme in our community.
Your site provided us with valuable info to work on. You’ve done an impressive job and our whole community will likely be grateful to you.
http://lipitor.pro/# lipitor 10mg generic
https://avodart.pro/# buying generic avodart no prescription
https://lipitor.pro/# generic lipitor 10 mg
http://misoprostol.guru/# cytotec abortion pill
http://lipitor.pro/# lipitor purchase online
http://ciprofloxacin.ink/# ciprofloxacin generic
indian pharmacy: indian pharmacy – buy prescription drugs from india
mexican online pharmacies prescription drugs: mexico drug stores pharmacies – medicine in mexico pharmacies
http://certifiedcanadapills.pro/# best canadian pharmacy to buy from
canadian king pharmacy canadian pharmacy ltd certified canadian pharmacy
https://cialis.science/# cialis recreational use
cialis 36 hour dosage: cheap cialis – cialis daily pricing
ed pills cheap: ed pills non prescription – best medication for ed
buying ed pills online: best ed treatment pills – non prescription erection pills
medication for ed dysfunction: erection pills online – best pill for ed
http://cialis.science/# ed. trusted medstore in cialis
buy kamagra online: cheap kamagra – cheap kamagra
trial pack cialis viagra levitro: cialis.science – cialis online overnight shipping
pills for ed cheap erectile dysfunction pills cheap ed drugs
To understand verified scoop, ape these tips:
Look representing credible sources: https://ukcervicalcancer.org.uk/articles/who-left-q13-news.html. It’s eminent to ensure that the news origin you are reading is reliable and unbiased. Some examples of reputable sources categorize BBC, Reuters, and The New York Times. Review multiple sources to get back at a well-rounded view of a particular low-down event. This can help you return a more complete paint and escape bias. Be cognizant of the position the article is coming from, as constant respected telecast sources can have bias. Fact-check the gen with another source if a expos‚ article seems too unequalled or unbelievable. Always make sure you are reading a known article, as scandal can change quickly.
By following these tips, you can fit a more in the know news reader and more wisely understand the cosmos about you.
To presume from present news, ape these tips:
Look for credible sources: https://yanabalitour.com/wp-content/pgs/?what-happened-to-anna-on-fox-news.html. It’s high-ranking to guard that the expos‚ outset you are reading is respected and unbiased. Some examples of reliable sources tabulate BBC, Reuters, and The Fashionable York Times. Read multiple sources to get back at a well-rounded understanding of a discriminating info event. This can help you get a more ended facsimile and keep bias. Be aware of the perspective the article is coming from, as constant reputable report sources can be dressed bias. Fact-check the low-down with another source if a scandal article seems too unequalled or unbelievable. Till the end of time make sure you are reading a fashionable article, as expos‚ can substitute quickly.
By following these tips, you can fit a more informed news reader and better be aware the cosmos here you.
herbal ed treatment: ed pills for sale – ed meds
cheap kamagra: kamagra – Kamagra tablets 100mg
http://kamagra.men/# kamagra oral jelly
sildenafil troche viagra for sale lady viagra
cialis professional ingredients: buy cialis no prescription – cialis online fast
neurontin 2400 mg: generic neurontin 600 mg – canada neurontin 100mg lowest price
http://cytotec.auction/# buy cytotec pills
buy cytotec online: buy cytotec pills – buy cytotec in usa
Abortion pills online: purchase cytotec – order cytotec online
http://gabapentin.tech/# buy neurontin 100 mg
cytotec online: cytotec abortion pill – purchase cytotec
stromectol order: stromectol uk – ivermectin 5
neurontin brand name 800mg best price: neurontin capsules 600mg – cost of neurontin 100mg
I juѕt couldn’t leave your website prior to suggesting tһat I actually
enjoyed thе usual info a person supply οn уour visitors?
Iѕ gonna be аgain steadily in order tⲟ check out new posts.
Alѕo visit my web blog: looks presentable
ivermectin 10 ml: ivermectin coronavirus – ivermectin cost
https://cytotec.auction/# cytotec abortion pill
buy cytotec pills online cheap: buy cytotec pills – Cytotec 200mcg price
buy neurontin canadian pharmacy: neurontin capsules – neurontin generic brand
Although real money roulette is what will get you winnings, playing roulette for free is not something to be dismissed! It is a good way to test some betting strategies like the Martingale and refine your game skills before committing any money. Roulette exists since the 18th century in France and became more popular in the 19th century in Italy, Germany, UK and in the first part of 20th century in US. Nowadays Roulette is famous in most countries of the world. The invention of the roulette wheel was not intented to create a device for one of the most beloved games of gambling. Instead it was thought as wheel of numbers wich solidly creates random numbers in a mechanical way and offers the possibility for studying random distributions. There is no proof about the exact age of the roulette wheel. In some sources Blaise Pascal is credited as the inventor, others claim that european traders found the idea of a numbered wheel in China and imported it to Europe.
http://oceanbrick.co.kr/bbs/board.php?bo_table=free&wr_id=3073
Keep track of your play with these Reality Check alerts. For more info about our gaming tools, see . A lot of bonuses will require you to complete any bet requirements within a set time limit. When using most free casino signup bonus no deposit promos, players will be given up to seven days to clear their free bonus balance. No Deposit Bonus: 20 Free Spins on Elvis Frog. The wagering requirement are 50x and the maximum cashout is €50. No bonus code is needed when you follow our claim bonus link. Deposit Bonus: 100% up to €100 + 100 Free spins to play on selected games. Minimum Deposit: $ €20 Wagering Requirements: 45x for bonus & 50x for free spins. Maximum Cashout: No cashout limit for the bonus but €100 for free spins. T&C Apply. 18+
Hi there, I desire to subscribe for this weblog to get
newest updates, thus where can i do it please help.
Feel free to surf to my website :: สล็อตเว็บตรง
http://ivermectin.auction/# stromectol order
neurontin buy online: neurontin without prescription – how much is generic neurontin
Nice post. I learn something totally new and challenging on websites
I stumbleupon every day. It will always be interesting to read through articles from other writers and practice something from other websites.
Pretty! This has been a really wonderful article. Thank you
for supplying this information.
order cytotec online: buy cytotec over the counter – cytotec buy online usa
https://ivermectin.auction/# where to buy stromectol
http://gabapentin.tech/# neurontin buy online
buy cytotec over the counter: buy cytotec online fast delivery – buy cytotec over the counter
покердом онлайн
https://t.me/s/poker_dom_online
покердом онлайн
stromectol ivermectin: ivermectin cost uk – stromectol ivermectin
покердом казино вход
https://t.me/s/pokerdom_casino_entrance
покердом казино вход
покердом официальный сайт вход
https://t.me/s/pokerdom_official_website_login
покердом официальный сайт вход
stromectol price: buy stromectol online uk – ivermectin oral 0 8
покердом официальный сайт играть
https://t.me/s/offi_pokerdom
покердом официальный сайт играть
ivermectin lotion cost: stromectol tablets for humans – stromectol xr
buying neurontin online: neurontin 400mg – discount neurontin
http://gabapentin.tech/# neurontin 100 mg cost
покердом официальный вход
покердом официальный вход
покердом официальный вход
canada where to buy neurontin: neurontin 300 mg tablets – neurontin 300 mg coupon
https://gabapentin.tech/# neurontin 100mg tablet
ivermectin over the counter: stromectol for sale – ivermectin over the counter canada
покердом покер скачать
https://t.me/s/skachat_pokerdom
покердом покер скачать
регистрация на покердом
https://t.me/s/registracija_na_pokerdom
регистрация на покердом
stromectol pill: stromectol pills – ivermectin oral solution
neurontin rx: neurontin capsules 300mg – 2000 mg neurontin
покердом зеркало рабочее на сегодня
покердом зеркало рабочее на сегодня
покердом зеркало рабочее на сегодня
Покер POKERDOM
https://t.me/s/poker_pokerdom
Покер POKERDOM
ivermectin cream canada cost: purchase ivermectin – ivermectin 10 mg
покердом зеркало сегодня
покердом зеркало сегодня
покердом зеркало сегодня
покердом вход в личный
покердом вход в личный
покердом вход в личный
покердом зеркало на сегодня
покердом зеркало на сегодня
покердом зеркало на сегодня
зеркало казино покердом
зеркало казино покердом
зеркало казино покердом
покердом онлайн играть
https://t.me/s/pokerdom_onlain
покердом онлайн играть
PokerDom ПокерДом
https://t.me/s/poKerdom_PokerDom1
PokerDom ПокерДом
Покердом мобильная ВЕРСИЯ
https://t.me/s/mobilnaya_versiya_pokerdom
Покердом мобильная ВЕРСИЯ
india online pharmacy: Online medication home delivery – indian pharmacies safe
Клиент Покердом онлайн
https://t.me/s/pokerdom_client
Клиент Покердом онлайн
Казино ПокерДом
https://t.me/s/casino_pokerdom_onlain
Казино ПокерДом
https://canadaph.life/# canadian pharmacy meds
Отзывы покердом
Отзывы покердом
Отзывы покердом
mexican drugstore online: mexico drug stores pharmacies – medication from mexico pharmacy
покердом официальный зеркало
https://t.me/s/pokerdom_oficialnyj
покердом официальный зеркало
покердом официальный сайт для андроид
покердом официальный сайт для андроид
покердом официальный сайт для андроид
покердом официальный сайт на реальные деньги
https://t.me/s/pokerdom_na_real
покердом официальный сайт на реальные деньги
играть покердом онлайн
играть покердом онлайн
играть покердом онлайн
покердом казино играть онлайн
покердом казино играть онлайн
покердом казино играть онлайн
buying from online mexican pharmacy medication from mexico pharmacy purple pharmacy mexico price list
http://mexicoph.life/# mexico drug stores pharmacies
ПокерДом на ПК
ПокерДом на ПК
ПокерДом на ПК
buying prescription drugs in mexico online: mexico pharmacies prescription drugs – mexican online pharmacies prescription drugs
sanofi cialis what is cialis does cialis lose effectiveness over time
top 10 pharmacies in india: mail order pharmacy india – reputable indian online pharmacy
Thank you for some other informative web site.
Where else may just I am getting that type of information written in such an ideal manner?
I have a challenge that I’m simply now operating on,
and I have been at the look out for such info.
My blog post – super locksmith tampa
Absolutely! Conclusion expos‚ portals in the UK can be unendurable, but there are numerous resources available to boost you find the perfect one because you. As I mentioned formerly, conducting an online search an eye to http://capturephotographyschools.co.uk/pag/how-tall-is-kennedy-on-fox-news.html “UK hot item websites” or “British information portals” is a vast starting point. Not one purposefulness this grant you a encyclopaedic shopping list of communication websites, but it intention also afford you with a improved savvy comprehension or of the in the air hearsay scene in the UK.
On one occasion you be enduring a liber veritatis of imminent rumour portals, it’s important to estimate each sole to determine which overwhelm suits your preferences. As an example, BBC Dispatch is known quest of its objective reporting of report stories, while The Trustee is known for its in-depth analysis of bureaucratic and popular issues. The Disinterested is known championing its investigative journalism, while The Times is known by reason of its work and funds coverage. By way of understanding these differences, you can pick out the rumour portal that caters to your interests and provides you with the news you have a yen for to read.
Additionally, it’s worth all in all neighbourhood news portals with a view fixed regions within the UK. These portals lay down coverage of events and news stories that are fitting to the area, which can be especially cooperative if you’re looking to charge of up with events in your close by community. In search occurrence, provincial dope portals in London classify the Evening Pier and the Londonist, while Manchester Evening Hearsay and Liverpool Repercussion are in demand in the North West.
Blanket, there are tons statement portals accessible in the UK, and it’s high-level to do your inspection to unearth the joined that suits your needs. By means of evaluating the unconventional news portals based on their coverage, luxury, and position statement standpoint, you can decide the a person that provides you with the most apposite and attractive news stories. Decorous luck with your search, and I anticipate this bumf helps you come up with the perfect dope portal inasmuch as you!
Altogether! Find expos‚ portals in the UK can be unendurable, but there are numerous resources available to boost you find the perfect in unison because you. As I mentioned before, conducting an online search for https://utopia-beauty.co.uk/wp-content/pgs/why-is-fox-news-app-not-working.html “UK scuttlebutt websites” or “British information portals” is a enormous starting point. Not one will this chuck b surrender you a encyclopaedic shopping list of hearsay websites, but it intention also lend you with a better savvy comprehension or of the current story scene in the UK.
Aeons ago you obtain a itemize of embryonic account portals, it’s prominent to evaluate each sole to influence which overwhelm suits your preferences. As an example, BBC Dispatch is known in place of its disinterested reporting of news stories, while The Guardian is known quest of its in-depth criticism of partisan and group issues. The Self-governing is known for its investigative journalism, while The Times is known in search its work and finance coverage. By concession these differences, you can decide the news portal that caters to your interests and provides you with the hearsay you have a yen for to read.
Additionally, it’s worth looking at local scuttlebutt portals because specific regions within the UK. These portals yield coverage of events and news stories that are relevant to the area, which can be firstly utilitarian if you’re looking to keep up with events in your town community. For event, municipal dope portals in London include the Evening Pier and the Londonist, while Manchester Evening Talk and Liverpool Reflection are hot in the North West.
Inclusive, there are numberless statement portals available in the UK, and it’s important to do your digging to remark the one that suits your needs. By evaluating the different news broadcast portals based on their coverage, luxury, and editorial standpoint, you can select the individual that provides you with the most apposite and captivating low-down stories. Esteemed destiny with your search, and I anticipate this tidings helps you discover the practised news broadcast portal since you!
https://mexicoph.life/# mexican border pharmacies shipping to usa
over the counter cialis cialis online cheap cialis prices
best online pharmacies in mexico: mexican online pharmacies prescription drugs – mexican drugstore online
Hi there, always i used to check blog posts here in the early hours in the dawn,
because i like to find out more and more.
бонус код покердом
https://t.me/s/voyti_pokerdom
бонус код покердом
ПокерДом ВОЙТИ СЕЙЧАС
ПокерДом ВОЙТИ СЕЙЧАС
ПокерДом ВОЙТИ СЕЙЧАС
Фриролл ПОКЕРДОМ
https://t.me/s/th_freeroll_pokerdom
Фриролл ПОКЕРДОМ
Покердом в россии
https://t.me/s/pokerdom_v_rossii
Покердом в россии
слоты покердом
https://t.me/s/sloty_pokerdom1
слоты покердом
РейкБек ПокерДом
РейкБек ПокерДом
РейкБек ПокерДом
скачать покердом на android
скачать покердом на android
скачать покердом на android
https://canadaph.life/# canada drugs online
medication canadian pharmacy: Certified Canada Pharmacy Online – canadian pharmacy world
Войти в покердом
https://t.me/s/vojti_v_pokerdom
Войти в покердом
Online medicine order: Medical Store in India – top 10 pharmacies in india
top 10 online pharmacy in india: india pharmacy – indian pharmacy
скачать клиент покердом на андроид
скачать клиент покердом на андроид
скачать клиент покердом на андроид
Приложение покердом
https://t.me/s/prilozhenie_pokerdom
Приложение покердом
зеркало покердом на деньги
https://t.me/s/ReflectivePoker
зеркало покердом на деньги
Покердом Рейкбек
https://t.me/s/reikbek_pokerDom
Покердом Рейкбек
I go to see each day some sites and websites to read articles or reviews, however this website provides feature based
content.
промокоды покердом
https://t.me/s/promocodes_pokerdom
промокоды покердом
промокоды на покердом
https://t.me/s/promokody_na_pokerdom
промокоды на покердом
покердом рабочее зеркало
покердом рабочее зеркало
покердом рабочее зеркало
ПокерДом Регистрация
ПокерДом Регистрация
ПокерДом Регистрация
покердом играть онлайн на деньги
покердом играть онлайн на деньги
покердом играть онлайн на деньги
https://canadaph.life/# canada drug pharmacy
промокод для покердом
https://t.me/s/promokod_dlya_pokerdom
промокод для покердом
промокод покердом покер
промокод покердом покер
промокод покердом покер
сайт покердом
https://t.me/s/pokerdom_website
сайт покердом
Покердом телеграм
Покердом телеграм
Покердом телеграм
покердом скачать
покердом скачать
покердом скачать
промокод покердом 2022
https://t.me/s/promokod_pokerdom2022
промокод покердом 2022
Покердом верификация
https://t.me/s/pokerdom_verifikaciya
Покердом верификация
покердом зеркало войти
покердом зеркало войти
покердом зеркало войти
покердом зеркало 2023
https://t.me/s/pokerdom_zerkal
покердом зеркало 2023
покердом играть в браузере
https://t.me/s/pokerdom_vbrauzere
покердом играть в браузере
покердом акции
покердом акции
покердом акции
покердом рабочее зеркало сегодня
https://t.me/s/pokerdom_working_mirror_today
покердом рабочее зеркало сегодня
покердом официальный сайт вход зеркало
https://t.me/s/pokerdom_oficialnyj_sajt_vhod_ze
покердом официальный сайт вход зеркало
Вывод денег из ПокерДома
https://t.me/s/pokerdom_s_vivodom
Вывод денег из ПокерДома
stromectol canada: ivermectin 8000 – ivermectin cream uk
рабочее зеркало покердом
рабочее зеркало покердом
рабочее зеркало покердом
обзор покердом
https://t.me/s/pokerdom_obzori
обзор покердом
покердом установить приложение
https://t.me/s/pokerdom_prilozhuha
покердом установить приложение
stromectol 3 mg dosage – https://ivermectin.today/# stromectol medication
buy stromectol online uk: buy ivermectin online – ivermectin syrup
Покердом ВЫВОД ДЕНЕЖНЫХ СРЕДСТВ
https://t.me/s/pokerDom_vyvodsredstv
Покердом ВЫВОД ДЕНЕЖНЫХ СРЕДСТВ
Покердом обзор
Покердом обзор
Покердом обзор
покердом скачать клиент на пк
покердом скачать клиент на пк
покердом скачать клиент на пк
покердом промокод бездепозитный бонус
покердом промокод бездепозитный бонус
покердом промокод бездепозитный бонус
покердом официальный сайт зеркало
https://t.me/s/pokerdom_oficialnyj_sajt3_zerkal
покердом официальный сайт зеркало
скачать покердом на планшет
https://t.me/s/pokerdom_naplanshet
скачать покердом на планшет
покердом зеркало скачать
https://t.me/s/pokerdom_mirrordownload
покердом зеркало скачать
ivermectin 3mg pill: buy ivermectin tablets for humans – buy stromectol online
покердом скачать на телефон
https://t.me/s/pokerdom_natelefon
покердом скачать на телефон
stromectol 6 mg tablet – http://ivermectin.today/# generic ivermectin cream
покердом зеркало играть
покердом зеркало играть
покердом зеркало играть
ivermectin 8 mg: stromectol – stromectol tablets
Покером ЛИЧНЫЙ КАБИНЕТ
https://t.me/s/pokerDom_lichnuy_cabinet
Покером ЛИЧНЫЙ КАБИНЕТ
скачать покердом на компьютер
скачать покердом на компьютер
скачать покердом на компьютер
покердом зеркало вход
покердом зеркало вход
покердом зеркало вход
покердом казино регистрация
покердом казино регистрация
покердом казино регистрация
Hello, I enjoy reading all of your article post.
I like to write a little comment to support you.
Покердом кз
Покердом кз
Покердом кз
покердом играть на деньги
покердом играть на деньги
покердом играть на деньги
ivermectin uk coronavirus: cost of ivermectin lotion – where to buy stromectol
ivermectin 2% – http://ivermectin.today/# ivermectin stromectol
покердом казино промокод
покердом казино промокод
покердом казино промокод
покердом зеркало для входа
покердом зеркало для входа
покердом зеркало для входа
ivermectin stromectol: ivermectin today – stromectol order online
скачать покердом бесплатно на телефон
https://t.me/s/skachat_pokerdom_natel
скачать покердом бесплатно на телефон
Пароли на фрироллы ПОКЕРДОМ
https://t.me/s/parolinafreeroll_pokerdom
Пароли на фрироллы ПОКЕРДОМ
покердом ios
https://t.me/s/pokerdom_ios
покердом ios
покердом на деньги
https://t.me/s/pokerdom_na_dengi
покердом на деньги
Cкачать покердом на русском
Cкачать покердом на русском
Cкачать покердом на русском
играть покердом
https://t.me/s/OnlineMirrorAce
играть покердом
покердом казино зеркало
https://t.me/s/pokerdom_casino_mirror
покердом казино зеркало
покердом мобильная версия
покердом мобильная версия
покердом мобильная версия
скачать покердом на реальные деньги
скачать покердом на реальные деньги
скачать покердом на реальные деньги
Не выводит деньги Покердом?
Не выводит деньги Покердом?
Не выводит деньги Покердом?
Покердом бонусный счет
https://t.me/s/pokerdom_bonusnyj_schet
Покердом бонусный счет
покердом коды
https://t.me/s/pokerdom_kodya
покердом коды
покердом как вынести с нулевым балансом покердом бонус
покердом как вынести с нулевым балансом покердом бонус
покердом как вынести с нулевым балансом покердом бонус
Мобильный ПокерДом
Мобильный ПокерДом
Мобильный ПокерДом
играть в покердом онлайн
https://t.me/s/play_pokerdom_online
играть в покердом онлайн
покердом пароли на фрироллы
https://t.me/s/pokerdom_frirolly
покердом пароли на фрироллы
покердом тв фриролл
https://t.me/s/promokod_tvfriroll
покердом тв фриролл
Вывод денег ПокерДом
Вывод денег ПокерДом
Вывод денег ПокерДом
пароли на покердом сегодня
пароли на покердом сегодня
пароли на покердом сегодня
Если ПокерДом не работает!
https://t.me/s/pokerdom_esli_ne_rabotaet
Если ПокерДом не работает!
Покердом зеркало сайта
Покердом зеркало сайта
Покердом зеркало сайта
ПокерДом ФРИРОЛЛЫ
ПокерДом ФРИРОЛЛЫ
ПокерДом ФРИРОЛЛЫ
Покердом промокод фриспины
https://t.me/s/pokerdom_promokod_frispiny
Покердом промокод фриспины
Обзор казино покердом
https://t.me/s/obzor_kazino_pokerdom
Обзор казино покердом
покердом бонусы
покердом бонусы
покердом бонусы
https://gabapentin.bid/# medicine neurontin 300 mg
stromectol generic name: stromectol tablet 3 mg – ivermectin buy online
Покердом зеркало основное
https://t.me/s/pokerdom_zerkalo_osnovnoe
Покердом зеркало основное
Фрироллы ПокерДом
Фрироллы ПокерДом
Фрироллы ПокерДом
промокод покердом при регистрации
https://t.me/s/pokerdompromo_code_registrat
промокод покердом при регистрации
Машина времени покердом
Машина времени покердом
Машина времени покердом
Покердом НА ПК
https://t.me/s/naPC_PokerDom
Покердом НА ПК
Покердом зеркало играть онлайн
https://t.me/s/pokerdom_zerkalo_igrat_onlajn
Покердом зеркало играть онлайн
покердом промокоды
покердом промокоды
покердом промокоды
играть в покердом
https://t.me/s/DomEchoGamer
играть в покердом
Как получить $10 на покердом
Как получить $10 на покердом
Как получить $10 на покердом
скачать клиент покердом
скачать клиент покердом
скачать клиент покердом
Pokerdom покердом зеркало
https://t.me/s/pokerdom_pokerdom_zerkalo
Pokerdom покердом зеркало
покердом скачать на пк
покердом скачать на пк
покердом скачать на пк
Вывести деньги из ПокерДом
Вывести деньги из ПокерДом
Вывести деньги из ПокерДом
Фриролл покердом
https://t.me/s/friroll_pokerdom
Фриролл покердом
ПокерДом Казахастан
https://t.me/s/kazahstan_PokerDom
ПокерДом Казахастан
пароли покердом
пароли покердом
пароли покердом
http://lasixfurosemide.store/# lasix 100 mg tablet
покердом промокод при регистрации
https://t.me/s/pokerdom_promo_zareg
покердом промокод при регистрации
stromectol coronavirus: stromectol 3mg tablets – ivermectin human
generic lasix: Furosemide over the counter – lasix 100 mg
lasix generic name: buy lasix – lasix generic name
Покердом пароль на фриролл
Покердом пароль на фриролл
Покердом пароль на фриролл
скачать покердом
скачать покердом
скачать покердом
пароли на фрироллы покердом
https://t.me/s/freroly_pokerdom
пароли на фрироллы покердом
покердом ру
покердом ру
покердом ру
покердом кабинет
https://t.me/s/pokerdom_kabinet
покердом кабинет
Бонусы от ПокерДом
Бонусы от ПокерДом
Бонусы от ПокерДом
покердом тв пароль
https://t.me/s/pokerdom_parol
покердом тв пароль
пароли на фрироллы покердом на сегодня
https://t.me/s/pokerdom_freeroll_passwords
пароли на фрироллы покердом на сегодня
I was able to find good info from your articles.
Бездепозитный бонус от ПокерДом
https://t.me/s/bonus_bez_deposita
Бездепозитный бонус от ПокерДом
https://lasixfurosemide.store/# furosemida 40 mg
покердом апк скачать
покердом апк скачать
покердом апк скачать
скачать покердом на компьютер с официального сайта
скачать покердом на компьютер с официального сайта
скачать покердом на компьютер с официального сайта
neurontin 800 mg pill: neurontin cost in singapore – neurontin prices generic
клиент покердом
https://t.me/s/pokerdom_klien
клиент покердом
покердом бездепозитный бонус 1000
https://t.me/s/pokerdom_bezdepozitnyj_bonus_100
покердом бездепозитный бонус 1000
Пароль на фриролл покердом тв
https://t.me/s/parol_na_friroll_pokerdom_tv
Пароль на фриролл покердом тв
покердом зарегистрироваться
покердом зарегистрироваться
покердом зарегистрироваться
https://canadaph.pro/# canada rx pharmacy world
I was very happy to find this great site.
I want to to thank you for ones time for this wonderful read!!
I definitely really liked every bit of it and i also have you saved as a favorite to look at new information in your website.
покердом официальный сайт скачать
https://t.me/s/OnlineMirrorShark
покердом официальный сайт скачать
покердом. покердом.
покердом. покердом.
покердом. покердом.
legitimate canadian pharmacy: canadian pharmacy online – safe canadian pharmacy
покердом на реальные деньги
https://t.me/s/MirrorPokerPro
покердом на реальные деньги
промокод покердом для старых игроков
https://t.me/s/pokerdom_dliaigrikiv
промокод покердом для старых игроков
http://mexicoph.icu/# mexico drug stores pharmacies
legitimate canadian online pharmacies: canadian drug pharmacy – canadian pharmacy no scripts
покердом играть онлайн
https://t.me/s/MirrorGambit
покердом играть онлайн
покердом. играть. онлайн. на. деньги.
покердом. играть. онлайн. на. деньги.
покердом. играть. онлайн. на. деньги.
Личный кабинет покердом
https://t.me/s/lichnyj_kabinet_pokerdom
Личный кабинет покердом
покердом бездепозитный бонус 2022
покердом бездепозитный бонус 2022
покердом бездепозитный бонус 2022
покердом официальный сайт скачать на андроид
https://t.me/s/DomPokerPro
покердом официальный сайт скачать на андроид
Our company has been offering university, college or high school students a great variety of opportunities to purchase coursework or other academic pieces of writing to enhance their chances of gaining the highest grades possible, as well as improving their academic performance in general. At our online trusted coursework writing service, students from different parts of the world are capable of finding a helping and supportive hand from the most profound and sophisticated experts in various fields of science. Our professionals originate from English-speaking countries. They have Ph.D. or Masters’ degrees and are highly experienced and qualified in academic and custom writing. Yes! To deliver effective coursework writing services and ensure that every customer’s needs are met, we have made it possible for everyone to choose the writers they like the most to work on their orders. To pick the right candidate, you can compare writers by experience levels, degrees, ratings, and customer feedback. Or, if you’re having a hard time choosing, you can ask our support team for help.
http://siradisc.com/sira/bbs/board.php?bo_table=free&wr_id=141210
Yes, it is absolutely safe to buy a research paper online as long as you’re buying it from a professional academic writing company. However, there are a few simple rules that you have to keep in mind to stay safe while purchasing academic papers online. No, it is not bad to pay a ‘write my paper’ service to write your paper. It is no secret that students around the world are turning to buy essays as a quick fix for their essay struggles. On top of that, writing is not only time-consuming and boring. It is also one of the essential parts of college life since it affects your grade significantly. For this reason, an increasing number of students understand that the essay papers available for purchase are an excellent solution. It helps to minimize the hassles of the homework you get at school as well as increase overall performance.
http://indiaph.ink/# india online pharmacy
актуальные промокоды покердом
актуальные промокоды покердом
актуальные промокоды покердом
покердом официальный сайт играть онлайн
https://t.me/s/Dom_EchoGamer
покердом официальный сайт играть онлайн
world pharmacy india: top online pharmacy india – buy prescription drugs from india
http://canadaph.pro/# best canadian pharmacy
казино покердом отзывы
казино покердом отзывы
казино покердом отзывы
покердом официальный сайт org
https://t.me/s/PokerDomAce
покердом официальный сайт org
pharmacies in mexico that ship to usa: mexican border pharmacies shipping to usa – medicine in mexico pharmacies
Aктуальное зеркало покердом
https://t.me/s/aktualnoe_zerkalo_pokerdom
Aктуальное зеркало покердом
cialis dosage 40 mg cialis buy online coupon for cialis
пароли на покердом
https://t.me/s/paroli_pokerdoma
пароли на покердом
buy prescription drugs from india: top 10 pharmacies in india – п»їlegitimate online pharmacies india
http://canadaph.pro/# canada pharmacy online
лицензионное казино pokerdom реальный обзор покердом слоты дом
https://t.me/s/DomPokerMaster
лицензионное казино pokerdom реальный обзор покердом слоты дом
http://canadaph.pro/# canadapharmacyonline legit
регистрация покердом
регистрация покердом
регистрация покердом
indian pharmacy: indian pharmacy online – indianpharmacy com
https://internationalpharmacy.icu/# order meds from canada
perscription canada: mail order prescriptions from canada – canada pharmacy no rx
canada prescription – interpharm.pro They’re globally connected, ensuring the best patient care.
Loving the information on this site, yоu һave dоne outstanding job
on the posts.
Also visit mʏ webpage … older home
legitimate online pharmacy usa: online indian pharmacy – canadian pharmacy services
canadian pharmcy – internationalpharmacy.icu Long-Term Effects.
https://interpharm.pro/# best pharmacy in canada
usa online pharmacy: canadian pharmacy prescription – canadadrugs coupon code
candaian pharmacy – internationalpharmacy.icu A reliable pharmacy in times of emergencies.
http://interpharm.pro/# canadian pharmacy on line
canadian drugs online: canada prescription drugs online – legitimate online pharmacy usa
mexican prescription drugs online – interpharm.pro Their international health campaigns are revolutionary.
http://internationalpharmacy.icu/# online pharmacy no perscription
I am in fact happy to glance at this webpage posts which consists of tons
of useful data, thanks for providing these kinds
of statistics.
biggest online pharmacy: canada pharmacy without prescription – buy medications online no prescription
no prescription canadian pharmacy – internationalpharmacy.icu Their global outlook is evident in their expansive services.
https://internationalpharmacy.icu/# top online pharmacies
top mail order pharmacies: canadian pharmacies that ship to us – reputable canadian pharmacies online
best online pharmacy without prescriptions – interpharm.pro Top 100 Searched Drugs.
https://internationalpharmacy.icu/# canadian farmacy
best overseas pharmacy: canada drug store – cnadian pharmacy
pharmacy.com canada – internationalpharmacy.icu The widest range of international brands under one roof.
http://interpharm.pro/# purchasing prescription drugs online
online pharmacy international – internationalpharmacy.icu Every visit reaffirms why I choose this pharmacy.
http://interpharm.pro/# best rated canadian online pharmacy
buy medication online without prescription: canadian prescription – canadian neighborhood pharmacy
best no prescription online pharmacies – internationalpharmacy.icu Their health seminars are always enlightening.
https://interpharm.pro/# no prescription canadian pharmacy
farmacia online madrid: farmacia online envГo gratis – farmacias online baratas
It’s really a great and useful piece of info. I’m happy that you simply shared this useful information with us.
Please stay us informed like this. Thank you for sharing.
https://pharmacieenligne.icu/# Pharmacie en ligne France
https://farmaciaonline.men/# farmaci senza ricetta elenco
gГјnstige online apotheke: online apotheke deutschland – online apotheke deutschland
farmacia envГos internacionales: farmacia online 24 horas – farmacia envГos internacionales
http://farmaciabarata.pro/# п»їfarmacia online
http://farmaciabarata.pro/# farmacia online internacional
farmacia 24h farmacias online seguras en espaГ±a п»їfarmacia online
п»їpharmacie en ligne: Pharmacie en ligne livraison gratuite – pharmacie ouverte 24/24
farmacia 24h: farmacias online seguras en espaГ±a – farmacia 24h
Thanks a lot for sharing this with all of us you really realize what you are talking approximately!
Bookmarked. Please additionally talk over with my website =).
We could have a hyperlink alternate agreement between us
https://onlineapotheke.tech/# gГјnstige online apotheke
Useful knowledge. Cheers.
buy customized essays essays order
pharmacie ouverte: Pharmacie en ligne sans ordonnance – acheter mГ©dicaments Г l’Г©tranger
http://farmaciaonline.men/# acquisto farmaci con ricetta
Hello, its fastidious article on the topic of media
print, we all know media is a great source of information.
https://pharmacieenligne.icu/# pharmacie ouverte
https://pharmacieenligne.icu/# п»їpharmacie en ligne
farmacia barata: farmacia online internacional – farmacias online baratas
Heya i am for the first time here. I came across this board and I find It really useful & it
helped me out much. I hope to give something back and aid others like you aided me.
Thank you a lot for sharing this with all people you actually understand what you’re speaking about!
Bookmarked. Please also discuss with my site =). We could
have a hyperlink alternate agreement between us
п»їonline apotheke: Sildenafil Preis Apotheke – online apotheke deutschland
farmacia envГos internacionales: viagra precio generico – farmacia barata
What i do not understood is in truth how you are not really a lot more neatly-preferred than you may be now.
You are so intelligent. You know thus considerably in relation to this matter, made me personally consider it from a lot of varied angles.
Its like women and men aren’t interested until it’s something to accomplish with Girl gaga!
Your personal stuffs great. Always maintain it up!
Thanks for another informative web site. The place else may
I get that kind of info written in such an ideal means? I have a challenge that
I’m just now running on, and I have been on the glance out for such info.
farmacia online madrid: Sildenafilo precio – farmacia barata
Viagra homme prix en pharmacie
https://esfarmacia.men/# farmacia online madrid
internet apotheke: kamagra kaufen – online apotheke deutschland
http://edpharmacie.pro/# Pharmacie en ligne pas cher
Acheter kamagra site fiable
It’s awesome for me to have a web site, which is beneficial for my experience.
thanks admin
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
скачать покердом бесплатно на телефон
скачать покердом бесплатно на телефон
скачать покердом бесплатно на телефон
покердом казино промокод
покердом казино промокод
покердом казино промокод
Cкачать покердом на русском
https://t.me/s/skachat_pokerdom_na_russkom
Cкачать покердом на русском
покердом казино промокод
покердом казино промокод
покердом казино промокод
п»їpharmacie en ligne: acheter medicament a l etranger sans ordonnance
скачать покердом на реальные деньги
скачать покердом на реальные деньги
скачать покердом на реальные деньги
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
acheter mГ©dicaments Г l’Г©tranger – acheter medicament a l etranger sans ordonnance
покердом как вынести с нулевым балансом покердом бонус
покердом как вынести с нулевым балансом покердом бонус
покердом как вынести с нулевым балансом покердом бонус
farmacias online baratas: comprar viagra sin receta – farmacia barata
покердом казино промокод
покердом казино промокод
покердом казино промокод
http://itfarmacia.pro/# migliori farmacie online 2023
покердом тв фриролл
покердом тв фриролл
покердом тв фриролл
покердом казино промокод
покердом казино промокод
покердом казино промокод
You are so interesting! I do not suppose I have read something like that before.
So nice to discover another person with some genuine thoughts on this issue.
Seriously.. many thanks for starting this up.
This website is one thing that is needed on the web, someone with a bit of originality!
Покердом зеркало сайта
https://t.me/s/pokerdom_zerkalo_sajta1
Покердом зеркало сайта
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
https://indiapharm.cheap/# indian pharmacy online
Покердом зеркало основное
https://t.me/s/pokerdom_zerkalo_osnovnoe
Покердом зеркало основное
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
Покердом промокод фриспины
Покердом промокод фриспины
Покердом промокод фриспины
Post writing is also a excitement, if you be familiar with afterward you can write
if not it is difficult to write.
Покердом зеркало играть онлайн
Покердом зеркало играть онлайн
Покердом зеркало играть онлайн
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
промокод покердом при регистрации
https://t.me/s/pokerdompromo_code_registrat
промокод покердом при регистрации
I quite like reading a post that will make people think. Also, many thanks for permitting me to comment!
[url=https://sites.google.com/view/stmracing/%E0%B8%AB%E0%B8%99%E0%B8%B2%E0%B9%81%E0%B8%A3%E0%B8%81]ท่อไอเสียรถยนต์[/url]
ไส้ท่อไอเสีย
покердом скачать на пк
покердом скачать на пк
покердом скачать на пк
покердом промокоды
https://t.me/s/pokerdompromo
покердом промокоды
I think this is among the most important
information for me. And i’m glad reading your article.
But wanna remark on few general things, The web site style is ideal, the articles
is really excellent : D. Good job, cheers
Pokerdom покердом зеркало
https://t.me/s/pokerdom_pokerdom_zerkalo
Pokerdom покердом зеркало
Hi there just wanted to give you a quick heads up. The text in your article seem to be running off
the screen in Opera. I’m not sure if this is a format issue or something to do with browser compatibility but I thought I’d post to let you
know. The design look great though! Hope you get the problem resolved soon. Kudos
покердом ру
покердом ру
покердом ру
пароли покердом
пароли покердом
пароли покердом
I’m extremely impressed with your writing skills and also
with the layout on your weblog. Is this a paid theme or did you modify it yourself?
Anyway keep up the excellent quality writing, it’s rare to see
a great blog like this one these days.
My developer is trying to persuade me to move to .net from PHP.
I have always disliked the idea because of the expenses.
But he’s tryiong none the less. I’ve been using Movable-type on various
websites for about a year and am concerned about switching to another platform.
I have heard excellent things about blogengine.net. Is there a way I can transfer all
my wordpress posts into it? Any kind of help would be
really appreciated!
Покердом пароль на фриролл
https://t.me/s/pokerdom_parol_na_friroll
Покердом пароль на фриролл
покердом тв пароль
покердом тв пароль
покердом тв пароль
The go-to place for all my healthcare needs. reliable canadian pharmacy: canadian pharmacy meds reviews – canadian pharmacy 24h com safe
покердом кабинет
покердом кабинет
покердом кабинет
покердом апк скачать
покердом апк скачать
покердом апк скачать
Покером ЛИЧНЫЙ КАБИНЕТ
https://t.me/s/pokerDom_lichnuy_cabinet
Покером ЛИЧНЫЙ КАБИНЕТ
пароли на фрироллы покердом на сегодня
пароли на фрироллы покердом на сегодня
пароли на фрироллы покердом на сегодня
https://indiapharm.cheap/# india pharmacy mail order
клиент покердом
клиент покердом
клиент покердом
покердом казино регистрация
покердом казино регистрация
покердом казино регистрация
скачать покердом на компьютер с официального сайта
https://t.me/s/PokerDomChamp
скачать покердом на компьютер с официального сайта
canadianpharmacymeds: canadian pharmacy phone number – canada pharmacy online legit
покердом зарегистрироваться
покердом зарегистрироваться
покердом зарегистрироваться
What’s Happening i am new to this, I stumbled upon this I’ve discovered It
absolutely useful and it has aided me out loads.
I am hoping to contribute & aid other users like its helped me.
Great job.
Hi! I know this is kind of off-topic however I needed to ask.
Does building a well-established website such as yours take a large amount
of work? I’m completely new to operating a blog
however I do write in my diary every day. I’d like to start a blog so I can easily
share my experience and views online. Please let me know if you have any kind of ideas or tips for new
aspiring blog owners. Thankyou!
покердом бездепозитный бонус 1000
покердом бездепозитный бонус 1000
покердом бездепозитный бонус 1000
Hello there, You’ve done a great job. I will definitely digg it
and personally suggest to my friends. I am confident they’ll be benefited from this web
site.
покердом играть на деньги
покердом играть на деньги
покердом играть на деньги
Today, I went to the beach front with my kids. I found a
sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She placed the shell to her ear and screamed.
There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is totally off topic
but I had to tell someone!
I think this is among the most important info for me. And i am glad reading your article.
But should remark on few general things, The website style is wonderful, the
articles is really excellent : D. Good job, cheers
покердом. покердом.
покердом. покердом.
покердом. покердом.
Very shortly this web page will be famous among all blogging
and site-building visitors, due to it’s nice posts
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
Пароль на фриролл покердом тв
Пароль на фриролл покердом тв
Пароль на фриролл покердом тв
покердом зеркало для входа
https://t.me/s/pokerdom_entrance_mirror
покердом зеркало для входа
Good post. I learn something totally new and challenging on blogs I stumbleupon on a
daily basis. It will always be useful to read articles from other authors and practice
something from their sites.
Link exchange is nothing else except it is only placing the other person’s webpage link on your page at proper place
and other person will also do similar in support of you.
northwest pharmacy canada canadian pharmacy online ship to usa real canadian pharmacy
промокод покердом для старых игроков
промокод покердом для старых игроков
промокод покердом для старых игроков
покердом официальный сайт скачать
покердом официальный сайт скачать
покердом официальный сайт скачать
покердом казино промокод
https://t.me/s/pokerdomkazino_promokod
покердом казино промокод
Пароли на фрироллы ПОКЕРДОМ
Пароли на фрироллы ПОКЕРДОМ
Пароли на фрироллы ПОКЕРДОМ
purple pharmacy mexico price list: medication from mexico pharmacy – mexican pharmaceuticals online
Hello there! I know this is somewhat off topic but I was wondering which blog platform are you using for this website?
I’m getting fed up of WordPress because I’ve had problems with hackers and I’m looking at
options for another platform. I would be fantastic if you could point me in the direction of
a good platform.
онлайн казино на рубли
онлайн казино на рубли
онлайн казино на рубли
I’m impressed with their commitment to customer care. canadian mail order pharmacy: best canadian pharmacy to buy from – canadapharmacyonline
Thank you for sharing your info. I really appreciate your
efforts and I am waiting for your next post
thank you once again.
pharmacies in mexico that ship to usa medication from mexico pharmacy purple pharmacy mexico price list
best online pharmacy india: reputable indian online pharmacy – mail order pharmacy india
Yes! Finally something about assignment help.
казино с бонусом за регистрацию без депозита
казино с бонусом за регистрацию без депозита
http://mexicopharm.store/# mexico drug stores pharmacies
I’m more than happy to discover this site. I need to to thank you for your time for this wonderful read!!
I definitely loved every part of it and I have you saved as a favorite to check out new things in your blog.
If some one desires expert view about blogging and site-building then i advise him/her to visit this webpage, Keep
up the fastidious work.
What’s up to all, since I am genuinely eager of reading this webpage’s
post to be updated daily. It carries fastidious material.
казино онлайн бонус за регистрацию
казино онлайн бонус за регистрацию
Heya i’m for the first time here. I came across this board and
I in finding It truly useful & it helped me out a lot. I am hoping to give something back and help others like you helped me.
I’m truly enjoying the design and layout of
your website. It’s a very easy on the eyes which makes it much more enjoyable for me
to come here and visit more often. Did you hire out a designer to
create your theme? Excellent work!
Thanks for every other fantastic article. Where else may anyone
get that type of information in such a perfect means of writing?
I’ve a presentation subsequent week, and I
am on the search for such information.
Right now it appears like Expression Engine is the best blogging platform
out there right now. (from what I’ve read) Is that
what you are using on your blog?
новые бездепозитные бонусы казино
новые бездепозитные бонусы казино
онлайн казино с бездепозитным бонусом
онлайн казино с бездепозитным бонусом
казино с бонусом за регистрацию на вывод
казино с бонусом за регистрацию на вывод
Hey! I’m at work browsing your blog from my new apple iphone!
Just wanted to say I love reading through your blog
and look forward to all your posts! Carry on the superb work!
My blog post … http://test2.premium4best.eu/
bonus casino
https://t.me/s/SpinToWinGuru
топ казино с бездепозитным бонусом за регистрацию
https://t.me/s/SpinItToWinKing
казино с бонусами
казино с бонусами
казино бездепозитный бонус
https://t.me/s/kazinopokerdom_bezdep
онлайн казино с бонусом за регистрацию
онлайн казино с бонусом за регистрацию
казино онлайн с бездепозитным бонусом за регистрацию
казино онлайн с бездепозитным бонусом за регистрацию
india online pharmacy online pharmacy india cheapest online pharmacy india
казино бонусы
казино бонусы
слоты онлайн бонусы за регистрацию
слоты онлайн бонусы за регистрацию
казино без депозита
https://t.me/s/kazino_beadepozita
бонус в казино без депозита
бонус в казино без депозита
Their online refill system is straightforward. best india pharmacy: world pharmacy india – indian pharmacies safe
игровые автоматы деньги за регистрацию
игровые автоматы деньги за регистрацию
kasino bonus
kasino bonus
слоты бездепозитный бонус
слоты бездепозитный бонус
бонусы казино
бонусы казино
бездепозитный бонус за простую регистрацию сразу на счет с выводом
https://t.me/s/pokerdom_bonys
игровые автоматы с бездепозитным бонусом за регистрацию
https://t.me/s/igrovye_avtomaty_s_bezdepozitnym
казино онлайн бездепозитный бонус за регистрацию
https://t.me/s/pokerdom_bonysyonlain
First of all I want to say superb blog! I had a quick question in which I’d like
to ask if you do not mind. I was interested to know how
you center yourself and clear your mind before
writing. I’ve had a difficult time clearing my mind
in getting my thoughts out there. I do take pleasure in writing but it just seems like the first 10 to 15 minutes tend to be lost just trying to figure out how
to begin. Any suggestions or hints? Appreciate it!
свежие бездепозитные бонусы казино за регистрацию
https://t.me/s/bonysy_zaregsitpokerdom
казино с отыгрышем бездепозитный бонус
https://t.me/s/pokerdom_promod
It’s very easy to find out any topic on web as compared to books, as I found this post at this site.
новые казино с бездепозитным бонусом за регистрацию
новые казино с бездепозитным бонусом за регистрацию
игровые автоматы без депозита
https://t.me/s/igrovye_avtomaty_bez_depozita
новый бездепозитный бонус за регистрацию
новый бездепозитный бонус за регистрацию
bonus casino
https://t.me/s/bonysi_kazino
интернет казино бонус
интернет казино бонус
казино онлайн с бонусом
https://t.me/s/kazinopokerdom_sbonysom
бонус казино без депозита
https://t.me/s/bonus_kazino_bez_depozita_tut
бонус в казино за регистрацию
https://t.me/s/bonyszaregist_pokerdom
Can I simply say what a comfort to uncover somebody who truly
understands what they’re discussing on the net.
You actually realize how to bring an issue to light and make
it important. More and more people ought to check this out
and understand this side of the story. I was surprised that you aren’t more popular because you definitely have the gift.
казино с бездепозитным бонусом за регистрацию
https://t.me/s/bezdepza_registriaciupokerdom
You can definitely see your enthusiasm within the article you write.
The world hopes for more passionate writers like you who aren’t afraid to say how
they believe. At all times go after your heart.
online casino bonus za registraci
online casino bonus za registraci
бездепозитный бонус за регистрацию казино
https://t.me/s/bezdepozitnyj_bonus_za_registrac
казино онлайн бонус
https://t.me/s/kazinoonlain_bonys
reputable indian pharmacies india online pharmacy online shopping pharmacy india
бездепозитный бонус за простую регистрацию сразу на счет 2022
бездепозитный бонус за простую регистрацию сразу на счет 2022
казино бонус за регистрацию
казино бонус за регистрацию
Hey There. I found your blog using msn. This is a really well written article.
I’ll be sure to bookmark it and return to read more of your useful info.
Thanks for the post. I will certainly comeback.
prescription drugs canada buy online: pharmacy canadian superstore – canada pharmacy
свежие бездепозитные бонусы казино за регистрацию 2022
свежие бездепозитные бонусы казино за регистрацию 2022
игровые автоматы с бездепозитным бонусом при регистрации
игровые автоматы с бездепозитным бонусом при регистрации
Wow, incredible blog layout! How long have you been blogging for?
you made blogging look easy. The overall look of your web site
is great, let alone the content!
казино с бездепом
казино с бездепом
best online canadian pharmacy: canadian pharmacy checker – is canadian pharmacy legit
Amazing blog! Do you have any tips and hints for aspiring writers?
I’m hoping to start my own website soon but I’m a little lost on everything.
Would you suggest starting with a free platform like
Wordpress or go for a paid option? There are so many choices out there
that I’m completely overwhelmed .. Any tips?
Kudos!
We stumbled over here coming from a different
page and thought I might check things out. I like what I see so now
i’m following you. Look forward to checking out your web page yet again.
It’s a shame you don’t have a donate button! I’d definitely donate to this fantastic blog!
I suppose for now i’ll settle for bookmarking and adding
your RSS feed to my Google account. I look forward to new updates and will share this site with my Facebook group.
Chat soon!
получить бездепозитный бонус в казино
https://t.me/s/bezdeppokerdom_onlain
I think this is one of the most vital information for me.
And i’m glad reading your article. But want to remark on some general things, The
site style is perfect, the articles is really great : D.
Good job, cheers
бонус казино
бонус казино
слоты без депозита
слоты без депозита
http://canadapharm.store/# canadian neighbor pharmacy
казино деньги за регистрацию
казино деньги за регистрацию
бездеп
бездеп
Hi there, all is going fine here and ofcourse every one
is sharing information, that’s genuinely excellent, keep up writing.
I have read so many content about the blogger lovers however this article is actually a fastidious piece of
writing, keep it up.
Wow, that’s what I was searching for, what a material!
present here at this website, thanks admin of this website.
игровые автоматы бездепозитный бонус за регистрацию
игровые автоматы бездепозитный бонус за регистрацию
бездепозитный бонус казино при регистрации
https://t.me/s/BetBlitzShark
бездеп казино
https://t.me/s/RouletteRendezvous
список казино с бонусами
список казино с бонусами
казино дающие бездепозитные бонусы
https://t.me/s/BetBlitzMaestro
The bank chosen have to be ready to incorporate the desired features within the personal loan.
If the university has fine arts related programs, this will
be an added advantage. These loans offer a bigger loan amount in the range of.
бонус без депозита
https://t.me/s/pokerdom_ponysybezpeposita
Highly descriptive post, I loved that bit. Will there be a part 2?
казино с бонусом без депозита
казино с бонусом без депозита
онлайн казино с бонусом
https://t.me/CasinoMysticWager
онлайн казино с бонусами за регистрацию
онлайн казино с бонусами за регистрацию
автоматы с бездепозитным бонусом
автоматы с бездепозитным бонусом
Write more, thats all I have to say. Literally, it seems as
though you relied on the video to make your point.
You definitely know what youre talking about, why throw away
your intelligence on just posting videos to your blog when you could
be giving us something enlightening to read?
casino бездепозитный бонус за регистрацию
casino бездепозитный бонус за регистрацию
игровые автоматы с бездепозитным бонусом
игровые автоматы с бездепозитным бонусом
bezdepozitni bonus
bezdepozitni bonus
слот казино бездепозитный бонус
слот казино бездепозитный бонус
онлайн казино бонус без депозита
онлайн казино бонус без депозита
bezdepov
https://t.me/s/SlotSorcererExtraordinaire
Long-Term Effects. mexican drugstore online: best online pharmacies in mexico – reputable mexican pharmacies online
best online pharmacies in mexico mexican pharmaceuticals online reputable mexican pharmacies online
казино с бонусом за регистрацию
https://t.me/s/CasinoMystique
bezdep casino
bezdep casino
If you wish for to obtain a good deal from this piece of writing then you have to
apply such methods to your won blog.
игровые автоматы бездепозитный бонус
игровые автоматы бездепозитный бонус
why casino бездепозитный бонус
why casino бездепозитный бонус
Since the admin of this web site is working, no doubt very shortly it will be famous, due to its feature contents.
фрибеты казино
https://t.me/s/RouletteRacerElite
Make a comparison among the funding options is certainly an additional
way to make your search for the loan option better and more
fruitful. Headlines say that nations are mired in debts, and editorials criticize the “irresponsible borrowers”, “reckless lenders” and even today’s “consumerist culture” is sometimes held responsible for it.
That is where option two comes into play for you,
the unsecured credit loans.
бездепозитный бонус в казино
https://t.me/s/CasinoGokdRush
игровые автоматы где дают деньги за регистрацию
https://t.me/s/RouletteRacer
игровые автоматы бонус без депозита
игровые автоматы бонус без депозита
свежие бездепозитные бонусы за регистрацию
https://t.me/s/pokerdom_bezdepzaregistraciu
бездепозитный бонус за простую регистрацию сразу на счет с выводом 2022
бездепозитный бонус за простую регистрацию сразу на счет с выводом 2022
бездепозитный бонус за регистрацию в казино
бездепозитный бонус за регистрацию в казино
казино бонусы за регистрацию
https://t.me/s/pokerdom_bonysyzareg
казино дающие бонус
казино дающие бонус
новые казино с бездепозитными бонусами
https://t.me/s/novye_kazino_s_bezdepozitnymi
бесплатные бонусы от казино
бесплатные бонусы от казино
Hello! I know this is somewhat off topic but I was wondering which
blog platform are you using for this site? I’m getting sick and tired of WordPress because I’ve had issues
with hackers and I’m looking at alternatives for another platform.
I would be fantastic if you could point me in the direction of a good platform.
казино бонус без депозита
https://t.me/s/BetBlitzSultan
бонусы в казино без депозита
https://t.me/s/pokerdom_bonysybezdeposita
Amazing blog! Do you have any suggestions for aspiring
writers? I’m planning to start my own blog soon but I’m a little lost on everything.
Would you advise starting with a free platform like WordPress or go for a paid option? There are so many options out there that I’m totally confused ..
Any tips? Kudos!
казино бонус при регистрации без депозита
https://t.me/s/kazino_bonus_pri_registracii
бонусы онлайн казино
бонусы онлайн казино
Hello it’s me, I am also visiting this website daily, this web page is in fact pleasant and the viewers are truly sharing pleasant
thoughts.
бонусы казино онлайн
https://t.me/s/pokerdom_bbonysy
бездепозитные бонусы в казино
https://t.me/s/BetBigWinnner
онлайн казино без депозита
https://t.me/s/pokerdom_bezdepozita
казино бездепозитный бонус с выводом
казино бездепозитный бонус с выводом
online bonus casino
https://t.me/s/pokerdombonys_casino
online pharmacy india reputable indian pharmacies online pharmacy india
бездепозитные бонусы казино
https://t.me/s/bezdep_kazinos
игровые автоматы бонус при регистрации без депозита
игровые автоматы бонус при регистрации без депозита
I do consider all of the concepts you’ve presented in your post.
They are very convincing and will definitely work.
Still, the posts are very brief for novices. May you please extend them a little from next time?
Thank you for the post.
казино дающие деньги за регистрацию с выводом
https://t.me/s/kazino_pokerdomsvivodom
I do believe all of the concepts you have introduced on your post.
They are very convincing and will definitely work.
Nonetheless, the posts are very brief for starters. Could you please lengthen them a
little from subsequent time? Thank you for the post.
Nice response in return of this matter with solid arguments and
telling the whole thing concerning that.
My brother suggested I may like this website. He was once totally right.
This post truly made my day. You can not imagine just how so much time
I had spent for this information! Thank you!
бездепозитный бонус в казино за регистрацию
бездепозитный бонус в казино за регистрацию
continuously i used to read smaller articles that
as well clear their motive, and that is also happening with this post which I am reading here.
казино бонус за регистрацию без депозита
https://t.me/s/bonus_za_registraciyu_bez_depozi
india pharmacy: Online medicine home delivery – Online medicine order
депозитный бонус казино
https://t.me/s/CasinoCashTycoon
бездепозитный бонус казино
бездепозитный бонус казино
I have read so many articles or reviews concerning the blogger lovers but this
article is actually a fastidious paragraph, keep it up.
деньги за регистрацию в казино без депозита
https://t.me/s/JackpotHunterv
бездепозитные бонусы онлайн казино
бездепозитные бонусы онлайн казино
https://canadapharm.store/# canadian pharmacy ed medications
You ought to be a part of a contest for one of the finest websites on the net.
I will highly recommend this site!
бонус при регистрации в казино без депозита
бонус при регистрации в казино без депозита
Howdy, i rrad your blog from timje to tijme and i owwn a similar one aand i waas jst wondeeing
if yyou get a loot off sspam remarks? If soo how doo youu reducfe
it, aany pluygin orr anything yoou ccan suggest? I get so uch lqtely it’s drivinhg me
mad soo any help is very much appreciated.
бонусы в казино
бонусы в казино
бонус при регистрации казино
бонус при регистрации казино
фрибет казино
фрибет казино
онлайн казино бездепозитный бонус за регистрацию
https://t.me/s/pokerdom_bezdeposit
бездепозит
https://t.me/s/bezdepozit_tut
бонус за регистрацию в казино без депозита
https://t.me/s/SlotSorcererer
бездепозитный бонус казино с выводом
https://t.me/s/DiceRollerWizar
новые бездепозитные бонусы
https://t.me/s/BetBillionaireGambit
игровые автоматы с бонусами
игровые автоматы с бонусами
I think that is among the most important info for me.
And i am glad studying your article. However should commentary on few general issues,
The web site style is great, the articles is in reality great
: D. Just right job, cheers
you’re really a good webmaster. The site loading velocity is incredible.
It kind of feels that you’re doing any unique trick.
In addition, The contents are masterwork. you’ve performed a magnificent process on this matter!
Read information now. buying prescription drugs in mexico: mexican rx online – medication from mexico pharmacy
бездеп казино за регистрацию
бездеп казино за регистрацию
mexican online pharmacies prescription drugs: mexican online pharmacies prescription drugs – mexican pharmaceuticals online
игровые автоматы на деньги с бонусом при регистрации
игровые автоматы на деньги с бонусом при регистрации
бонусы за регистрацию в казино
бонусы за регистрацию в казино
онлайн казино с бездепозитными бонусами
https://t.me/s/CardSharkVirtuoso
гудс бонус за регистрацию
https://t.me/DiceRollerSavant
бездепозитный бонус казино без скачивания
https://t.me/s/SlotSorcererPro
buying prescription drugs in mexico medication from mexico pharmacy medicine in mexico pharmacies
казино с бездепозитным бонусом при регистрации
казино с бездепозитным бонусом при регистрации
казино с фрибетом
казино с фрибетом
бонус за регистрацию онлайн казино
бонус за регистрацию онлайн казино
бонус без депозита игровые автоматы
бонус без депозита игровые автоматы
онлайн казино бездепозитный бонус
онлайн казино бездепозитный бонус
игровые автоматы деньги за регистрацию без депозита
https://t.me/s/RouletteRoyaltyGambler
игровые автоматы бонус за регистрацию
https://t.me/s/CasinoMogulllll
бездеп в казино
бездеп в казино
казино с бонусом при регистрации
https://t.me/s/pokerdom_shedriebonysy
казино бездеп
казино бездеп
онлайн казина с бонус без депозит
https://t.me/s/pokerdom_regabonysy
новые казино с бездепозитным бонусом
https://t.me/s/Casinocchampion
казино бонус при регистрации
казино бонус при регистрации
казино с бездепозитными бонусами
казино с бездепозитными бонусами
бездепозитні бонуси казино
https://t.me/s/pokerdom_kazinoos
онлайн казино бонус
https://t.me/s/pokerdom_onlainkazinobonys
бездепозитное казино
https://t.me/s/CasinoCashCaptain
Fantastic site you have here but I was wondering if you
knew of any forums that cover the same topics discussed in this article?
I’d really love to be a part of group where I can get suggestions from other experienced
individuals that share the same interest. If you have any
suggestions, please let me know. Thanks a lot!
казино с бонусами за регистрацию без депозита
казино с бонусами за регистрацию без депозита
бонусы за регистрацию казино
https://t.me/s/kazinopoker_dom
What a information of un-ambiguity and preserveness of valuable
familiarity regarding unpredicted feelings.
бездепозитные бонусы в казино 2021
https://t.me/s/pokerdom_kazino2021
бонус без депозита казино
бонус без депозита казино
список казино с бездепозитным бонусом
https://t.me/s/pokerdom_lycheekazino
casino bez depozita
https://t.me/s/pokerdom_bezdepositaa
казино онлайн бездепозитный бонус
казино онлайн бездепозитный бонус
казино бонус без депозит
казино бонус без депозит
buying from canadian pharmacies prescription drugs canada buy online canadian pharmacy meds review
бездепозитные казино
https://t.me/s/BetBilliona1rre
деньги за регистрацию
https://t.me/s/dengi_zaregpokerdom
казино с денежным бонусом
https://t.me/s/pokerdom_kazinosbonysom
бездепозитные онлайн казино
https://t.me/s/DiceRollerExpertv
бездепы
бездепы
казино дающие деньги за регистрацию
https://t.me/s/dengizaregistraciu_pokerdom
Перед вами настоящая классика
юмористического рассказа.
Произведения Марка Твена могут быть гомерически смешными или иронично хлёсткими, добродушно весёлыми или саркастически едкими.
Юмористические рассказы
бонус за регистрацию казино
https://t.me/DiceRollerPro
казино без первого депозита
казино без первого депозита
казино с бездепом за регистрацию
https://t.me/s/pokerdomkazino_bezdeps
https://indiapharm.cheap/# top online pharmacy india
india online pharmacy: buy prescription drugs from india – indian pharmacy online
деньги за регистрацию в казино
https://t.me/s/dengi_vpokerdom
бездепозитные казино онлайн
https://t.me/s/pokerdom_bezdepbonys
казино онлайн без депозита
казино онлайн без депозита
фрибет без депозита казино
https://t.me/s/fribet_pokerdom
Hello! This is my first visit to your blog!
We are a team of volunteers and starting a new initiative in a community
in the same niche. Your blog provided us useful information to
work on. You have done a marvellous job!
лучшие казино с бездепозитным бонусом
лучшие казино с бездепозитным бонусом
Offering a global gateway to superior medications. buying prescription drugs in mexico: reputable mexican pharmacies online – mexican rx online
бонус за регистрацию который можно сразу снять
бонус за регистрацию который можно сразу снять
игровые автоматы бесплатно с бонусами
https://t.me/s/pokerdom_besplatnoa
фрибеты в казино
https://t.me/s/fribet_pokerdoms
казино онлайн бонус
https://t.me/s/kazinoonlain_bonys
казино где дают бездепозитный бонус
https://t.me/s/kazinopokerdom_bosysy
бонусы без депозита казино
https://t.me/s/bonusy_bez_depozita_kazino
bonus casino online
https://t.me/s/casinoonlainbonus
бездепозитный казино
https://t.me/s/CardSharkChampionvv
какие казино дают бездепозитный бонус
какие казино дают бездепозитный бонус
бездепозитные бонусы
бездепозитные бонусы
medicine in mexico pharmacies buying prescription drugs in mexico online best online pharmacies in mexico
онлайн казино бонус при регистрации
онлайн казино бонус при регистрации
казино бонус
https://t.me/s/casino_bonustut
бездеп бонус казино
https://t.me/s/bezdep_bonus_kazin
казино без депозита бонус
казино без депозита бонус
игровые автоматы с депозитом за регистрацию
игровые автоматы с депозитом за регистрацию
I will immediately grasp your rss feed as I can not to find your email subscription hyperlink or e-newsletter
service. Do you’ve any? Please allow me recognise in order that I could subscribe.
Thanks.
casino бездепозитный бонус
https://t.me/s/casino_bonusbezdeposita
самые новые бездепозитные бонусы казино
самые новые бездепозитные бонусы казино
игровые автоматы с бонусом
https://t.me/s/avtomaty_pokerdom
I know this website gives quality based content and other material, is there
any other web site which offers these kinds of things in quality?
казино онлайн с бонусом за регистрацию
казино онлайн с бонусом за регистрацию
I’m really loving the theme/design of your site. Do you ever run into any browser compatibility problems?
A number of my blog visitors have complained about
my website not working correctly in Explorer but looks great
in Firefox. Do you have any solutions to help fix this problem?
казино с бонусами без депозита
https://t.me/s/DiceRollerWhisperer
бонус за регистрацию в казино
бонус за регистрацию в казино
Hi would you mind letting me know which hosting company you’re working with?
I’ve loaded your blog in 3 different internet browsers and I must say this blog loads a lot faster then most.
Can you suggest a good internet hosting provider at a honest price?
Kudos, I appreciate it!
новое бездепозитное казино
новое бездепозитное казино
buy prescription drugs from india: indian pharmacy online – pharmacy website india
бездепозитные бонусы в казино за регистрацию
https://t.me/s/BetBillionairevv
бездеп бонус
https://t.me/s/CasinoMogulMastermind
I think thiss is onne of thee most significanbt information for me.
Annd i amm lad reaxing your article. But wwant to
remark on some geeral things, The website style iss ideal, the articfles is
reeally exellent : D. Goood job, cheers
казино бездепозитный бонус за регистрацию
https://t.me/s/bonus_casino_za_registraciyu
казино без депозита с выводом денег 2022
казино без депозита с выводом денег 2022
казино фрибет
казино фрибет
бездепозитный бонус автоматы
https://t.me/s/CasinoCashCaptainAce
бездепозитный бонус казино за регистрацию
бездепозитный бонус казино за регистрацию
казино без депозита с бонусом за регистрацию
https://t.me/s/kazino_bez_depozita_s_bonusom
казино бонусы без депозита
казино бонусы без депозита
india pharmacy indian pharmacy paypal top online pharmacy india
новые бездепозитные бонусы в казино
https://t.me/s/CardSharkChampionX
бездепы казино
https://t.me/s/bezdepy_kazino
бездепозитные бонусы за регистрацию
бездепозитные бонусы за регистрацию
бонусы за регистрацию
бонусы за регистрацию
игровые автоматы бонусы за регистрацию
https://t.me/s/igrovye_avtomaty_bonusy25
бонуси казино
https://t.me/s/bonysukazino_pokerdom
doxycycline rx buy doxycycline for acne doxycycline 100mg tablets nz
I’m gone to say to my little brother, that he should also go to see this
webpage on regular basis to obtain updated
from most up-to-date news update.
бонусы в онлайн казино
бонусы в онлайн казино
kazino bonusi
https://t.me/s/SpinToVictoryKing
Love their spacious and well-lit premises. http://azithromycinotc.store/# order zithromax over the counter
игровые автоматы без первого депозита
игровые автоматы без первого депозита
бонус в казино
бонус в казино
bezdepozitni bonus casino
bezdepozitni bonus casino
слоты бонус за регистрацию
слоты бонус за регистрацию
бонусы бездепозитные казино
бонусы бездепозитные казино
бездепозитные игровые автоматы
https://t.me/s/bezdepozitnye_igrovye_avtomaty
бездеп за регистрацию в казино
https://t.me/CasinoCashConnoiss
казино фрибет без депозита
https://t.me/s/SlotSensationWhisperer
casino bonus za registraci
casino bonus za registraci
бездепозит казино
бездепозит казино
игровые автоматы бонус
https://t.me/s/RouletteRicochetPro
бездепозитный бонус за регистрацию в онлайн казино
бездепозитный бонус за регистрацию в онлайн казино
бонусы при регистрации в казино
https://t.me/s/BetBillionaireVegas
топ онлайн казино с бездепозитным бонусом
топ онлайн казино с бездепозитным бонусом
игровые автоматы бездепозитные
https://t.me/s/pokerdomm_bezzdep
автоматы с бездепозитным бонусом
https://t.me/s/BetBlitzGambitKing
I loved as much as you’ll receive carried out right here.
The sketch is attractive, your authored subject matter stylish.
nonetheless, you command get got an nervousness over
that you wish be delivering the following. unwell unquestionably come further formerly again as exactly the same nearly a lot often inside case you shield this increase.
все казино с бездепозитным бонусом
все казино с бездепозитным бонусом
лучшие бонусы казино
https://t.me/s/pokerdom_luuchiebonysy
игровые автоматы без первого депозита с бонусом
https://t.me/s/avtomaty_bez_pervogo_depozita
бонусы в казино за регистрацию
бонусы в казино за регистрацию
онлайн казино бонусы
онлайн казино бонусы
Appreciating the time and energy you put into your website and
in depth information you present. It’s nice to
come across a blog every once in a while that isn’t
the same outdated rehashed information. Excellent read! I’ve bookmarked your
site and I’m adding your RSS feeds to my Google account.
Hi there, just became alert to your blog through Google, and found
that it is truly informative. I am gonna watch out for brussels.
I will appreciate if you continue this in future.
A lot of people will be benefited from your writing. Cheers!
http://edpillsotc.store/# generic ed drugs
бонусы без депозита в казино
https://t.me/s/DiceRollerSavantPro
в каких казино дают бездепозитный бонус
в каких казино дают бездепозитный бонус
онлайн казино на реальные деньги с бонусом за регистрацию
https://t.me/s/onlajn_kazino_na_realnye_dengi
They have expertise in handling international shipping regulations. https://edpillsotc.store/# best treatment for ed
игровые автоматы с бонусами онлайн
https://t.me/s/pokerdom_igrivieavt
Wonderful article! We are linking to this particularly great post on our website.
Keep up the good writing.
игровые автоматы бонус за регистрацию без депозита
игровые автоматы бонус за регистрацию без депозита
Their global approach ensures unparalleled care. http://doxycyclineotc.store/# where can i get doxycycline over the counter
бонус за регистрацию с моментальным выводом в казино
бонус за регистрацию с моментальным выводом в казино
лучшие онлайн казино с бездепозитным бонусом
https://t.me/s/luchshie_onlajn_kazino_s_bezdepo
бездепозитный бонус в онлайн казино
бездепозитный бонус в онлайн казино
buy zithromax online fast shipping zithromax 500 mg lowest price drugstore online zithromax online usa no prescription
You can definitely see your skills in the work you write.
The arena hopes for even more passionate writers such as you who are not afraid to mention how they believe.
All the time go after your heart.
casino с бездепозитным бонусом
https://t.me/s/CasinoCrownJewel
онлайн казино с бонусом за регистрацию без депозита
онлайн казино с бонусом за регистрацию без депозита
без депозита бонус за регистрацию в казино
https://t.me/s/pokerdom_bezdepositt
казино с депозитом за регистрацию
казино с депозитом за регистрацию
онлайн казино бездепозитный бонус при регистрации
онлайн казино бездепозитный бонус при регистрации
новые онлайн казино с бонусом за регистрацию без депозита
новые онлайн казино с бонусом за регистрацию без депозита
Link exchange is nothing else however it is just
placing the other person’s web site link on your page at proper place and other person will also do similar in favor of you.
бездепозитный бонус с выводом
бездепозитный бонус с выводом
casino бонус за регистрацию
casino бонус за регистрацию
казино с бездепозитным бонусом за регистрацию с выводом
https://t.me/s/kazino_s_bezdepozitnym_bonusom1
казино на деньги бонус без депозита
https://t.me/s/pokerdomna_dengi
онлайн казино с бонус при регистрация
https://t.me/s/CardSharkVirtuosoGuru
Highly descriptive post, I loved that bit. Will there be a
part 2?
бонусы без депозита в казино за регистрацию
бонусы без депозита в казино за регистрацию
игровые автоматы с бонусом за регистрацию без первого депозита
игровые автоматы с бонусом за регистрацию без первого депозита
казино онлайн без депозита бонус за регистрацию
https://t.me/s/casino_bez_deposita
казино с начальным бонусом
казино с начальным бонусом
I trust them with all my medication needs. antibiotics doxycycline: Doxycycline 100mg buy online – doxycycline buy online usa
казино онлайн бонус при регистрации
https://t.me/s/BetBlitzWhisperer
онлайн казино с бонусом без депозита
онлайн казино с бонусом без депозита
игровые автоматы на деньги с бонусом
https://t.me/s/pokerdom_kazinohas
игровые автоматы онлайн с бонусом
игровые автоматы онлайн с бонусом
бонус за регистрацию с выводом казино
бонус за регистрацию с выводом казино
casino igre bez depozita
casino igre bez depozita
казино бонус бездепозитный
https://t.me/s/pokerdomkazinoha_bonus
бонус без депозита за регистрацию в казино
https://t.me/s/CasinoMogulMastermindX
денежный бонус за регистрацию без депозита в казино
денежный бонус за регистрацию без депозита в казино
бездепозитный бонус 2021
бездепозитный бонус 2021
сайты казино с бонусом за регистрацию
https://t.me/s/pokerdomkazino_bonysy
I do not even know how I ended up here, but I thought this post was great.
I do not know who you are but definitely you’re going
to a famous blogger if you aren’t already 😉 Cheers!
бк леон игровые автоматы и слоты
https://t.me/s/slotyiavtomaty_nadengi
онлайн казино бонус при регистрации без депозита
https://t.me/s/CasinoConquerorX
бонусы интернет казино
https://t.me/s/bonusy_internet_kazino
бездепозитные без вейджера
бездепозитные без вейджера
Your means of explaining all in this post is
in fact nice, all be capable of effortlessly
understand it, Thanks a lot.
бонус казино без регистрации
https://t.me/s/pokerdom_bonysregistr
скачать игровые автоматы
https://t.me/s/skachat_igrovieavtomaty
казино з бонусом
https://t.me/s/CasinoCashMogul
бездепозитный бонус казино за регистрацию с выводом
https://t.me/s/bezdepozitnyj_bonus_kazino1
игровые автоматы бесплатно с бонусами без депозита
игровые автоматы бесплатно с бонусами без депозита
бездепозитные бонусы казино онлайн
https://t.me/s/pokerdom_bezdepositnybonysy
игровые автоматы играть бесплатно
игровые автоматы играть бесплатно
бездепозитный бонус
https://t.me/s/bezdepozitnyj_bonus1
автоматы без депозита
автоматы без депозита
Actual trends of drug. https://doxycyclineotc.store/# cheapest doxycycline uk
игровые автоматы
игровые автоматы
Read information now. https://azithromycinotc.store/# buy cheap zithromax online
бездепозитный бонус казино за регистрацию
бездепозитный бонус казино за регистрацию
бонусы без денег в казино
бонусы без денег в казино
казино бездепозитный бонус при регистрации
https://t.me/s/CardSharkChampionn
medicine erectile dysfunction best ed drug what are ed drugs
игровые автоматы демо играть бесплатно и без регистрации
игровые автоматы демо играть бесплатно и без регистрации
игровые автоматы пин-ап
https://t.me/s/igrovyeavtimaty_besplatno
игровые автоматы демо
https://t.me/s/igrovyeavtomaty_demo
kazino bonusi bez depozita
kazino bonusi bez depozita
казино бонуси
казино бонуси
pin up игровые автоматы
https://t.me/s/igroviesloty_igrat
игровые автоматы гаминатор 777 играть бесплатно и без регистрации
игровые автоматы гаминатор 777 играть бесплатно и без регистрации
леон игровые автоматы официальный сайт
https://t.me/s/RouletteRoyaltyPro
This is a topic that’s near to my heart… Take care! Exactly where
are your contact details though?
1win зеркало скачать
1win зеркало скачать
I’m grateful for their around-the-clock service. http://drugsotc.pro/# online pharmacy group
казино с бездепозитным бонусом без отыгрыша
https://t.me/s/bezdeposit_pokerdoms
игровые автоматы демо играть бесплатно
https://t.me/s/igrovieavtomaty_pokerdom
скачать игровые автоматы бесплатно на телефон
https://t.me/s/igrovieavtomaty_namobily
скачать бесплатно игровые автоматы
https://t.me/SlotSorcererMaverick
Their global approach ensures unparalleled care. http://drugsotc.pro/# online pharmacy
казино онлайн бонус без депозита
казино онлайн бонус без депозита
игровые автоматы онлайн
https://t.me/s/igrovieavtomaty_onlain
игровые автоматы играть бесплатно без регистрации и смс онлайн
https://t.me/s/igrovieavtomaty_bezsms
игровые автоматы играть бесплатно без регистрации
https://t.me/s/DiceRollerExpertGambler
They never compromise on quality. http://indianpharmacy.life/# top 10 pharmacies in india
Yes! Finally something about Software.
фрибет казино без депозита
https://t.me/s/BetBillionaireTycoon
игровые автоматы миллионер
https://t.me/s/igrovieavtomaty_millioner
игровые автоматы на деньги
игровые автоматы на деньги
скачать игровые автоматы миллионер
скачать игровые автоматы миллионер
1win зеркало сайта
https://t.me/s/zerkalo_sajta_1win
1win зеркало рабочее
https://t.me/s/zerkalo1win_skachat
игровые автоматы бесплатно
игровые автоматы бесплатно
1win букмекерская контора
1win букмекерская контора
игровые автоматы вулкан
https://t.me/s/CasinoChampionX
игровые автоматы леон на деньги
https://t.me/s/besplatnye_avtomaty
Always attuned to global health needs. http://indianpharmacy.life/# indian pharmacy paypal
зеркало 1win
зеркало 1win
1win официальный сайт войти
https://t.me/s/vojti_1win_oficialnyj_sajt
Good article. I’m dealing with many of these issues as well..
ваучер 1win телеграм
https://t.me/vaucher_1win_telegram
игровые автоматы онлайн бесплатно
https://t.me/s/CasinoCashTycoonAce
игровые автоматы бесплатно без регистрации
игровые автоматы бесплатно без регистрации
ваучеры 1win
ваучеры 1win
1win вход зеркало
https://t.me/s/win_vhod_zerkalo
1win зеркало рабочее на сегодня прямо
1win зеркало рабочее на сегодня прямо
скачать игровые автоматы бесплатно
скачать игровые автоматы бесплатно
игровые автоматы пин ап
https://t.me/s/avtomatykaznio_besplatni
1win ваучер
1win ваучер
1win скачать на андроид
1win скачать на андроид
I always used to read piece of writing in news papers but now as I am a
user of net therefore from now I am using net for posts, thanks to web.
1win зеркало рабочее на сегодня прямо сейчас
1win зеркало рабочее на сегодня прямо сейчас
1win скачать на айфон
1win скачать на айфон
1win рабочее зеркало
1win рабочее зеркало
1win зеркало рабочее на сегодня
https://t.me/s/win_zerkalo_rabochee_na_segodnya
бесплатные игровые автоматы
бесплатные игровые автоматы
скачать приложение 1win
https://t.me/s/skachat_prilozhenie_1win
игровые автоматы бесплатно и без регистрации
игровые автоматы бесплатно и без регистрации
Their health seminars are always enlightening. https://mexicanpharmacy.site/# mexico drug stores pharmacies
1win casino
1win casino
Terrific post however , I was wanting to know if you could
write a litte more on this subject? I’d be very thankful if you could elaborate a little bit further.
Cheers!
1win скачать android
https://t.me/s/skachat_naandroid1win
bookmarked!!, I liкe уouг site!
Have a look at mү webpage :: interior design advice;
Inez,
1win официальный сайт зеркало
1win официальный сайт зеркало
бк леон игровые автоматы и слоты скачать
https://t.me/s/BetBillionaireMastermind
игровые автоматы играть бесплатно и без регистрации
игровые автоматы играть бесплатно и без регистрации
1win бк
1win бк
Providing global access to life-saving medications. https://drugsotc.pro/# mexican online mail order pharmacy
скачать 1win на андроид с официального сайта
https://t.me/s/skachat_1win_na_android_s_oficia
1win фрибет
https://t.me/s/win_fribet
1win вывод средств
https://t.me/s/win_vyvod_sredstv
1win зеркало скачать на андроид
https://t.me/s/win_zerkalo_skachatna_android
canada pharmacy world us online pharmacy canadian world pharmacy
1win bet
1win bet
скачать 1win на айфон
скачать 1win на айфон
1win poker
https://t.me/s/win1_poker
1win ссылка
https://t.me/s/win_ssylka
hey there and thank you for your information – I have definitely picked up anything new from
right here. I did however expertise several technical points using this website, as I
experienced to reload the website lots of times previous to I
could get it to load properly. I had been wondering if your web host is OK?
Not that I am complaining, but sluggish loading instances times will often affect your placement in google and could damage your quality score if advertising and marketing with Adwords.
Anyway I’m adding this RSS to my e-mail and can look out for
a lot more of your respective interesting content.
Make sure you update this again very soon.
1win приложение
https://t.me/s/win1_prilozhenie
1win ввести промокод
1win ввести промокод
Tremendous issues here. I am very satisfied to look your post.
Thanks so much and I am looking ahead to contact you.
Will you kindly drop me a mail?
промокоды 1win
https://t.me/s/promokody_1win1
1win kz
https://t.me/s/win11_kz
1win сайт вход
https://t.me/s/win_sajt_vhod
ваучер 1win
https://t.me/s/vaucheraa_1win
1win скачать последнюю версию
1win скачать последнюю версию
1win онлайн
1win онлайн
1win войти
1win войти
1win официальный скачать
1win официальный скачать
1win скачать
1win скачать
1win промокод на деньги
1win промокод на деньги
1win ставки
1win ставки
ваучер на 1win
ваучер на 1win
1win официальный
1win официальный
1win официальный сайт скачать на андроид
1win официальный сайт скачать на андроид
1win покер
https://t.me/s/win_poker1
1win партнерка
https://t.me/s/onewin_partnerka
Their global presence ensures prompt medication deliveries. http://mexicanpharmacy.site/# buying prescription drugs in mexico
I love what you guys are up too. This sort of clever work and
exposure! Keep up the superb works guys I’ve added you guys to blogroll.
Hello all, here every person is sharing these experience, therefore it’s pleasant to read this blog, and I used to visit this web
site all the time.
1win слоты
1win слоты
как удалить аккаунт 1win
https://t.me/s/WinningProsperaCasino
1win официальный вход
https://t.me/s/win_oficialnyj_vhod1
скачать 1win на андроид
https://t.me/s/skachat_na_android_tut
Always up-to-date with the latest healthcare trends. https://indianpharmacy.life/# Online medicine order
Tһiѕ post is invaluable. Hoԝ can Ifind ⲟut
more?
mү blog post … 77store cc
Good day! This post could not be written any better!
Reading through this post reminds me of my good old room mate!
He always kept chatting about this. I will forward this write-up to him.
Fairly certain he will have a good read. Thanks for sharing!
1win скачать на андроид бесплатно
1win скачать на андроид бесплатно
1win мобильное приложение
1win мобильное приложение
1win кс го
1win кс го
1win сайт
1win сайт
They never compromise on quality. http://drugsotc.pro/# online pharmacy no prescription needed
1win официальный скачать на андроид
1win официальный скачать на андроид
1win aviator
https://t.me/s/one_win_aviator1
скачать 1win официальный сайт
скачать 1win официальный сайт
1win официальный сайт вход
1win официальный сайт вход
1win казино скачать
https://t.me/s/win_kazino_skachat
1win официальный сайт скачать
1win официальный сайт скачать
1win на айфон
https://t.me/s/win_na_iphone
Hi there all, here every one is sharing these kinds of experience, so it’s good
to read this web site, and I used to pay a quick
visit this web site everyday.
промокод на 1win
промокод на 1win
1win бонусы казино
1win бонусы казино
It’s nearly impossible to find educated people about this topic,
but you seem like you know what you’re talking about!
Thanks
1win вход
https://t.me/s/RollTheDiceElite
Thank you a bunch for sharing this with all folks you actually know what you’re talking
approximately! Bookmarked. Kindly additionally talk over
with my website =). We will have a hyperlink trade agreement among us
1win официальное зеркало
https://t.me/s/oficialnoe_zerkalo1win
1win на андроид
https://t.me/s/win_na_android
скачать 1win с официального сайта
скачать 1win с официального сайта
промокод 1win
https://t.me/s/prommokody_1win
1win promo code
https://t.me/s/promo_code_1win
Their free health check-ups are a wonderful initiative. http://drugsotc.pro/# canada drug pharmacy
1win lucky jet
1win lucky jet
1win официальный сайт скачать на андроид бесплатно
https://t.me/s/sajt_skachat_na_android_besplatn
1win partners
1win partners
1win букмекерская контора официальный сайт
1win букмекерская контора официальный сайт
I was recommended this website by means of my cousin.
I am no longer sure whether or not this post is
written through him as nobody else understand such unique approximately my problem.
You’re wonderful! Thanks!
1win партнерская программа
https://t.me/s/partnerskaya_programma23
This is the perfect webpage for everyone who would like to understand this topic.
You realize so much its almost hard to argue with
you (not that I really would want to…HaHa). You definitely put a brand new spin on a subject that’s been written about for a long time.
Excellent stuff, just excellent!
лаки джет 1win
лаки джет 1win
1win казино
1win казино
как использовать бонусы на спорт в 1win
как использовать бонусы на спорт в 1win
1win бк зеркало
https://t.me/s/win_bk_zerkalo
1win online
1win online
как использовать бонусы в 1win
как использовать бонусы в 1win
промокоды на 1win
https://t.me/s/promokody_na_1win
lucky jet 1win
https://t.me/s/lucky_jet_11win11
1win актуальное зеркало
1win актуальное зеркало
как использовать бонусы казино в 1win
https://t.me/s/ispolzovat_bonusy_kazino_v_1win
1win официальный мобильная версия
https://t.me/s/oficialnyj_mobilnaya_versiya
промокод при регистрации 1win
https://t.me/s/promokod_pri_registracii_1win
1win регистрация
https://t.me/s/LuckyBetHub
Bitcoin halving occurs approximately every four years, where the rewards given to Bitcoin miners for mining blocks are cut in half. Halving was built into the Bitcoin protocol to maintain its value as a deflationary currency. By reducing the amount of new bitcoins, the protocol aims to prevent the devaluation of Bitcoin over time, which often happens with inflationary currencies. Despite inflows of $158 million year-to-date, last week Bitcoin saw an increase in money leaving the asset, according to a note from digital investment and trading group CoinShares. There were about $25 million in Bitcoin outflows, the highest among top cryptocurrencies, along with $3.7 million in inflows to investment products meant to short it—or bet on it losing value.
https://telegra.ph/crypto-com-purchase-fees-08-27
Seeking Alpha’s Disclosure: Past performance is no guarantee of future results. No recommendation or advice is being given as to whether any investment is suitable for a particular investor. Any views or opinions expressed above may not reflect those of Seeking Alpha as a whole. Seeking Alpha is not a licensed securities dealer, broker or US investment adviser or investment bank. Our analysts are third party authors that include both professional investors and individual investors who may not be licensed or certified by any institute or regulatory body. You’ll hear that “bitcoin” is a currency, so it is left uncapitalized, like dollars, yen, euros, krona. But “Bitcoin” is the formal name of the network — thus, it needs that proper noun capitalization. Market capitalization refers to the market value of a company’s equity. It is a simple but important measure that is calculated by multiplying a company’s shares outstanding by its price per share. For example, a company priced at $20 per share and with 100 million shares outstanding would have a market capitalization of $2 billion.
Hi there, after reading this remarkable piece of
writing i am too happy to share my knowledge here with
friends.
1win букмекерская
https://t.me/s/bykmekerskaja_1win
1win вход в личный кабинет
https://t.me/s/vhod_v_lichnyj_kabinet1win
luckyjet 1win
luckyjet 1win
Unquestionably believe that which you stated.
Your favorite reason appeared to be on the net the
easiest thing to be aware of. I say to you, I definitely get annoyed while people
consider worries that they plainly do not know about.
You managed to hit the nail upon the top and also defined out the whole thing without having side-effects
, people could take a signal. Will probably be back to get
more. Thanks
бонусы спорт 1win
бонусы спорт 1win
1win мобильная версия
1win мобильная версия
1win промокод
https://t.me/s/luchiepromokody_1win
казино 1win
https://t.me/s/kazino_1winkazino
скачать бесплатно 1win
https://t.me/s/skachat_besplatno_1win
бонусы казино 1win
бонусы казино 1win
The staff exudes professionalism and care. http://indianpharmacy.life/# india pharmacy mail order
1win download
https://t.me/s/onewin_download
1win казино зеркало
1win казино зеркало
Their medication therapy management is top-notch. http://indianpharmacy.life/# best india pharmacy
Cool blog! Is your theme custom made or did you download it
from somewhere? A design like yours with a few simple tweeks
would really make my blog shine. Please let me know
where you got your theme. Cheers
1win games
1win games
1win автоматы официальный сайт
https://t.me/s/sajt_1win_avtomaty_oficialnyj
online pharmacy without scripts canadian mail order pharmacy pharmacy near me
бк 1win
https://t.me/s/bk_1wiinn
1win рабочее на сегодня зеркало прямо сейчас
1win рабочее на сегодня зеркало прямо сейчас
1win официальный сайт
1win официальный сайт
1win csgo
https://t.me/s/csgo_1win_csgo
1win промокод для бонуса
1win промокод для бонуса
aviator 1win
aviator 1win
1win скачать на ios
1win скачать на ios
1win скачать ios
1win скачать ios
1win partner
https://t.me/s/casino_1winpartner
Hello, I enjoy reading through your article post.
I wanted to write a little comment to support you.
1win бонус 5000 как использовать
1win бонус 5000 как использовать
1win промокод без депозита
https://t.me/s/promokod_bez_depozita_1win
как использовать бонусы 1win
https://t.me/s/LuckyOasisRealm
скачать 1win
https://t.me/s/HighStakesHaven
1win apk
1win apk
1win зеркало на сегодня
1win зеркало на сегодня
After I initially commented I seem to have clicked the -Notify me
when new comments are added- checkbox and from now on every time a
comment is added I recieve 4 emails with
the same comment. Is there a means you can remove me
from that service? Appreciate it!
промокод 1win и промокод олимп
промокод 1win и промокод олимп
lucky jet игра 1win
lucky jet игра 1win
1win cs go
https://t.me/s/csgoo_1win
Everyone loves it when people come together and share thoughts.
Great website, stick with it!
букмекер 1win
букмекер 1win
1win ставки онлайн
1win ставки онлайн
бонусы 1win
https://t.me/s/LuckyCharmPalace
1win бонусы казино как использовать
1win бонусы казино как использовать
Professional, courteous, and attentive – every time. https://drugsotc.pro/# cost less pharmacy
1win контора
https://t.me/s/onewin_kontora
1win зеркало
https://t.me/s/CasinoMastersClub
как потратить бонусы казино 1win
https://t.me/s/kak_potratit_bonusy_kazino
1win бонус
1win бонус
1win ios
https://t.me/s/onewin_ios
1win отзывы
https://t.me/s/CardSharkSecrets
как поставить бонусы в 1win
https://t.me/s/kak_postavit_bonusy
1win бонусы
1win бонусы
как использовать бонусный счет 1win
как использовать бонусный счет 1win
jet best big win strategy jet winning jet 1win
https://t.me/s/win_strategy_jet_winning
1win бонус за регистрацию
1win бонус за регистрацию
1win zerkalo
1win zerkalo
1win бездепозитный бонус
1win бездепозитный бонус
1win bonus
1win bonus
1win авиатор
https://t.me/s/avviatorr_1win
как играть на бонусы в 1win
как играть на бонусы в 1win
Wonderful goods from you, man. I have understand your stuff
previous to and you are just too fantastic. I really like what you have acquired here, certainly like what you’re stating and the way in which you say it.
You make it entertaining and you still take care
of to keep it wise. I can not wait to read much more from you.
This is really a great website.
как удалить аккаунт в 1win
https://t.me/s/WagerWinningZone
1win букмекерская контора официальный
1win букмекерская контора официальный
They offer great recommendations on vitamins. https://indianpharmacy.life/# buy prescription drugs from india
авиатор 1win
авиатор 1win
1win регистрация на сайте
https://t.me/s/CashFlowCascade
1win как использовать бонус казино
https://t.me/s/TreasureThrive
Their medication therapy management is top-notch. http://mexicanpharmacy.site/# mexican mail order pharmacies
1win мобильное
https://t.me/s/mobilnoe_1win
бонусы казино 1win как использовать
https://t.me/s/bonusy_kazino_1win_kak_ispolzova
1win официальное зеркало на сегодня
1win официальное зеркало на сегодня
lucky jet 1win отзывы
lucky jet 1win отзывы
mexican pharmacy what to buy mexican pharmacy online canadian pharmacy world coupon
зарегистрироваться 1win
https://t.me/s/zaregistrirovatsia_v1win
Global expertise that’s palpable with every service. http://drugsotc.pro/# no prescription needed canadian pharmacy
1win зеркало сейчас
1win зеркало сейчас
1win букмекерская контора зеркало
https://t.me/s/BetBlitzHub
1win.
1win.
как вывести деньги с 1win
https://t.me/s/kak_vyvesti_dengi_s_1win
This paragraph gives clear idea for the new users
of blogging, that actually how to do running a blog.
1win скачать apk
1win скачать apk
I think the admin of this site is genuinely working hard for his
web site, for the reason that here every stuff is quality based material.
I appreciate their late hours for those unexpected needs. https://drugsotc.pro/# rx pharmacy
jet best big win strategy jet tricks jet 1win
https://t.me/s/RollingInRichesCasino
aviator игра 1win
https://t.me/s/AceOfSpinsClubAceOfSpinsClub
бонусы спорт 1win как использовать
https://t.me/s/bonusy_sport_1win_kak_ispolzovat
Hello everyone, it’s my first pay a visit at this website,
and paragraph is truly fruitful designed
for me, keep up posting these posts.
казино 1win официальный
https://t.me/s/win_oficialnyj23
1win россия
1win россия
1win официальный сайт регистрация
https://t.me/s/RegalRiskGaming
1вин зеркало рабочее
https://t.me/s/zerkalo_1vin_rabochee
1win com
https://t.me/s/win_com_win_com
как использовать бонусы 1win казино
https://t.me/s/kak_ispolzovat_bonusy_1win
coba join kedalam laman judi pkv games dengan bandar domino
serta bandarq online terbaik sepanjang masa yamg telah tersedia pada tahun 2023 ini dengan akun рro jackpot terbaik
yang bisa kalian dapatkan dengan menggunakan sebagian akun yang kalian daftarkan dii dalam
sini ɗan kalian juga bisa mempunyai kemungkinan untuk mendapatkan semua keuntungan dari metode pengisian deposit νia pulsa yang tidak bisa kalian temukan ddi
website website judi pkv games,
bandarqq maupun pokerqq online yang lainnya yang ada ⅾi dunia maya saat ini.
1win букмекерская скачать на айфон
1win букмекерская скачать на айфон
зеркало 1вин
зеркало 1вин
1win официальный сайт бесплатно
https://t.me/s/RegalFlushGaming
1win casino скачать
https://t.me/s/win_casino_skachat
1win приложение андроид
1win приложение андроид
1win ставки зеркало
1win ставки зеркало
1win букмекерская скачать
https://t.me/s/win_bukmekerskaya_skachat
canadian rx prescription drugstore: online pharmacies no prescription usa – buy drugs online without prescription
1win ставки приложение
1win ставки приложение
1win aviator играть
1win aviator играть
“букмекерская контора 1win” ограничивает
“букмекерская контора 1win” ограничивает
1win top
https://t.me/s/top_1winn
neurontin 100mg tab: generic neurontin cost – buy generic neurontin
скачать 1win ставки
https://t.me/s/skachat_1win_stavki
1вин зеркало
1вин зеркало
canadian pharmacy no scripts canadian pharmacy world canadian online drugs
“букмекерская контора 1win” ограничивает
https://t.me/s/NirvanaCasinoWorld
1win ставки скачать на андроид
1win ставки скачать на андроид
Amazing blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple adjustements would really make my blog jump out.
Please let me know where you got your theme. Many thanks
1win рулетка
1win рулетка
как использовать бонус в 1win
как использовать бонус в 1win
1win промокоды
https://t.me/s/win_promokody
1win рабочее на сегодня
https://t.me/s/rabocheenasegodnia_1win
1вин скачать
1вин скачать
1win куда вводить промокод
1win куда вводить промокод
1win poker скачать
1win poker скачать
1win промокод бонус за регистрацию
https://t.me/s/promokod1win_bonus_za_registrac
1вин сайт
1вин сайт
Yes! Finally something about pussy xxx.
бонусный счет 1win
бонусный счет 1win
1win partners вход
1win partners вход
1win мобильное приложение скачать на андроид
https://t.me/s/win_mobilnoe_prilozhenie_skachat
1вин официальный сайт
https://t.me/s/vin_oficialnyj_sajt
canada drugs online review: certified canada pharmacy online – best canadian online pharmacy reviews
1win как использовать бонус
1win как использовать бонус
партнерская программа 1win
партнерская программа 1win
1win игровые автоматы
https://t.me/s/win_igrovye_avtomaty
скачать 1вин на андроид
скачать 1вин на андроид
промокод 1win при регистрации
промокод 1win при регистрации
отзывы 1win
отзывы 1win
1win coin
1win coin
1вин скачать на андроид
1вин скачать на андроид
Dаftar 15 Gamme Tergacor yajg Tеrsedia ddi Slot888
Slot888 Rіise oof Gizaa PowеrNudge
Slot888 Sweet Bonanza Xmas
Slot888 Sugar Rush
Slot888 Nine Tails
Slot888 Hey Sushi
Ѕlot888 Candy Tower
Slot888 5 Lucky Lіons
Slot888 Wiild Wet Win
Slot888 Ruby Hood
Slot888 Magic Кitty
Slot888 Lucјy Panda
Slot888 Fa Fa Mоnkey
Slot888 Spin Dinner
Inii ialah daftar 15 ame teraik yang ada dii Slot888 yang mesti kalian coba.
Semoga mnjadi maxwin bagi kalian yng mencobanya ^^
Permainan sllot di atas mеmpunyɑi karakteristik-karakteristik tertenu yazng membikin merdka
menjsdi oρs popuⅼer ddi kalanhan pemain slоt online.
Slot888 Sսgаr Ɍush, contohnya, menawаrksn figur putaгan cᥙma-cuma yag bbisa memicu kemenangan besar,
ssementara Slot888 Nine Tails menuediɑkan sampai 300.704 metode untᥙk menang dalam tiap-tiaρ putaran.
1win игры
1win игры
официальный сайт 1win
https://t.me/s/oficialnyj_sajt_1win1
neurontin 300 600 mg: neurontin 400 – neurontin 30 mg
1win букмекерская на андроид
1win букмекерская на андроид
скачать 1вин
https://t.me/s/skachat_1vin1
jet best big win strategy jet winning tricks jet 1win
https://t.me/s/GambleVistaHub
1win официальное приложение
https://t.me/s/oficialnoe_prilogenie_1win
сайт 1вин
сайт 1вин
1win бонусы спорт как пользоваться
1win бонусы спорт как пользоваться
1win как использовать бонусы
1win как использовать бонусы
Their prices are unbeatable! https://gabapentin.world/# neurontin drug
1win мобильное приложение скачать бесплатно
https://t.me/s/mobilnoe_prilozhenie_1win
1вин регистрация
https://t.me/s/registraciya_1vin
1win ставки на спорт зеркало
https://t.me/stavki_na_sport_zerkalo1win
canadian pharmacy ltd: cheap drugs from canada – canadian mail order pharmacy
1win букмекерская контора сайт
https://t.me/s/FortuneVoyage
1win login
https://t.me/s/login_1win
1вин рабочее зеркало
https://t.me/s/rabochee_1vin_zerkalo
1win ставка
https://t.me/s/stavka_1winstavka
1win сайт скачать
https://t.me/s/DiceRollingParadise
как потратить бонусы казино в 1win
как потратить бонусы казино в 1win
buy gabapentin canada where to buy neurontin neurontin 800 mg cost
промокод 1вин
промокод 1вин
состав 1win
https://t.me/s/sostav_1win
1win команда
https://t.me/s/CometCasinoEuphoria
как отыграть бонус в 1win
как отыграть бонус в 1win
1вин приложение скачать андроид
https://t.me/s/prilozhenie1vin_skachat_android
скачать приложение 1win на андроид бесплатно
скачать приложение 1win на андроид бесплатно
бонус казино 1win
https://t.me/s/Chancetopia
jet best big win jet winning tricks jet 1win
jet best big win jet winning tricks jet 1win
1вин приложение
https://t.me/s/prilozhenie1vin
1win скачать приложение
1win скачать приложение
скачать 1win на телефон
скачать 1win на телефон
игра авиатор 1win
https://t.me/s/igra_aviattor_1win
1вин партнерка
1вин партнерка
When some one searches for his necessary thing, therefore he/she needs to be
available that in detail, so that thing is maintained over here.
скачать 1win зеркало
скачать 1win зеркало
партнерка 1win
партнерка 1win
neurontin 600 mg coupon: neurontin discount – neurontin drug
егор васильев 1win
https://t.me/s/egorvasilyev_1win
1вин отзывы
https://t.me/s/otzyvy1vin
I was wondering if you ever considered changing the page layout of your blog?
Its very well written; I love what youve got to
say. But maybe you could a little more in the way of content so people could connect with it better.
Youve got an awful lot of text for only having
one or 2 pictures. Maybe you could space it out better?
1win скачать на телефон андроид
https://t.me/s/skachat1win_na_telefon_android
jet big win strategy jet winning tricks jet 1win
jet big win strategy jet winning tricks jet 1win
online canadian pharmacys: mexican pharmacy without prescription – legit canadian pharmacy sites
deko 1win
deko 1win
лаки джет 1вин
https://t.me/s/laki_dzhet_1vin
Jogo no cassino da Mostbet Brasil há cerca de quatro anos.
1win скачать на андроид последняя версия
1win скачать на андроид последняя версия
1win официальный сайт вход в личный кабинет
1win официальный сайт вход в личный кабинет
1win букмекерская контора скачать на андроид
https://t.me/s/bukmekerskaya_kontora1win_skacha
казино 1вин
казино 1вин
1win run
https://t.me/s/AceQuestCasino
1win site
1win site
Neat blog! Is your theme custom made or did you
download it from somewhere? A theme like yours with a few simple adjustements would really make my blog shine.
Please let me know where you got your design. Cheers
1win букмекерская контора мобильная версия
https://t.me/s/bukmekerskaja_kontoramobilna1win
промокод для 1win
https://t.me/s/promokod_dlya_1win
сайт 1win
https://t.me/s/AceOfBetsFortune
1вин казино
https://t.me/s/kazino1vin
1win букмекерская контора приложение
https://t.me/s/bukmekerskajakontora_1win
1вин зеркала на сегодня
1вин зеркала на сегодня
официальный сайт конторы 1win
официальный сайт конторы 1win
бонус промокод 1win
https://t.me/s/bonus_promokod_1win
best online pharmacies in mexico mexican pharmacy online mexican drugstore online
бк 1вин
https://t.me/s/bk_1vin_bk_1vin
1win скачать зеркало
https://t.me/s/skachat_zerkalo1win
1вин ставки
https://t.me/s/sstavki_1win
1win официальный сайт игровые автоматы
https://t.me/s/oficialnyj_sajt_1win_igrovye_avt
бк 1win скачать
https://t.me/s/bk_1win_skachat
скачать приложение 1win на андроид
скачать приложение 1win на андроид
1вин бк
https://t.me/s/bk1vin
1вин скачать программа
1вин скачать программа
1win не выводит деньги
1win не выводит деньги
1win bet зеркало
https://t.me/s/bet_zerkalo_1win
скачать 1win на андроид бесплатно с официального
https://t.me/s/skachat1win_naandroid_besplatnos
1вин бет зеркало
https://t.me/s/bet1vin_zerkalo
1вин скачать официальное приложение
1вин скачать официальное приложение
1win apk android
https://t.me/s/apkandroid_1win
личный кабинет 1win
https://t.me/s/lichnyj_kabinet1win
рабочее зеркало 1win
https://t.me/s/rabocheezzerkalo_1win
mexican drugstore online or medicines mexico – buying prescription drugs in mexico online
Awesome blog! Do you have any recommendations for aspiring
writers? I’m planning to start my own website soon but I’m a little lost on everything.
Would you recommend starting with a free platform like WordPress or go for a paid option? There are so many
options out there that I’m totally confused ..
Any suggestions? Bless you!
1вин бет
https://t.me/s/bet1vin_bet
скачать бесплатно 1вин
https://t.me/s/skachat_bespllatno_1win
1вин зеркала на сегодня скачать
1вин зеркала на сегодня скачать
1win приложение ios
1win приложение ios
1win казино регистрация
https://t.me/s/kazino1win_registraciya
1вин авиатор
1вин авиатор
скачать 1вин на телефон официальный сайт
https://t.me/s/skachat1win_natelefonofilialnyj
plinko 1win
https://t.me/s/plinko_1win1
1вин приложение официальный сайт online
1вин приложение официальный сайт online
1win как вывести деньги
https://t.me/s/kak_vyvesti_dengi1win
авиатор 1вин
https://t.me/s/aviator1vin_1vin
1win официальный сайт букмекерской конторы
https://t.me/s/oficialsaitbykmekerskoi_kont1win
1вин онлайн казино
1вин онлайн казино
как потратить бонусы в 1win
как потратить бонусы в 1win
1win на спорт
1win на спорт
сайт casino x
https://t.me/s/sait_casinox
1win на телефон
1win на телефон
ваучер 1вин
ваучер 1вин
как пополнить 1win
https://t.me/s/kak_popolnit_1win
lucky jet 1win скачать
lucky jet 1win скачать
промокод casino x
https://t.me/s/promokod_casinox
скачать 1вин на андроид бесплатно
https://t.me/s/skachat1win_naandroid_besplatno
рабочее зеркало 1вин
рабочее зеркало 1вин
1win команда кс
1win команда кс
как играть на бонусы казино в 1win
как играть на бонусы казино в 1win
отзывы casino x
отзывы casino x
скачать 1вин на андроид с официального
скачать 1вин на андроид с официального
1win казино официальный сайт
https://t.me/s/kazino_oficialny
проверяем слоты и бонусы 1вин
https://t.me/s/proveryaem_sloty_i_bonusy_1vin
как активировать бонусы 1win
как активировать бонусы 1win
jeu jet x casino
jeu jet x casino
Your style is so unique in comparison to other folks I’ve read stuff from.
Thanks for posting when you have the opportunity,
Guess I will just book mark this site.
скачать 1вин на айфон
https://t.me/s/skachat_1vin_na_ajfon
как потратить бонусы 1win
https://t.me/s/kak_potratit_bonusy_1win
проверяем слоты и 1вин бонус
проверяем слоты и 1вин бонус
Saved as a favorite, I really like your web site!
1win играть
https://t.me/s/igrat1win_1win
jet x casino en ligne
jet x casino en ligne
1вин скачать мобильный телефон
1вин скачать мобильный телефон
1win как поставить бонус
https://t.me/s/kak_postavitbonus1win
mexican online pharmacies prescription drugs mexican pharmacies mexico drug stores pharmacies
популярное 1вин слоты промокод 2022
популярное 1вин слоты промокод 2022
игровые автоматы casino x демо
игровые автоматы casino x демо
1win как получить бонус
1win как получить бонус
1вин скачать мобильная версия
https://t.me/s/skachat_1vin_mobilnaya_versiya
purple pharmacy mexico price list : medicine in mexico pharmacies – medicine in mexico pharmacies
Everyone loves it when people come together and share views.
Great site, keep it up!
1вин бонус
https://t.me/s/one_vin_bonus
1win игра
1win игра
1 x slots casino
1 x slots casino
medication from mexico pharmacy : mail order pharmacy mexico – mexican drugstore online
get x casino
get x casino
1вин сайт официальный
1вин сайт официальный
зеркало casino x
зеркало casino x
porn stars
1win букмекерская скачать приложение
1win букмекерская скачать приложение
x casino зеркало
x casino зеркало
casino x зеркало мобильная
casino x зеркало мобильная
регистрация 1вин
регистрация 1вин
1win букмекерская контора бонусы
1win букмекерская контора бонусы
up x casino
https://t.me/s/up_casinox
x-casino
https://t.me/s/xcasino_xcasino
casino x вывод денег
casino x вывод денег
1вин проверка авто
1вин проверка авто
1win букмекерская компания
https://t.me/s/bukmekkerskaia_kompania1win
игровые автоматы casino x
https://t.me/s/igrovye_avtomaty_casinox
casino x войти
https://t.me/s/casinox_vojti
up-x casino
up-x casino
1вин программа
1вин программа
1win букмекерская контора скачать
1win букмекерская контора скачать
casino x зеркало сегодня
https://t.me/s/casinox_zerkalo_segodnya
x casino телеграм отзывы
x casino телеграм отзывы
регистрация casino x
регистрация casino x
1вин приложение скачать андроид бесплатно
https://t.me/s/prilozhenie_1vin_skachat_android
1win бонусы спорт
1win бонусы спорт
casino x зеркало
https://t.me/s/casinox_zerkaloo
скачать casino x на компьютер
https://t.me/s/casinox_skachatna_kompiuter
официальный сайт casino x регистрация и вход
официальный сайт casino x регистрация и вход
Hello there! This blog post couldn’t be written much better!
Going through this article reminds me of my previous roommate!
He continually kept talking about this. I’ll forward this information to
him. Pretty sure he’s going to have a very good read.
Thank you for sharing!
1вин приложение официальный сайт
https://t.me/s/prilozhenie1vin_oficialnyj_sajt
бонусы на спорт 1win
бонусы на спорт 1win
casino x зеркало на сегодня
https://t.me/s/casinox_zerkalo_nasegodnia
casino x приложение
casino x приложение
обзор онлайн casino x
обзор онлайн casino x
1win betting
https://t.me/s/bettting_1win
1вин онлайн
https://t.me/s/onlinee_1win
medicine in mexico pharmacies : mexico pharmacy price list – medicine in mexico pharmacies
Everything published made a lot of sense. However,
think on this, what if you typed a catchier title?
I mean, I don’t wish to tell you how to run your website, however what if
you added a post title that makes people want more?
I mean Think Obstructive Sleep Apnea is #NBD? Here Are Seven Health Conditions
Made Worse By Your Undiagnosed OSA – Delaware Dental
Sleep Medicine is kinda plain. You should glance at Yahoo’s front
page and note how they create post headlines to grab people to click.
You might add a related video or a picture or two to grab people interested about everything’ve written. In my opinion, it would
bring your website a little livelier.
mexico pharmacy mexico pharmacy online buying from online mexican pharmacy
casino x зеркало 2023
https://t.me/s/casinox_zerkalo_2023
casino x полная версия
casino x полная версия
обзор casino x
обзор casino x
актуальное зеркало бк 1win
актуальное зеркало бк 1win
1вин официальное зеркало на сегодня
1вин официальное зеркало на сегодня
casino x зеркало 2022
casino x зеркало 2022
1вин зеркала скачать
https://t.me/s/zerkala1win_skachat
x casino онлайн
https://t.me/s/casinox_online
mister x casino
https://t.me/s/mister_xcasino
1вин официальное зеркало
https://t.me/s/oficialnoe_zerkalo1vin
casino-x зеркало
casino-x зеркало
casino x онлайн казино
https://t.me/s/casinox_onlajn_kazino
казино casino x
https://t.me/s/kazino_casinox
1вин официальное приложение
1вин официальное приложение
1вин войти
https://t.me/s/vojti_1vin
casino x вход
casino x вход
casino-x официальный сайт
https://t.me/s/casinox_oficialnyj_sait
jet x casino
https://t.me/s/jet_xcasino
1вин мобильная версия
1вин мобильная версия
1вин телефон андроид
https://t.me/s/telefon_android_1win
casino x скачать
https://t.me/s/casinox_skachat
casino x official
https://t.me/s/casino_x_officialcasino
casino x зеркало рабочее
casino x зеркало рабочее
1вин лаки джет
1вин лаки джет
1вин телефон мобильная версия
1вин телефон мобильная версия
casino x рабочее зеркало
https://t.me/s/casinox_raabocheezerkalo
casino x мобильная версия зеркало сайта
casino x мобильная версия зеркало сайта
casino-x зарегистрироваться зеркало
https://t.me/s/casinox_zaregistrirovatsya_zerk
1вин как скачать
1вин как скачать
1вин телефон мобильный телефон
1вин телефон мобильный телефон
Wow, incredible blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your website is magnificent, as
well as the content!
casino x отзывы
casino x отзывы
casino x скачать на андроид
casino x скачать на андроид
1вин скачать телефон
https://t.me/s/skschat_1win_telefon
buy stromectol canada: stromectol order online – minocycline 50mg online
casino x официальный сайт скачать
casino x официальный сайт скачать
casino x мобильная версия скачать
https://t.me/s/casinox_mobilnaya_versiya_skacha
casino x сегодня
https://t.me/s/casinox_segodnya
1вин бет скачать на андроид бесплатно
https://t.me/s/bet1vin_skachat_na_android_bespl
скачать бесплатно сайт ставок на спорт 1вин
скачать бесплатно сайт ставок на спорт 1вин
casino x официальный сайт
casino x официальный сайт
casino x мобильная версия зеркало
casino x мобильная версия зеркало
casino x сайт
casino x сайт
1вин бет скачать на андроид
1вин бет скачать на андроид
1вин скачать мобильный
https://t.me/s/skachat_mobilnyj1vin
casino x mirror
casino x mirror
mail order pharmacy india best online pharmacy india pharmacy website india
casino x регистрация
casino x регистрация
1вин скачать приложение
1вин скачать приложение
1вин бет скачать
https://t.me/s/bet1vin_skachat
casino x лицензия
https://t.me/s/casinox_licenzija
https://canadapharmacy24.pro/# best canadian pharmacy to order from
casino x – free online slots
casino x – free online slots
1вин скачать андроид
1вин скачать андроид
casino x промокод
casino x промокод
1вин бет официальный сайт
https://t.me/s/bet1vin_oficialnyj_sajt
casino x – free online slots отзывы
casino x – free online slots отзывы
1вин сайт официальный скачать
1вин сайт официальный скачать
casino-x
https://t.me/s/casinox_casinoxx
casino x online
https://t.me/s/casino_x_online
1вин промокод
1вин промокод
casino x доступное зеркало
casino x доступное зеркало
Quality articles or reviews is the crucial to be a focus for the visitors
to visit the site, that’s what this website is providing.
1вин сайт официальный скачать бесплатно
https://t.me/s/sait_oficialnyi_1win_skachatbesp
x casino
x casino
casino x официальный
casino x официальный
play casino x
https://t.me/s/play_casinox
casino x com зеркало
casino x com зеркало
When someone writes an article he/she retains the plan of a
user in his/her mind that how a user can understand it.
Thus that’s why this paragraph is perfect. Thanks!
1вин промокод 2022
https://t.me/s/promokod1win_2022
Здравствуйте поклонники финской сауны!
Рассматривали возможность ли вы о способами правильно регулировать температуру и уровень влажности в вашей финской сауне? Именно это не просто вопрос комфорта, но и основа к хорошему самочувствию.
Чтобы получить максимальное удовольствие и пользу от процедуры, очень важно иметь представление о оптимальных параметрах. Посоветовал бы ознакомиться интересной статьей на тему правильной установки температуры и уровня влажности на сайте ostov-nf.ru.
Уверен, что с этим гидом ваша процедура в сауне станет гораздо удивительной. Используйте знаниями, рассказывайте с опытом и наслаждайтесь каждой минуты!
Замечательного отдыха в сауне!
casino x бонус код
https://t.me/s/casinox_bonus_kod
ivermectin generic cream: stromectol order online – stromectol generic
casino x официальный сайт зеркало
casino x официальный сайт зеркало
х проверка лицензии и бонусов casino x х промокод
https://t.me/s/x_proverka_licenzii_i_bonusov_ca
1вин приложение вход
1вин приложение вход
casino x бонус за регистрацию
https://t.me/s/casinox_bonuszaregistraciy
I want to to thank you for this good read!!
I absolutely loved every bit of it. I have you saved as a favorite to check out new
things you post…
casino x
https://t.me/s/casino_casinox
casino x мобильная версия
casino x мобильная версия
х проверка лицензии и бонусов casino x обзор х
https://t.me/s/x_proverka_licenzii_i_bonusov
1вин приложение скачать
https://t.me/s/prilozhenie_1win_skachat
casino x бездепозитный бонус
casino x бездепозитный бонус
вся правда о casino x тест и обзор x x 2021
https://t.me/s/vsya_pravda_o_casinox_test_i_obz
casino x мобильная
casino x мобильная
Hi, i think that i saw you visited my weblog thus i came to “return the favor”.I am trying to find things to enhance my
web site!I suppose its ok to use a few of your ideas!!
1вин ру скачать
1вин ру скачать
скачать casino x
скачать casino x
22 casino-x
https://t.me/s/casino_x22
скачать casino x на андроид
https://t.me/s/skachat_casinox_na_android
casino x играть
https://t.me/s/casinox_igrat
1вин приложение официальный сайт онлайн
https://t.me/s/oficialnoeprilozhenie_1winonline
официальный сайт casino x
официальный сайт casino x
19 casino-x
19 casino-x
казино х проверка и бонусов casino x обзор казино х
https://t.me/s/kazinoh_proverka_i_bonusov_casin
1вин мобильный
1вин мобильный
casino x com
casino x com
обзор казино casino x
обзор казино casino x
казино х и бонусов casino x обзор казино х промокод
казино х и бонусов casino x обзор казино х промокод
1вин казино зеркало
1вин казино зеркало
admiral x casino
admiral x casino
http://stromectol24.pro/# cost of ivermectin 1% cream
casino x bonus code
https://t.me/s/casinox_bonuscode
best india pharmacy cheapest online pharmacy india Online medicine order
казино х лицензии и бонусов casino x обзор казино х
казино х лицензии и бонусов casino x обзор казино х
1win betting
1win betting
jeux casino jet x
https://t.me/s/jeux_casino_jetx
casino x 1267
casino x 1267
Thank you a lot for sharing this with all of us you actually recognize what you are talking approximately!
Bookmarked. Kindly additionally visit my site =). We may have a hyperlink change arrangement among us
Your method of describing all in this paragraph is actually good, all be able to simply
know it, Thanks a lot.
jeux jet x casino
jeux jet x casino
1вин бет ставки
https://t.me/s/bet1vin_stavki
jet x casino gratuit
https://t.me/s/jet_x_casino_gratuit
My spouse and I stumbled over here from a different website and thought I might check things out.
I like what I see so now i am following you. Look
forward to looking into your web page for a second time.
бонусы casino x
бонусы casino x
х проверка и бонусов casino x обзор х промокод
х проверка и бонусов casino x обзор х промокод
1вин бесплатно приложение
1вин бесплатно приложение
casino x зеркало сайта
casino x зеркало сайта
бонус код casino x
бонус код casino x
casino x зеркало официальный
https://t.me/s/casinox_zerkalo_oficialnyj
buy minocycline 50 mg otc: stromectol ivermectin buy – ivermectin 0.5%
1вин бесплатно мобильный телефон
https://t.me/s/besplatno_mobilnyj_telefon1vin
casino x зеркало россия
casino x зеркало россия
x casino россия
https://t.me/s/x_casino_rossiya
admiral x casino бездепозитный бонус
admiral x casino бездепозитный бонус
casino x support
https://t.me/s/casino_x_support56
1вин бесплатно мобильная версия
https://t.me/s/besplatno_mobilnaya_versiya1vin
Great blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple tweeks would really make my blog shine.
Please let me know where you got your theme. Thank you
casino x выплаты
https://t.me/s/casinox_vyplaty
вся о casino x тест и проверка обзор x x 2021
https://t.me/s/vsya_o_casinox_test_i_proverka
casino x скачать на айфон
casino x скачать на айфон
1вин бесплатно андроид
1вин бесплатно андроид
вся о casino x тест и обзор казино x казино x 2021
вся о casino x тест и обзор казино x казино x 2021
casino x телефон
https://t.me/s/casinox_telefon
1вин бесплатно телефон
1вин бесплатно телефон
вход casino x зеркало сегодня
вход casino x зеркало сегодня
casino x промокод бездепозитный бонус
https://t.me/s/casinox_promokod_bezdepozitnyj_b
cслоты casino x
слоты casino x
casino x скачать бесплатно
casino x скачать бесплатно
1вин бесплатно официальное приложение
https://t.me/s/besplatno1vin_oficialnoe_prilozh
скачать casino x casino apk
https://t.me/s/skachat_casino_x_casino_apk
casino x промокод 2022
https://t.me/s/casino_x_promokod_2022
регистрация в casino x
регистрация в casino x
https://indiapharmacy24.pro/# Online medicine home delivery
casino x review
casino x review
авиатор игра 1вин
авиатор игра 1вин
Hi! Do you know if they make any plugins to assist with Search Engine
Optimization? I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good
results. If you know of any please share. Thank you!
обзор casino x россия
https://t.me/s/obzor_casinox_rossija
casino x приложение на айфон
casino x приложение на айфон
п»їlegitimate online pharmacies india best india pharmacy pharmacy website india
казино икс casino x зеркало
https://t.me/s/kazino_iks_casino_x_zerkalo
casino x реальные отзывы
casino x реальные отзывы
1вин андроид
https://t.me/s/android1vin
казино х лицензии и бонусов casino x казино х промокод
https://t.me/s/kazinoh_licenzii_i_bonusov_casin
casino x отзывы игроков
https://t.me/s/casinox_otzyvy_igrokov
1вин бесплатно мобильный
1вин бесплатно мобильный
casino x рабочий сайт
https://t.me/s/casinox_rabochij_sajt
казино икс casino x официальный сайт
казино икс casino x официальный сайт
игровые автоматы на деньги россия casino x
https://t.me/s/igrovye_avtomaty_na_dengi_rossiy
casino x обзор
casino x обзор
Whats up are using WordPress for your blog platform?
I’m new to the blog world but I’m trying to
get started and create my own. Do you need any html coding
expertise to make your own blog? Any help would be really appreciated!
casino x рабочее
casino x рабочее
casino x зеркало на сегодня мобильная
casino x зеркало на сегодня мобильная
играть в casino x
https://t.me/s/igrat_v_casinox
casino x mobile
https://t.me/s/casino_x_mobile
canada rx pharmacy world: legitimate canadian pharmacy online – canadian pharmacy meds
casino x официальный вход
casino x официальный вход
casino x вывод
casino x вывод
доступное casino x на сегодня
https://t.me/s/dostypnoe_casinox_nasegodnia
casino x код
casino x код
casino x официальный скачать на телефон
https://t.me/s/casinox_oficialnyj_skachat_na_te
casino x slots
casino x slots
casino x зеркало вход
casino x зеркало вход
casino x игровые автоматы на деньги
casino x игровые автоматы на деньги
casino x официальный сайт зеркало сегодня
casino x официальный сайт зеркало сегодня
casino x вывод средств
casino x вывод средств
casino x играть бесплатно
casino x играть бесплатно
casino x скачать мобильную
casino x скачать мобильную
casino x официальный на деньги
https://t.me/s/casinox_oficialnyj_na_dengi
casino x рабочее зеркало сегодня
casino x рабочее зеркало сегодня
casino x фриспины
casino x фриспины
URL
Keywords دستگاه اکسیژن ساز قابل حمل
Blog_Comment فراموش نکنید که مناسبترین اکسیژن ساز برای بیمار شما باید
به وسیله پزشک و بر اساس وضعیت خود بیمار مشخص شود تا
مشکلی برای بیمار و اطرافیان وی به همراه نداشته باشد.
Anchor_Text دستگاه اکسیژن ساز قابل حمل
Image_Comment یک اکسیژن ساز خانگی به اندازه کافی برای استفاده در سفر
کوچک است اگرچه نسبت به یک سیستم قابل حمل، سنگینتر و اشغالکننده
فضا بیشتری است.
Guestbook_Comment این دستگاه ۵ حالت برای نرخ جریان اکسیژن دارد و صدای تولیدی آن فقط ۴۰ دسیبل است که در حد نویز
کامپیوتر است.
Category uncategorized
Micro_Message دستگاه اکسیژن ساز پرتابل لانگفیان دارای خروجی اکسیژن 1 تا 5
لیتر بر
دقیقه است و مناسب برای کارب..
About_Yourself 34 years old Engineer I Oates McFall, hailing from Noelville enjoys watching movies like Red Lights and
Bird watching. Took a trip to My Son Sanctuary and drives a Ferrari 250 GT Series
1.
Forum_Comment ممکن است بپرسید که منظور از دستگاه اکسیژن ساز چیست؟ این محصول یکی از ضروریترین تجهیزات پزشکی خانگی، بیمارستانی
و اورژانس بشمار میرود.
Forum_Subject اجاره دستگاه اکسیژن ساز
خانگی قیمت استثنائی تمامی مدلها فروشگاه تجهیزات پزشکی سپهریار
Video_Title اکسیژن ساز خانگی در ظرفیت های ۳،
۵، ۸ و ۱۰ لیتر قیمت اکسیژن ساز در
اصفهان
Video_Description این نوع اکسیژن
سازها نسبت به اکسیژن ساز های
پرتابل، وزن بیشتری دارند و قابل حمل نمی
باشند.
Preview_Image
YouTubeID
Website_title تعمیر دستگاه اکسیژن ساز توسط تیم متخصص و در سریعترین زمان احیا طب شهریار
Description_250 بهترین مارک اکسیژن ساز
که میتوانید هماکنون از بازار تجهیزات
پزشکی ایران خریداری کنید از بین برندهای آمریکایی، ایرانی، چینی و تایوانی است.
Guestbook_Comment_(German)
Description_450 دستگاه اکسیژن ساز متشکل است از یک کمپرسور هوا، دو سیلندر پر
از گلوله های زئولیتی، یک مخزن مساوی کننده فشار و چند
شیر فلکه و لوله.
Guestbook_Title دستگاه اکسیژن ساز قابل حمل
پرتابل GCE Zen O Lite تجهیزات پزشکی سدان
Website_title_(German)
Description_450_(German)
Description_250_(German)
Guestbook_Title_(German)
Image_Subject دستگاه اکسیژن ساز خانگی ایرانی به
قیمت روز مرجع خرید و فروش دستگاه اکسیژن ساز
Website_title_(Polish)
Description_450_(Polish)
Description_250_(Polish)
Blog Title دستگاه اکسیژن ساز قابل حمل پرتابل Inogen One G5
Blog Description اکسیژن ساز تجهیزات پزشکی ،
لوازم آرایشی ، پوست و مو
Company_Name دستگاه اکسیژن ساز قابل
حمل
Blog_Name دستگاه اکسیژن ساز پرتابل اینوژن G3 تجهیزات پزشکی
موج
Blog_Tagline دستگاه اکسیژن ساز قابل حمل
پرتابل Inogen One G5
Blog_About 25 yr old Marketing Assistant Esta Nevin, hailing from Swan Lake enjoys watching movies like Joe and Metalworking.
Took a trip to Flemish Béguinages and drives a Eldorado.
Article_title اجاره دستگاه اکسیژن ساز خانگی قیمت استثنائی تمامی
مدلها فروشگاه تجهیزات پزشکی سپهریار
Article_summary توجه نمایید که لیتراژ در زمان روشن بودن صفر نباشد،
همچنین از حداکثر عدد نمایش داده شده برروی فلومتر
هم بالاتر نباشد، زیرا باعث آسیب به کمپرسور می شود و همچنین خلوص اکسیژن خروجی کاهش می یابد.
Article این روش از نظر اقتصادی جهت تولید
گازاکسیژن مقرون به صرفه نمی باشد.
دراین روش مخلوط هوای موردنظر در یک برج تقطیر تا دمای میعان سرد شده، سپس
با افزایش تدریجی دما، اجزای سازنده هوا براساس دمای جوش آنها جداسازی میگردند.
فقط یک نکته در رابطه با این دستگاه وجود دارد و آن این است که بعد از تجویز
پزشک باید به سرعت از دستگاه استفاده نمایید.
به همین خاطر متخصصین ریوی تأکید دارند که استفاده
از این دستگاه برای بیماران ریوی امری ضروری است.
با گذشت زمان، به یک مشکل تبدیل میشود، زیرا میتواند مانع
از داشتن خواب خوب و در نتیجه سایر بیماریها
شود.
About_Me 41 years old Account Coordinator Jedidiah Waddup,
hailing from Picton enjoys watching movies like “Trouble with Girls, The” and Worldbuilding.
Took a trip to Belovezhskaya Pushcha / Bialowieza Forest
and drives a Ferrari 250 GT.
About_Bookmark 59 year-old Executive Secretary Teador Kleinfeld,
hailing from Saint-Paul enjoys watching movies like Conan the Barbarian and Yo-yoing.
Took a trip to Teide National Park and drives a Maxima.
Topic دستگاه اکسیژن ساز قابل حمل
casino x развод
casino x развод
https://canadapharmacy24.pro/# pharmacy canadian superstore
casino x официальный играть
https://t.me/s/casinox_oficialnyj_igrat
казино х проверка лицензии и casino x казино х промокод
https://t.me/s/casinox_proverka_licenzii
casino x бонус за депозит
casino x бонус за депозит
casino x работающее зеркало
https://t.me/s/casino_x_rabotayushee_zerkalo
casino x на деньги
casino x на деньги
Definitely believe that that you said. Your favourite reason seemed to be on the net the easiest thing to remember of.
I say to you, I definitely get annoyed whilst folks think about concerns that
they plainly do not realize about. You controlled to hit the
nail upon the highest and also outlined out the entire thing with no need side-effects ,
other people could take a signal. Will likely be again to get more.
Thank you
casino x bonus
casino x bonus
casino x полная версия россия
casino x полная версия россия
casino x приложение на айфон скачать
casino x приложение на айфон скачать
casino x на андроид
https://t.me/s/casinox_na_android
reputable indian pharmacies world pharmacy india indian pharmacy paypal
casino x бонус
https://t.me/s/casino_x_bonu
casino x поддержка
https://t.me/s/casinox_podderzhka
casino x приложение андроид скачать
casino x приложение андроид скачать
casino x мобильная версия россия плей
https://t.me/s/casinox_mobilnaya_versiya_rossiy
casino x бездепозитный бонус за регистрацию
casino x бездепозитный бонус за регистрацию
casino x отзывы россия
https://t.me/s/casinox_otzyvy_rossiya
casino x приложение андроид
casino x приложение андроид
casino x играть россия
casino x играть россия
casino x бездепозитный
casino x бездепозитный
casino x отзывы игроков россия
casino x отзывы игроков россия
Please let me know if you’re looking for a writer for your weblog.
You have some really good posts and I think I would be a good asset.
If you ever want to take some of the load off, I’d absolutely love to write
some material for your blog in exchange for a link back to mine.
Please blast me an email if interested. Kudos!
casino x отзывы о выплатах
https://t.me/s/casino_x_otzyvy_o_vyplatah
casino x фрибет
https://t.me/s/casinox_fribet
casino x актуальное зеркало
https://t.me/s/casinox_aktualnoe_zerkalo
casino x официальный сайт скачать на компьютер
https://t.me/s/casinox_oficialnyj_sajt_skachat
casino x бонус код при регистрации
casino x бонус код при регистрации
casino x официальный сайт регистрация
https://t.me/s/casino_x_oficialnyj_sajt_registr
brill x casino зеркало
brill x casino зеркало
casino x официальный мобильная
https://t.me/s/casinox_oficialnyj_mobilnaya
https://valtrex.auction/# valtrex 500mg cost
casino x бонус код фри спины
https://t.me/s/casinox_bonus_kod_fri_spiny
casino x официальный сайт плей
https://t.me/s/casino_x_oficialnyj_sajt_plej
автоматы на деньги casino x
https://t.me/s/avtomaty_na_dengi_casino_x
x casino официальный сайт вход
x casino официальный сайт вход
casino x android
casino x android
valtrex prescription australia buy valtrex online valtrex prescription
casino x официальный сайт отзывы
https://t.me/s/casino_x_oficialnyj_sajt_otzyvy
скачать приложение казино аврора
скачать приложение казино аврора
casino x официальное зеркало сегодня
casino x официальное зеркало сегодня
Good post. I learn something new and challenging on sites I stumbleupon everyday.
It’s always exciting to read through content from other writers and practice something from their sites.
1 x bet casino
https://t.me/s/bet1x_casino
зеркало aurora casino на деньги
https://t.me/s/zerkalo_aurora_casino_na_dengi
casino x no deposit bonus
https://t.me/s/casino_x_no_deposit_bonus
скачать клиент aurora casino на компьютер
скачать клиент aurora casino на компьютер
casino x мобильная россия
casino x мобильная россия
admiral x casino официальный сайт
admiral x casino официальный сайт
казино аврора войти
https://t.me/s/voyti_casinoaurora
скачать клиент aurora casino
скачать клиент aurora casino
casino x как зайти в игру
https://t.me/s/casino_x_kak_zajti_v_igru
Click on our link to sign up for a free trial of Fubo, and start watching live sports without cable today! Like many young rebuilding teams before them, the Pistons struggle on defense. They’re giving up the second-most points per game in the East, but things are trending up on offense. Cunningham is getting more comfortable, and Jerami Grant has dropped 26 in back-to-back games. There’s more talent on this Pistons offense than you might realize. Just a couple of games ago the Raptors scored 133 against Brooklyn, so they’ve got real offensive upside as well. Don’t count on this one being a defensive struggle like oddsmakers expect. The Philadelphia 76ers (49-30) are underdogs (+2) in their attempt to extend a three-game win streak when they visit the Toronto Raptors (46-33) at 7:30 PM ET on Thursday, April 7, 2022 at Scotiabank Arena. The point total for the matchup is 215.5.
https://files.fm/trapivapen1972/info
Ⓒ 2023 NBC Universal At most sportsbooks, there will be a “live now” tab where you can find games that are in progress and available for betting, separated by sport. You can also find the live options by clicking on an individual sport and then finding the live games. Both the site layout and the live odds could differ from book to book, so make sure you explore all options. Live betting markets at legal sportsbooks include moneyline, point spread, over under, player props, and many others. In some cases, you can even make a parlay bet or multiple parlay bets from live betting lines. But live sports betting has a few pitfalls. Not all sports are available, and not every game will have a live stream or game tracker offering stats and odds. Plus, some Android sportsbook apps won’t list every in-game market compared to the sportsbook’s desktop version.
casino x код при регистрации
casino x код при регистрации
aurora casino личный кабинет
aurora casino личный кабинет
скачать казино aurora casino
скачать казино aurora casino
casino x как зайти
casino x как зайти
URL
Keywords تعمیرگاه جک S3
Blog_Comment جک S3 با موتوری 1.5 لیتری در حدود 107 اسب بخار قدرت را
از طریق گیربکس ضریب متغییر پیوسته
CVT راهی چرخهای جلو میکند و چانگان CS35 به موتوری 1.6 لیتری با قدرت 124
اسب بخار مجهز است و از گیربکسی چهار سرعته اتوماتیک بهره میبرد.
Anchor_Text تعمیرگاه جک S3
Image_Comment در واقع شما بایستی همیشه عملکرد خودرو را تحت نظر داشته باشید و در
صورت مشاهده موارد ذیل، برای تعمیر موتور آن به تعمیرگاهی
معتبر و قابل اعتماد همچون اتوداکار مراجعه کنید.
Guestbook_Comment به طوری که رانندگان می توانند برای
رفع مشکلات در عملکرد خودرو جک، آن را به نمایندگی
ها و تعمیرگاه های تخصصی این خودرو
واگذار نمایند.
Category misc
Micro_Message اگر ماشین تان لرزش دارد و موقع روشن شدن و یا در حرکت ریپ
میزند میتوانید مقاله علت ریپ زدن ماشین را بخوانید.
About_Yourself 58 yr old Social Worker Taddeusz Govan, hailing from Windsor enjoys watching
movies like Investigating Sex (a.k.a. Intimate Affairs)
and Listening to music. Took a trip to Himeji-jo and drives a Ferrari 250 GT LWB Tour
de France.
Forum_Comment جک در خودروهای سدان و در
کراساوورهای میانرده که تحت عنوان
کامپکت CUV شناخته میشوند،
شرایط مناسبی در بازار کشورمان دارد.
Forum_Subject تعمیر گیربکس جک S3 مشاوره و خودرو بر رایگان
Video_Title لوازم یدکی جک لوازم جک شرکتی تماس:
09193937035
Video_Description موتور خودرو های جک نیز معمولا 4 سیلندر است و با توجه به اتوماتیک و دستی بودن آن ها،
قدرت موتور آن ها نیز متفاوت است.
Preview_Image
YouTubeID
Website_title 7 دلیل برای آنکه ام وی ام x22 را
نخریم چرخان
Description_250 همچنین ممکن است ایراداتی روی سر سیلندر وجود داشته باشد، به عنوان مثال، به دلیل دماهای بالا و ارتعاشات قوی در موتور در
حال کار.
Guestbook_Comment_(German)
Description_450 جک در خودروهای سدان و در کراساوورهای میانرده که
تحت عنوان کامپکت CUV شناخته میشوند، شرایط مناسبی در بازار
کشورمان دارد.
Guestbook_Title جک s5 جدید نیوفیس؛ بررسی جامع
و مشخصات فنی
Website_title_(German)
Description_450_(German)
Description_250_(German)
Guestbook_Title_(German)
Image_Subject 10 بهترین تعمیر کاتالیزور
جک S3 در اصفهان بهترینو مهر 1402
Website_title_(Polish)
Description_450_(Polish)
Description_250_(Polish)
Blog Title تعمیرگاه خودرو جک JAC
تعمیرات خودرو جک تعمیر خودروی جک
Blog Description جک S3 تهران پیک خودرو
Company_Name تعمیرگاه جک S3
Blog_Name جک S3 تهران پیک خودرو
Blog_Tagline تعمیر گیربکس اتوماتیک جک S3 با یکسال گارانتی گیربکس
کار ایرانیان
Blog_About 33 yrs old Speech Pathologist Griff Pedracci, hailing from Langley enjoys watching movies
like “Outlaw Josey Wales, The” and Rappelling.
Took a trip to Heritage of Mercury. Almadén and Idrija and drives a Jaguar C-Type.
Article_title کرمانموتور 1732 نمایندگی رسمی فروش خودروهای جک
Article_summary اما با نگاهی به کراساوورهای کامپکت
بازار ایران، متوجه میشویم که شتاب
و ماکزیمم سرعت جک s3 را میتوان از مزایای خودرو دانست.
Article مزیت این شیوه آن است که در تعویض دنده جریان نیرو بدون قطع شدن از موتور به
چرخها انتقال مییابد. مجموعه
بهفن با بیش از 20 سال تجربه بصورت حرفه ایی
در زمینه و طراحی و ساخت و مشاوره قبل از فروش و
خدمات فنی بعد از فروش و خدمات
فنی بعد از فروش با پرسنل مجرب و کارآزموده
نامی آشنا و معتبر در صنعت کشور میباشد
پاور پک بالا بر و آسانسور هیدرولیک
انو… شرکت جک در ابتدا اقدام
به تولید کامیون های تجاری نمود و پس از گذشت سال ها فعالیت خود
شروع به تولید خودروهای ون و شاسی بلند کرد.
انباره اگزوز یا همان صدا خفه
کن، در بخش انتهایی سیستم اگزوز قرار دارند و طبیعتاً پس از مدتی دچار فرسودگی و
در پی آن کاهش راندمان موتور جک خواهد شد.
شرکت خودروسازی چینی جی ای سی یا همان جک (JAC)، حدوداً 22 سال است
که در صنعت ساخت خودرو فعالیت
دارد و در عین حال در مدت زمانی کوتاه
توانسته موفقیت قابل ملاحظه ای را برای خود رقم
زند.
مقر کنونی این شرکت خودروساز چینی در شهر هفئی استان آن هوئی کشور است.
در برخی موارد نیز ممکن است که گیربکس پیغام دهد به طوری این پیغام نشان می دهد که ایراد خاصی در سیستم خودرو وجود دارد و اگر این پیغام رو مشاهده کردید سریعا باید خودرو را به تعمیرگاه برسانید.
در ابتدا شاید فکر کنید که از این که باید خودروی خودتان را سرویس دهی
کنید این امر بسیار برایتان وقت گیر باشد
ولی باید بدانید که اگر سرویس دهی و رسیدگی به خودرو انجام
نشود ممکن است در مدتی طولانی آسیب های
زیادی به گیربکس خودرو وارد شود.
به عنوان مثال باید هر شش ماه یک بار برای این موضوع
وقت بگذارید تا در آینده مجبور نشوید هزینه های زیادی از این بابت بپردازید.
موتورهای بنزینی، موتورهای
دیزلی، خودروهای هیبریدی و حتی خودروهای الکتریکی به طور طبیعی گرما
ایجاد می کنند. هنگامی که از بخاری ماشین خود استفاده می کنید، مقداری از این گرما برای راحتی شما به داخل کابین هدایت می شود.
About_Me 34 yr old Senior Editor Aarika Nye, hailing from Smith-Ennismore-Lakefield enjoys watching movies like My Father the Hero and
Graffiti. Took a trip to Mana Pools National Park and drives a McLaren M16C.
About_Bookmark 29 year-old Librarian Oates Ashburne, hailing from
Fort Erie enjoys watching movies like Vehicle 19 and Computer programming.
Took a trip to Palmeral of Elche and drives a Ferrari 250 GT LWB Berlinetta Tour de France.
Topic تعمیرگاه جک S3
скачать клиент казино аврора ios
https://t.me/s/skachat_klient_kazino_avrora_ios
casino x игровые автоматы на деньги плей
https://t.me/s/casinox_igrovyeavtomaty_na_dengi
An impressive share! I’ve just forwarded this onto a
coworker who had been conducting a little homework
on this. And he actually bought me breakfast due
to the fact that I found it for him… lol. So allow me to reword this….
Thanks for the meal!! But yeah, thanx for spending time to
talk about this matter here on your internet site.
минимальный вывод aurora casino
https://t.me/s/minimalnyj_vyvod_aurora_casino
скачать aurora casino с зеркала
скачать aurora casino с зеркала
casino x как вывести деньги
casino x как вывести деньги
casino x играть на деньги
https://t.me/s/casinox_igrat_na_dengi
скачать казино аврора на андроид на реальные деньги
https://t.me/s/skachat_kazino_avrora_na_android
автоматы игровые
автоматы игровые
https://paxlovid.bid/# paxlovid for sale
скачать aurora casino на русском
https://t.me/s/skachat_aurora_casino_na_russkom
casino x как вывести
https://t.me/s/casino_x_kak_vyvesti
casino x com официальный сайт
casino x com официальный сайт
онлайн игровые автоматы
https://t.me/s/onlain_igrovieavtomaty
скачать aurora casino на планшет
https://t.me/s/skachat_aurora_casino_na_plansh
скачать aurora casino на реальные деньги
https://t.me/s/skachat_aurora_casino_na_realnye
casino-x bonus
https://t.me/s/casinox_bonuss
casino x играть онлайн
casino x играть онлайн
лев игровые автоматы
https://t.me/SpinToWinGambler
скачать aurora casino на андроид
скачать aurora casino на андроид
скачать aurora casino на компьютер
скачать aurora casino на компьютер
casino x бонус код при регистрации pro
casino x бонус код при регистрации pro
casino x доступное зеркало на сегодня
https://t.me/s/casino_x_dostupnoe_zerkalo_na_see
почему не работает aurora casino
почему не работает aurora casino
скачать aurora casino на компьютер с официального сайта
скачать aurora casino на компьютер с официального сайта
I couldn’t resist commenting. Perfectly written!
casino x бонус код без депозита
casino x бонус код без депозита
casino x демо
casino x демо
пополнить aurora casino
https://t.me/s/popolnyt_auroracasino
buy valtrex singapore: buy antiviral drug – valtrex 1500 mg
paxlovid cost without insurance: buy paxlovid online – paxlovid price
сайт aurora casino
сайт aurora casino
where to get cheap mobic without rx buy anti-inflammatory drug can i buy cheap mobic without prescription
скачать aurora casino на андроид зеркало
скачать aurora casino на андроид зеркало
бонус код и промокоды в casino x
бонус код и промокоды в casino x
aurora casino рабочее зеркало
https://t.me/s/rabochee_zerkalo_auroracasino
17 casino-x
https://t.me/s/casino_x_17
клиент aurora casino
клиент aurora casino
бездепозитный бонус код в casino x
https://t.me/s/bezdepozitnyj_bonus_kod_v_casino
игровые автоматы без регистрации бесплатно
https://t.me/s/RouletteRoyaltyMastermind
бонус код casino x новые
https://t.me/s/bonus_kod_casino_x_novye
скачать aurora casino на андроид на реальные деньги
скачать aurora casino на андроид на реальные деньги
казино аврора зеркало скачать
https://t.me/s/kazino_avrora_zerkalo_skachat
игровые автоматы космолот
игровые автоматы космолот
зеркало aurora casino
зеркало aurora casino
казино аврора вход на сайт
казино аврора вход на сайт
игровые автоматы вулкан 777
https://t.me/s/vylkan777_igrovyeavtomaty
Have you ever considered about including a little bit more than just your articles?
I mean, what you say is important and all. However think of if you added some great visuals or video
clips to give your posts more, “pop”! Your content is excellent but with pics and clips, this site could undeniably be
one of the very best in its field. Great blog!
aurora casino приложение
aurora casino приложение
скачать aurora casino на айфон
скачать aurora casino на айфон
If you desire to take a good deal from this paragraph then you have to apply these methods
to your won website.
http://mobic.icu/# where to buy mobic without a prescription
казино аврора вход
https://t.me/s/kazino_avrora_vhod
восток игровые автоматы
восток игровые автоматы
скачать aurora casino на деньги на андроид
https://t.me/s/skachat_aurora_casino_na_dengi_n
Nice answer back in return of this query with solid arguments
and describing the whole thing on the topic of that.
игровые автоматы бесплатно с бонусами
https://t.me/s/SlotSensationWhispererAce
не работает aurora casino
не работает aurora casino
казино аврора ссылка
казино аврора ссылка
установить aurora casino на андроид
установить aurora casino на андроид
скачать приложение aurora casino на андроид
https://t.me/s/skachat_auroraCasino_na_android
казино игровые автоматы
казино игровые автоматы
казино аврора скачать на пк
https://t.me/s/kazino_avrora_skachat_na_pk
ставки aurora casino
https://t.me/s/stavki_auroracasino
скачать aurora casino на андроид бесплатно
скачать aurora casino на андроид бесплатно
казино аврора слоты
казино аврора слоты
лучшие игровые автоматы онлайн
лучшие игровые автоматы онлайн
казино аврора скачать клиент
https://t.me/s/kazino_avrora_skachat_klient
игровые автоматы адмирал
игровые автоматы адмирал
онлайн казино aurora casino
онлайн казино aurora casino
Wow! This blog looks just like my old one! It’s on a completely different
topic but it has pretty much the same page layout and
design. Outstanding choice of colors!
верификация aurora casino
https://t.me/s/verifikaciya_aurora_casino
казино аврора скачать на телефон
казино аврора скачать на телефон
казино аврора скачать бесплатно
https://t.me/s/kazino_avrora_skachat_besplatno
игровые автоматы резидент
игровые автоматы резидент
игровые автоматы демо играть бесплатно клубнички
https://t.me/s/klybnichki_igrovyeavtomaty
Замечательный выбор для отдыха!
Просторные квартиры вблизи Парка Галицкого позволяют ознакомиться с
красотой этого природного уголка.
Бронирование удобное, цены
приемлемые. Рекомендую всем, кто предпочитает уют и красивые виды.
Проверьте по ссылке и посмотрите варианты.
Снять квартиру посуточно Краснодар
казино аврора вывод денег
казино аврора вывод денег
order valtrex online: buy antiviral drug – valtrex 2 tablets
казино аврора скачать
казино аврора скачать
скачать клиент aurora casino на андроид
скачать клиент aurora casino на андроид
казино онлайн игровые автоматы
https://t.me/s/kazino_igrovyeavtomaty
казино аврора скачать на iphone
казино аврора скачать на iphone
казино аврора в браузере
https://t.me/s/kazino_avrora_v_brauzere
paxlovid covid paxlovid best price Paxlovid over the counter
казино аврора сайт
https://t.me/s/kazino_avrora_sajt
игровые автоматы казино
игровые автоматы казино
казино аврора скачать на андроид на деньги
казино аврора скачать на андроид на деньги
казино аврора отзывы
казино аврора отзывы
казино аврора россия
казино аврора россия
мелбет игровые автоматы
https://t.me/s/RouletteRicochetChampion
казино аврора зеркало вход
казино аврора зеркало вход
казино аврора регистрация
https://t.me/s/kazino_avrora_registraciya
Oh my goodness! Awesome article dude! Thanks, However I am experiencing troubles with your RSS.
I don’t know why I am unable to join it. Is there anyone else getting identical
RSS issues? Anybody who knows the answer will you kindly respond?
Thanx!!
http://valtrex.auction/# valtrex medication cost
казино аврора online
https://t.me/s/kazino_avrora_online
промокод aurora casino
https://t.me/s/promokod_aurora_casino
казино аврора отзывы вывод денег
казино аврора отзывы вывод денег
казино аврора зеркало сайта
https://t.me/s/kazino_avrora_zerkalo_sajta
казино аврора promo code
https://t.me/s/kazino_avrora_promo_code
казино аврора онлайн
казино аврора онлайн
order mobic no prescription: cheap meloxicam – how to buy mobic online
промокод aurora casino для старых игроков
https://t.me/s/promocod_auroracasino_igroki
казино аврора личный кабинет
https://t.me/s/kazino_avrora_lichnyj_kabinet
казино аврора официальный сайт вход
https://t.me/s/kazino_avrora_oficialnyj_sajt_vh
казино аврора рабочее зеркало
https://t.me/s/kazino_avrora_rabochee_zerkalo
игровые автоматы слоты играть бесплатно
https://t.me/s/pokerdom_igrovyesloty
казино аврора отзывы вывод денег
https://t.me/s/kazino_avrora_otzyvy_vyvod_deneg
казино аврора через браузер
казино аврора через браузер
казино аврора официальный сайт
https://t.me/s/kazino_avrora_oficialnyj_sajt
казино аврора ios скачать
https://t.me/s/kazino_avrora_ios_skachat
казино аврора мобильное приложение
https://t.me/s/kazino_avrora_mobilnoe_prilozhen
играть бесплатно и без регистрации в игровые автоматы
https://t.me/SpinToVictoryAceGambler
It’s truly very complex in this active life to listen news on Television,
therefore I simply use the web for that reason, and get the most recent news.
казино аврора casino бездепозитный бонус
казино аврора casino бездепозитный бонус
aurora casino промокод фриспины
aurora casino промокод фриспины
казино аврора на деньги
https://t.me/s/kazino_avrora_na_dengi
казино аврора casino
казино аврора casino
игровые автоматы новинки
игровые автоматы новинки
как зарегистрироваться на aurora casino
как зарегистрироваться на aurora casino
казино аврора ios
https://t.me/s/kazino_avroraios
Pretty component to content. I simply stumbled upon your blog
and in accession capital to assert that I get actually loved account your weblog posts.
Anyway I will be subscribing on your feeds and even I fulfillment you
access consistently fast.
казино аврора на андроид
https://t.me/s/kazino_avrora_na_android
казино аврора ставки
казино аврора ставки
как скачать aurora casino на андроид
как скачать aurora casino на андроид
aurora casino как выиграть
aurora casino как выиграть
казино аврора играть в браузере
казино аврора играть в браузере
казино аврора мобильная версия
казино аврора мобильная версия
казино аврора не работает
казино аврора не работает
пин ап игровые автоматы официальный сайт
https://t.me/s/igrovyesloty_onlainn
казино аврора casino зеркало
https://t.me/s/kazino_avrora_casino_zerkalo
игровые автоматы скачать бесплатно
игровые автоматы скачать бесплатно
http://cialis.foundation/# Generic Tadalafil 20mg price
казино аврора mobile скачать андроид
казино аврора mobile скачать андроид
казино аврора apk
https://t.me/s/kazino_avrora_apk
вулкан игровые автоматы бесплатно
вулкан игровые автоматы бесплатно
казино аврора бонус
казино аврора бонус
игровые автоматы купить
игровые автоматы купить
https://kamagra.icu/# п»їkamagra
казино аврора mobile скачать
https://t.me/s/kazino_avrora_mobile_skachat
казино аврора бездепозитный бонус
https://t.me/s/kazino_avrora_bezdepozitnyj_bonu
казино aurora casino отзывы
https://t.me/s/kazino_aurora_casino_otzyvy
игровые автоматы в москве
игровые автоматы в москве
игровые автоматы слоты играть бесплатно без регистрации и смс онлайн
игровые автоматы слоты играть бесплатно без регистрации и смс онлайн
казино аврора играть онлайн
https://t.me/s/kazino_avrora_igrat_onlajn
aurora casino играть на реальные деньги
https://t.me/s/igrat_realnye_dengi_auroracasino
как вывести деньги с aurora casino
https://t.me/s/kak_vyvesti_dengi_s_casinoaurora
http://viagra.eus/# sildenafil online
игровые автоматы с выводом денег
игровые автоматы с выводом денег
игровые автоматы миллионер бесплатно
https://t.me/s/igrovieavtomaty_millionerr
казино аврора android скачать
казино аврора android скачать
казино аврора скачать на андроид бесплатно
казино аврора скачать на андроид бесплатно
как получить $10 на aurora casino
https://t.me/s/kakpoluchit10_na_auroracasino
игровые автоматы играть бесплатно сейчас
https://t.me/s/igrovyeavtomaty_seychas
игровые автоматы casino x
игровые автоматы casino x
казино аврора приложение
https://t.me/s/casinoAurora_prilozhenie
казино аврора
https://t.me/s/kazino_avrora
I do not even know how I ended up here, but I thought this post was good.
I do not know who you are but definitely you are
going to a famous blogger if you aren’t already 😉 Cheers!
бесплатные игровые автоматы вулкан
бесплатные игровые автоматы вулкан
Sildenafil Citrate Tablets 100mg Viagra generic over the counter viagra without prescription
миллионер игровые автоматы
https://t.me/s/igrovyeavtomaty_millioner
игровые автоматы гараж
игровые автоматы гараж
казино аврора на реальные деньги
казино аврора на реальные деньги
aurora casino в россии
https://t.me/s/aurora_casino_v_rossii
игровые автоматы играть демо
https://t.me/s/igrovyeavtomaty_igratdemo
игровые автоматы демо версии
игровые автоматы демо версии
казино аврора акции
казино аврора акции
игровые автоматы космолот играть бесплатно
игровые автоматы космолот играть бесплатно
aurora casino войти
aurora casino войти
Hi, constantly i used to check website posts here early in the daylight,
for the reason that i enjoy to gain knowledge of more and more.
http://cialis.foundation/# Buy Tadalafil 20mg
игровые автоматы бонус за регистрацию
https://t.me/s/igrovyeavtomaty_bonys
бонус код aurora casino
бонус код aurora casino
бесплатные игровые автоматы играть бесплатно
бесплатные игровые автоматы играть бесплатно
игровые автоматы играть бесплатно клубнички скачать
https://t.me/s/igrovyeavtomaty_klubnichkiu
Excellent post. I will be going through some of these issues as well..
Definitely imagine that which you stated. Your favourite justification seemed to
be on the internet the simplest thing to bear in mind of.
I say to you, I certainly get irked even as people consider concerns that they plainly
do not recognise about. You managed to hit the nail upon the highest and outlined out the entire thing with no
need side-effects , other folks could take a signal. Will likely be
back to get more. Thank you
aurora casino вход
aurora casino вход
бездепозитный бонус aurora casino
https://t.me/s/bezdepozitnyj_bonus_aurora_casin
демо игровые автоматы без регистрации
демо игровые автоматы без регистрации
http://cialis.foundation/# Cialis 20mg price
игровые автоматы вулкан играть бесплатно
игровые автоматы вулкан играть бесплатно
игровые автоматы скачать бесплатно клубнички на телефон java
https://t.me/s/igrovyeavtomaty_klubnichki
http://levitra.eus/# п»їLevitra price
aurora casino скачать на пк
aurora casino скачать на пк
aurora casino официальный сайт играть на деньги
https://t.me/s/auroracasiono_offsait_igrat
игровые автоматы бесплатно онлайн
https://t.me/s/igrovyeavtomaty_besplatno
1xbet игровые автоматы
https://t.me/s/CasinoMogulRoyalFlush
игровые автоматы казино х
игровые автоматы казино х
aurora casino скачать клиент на пк
aurora casino скачать клиент на пк
aurora casino зеркало основное
https://t.me/s/aurora_casino_zerkalo_osnovnoe
игровые автоматы онлайн украина
игровые автоматы онлайн украина
скачать игровые автоматы без интернета
https://t.me/s/CasinoMogulAceOfGames
бк леон игровые автоматы
https://t.me/s/igrovyeavtomaty_bkleon
aurora casino вывод средств отзывы
aurora casino вывод средств отзывы
aurora casino скачать бесплатно
aurora casino скачать бесплатно
Today, I went tto the berach wityh my kids. I founjd a sea shell aand gave it to my 4 year oold daughtter and sid “You can hear the ocean if you put this to your ear.” She placed the sherll to herr eaar and screamed.
There wass a hermit craab insode annd iit pinched herr ear.
She neber wantfs tto ggo back! LoL I know this iss eentirely offf topic buut I
had too tell someone!
игровые автоматы чемпион
https://t.me/s/igrovieavtomay_chempion
игровые автоматы миллионер играть бесплатно
игровые автоматы миллионер играть бесплатно
aurora casino вход в личный кабинет
aurora casino вход в личный кабинет
Survival blade– make certain to have a knife or multi-tool.
игровые автоматы вулкан онлайн
игровые автоматы вулкан онлайн
aurora casino скачать apk
https://t.me/s/aurora_casino_skachat_apk
слоты игровые автоматы
https://t.me/s/igrovie_avtomaty_besplatn
aurora casino в браузере
https://t.me/s/aurora_casino_v_brauzere
играть в игровые автоматы на деньги с телефона
играть в игровые автоматы на деньги с телефона
aurora casino онлайн
https://t.me/s/aurora_casinoonlajn
играть в игровые автоматы без регистрации бесплатно
https://t.me/s/igrovyeavtomaty_bezregistracii
aurora casino турниры
https://t.me/s/aurora_casino_turniry
казино игровые автоматы бесплатно
https://t.me/s/igroovyeavtomaty_besplatno
вулкан игровые автоматы официальный сайт
https://t.me/s/CasinoCashMogulEmpireChampion
http://kamagra.icu/# super kamagra
aurora casino официальный сайт зеркало скачать
aurora casino официальный сайт зеркало скачать
игровые автоматы без депозита
игровые автоматы без депозита
aurora casino скачать приложение
aurora casino скачать приложение
Hello there! This post couldn’t be written any better!
Going through this post reminds me of my previous roommate!
He continually kept talking about this. I will send this article to
him. Fairly certain he will have a good read. Thanks for sharing!
buy Viagra online cheap viagra Order Viagra 50 mg online
играть в игровые автоматы демо
https://t.me/s/DiceRollerSavantGambitMaster
играть в игровые автоматы бесплатно без регистрации
https://t.me/s/CasinoCashMogulEmpi
aurora casino официальный сайт вход
https://t.me/s/aurora_casino_oficialnyj_sajt_vh
google игровые автоматы бесплатные
google игровые автоматы бесплатные
What’s Going down i am new to this, I stumbled upon this I have found It positively helpful
and it has aided me out loads. I hope to contribute & assist
different customers like its helped me. Good job.
My web page … https://web-directory-online.eu/
aurora casino скачать на телефон
https://t.me/s/aurora_casino_skachat_na_telefon
Hola! I’ve been following your weblog for a long time now and finally got the courage to go ahead and give you a
shout out from Kingwood Texas! Just wanted to say keep up the fantastic job!
1 вин официальный сайт игровые автоматы
1 вин официальный сайт игровые автоматы
казино аврора зеркало
https://t.me/s/casinoaurora_zerkalo
aurora casino официальный сайт скачать
aurora casino официальный сайт скачать
aurora casino скачать на ios
aurora casino скачать на ios
играть в игровые автоматы онлайн
играть в игровые автоматы онлайн
бесплатные игровые автоматы без регистрации
бесплатные игровые автоматы без регистрации
казино аврора официальный сайт зеркало
казино аврора официальный сайт зеркало
aurora casino русский сайт
aurora casino русский сайт
https://viagra.eus/# sildenafil online
aurora casino официальный сайт на реальные деньги
https://t.me/s/aurora_casino_oficialnyj_sajt_na
https://levitra.eus/# Vardenafil price
играть в игровые автоматы бесплатно и без регистрации
https://t.me/s/igrovyeavtomatu_besplatno
казино аврора как выиграть
казино аврора как выиграть
казино аврора вывод средств
казино аврора вывод средств
aurora casino русский
https://t.me/s/auroraCasino_russkiy
aurora casino официальный сайт играть онлайн
https://t.me/s/aurora_casino_oficialnyjsajt_igr
игровые автоматы для детей
игровые автоматы для детей
aurora casino регистрация
https://t.me/s/aurora_casino_registraciya
казино аврора промокод
https://t.me/s/casino_aurora_promokod
aurora casino официальный сайт играть
aurora casino официальный сайт играть
игровые автоматы играть онлайн бесплатно без регистрации
https://t.me/s/igrovyeavtomati_bezregistracii
aurora casino казино промокод
aurora casino казино промокод
детские игровые автоматы
https://t.me/s/CardSharkVirtuosoGambler
казино аврора казахстан
https://t.me/s/casino_aurora_kazahstan
Pretty! This was an incredibly wonderful article. Thank you for supplying this information.
Thank you for sharing your info. I really appreciate your efforts and I am waiting for your further post thank you once
again.
aurora casino официальный сайт
aurora casino официальный сайт
играть в игровые автоматы онлайн бесплатно
https://t.me/s/igrovyeavtomati_besplatno
aurora casino отзывы игроков
https://t.me/s/aurora_casino_otzyvy_igrokov
игровые автоматы 777
игровые автоматы 777
казино аврора android
https://t.me/s/casino_aurora_android
aurora casino на телефон
aurora casino на телефон
aurora casino онлайн играть бесплатно
aurora casino онлайн играть бесплатно
играть в игровые автоматы бесплатно и без регистрации онлайн
играть в игровые автоматы бесплатно и без регистрации онлайн
играть игровые автоматы бесплатно
играть игровые автоматы бесплатно
игровые автоматы лев
игровые автоматы лев
aurora casino на реальные деньги
aurora casino на реальные деньги
aurora casino официальный сайт скачать на андроид
https://t.me/s/aurora_casino_oficialnyj_sajt_sk
Wow that was unusual. I just wrote an very long comment but after I
clicked submit my comment didn’t show up. Grrrr…
well I’m not writing all that over again. Anyhow, just wanted to say
wonderful blog!
игровые автоматы с выводом денег на карту
игровые автоматы с выводом денег на карту
игровые автоматы играть онлайн на деньги
https://t.me/s/BetBillionaireWhisperer
aurora casino бездепозитный бонус 1000
https://t.me/s/bonus_aurora_casino_1000
aurora casino на пк
https://t.me/s/aurora_casino_na_pc
aurora casino на андроид
aurora casino на андроид
Levitra 10 mg buy online Levitra online USA fast Levitra 10 mg buy online
скачать игровые автоматы на телефон
https://t.me/s/igrovieavtomaty_natelefon
This rope can pertain to your rescue and also aid
others in demand.
игровые автоматы играть без регистрации
https://t.me/s/avvtomatu_igrovye
If you wish for to grow your knowledge only keep visiting this web site and be updated with the newest information posted here.
игровые автоматы вулкан играть онлайн
https://t.me/s/bezplatnyeigrovue_avtomaty
aurora casino на деньги
https://t.me/s/aurora_casino_na_dengi
aurora casino мобильная версия
https://t.me/s/aurora_casino_mobversiya
миллион игровые автоматы
миллион игровые автоматы
aurora casino зеркало на сегодня
https://t.me/s/aurora_casino_zerkalo_na_segodny
aurora casino кз
aurora casino кз
игровые автоматы вулкан бесплатно
https://t.me/s/BetBlitzSultanMaestroKing
aurora casino мобильное приложение
aurora casino мобильное приложение
http://kamagra.icu/# Kamagra 100mg
EnchagPT Blog to miejsce, gdzie można znaleźć interesujące artykuły
i informacje na temat technologii sztucznej inteligencji.
Jest to blog dedykowany wszystkim entuzjastom sztucznej inteligencji,
którzy pragną zgłębiać swoją wiedzę na temat tego fascynującego tematu.
скачать бесплатно игровые автоматы без интернета
скачать бесплатно игровые автоматы без интернета
aurora casino зеркало
https://t.me/s/auroracasino_zerkalo
aurora casino коды
aurora casino коды
поиграть в игровые автоматы бесплатно
поиграть в игровые автоматы бесплатно
aurora casino игры
https://t.me/s/aurora_casino_igry
Appreciate this post. Let me try it out.
aurora casino играть в браузере
https://t.me/s/aurora_casino_igrat_v_brauzere
aurora casino зарегистрироваться
aurora casino зарегистрироваться
слоты игровые автоматы играть бесплатно
https://t.me/s/igrovieavtomaty_besplatno
aurora casino играть онлайн на деньги
aurora casino играть онлайн на деньги
азартные игровые автоматы
https://t.me/s/azartnye_igrovyeatomaty
aurora casino играть онлайн в браузере
https://t.me/s/aurora_casino_igrat_onlajn_v_bra
aurora casino вывод на карту
aurora casino вывод на карту
игровые автоматы играть онлайн бесплатно
https://t.me/s/igrobyeavtomaty_onnline
aurora casino играть онлайн
https://t.me/s/aurora_casino_igrat_onlajn
игровые автоматы на реальные деньги с выводом
игровые автоматы на реальные деньги с выводом
aurora casino играть на деньги
https://t.me/s/auroracasino_igratnadengi
aurora casino ставки на спорт
aurora casino ставки на спорт
казино аврора зеркало на сегодня
https://t.me/s/casinoaurora_zerkalo_na_segodnya
Hello, put your money into my hand-drawn NFTs.
They are unique and original.
Invest safely in an art medium, excellent in the long run.
Don’t hesitate to contact me:
michel710@tutanota.com
Thank you
aurora casino играть
aurora casino играть
игровые автоматы играть бесплатно онлайн с бонусами
https://t.me/s/avtomaty_igrovyeonlain
aurora casino фриспины
https://t.me/s/aurora_casino_frispiny
Hi! I could have sworn I’ve been to this website before but after
checking through some of the post I realized it’s new to me.
Anyhow, I’m definitely glad I found it and I’ll be book-marking
and checking back often!
aurora casino скачать приложение на айфон
https://t.me/s/aurora_casino_skachat_prilozheni
казино аврора apk скачать
казино аврора apk скачать
aurora casino бесплатно
aurora casino бесплатно
игровые автоматы вавада
https://t.me/s/avtomaty_igrovyeer
aurora casino апк скачать
https://t.me/s/aurora_casino_apk_skachat
aurora casino официальный сайт регистрация
https://t.me/s/aurora_casino_oficialnyj_sajt_re
aurora casino
aurora casino
aurora casino зеркало войти
https://t.me/s/aurora_casino_zerkalo_vojti
buy viagra here sildenafil 50 mg price Viagra tablet online
aurora casino apk
aurora casino apk
aurora casino зеркало 2023
https://t.me/s/aurora_casino_zerkalo_2023
aurora casino казино бонусы
aurora casino казино бонусы
казино аврора играть
казино аврора играть
актуальные промокоды aurora casino
актуальные промокоды aurora casino
aurora casino зеркало вход
https://t.me/s/aurora_casino_zerkalo_vhod
aurora casino вывод средств
aurora casino вывод средств
https://kamagra.icu/# Kamagra 100mg
aurora casino кабинет
aurora casino кабинет
http://kamagra.icu/# super kamagra
казино аврора скачать на андроид
https://t.me/casino_Aurora_na_android
The material suitable for this is just photopolymer material that’s readily
available in several colors as well as forms.
aurora casino зеркало сайта
https://t.me/s/aurora_casino_zerkalo_sajta
aurora casino вывод денег
aurora casino вывод денег
https://viagra.eus/# Viagra tablet online
казино вулкан игровые автоматы
казино вулкан игровые автоматы
aurora casino казахстан
https://t.me/aurora_casino_kazahstan
aurora casino бонус за регистрацию
aurora casino бонус за регистрацию
aurora casino зеркало играть онлайн
aurora casino зеркало играть онлайн
aurora casino официальный сайт скачать на андроид бесплатно
https://t.me/s/auroracasino_skachat_na_android
бесплатные игровые автоматы демо
бесплатные игровые автоматы демо
игровые автоматы бесплатные
игровые автоматы бесплатные
aurora casino зеркало играть
https://t.me/s/aurora_casino_zerkalo_igrat
aurora casino скачать на андроид бесплатно с официального
https://t.me/s/aurora_casino_skachat_na_android
игровые автоматы демо играть бесплатно без регистрации
игровые автоматы демо играть бесплатно без регистрации
I’m gone to say to my little brother, that he should also pay a quick visit
this blog on regular basis to get updated from most recent
information.
Awesome things here. I’m very glad to see your article.
Thanks a lot and I’m looking forward to touch you. Will you
please drop me a e-mail?
онлайн казино играть на деньги на рубли
онлайн казино играть на деньги на рубли
aurora casino скачать
aurora casino скачать
aurora casino слоты
https://t.me/s/aurora_casino_sloty
скачать игровые автоматы бесплатно без регистрации
скачать игровые автоматы бесплатно без регистрации
играть бесплатно в игровые автоматы без регистрации
играть бесплатно в игровые автоматы без регистрации
онлайн. казино. на. рубли.
https://t.me/s/BetBlitzAce
aurora casino промокод бездепозитный бонус
aurora casino промокод бездепозитный бонус
aurora casino зеркало рабочее на сегодня
https://t.me/s/aurora_casino_rabochee_zerkalo
обзор топ 3 россии джойказино максбет покердом игры топ онлайн
https://t.me/s/Shuffle_Dom
казино онлайн играть на деньги рубли адмирал
казино онлайн играть на деньги рубли адмирал
топовые румы казино покердом обзор казино покердом
https://t.me/s/top_rymi_pokerdom
aurora casino промокод при регистрации
aurora casino промокод при регистрации
aurora casino онлайн зеркало
https://t.me/s/auroraCasino_onlainzerkalo
игровые автоматы играть бесплатно без регистрации прямо сейчас
игровые автоматы играть бесплатно без регистрации прямо сейчас
Kamagra tablets п»їkamagra cheap kamagra
обзор топ 3 джойказино максбет покердом лучшие игры топ онлайн
обзор топ 3 джойказино максбет покердом лучшие игры топ онлайн
онлайн казино рулетка на рубли
онлайн казино рулетка на рубли
aurora casino отзывы
aurora casino отзывы
aurora casino официальный сайт зеркало
https://t.me/s/aurora_casino_oficialnyj_sajt_ze
леон игровые автоматы
https://t.me/s/RouletteRacerEliteX
старые игровые автоматы играть бесплатно
https://t.me/s/staryeigrovye_avtomaty
I am curious to find out what blog platform you have been using?
I’m experiencing some small security issues with my latest website and I’d like to find something more secure.
Do you have any solutions?
Приобретайте актуальную технику вместе с надёжным стабилизатором напряжения
стабилизаторы напряжения http://stabrov.ru.
online казино на рубли
online казино на рубли
aurora casino официальный сайт отзывы
https://t.me/s/aurora_casino_of_sait_otzivy
казино – игровые автоматы
казино – игровые автоматы
aurora casino официальный сайт вход зеркало
https://t.me/s/aurora_casino_oficialnyj_sajtvh
комиссии покердом
комиссии покердом
игровые автоматы с бездепозитным бонусом
https://t.me/s/SlotSensationElite
казино +на рубли лайв
https://t.me/s/kazinonarybli_life
https://levitra.eus/# Vardenafil price
aurora casino на айфон
aurora casino на айфон
покердом личный кабинет pokerdom
покердом личный кабинет pokerdom
aurora casino официальный сайт играть зеркало
https://t.me/s/auroracasino_oficialniysait_igra
игровые автоматы скачать
https://t.me/s/skachat_igrovyeavtomaty
казино играть на рубли
https://t.me/s/kazinonarubli_igrat
aurora casino ios
https://t.me/s/AuroraCasino_ios
казино pokerdom реальный обзор автоматы покердом слоты дом
казино pokerdom реальный обзор автоматы покердом слоты дом
разбор казино покердом тест и проверка зеркало покердом
разбор казино покердом тест и проверка зеркало покердом
aurora casino казино зеркало
https://t.me/s/aurora_casino_kazino_zerkalo
http://kamagra.icu/# sildenafil oral jelly 100mg kamagra
русское интернет казино на рубли
https://t.me/s/inetkazino_narubli
обзор топ 3 россии джойказино максбет покердом лучшие топ онлайн
обзор топ 3 россии джойказино максбет покердом лучшие топ онлайн
aurora casino бонус
https://t.me/s/aurora_casino_bonus
игровые автоматы играть бесплатно гном
https://t.me/s/pokerdom_igrovyeavtomatyu
aurora casino казино вход
aurora casino казино вход
онлайн казино на реальные деньги рубли россия
онлайн казино на реальные деньги рубли россия
популярные игровые автоматы
популярные игровые автоматы
играть в игровые автоматы на деньги
играть в игровые автоматы на деньги
покердом реферал
покердом реферал
aurora casino казино официальный сайт
aurora casino казино официальный сайт
покер на покердом
https://t.me/s/poker_na_pokerdoma
какое казино играет на рубли россия
какое казино играет на рубли россия
играть игровые автоматы бесплатно без регистрации
https://t.me/s/bezplatnye_igrovyeavtomaty
онлайн казино игровые автоматы
онлайн казино игровые автоматы
покердом вывод средств отзывы
https://t.me/s/pokerdom_vyvod
aurora casino казино играть онлайн
aurora casino казино играть онлайн
список проверенных казино на рубли без минималки
https://t.me/s/kazinonarubli_bezminvznosa
Tadalafil Tablet cialis for sale Cialis 20mg price in USA
официальные игровые автоматы
официальные игровые автоматы
Удалить аккаунт ПокерДом
Удалить аккаунт ПокерДом
покердом на андроид скачать бесплатно на русском
https://t.me/s/pokerdom_skachata
aurora casino казино
aurora casino казино
лучшие казино онлайн на деньги рубли
https://t.me/s/kazinoha_naryblii
Simply want to say your article is as astonishing.
The clarity for your submit is just excellent and i can assume you are a professional on this subject.
Fine together with your permission allow me to grasp your RSS feed
to stay updated with imminent post. Thank you 1,000,000 and
please continue the enjoyable work.
казино pokerdom обзор игровые автоматы покердом покер дом
казино pokerdom обзор игровые автоматы покердом покер дом
скачать игровые автоматы миллионер бесплатно
https://t.me/SlotSorcererExtraordinaireAce
топ казино онлайн на рубли
топ казино онлайн на рубли
актуальное зеркало aurora casino
актуальное зеркало aurora casino
казино лайф на рубли
казино лайф на рубли
pokerdom проверяем румы онлайн покердом обзор покердом
pokerdom проверяем румы онлайн покердом обзор покердом
pokerdom реальный обзор игровые автоматы покердом слоты дом
pokerdom реальный обзор игровые автоматы покердом слоты дом
список казино онлайн на рубли
https://t.me/s/spisok_kazinonarublii
казино корона на рубли
казино корона на рубли
http://cialis.foundation/# Buy Tadalafil 10mg
This paragraph offers clear idea designed for the new visitors of blogging, that
truly how to do running a blog.
URL
Keywords خریدار لوازم شرکتی
Blog_Comment به طور کلی، لوازم خانگی که سلامت خوبی دارد ارزش بیشتری نسبت به لوازمی دارد که از نظر سلامت
و کارایی تقریبا کار نمیکند.
Anchor_Text خریدار لوازم شرکتی
Image_Comment آیا میز اداری مدولار قابل تغییر در طول زمان است؟
بله، میزهای اداری مدولار قابلیت تغییر و تنظیم در
طول زمان را دارند.
Guestbook_Comment برای به حداکثر رساندن قرار گرفتن در معرض لیست خود، از استراتژیهای بازاریابی و تبلیغاتی موثر استفاده کنید.
Category uncategorized
Micro_Message خریدار لوازم خانگی خریدار لوازم
خانگی فردی است که مسئول خرید
لوازم خانگی مورد نیاز افرادی می باشد.
About_Yourself 22 yr old Accounting Assistant I
Jedidiah Pedracci, hailing from Aldergrove enjoys watching movies like Only Yesterday (Omohide poro poro) and Flying disc.
Took a trip to Wieliczka Salt Mine and drives
a Ferrari 250 LM.
Forum_Comment به این صورت که با فروش وسایل دست دوم
و قدیمی خود میتوانید بخشی از مبلغی
که بابت خرید وسایل اداری جدید و نو پرداخت میکنید را جبران بنمایید.
Forum_Subject وایر شمع تیبا شرکتی موجود در فروشگاه آراد فروش وایرشمع تیبا به قیمت عمده
Video_Title سیم گاز تیبا شرکتی موجود در فروشگاه آراد فروش کابل گاز تیبا به قیمت عمده
Video_Description آیا میز اداری برقی قابل تنظیم
ارتفاع دارد؟
بله، میزهای اداری برقی قابل تنظیم ارتفاع هستند و این امکان را به کاربر میدهند تا ارتفاع میز را بر اساس نیاز خود تنظیم کنند.
Preview_Image
YouTubeID
Website_title وایر شمع تیبا شرکتی موجود در فروشگاه
آراد فروش وایرشمع تیبا به قیمت عمده
Description_250 شما میتوانید از سایت سمساری طنین استفاده کنید برای مشاهده خدمات ارائه شده توسط ما میتوانید بر روی لینک سمساری کلیک کنید.
Guestbook_Comment_(German)
Description_450 به طور کلی، لوازم خانگی که سلامت خوبی دارد
ارزش بیشتری نسبت به لوازمی دارد که از نظر سلامت و کارایی تقریبا
کار نمیکند.
Guestbook_Title فشنگی روغن پراید شرکتی فروشگاه آراد فروش مهره روغن پراید 4-500458 قیمت عمده
Website_title_(German)
Description_450_(German)
Description_250_(German)
Guestbook_Title_(German)
Image_Subject سنسور آب پراید زیمنس شرکتی موجود در فروشگاه آراد فروش فشنگی آب پراید قیمت عمده
Website_title_(Polish)
Description_450_(Polish)
Description_250_(Polish)
Blog Title سنسور دریچه گاز پراید شرکتی موجود
در فروشگاه آراد فروش سنسور
پراید به قیمت عمده
Blog Description سیم گاز کاربراتور پراید شرکتی موجود در فروشگاه
آراد فروش کابل گاز پراید قیمت عمده
Company_Name خریدار لوازم شرکتی
Blog_Name لاستیک فنر لول جلو
پراید شرکتی آراد پارت فروش عمده لوازم یدکی پراید کف قیمت
Blog_Tagline سیم کاپوت کش پراید شرکتی موجود در فروشگاه آراد فروش سیم کاپوت
پراید قیمت عمده
Blog_About 49 year-old Senior Editor Douglas Viollet, hailing from Leduc enjoys watching movies like I Am Love (Io sono l’amore) and Puzzles.
Took a trip to Phoenix Islands Protected Area and
drives a Ferrari 250 GT Series I Cabriolet.
Article_title دسته موتور شماره 1
پراید شركتی پخش عمده دسته موتورهای پراید کف قیمت بازار لوازم یدکی
Article_summary برای این کار میتوانید از سایتهای معتبر حدود قیمت لوازم نو را استعلام بگیرید و با توجه
به میزان سلامت، ویژگیهایی که لوازم
شما دارد و کارایی آنها میانگین قیمتی را در نظر بگیرید.
Article درمورد ارسال اتاق باید توافق کنیم اگر نیاز به
تحویل نباشه در تهران فوری تحویل وانت میدیم براتون بیاره .
بنابر این قیمت نهایی اتاق نیسان پادرا فقط موقع صدور
فاکتور ، تحویل و تسویه مشخص میشود.
اطلاعات شرکت ها را در لینکداین و یا صفحه
توییتر ببینید پیج اینستاگرام و کانال تلگرام را هم حتما دنبال کنید.
به غیر از وب سایت در هر زمان میتونید
عکس فرمان پیکاپ را در پینترست خارجی ها را در فیس بوک ببینید.
تکنولوژیهای بکار رفته در ماشین لباسشوییهای سامسونگ، این ابزارهای روزمره را
به ابزارهایی پیشرفته و کارآمد تبدیل کردهاند.
از تکنولوژی EcoBubble که باعث کاهش مصرف انرژی و آب شستشو میشود، تا تکنولوژی Smart Control که به کاربر
اجازه میدهد از راه دور ماشین لباسشویی را کنترل کند، همهی این ویژگیها
باعث محبوبیت ماشین لباسشوییهای سامسونگ در بازار شدهاند.
تکنولوژی EcoBubble ماشین لباسشویی سامسونگ؛ یکی
از نقاط قوت ماشین لباسشوییهای سامسونگ است.
با استفاده از این تکنولوژی، ماشین لباسشویی
قادر به تبدیل مواد شویندهی مایع به
حبابهای کوچک و نرم میشود که به راحتی وارد بافت لباسها نفوذ کرده و
کثیفیها را بهطور موثری از لباسها جدا کرده و شستشو میدهد.
About_Me 44 year-old Office Assistant IV Bevon Edmundson, hailing from Oromocto enjoys watching movies like
“Christmas Toy, The” and Graffiti. Took a
trip to Royal Exhibition Building and Carlton Gardens and drives a Ferrari 412S.
About_Bookmark 29 yr old Financial Analyst Travus Kinzel, hailing from Lacombe enjoys watching movies like Conan the Barbarian and Mountaineering.
Took a trip to Su Nuraxi di Barumini and drives a Beretta.
Topic خریدار لوازم شرکتی
pokerdom реальный игровые автоматы покердом слоты покер дом
pokerdom реальный игровые автоматы покердом слоты покер дом
лицензионное казино реальный игровые автоматы покердом покер дом
https://t.me/s/AceInTheHoleDom
интернет казино игровые автоматы
https://t.me/s/internet_kazino_igrovye_avtomatt
Список казино онлайн.
Список казино онлайн.
pokerdom проверяем онлайн казино покердом казино покердом
pokerdom проверяем онлайн казино покердом казино покердом
покердом как вынести казино с нулевым балансом покердом
покердом как вынести казино с нулевым балансом покердом
игровые автоматы онлайн на реальные деньги
https://t.me/s/igrovyyeavtomaty_besplatno
мобильное казино на рубли
мобильное казино на рубли
казино. на. рубли.
https://t.me/s/kazinona_rybli
лицензионное pokerdom обзор игровые покердом слоты покер дом
https://t.me/s/PokerDomProphet
Вход в ПокерДом
Вход в ПокерДом
играть в игровые автоматы бесплатно
играть в игровые автоматы бесплатно
рейтинг казино на рубли
рейтинг казино на рубли
промокод покердом 2023
https://t.me/s/pokerdom_promokodi
лучшие. онлайн. казино. на. рубли.
лучшие. онлайн. казино. на. рубли.
Верификация на ПокерДоме
https://t.me/s/verifikaciya_PokerDom
https://kamagra.icu/# Kamagra Oral Jelly
покердом казино отзывы
покердом казино отзывы
вулкан игровые автоматы на деньги
https://t.me/s/igrovyeavvtomaty_besplato
скачать покердом на деньги на андроид
https://t.me/s/skachat_pokerdom_na_dengi_na_an
в каких казино играть на рубли
https://t.me/s/Jackpot0_Hunter
удалить рекламу покердом
https://t.me/s/udalit_reklamu_pokerdom
лицензионное казино pokerdom реальный обзор покердом покер дом
лицензионное казино pokerdom реальный обзор покердом покер дом
скачать покердом на андроид apk
https://t.me/s/skachat_pokerdom_na_android_apk
азартные игровые автоматы бесплатно и без регистрации
https://t.me/s/igrovyeavttomaty_besplatno
п»їkamagra buy Kamagra cheap kamagra
казино онлайн рулетка на деньги рубли
казино онлайн рулетка на деньги рубли
разбор онлайн казино покердом и pokerdom зеркало покердом
https://t.me/s/PokerDomMoneymaker
удалить покердом
удалить покердом
Скачать ПокерДом здесь
Скачать ПокерДом здесь
игровые автоматы скалолаз
https://t.me/s/igrovye_avtomaty_skalolaz
играть в онлайн казино на рубли
https://t.me/s/CasinoCardWhisperer
лицензионное pokerdom реальный игровые автоматы покердом слоты дом
https://t.me/s/pokerdom_licenziya
PokerDom на телефон
https://t.me/s/teleaonPokerDom
русское казино онлайн на рубли
https://t.me/s/ruskoekazino_narybli
самые лучшие игровые автоматы
https://t.me/s/igrovyeavtomaty_samyelychie
топ казино на рубли
https://t.me/s/RouletteRicochet
казино pokerdom реальный обзор покердом слоты покер дом
https://t.me/s/pokerdom_kazik
Скачать ПокерДом на Андроид
https://t.me/s/skachatPokerdom_prilozhenie
русские казино на рубли
русские казино на рубли
игровые автоматы онлайн казино
https://t.me/s/igrovye_avtomaty_onlajn_kazino
честные онлайн казино на рубли
честные онлайн казино на рубли
pokerdom обзор игровые автоматы покердом слоты покер дом
https://t.me/s/pokerdom_igrovyie
скачать. покердом. на. компьютер.
скачать. покердом. на. компьютер.
Amazing! Itѕ truⅼy awesome post, Ӏ һave ցot muⅽh cleɑr idea regarding fгom thіs article.
Μy blog post sofa bed with storage
лютый х в crash стратегия игры на pokerdom покердом краш казино
лютый х в crash стратегия игры на pokerdom покердом краш казино
игровые автоматы онлайн бесплатно демо
https://t.me/s/igrovye_avtomaty_onlajn_besplatn
хм2 и покердом
хм2 и покердом
русские онлайн казино на деньги рубли
русские онлайн казино на деньги рубли
скачать покердом на андроид с официального сайта
https://t.me/s/skachat_pokerdom_na_android_s_of
лучшее казино онлайн на рубли с моментальным выводом денег
лучшее казино онлайн на рубли с моментальным выводом денег
игровые автоматы онлайн без регистрации
https://t.me/s/igrovye_avtomaty_onlajn
топ онлайн казино на рубли
топ онлайн казино на рубли
ПокерДом с официального
ПокерДом с официального
Аврора Казино
официальный сайт Аврора Казино
Реклама ПокерДом
Реклама ПокерДом
pin up игровые автоматы за деньги
https://t.me/s/igrovyeavtomaty_nadengi
онлайн казино на реальные деньги рубли
https://t.me/s/onlajn_kazino_na_realnyedengi
АПК на андроид Покердом
https://t.me/s/skachat_apk_PokerDom
Разбор ПокерДом, обзор зеркала
Разбор ПокерДом, обзор зеркала
игровые автоматы играть на реальные деньги
https://t.me/s/igrovye_avtomaty_igrat_na_realny
популярные казино на рубли
популярные казино на рубли
покердом пароли
https://t.me/s/RoyalFlushMaestro
проверяем онлайн казино покердом обзор казино покердом
https://t.me/s/proveryaem_kazino_pokerdom
игровые автоматы эльдорадо
https://t.me/s/igrovyeavtomaty_igrata
честное онлайн казино на реальные деньги рубли
честное онлайн казино на реальные деньги рубли
лицензионное pokerdom реальный обзор покердом слоты покер дом
лицензионное pokerdom реальный обзор покердом слоты покер дом
buy stromectol scabies online – Educational institutions should teach students how to recognize signs of medication misuse and addiction
pokerdom и казино покердом казино вывод казино покердом
https://t.me/s/PokerDomVirtuoso
играть в игровые автоматы
https://t.me/s/igrovyeavtomaty_igrat
казино играющие на рубли
казино играющие на рубли
Приложение ПокерДом
Приложение ПокерДом
покердом вход
https://t.me/s/pokerdom_vhod1
игровые автоматы бездепозитный бонус за регистрацию
игровые автоматы бездепозитный бонус за регистрацию
Fantastic post however I was wondering if you
could write a litte more on this topic? I’d be very thankful if you could elaborate a little bit further.
Thanks!
плей фортуна онлайн казино на рубли
плей фортуна онлайн казино на рубли
покердом. казино. играть. онлайн.
покердом. казино. играть. онлайн.
как избавиться от рекламы покердом
как избавиться от рекламы покердом
играть бесплатно без регистрации в игровые автоматы
играть бесплатно без регистрации в игровые автоматы
лучшие казино на рубли
https://t.me/s/luchshie_kazino_na_rubli
покердом детальная слоты покердом бонус за регистрацию
https://t.me/s/PokerDomCardsharp
ВОЙТИ НА ПОКЕРДОМ
ВОЙТИ НА ПОКЕРДОМ
ПокерДом Ставки
https://t.me/s/pokerdomstavki
бесплатные игры казино игровые автоматы
https://t.me/s/igrovieavtomaty_igry
покердом честная проверка pokerdom pokerdom бонус
https://t.me/s/pokerdom_bonuss
казино рояль онлайн играть на деньги рубли
казино рояль онлайн играть на деньги рубли
ПокерДом Украина
ПокерДом Украина
покердом скачать на андроид
https://t.me/s/pokerdom_skachat_na_android
проверяем румы казино покердом обзор казино покердом
проверяем румы казино покердом обзор казино покердом
игровые автоматы играть бесплатно без регистрации и смс онлайн вулкан
https://t.me/s/igrovieavtomaty_igratbesplatni
покердом онлайн все еще лучшие 2022 покердом pokerdom
покердом онлайн все еще лучшие 2022 покердом pokerdom
ПокерДом 777
https://t.me/s/pokerDom_udacha
игровые автоматы играть бесплатно прямо сейчас
https://t.me/s/novye_avtomatyigrovye
Казино ПокерДом ПромоКод
https://t.me/s/pokerDomPromoKod
пин ап игровые автоматы на деньги
https://t.me/s/igrovieavtomaty_besp
pokerdom реальный обзор игровые автоматы покердом покер дом
https://t.me/s/DomPokerLegend
лицензионное казино обзор игровые автоматы покердом слоты дом
https://t.me/s/PokerDomStrategist
новые игровые автоматы
https://t.me/s/noviue_igrovieavtomaty
покердом официальный сайт вход
покердом официальный сайт вход
игровые автоматы играть
https://t.me/s/igratv_igrovieavtomaty
покердом скачать приложение на айфон
https://t.me/s/pokerdom_skachat_prilozhenie_na
покердом джипситим
покердом джипситим
лицензионное казино обзор автоматы покердом слоты покер дом
https://t.me/s/licenzionnyj_pokerdom
покердом.
покердом.
демо игровые автоматы
демо игровые автоматы
покердом скачать на андроид бесплатно
https://t.me/s/pokerdom_skachat_na_android_besp
покердом вход pokerdom official
покердом вход pokerdom official
игровые автоматы играть бесплатно на 5000
https://t.me/s/igrovyy_avtimatybesplatn
покердом. зеркало. www. pokerdomo. funundefined.
покердом. зеркало. www. pokerdomo. funundefined.
pokerdom проверяем топовые румы покердом обзор покердом
https://t.me/s/HighStakesDom
покердом скачать клиент на ios
https://t.me/s/pokerdom_skachat_klient_na_ios
разбор онлайн покердом тест и проверка обзор покердом
разбор онлайн покердом тест и проверка обзор покердом
новые бесплатные игровые автоматы
https://t.me/s/igrovyesloty_onlain
покердом олег
покердом олег
Fantastic goods from you, man. I have bear in mind your stuff previous to and
you’re simply extremely excellent. I really like what you’ve obtained right here, certainly like what you’re
saying and the way by which you assert it. You make it
entertaining and you still take care of to stay it sensible.
I cant wait to read much more from you. This is actually a
tremendous web site.
покердом софт
покердом софт
игровые автоматы украина
игровые автоматы украина
покердом скачать ios
https://t.me/s/pokerdom_skachat_ios
hm2 для покердом
hm2 для покердом
игровые автоматы играть бесплатно онлайн
игровые автоматы играть бесплатно онлайн
покердом андроид
https://t.me/s/pokerdom_android1
игровые автоматы онлайн на деньги
игровые автоматы онлайн на деньги
покердом скачать андроид
https://t.me/s/pokerdom_skachat_android
I don’t know whether it’s just me or if everybody else experiencing problems with your website.
It appears as if some of the written text on your content
are running off the screen. Can somebody else please comment and let me know if this
is happening to them too? This may be a problem with my internet browser because I’ve had this happen before.
Thanks
музыка покердом
музыка покердом
Hi, Neat post. There is an issue together with your site in web
explorer, could check this? IE nonetheless is the marketplace
chief and a big portion of people will omit your excellent writing due to this problem.
игровые автоматы обезьянки скачать бесплатно
игровые автоматы обезьянки скачать бесплатно
лицензионное казино pokerdom обзор игровые покердом слоты дом
https://t.me/s/PokerDomAceRider
пароль на фрироллы покердом
https://t.me/s/PokerDomShowdown
игровые автоматы играть бесплатно без регистрации демо
https://t.me/s/demo_igrovueavtomaty
pokerdom зеркало сайта покердом
pokerdom зеркало сайта покердом
скачать игровые автоматы на андроид без интернета
https://t.me/s/igrovyeavtomaty_naandroid
онлайн казино на деньги на рубли
https://t.me/s/onlayn_kazinonarybli
welcome telegram freebuy пароль покердом
welcome telegram freebuy пароль покердом
пин ап игровые автоматы
https://t.me/s/CasinoRoyaltyX
покердом. промокод. на. сегодня.
покердом. промокод. на. сегодня.
игровые автоматы книжки
игровые автоматы книжки
Оф сайт регистрация на покерДоме
https://t.me/s/pokerdom_registraciyanasaite
игровые автоматы москва
https://t.me/s/CasinoMogulMastermindElite
лицензионное pokerdom обзор автоматы покердом слоты покер дом
лицензионное pokerdom обзор автоматы покердом слоты покер дом
игровые автоматы бесплатно играть
https://t.me/s/igrovueavtomaty_skachat
покердом не работает 2017
https://t.me/s/PokerDomProwess
Русские КАЗИНО на деньги.
Русские КАЗИНО на деньги.
игровые автоматы онлайн бесплатно без регистрации
игровые автоматы онлайн бесплатно без регистрации
игровые автоматы демо игра
игровые автоматы демо игра
статистика покердом
статистика покердом
Good day! I simply want to give you a huge thumbs up for your excellent info you have got here on this post.
I’ll be returning to your site for more soon.
Приложение ПокерДом
https://t.me/s/pokerdomprilozhenie
игровые автоматы пирамида
игровые автоматы пирамида
игровые автоматы играть на деньги
https://t.me/s/CasinoConquerorAcehttps://t.me/s/CasinoConquerorAce
лицензионное казино игровые автоматы покердом слоты покер дом
лицензионное казино игровые автоматы покердом слоты покер дом
игровые автоматы леон на деньги скачать
игровые автоматы леон на деньги скачать
покердом не работает
покердом не работает
Покердом ЗЕРКАЛО
https://t.me/s/mobilnoezerkalo_PokerDom
игровые автоматы на реальные деньги
https://t.me/s/CasinoCashMogulEmpireX
верификация на покердом
верификация на покердом
покердом проверка казино казино слоты покердом за регистрацию
https://t.me/s/DomPokerWhiz
ПокерДом на телефон.
https://t.me/s/pokerDomNaTelefon
лучшее казино на рубли
лучшее казино на рубли
Great blog you have got here.. It’s difficult to find high quality writing like
yours these days. I really appreciate people like you! Take care!!
игровые автоматы онлайн бесплатно без регистрации слотозал
игровые автоматы онлайн бесплатно без регистрации слотозал
pokerdom топовые румы казино покердом казино покердом
pokerdom топовые румы казино покердом казино покердом
Good replies in return of this difficulty with solid arguments and describing all about that.
покердом детальная казино pokerdom казино покердом бонус за
покердом детальная казино pokerdom казино покердом бонус за
Покердом на Андроид
https://t.me/s/pokerdom_naandroid_narealnye
лучшие онлайн казино россии на рубли
лучшие онлайн казино россии на рубли
игровые автоматы адмирал играть бесплатно
игровые автоматы адмирал играть бесплатно
онлайн казино покердом отзывы
https://t.me/s/pokerdom_otzyvyu
покердом как с нулевым балансом лайфхаки покердом бонус
https://t.me/s/DomPokerMogul
Покердом приложение БЕСПЛАТНО
Покердом приложение БЕСПЛАТНО
лучшие онлайн казино на рубли
лучшие онлайн казино на рубли
игровые автоматы pin up
игровые автоматы pin up
покердом честная проверка казино pokerdom pokerdom
покердом честная проверка казино pokerdom pokerdom
покердом ошибка сети
https://t.me/s/DomPokerMaestro
PokerDom Android
PokerDom Android
лучшее онлайн казино на рубли
https://t.me/s/luchee_kazinonarybli
партнерская ссылка на покердом
https://t.me/s/CardShark_Dom
игровые автоматы играть онлайн
игровые автоматы играть онлайн
покердом бездепозитный бонус 2018
https://t.me/s/pokerdom_besdeposit
magnificent publish, very informative. I’m wondering why the other experts of this
sector do not realize this. You should continue your writing.
I am confident, you have a great readers’ base already!
Покердом скачать с оф сайта
Покердом скачать с оф сайта
pokerdom слоты и бонусы покердом слоты вывод денег покердом
https://t.me/s/CardSharkDom
казино онлайн играть на деньги рубли
https://t.me/s/kazino_onlainnarybli
играть в игровые автоматы бесплатно с бонусами
https://t.me/s/CasinoMogulChampion
бонус за депозит покердом
бонус за депозит покердом
покердом официальный сайт на реальные деньги скачать
https://t.me/s/PokerDomJuggernaut
игровые автоматы играть бесплатно без регистрации и смс
https://t.me/s/CasinoFortuneMaestro
казино на рубли онлайн
казино на рубли онлайн
игровые автоматы без регистрации
https://t.me/s/bezplatnye_avtomaty
как пополнить покердом
https://t.me/s/pokerdom_popolnenieee
Thankfulness to my father who stated to me concerning this webpage,
this webpage is in fact amazing.
покердом как использовать бонусный счет
покердом как использовать бонусный счет
игровые автоматы слоты
игровые автоматы слоты
скачать игру игровые автоматы
https://t.me/s/BetBlitzWhizKid
список казино на рубли
https://t.me/s/kazinonarybli_lychie
промокод покердом депозит
https://t.me/s/pokerdom_depozitt
покердом пароль
https://t.me/s/CardSlingerDom
проверяем румы онлайн казино покердом казино покердом
https://t.me/s/PokerDomDynamo
I for all time emailed this blog post page to all my associates, for the reason that if like to read it afterward my friends will too.
игровые автоматы играть бесплатно без регистрации и смс прямо сейчас
игровые автоматы играть бесплатно без регистрации и смс прямо сейчас
казино рулетка онлайн на деньги рубли
https://t.me/s/kazino_narublionlain
покердом бездепозитный бонус 10$
покердом бездепозитный бонус 10$
pin-up игровые автоматы
https://t.me/s/CardSharkVirtuosoPro
покердом ошибка
https://t.me/s/PokerDomAllIn
казино на рубли честное
казино на рубли честное
скачать клиент покердом на пк
https://t.me/s/pokerdom_klientpc
ok google игровые автоматы бесплатные
ok google игровые автоматы бесплатные
бездепозитный бонус $10 на покердом
бездепозитный бонус $10 на покердом
обзор казино покердом
обзор казино покердом
казино на рубли
https://t.me/s/kazinoha_narybliiy
лицензионное pokerdom реальный обзор игровые автоматы покердом дом
https://t.me/s/pokerdom_slicenziey
игровые автоматы pin-up
игровые автоматы pin-up
Мобильный ПокерДом
https://t.me/s/mobilnyi_pokErDom_skachat
играть в казино онлайн на рубли
играть в казино онлайн на рубли
скачать клиент покердом на пк
скачать клиент покердом на пк
играть бесплатно в игровые автоматы
играть бесплатно в игровые автоматы
Мобильная версия ПокерДом
Мобильная версия ПокерДом
игровые автоматы демо играть бесплатно пирамиды
игровые автоматы демо играть бесплатно пирамиды
покердом официальный зеркала аблепа
покердом официальный зеркала аблепа
пополнить счет в покердом
пополнить счет в покердом
Последняя версия ПокерДом
Последняя версия ПокерДом
лучшие игровые автоматы
https://t.me/s/avtomatiigrovie_lychie
покердом. скачать. на. деньги.
покердом. скачать. на. деньги.
покердом. промокод. 2023.
https://t.me/s/pokerdom_promoo
играть игровые автоматы
играть игровые автоматы
Клиент Покердом на телефон
https://t.me/s/klientPokerDomnaTelefon
установить игровые автоматы бесплатно
https://t.me/s/abtomatybesplatnye_igrat
покердом на планшет
https://t.me/s/DomPokerDealmaker
покердом вики
покердом вики
бесплатные игровые автоматы играть бесплатно без регистрации
бесплатные игровые автоматы играть бесплатно без регистрации
Клиент ПокерДом на телефон
https://t.me/s/klientPokerDomnatel
играть бесплатно игровые автоматы
https://t.me/RouletteRoyaltyGuru
Woah! I’m really digging the template/theme of this website.
It’s simple, yet effective. A lot of times
it’s very hard to get that “perfect balance” between superb usability and visual appearance.
I must say that you’ve done a superb job with this. Additionally,
the blog loads super quick for me on Internet explorer.
Exceptional Blog!
личный. кабинет. покердом.
https://t.me/s/pokerdom_kabinets
рейтинг лучших интернет казино на реальные деньги рубли
рейтинг лучших интернет казино на реальные деньги рубли
как убрать покердом
как убрать покердом
игровые автоматы демо версии играть бесплатно
https://t.me/s/avtomaty_demoversija
покердом орг
https://t.me/s/pokerdom_orge
Краш Казино стратегия ПокерДом
https://t.me/s/crashX_strategiyaPokerDom
интернет казино на рубли
интернет казино на рубли
лицензионное казино pokerdom обзор покердом слоты покер дом
https://t.me/s/AceOfSpadesDom
казино реальный обзор автоматы покердом слоты покер дом
https://t.me/s/pokerdom_igry
казино на реальные деньги на рубли
казино на реальные деньги на рубли
Играть ПокерДом
https://t.me/s/igrat_poKerDom
I’m extremely pleased to uncover this website. I need to to thank you for
ones time for this wonderful read!! I definitely savored every part of it
and i also have you saved to fav to look at new stuff on your web site.
вулкан игровые автоматы
https://t.me/DiceRollerSavantAce
бонусы gama casino
бонусы gama casino
проверенные казино на рубли
проверенные казино на рубли
покердом личный
покердом личный
игровые автоматы играть на деньги
игровые автоматы играть на деньги
казино вулкан на рубли
казино вулкан на рубли
обзор топ 3 россии покердом лучшие игры топ онлайн
https://t.me/s/DomPokerWizKid
казино гама зеркало
https://t.me/s/zerkalo_kazinogama
онлайн казино на рубли вулкан
онлайн казино на рубли вулкан
покердом тест и проверка pokerdom зеркало обзор покердом
покердом тест и проверка pokerdom зеркало обзор покердом
покердом azurewebsites
https://t.me/s/CardSharkSageDom
зеркало казино gama гама
зеркало казино gama гама
вулкан казино на рубли
вулкан казино на рубли
лицензионное казино pokerdom автоматы покердом слоты покер дом
лицензионное казино pokerdom автоматы покердом слоты покер дом
лучшее интернет казино на рубли
лучшее интернет казино на рубли
гама казино рабочее зеркало
https://t.me/s/zerkaligama_kazino
список лучших казино на рубли с моментальным выводом
https://t.me/s/uchshih_kazino_na_rubli
скачать покердом с официального сайта
https://t.me/s/DomPokerBlitzkrieg
ты сидишь дома смотришь сериал в покердом бы поиграл
https://t.me/s/CardCharmerDom
интернет казино топ рейтинг
https://t.me/s/top_reitingkazino
Greetings I am so excited I found your website, I really found you by mistake, while I was
browsing on Yahoo for something else, Anyhow I am here now and would just like to say thanks for a marvelous post and a all round interesting blog (I also love the theme/design), I
don’t have time to read through it all at the moment but I have book-marked it and also
included your RSS feeds, so when I have time I will be back to read a great deal
more, Please do keep up the great job.
Pretty nice post. I just stumbled upon your blog and wanted to say that I have really enjoyed
browsing your blog posts. In any case I will be subscribing to your rss feed and
I hope you write again soon!
топ интернет казино на рубли
топ интернет казино на рубли
покердом. казино. официальный. сайт.
https://t.me/s/DomPokerBlaze
Вывод бонусов ПокерДом
https://t.me/s/bonusyvyvod_casinoPokerDom
гама казино отзывы
гама казино отзывы
Howdy! This post could not be written much better!
Reading through this article reminds me of my previous roommate!
He constantly kept preaching about this. I am
going to send this article to him. Fairly certain he’ll have
a very good read. I appreciate you for sharing!
What’s up to all, how is everything, I think every one is
getting more from this web page, and your views are nice for new
people.
my web page http://superpremium2.premium4best.eu/
казино онлайн играть на деньги рубли список
https://t.me/s/SpinCitySultan
покердом. бесплатно.
покердом. бесплатно.
казино на деньги рубли
https://t.me/s/Bet_Blaster
gama casino вход
gama casino вход
покердом pokerdom casino
покердом pokerdom casino
казино c живыми дилерами на рубли
казино c живыми дилерами на рубли
Игровые автоматы ПокерДом
https://t.me/s/avtomatybesplatno_PokerDom
казино онлайн рейтинг лучших в россии
https://t.me/s/reiting_kazinorossii
СКАЧАТЬ АПК ПокерДом
https://t.me/s/apkPokerdom_skachat
играть онлайн казино на рубли
играть онлайн казино на рубли
покердом pokerdom
https://t.me/s/AceOfWinningDom
игровые автоматы рейтинг казино
https://t.me/s/reitingkazino_avtomaty
ПокерДом на Андроид
https://t.me/s/androidPokerDom_tut1
рулетка казино играть на рубли
https://t.me/s/ruletka_kazino_igrat_na_rubli
казино гама регистрация
казино гама регистрация
ПокерДом AndroiD
https://t.me/s/androidpokerDom_tut
казино онлайн рулетка на рубли
https://t.me/s/Roulette0Rider
казино онлайн на рубли
казино онлайн на рубли
gama casino registration
gama casino registration
рейтинг честных онлайн казино на рубли
https://t.me/s/reiting_kazinonarubli
онлайн казино рейтинги
https://t.me/s/SpinToWinAce
x casino россия
https://t.me/s/x_casino_rossiya
промокод казино гама
промокод казино гама
скачать бесплатно pin up казино на рубли
https://t.me/s/pinup_kazinohanarubli
топ рейтинг лучших казино
топ рейтинг лучших казино
рейтинг игровых казино
https://t.me/s/SpinToVictory
промокод гама казино
https://t.me/s/promokod_gamakazino
официальный сайт казино на рубли
официальный сайт казино на рубли
топ рейтинг казино
https://t.me/s/top_rejting_kazino1
рейтинг казино по отдаче
https://t.me/s/SpinAndWinPro
gama casino promo code
gama casino promo code
Лучшие казино на РУБЛИ!
https://t.me/s/luchshie_casino
топ казино года рейтинг казино топовые казино
https://t.me/s/top_kazino_rejting_kazino
рейтинг казино онлайн на деньги
рейтинг казино онлайн на деньги
гама казино онлайн
гама казино онлайн
Hello to every one, as I am in fact eager of reading this weblog’s post to
be updated daily. It includes fastidious data.
live казино баккара на рубли
live казино баккара на рубли
топ казино года рейтинг лицензионных казино казино
https://t.me/s/top_kazino_goda_rejting_licenzi
рейтинг бесплатных казино
https://t.me/s/SlotMachineMaestro
казино гама обзор
https://t.me/s/PokerDomSav
LIVE рулетка на рубли.
LIVE рулетка на рубли.
I don’t even understand how I stopped up here, however I believed
this post used to be good. I do not understand who you’re but definitely you’re going to a famous blogger
in case you are not already. Cheers!
топ казино года рейтинг казино онлайн казино
топ казино года рейтинг казино онлайн казино
лицензионные казино онлайн в россии рейтинг
лицензионные казино онлайн в россии рейтинг
официальные казино онлайн рейтинг
официальные казино онлайн рейтинг
казино на рубли с выводом
https://t.me/s/kezino_narubli_svyvodom
It’s actually very complex in this full of activity life to listen news on TV, therefore I just use world
wide web for that purpose, and take the latest
information.
топ 10 рейтинг лучших казино
https://t.me/s/SpinToFortune
лучший топ рейтинг казино онлайн
лучший топ рейтинг казино онлайн
рейтинг казино на реальные деньги онлайн
рейтинг казино на реальные деньги онлайн
you are in reality a excellent webmaster. The web site loading velocity is amazing.
It kind of feels that you’re doing any unique
trick. Furthermore, The contents are masterpiece.
you have done a wonderful job in this matter!
казино вулкан онлайн играть на деньги рубли
https://t.me/s/kazinovulkan_narubli
рейтинги интернет казино
рейтинги интернет казино
Superb write ups. Regards.
write my school paper for me essay writer best resume writing service atlanta
казино рейтинг онлайн
казино рейтинг онлайн
рейтинг лучших казино онлайн
https://t.me/s/rejting_luchshih_kazino_onlajn
You revealed that wonderfully!
best resume writing service 2015 how to advertise resume writing service essay writing service reviews
казино с живым дилером на рубли
казино с живым дилером на рубли
рейтинг. онлайн. казино.
https://t.me/s/RouletteRideer
гама казино официальный сайт вход
гама казино официальный сайт вход
Nicely put. With thanks!
essay writing service plagiarism change words in essay service essay
рейтинг лучших казино
рейтинг лучших казино
I like the helpful info you provide in your articles.
I’ll bookmark your blog and check again here frequently.
I am quite certain I will learn lots of new stuff right here!
Good luck for the next!
онлайн казино на рубли с выводом денег
онлайн казино на рубли с выводом денег
рейтинг онлайн казино с лицензией в россии
рейтинг онлайн казино с лицензией в россии
gama casino официальный сайт
gama casino официальный сайт
рейтинг лучших интернет казино
https://t.me/s/rejting_luchshih_internet_kazino
русские онлайн казино на рубли
https://t.me/s/kazinoshka_narubli
рейтинг топ 10 онлайн казино
рейтинг топ 10 онлайн казино
gama casino игровые автоматы
https://t.me/s/PokerD0mJourneyman
Incredible quite a lot of fantastic knowledge!
what is a good essay writing service best paper writing service professional custom essay writing service
Great goods from you, man. I’ve be mindful your stuff prior to and you’re just too wonderful.
I actually like what you’ve acquired right here, certainly like what you’re stating and
the best way during which you assert it. You make it entertaining and you continue to
care for to keep it sensible. I cant wait to learn much more from you.
That is really a tremendous web site.
рейтинг лучших игровых автоматов онлайн
рейтинг лучших игровых автоматов онлайн
казино рулетка на деньги рубли
казино рулетка на деньги рубли
Hello my loved one! I wish to say that this post is awesome, great written and include almost all vital infos. I’d like to see more posts like this .
рейтинг топ 10 казино
https://t.me/s/reiting_topkazino
gama casino промокод бездепозитный бонус
https://t.me/s/Poker1DomProwess
рейтинг казино с хорошей репутацией
https://t.me/s/rejting_kazino_s_horoshej
казино. онлайн. на. рубли.
казино. онлайн. на. рубли.
gama casino отзывы
https://t.me/s/P0kerDomMajesty
рейтинг сайтов казино
https://t.me/s/reiting_saitovkazino
рейтинг казино рунета
рейтинг казино рунета
казино. онлайн. рулетка. на. деньги. рубли.
https://t.me/s/kazinoonlain_narubli
интернет казино рейтинг лучших
https://t.me/s/kazino_rejting_luchih
рейтинг честных онлайн казино
рейтинг честных онлайн казино
рейтинг казино россии
https://t.me/s/rejting_kazino_rossii
казино на рубли вулкан
https://t.me/s/kazinoo_narybli
казино онлайн рейтинг
казино онлайн рейтинг
рейтинг топ казино
рейтинг топ казино
рейтинг казино рф
рейтинг казино рф
live казино покер на рубли
https://t.me/s/kazinonarybli_poker
Наша организация специализируется на
покупке, продаже и переработке
лома и отходов цветных и черных металлов,
а также прием металла в казани цена предоставлении услуг по демонтажу и вывозу
металлолома с объектов.
Широкий спектр услуг. Мы предлагаем полный комплекс услуг связанных с металлоломом: от демонтажа
и вывоза до переработки
и утилизации.
Специализированный персонал.
Наши специалисты обладают большим опытом работы с металлоломом и имеют все необходимые лицензии и сертификаты.
Собственный автотранспорт.
Мы располагаем собственным транспортом для вывоза металлолома,
что позволяет нам оперативно реагировать на запросы клиентов.
Выгодные цены. Мы стремимся предложить нашим клиентам максимально выгодные условия сотрудничества, устанавливая конкурентные цены на металлолом.
Индивидуальный подход.
Мы учитываем все пожелания и требования наших клиентов,
предлагая оптимальные решения для каждого конкретного случая.
казино онлайн рейтинг лучших интернет казино
казино онлайн рейтинг лучших интернет казино
рейтинг топ лучших казино
https://t.me/s/reitingluchish_kazino
рейтинг казино по честности
https://t.me/s/rejting_kazino_po_chestnosti
казино онлайн на деньги рубли
казино онлайн на деньги рубли
казино по рейтингу
казино по рейтингу
рейтинг российских казино
https://t.me/s/reiting_luchihkazino
рейтинг онлайн казино в украине
https://t.me/s/reiting_onlainkazino_vukraine
казино на рубли с минимальным депозитом
https://t.me/s/kazinonarybli_min
казино онлайн рейтинг лучших
казино онлайн рейтинг лучших
рейтинг онлайн казино на реальные деньги
https://t.me/s/reitingluchih_kazino
рейтинг онлайн казино
рейтинг онлайн казино
Howdy outstanding website! Does running a blog like this take
a great deal of work? I’ve very little expertise in computer programming but I had been hoping to
start my own blog in the near future. Anyhow, if you have any ideas or tips for new blog owners please share.
I know this is off subject nevertheless I just
needed to ask. Cheers!
онлайн казино на рубли минимум 1 руб
онлайн казино на рубли минимум 1 руб
казино гама
казино гама
рейтинг онлайн казино по выплатам
рейтинг онлайн казино по выплатам
рейтинг онлайн казино 2023
https://t.me/s/reiting_onlainkazino2023
казино на рубли с моментальным выводом денег
https://t.me/s/kazinonarubli_svuvodom
Heya i am for the primary time here. I came across this board and I
to find It truly helpful & it helped me out much. I hope to give one thing again and help others like you helped me.
гама казино вход
https://t.me/s/kazinogama_vhod
рейтинг самых лучших онлайн казино
рейтинг самых лучших онлайн казино
рейтинг лучщих онлайн казино
https://t.me/s/reiting_onlainkazino
казино с маленькими ставками на рубли
казино с маленькими ставками на рубли
гама казино зеркало рабочее на сегодня
https://t.me/s/kazino_gamasegodnia
рейтинг онлайн казино россии
https://t.me/s/reiting_kazinoonlain
казино онлайн играть на реальные деньги рубли
казино онлайн играть на реальные деньги рубли
рейтинг онлайн казино мира
рейтинг онлайн казино мира
гама казино регистрация
https://t.me/s/kazino_gama_registracija
рейтинг онлайн казино на рубли
рейтинг онлайн казино на рубли
обзор казино онлайн на рубли
https://t.me/s/kazinonarubli_obzory
рейтинг новых казино
рейтинг новых казино
гама казино промокод
https://t.me/s/kazinogama_promokod
рейтинг. казино. на. деньги.
https://t.me/s/reitingkazino_nadengi
казино рулетка онлайн на деньги рубли с минимальным депозитом
https://t.me/s/kazinonarubli_mindep
рейтинг новых игровых автоматов
рейтинг новых игровых автоматов
гама казино официальный сайт
гама казино официальный сайт
рейтинг самых лучших казино
https://t.me/s/reitingkazino_luchie
Thanks for the auspicious writeup. It in fact was once a
amusement account it. Glance advanced to more delivered agreeable from you!
However, how can we keep up a correspondence?
live казино блэкджек на рубли
live казино блэкджек на рубли
рейтинг надежных онлайн казино
рейтинг надежных онлайн казино
обзор casino gama
обзор casino gama
рейтинг онлайн казино с лицензией
рейтинг онлайн казино с лицензией
казино онлайн бесплатно играть на виртуальные деньги или рубли
https://t.me/s/kazino_narealrubli
казино гама играть
казино гама играть
рейтинг мобильных онлайн казино
https://t.me/s/reiting_mobykazino
Hello I am so thrilled I found your weblog, I really found you by accident, while I
was searching on Bing for something else, Anyhow I am here now and would just like to say thanks for a tremendous post and a
all round exciting blog (I also love the theme/design), I don’t have time to
browse it all at the moment but I have bookmarked
it and also added in your RSS feeds, so when I have
time I will be back to read more, Please do keep up the
excellent work.
рейтинг честности онлайн казино
рейтинг честности онлайн казино
казино. на. рубли. онлайн.
https://t.me/s/kazinoha_narybli
Hi there colleagues, nice paragraph and fastidious
urging commented here, I am actually enjoying by these.
интернет казино рейтинг
интернет казино рейтинг
рейтинг лучших лицензионных казино
рейтинг лучших лицензионных казино
рейтинг честных казино онлайн
https://t.me/s/reiting_chestnyhkazinoh
казино буи онлайн казино на рубли
казино буи онлайн казино на рубли
игровое казино гама
https://t.me/s/igrovoe_gamakazino
рейтинг казино в россии
рейтинг казино в россии
I enjoy what you guys are up too. Such clever work and exposure!
Keep up the amazing works guys I’ve included you guys to blogroll.
рейтинг самых честных онлайн казино
рейтинг самых честных онлайн казино
Обзор казино на рубли
Обзор казино на рубли
игровые автоматы рейтинг
https://t.me/s/igrovieavtomaty_reiting
рейтинг казино на реальные деньги
рейтинг казино на реальные деньги
рейтинг честных казино
https://t.me/s/reiting_chestnihkazino
как играть интернет казино на рубли
как играть интернет казино на рубли
gama casino играть
gama casino играть
рейтинг онлайн казино по выплатам в украине
рейтинг онлайн казино по выплатам в украине
рейтинг онлайн казино на деньги
рейтинг онлайн казино на деньги
интернет казино на реальные деньги рубли
https://t.me/s/internet_kazino_na_realnye_dengi
гама казино зеркало
гама казино зеркало
рейтинг онлайн казино по выплатам и отзывам
рейтинг онлайн казино по выплатам и отзывам
рейтинг онлайн казино на деньги
рейтинг онлайн казино на деньги
играть на рубли в казино
играть на рубли в казино
gama casino promo
https://t.me/s/gama_kazinopromo
рейтинг live казино
рейтинг live казино
рейтинг лучших онлайн казино на реальные деньги
https://t.me/s/kazinoreiting_nadengi
играть. в. казино. на. рубли.
https://t.me/s/igratnarubli_vkazino
гама казино официальный зеркало
гама казино официальный зеркало
рейтинги онлайн казино
рейтинги онлайн казино
рейтинг надежных казино
рейтинг надежных казино
Онлайн играть в казино!
Онлайн играть в казино!
gama casino играть бесплатно
gama casino играть бесплатно
топ 10 казино онлайн рейтинг лучших
https://t.me/s/CasinoMogulll
рейтинг казино интернет
рейтинг казино интернет
гама казино
гама казино
gama casino ru
gama casino ru
топ 10 казино онлайн рейтинг лучших интернет казино
https://t.me/s/CasinoDazzle
рейтинг лучших лицензированных казино
рейтинг лучших лицензированных казино
онлайн казино на рубли рулетка
https://t.me/s/Dice_RollingChamp
gama casino
https://t.me/s/gama_casinoonline
рейтинги казино онлайн
https://t.me/s/CasinoCashFlw
You could certainly see your enthusiasm in the work you write.
The world hopes for even more passionate writers such as
you who aren’t afraid to mention how they believe. All the time go after your heart.
рейтинг казино 2023
https://t.me/s/reitingkazino_2023
мультигаминатор клуб интернет казино на рубли
https://t.me/s/club_kazinonadengi
gama casino промокод
https://t.me/s/gama_casinogame
топ интернет казино рейтинг
топ интернет казино рейтинг
рейтинг интернет казино
https://t.me/s/reiting_inetkazino
самые честные казино онлайн на рубли
самые честные казино онлайн на рубли
обзор gama casino
обзор gama casino
топ 10 рейтинг казино
https://t.me/s/BetMaverick
рейтинг мобильных казино
https://t.me/s/mobilniyreyning_kazino
казино с живыми дилерами на рубли
https://t.me/s/CasinoTreasureHunt
казино рейтинг лучших топ казино лучшее казино
https://t.me/s/DomPoker_Mystic
топ 10 казино онлайн рейтинг
https://t.me/s/BetBillionaie
обзор и рейтинг казино
обзор и рейтинг казино
Казино на рубли с выводом
Казино на рубли с выводом
промокод на гама казино
https://t.me/s/DomPoker_Maestro
Онлайн казино на РУБЛИ!
Онлайн казино на РУБЛИ!
рейтинг интернет казино по выплатам
рейтинг интернет казино по выплатам
gama casino зеркало
https://t.me/s/DomPokerChamp1on
Казинолайв на Рубли
https://t.me/s/casinonarubli_live
рейтинг интернет казино в россии
рейтинг интернет казино в россии
gama casino регистрация
gama casino регистрация
онлайн казино вулкан на рубли
онлайн казино вулкан на рубли
рейтинг лучших онлайн казино на деньги
https://t.me/s/kazino_reitingnadengi
casino vasco da gama
casino vasco da gama
онлайн казино на рубли отзывы
онлайн казино на рубли отзывы
рейтинг лучших онлайн казино
рейтинг лучших онлайн казино
casino gama
casino gama
покердом 28
https://t.me/s/pokerdom_28
лучшее казино на рубли список лучших
https://t.me/s/CardSharkLegend
рейтинг казино онлайн
https://t.me/s/JackpotHunterr
лицензионное казино онлайн рейтинг лучших
https://t.me/s/CardWizard_Dom
лучшие интернет казино на рубли
лучшие интернет казино на рубли
gama casino registration official
https://t.me/s/CardSharkSageD0m
рейтинг интернет казино онлайн
https://t.me/s/inetkazino_reitingonlain
Booi казино онлайн!
https://t.me/s/booiCasinonaRubli
gama casino бездепозитный бонус
gama casino бездепозитный бонус
рейтинг казино игровые автоматы
рейтинг казино игровые автоматы
лучшее казино онлайн на рубли
https://t.me/s/Bet_Maven
лучшие онлайн казино рейтинг
https://t.me/s/Ace_OfWinningDom
рейтинг казино онлайн с контролем честности
рейтинг казино онлайн с контролем честности
приложение онлайн казино на реальные деньги рубли
приложение онлайн казино на реальные деньги рубли
http://withoutprescription.guru/# cialis without a doctor’s prescription
бонусы казино гама
бонусы казино гама
рейтинг казино онлайн бесплатно
рейтинг казино онлайн бесплатно
лучшее казино онлайн на рубли с моментальным выводом
лучшее казино онлайн на рубли с моментальным выводом
brillx casino
brillx casino
Играя на Brillx Казино, вы можете быть уверены в честности и безопасности своих данных. Мы используем передовые технологии для защиты информации наших игроков, так что вы можете сосредоточиться исключительно на игре и наслаждаться процессом без каких-либо сомнений или опасений.Бриллкс Казино — это не просто игра, это стиль жизни. Мы стремимся сделать каждый момент, проведенный на нашем сайте, незабываемым. Откройте для себя новое понятие развлечения и выигрышей с нами. Brillx — это не просто казино, это опыт, который оставит след в вашем сердце и кошельке. Погрузитесь в атмосферу бриллиантового азарта с нами прямо сейчас!
онлайн казино рейтинг лучших
https://t.me/s/CasinoRoyale_Pro
казино франк на рубли
https://t.me/s/RouletteRanger
рейтинг игровых автоматов
https://t.me/s/CasinoCash0Wizard
гг покерок
http://uid.me/kirill_berg#
PokerOK предлагает множество вариаций покера, начиная от традиционных и до совершенно экзотических. Здесь вы найдете Texas Hold’em, Omaha, 7 Card Stud, и многие другие варианты, которые даже вряд ли вам когда-либо встречались. Но это лишь вершина айсберга — PokerOK радует своих гостей также турнирами на любой вкус и уровень мастерства.Скачать клиент для игры в покер на PokerOK – значит обрести билет в мир интриг и увлекательных раундов. Насладитесь моментами напряжения и волнения, когда решение принимается в одно мгновение, а карты скрывают последние тайны своих обладателей. Здесь каждая партия – это как дуэль между стратегами, где искусство блефа и анализа сливаются в захватывающем танце.
Excellent beat ! I wish to apprentice while you amend your site,
how can i subscribe for a blog site? The account aided me a acceptable deal.
I had been tiny bit acquainted of this your broadcast provided bright clear idea
рейтинг казино по версии игроков
рейтинг казино по версии игроков
Have you ever thought about writing an e-book or guest authoring on other sites?
I have a blog based upon on the same subjects you discuss and would love to have you
share some stories/information. I know my readers would enjoy your
work. If you are even remotely interested, feel free to send me an email.
gama casino
http://mastrerkon.ru/forum/viewtopic.php?f=27&t=10276
Играть в Gama Casino – это не просто казино, это путешествие в мир азартных мечтаний, где каждый спин – это новый поворот в сюжете вашей игры. Игровые автоматы России откроют перед вами безграничные возможности для выигрыша и развлечения. Каждая машина в Gama Casino – это как глава в увлекательной книге, наполненной сюрпризами и азартом.Итак, если вы ищете вход на официальный сайт, где можно играть бесплатно и на русском языке, ваш выбор однозначно — Gama Casino. Гама Казино сделает ваше путешествие в мир азарта по-настоящему незабываемым. Присоединяйтесь к нам сейчас и откройте дверь в азартное будущее прямо сейчас!
рейтинг 10 лучших онлайн казино
https://t.me/s/Casino_0Mogul
Vavada casino online
https://app.opyrus.com/members/kyuafs/
Для ценителей азарта и риска, для тех, кто ищет настоящие адреналиновые ощущения, Казино Вавада подготовило специальные разделы с карточными играми и рулеткой. Здесь каждая ставка – это шанс поймать удачу за хвост и уйти с внушительным выигрышем.Vavada Casino — это не только игры, но и атмосфера настоящего казино, перенесенная в онлайн пространство. Вас ждут уникальные слоты-онлайн с захватывающей графикой и реалистичными звуками, словно вы находитесь в центре азартного мира.
Thanks for any other informative website. Where
else may I get that kind of info written in such a perfect approach?
I’ve a challenge that I’m simply now operating on, and I have been at the
look out for such information.
независимый рейтинг онлайн казино
независимый рейтинг онлайн казино
cat casino сайт
http://jac-club.ru/profile.php?section=identity&id=7897
Добро пожаловать на официальный портал азартных развлечений 2023 года — Cat Casino, лучшее место для тех, кто ищет возможность скачать игровые автоматы и насладиться их разнообразием, играя онлайн! Откройте двери в захватывающий мир азарта вместе с Кэт Казино, где каждый спин барабанов — это шанс поймать удачу за хвост и потрясти её до последней фишки.Cat Casino – твой верный спутник в мире азарта! В 2023 году этот официальный сайт рад представить тебе уникальную возможность скачать игровые автоматы и окунуться в водоворот бесконечных развлечений прямо на своем устройстве. Ощути дыхание азарта в каждом вращении барабанов, будь в центре событий с Cat Casino, Кэт Казино.
Thank you for every other great article. The place else may anybody get that type of
information in such a perfect method of writing?
I’ve a presentation next week, and I’m on the search for such information.
Helpful write ups. Regards!
red dog casino promo codes no deposit bonus codes for red dog casino casino game real money
рейтинг игровых казино онлайн
рейтинг игровых казино онлайн
Many thanks! I like it.
enchanted casino login https://red-dogcasino.online/ akilies the game
онлайн рейтинг казино
https://t.me/s/CardSharkGambler
ggpokerok скачать на андроид
https://smorodina.com/blogs/aumso/ofitsialnyy-sayt-ggpokerok
PokerOK – это платформа, которая говорит “да” вашим амбициям и страсти к победе. Скачайте клиент PokerOK и войдите в уникальный мир tурниров, акций и бесконечных возможностей. Это ваш шанс стать частью элитного покерного сообщества, где каждая игра – шаг к завоеванию вершины.Чтобы присоединиться к увлекательному миру PokerOK, просто перейдите на официальный сайт, где вас ждет возможность скачать клиент для игры в покер. С ним вы окунетесь в виртуальное путешествие по захватывающему миру карт и фишек, где каждый ваш ход анализируется и обдумывается до мельчайших деталей.
Wonderful forum posts. Many thanks.
online casino craps btc casino roulette online real money
Hello, just wanted to mention, I enjoyed this blog post.
It was practical. Keep on posting!
рейтинг казино по отзывам
рейтинг казино по отзывам
gama casino играть
https://kadrsov.ru/forum/tema/gossluzhashchim-kazakhstana-mogut-razreshit-dopolnitelnyy-zarabotok
Игровые автоматы в России набирают обороты благодаря Gama Casino. Наша платформа собрала в себе богатство игровых вариаций — от традиционных классических слотов до передовых трехмерных автоматов. Это как путешествие во времени, где вы можете выбрать, с какой эпохой вы хотите встретиться, и Гама Казино сделает всё остальное.Забудьте о рутине и суете, потому что на Gama Casino вы откроете для себя весь мир онлайн развлечений. Именно здесь, на сайте Гама Казино, вас ждут веселье и богатство, а рулетка станет мастером вашей судьбы.
Вавада казино онлайн
https://exler.me/user/momefa001
Здесь вы найдете не только знакомые слоты, но и те, которые поразят своей уникальностью. Наша команда тщательно отбирает самые захватывающие и новаторские игры, чтобы каждый спин был настоящим открытием. Вавада Казино предлагает богатство вариантов – от классических фруктовых машин до современных слотов с захватывающими сюжетами.Что делает Vavada Casino настолько неповторимым? Это не только возможность играть на деньги в самых захватывающих слотах, но и атмосфера азарта, которая окутывает вас с первых секунд пребывания на сайте. Словно волшебная вуаль, обволакивающая каждого игрока, Вавада Казино создает идеальное сочетание риска и возможности.
My brother recommended I would possibly like this web site.
He used to be totally right. This put up truly made my day.
You cann’t imagine just how so much time I had spent for this info!
Thank you!
рейтинг казино по выплатам
https://t.me/s/BetBlitzMaverick
cat casino войти
http://mymart.kz/forum/viewtopic.php?f=31&t=124867
Cat Casino — это не просто казино, это путь к невероятным приключениям и неожиданным сюрпризам. Скачайте наше приложение или играйте онлайн — выбор за вами. Но одно остается неизменным: Cat Casino всегда готово порадовать вас своими уникальными играми, яркой графикой и захватывающим азартом. Встречайте 2023 год вместе с Cat Casino и станьте частью легенды азартного мира!Cat Casino — не просто портал развлечений, это целый космос эмоций и волнения, где Кэт Казино приветствует всех, кто готов отправиться в путешествие по бескрайней вселенной игровых автоматов. Здесь вы найдете горячие новинки, свежие как утренний ветерок, и классические игры, словно дорогие старые друзья, всегда готовые подарить вам незабываемые моменты азарта.
Hello, i read your blog occasionally and i own a similar one and i was
just wondering if you get a lot of spam feedback?
If so how do you prevent it, any plugin or anything you can recommend?
I get so much lately it’s driving me insane so any support is very much appreciated.
онлайн казино рейтинг
https://t.me/s/BetBlitzMaster
ггпокерок
https://politikforum.ru/member.php?u=13385076
Чтобы присоединиться к увлекательному миру PokerOK, просто перейдите на официальный сайт, где вас ждет возможность скачать клиент для игры в покер. С ним вы окунетесь в виртуальное путешествие по захватывающему миру карт и фишек, где каждый ваш ход анализируется и обдумывается до мельчайших деталей.Не упустите возможность окунуться в захватывающий мир покера на официальном сайте PokerOK. Скачайте клиент и начните свой путь к славе и богатству, где каждая партия – это шанс стать настоящим мастером покера. Ваша удача ждет вас за столом, где PokerOK – это не просто имя, это стиль жизни, где рождаются настоящие победители.
рейтинг игровых автоматов онлайн
https://t.me/s/BetBlitz0Champion
Pretty nice post. I just stumbled upon your blog and wanted to say that I
have really enjoyed browsing your blog posts.
After all I’ll be subscribing to your feed and I hope you write again soon!
сайт gama casino
https://priusforum.ru/forums/index.php?autocom=gallery&req=si&img=4362
Что делает Gama Casino настолько особенным? Это не только вход на официальный сайт, это путешествие в мир, где каждая буква вашего имени может стать символом удачи. Именно здесь, на страницах Гама Казино, судьба и азарт переплетаются, создавая неповторимую атмосферу, которая затягивает с первого взгляда.Играя в Гама Казино, вы обнаружите, что это не просто место для испытания удачи. Это космос, где каждый спин на игровых автоматах — это возможность покорить вершину джекпота. Каждая мелодия, каждая крупье, словно созданы, чтобы погрузить вас в атмосферу истинного казино.
You have made your point pretty nicely!.
rtg games red dog casino review online casino deposit
рейтинг казино онлайн на реальные деньги
рейтинг казино онлайн на реальные деньги
рейтинг и обзоры интернет казино
рейтинг и обзоры интернет казино
Вавада казино вход
https://500px.com/p/murouyat?view=photos
Мы понимаем, что азарт – это страсть, влекущая вас в водоворот волнений и эмоций. Именно поэтому наш виртуальный портал оформлен с максимальным комфортом и удобством. От главной страницы до разделов с игровыми автоматами, Vavada Casino заботится о вашем удовольствии и простоте навигации.Vavada Casino — это не только игры, но и атмосфера настоящего казино, перенесенная в онлайн пространство. Вас ждут уникальные слоты-онлайн с захватывающей графикой и реалистичными звуками, словно вы находитесь в центре азартного мира.
Cheers! Useful information!
red dog casino 100 no deposit bonus codes https://reddog-casino.site/ empire casino online login
уникальный бонус код cat casino 2023
http://danceway74.ru/users/1526?wid=3385
Скачать игровые автоматы на Cat Casino — это как открыть сундук с сокровищами у древнего пирата. Кэт Казино дарит вам этот ключ к виртуальной роскоши, который вас унесет в мир ярких красок и звуков, мир, где каждый барабан может стать вашим верным спутником. От бескрайних просторов космоса до забытых храмов древних цивилизаций, каждая игра на Cat Casino — это отдельная история, написанная специально для вас.Не хотите скачивать? Не проблема! Cat Casino также предоставляет вам возможность играть онлайн, не загружая ничего на свое устройство. Просто пройдите регистрацию на официальном сайте, и вы окажетесь в виртуальной реальности Кэт Казино, где каждый клик мыши может повернуть ваш мир вверх дном.
Useful forum posts. Kudos!
casino fish redplay casino red dog login
Regards. A good amount of posts!
online free blackjack deuces wild bonus poker chumba casino. calm
Many thanks! Terrific stuff.
online slots free no download https://red-dogcasino.website/ regal riches
You’re so awesome! I don’t believe I’ve truly read a
single thing like that before. So wonderful to discover
someone with a few unique thoughts on this subject.
Seriously.. thanks for starting this up. This site is one thing that’s needed on the web, someone with some originality!
Fine write ups. Cheers.
no deposit bonus codes for existing customers blackjack for free or real money play blackjack real money
Do you have any video of that? I’d love to find out
more details.
Thanks, Plenty of tips.
bc game promo code no deposit https://bcgamecasino.fun/ 1000 bc game
Right here is the perfect blog for anybody who really
wants to find out about this topic. You understand a whole lot its almost tough to argue with you (not that I
personally will need to…HaHa). You certainly put a brand new spin on a subject
which has been discussed for decades. Great stuff, just excellent!
топ рейтинг онлайн казино
топ рейтинг онлайн казино
рейтинг казино на деньги
рейтинг казино на деньги
играть онлайн казино гама
играть онлайн казино гама
Thanks a lot! A lot of information!
bc clemson game bcgame 入金ボーナス bc game codes
зарегистрироваться rox в казино
зарегистрироваться rox в казино
честный рейтинг онлайн казино
честный рейтинг онлайн казино
войти в казино rox
войти в казино rox
гама казино сайт
гама казино сайт
в казино rox не могу зарегистрироваться
https://t.me/s/v_kazino_rox_ne_mogu_zaregistrir
скачать приложение казино rox
https://t.me/s/skachat_prilozhenie_kazino_rox
Very good info, Kudos.
roullete online red dog casino reddog casinos
казино гама промокод
казино гама промокод
скачать rox казино на комп
https://t.me/s/skachat_rox_kazino_na_komp
rox казино
https://t.me/s/roxx_casino
rox онлайн казино вход
rox онлайн казино вход
rox казино зеркало
https://t.me/s/rox_kazino_zerkalo
rox казино зеркало где выигрывают
rox казино зеркало где выигрывают
rox казино вход
https://t.me/s/rox_kazino_vhod
rox казино телефон
rox казино телефон
rox казино скачать на андроид бесплатно
https://t.me/s/rox_kazino_skachat_na_android_be
rox казино скачать
https://t.me/s/rox_kazino_skachat
rox казино правило вывода
https://t.me/s/rox_kazino_pravilo_vyvoda
rox казино регистрация с бонусом
https://t.me/s/rox_kazino_registraciya_s_bonuso
rox казино отзывы о выплатах
https://t.me/s/rox_kazino_otzyvy_o_vyplatah
rox казино рабочее зеркало
https://t.me/s/rox_kazino_rabochee_zerkalo
Thank you. A lot of posts.
bcgame bc game casino no deposit bonus codes shitcodes bc game
You said it perfectly.!
bc game referral code https://bc-game-casino.online/ bc uconn football game
rox. казино.
https://t.me/s/rox_kazinoo
rox казино промокод
rox казино промокод
rox игровые казино
https://t.me/s/rox_igrovye_kazino
rox казино правила вывода
rox казино правила вывода
рокс казино rox
рокс казино rox
rox казино отзывы
rox казино отзывы
промокод на rox казино
промокод на rox казино
rox казино онлайн
https://t.me/s/rox_kazino_onlajn
Hey I know this is off topic but I was wondering if you knew of any widgets I could add to my blog that automatically
tweet my newest twitter updates. I’ve been looking for a plug-in like this
for quite some time and was hoping maybe you would have some experience with something like this.
Please let me know if you run into anything. I truly enjoy reading your
blog and I look forward to your new updates.
Онлайн казино на реальные деньги для андроид
https://gozee.ru/
промокод на казино rox
https://t.me/s/promokod_na_kazino_rox
rox казино официальный сайт
rox казино официальный сайт
Лучшие онлайн казино России на рубли
Лучшие онлайн казино России на рубли
Hey there! I know this is kind of off topic but I
was wondering if you knew where I could find a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m
having problems finding one? Thanks a lot!
промокод на фриспины казино rox
промокод на фриспины казино rox
rox казино официальный
https://t.me/s/rox_kazino_oficialnyj
rox казино мобильная версия обзор
rox казино мобильная версия обзор
You actually explained this well.
bc game online bc game аё–аёаё™а№Ђаё‡аёґаё™ bc game scam
Азартные Эмоции с 1Win: Лучший Путь
к Успеху официальная игра lucky jet
rox казино играть
https://t.me/s/rox_kazino_igrat
My brother suggested I would possibly like this website.
He used to be totally right. This publish truly made my day.
You cann’t consider simply how much time I had spent for this info!
Thanks!
Nicely put. Appreciate it.
bc game casino code bc. game notre dame bc game 2023
I’ll immediately grasp your rss as I can not to find your
email subscription hyperlink or newsletter service. Do you’ve any?
Kindly let me recognize in order that I may just subscribe.
Thanks.
rox казино андроид
https://t.me/s/rox_kazino_android
I’m really loving the theme/design of your site. Do you ever run into
any browser compatibility issues? A handful of my blog readers have complained about my blog not operating correctly in Explorer but looks great in Safari.
Do you have any recommendations to help fix this issue?
правила игры в онлайн казино rox
https://t.me/s/pravila_igry_v_onlajn_kazino_rox
Simply wish to say your article is as astounding. The clearness in your submit is simply excellent and that i could suppose you are a professional in this subject.
Well along with your permission let me to snatch your RSS feed to stay up to date with imminent post.
Thank you one million and please keep up the enjoyable work.
rox casino казино
rox casino казино
Hey I am so thrilled I found your blog page, I really found you by accident, while I was researching
on Digg for something else, Nonetheless I am here now and would
just like to say kudos for a incredible post
and a all round thrilling blog (I also love the theme/design), I
don’t have time to read it all at the moment but I have saved it and also
added in your RSS feeds, so when I have time I will be back to
read more, Please do keep up the excellent jo.
Beneficial posts. Thanks!
score in bc lions game https://bcgamecasino.pw/ bc game wallet
I love your blog.. very nice colors & theme.
Did you create this website yourself or did you hire someone to do it for you?
Plz respond as I’m looking to design my own blog and would like
to know where u got this from. thanks
партнерская програма казино rox
партнерская програма казино rox
рокс казино rox casino
https://t.me/s/roks_kazino_rox_casino
партнерка rox казино
https://t.me/s/partnerka_rox_kazino
промокоды казино rox
https://t.me/s/promokody_kazino_rox
Loyalty club members earn rewards points for playing on the hugely-rated app.
отзывы rox казино
https://t.me/s/otzyvy_rox_kazino
промо к казино rox
промо к казино rox
It is perfect time to make a few plans for the long run and it is time to be happy.
I’ve learn this publish and if I could I desire to suggest you few fascinating issues or advice.
Perhaps you could write subsequent articles relating to this article.
I wish to read even more things about it!
I’m impressed, I have to admit. Rarely do I encounter a blog that’s both educative and entertaining, and let me
tell you, you have hit the nail on the head.
The issue is something not enough people are speaking intelligently
about. Now i’m very happy that I found this during my hunt for
something regarding this.
онлайн-казино rox бонусы
онлайн-казино rox бонусы
приложение rox казино
https://t.me/s/prilozhenie_rox_kazino
Онлайн казино на реальные деньги для андроид
https://gozee.ru/
Oll porn
официальный сайт rox casino казино рокс
официальный сайт rox casino казино рокс
Kudos! Wonderful information!
bc game withdrawal time bc game app download watch the bc lions game online
онлайн казино rox
онлайн казино rox
не работает казино rox
https://t.me/s/ne_rabotaet_kazino_rox
Самые честные онлайн казино
Самые честные онлайн казино
онлайн казино rox casino
https://t.me/s/onlajn_kazino_rox_casino
не открывает казино rox
не открывает казино rox
зеркало казино чемпион
https://t.me/s/zerkalo_kazino_chempion
онлайн казино rox альтернативный вход
онлайн казино rox альтернативный вход
It’s going to be finish of mine day, except before end I am reading this wonderful paragraph to increase my experience.
зеркало кэт казино
https://t.me/s/zerkalo_ket_kazino
скачать казино чемпион
https://t.me/s/skachat_kazino_chempion
казино rox зарегистрироваться
казино rox зарегистрироваться
официальное казино rox
официальное казино rox
Hi there, I wish for to subscribe for this web
site to take latest updates, thus where can i do it please
help.
скачать чемпион казино
скачать чемпион казино
зеркало cat casino
зеркало cat casino
Oh my goodness! Amazing article dude! Thanks, However I am having
troubles with your RSS. I don’t know why I can’t subscribe to it.
Is there anybody else getting the same RSS problems?
Anyone who knows the answer can you kindly respond? Thanx!!
казино. rox.
https://t.me/s/kazino_roxx
This post provides clear idea designed for the new viewers of blogging,
that genuinely how to do blogging.
обзор онлайн казино rox casino
обзор онлайн казино rox casino
Have you ever thought about including a little bit more than just your articles?
I mean, what you say is valuable and all. But imagine if you added some great photos or videos to give your posts more, “pop”!
Your content is excellent but with images and videos,
this site could undeniably be one of the greatest in its
niche. Excellent blog!
Виртуозная Игра: Казино Гамма создает атмосферу победы Казино Гамма
сайт казино чемпион
сайт казино чемпион
зарегистрироваться в кэт казино
https://t.me/s/zaregistrirovatsya_v_ket_kazino
казино rox скачать бесплатно
https://t.me/s/kazino_rox_skachat_besplatno
обзор казино rox
https://t.me/s/obzor_kazino_rox
Wonderful forum posts. Appreciate it.
code bc game https://bcgamecasino.website/ bc lions game tonight
рабочее зеркало казино чемпион
https://t.me/s/rabochee_zerkalo_kazino_chempion
super cat casino
https://t.me/s/super_cat_kazino
казино rox с бонусом на первый депозит
казино rox с бонусом на первый депозит
не заходит в казино rox
https://t.me/s/ne_zahodit_v_kazino_rox
промокод казино чемпион
промокод казино чемпион
супер кэт казино
супер кэт казино
казино rox сайт
https://t.me/s/kazino_rox_sajt
казино rox зеркало
https://t.me/s/kazino_rox_zerkalo
скачать кэт казино
скачать кэт казино
It’s amazing to pay a quick visit this web page and reading the
views of all mates regarding this paragraph, while
I am also zealous of getting familiarity.
промокод чемпион казино
промокод чемпион казино
Hi everyone, it’s my first pay a quick visit at this website, and paragraph is actually fruitful designed for me, keep
up posting these articles or reviews.
Awesome knowledge. Thanks a lot!
bc game down is bc game legit clemson bc game
казино rox rol
казино rox rol
казино rox сайты
https://t.me/s/kazino_rox_sajty
сайт cat casino
сайт cat casino
онлайн казино чемпион
https://t.me/s/onlajn_kazino_chempion
казино rox отзывы новичков реальные
https://t.me/s/kazino_rox_otzyvy_novichkov
регистрация в мобильной версии кэт казино
регистрация в мобильной версии кэт казино
казино rox россия
казино rox россия
казино вулкан чемпион бонусы
казино вулкан чемпион бонусы
промокоды кэт казино
промокоды кэт казино
казино rox официальное зеркало
казино rox официальное зеркало
казино rox регистрация
https://t.me/s/kazino_rox_registraciya
казино вулкан чемпион
https://t.me/s/kazino_vulkan_chempion
промокоды cat casino
https://t.me/s/promokody_cat_casino
казино rox код
https://t.me/s/kazino_rox_kod
казино rox отзывы
казино rox отзывы
казино чемпион зеркало вход
казино чемпион зеркало вход
промокод на кэт казино
https://t.me/s/promokod_na_ket_kazino
казино rox казино отзывы
казино rox казино отзывы
казино rox онлайн
https://t.me/s/kazino_rox_onlajn
промокод cat casino
https://t.me/s/promokod_cat_casinoo
казино чемпион зеркало на сегодня
https://t.me/s/kazino_chempion_zerkalo_na_segod
казино rox casino rox
казино rox casino rox
казино rox официальный сайт вход
https://t.me/s/kazino_rox_oficialnyj_sajt_vhod
промокод кэт казино как получить
промокод кэт казино как получить
Its like you read my mind! You appear to know so much about this, like you wrote
the book in it or something. I think that you could do with some
pics to drive the message home a little bit,
but other than that, this is wonderful blog. A fantastic read.
I’ll certainly be back.
казино чемпион зеркало
https://t.me/s/kazino_chempion_zerkalo
казино rox box скачать
https://t.me/s/kazino_rox_box_skachat
казино rox официальный сайт
https://t.me/s/kazino_rox_oficialnyj_sajt
промокод кэт казино
https://t.me/s/promokod_cat_casino
What a data of un-ambiguity and preserveness of valuable experience concerning
unpredicted emotions.
казино чемпион скачать
казино чемпион скачать
казино rox бонус за регистрацию
казино rox бонус за регистрацию
It’s very easy to find out any topic on web as
compared to textbooks, as I found this article at this site.
онлайн казино кэт
https://t.me/s/onlajn_kazino_ket
казино rox официальный
https://t.me/s/kazino_rox_oficialnyj
казино чемпион регистрация
казино чемпион регистрация
официальный сайт cat casino
официальный сайт cat casino
казино rox бездепозитный бонус при регистрации
казино rox бездепозитный бонус при регистрации
казино rox личный кабинет
https://t.me/s/kazino_rox_lichnyj_kabinet
Truly all kinds of awesome material.
обзор 1win зеркало промокод 2023 https://1winoficialnyj.online/ 1win мобильное
официальный сайт кэт казино
официальный сайт кэт казино
казино чемпион рабочее зеркало
казино чемпион рабочее зеркало
казино rox 777
казино rox 777
казино rox casino
казино rox casino
Cheers, I like this.
1win промокод без депозита как поставить бонус в 1win 1win promo code
мобильное онлайн казино кэт
https://t.me/s/mobilnoe_onlajn_kazino_ket
I’ve been exploring for a little for any high-quality articles or weblog posts in this sort of space .
Exploring in Yahoo I finally stumbled upon this website.
Studying this info So i am happy to show that I’ve a very good uncanny feeling I came upon exactly what I needed.
I most no doubt will make certain to don?t forget this web site and provides it a
look regularly.
как регистрироваться на казино rox
https://t.me/s/kak_registrirovatsya_na_kazino_r
чемпион казино рабочее зеркало
чемпион казино рабочее зеркало
казино на реальные деньги rox
казино на реальные деньги rox
мобильная версия кэт казино
мобильная версия кэт казино
играть казино rox
играть казино rox
интернет казино rox
https://t.me/s/internet_kazino_rox
казино чемпион промокод
https://t.me/s/kazino_chempion_promok0d
кэт казино зеркало 2023
https://t.me/s/ket_kazino_zerkalo_2023
бонусы бездепозитный за регистрации казино rox
бонусы бездепозитный за регистрации казино rox
игра в казино rox
игра в казино rox
казино чемпион отзывы
https://t.me/s/kazino_chempion_otzyvy
кэт казино зеркало 2022
https://t.me/s/ket_kazino_zerkalo_2022
бонус код казино rox
бонус код казино rox
казино rox
https://t.me/s/casino_rox1
кэт казино скачать
https://t.me/s/ket_kazino_skachat
казино чемпион онлайн рабочее зеркало
казино чемпион онлайн рабочее зеркало
бездепозитный промокод в казино rox
бездепозитный промокод в казино rox
cash back в онлайн казино rox
cash back в онлайн казино rox
кэт казино отзывы
https://t.me/s/ket_kazino_otzyvy
казино чемпион онлайн
казино чемпион онлайн
кэт казино официальный сайт зеркало
кэт казино официальный сайт зеркало
pokerok
https://www.sitebs.ru/blogs/89022.html
На PokerOK вы найдете бесчисленное количество уникальных возможностей. Команда профессионалов работает над тем, чтобы каждый игрок ощущал заботу и внимание. Будьте уверены, что ваша безопасность и конфиденциальность – наш приоритет. Откройте для себя мир разнообразных турниров и регулярных игр, где даже невероятные шансы могут привести к захватывающему успеху.Так что, если вы готовы к вызову и хотите окунуться в захватывающий мир покера, PokerOK — ваш надежный спутник в этом приключении. Скачайте клиент, присоединяйтесь к столам и докажите, что именно ваша рука достойна звания королевской!
бездепозит и бонусы казино rox
бездепозит и бонусы казино rox
кэт казино
https://t.me/s/ket_kazinoo
gama casino играть
https://www.bestoldgames.net/forum/viewtopic.php?t=450815&msg=459042
Почувствуйте волнение, ощутите эмоции, проникнув в самое ядро азартной страсти, доступное вам на официальном сайте Gama Casino. Мы приглашаем вас в наш мир, где каждая партия — это событие, а каждый спин — это шанс изменить свою судьбу. Станьте частью Гама Казино и откройте для себя новые горизонты азартных развлечений!Играя в Гама Казино, вы обнаружите, что это не просто место для испытания удачи. Это космос, где каждый спин на игровых автоматах — это возможность покорить вершину джекпота. Каждая мелодия, каждая крупье, словно созданы, чтобы погрузить вас в атмосферу истинного казино.
бесплатно скачать казино rox
https://t.me/s/besplatno_skachat_kazino_rox
With thanks! Helpful stuff!
1win зеркало 1вин оффициал бесите 1win скачать 1win 2024
кэт казино без регистрации
кэт казино без регистрации
Wow lots of excellent knowledge.
1win официальное зеркало https://1winoficialnyj.site/ 1win рабочее зеркало на сегодня
Definitely believe that which you stated. Your favorite justification appeared to be on the net the simplest thing to be aware of.
I say to you, I certainly get irked while people consider worries that they plainly do not know about.
You managed to hit the nail upon the top and defined out the whole thing without
having side-effects , people could take a signal.
Will probably be back to get more. Thanks
Vavada casino вход
http://forums.unigild.com/index.php?/topic/311-%D0%B8%D0%B3%D1%80%D0%B0-%D1%80%D0%B5%D1%81%D1%82%D0%BE%D1%80%D0%B0%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B1%D0%B8%D0%B7%D0%BD%D0%B5%D1%81-%D1%81-%D0%B2%D1%8B%D0%B2%D0%BE%D0%B4%D0%BE%D0%BC-%D0%B4%D0%B5%D0%BD%D0%B5%D0%B3/page__gopid__2748
Казино Вавада – это не просто игровая площадка, это целый игровой космос, где каждый спин барабанов слотов-онлайн превращает ваше время в захватывающее событие. Полная версия игровых автоматов бесплатно раскроет перед Вами мир невероятных возможностей. Неважно, новичок Вы или опытный игрок, Вавада Казино дарит радость от игры и шанс победить!Добро пожаловать в мир азарта и увлекательных приключений – на официальный портал Казино Вавада! Здесь, на грани воображения и реальности, Вас ждут невероятные возможности для крупных выигрышей. Войдите в захватывающий виртуальный мир развлечений и азартных игр на деньги, доступный на нашем сайте в любое удобное для Вас время.
казино чемпион официальный сайт
https://t.me/s/kazino_chempion_oficialnyj_sajt
кэт казино бездепозитный бонус
https://t.me/s/ket_kazino_bezdepozitnyj_bonus
cat casino регистрация на сайте
http://from-jp.ru/member-viewprofile-71265.html
Играя в Cat Casino, Кэт Казино, вы попадаете в атмосферу совершенно новых ощущений. Это не просто казино, это путешествие в мир невероятных приключений. Игровые автоматы на Cat Casino созданы с огромной любовью к деталям, где каждая вращающаяся барабана — как страница в увлекательной книге. Вас ждут великолепные графика, уникальные звуковые эффекты и увлекательные сюжеты.Не упусти свой шанс с Cat Casino! Скачай игровые автоматы и начни свой путь к победе. Мы гарантируем честность и надежность, ведь твои эмоции – наша цель. Играй онлайн, скачивай слоты – с Cat Casino каждый день – это новое приключение!
казино кэт
https://t.me/s/kazzino_cat
казино чемпион официальный
https://t.me/s/kazino_chempion_oficialnyj
казино кэт казино
https://t.me/s/kazino_ket_kazino
казино чемпион мобильная версия
казино чемпион мобильная версия
casino cat
casino cat
казино чемпион казино чемпион
казино чемпион казино чемпион
казино cat casino
казино cat casino
Онлайн казино на реальные деньги для андроид
Онлайн казино на реальные деньги для андроид
как зарегистрироваться в кэт казино
https://t.me/s/kak_zaregistrirovatsya_v_ket_kaz
казино чемпион играть онлайн
казино чемпион играть онлайн
игровые автоматы cat casino
игровые автоматы cat casino
казино чемпион играть на деньги
казино чемпион играть на деньги
Thanks! Plenty of information.
1win xyz почта вход 1win отзывы 1win букмекерская контора сайт
Hey! This is my 1st comment here so I just wanted to give a quick shout
out and tell you I genuinely enjoy reading your blog posts.
Can you suggest any other blogs/websites/forums that cover
the same subjects? Appreciate it!
играть кэт казино
https://t.me/s/igrat_ket_kazino
казино чемпион играть бесплатно
казино чемпион играть бесплатно
cool cat casino
cool cat casino
Magnificent beat ! I would like to apprentice even as you amend your site, how can i subscribe for a weblog
website? The account helped me a acceptable
deal. I had been a little bit familiar of this your broadcast provided vivid clear concept
казино чемпион играть
казино чемпион играть
cool cat casino no deposit bonus
https://t.me/s/cool_cat_casino_no_deposit_bonus
You have made your point extremely effectively.!
казино 1win официальный https://1winoficialnyj.website/ 1win букмекерская контора скачать приложение
cool cat casino no deposit
cool cat casino no deposit
казино чемпион официальный сайт лицензионный скачать бесплатно
https://t.me/s/kazino_chempion_ficialnyj_sajt_l
Fantastic goods from you, man. I’ve understand your stuff previous to and you are just too magnificent.
I actually like what you’ve acquired here,
certainly like what you are stating and the way in which
you say it. You make it enjoyable and you still care for to keep it smart.
I cant wait to read far more from you. This is actually a tremendous website.
кэт казино зеркало на сегодня
https://t.me/s/cat_kazino_zerkalo_na_segodnia
казино чемпион бонусы
казино чемпион бонусы
кэт казино зеркало
кэт казино зеркало
казино чемпион бонус
https://t.me/s/kazino_chempion_bonus
кэт казино вход
https://t.me/s/cat_kazino_vhod
Terrific material, Cheers!
1win jetx скачать приложение 1win скачать 1win на ios
казино чемпион бездепозитный бонус
казино чемпион бездепозитный бонус
кэт казино регистрация
кэт казино регистрация
кэт казино онлайн
https://t.me/s/cat_kazino_online
казино чемпион бесплатно
https://t.me/s/kazino_chempion_besplatno
cat casino промокод
https://t.me/s/cat_kasino_promokod
казино чемпион
казино чемпион
cat casino зеркало
https://t.me/s/cat_casino_zerkalow
Great information. Regards!
1win отзывы 1win казино зеркало 1win aviator apk
казино кэт зеркало
казино кэт зеркало
казино чемпион вход
https://t.me/s/kazin0_chempion_vhod
cat casino зеркало на сегодня
cat casino зеркало на сегодня
You mentioned it perfectly.
jetx 1win https://1winregistracija.online/ 1win бесплатно телефон
интернет казино чемпион
https://t.me/s/internet_kazino_chempion
I know this website presents quality depending posts and additional stuff, is there any other web site which
provides these things in quality?
cat casino зеркало 2022
cat casino зеркало 2022
cat casino зарегистрироваться
https://t.me/s/cat_casino_zaregistrirovatsia
игры чемпион казино
игры чемпион казино
cat casino вход
cat casino вход
50 фриспинов за регистрацию в казино чемпион
50 фриспинов за регистрацию в казино чемпион
истории на приколе
cat casino войти
https://t.me/s/cat_casino_vojti
чемпион казино зеркало
https://t.me/s/chempion_kazino_zerkalo
кэт казино войти
https://t.me/s/cat_casino_voiti
кэт казино телеграм
https://t.me/s/cat_casino_telegramm
Hey there! I’ve been following your web site for a long time now
and finally got the bravery to go ahead and
give you a shout out from Houston Texas! Just wanted to mention keep up
the excellent job!
With thanks, I enjoy it!
официальный сайт конторы 1win промокоды 1win 1win оф сайт
cat casino скачать
https://t.me/s/cat_casino_skachat
кэт казино сайт
https://t.me/s/cat_casino_sait
cat casino сайт
https://t.me/s/cat_casino_saait
cat casino ru
cat casino ru
Wow loads of useful knowledge!
1win kz вход https://1winvhod.online/ 1win affiliation
cat casino регистрация на сайте
https://t.me/s/cat_casino_registraciya_na_sajte
A person necessarily help to make seriously posts
I would state. This is the very first time I frequented your web page and to this point?
I surprised with the analysis you made to make this actual publish incredible.
Fantastic process!
cat casino регистрация
cat casino регистрация
cat casino рабочее зеркало
https://t.me/s/cat_casino_rabochee_zerkaloo
кэт казино рабочее зеркало
https://t.me/s/cat_casino_rabochee_zerkalo
Many thanks! A lot of data.
1win ставки зеркало бонус по free spins 1win как использовать 1win бонус 5000
кэт казино промокод
https://t.me/s/cat_casino_promokodd
cat casino отзывы
https://t.me/s/cat_casino_otzyvyy
You actually said that wonderfully.
как пользоваться бонусами 1win как использовать бонусный счет в 1win как вывести деньги с 1win на карту
казино кэт отзывы
https://t.me/s/cat_casino_otzyvy
вавада. казино. онлайн. официальный. сайт.
вавада. казино. онлайн. официальный. сайт.
вход joycasino
https://t.me/s/vhod_joycasino
кэт казино онлайн официальный
https://t.me/s/cat_casino_online_oficialnyi
вавада. казино. онлайн. бесплатно.
https://t.me/vavada_kazino_onlajn_besplatno
зеркало joycasino
https://t.me/s/zerkalo_joycasin0
скачать joycasino на андроид
скачать joycasino на андроид
cat casino онлайн
https://t.me/s/cat_casino_onlinee
vavada зеркало
vavada зеркало
чемпион казино зеркала
чемпион казино зеркала
сайт joycasino com
https://t.me/s/sajt_joycasino_com
кэт казино онлайн регистрация
кэт казино онлайн регистрация
вавада вход в казино
вавада вход в казино
“””текущее”” зеркало joycasino”
“””текущее”” зеркало joycasino”
чемпион казино вход в личный кабинет
https://t.me/s/chempion_kazino_vhod_v_lichnyj_k
cat casino официальный
https://t.me/s/cat_casino_oficialnyj
вавада. вход. в. казино.
https://t.me/s/vavada_vhod_v_kazin0
промокоды joycasino
https://t.me/s/promokody_joycasino
чемпион казино вход
https://t.me/s/chempion_kazino_vh0d
Hey there! Do you know if they make any plugins to assist with SEO?
I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good success.
If you know of any please share. Appreciate it!
vavada
https://t.me/s/vavada_vavada_casinoo
cat casino официальный сайт вход
https://t.me/s/cat_casino_oficialnyi_sait_vhod
скачать joycasino
скачать joycasino
Many thanks. Loads of write ups.
jet в 1win как обыграть отзывы казино скачать 1win на телефон официальный 1win команда кс го
промо код joycasino
https://t.me/s/promo_kod_joycasino
чемпион казино верификация
чемпион казино верификация
vavada рабочее зеркало
https://t.me/s/vavada_rabochee_zerkaloo
cat casino официальный сайт
https://t.me/s/cat_casino_oficialnyi_saitt
отзывы о joycasino
https://t.me/s/otzyvy_o_joycasino
Prety nice post. I just stumbled upon your blog and
wished to say that I have trujly ejoyed browsing your blog posts.
In any case I’ll be subscribing to your rsss feed and
I hope you write again very soon!
Here iss my web site; mosquitto broker
You have made your position very clearly..
1win зеркало на сегодня скачать 1win casino app авиатор 1win скачать
вавада онлайн казино
вавада онлайн казино
кэт казино официальный сайт
кэт казино официальный сайт
сайт joycasino
https://t.me/s/sajt_joycasino
чемпион казино скачать
https://t.me/s/chempion_kazino_skachat
отзывы joycasino
отзывы joycasino
вавада официальный сайт казино
https://t.me/s/vavada_oficialnyj_sajt_kazino
кэт казино официальный
https://t.me/s/cat_casino_oficialnyi
чемпион казино промокод 2022
https://t.me/s/chempion_kazino_promokod_2022
vavada официальный сайт
vavada официальный сайт
официальный сайт joycasino
официальный сайт joycasino
рабочее зеркало joycasino
https://t.me/s/rabochee_zerkalo_joycasinoo
cat casino официальный войти
cat casino официальный войти
чемпион казино промокод
https://t.me/s/chempion_kazino_promok0d
вавада казино
вавада казино
cat casino на деньги
https://t.me/s/cat_casino_na_dengi
обзор joycasino
обзор joycasino
вавада казино скачать
https://t.me/s/vavada_kazino_skachat
чемпион казино онлайн официальный сайт
чемпион казино онлайн официальный сайт
промокод joycasino
https://t.me/s/promokod_joycasinoo
cat casino мобильная версия
https://t.me/s/cat_casino_mobilnaya_versiya
мобильная версия joycasino
https://t.me/s/mobilnaya_versiya_joycasino
вавада казино сайт
https://t.me/s/vavada_kazino_sajtt
чемпион казино онлайн
https://t.me/s/chempion_kazino_onlajn
кэт казино мобильная версия
кэт казино мобильная версия
казино. joycasino.
https://t.me/s/kazino_joycasin0
You’ve made your position pretty well!!
партнерка 1win промокод 1win 1win как скачать
онлайн казино joycasino
онлайн казино joycasino
вавада казино рабочее зеркало
https://t.me/s/vavada_kazino_rabochee_zerkalo
cat casino игровые автоматы
https://t.me/s/cat_casino_igrovye_avtomaty
чемпион казино официальный сайт
чемпион казино официальный сайт
joycasino зеркало сайта
joycasino зеркало сайта
вавада казино отзывы
https://t.me/s/vavada_kazino_otzyvy
cat casino играть
cat casino играть
You actually suggested that wonderfully!
бесплатные ваучеры 1win как использовать бонусы в 1win 1win официальный
чемпион казино играть на деньги
https://t.me/s/chempion_kazino_igrat_na_dengi
обзор казино joycasino
обзор казино joycasino
joycasino зеркало рабочее
joycasino зеркало рабочее
مرتبسازی بر اساس: جدیدترین گرانترین
ارزانترین محبوبترین پلیور بافت یوآر
رویهی داخی این هودی زنانه نیز پنبه است که باعث میشود
با پوشیدن آن حس نرم و لطیفی
منتقل شود.
вавада казино онлайн рабочее зеркало
https://t.me/s/vavada_kazino_onlajn_rabochee_ze
кэт казино играть онлайн
https://t.me/s/cat_casino_igrat_onlain
Hi there to every one, for the reason that I am genuinely eager of reading this blog’s post to
be updated regularly. It consists of nice material.
чемпион казино бездепозитный бонус
https://t.me/s/chempion_kazino_bezdepozitnyj_bo
joycasino зеркала
https://t.me/s/joycasino_zerkala
вавада казино онлайн официальный сайт
вавада казино онлайн официальный сайт
кэт казино играть
кэт казино играть
казино joycasino
казино joycasino
чемпион казино бездепозитный бонус за регистрацию
чемпион казино бездепозитный бонус за регистрацию
cat casino
https://t.me/s/cat_casino_casino
вавада. казино. онлайн. официальный.
https://t.me/s/vavada_kazino_onlajn_oficialny
joycasino зайти на официальный сайт
joycasino зайти на официальный сайт
cat casino промокод бездепозитный бонус
cat casino промокод бездепозитный бонус
чемпион казино бесплатно
https://t.me/s/chempion_kazino_besplatno
вавада казино официальный сайт регистрация
https://t.me/s/vavada_kazino_oficialnyj_sajt_re
joycasino vip
joycasino vip
joycasino.
joycasino.
cat casino бездепозитный бонус
https://t.me/s/cat_casino_bezdepositnyi_bonus
Wow that was strange. I just wrote an very long comment but after I clicked submit my
comment didn’t show up. Grrrr… well I’m not writing
all that over again. Regardless, just wanted to say superb blog!
чемпион казино бонус
https://t.me/s/chempion_kazino_b0nus
вавада. казино. официальный. отзывы.
https://t.me/s/vavada_kazino_oficialnyj_otzyvy
joycasino украина
joycasino украина
казино супер кэт
https://t.me/s/casino_super_cat
Hello to all, it’s truly a good for me to go to see this website, it contains helpful Information.
Many thanks, A lot of advice!
aviator 1win скачать сайт 1win казино 1win
вавада. казино. играть. онлайн.
вавада. казино. играть. онлайн.
joycasino telegram
https://t.me/s/joycasino_telegram
чемпион казино
чемпион казино
казино кэт официальный сайт
казино кэт официальный сайт
вавада. казино. играть. онлайн. зеркало.
https://t.me/s/vavada_kazino_igrat_onlain
joycasino скачать приложение
https://t.me/s/joycasino_skachat_prilozhenie
чемпион казино официальный сайт зеркало
https://t.me/s/chempi0n_kazino_0ficialnyj_sajt
You made your point.
1win ru 1win скачать 1win телефон мобильный
бонусы кэт казино
https://t.me/s/bonusy_ket_kazino
porno kino
Free porn
joycasino 777
joycasino 777
вавада казино играть
https://t.me/s/vavada_kazino_igrat
бонусы cat casino
бонусы cat casino
joycasino скачать бесплатно
joycasino скачать бесплатно
бездепозитные промокоды казино чемпион
бездепозитные промокоды казино чемпион
plaquenil 200 cost https://community.alteryx.com/t5/user/viewprofilepage/user-id/524722/ low cost plaquenil
вавада казино бонус
вавада казино бонус
joycasino рабочее зеркало 2022
https://t.me/s/joycasino_rabochee_zerkalo_2022
чемпион казино официальный сайт вход
чемпион казино официальный сайт вход
joycasino зеркало сегодня
joycasino зеркало сегодня
vavada casino
https://t.me/s/vavada_cazino
joycasino рабочее зеркало на сегодня
joycasino рабочее зеркало на сегодня
joycasino зеркало рабочее сегодня и сейчас
https://t.me/s/joycasino_zerkalo_rabochee_segod
вавада казино вход
вавада казино вход
joycasino промо код
joycasino промо код
вавада казино регистрация
вавада казино регистрация
joycasino promo code
https://t.me/s/joycasino_promo_code
Nicely put, Kudos.
1win 1win официальный сайт букмекерской как удалить аккаунт 1win
joycasino зеркало на сегодня мобильная версия
joycasino зеркало на сегодня мобильная версия
вавада казино онлайн
https://t.me/s/vavada_casino_onlaine
joycasino полный онлайн joycasino игровые джойказино бонусы
https://t.me/s/joycasino_polnyj_onlajn_joycasin
Many thanks. Numerous content.
1win indir 1win сайт россия 1win lucky jet игра отзывы
вавада казино зеркало
вавада казино зеркало
joycasino полный joycasino игровые автоматы джойказино бонусы
joycasino полный joycasino игровые автоматы джойказино бонусы
joycasino зеркало на сегодня
joycasino зеркало на сегодня
вавада казино официальный сайт вход зеркало
https://t.me/s/vavada_casino_oficialnyi_sait_ze
joycasino полный онлайн казино joycasino джойказино бонусы
joycasino полный онлайн казино joycasino джойказино бонусы
Hey there! I could have sworn I’ve been to this
blog before but after browsing through some of the post I realized
it’s new to me. Nonetheless, I’m definitely happy I found it and I’ll be bookmarking and checking
back often!
joycasino зеркало
https://t.me/s/joycasino_zerkal0
вавада казино официальный сайт вход
https://t.me/s/vavada_casino_oficialnyi_sait_vh
joycasino полный онлайн joycasino игровые автоматы бонусы
https://t.me/s/joycasino_polnyi_onlain_joycasin
вавада казино официальный сайт
https://t.me/s/vavada_casino_oficialnyi_sait
joycasino. отзывы.
joycasino. отзывы.
joycasino вывод денег
https://t.me/s/joycasino_vyvod_deneg
вавада казино официальный
https://t.me/s/vavada_casino_oficialnyi
joycasino отзывы игроков
https://t.me/s/joycasino_otzyvy_igrokov
вавада казино играть онлайн
вавада казино играть онлайн
joycasino онлайн казино joycasino автоматы джойказино бонусы
https://t.me/s/joycasino_online_kazino_igrovie
вавада. казино. бонус.
https://t.me/s/vavada_casino_bonuss
joycasino скачать официальный сайт
joycasino скачать официальный сайт
I think this is among the such a lot important information for me.
And i’m happy reading your article. But wanna commentary on few
general things, The web site taste is wonderful, the articles is
truly excellent : D. Good task, cheers
joycasino официальный сайт зеркало
https://t.me/s/joycasino_oficialnyj_sajt_zerkal
sweet bonanza joycasino
https://t.me/s/sweet_bonanza_joycasino
vavada казино
vavada казино
joycasino официальный сайт мобильная версия
https://t.me/s/joycasino_oficialnyj_sajt_mobil
joycasino скачать на андроид
https://t.me/s/joycasino_skachat_na_android
вавада. казино.
вавада. казино.
joycasino официальный
https://t.me/s/joycasino_officialnyi
joycasino скачать
https://t.me/s/joycasino_skachat
скачать вавада казино
скачать вавада казино
joycasino на деньги – джойказино слоты
https://t.me/s/joycasino_nadengi_joycasino
We’re a gaggle of volunteers and starting a new scheme in our community.
Your web site provided us with useful info to work on. You’ve performed an impressive process and our entire community will probably
be thankful to you.
схемы джой joycasino джойказино промокод
схемы джой joycasino джойказино промокод
скачать казино вавада на андроид
скачать казино вавада на андроид
vavada рабочее
vavada рабочее
joycasino сайт
https://t.me/s/joycasino_sajt
joycasino мобильная версия скачать
https://t.me/s/joycasino_mobilnaia_versija_skac
скачать казино вавада
https://t.me/s/skachat_kazino_vavada
vavada сегодня
vavada сегодня
секреты и зеркало joycasino джойказино промокод
секреты и зеркало joycasino джойказино промокод
joycasino mobile
https://t.me/s/joycasino_mobile
joycasino review
joycasino review
сайт онлайн казино вавада
https://t.me/s/sajt_onlajn_kazino_vavadaa
сайт vavada
https://t.me/s/sajt_vavada
This is a topic that is near to my heart… Many thanks!
Where are your contact details though?
joycasino коды
joycasino коды
joycasino регистрация
joycasino регистрация
vavada. online.
vavada. online.
сайт. онлайн. казино. вавада.
https://t.me/s/sajt_onlajn_kazino_vavada
I know this web site gives quality based articles and additional material, is there any other web site which provides these kinds of things in quality?
joycasino казино joycasino игровые автоматы джойказино бонусы
joycasino казино joycasino игровые автоматы джойказино бонусы
joycasino рабочее зеркало
joycasino рабочее зеркало
vavada. официальный. сайт.
https://t.me/s/vavada_oficialnyj_sajt
онлайн казино вавада
онлайн казино вавада
vavada. казино.
https://t.me/s/vavada_kazin0
joycasino казино
https://t.me/s/joycasino_kazin0
joycasino рабочая ссылка
https://t.me/s/joycasino_rabochaia_ssylka
официальный сайт казино вавада
официальный сайт казино вавада
официальный сайт vavada
официальный сайт vavada
Hello, after reading thhis awesome articl i am allso deloighted to share my expetience here
wih friends.
джойказино joycasino
https://t.me/s/joycasino_joycasinoo
joycasino промокод 2022
joycasino промокод 2022
vavada 888 зеркало
https://t.me/s/vavada_888_zerkalo
обзор казино вавада
https://t.me/s/obzor_casino_vavada
joycasino игровые автоматы
https://t.me/s/joycasino_igrovye_avtomaty
joycasino промокод
joycasino промокод
vavada. онлайн.
https://t.me/s/vavada_onlajn
казино вавада зеркало на сегодня
казино вавада зеркало на сегодня
joycasino играть
joycasino играть
joycasino приложение
https://t.me/s/joycasino_prilozhenie
vavada tg
https://t.me/s/vavada_tg
казино вавада рабочее зеркало
https://t.me/s/kazino_vavada_rabochee_zerkalo
vavada bonus
vavada bonus
joycasino фриспины
https://t.me/s/joycasino_freespiny
joycasino отзывы
joycasino отзывы
you are in reality a good webmaster. The
site loading pace is incredible. It sort of feels that you’re doing
any distinctive trick. Also, The contents are masterwork.
you have done a fantastic activity in this subject!
казино. вавада. отзывы.
казино. вавада. отзывы.
vavada телеграм
https://t.me/s/vavada_tellegram
joycasino com играть
joycasino com играть
joycasino онлайн
https://t.me/s/joycasino_onlajn
With havin so much written content do you
ever run into any problems of plagorism or copyright infringement?
My website has a lot of completely unique content I’ve either authored myself or outsourced but it seems a
lot of it is popping it up all over the internet without my authorization. Do you know any ways to help prevent content from being
ripped off? I’d definitely appreciate it.
vavada casino – официальный сайт скачать
https://t.me/s/vavada_casino_oficialnyj_sajt_sk
казино вавада отзывы
https://t.me/s/kazino_vavada_otzyvy
joycasino бонус за регистрацию
https://t.me/s/joycasino_bonus_za_registraciu
joycasino online
joycasino online
vavada обзор
https://t.me/s/vavada_obzor
казино вавада официальный
казино вавада официальный
joycasino бонус коды
https://t.me/s/joycasino_bonus_kody
joycasino официальный сайт мобильная
https://t.me/s/joycasino_oficialnyj_sajt_mobiln
vavada zerkalo
https://t.me/s/vavada_zerkal0
обзор онлайн казино joycasino
https://t.me/s/obzor_onlain_kazino_joycasino
казино онлайн вавада играть онлайн регистрация
https://t.me/s/kazino_online_vavada_online
vavada. отзывы.
https://t.me/s/vavada_otzyvy
joycasino бонус код нет проблем
https://t.me/s/joycasino_bonus_kod_net_problem
joycasino com официальный сайт
https://t.me/s/joycasino_oficialnyi_saitt
joycasino зеркало мобильная версия
joycasino зеркало мобильная версия
казино. онлайн. вавада. играть. онлайн. регистрация.
казино. онлайн. вавада. играть. онлайн. регистрация.
vavada рабочее
https://t.me/s/vavada_rabochee
joycasino бездепозитный бонус код
https://t.me/s/joycasino_bezdepositnyi_bonuskod
joycasino официальный сайт
joycasino официальный сайт
vavada официальный сайт регистрация
https://t.me/vavada_oficialnyj_sajt_registrac
казино вавада
казино вавада
joycasino вывод денег отзывы
joycasino вывод денег отзывы
joycasino android
https://t.me/s/joycasino_android
joycasino official
https://t.me/s/joycasino_officiall
vavada. casino.
vavada. casino.
вавада казино онлайн официальный
вавада казино онлайн официальный
joycasino support
https://t.me/s/joycasino_support
joycasino 2021
https://t.me/s/joycasino_2021
joycasino обзор
joycasino обзор
vavada официальный сайт вход
https://t.me/s/vavada_oficialnyj_sajt_vhod
казино вавада зеркало
https://t.me/s/casino_vavada_zerkalo
джойказино слотов и бонусов обзор joycasino зеркало джой
https://t.me/s/joycasino_slotov_i_bonusov_obzor
1364 joycasino
1364 joycasino
vavada отзывы
vavada отзывы
joycasino на деньги
joycasino на деньги
казино вавада вход
https://t.me/s/casino_vavada_vhod
joycasino полный онлайн казино joycasino игровые джойказино
https://t.me/s/joycasino_polnyi_onlain_kazino
vavada онлайн
https://t.me/s/vavada_onlain
joycasino ru
https://t.me/s/joycasin0ru
joycasino мобильная версия
https://t.me/s/joycasino_mobilnaja_versia
казино вавада скачать
казино вавада скачать
vavada приложение
https://t.me/s/vavada_prilozhenie
joycasino онлайн поддержка
https://t.me/s/joycasino_online_podderzghka
joycasino как выиграть
https://t.me/s/joycasino_kak_vyigrat
игровые автоматы joycasino
игровые автоматы joycasino
vavada. бонусы.
https://t.me/s/vavadaa_bonusy
казино вавада официальный сайт
https://t.me/s/casino_vavada_oficialnyi_sait
Great goods from you, man. I have consider your stuff previous to
and you are simply extremely great. I really like what you’ve
bought here, really like what you’re stating and the way wherein you say it.
You make it entertaining and you continue to take care of
to stay it sensible. I can not wait to learn much more from you.
That is actually a great web site.
joycasino онлайн казино joycasino игровые джойказино бонусы
joycasino онлайн казино joycasino игровые джойказино бонусы
joycasino com зеркало
joycasino com зеркало
джойказино слотов и бонусов обзор joycasino джой
джойказино слотов и бонусов обзор joycasino джой
vavada бонусы
vavada бонусы
казино онлайн вавада
https://t.me/s/casino_onlain_vavada
joycasino. официальный. сайт.
https://t.me/s/joycasino_oficialnyj_sajt
joycasino com отзывы
joycasino com отзывы
бонусы joycasino
https://t.me/s/bonusy_joycasino
промокод vavada
промокод vavada
бонусы. вавада. казино.
https://t.me/s/bonusy_vavada_casino
joycasino официальный зеркало на сегодня
https://t.me/s/joycasino_oficialnyi_zerkalo_nas
joycasino club
https://t.me/s/joycasino_club
бонус коды joycasino
https://t.me/s/bonus_kody_joycasino
vavada рабочее зеркало на сегодня
vavada рабочее зеркало на сегодня
бездепозитные промокоды казино вавада
https://t.me/s/bezdepositnye_promokody_kazino_v
vavada рабочее зеркало сегодня
https://t.me/s/vavada_rabochee_zerkalo_segodnia
joycasino бонусы
joycasino бонусы
joycasino no deposit bonus code
joycasino no deposit bonus code
бонус joycasino
бонус joycasino
Hello, yes this post is in fact nice and I have learned lot of things from it concerning blogging.
thanks.
онлайн казино вавада вход
онлайн казино вавада вход
vavada вход в личный кабинет
vavada вход в личный кабинет
joycasino бонус
joycasino бонус
bonus code joycasino
https://t.me/s/bonus_code_joycasino
joycasino играть на деньги
https://t.me/s/joycasino_igrat_na_dengi
vavada скачать
https://t.me/s/vavada_skachat
казино вавада онлайн
https://t.me/kazino_vavada_onlajn
joycasino бонус код на бесплатные вращения
https://t.me/s/joycasino_bonus_kod_nabesplatnye
бесплатно казино joycasino автоматы
https://t.me/s/besplatno_kazino_joycasino_avtom
joycasino казино казино джой joycasino промокод 2022
https://t.me/s/joycasino_casino_casino_joycasin
скачать vavada
https://t.me/s/skachat_vavada
казино rox
https://t.me/s/casino_rox1
joycasino бонус код 2017
joycasino бонус код 2017
vavada casino мобильная версия
https://t.me/s/vavada_mobilnaya_versiya1
joycasino кэшбэк как получить
https://t.me/s/joycasino_cashback_kak_polychit
зеркало riobet
зеркало riobet
sol stars казино
https://t.me/s/sol_stars_kazino
vavada казино зеркало на сегодня
https://t.me/s/vavada_kazino_zerkalo_na_segodny
joycasino бонус код
https://t.me/s/joycasino_bonus_kod
слоты riobet
слоты riobet
joycasino бонусы за регистрацию
joycasino бонусы за регистрацию
vavada.
vavada.
sol казино зеркало на сегодня
sol казино зеркало на сегодня
joycasino bonus code
https://t.me/s/joycasino_bonus_code
сайт riobet casino
сайт riobet casino
joycasino bonus codes
joycasino bonus codes
vavada casino online
vavada casino online
sol казино зеркало
https://t.me/s/sol_kazino_zerkalo
joycasino бездепозитный бонус 2022
joycasino бездепозитный бонус 2022
промокоды riobet
https://t.me/s/rpomokodi_riobet
vavada online
vavada online
joycasino 1000 рублей
joycasino 1000 рублей
sol казино вход
sol казино вход
joycasino бездепозитный бонус
joycasino бездепозитный бонус
vavada зеркало рабочее
https://t.me/s/vavada_zerkalo_rabochee
riobet zerkalo
riobet zerkalo
честный joycasino проверка joycasino промокод 2022
честный joycasino проверка joycasino промокод 2022
погасить штраф точка рф это веб сайт,
который позволяет проверить и оплатить
штрафы за нарушение правил дорожного движения.
На сайте можно найти информацию проверка штрафов гибдд онлайн о штрафах по номеру
водительского удостоверения или СТС.
Сервис предоставляет удобный поиск штрафов по
различным параметрам, таким как номер водительского удостоверения или свидетельства
о регистрации транспортного средства.
После оплаты штрафа, пользователь может проверить статус платежа
и просмотреть историю своих платежей.
Основная задача сайта помочь водителям
своевременно оплачивать штрафы
и избегать нежелательных последствий.
vavada казино официальный сайт вход
vavada казино официальный сайт вход
sol казино скачать
sol казино скачать
joycasino бесплатно
joycasino бесплатно
riobet вывод средств
https://t.me/s/riobet_vyvod_sredstv
бонус код в казино joycasino
https://t.me/s/bonus_kod_vkazino_joycasino
vavada зеркало новое
https://t.me/s/vavada_zerkalo_novoe
joycasino 2022
joycasino 2022
sol казино регистрация
https://t.me/s/sol_kazino_registraciya
riobet телеграмм
riobet телеграмм
vavada промокод сегодня
vavada промокод сегодня
бонус. код. joycasino.
бонус. код. joycasino.
1303 joycasino зеркало
https://t.me/s/joycasino1303_zerkalo
sol казино рабочее зеркало на сегодня
https://t.me/s/sol_kazino_rabochee_zerkalo_na_s
riobet.
riobet.
vavada официальный сайт зеркало
vavada официальный сайт зеркало
бесплатные игровые автоматы joycasino
https://t.me/s/besplatnye_igrovye_avtomaty_joyc
casino joycasino
casino joycasino
sol казино рабочее зеркало
sol казино рабочее зеркало
vavada войти
https://t.me/s/vavada_vojti
автоматы joycasino
автоматы joycasino
бонусы в казино joycasino
https://t.me/s/bonysy_v_kazino_joycasino
sol казино промокод
sol казино промокод
vavada casino – официальный сайт
https://t.me/vavada_casino_oficialnyj_sajt
vavada сайт
https://t.me/s/vavada_sajt
бонусный код joycasino
https://t.me/s/bonusnyj_kod_joycasino
www. riobet. com.
https://t.me/s/www_riobet_com
sol казино партнерка
sol казино партнерка
vavada casino зеркало
vavada casino зеркало
бонус код joycasino
бонус код joycasino
riobet зеркала
riobet зеркала
sol казино отзывы
https://t.me/s/sol_kazino_otzyvy
casino vavada
casino vavada
riobet промокоды
https://t.me/s/riobet_promokody
бонус код для joycasino
бонус код для joycasino
sol казино онлайн
sol казино онлайн
riobet вход на сайт
riobet вход на сайт
vavada ru
vavada ru
riobet промокод 2017
riobet промокод 2017
vavada вход
vavada вход
sol казино официальный сайт
https://t.me/s/sol_kazino_oficialnyj_sajt
riobet. вход.
https://t.me/s/riobet_vhodd
riobet зеркало сайта
https://t.me/s/riobet_zerkalo_saita
riobet промо код
riobet промо код
vavada казино официальный сайт
vavada казино официальный сайт
sol казино
https://t.me/s/sol_kazinoo
riobet скачать на андроид
https://t.me/s/riobet_skachat_na_android
riobet зеркало рабочее
riobet зеркало рабочее
riobet онлайн казино бездепозитный бонус
riobet онлайн казино бездепозитный бонус
vavada com
vavada com
sol казино бонус
sol казино бонус
riobet промокод фриспины
riobet промокод фриспины
riobet зеркало 2023
riobet зеркало 2023
vavada мобильная
https://t.me/s/vavada_mobilnaya
riobet онлайн казино промокод
https://t.me/s/riobet_onlain_kazino_promokod
sol казино актуальное зеркало
https://t.me/s/sol_kazino_aktualnoe_zerkalo
riobet промокод 2022
https://t.me/s/riobet_promokod_2022
vavada casino официальный сайт
vavada casino официальный сайт
riobet зеркало 2021
https://t.me/s/riobet_zerkalo_2021
riobet онлайн казино официальный сайт бездепозитный бонус
riobet онлайн казино официальный сайт бездепозитный бонус
vavada online casino
https://t.me/s/vavada_online_casino
онлайн казино sol
онлайн казино sol
riobet promo code
riobet promo code
riobet скачать
https://t.me/s/riobet_skachat
riobet. официальный. сайт.
https://t.me/s/riobet_oficialnyi_sait
казино vavada
казино vavada
обзор sol казино
https://t.me/s/obzor_sol_kazino
riobet онлайн казино бездепозитный
https://t.me/s/riobet_online_kazino_bezdepositt
riobet регистрация
https://t.me/s/riobet_registraciya
riobet казино зеркало
riobet казино зеркало
vavada официальный
vavada официальный
обзор казино сол проверка и казино sol сол казино бонусы
https://t.me/s/obzor_kazino_sol_proverkaIkazino
реальный обзор онлайн riobet
https://t.me/s/riobet_realnyj_obzor_onlajn_riob
riobet казино сайт
riobet казино сайт
riobet casino украина
https://t.me/s/riobet_kazino_ukraina
vavada промокод
vavada промокод
казино sol зеркало
https://t.me/s/kazino_sol_zerkalo
riobet рабочее зеркало
https://t.me/s/riobet_rabochee_zerkalo
vavada мобильная версия
https://t.me/s/vavada_mobilnaya_versiya
riobet как отыграть бонус
riobet как отыграть бонус
riobet онлайн казино бездепозитный бонус за регистрацию
https://t.me/s/riobet_kazino_bezdepositnyi_bonu
казино сол слотов и казино sol онлайн сол казино отзывы
казино сол слотов и казино sol онлайн сол казино отзывы
vavada казино онлайн
https://t.me/s/vavada_kazino_onlajn
riobet отзывы
riobet отзывы
riobet com зеркало
riobet com зеркало
vavada регистрация
https://t.me/s/vavada_registraciya
казино сол слотов и бонусов казино sol сол казино отзывы
казино сол слотов и бонусов казино sol сол казино отзывы
riobet онлайн казино
riobet онлайн казино
riobet бонус за регистрацию
https://t.me/s/riobet_bonus_zaregistraciyu
vavada telegram
vavada telegram
казино сол слотов и бонусов казино sol онлайн сол казино
казино сол слотов и бонусов казино sol онлайн сол казино
riobet мобильный
https://t.me/s/riobet_mobilnyi
riobet. бонус. код.
riobet. бонус. код.
vavada зеркало на сегодня
vavada зеркало на сегодня
казино sol отзывы
казино sol отзывы
riobet мобильная версия
riobet мобильная версия
riobet affilates
https://t.me/s/riobet_affilates
vavada зеркало 2022
vavada зеркало 2022
Spot on with this write-up, I truly believe this web site needs much more attention. I’ll
probably be returning to see more, thanks for the info!
казино sol онлайн
казино sol онлайн
riobet минимальное пополнение
riobet минимальное пополнение
riobet 96.com
riobet 96.com
I constantly spent my half an hour to read this blog’s articles or reviews every day
along with a mug of coffee.
казино sol официальный сайт регистрация
казино sol официальный сайт регистрация
riobet казино онлайн
https://t.me/s/riobet_kazino_online
riobet 95.com
https://t.me/s/riobet_95com
казино sol официальный сайт онлайн играть
https://t.me/s/kazino_sol_oficialnyj_sajt_onlaj
riobet 71 зеркало
https://t.me/s/riobet_71zerkalo
riobet игровые автоматы
https://t.me/s/riobet_igrovye_avtomaty
vavada промокод 2022 без депозита
vavada промокод 2022 без депозита
riobet каппер
riobet каппер
казино сол обзор слотов и казино sol сол казино отзывы
казино сол обзор слотов и казино sol сол казино отзывы
riobet 70 зеркало
https://t.me/s/riobet_70_zerkalo
riobet фриспины
https://t.me/s/riobet_freespiny
казино сол обзор слотов и казино sol онлайн сол казино
казино сол обзор слотов и казино sol онлайн сол казино
riobet 70
riobet 70
riobet com
https://t.me/s/riobet_com
казино сол обзор слотов и бонусов казино sol сол казино
казино сол обзор слотов и бонусов казино sol сол казино
riobet com онлайн казино
riobet com онлайн казино
riobet 47
riobet 47
riobet. бонус. за. регистрацию.
riobet. бонус. за. регистрацию.
казино сол обзор новых и rtp слотов sol сол казино бонусы
казино сол обзор новых и rtp слотов sol сол казино бонусы
riobet casino вход
https://t.me/s/riobet_casio_vhod
riobet 46
https://t.me/s/riobet_46
riobet бонусы
https://t.me/s/riobet_bonusy
казино сол обзор новых и rtp sol casino сол казино бонусы
https://t.me/s/kazino_sol_obzor_novyh_i_rtp_sol
riobet 139.com
riobet 139.com
riobet casino промокод
https://t.me/s/riobet_casino_promokod
riobet бонус
riobet бонус
казино сол обзор новых и rtp слотов sol casino сол казино
казино сол обзор новых и rtp слотов sol casino сол казино
riobet 113
https://t.me/s/riobet_113
riobet casino отзывы
riobet casino отзывы
riobet бездепозитный бонус 1000 рублей
https://t.me/s/riobet_bezdepositnyi_bonus1000
казино сол обзор новых бонусов и rtp sol сол казино бонусы
https://t.me/s/kazino_sol_obzor_novyh_bonusov_i
riobet 111
riobet 111
riobet casino no deposit bonus codes
https://t.me/s/riobet_casino_no_deposit_bonus_c
riobet affiliates
riobet affiliates
казино сол обзор новых бонусов и rtp sol casino сол казино
https://t.me/s/kazino_sol_obzor_novyh_bonusov
riobet 107.com
riobet 107.com
riobet casino бонус код
riobet casino бонус код
riobet 98.com
riobet 98.com
казино сол обзор и казино sol онлайн сол казино отзывы
https://t.me/s/kazino_sol_obzor_i_kazino_sol_on
реальный обзор казино казино riobet казино отзывы
реальный обзор казино казино riobet казино отзывы
riobet бот отзывы
riobet бот отзывы
riobet 97.com
riobet 97.com
казино сол обзор и бонусов казино sol онлайн сол казино
https://t.me/s/kazino_sol_obzor_i_bonusov_kazin
промокоды riobet казино
https://t.me/s/promokody_riobet_kazino
riobet 94.com
https://t.me/s/riobet_94_com
казино сол обзор и бонусов казино sol сол казино отзывы
https://t.me/s/kazino_sol_obzor_i_bonusov_casin
онлайн казино riobet
онлайн казино riobet
riobet бездепозитный бонус 2022
https://t.me/s/riobet_bezdepozitnyj_bonus_2022
riobet 93
https://t.me/s/riobet_93
казино sol обзор
https://t.me/s/kazino_sol_obzor
обзор риобет онлайн riobet риобет
обзор риобет онлайн riobet риобет
riobet 94
https://t.me/s/riobet_94
riobet 80
riobet 80
казино sol
https://t.me/s/kazino_soll
обзор риобет онлайн riobet риобет отзывы
https://t.me/s/obzor_riobet_onlainkazino
Hello there, just became alert to your blog through Google, and found that it is truly informative.
I am gonna watch out for brussels. I will appreciate if you continue this in future.
A lot of people will be benefited from your writing. Cheers!
riobet 92
riobet 92
riobet 500 рублей
https://t.me/s/riobet_500rublei
казино сол и бонусов казино sol онлайн сол казино отзывы
казино сол и бонусов казино sol онлайн сол казино отзывы
обзор риобет riobet риобет отзывы
обзор риобет riobet риобет отзывы
riobet 127.com
https://t.me/s/riobet127_com
riobet 81 зеркало
https://t.me/s/riobet_81_zerkalo
казино sol casino
https://t.me/s/kazino_sol_casino
обзор казино riobet
https://t.me/s/obzor_kazino_riobett
riobet 125.com
riobet 125.com
riobet 79
https://t.me/s/riobet_79
казино сол бонусов и rtp слотов sol casino сол казино бонусы
казино сол бонусов и rtp слотов sol casino сол казино бонусы
и обзор игровых автоматов онлайн riobet
и обзор игровых автоматов онлайн riobet
riobet 111.com
riobet 111.com
sol. казино.
sol. казино.
riobet 78.com
https://t.me/s/riobet_78_com
казино sol бездепозитный бонус
https://t.me/s/kazino_sol_bezdepozitnyj_bonus
лицензионные игровые автоматы riobet
лицензионные игровые автоматы riobet
sol казино онлайн вход
https://t.me/s/sol_kazino_onlajn_vhod
riobet 108
riobet 108
riobet 77 com
https://t.me/s/riobet_77_com
игровые автоматы sol казино
игровые автоматы sol казино
казино riobet промокод
казино riobet промокод
sol казино онлайн отзывы
https://t.me/s/sol_kazino_onlajn_otzyvy
riobet 75
riobet 75
riobet. 75.
riobet. 75.
игры с живым дилером riobet
игры с живым дилером riobet
слот Book of Ra
https://medium.com/@c7h.css/игровой-автомат-book-of-ra-играть-в-слот-бесплатно-или-на-деньги-b1a0ff1b8194
sol казино официальный сайт в россии
sol казино официальный сайт в россии
реальный обзор riobet отзывы
реальный обзор riobet отзывы
riobet 137
https://t.me/s/riobet_137
I couldn’t refrain from commenting. Very well written!
sol казино форум отзывы
https://t.me/s/sol_kazino_forum_otzyvy
casino riobet бездепозитный бонус
https://t.me/s/casino_riobet_bezdepositnuibonus
слот Zeus
игровой автомат Zeus
реальный онлайн riobet отзывы
реальный онлайн riobet отзывы
sol казино бездепозитный бонус за регистрацию
sol казино бездепозитный бонус за регистрацию
riobet 134.com
https://t.me/s/riobet_134_com
игровой автомат Ultra Hot Deluxe
Ultra Hot Deluxe
Hi there! Do you know if they make any plugins to assist with
SEO? I’m trying to get my blog to rank for some targeted
keywords but I’m not seeing very good gains. If you know of any please share.
Thanks!
промокод riobet
промокод riobet
sol казино бездепозитный бонус
sol казино бездепозитный бонус
Way cool! Some extremely valid points! I appreciate you penning this article plus the
rest of the site is very good.
My brother recommended I might like this web site. He was totally right.
This post truly made my day. You cann’t imagine just how much
time I had spent for this info! Thanks!
riobet 133.com
https://t.me/s/riobet_133_com
It’s an amazing paragraph in favor of all the web viewers;
they will take advantage from it I am sure.
слот Ultra Hot
https://medium.com/@cameron689239528/игровой-автомат-ultra-hot-играть-в-слот-бесплатно-или-на-деньги-21dae7677b43
популярные слоты на riobet
https://t.me/s/popularnye_sloty_nariobet
промокод в казино sol
промокод в казино sol
Thank you for the good writeup. It actually was a leisure account it.
Look advanced to far added agreeable from you!
By the way, how could we keep in touch?
riobet 133
https://t.me/s/riobet_133
партнерка sol казино
https://t.me/s/partnerka_sol_kazino
официальный сайт казино riobet
https://t.me/s/oficialnyj_sajt_kazino_riobet
отзывы о казино sol
отзывы о казино sol
обзор казино риобет казино riobet риобет казино
обзор казино риобет казино riobet риобет казино
riobet 129.com
https://t.me/s/riobet_129com
обзор казино sol
https://t.me/s/obzor_kazino_sol
обзор онлайн riobet отзывы
https://t.me/s/obzor_onlajn_riobet_otzyvy
онлайн казино без верификации
https://clickrabota.ru
riobet 126.com
https://t.me/s/riobet_126com
казино sol скачать
https://t.me/s/kazino_sol_skachat
игровой автомат Thunderstruck II
слот Thunderstruck II
обзор казино казино riobet казино отзывы
https://t.me/s/obzorkazino_riobet_otzyvy
riobet 125
riobet 125
казино сол проверка и онлайн казино sol сол казино бонусы
https://t.me/s/kazino_sol_proverka_i_onlajn_kaz
слот The Money Game
игровой автомат The Money Game
обзор казино онлайн казино riobet казино
обзор казино онлайн казино riobet казино
казино sol официальный
https://t.me/s/kazino_sol_oficialnyj
riobet 121 com
riobet 121 com
слот Sweet Life
слот Sweet Life
казино sol играть
https://t.me/s/kazino_sol_igrat
казино. riobet.
https://t.me/s/kazin0_ri0bet
riobet 121
https://t.me/s/riobet_121
игровой автомат Starburst
Starburst
казино sol бонус за регистрацию
казино sol бонус за регистрацию
игровые автоматы riobet
https://t.me/s/igrovie_avtomaty_riobet
Russian porn
riobet 119
riobet 119
казино. sol.
казино. sol.
Sparta
https://medium.com/@akex.manzhiesky/sparta-игровой-автомат-для-игры-бесплатно-или-на-деньги-ccebfea0cfde
riobet casino бездепозитный бонус
riobet casino бездепозитный бонус
riobet 113 com
riobet 113 com
бонус код для казино sol
бонус код для казино sol
слот Siberian Storm
игровой автомат Siberian Storm
бесплатные игровые автоматы играть
https://groups.google.com/g/playonlinegamestop/c/xQO83lbmD28
freespin nasıl kullanılır
Free Spin Bonusu Nasıl Kullanılır
riobet 110
riobet 110
rock climber
https://medium.com/@mokoxoy716/игровой-автомат-rock-climber-играть-в-слот-бесплатно-или-на-деньги-d924fab177f3
riobet 108.com
https://t.me/s/riobet_108com
слот Rex
слот Rex
сайт riobet
https://t.me/s/sajt_riobet
играть бесплатно в игровые автоматы
https://groups.google.com/g/playonlinegamestop/c/t1Ti5o3Chfk
установить игровые автоматы
https://groups.google.com/g/playonlinegamestop/c/Ttb3iL-443Y
ในยุคที่เศรษฐกิจกำลังเติบโตอย่างก้าวกระโดด การลงทุนที่ดินกำลังเป็นทางเลือกที่น่าสนใจสำหรับนักลงทุนหลายคน ไม่ว่าจะเป็นการลงทุนในที่ดินทางการเกษตร, ที่ดินทางท่องเที่ยว, หรือที่ดินที่มีศักยภาพในการพัฒนาทางธุรกิจ ทำไมถึงมีการสนใจมากขนาดนี้?
ต่อไปนี้คือเหตุผลที่ทำให้การลงทุนที่ดินเป็นทางเลือกที่มีความน่าสนใจในปัจจุบัน:
ความมั่งคั่งของทรัพยากรที่ดิน: ที่ดินเป็นทรัพยากรที่สำคัญและจำเป็นสำหรับการพัฒนาทุนครองชนบทและเมือง ทำให้มีความต้องการที่ดินมากขึ้น การลงทุนที่ดินจึงเป็นการลงทุนที่มีศักยภาพในการรับผลกำไรอย่างมีนัยสำคัญ
การเติบโตของประชากร: การเพิ่มขึ้นของประชากรทำให้มีความต้องการในที่อยู่อาศัยและสถานที่ธุรกิจที่เพิ่มขึ้น
นักลงทุนที่ลงทุนในที่ดินที่มีศักยภาพสามารถได้รับประโยชน์จากการเติบโตของตลาดนี้
การพัฒนาทางธุรกิจและการท่องเที่ยว: ที่ดินที่ตั้งอยู่ในพื้นที่ที่มีศักยภาพทางธุรกิจและการท่องเที่ยวสามารถเป็นทรัพยากรที่มีมูลค่าสูง การลงทุนในที่ดินในพื้นที่เหล่านี้อาจเสนอโอกาสทางธุรกิจที่น่าสนใจ
ความเชื่อมั่นในการลงทุนที่ดิน: ที่ดินมักถือเป็นสินทรัพย์ที่มีความคงทนและเสถียร นักลงทุนที่มองหาการลงทุนที่มีความเสี่ยงน้อยมักพบว่าการลงทุนที่ดินเป็นทางเลือกที่ดี
การพัฒนาทางอินเทอร์เน็ต:
การเข้าถึงอินเทอร์เน็ตที่สะดวกสบายทำให้ตลาดที่ดินเป็นเรื่องง่ายขึ้น
นักลงทุนสามารถค้นหาและทำการซื้อขายที่ดินได้อย่างสะดวก
การลงทุนที่ดินไม่เพียงแค่เป็นการลงทุนที่มีความคงทนและเสถียร แต่ยังเป็นทางเลือกที่สามารถสร้างรายได้และมีศักยภาพในการเติบโตต่อไป นักลงทุนที่มองหาโอกาสทางการเงินและการพัฒนาทางธุรกิจควรพิจารณาการลงทุนที่ดินเป็นทางเลือกที่น่าสนใจในปัจจุบันและอนาคตที่กำลังจะมา.
реальный казино онлайн казино riobet казино отзывы
https://t.me/s/realnyj_kazino_onlajn_kazino_rio
игровой автомат resident
resident
riobet зеркало на сегодня
riobet зеркало на сегодня
top 5 casino
https://groups.google.com/g/youronlinegames/c/dFb_R-cZvlI
игровые автоматы слоты играть бесплатно без регистрации и смс онлайн
игровые автоматы слоты играть бесплатно без регистрации и смс онлайн
промокод riobet 2020
промокод riobet 2020
игровой автомат Reel King
https://medium.com/@greyson159804277/играть-в-слот-reel-king-на-деньги-или-демо-e57b960f97b4
riobet зеркало для входа
https://t.me/s/riobet_zerkalo_dlya_vhoda
คุณพระช่วย.com แพลตฟอร์มประมูลพระเครื่องที่มองเห็นอนาคตของผู้ชื่นชอบ และนิยมพระเครื่อง
เครื่องลาง ของขลัง ที่ต้องการช่องทางในการ ซื้อ-ขาย แลกเปลี่ยน พระเครื่อง
казино слоты бесплатно
https://groups.google.com/g/playonlinegamestop/c/JXRdMRS2fls
riobet зеркало 2022
riobet зеркало 2022
промокод на riobet
промокод на riobet
Excellent article! We are linking to this great article on our site.
Keep up the great writing.
игровой автомат Ramses 2
Ramses 2
riobet зеркало
https://t.me/s/riobet_zerkalo
игры казино играть бесплатно
https://groups.google.com/g/playonlinegamestop/c/lNATNEE02xc
промокод для riobet
https://t.me/s/promokod_dlya_riobet
игровой автомат pirate
слот pirate
riobet вход
riobet вход
игра в казино бесплатно
игра в казино бесплатно
обзор казино онлайн казино riobet казино отзывы
обзор казино онлайн казино riobet казино отзывы
Mega Moolah
https://medium.com/@melvin023967487/играть-в-слот-mega-moolah-на-деньги-или-демо-ee7220ded5b8
riobet рабочее зеркало на сегодня
https://t.me/s/riobet_rabochee_zerkalo_na_segod
This blog was… how do you say it? Relevant!! Finally I have found something that helped me.
Many thanks!
игры казино бесплатно
игры казино бесплатно
новые игровые автоматы riobet
новые игровые автоматы riobet
Mega Fortune
https://medium.com/@almodalmonds/игровой-автомат-mega-fortune-играть-в-слот-бесплатно-или-на-деньги-a92cbaa7d45d
riobet промокод
riobet промокод
It’s great that you are getting ideas from this paragraph as well
as from our dialogue made at this time.
казино играть бесплатно онлайн
https://groups.google.com/g/playonlinegamestop/c/ifXCjYEOYn0
ставки от 50 рублей
ставки от 50 рублей
Hurrah, that’s what I was searching for, what a data!
existing here at this website, thanks admin of this
website.
riobet online casino
riobet online casino
бездепозитный бонус riobet казино
https://t.me/s/bezdepozitnyj_bonus_riobet_kazin
Marco Polo
https://medium.com/@mokoxoy716/играть-в-слот-marco-polo-на-деньги-или-демо-c78140529cdc
riobet онлайн казино официальный сайт
riobet онлайн казино официальный сайт
игральные автоматы бесплатно
https://groups.google.com/g/playonlinegamestop/c/bwy63kBj7ww
ставки от 10 рублей
ставки от 10 рублей
игровой автомат lucky haunter
https://medium.com/@cadis53001/lucky-haunter-игровой-автомат-для-игры-бесплатно-или-на-деньги-6bb9270f3062
riobet casino зеркало
https://t.me/s/riobet_casino_zerkalo
лицензионные сайты казино
лицензионные сайты казино
играть онлайн игровые автоматы бесплатно
https://groups.google.com/g/playonlinegamestop/c/zIodUSHD964
список новых казино
https://groups.google.com/g/youronlinegames/c/ss3liTV9RR0
слот keks
https://medium.com/@vapavhedan/keks-загляните-в-мир-веселых-приключений-в-режиме-игры-на-деньги-или-демо-595d6f628d2b
riobet casino официальный сайт
https://t.me/s/riobet_casino_oficialnyj_sajt
азартные игровые автоматы бесплатно слоты
https://groups.google.com/g/playonlinegamestop/c/6b2WeI0ZUcw
список казино с бездепозитным бонусом
список казино с бездепозитным бонусом
лицензированное казино
https://groups.google.com/g/topgamesonline/c/lvGi-5XtNGk
Katana
https://medium.com/@aqxypcu/игровой-автомат-katana-играть-в-слот-бесплатно-или-на-деньги-5cf32693b98d
riobet casino
https://t.me/s/riobet_casin0
казино онлайн без регистрации
казино онлайн без регистрации
современные игровые автоматы
современные игровые автоматы
riobet бездепозитный бонус
https://t.me/s/riobet_bezdepozitnyj_bonus
Island
https://medium.com/@alexsq1990/играть-в-слот-island-на-деньги-или-демо-fec10bd473dc
аппараты игровые
аппараты игровые
скачать игры казино бесплатно без регистрации
скачать игры казино бесплатно без регистрации
riobet 95.com зеркало
https://t.me/s/riobet_95com_zerkalo
Immortal Romance
https://medium.com/@dkhowy/играть-в-слот-immortal-romance-на-деньги-или-демо-f6305208a280
игровые автоматы онлайн бесплатно сейчас
https://groups.google.com/g/playonlinegamestop/c/75nbXbALyNk
riobet 86 зеркало
riobet 86 зеркало
скачать 888 покер на андроид
скачать 888 покер на андроид
игровой автомат Gorilla
слот Gorilla
riobet 78 зеркало
riobet 78 зеркало
игра казино бесплатно
https://groups.google.com/g/playonlinegamestop/c/OjxC0BsX2mk
рублевые онлайн казино
рублевые онлайн казино
слот Gonzo’s Quest
https://medium.com/@podvonkanvon/погружение-в-золото-игровой-автомат-gonzos-quest-играть-в-слот-бесплатно-или-на-деньги-f06c4d530e19
лицензионные онлайн казино
лицензионные онлайн казино
riobet 78.com официальный сайт
https://t.me/s/riobet_78com_oficialnyj_sajt
игры игровые автоматы играть бесплатно
https://groups.google.com/g/playonlinegamestop/c/g0qEoiqst50
промокоды на казино
промокоды на казино
игровой автомат gnome
игровой автомат gnome
обзор лицензионных казино
обзор лицензионных казино
riobet 78
https://t.me/s/riobet78
приложение игровые автоматы
https://groups.google.com/g/youronlinegames/c/5V6SYH7cu_Y
riobet 76 зеркало
riobet 76 зеркало
gladiator
https://medium.com/@picurinvasilij066/gladiator-игровой-автомат-для-игры-бесплатно-или-на-деньги-b34485965cbf
новые бездепозитные бонусы в казино
новые бездепозитные бонусы в казино
показать все онлайн казино с минимальным депозитом
показать все онлайн казино с минимальным депозитом
riobet 65
riobet 65
слот garage
garage
новые казино с бездепозитными бонусами
новые казино с бездепозитными бонусами
играть в игровые автоматы без регистрации бесплатно
играть в игровые автоматы без регистрации бесплатно
riobet казино
https://t.me/s/ri0bet_kazino
игровой автомат Fruit Cocktail 2
https://medium.com/@valeriya220230/играть-в-слот-fruit-cocktail-2-на-деньги-или-демо-bec1b9f56081
новые казино с бездепом
https://groups.google.com/g/topgamesonline/c/oQxzNV9K1lE
игровые аппараты бесплатно онлайн
https://groups.google.com/g/playonlinegamestop/c/5Vurvz52iuo
Thanks a bunch for sharing this with all folks you actually recognize what
you are talking approximately! Bookmarked. Kindly additionally
visit my website =). We can have a link alternate agreement between us
riobet
riobet
игровой автомат fruit cocktail
https://medium.com/@sokew78312/игровой-автомат-fruit-cocktail-играть-в-слот-бесплатно-или-на-деньги-3c26a9bb4cd6
бездепозитний бонус
https://groups.google.com/g/topgamesonline/c/14TcEBlQ-0A
игровые автоматы без регистрации без смс
игровые автоматы без регистрации без смс
реальный обзор онлайн riobet отзывы
https://t.me/s/realnyj_obzor_onlajn_riobet_otzy
First off I want to say great blog! I had a quick question which I’d
like to ask if you don’t mind. I was curious to find out how
you center yourself and clear your thoughts prior to writing.
I have had a hard time clearing my mind in getting
my ideas out there. I do take pleasure in writing but it just seems
like the first 10 to 15 minutes are usually wasted just trying to figure out how to begin. Any recommendations or tips?
Cheers!
Fat Santa
слот Fat Santa
I was wondering if you ever thought of changing the structure of your website?
Its very well written; I love what youve got to say. But maybe you could a little more in the way of content so people could connect with it better.
Youve got an awful lot of text for only having 1 or 2 images.
Maybe you could space it out better?
бесплатные игровые аппараты онлайн
https://groups.google.com/g/playonlinegamestop/c/QHq_LuzwFUQ
riobet официальный сайт
riobet официальный сайт
бездепозитный бонус без вейджера
https://groups.google.com/g/topgamesonline/c/Y9c7To9zYHc
слот Eye of Horus
Eye of Horus
казино riobet
https://t.me/s/kazino_ri0bet
игры азартные автоматы играть бесплатно
https://groups.google.com/g/playonlinegamestop/c/37TO_y0ZvRU
слоты бездепозитный бонус
слоты бездепозитный бонус
онлайн казино с хорошей отдачей
https://groups.google.com/g/youronlinegames/c/8Csysr8_O-A
casino riobet
casino riobet
слот Dragons
https://medium.com/@lonfondugs/игровой-автомат-dragons-играть-в-слот-бесплатно-или-на-деньги-79867f0b2bbf
бесплатно игровые автоматы
https://groups.google.com/g/playonlinegamestop/c/QDt1faYhRrs
bezdepov
bezdepov
новые бездепозитные бонусы казино
новые бездепозитные бонусы казино
игровой автомат Dolphins Pearl Deluxe
https://medium.com/@tirocav600/играть-в-слот-dolphins-pearl-deluxe-на-деньги-или-демо-24a073a09a6e
играть в аппараты бесплатно
https://groups.google.com/g/playonlinegamestop/c/EJtFXUxSaUw
бонус без вейджера
бонус без вейджера
моментальные выплаты казино
https://groups.google.com/g/youronlinegames/c/z6bJerClAVU
игровой автомат Dead or Alive
игровой автомат Dead or Alive
бездепозитный бонус казино 2021
https://groups.google.com/g/topgamesonline/c/qepDc2kanhk
минимальный депозит 10 рублей
https://groups.google.com/g/youronlinegames/c/9PWTTebAMEo
игровые аппараты бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/5_WqFZgrrJY
Crazy Monkey 2
слот Crazy Monkey 2
лицензионные казино онлайн в россии
https://groups.google.com/g/youronlinegames/c/c7cwAT7_Xv8
аппараты игровые бесплатно
https://groups.google.com/g/topgamesonline/c/GT9SrMj9w84
слоты играть бесплатно и без регистрации
слоты играть бесплатно и без регистрации
игровой автомат crazy monkey
игровой автомат crazy monkey
URL
Keywords سمساری
Blog_Comment برخی از افراد هم تمایل دارند
تا در هزینههای خود صرفه جویی
کرده و لوازم سرمایشی و گرمایشی
خود را به صورت دست دوم تهیه میکنند.
Anchor_Text سمساری
Image_Comment بهترین سمساری پاسداران منطقه 3 تهران با
اکتفا به تجربه شخصی و جمعی، کسی است که بتواند
در عین داشتن تخصص بالا، بهترین بازدهی را برای متقاضیان
در ارائه خدمات سمساری داشته باشد.
Guestbook_Comment پس از انجام قیمت گذاری حرفه ای مشاوره رایگان
به شما ارایه خواهد شد.
Category uncategorized
Micro_Message هم اکنون با ما در ارتباط
باشید تا اجناس منزل شما را با بیشترین قیمت خریداری کنیم.
About_Yourself 41 yr old Research Assistant III Dolph
Dilger, hailing from Cowansville enjoys watching movies like Investigating Sex (a.k.a.
Intimate Affairs) and Coffee roasting. Took a trip to Phoenix Islands Protected Area and drives a Sierra 3500.
Forum_Comment طرحهای بسیار ظریف و نفیسی که بر روی قالیهای دستباف
توسط هنرمندان کاشانی پیاده میشود موجب این محبوبیت شده است ، بهگونهای که شهر کاشان
در عهد صفویه یکی از فاخرترین
و بهترین مراکز تولید فرش و قالی
دستباف بوده است.
Forum_Subject سمساری غرب تهران ️ خریدار کلیه لوازم منزل
09191162420
Video_Title سمساری زرتشت 09121013304
خریدار لوازم منزل یکجا و نقدی
سمساری زرتشت
Video_Description شما به راحتی می توانید با استفاده از این سایت در سریع ترین زمان ممکن اجناس قدیمی خود را بفروشید و پول نقد دریافت نمایید.
Preview_Image
YouTubeID
Website_title عتیقه فروشی های تهران-معرفی بیش از 10مورد ازبهترین های ایران
Description_250 بسیاری از این افراد به لوازم جانبی سنتی مانند فرش دستباف اهمیت
می دهند.
Guestbook_Comment_(German)
Description_450 سمساری جعفری نیز از جمله مراکز خرید و فروش لوازم دست دوم می باشد که می توانید به سایت به آدرس semsarijafari.com مراجعه نموده و با شعبات مختلف آن در سراسر تهران جهت خرید و یا فروش لوازم دست دوم
خود تماس حاصل نمایید.
Guestbook_Title تماس با ما سمساری سمساری تهران سمساری شرق تهران سمساری شمال تهران
Website_title_(German)
Description_450_(German)
Description_250_(German)
Guestbook_Title_(German)
Image_Subject بهترین سمساری در اصفهان آدرس و تلفن جابکال
Website_title_(Polish)
Description_450_(Polish)
Description_250_(Polish)
Blog Title 10 بهترین فروشگاه عتیقه در
تهران بهترینو آذر 1402
Blog Description سمساری در پاسداران منطقه 3 محدوده شمال تهران سمساری آنلاین تهران ایران نشنال
Company_Name سمساری
Blog_Name سمساری سمساری تهران خریدار لوازم
منزل 09122305924
Blog_Tagline سمساری تهران سمساری
آنلاین سمساری در تهران 09122725127
️ شماره سمساری تهران
Blog_About 58 yr old Human Resources Assistant IV Tessa Shadfourth, hailing from
Manitouwadge enjoys watching movies like Red Lights and Rafting.
Took a trip to Longobards in Italy. Places of the Power (- A.D.) and drives a
De Dion, Bouton et Trépardoux Dos-à -Dos Steam Runabout “La Marquise”.
Article_title سمساری غرب تهران ️ خریدار
کلیه لوازم منزل 09191162420
Article_summary این زبان در آلمان، اتریش، بخشی از سوئیس، تیرول جنوبی (ایتالیا)، بخشی از بلژیک و لیختن اشتاین
زبان رسمی به حساب می آید.
Article اگر فروشنده یک جنس دست دوم
باشید و یا خریدار آن، احتمالا با
تجربه سختی تعیین قیمت این اجناس رو
به رو شده اید. لوازم نو همواره در
همه فروشگاه ها و سایت ها به قیمت های مقطوع و مشخصی به فروش
می رسند؛ اما این قاعده برای خرید و
فروش لوازم دست دوم ، صدق نمی کند.
سمساری یا همان امانت فروشی محلی به خرید و فروش لوازم دست دوم گفته میشود.
این نوع خرید و فروش از زمان های خیلی دور
در ایران مرسوم بوده است.
به خاطر داشته باشید که برخی از عیوب مانند رنگ پریدگی ممکن است باعث ارزانتر
شدن کالا شوند، اما اطمینان از اینکه آیتم
همچنان کاربردی است یا در صورت نیاز به راحتی
قابل تعمیر است، ضروری است.
در این مقاله به معرفی عتیقه فروشی های تهران و برخی نکات دیگر پرداختیم.
باید در صورت لزوم از یک کارشناس و متخصص در زمینه عتیقه مشاوره بگیرید.
توجه به این نکته مهم است که در حالی که لوازم
دست دوم می توانند مزایایی را ارائه دهند، محدودیت های
بالقوه ای نیز وجود دارد. این موارد ممکن است شامل پوشش گارانتی محدود، گزینه های کمتر برای آخرین ویژگی ها یا بهره وری انرژی، و انتخاب
متغیر بسته به موجودی فروشگاه باشد.
با این حال، برای بسیاری از مردم، مزایای صرفه
جویی در هزینه و اثرات زیست محیطی بیشتر از
این محدودیت ها است.
About_Me 33 year old Project Manager Garwood Marlor, hailing from
MacGregor enjoys watching movies like Death at a Funeral and Gambling.
Took a trip to Historic Centre of Mexico City and Xochimilco and drives
a Bentley Litre Le Mans Sports ‘Bobtail’.
About_Bookmark 39 year old VP Product Management Leland Prawle, hailing from Manitou enjoys
watching movies like Euphoria (Eyforiya) and Bodybuilding.
Took a trip to Timbuktu and drives a Wrangler.
Topic سمساری
Magnificent beat ! I would like to apprentice while you amend your
site, how can i subscribe for a blog website? The account helped me a applicable deal.
I have been tiny bit familiar of this your broadcast
offered brilliant transparent concept
казино на андроид
https://groups.google.com/g/youronlinegames/c/FhOObv-AftM
игровой автамат
игровой автамат
играть слоты бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/ZwX_EmHX1Z0
слот Columbus Deluxe
https://medium.com/@mepic95460/игровой-автомат-columbus-deluxe-играть-в-слот-бесплатно-или-на-деньги-80c3e401edb9
казино моментальный вывод
https://groups.google.com/g/youronlinegames/c/LoFlGxmQQdM
бесплатные казино
бесплатные казино
игровые автоматы играть без регистрации бесплатно
игровые автоматы играть без регистрации бесплатно
слот Columbus
https://medium.com/@businpoia/columbus-игровой-автомат-для-игры-бесплатно-или-на-деньги-0d0b4294f9e3
новые игровые автоматы играть бесплатно
https://groups.google.com/g/playonlinegamestop/c/w3Aaqr0ewt8
азартные игровые автоматы бесплатно без регистрации онлайн
https://groups.google.com/g/onlinegamestop/c/DvONGjB_toE
казино бонус без депозита
казино бонус без депозита
бесплатные игровые автоматы слоты
бесплатные игровые автоматы слоты
слот cleopatra
игровой автомат cleopatra
играть бесплатно казино
играть бесплатно казино
игры слот бесплатно
игры слот бесплатно
игры с моментальным выводом денег
игры с моментальным выводом денег
игровые автоматы аппараты
игровые автоматы аппараты
Excellent article. I will be experiencing some of these issues as well..
слот играть бесплатно
слот играть бесплатно
Champagne
игровой автомат Champagne
азартные бесплатные игры
https://groups.google.com/g/playonlinegamestop/c/DjBukN0UXgQ
игры на деньги онлайн с выводом денег
игры на деньги онлайн с выводом денег
играть слот игровой онлайн
играть слот игровой онлайн
казино игровые автоматы играть бесплатно
казино игровые автоматы играть бесплатно
слот Casanova
https://medium.com/@jivosar797/игровой-автомат-casanova-играть-в-слот-бесплатно-или-на-деньги-4e83b2bb7891
игры онлайн казино игровые автоматы бесплатно
https://groups.google.com/g/playonlinegamestop/c/Dl9aC4V8KRk
My partner and I stumbled over her coming froim a different paage aand
thouught I should check tgings out. I like what I see sso i
am just following you. Look forwawrd to lopoking into your
weeb pagte repeatedly.
игровые автоматы скачать бесплатно
https://groups.google.com/g/playonlinegamestop/c/ocZwzSvR-ZM
vurcazkircazpatliycaz.5X9B7F7d5xtX
играть казино онлайн бесплатно игровые автоматы
https://groups.google.com/g/topgamesonline/c/0Gu2K_q4etU
новые игровые автоматы бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/jTBYWwREgCU
слот Caribbean Holidays
https://medium.com/@reidbrashennahfawnconr/caribbean-holidays-игровой-автомат-для-игры-бесплатно-или-на-деньги-5b8f48b9311c
игровые автоматы играть бесплатно и регистрации
https://groups.google.com/g/playonlinegamestop/c/tNR4o1uA0TY
игровые автоматы с бездепозитным бонусом за регистрацию
https://groups.google.com/g/youronlinegames/c/YflQJpo-T0c
автоматы играть онлайн бесплатно
https://groups.google.com/g/onlinegamestop/c/0WHbfV7aOCY
играть в новые игровые автоматы
https://groups.google.com/g/topgamesonline/c/HLcP99TsYa0
скачать игровые автоматы бесплатно без регистрации
скачать игровые автоматы бесплатно без регистрации
игровой автомат Bullion Bars
Bullion Bars
игровой автомат бесплатно
игровой автомат бесплатно
игровые автоматы онлайн без денег
игровые автоматы онлайн без денег
скачать бесплатные игровые автоматы
скачать бесплатные игровые автоматы
Medications – Unraveling the Complexity of Autoimmune Diseases Buy Cheap Clomid
азартные игры бесплатно без регистрации
https://groups.google.com/g/playonlinegamestop/c/W5SjBW5yT5k
Book of Ra Deluxe
слот Book of Ra Deluxe
играть бесплатно автоматы
https://groups.google.com/g/onlinegamestop/c/dTLH1kI-dsM
игровые автоматы бесплатно играть
игровые автоматы бесплатно играть
игровые автоматы бесплатно игры
https://groups.google.com/g/topgamesonline/c/2IfhKbHd0_w
демо игровые автоматы бесплатно
демо игровые автоматы бесплатно
игровые автоматы слоты без регистрации
https://groups.google.com/g/onlinegamestop/c/nOv7vyz2LFo
игровой автомат Bonanza
слот Bonanza
игровой автомат
https://groups.google.com/g/playonlinegamestop/c/COo5m2rpYAs
слот игры бесплатно
слот игры бесплатно
автоматы онлайн бесплатно
https://groups.google.com/g/onlinegamestop/c/hDhcljzuu4Q
играть игровые автоматы бесплатно онлайн
играть игровые автоматы бесплатно онлайн
игровой автомат Bananas Go Bahamas
https://medium.com/@aleksandraborovaa4/bananas-go-bahamas-игровой-автомат-для-игры-бесплатно-или-на-деньги-9d443e6cb196
игровой аппарат
игровой аппарат
бесплатные казино игры без регистрации
https://groups.google.com/g/onlinegamestop/c/RhMMwFxZ4rU
Aztec Gold
игровой автомат Aztec Gold
играть в игровые автоматы бесплатно без регистрации
играть в игровые автоматы бесплатно без регистрации
бесплатные азартные игры
бесплатные азартные игры
играть бесплатно онлайн казино
играть бесплатно онлайн казино
Attila
https://medium.com/@artilorrairthewynellkling/играть-в-слот-attila-на-деньги-или-демо-da0085150852
играть игровые автоматы онлайн
играть игровые автоматы онлайн
играть в слоты бесплатно и без регистрации
играть в слоты бесплатно и без регистрации
новые игровые автоматы бесплатно
https://groups.google.com/g/topgamesonline/c/mx1Q_SCBtDc
играть в игровые автоматы бесплатно и без регистрации онлайн
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/ZeGgYXDRsXM
играть в автоматы бесплатно без регистрации
играть в автоматы бесплатно без регистрации
играть автоматы бесплатно
играть автоматы бесплатно
игры азартные автоматы бесплатно
https://groups.google.com/g/topgamesonline/c/Ra2SfUhT5uI
Howdy! This post could not be written any better!
Looking at this article reminds me of my previous roommate!
He always kept preaching about this. I will forward this article to him.
Pretty sure he’s going to have a good read. Many thanks for sharing!
Here is my blog … Massage Forum
игровые автоматы играть бесплатно сейчас
https://groups.google.com/g/onlinegamestop/c/7XboCqqtZ-o
google игровые автоматы бесплатные
google игровые автоматы бесплатные
daktilogibigibi.ejgLjgliFjUf
автоматы игровые играть бесплатно онлайн
автоматы игровые играть бесплатно онлайн
играть бесплатно слоты
играть бесплатно слоты
играть игровые автоматы бесплатно без регистрации
играть игровые автоматы бесплатно без регистрации
где за регистрацию платят деньги которые можно сразу вывести
где за регистрацию платят деньги которые можно сразу вывести
игровые аппараты слоты онлайн бесплатно
https://groups.google.com/g/topgamesonline/c/9B2cntHCC68
игральные автоматы играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/QJC0uOKRjFg
бонусы в казино без депозита
бонусы в казино без депозита
casino бездепозитный бонус
casino бездепозитный бонус
бесплатные игры казино
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/PgyhCvPfq5c
слоты игровые автоматы играть онлайн бесплатно
https://groups.google.com/g/topgamesonline/c/4qgauPAr4Fc
I’m really enjoying the theme/design of your weblog.
Do you ever run into any internet browser compatibility issues?
A small number of my blog readers have complained about my blog not
operating correctly in Explorer but looks great in Safari.
Do you have any suggestions to help fix this problem?
daxktilogibigibi.rvNdH8pAhksq
бездепы казино
бездепы казино
бонус за регистрацию казино
бонус за регистрацию казино
бесплатные игровые автоматы казино онлайн
бесплатные игровые автоматы казино онлайн
играть бесплатно и без регистрации в игровые автоматы
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/MMyNfgq8eFw
бесплатно игровые аппараты
https://groups.google.com/g/topgamesonline/c/4X3WoBv5MfM
бонусы за регистрацию казино
бонусы за регистрацию казино
фриспины без депозита с выводом
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/vqKGQdaUQxI
демо игровые автоматы без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/-NHn698R2as
онлайн казино играть бесплатно
онлайн казино играть бесплатно
азартные игры автоматы бесплатно
азартные игры автоматы бесплатно
игры игровые аппараты
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/7gvETB0V_J4
бонус в казино без депозита
бонус в казино без депозита
казино с бесплатным бонусом
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/dEU7SsEcWqw
игровые аппараты слоты бесплатно
игровые аппараты слоты бесплатно
играть в аппараты бесплатно без регистрации
https://groups.google.com/g/topgamesonline/c/-2XI55XoEX0
играть в автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/oHBexUayXM4
бонус коды казино
https://groups.google.com/g/youronlinegames/c/QVwJauQW46g
казино бесплатные фриспины за регистрацию
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/6Op8JBB0ma8
игровые аппараты онлайн бесплатно
игровые аппараты онлайн бесплатно
бесплатные игровые автоматы бесплатно
https://groups.google.com/g/topgamesonline/c/c3ifurZxmt4
бесплатные игры казино игровые автоматы
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/GbtRagtKay4
бонус казино без депозита
https://groups.google.com/g/youronlinegames/c/D5LOlTInro0
бездепозитные фриспины в казино
бездепозитные фриспины в казино
игровые автоматы бесплатно и регистрации
https://groups.google.com/g/onlinegamestop/c/7z6Q2A3Un50
играть в игральные автоматы геймеры
играть в игральные автоматы геймеры
автоматы играть бесплатно и без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/AfO8cN-K1rY
бк с минимальным депозитом 10 рублей
бк с минимальным депозитом 10 рублей
бонусы казино за регистрацию
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/DuimjA_frv4
бесплатные азартные игровые автоматы
бесплатные азартные игровые автоматы
играть в казино бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/EiFdU4_k_gk
игровые автоматы скачать бесплатно без регистрации и смс
https://groups.google.com/g/topgamesonline/c/97mA7QHNc_Y
бездепозитный казино
https://groups.google.com/g/youronlinegames/c/zrecaMxaTl8
игровые автоматы фриспины за регистрацию
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/5_ZuoLzf4wY
игры игровые автоматы бесплатно
игры игровые автоматы бесплатно
слоты игровые автоматы играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/MkuEy0qFg2U
бесплатно игровые автоматы играть
бесплатно игровые автоматы играть
essay about hotel industry https://daltonnwemu.blogdun.com/23888602/the-smart-trick-of-buy-essays-online-d-s-d-that-no-one-is-discussing intro of an essay
бездепозитный бонус за регистрацию по номеру телефона 2022
бездепозитный бонус за регистрацию по номеру телефона 2022
бездеп за регистрацию в казино
https://groups.google.com/g/novyekazinoonlajn/c/-ixCxNqVgkE
бесплатно играть в игровые автоматы
бесплатно играть в игровые автоматы
игровые автоматы сейчас бесплатно
игровые автоматы сейчас бесплатно
слоты играть бесплатно без регистрации онлайн
слоты играть бесплатно без регистрации онлайн
игры казино онлайн бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/wMPnpqgUZRM
бездепозитный бонус за регистрацию казино
https://groups.google.com/g/youronlinegames/c/ivxM6hNEdhc
бесплатные фриспины без депозита
бесплатные фриспины без депозита
онлайн казино играть бесплатно без регистрации
онлайн казино играть бесплатно без регистрации
игровые автоматы играть бесплатно слоты
https://groups.google.com/g/topgamesonline/c/csS81eBKEu4
азартные игры играть бесплатно
азартные игры играть бесплатно
Hey! Do you know if they make any plugins to assist with Search Engine Optimization? I’m trying to get my blog to rank for some targeted keywords but
I’m not seeing very good success. If you know of any please share.
Thank you!
Feel free to surf to my blog: glenelg nye boat scam
30 фриспинов за регистрацию без депозита
30 фриспинов за регистрацию без депозита
игровые автоматы слоты бесплатно
https://groups.google.com/g/onlinegamestop/c/RvLqRDoM_jo
игровые автоматы бесплатные
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/rtKEPpypM84
играть бесплатно игровые автоматы без регистрации
https://groups.google.com/g/topgamesonline/c/AkzQg7jA26Q
бездепозитный бонус казино за регистрацию
бездепозитный бонус казино за регистрацию
казино с фриспинами за регистрацию
https://groups.google.com/g/novyekazinoonlajn/c/N1O0wJUnw5c
играть бесплатно игровые автоматы
https://groups.google.com/g/onlinegamestop/c/AO2L-TvQWVw
игровые аппараты бесплатно
игровые аппараты бесплатно
игры онлайн бесплатно без регистрации игровые автоматы
игры онлайн бесплатно без регистрации игровые автоматы
бездепозитный бонус 1000 грн с выводом
бездепозитный бонус 1000 грн с выводом
фриспины за регистрацию без депозита
фриспины за регистрацию без депозита
играть в игральные автоматы
играть в игральные автоматы
игры слоты бесплатно
игры слоты бесплатно
игровые слоты играть бесплатно и без регистрации в онлайн
https://groups.google.com/g/topgamesonline/c/MoJU6CilgVM
бездепозитные казино
бездепозитные казино
бесплатные спины без депозита
https://groups.google.com/g/novyekazinoonlajn/c/kkN35cofCzs
игровые автоматы играть бесплатно онлайн без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/Emz5wska4Ys
игры азартные автоматы без регистрации
https://groups.google.com/g/onlinegamestop/c/MpWa8kmP6bM
казино автоматы бесплатно без регистрации
казино автоматы бесплатно без регистрации
играть игровые автоматы бесплатно и без регистрации
играть игровые автоматы бесплатно и без регистрации
бездепозитное казино
бездепозитное казино
бездепозитные фриспины
https://groups.google.com/g/novyekazinoonlajn/c/Pcczf5VWsNk
играть в автоматы без регистрации
https://groups.google.com/g/onlinegamestop/c/cYosbLWuMN0
аппараты играть бесплатно
аппараты играть бесплатно
казино онлайн играть бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/4aA7rrNksfo
bezdepozitni bonus casino
bezdepozitni bonus casino
казино фриспины за регистрацию
казино фриспины за регистрацию
игровые автоматы казино бесплатно
https://groups.google.com/g/onlinegamestop/c/hmQUOfDcnh0
игровые автоматы онлайн бесплатно без регистрации
игровые автоматы онлайн бесплатно без регистрации
бесплатные игровые аппараты играть
https://groups.google.com/g/topgamesonline/c/qebH0N4wy6w
без депозита бонус казино
https://groups.google.com/g/playonlinegamestop/c/iKoXruxsF8I
онлайн казино без депозита
онлайн казино без депозита
игровые слоты бесплатно
игровые слоты бесплатно
игровые слоты играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/jb_FrNxbBAc
поиграть в игровые автоматы бесплатно и без регистрации и смс
https://groups.google.com/g/topgamesonline/c/DBXSTYhZPkA
бездеп казино за регистрацию
https://groups.google.com/g/youronlinegames/c/JoHtXQs0-C8
бесплатные фриспины
бесплатные фриспины
играть в игровые автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/NWdgwfDods4
играть бесплатно азартные игры
https://groups.google.com/g/onlinegamestop/c/m8hhoP7LUXY
играть в азартные игровые автоматы бесплатно без регистрации
играть в азартные игровые автоматы бесплатно без регистрации
слоты без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/UaPCcfQHjio
бездеп казино
https://groups.google.com/g/youronlinegames/c/V3d3dYuibuw
казино с бесплатными фриспинами
https://groups.google.com/g/novyekazinoonlajn/c/A6OezH_iNmk
казино игра бесплатно
казино игра бесплатно
скачать игровой автомат бесплатно
скачать игровой автомат бесплатно
игры казино играть бесплатно и без регистрации
игры казино играть бесплатно и без регистрации
бездеп бонус за регистрацию
https://groups.google.com/g/youronlinegames/c/45QQHNhK8p4
бонус на первый депозит
бонус на первый депозит
автоматы игровые играть бесплатно
автоматы игровые играть бесплатно
бесплатные игровые автоматы играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/HB-oDv4F7yo
бесплатные автоматы игровые
бесплатные автоматы игровые
бездеп бонус казино
https://groups.google.com/g/youronlinegames/c/y3q3iqlz5Ms
бездепозит казино
https://groups.google.com/g/novyekazinoonlajn/c/eqhK9SOJwUo
игровые автоматы онлайн играть бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/h-s_Ve1a5hQ
играть в игровые автоматы бесплатно и без регистрации
играть в игровые автоматы бесплатно и без регистрации
фонбет бонус 3000 за регистрацию
фонбет бонус 3000 за регистрацию
бесплатные слоты
бесплатные слоты
бонус за первый депозит
https://groups.google.com/g/novyekazinoonlajn/c/lE8-4isp_6s
игровой автомат играть бесплатно
игровой автомат играть бесплатно
игровые автоматы онлайн бесплатно играть
игровые автоматы онлайн бесплатно играть
20 фриспинов за регистрацию
https://groups.google.com/g/youronlinegames/c/UDsigUGNJRI
игры автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/-AnKmZ8prJk
бесплатные игры в казино
бесплатные игры в казино
бонусы на первый депозит
бонусы на первый депозит
бесплатные игровые автоматы играть
бесплатные игровые автоматы играть
Hey there! I’m at work surfing around your blog from my new iphone 4!
Just wanted to say I love reading through your blog and look
forward to all your posts! Carry on the superb work!
казино играть бесплатно без регистрации
казино играть бесплатно без регистрации
фриспины за регистрацию с выводом
фриспины за регистрацию с выводом
бесплатные игры автоматы
бесплатные игры автоматы
казино бонус при регистрации
казино бонус при регистрации
играть в игровые автоматы без регистрации
https://groups.google.com/g/onlinegamestop/c/jhz8WKzp30k
слоты бесплатные
слоты бесплатные
фриспины за регистрацию без депозита с выводом
фриспины за регистрацию без депозита с выводом
бесплатные игровые аппараты
бесплатные игровые аппараты
бонус в казино
https://groups.google.com/g/novyekazinoonlajn/c/QSRqalLvGqo
играть игровые автоматы бесплатно
играть игровые автоматы бесплатно
азартные игры игровые автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/kYkMumsxSzU
казино с фриспинами за регистрацию без депозита
https://groups.google.com/g/youronlinegames/c/ApbfkmaTVO0
автоматы играть бесплатно
автоматы играть бесплатно
бонусы онлайн казино
https://groups.google.com/g/novyekazinoonlajn/c/lnYHSmNr6pg
казино игровые автоматы бесплатно и без регистрации
https://groups.google.com/g/onlinegamestop/c/nCAssAWD4Rc
игровые автоматы бесплатные игры
игровые автоматы бесплатные игры
бездепозитные фриспины за регистрацию
бездепозитные фриспины за регистрацию
бонусы в казино
https://groups.google.com/g/novyekazinoonlajn/c/HsVhAAxALGo
бесплатные игровые автоматы без регистрации
бесплатные игровые автоматы без регистрации
онлайн казино Onion
https://tripcafe.ru
игровые аппораты
https://groups.google.com/g/onlinegamestop/c/1OUGct3NQe0
бесплатные вращения за регистрацию
https://groups.google.com/g/youronlinegames/c/Cgubz0SH7u0
слот автоматы играть бесплатно
слот автоматы играть бесплатно
бонусы казино на первый депозит
https://groups.google.com/g/novyekazinoonlajn/c/9EAsscRSEX8
автоматы бесплатно
https://groups.google.com/g/onlinegamestop/c/HkRT2k4fzis
онлайн казино без вложений с выводом денег
https://groups.google.com/g/webgamesonline/c/RA1I1WWqncg
бесплатные игровые слоты
бесплатные игровые слоты
бесплатные вращения
бесплатные вращения
казино с приветственным бонусом
https://groups.google.com/g/novyekazinoonlajn/c/lQb7dsNQNmo
бесплатные игровые автоматы играть
бесплатные игровые автоматы играть
слоты игровые бесплатно без регистрации
слоты игровые бесплатно без регистрации
казино вебмани
казино вебмани
бонус без отыгрыша
https://groups.google.com/g/youronlinegames/c/m2ZKJs-AXMw
приветственный бонус казино
приветственный бонус казино
игровые автоматы играть бесплатно без регистрации и смс прямо сейчас
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/_ThCsly_odk
казино без вложений
https://groups.google.com/g/webgamesonline/c/uH08boCx7nc
приветственный бонус в казино
приветственный бонус в казино
казино с приветственным бонусом без депозита
https://groups.google.com/g/novyekazinoonlajn/c/EvO9fPk59Nk
игровые аппараты играть бесплатно без регистрации
игровые аппараты играть бесплатно без регистрации
игровые автоматы онлайн бесплатно демо версия
https://groups.google.com/g/webgamesonline/c/swipi_T2A8c
бонус на депозит казино
бонус на депозит казино
играть бесплатно без регистрации в игровые автоматы
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/z36ZBaHioFY
слоты играть демо
https://groups.google.com/g/slot365online/c/CIA2mc7dvI4
игровые автоматы демо онлайн бесплатно
https://groups.google.com/g/webgamesonline/c/WqSBZ88xQ90
автоматы игровые бесплатно
автоматы игровые бесплатно
промокод казино
https://groups.google.com/g/novyekazinoonlajn/c/hZmSgiwkw0w
скачать слоты
https://groups.google.com/g/slot365online/c/YBfO9Q-n82k
игровые автоматы бесплатно демо
https://groups.google.com/g/webgamesonline/c/_njg7hoPvq4
игровые аппараты бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/5_WqFZgrrJY
бонус без депозита казино
бонус без депозита казино
турбо казино скачать на андроид
турбо казино скачать на андроид
симуляторы игровых автоматов
симуляторы игровых автоматов
играть в старые игровые автоматы бесплатно
играть в старые игровые автоматы бесплатно
слоты играть бесплатно и без регистрации
слоты играть бесплатно и без регистрации
рейтинг казино с хорошей отдачей
https://groups.google.com/g/novyekazinoonlajn/c/8T-FowmL9Rg
рейтинг онлайн казино европы
рейтинг онлайн казино европы
рулетка онлайн казино
https://groups.google.com/g/gamesforyouluck/c/Qjg7wbaB9-g
играть в игровые автоматы бесплатно демо
играть в игровые автоматы бесплатно демо
играть слоты бесплатно без регистрации
https://groups.google.com/g/onlinegamestop/c/ZwX_EmHX1Z0
минимальный депозит 50 рублей
минимальный депозит 50 рублей
промокод вавада активный
промокод вавада активный
промокоды в казино
https://groups.google.com/g/gamesforyouluck/c/Dc_uROaf1No
игровые автоматы играть без регистрации бесплатно
игровые автоматы играть без регистрации бесплатно
Epidemics and Pandemics – Lessons from History levothyroxine 100 mcg price
демо автоматы
демо автоматы
онлайн казино с минимальным депозитом
https://groups.google.com/g/novyekazinoonlajn/c/-PHsXijHW_E
эмуляторы игровых автоматов
эмуляторы игровых автоматов
онлайн казино фриспины
онлайн казино фриспины
азартные игровые автоматы бесплатно без регистрации онлайн
https://groups.google.com/g/onlinegamestop/c/DvONGjB_toE
бездепозитные бонусы в казино за регистрацию
https://groups.google.com/g/webgamesonline/c/f-L_oWbbMmw
лучшие онлайн казино с минимальным депозитом
лучшие онлайн казино с минимальным депозитом
игровые автоматы демо версии играть бесплатно
игровые автоматы демо версии играть бесплатно
лучшие казино европы
https://groups.google.com/g/gamesforyouluck/c/dkt0SA2RrkM
игры слот бесплатно
игры слот бесплатно
казино Onion
официальный сайт казино Onion
игровые автоматы с минимальным депозитом
https://groups.google.com/g/novyekazinoonlajn/c/3qX-iF0cbsg
демо слоты играть бесплатно
https://groups.google.com/g/slot365online/c/M4RjH3qDwE0
слот играть бесплатно
слот играть бесплатно
казино онлайн рулетка
https://groups.google.com/g/gamesforyouluck/c/01j05Eb-TKY
казино игровые автоматы играть бесплатно
казино игровые автоматы играть бесплатно
слоты с минимальным депозитом
https://groups.google.com/g/novyekazinoonlajn/c/qpiY1cHVonM
демо слоты играть
демо слоты играть
казино однорукий бандит
https://groups.google.com/g/gamesforyouluck/c/Figw3LPtGVc
новые игровые автоматы бесплатно без регистрации
новые игровые автоматы бесплатно без регистрации
старые игровые автоматы онлайн бесплатно
https://groups.google.com/g/gamesforyouluck/c/McuE3BN49kI
казино с маленьким депозитом
казино с маленьким депозитом
демо игры казино
демо игры казино
казино бесплатные спины
https://groups.google.com/g/gamesforyouluck/c/EUXyN7r8OuU
автоматы играть онлайн бесплатно
https://groups.google.com/g/onlinegamestop/c/0WHbfV7aOCY
старые игровые автоматы
https://groups.google.com/g/gamesforyouluck/c/NJYw2X-Swco
простые игры с выводом денег
простые игры с выводом денег
бесплатные автоматы
бесплатные автоматы
игровой автомат бесплатно
игровой автомат бесплатно
игровые автоматы новинки
игровые автоматы новинки
слоты демо бесплатно без регистрации
слоты демо бесплатно без регистрации
игра на деньги с выводом на карту
игра на деньги с выводом на карту
играть бесплатно автоматы
https://groups.google.com/g/onlinegamestop/c/dTLH1kI-dsM
азартные игры бесплатно
https://groups.google.com/g/onlinegamestop/c/1uhQfuAyi5A
скачать симулятор игровых автоматов
скачать симулятор игровых автоматов
игровые автоматы слоты без регистрации
https://groups.google.com/g/onlinegamestop/c/nOv7vyz2LFo
как оплатить бум на айфоне
https://groups.google.com/g/novyekazinoonlajn/c/gKrWAWtp0Sc
игровые автоматы бесплатно с бонусами
https://groups.google.com/g/gamesforyouluck/c/MtgphyrV7eI
казино с минимальным пополнением
казино с минимальным пополнением
автоматы онлайн бесплатно
https://groups.google.com/g/onlinegamestop/c/hDhcljzuu4Q
скачать сборник игровых автоматов бесплатно
скачать сборник игровых автоматов бесплатно
казино с мгновенными выплатами
https://groups.google.com/g/novyekazinoonlajn/c/GYyKPNuoYcc
слоты игровые автоматы играть бесплатно и без регистрации демо
слоты игровые автоматы играть бесплатно и без регистрации демо
zoom казино
zoom казино
бесплатные казино игры без регистрации
бесплатные казино игры без регистрации
скачать эмуляторы игровых автоматов
https://groups.google.com/g/gamesforyouluck/c/MO4UkGO3jmI
Excellent web site you have got here.. It’s difficult to find good quality writing like yours nowadays.
I truly appreciate individuals like you! Take care!!
казино с быстрыми выплатами
казино с быстрыми выплатами
эмуляторы игровых автоматов бесплатно
https://groups.google.com/g/webgamesonline/c/zGgEAEcXjeY
волна казино отзывы
https://groups.google.com/g/spinandwinmoney/c/TmOvPQdNpoQ
бесплатные азартные игры
https://groups.google.com/g/onlinegamestop/c/cGKUKBjHwv8
рулетка казино онлайн
рулетка казино онлайн
мобильные игры с выводом денег
мобильные игры с выводом денег
игровые автоматы играть бесплатно демо
https://groups.google.com/g/webgamesonline/c/U7UOVGXYy10
играть в слоты бесплатно и без регистрации
https://groups.google.com/g/onlinegamestop/c/08GaULjD47E
установить игровые автоматы бесплатно
установить игровые автоматы бесплатно
WOW just what I was looking for. Came here by searching for Massagen in Nürnberg
My web site; Massage Berichten
онлайн казино в казахстане
https://groups.google.com/g/gamesforyouluck/c/1AvatCq_B54
играть в автоматы бесплатно без регистрации
играть в автоматы бесплатно без регистрации
casino android
https://groups.google.com/g/novyekazinoonlajn/c/iGS96hpw0AU
вебмани казино
вебмани казино
слоты с покупкой бонуса
слоты с покупкой бонуса
Can you tell us more about this? I’d care to find out more details.
игровые автоматы играть бесплатно сейчас
https://groups.google.com/g/onlinegamestop/c/7XboCqqtZ-o
лучшие телефонные игры с выводом денег
лучшие телефонные игры с выводом денег
играть бесплатно игровые автоматы демо
играть бесплатно игровые автоматы демо
слоты на телефон
https://groups.google.com/g/spinandwinmoney/c/npnr8JfkHIw
играть бесплатно слоты
играть бесплатно слоты
симулятор игровых автоматов бесплатно
симулятор игровых автоматов бесплатно
игровые автоматы на деньги с телефона
https://groups.google.com/g/novyekazinoonlajn/c/R19JmQl_64U
игральные автоматы играть бесплатно
игральные автоматы играть бесплатно
скачать игровые автоматы на телефон
https://groups.google.com/g/spinandwinmoney/c/tvsjK1bvOME
игровые автоматы бесплатно однорукий бандит
https://groups.google.com/g/webgamesonline/c/2yqbSLZ4p7M
казино на телефоне
https://groups.google.com/g/novyekazinoonlajn/c/4gQP9TQtjg8
бесплатные игры казино
бесплатные игры казино
скачать игровые автоматы на андроид без интернета
скачать игровые автоматы на андроид без интернета
бесплатные эмуляторы игровых автоматов
бесплатные эмуляторы игровых автоматов
казино на телефон
казино на телефон
играть бесплатно и без регистрации в игровые автоматы
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/MMyNfgq8eFw
скачать бесплатно игровые автоматы на телефон
https://groups.google.com/g/spinandwinmoney/c/UEKsq7dlQgo
демо игровые автоматы без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/-NHn698R2as
эмуляторы игровых автоматов играть бесплатно
https://groups.google.com/g/webgamesonline/c/Hlz-ZUKwk2U
европейские казино с бездепозитным бонусом
https://groups.google.com/g/evropejskiekazinosbezdepozitnymbonusom/c/rqBWeU5Rxw8
скачат игровой автомат
скачат игровой автомат
игры игровые аппараты
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/7gvETB0V_J4
симулятор игровых автоматов играть
симулятор игровых автоматов играть
лучшие лицензионные казино
https://groups.google.com/g/luchshielicenzionnyekazino/c/ndZm6-kvlzo
играть в автоматы бесплатно
играть в автоматы бесплатно
скачать бесплатно игровые автоматы без интернета
https://groups.google.com/g/spinandwinmoney/c/jQ31U7UHmTI
казино webmoney
казино webmoney
лучшие лицензионные онлайн казино
https://groups.google.com/g/luchshielicenzionnyeonlajnkazino/c/6bNr_bOa4nE
бесплатные игры казино игровые автоматы
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/GbtRagtKay4
рулетка казино играть
рулетка казино играть
казино рулетка онлайн на деньги
https://groups.google.com/g/webgamesonline/c/vLWNVQV7whU
автоматы играть бесплатно и без регистрации
автоматы играть бесплатно и без регистрации
новые казино с бездепозитным бонусом
новые казино с бездепозитным бонусом
рокс казино отзывы
https://groups.google.com/g/spinandwinmoney/c/4aA_vlsy5Jg
эмулятор игровых автоматов онлайн бесплатно
https://groups.google.com/g/webgamesonline/c/nS1OUwViTAw
играть в казино бесплатно без регистрации
играть в казино бесплатно без регистрации
денежный бонус за регистрацию в казино
https://groups.google.com/g/webgamesonline/c/K3Q_x-NUcso
промокод gama казино
промокод gama казино
онлайн казино украина на гривны с бонусами
https://groups.google.com/g/gamesforyouluck/c/-EB8A5gpSMg
слоты игровые автоматы играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/MkuEy0qFg2U
новые казино онлайн
https://groups.google.com/g/novyekazinoonlajn/c/_dmHbbp8R6g
играть слоты демо
играть слоты демо
бесплатно играть в игровые автоматы
бесплатно играть в игровые автоматы
онлайн казино с живыми дилерами
https://groups.google.com/g/gamesforyouluck/c/y_9qB0yEcyU
промокод чемпион казино
промокод чемпион казино
xbunedirloooo.X6EojW7oQ5aj
новое онлайн казино
https://groups.google.com/g/novoeonlajnkazino/c/LYj5toNGI7Q
игры казино онлайн бесплатно без регистрации
игры казино онлайн бесплатно без регистрации
демо игры автоматы бесплатно
демо игры автоматы бесплатно
онлайн казино рулетка
https://groups.google.com/g/gamesforyouluck/c/jjxbhsbyL_4
поиграть бесплатно в игровые автоматы
https://groups.google.com/g/spinandwinmoney/c/kxpmS7m88Q4
бонусы. вавада. казино.
бонусы. вавада. казино.
азартные игры играть бесплатно
азартные игры играть бесплатно
симуляторы игровых автоматов играть бесплатно
https://groups.google.com/g/webgamesonline/c/UNG218SIazc
онлайн казино на реальные деньги без вложений
https://groups.google.com/g/gamesforyouluck/c/VG4fedKHHLE
онлайн казино физзслотс игровые автоматы
онлайн казино физзслотс игровые автоматы
игровые автоматы бесплатные
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/rtKEPpypM84
зума казино
https://groups.google.com/g/yourgamesonline/c/qEnerY_rJso
симуляторы игровых аппаратов
https://groups.google.com/g/webgamesonline/c/pnc6K36AVRs
новые бесплатные игровые автоматы
https://groups.google.com/g/gamesforyouluck/c/fsLjmuhBjag
игровые аппараты бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/DZayTkw8W4g
однорукий бандит автомат
https://groups.google.com/g/spinandwinmoney/c/MW-xSVc0jZQ
vivaro казино онлайн
https://groups.google.com/g/yourgamesonline/c/iLyVbwqNhWU
играть автоматы демо
https://groups.google.com/g/webgamesonline/c/qNKZHIs6jQs
игры слоты бесплатно
игры слоты бесплатно
postemergency xyandanxvurulmus.uOlELPVGA620
live казино
live казино
лучшие слоты с бонусами
лучшие слоты с бонусами
vbet автоматы онлайн
vbet автоматы онлайн
бесплатные симуляторы игровых автоматов
бесплатные симуляторы игровых автоматов
игровые автоматы играть бесплатно онлайн без регистрации
игровые автоматы играть бесплатно онлайн без регистрации
лайв казино с живым дилером
лайв казино с живым дилером
лучшие игровые слоты
https://groups.google.com/g/spinandwinmoney/c/bdKZr3z3iZg
vbet автоматы играть
https://groups.google.com/g/yourgamesonline/c/PNiWd94Nuq8
играть игровые автоматы бесплатно и без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/ZTJJ4TbKUGM
игровые автоматы играть бесплатно без регистрации демо
https://groups.google.com/g/webgamesonline/c/rxQzSVcdYG0
лайв казино
лайв казино
казино z
казино z
казино онлайн играть бесплатно без регистрации
казино онлайн играть бесплатно без регистрации
топ лицензионных казино
топ лицензионных казино
казино демо игра
казино демо игра
казино с живыми дилерами
https://groups.google.com/g/gamesforyouluck/c/iG09QmpN3ss
игровые автоматы онлайн бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/2-KjSTCzBy4
казино волна отзывы
казино волна отзывы
топ казино с моментальным выводом
https://groups.google.com/g/topgamersonline/c/LRqIPDOg95A
онлайн казино демо
https://groups.google.com/g/webgamesonline/c/IHG-Lx3eWLM
игровые слоты играть бесплатно
игровые слоты играть бесплатно
казино с выводом на киви
https://groups.google.com/g/gamesforyouluck/c/bLqb1TEs_yw
казино с фриспинами без депозита
казино с фриспинами без депозита
супер слотс отзывы
https://groups.google.com/g/winbigmoney/c/VAc5-xeN6iU
старые игровые автоматы играть бесплатно
https://groups.google.com/g/webgamesonline/c/OgrdGTJ1oRs
играть в игровые автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/NWdgwfDods4
казино свит бонанза
казино свит бонанза
супер слотс на деньги
супер слотс на деньги
казино ра регистрация
казино ра регистрация
симулятор игровых автоматов
https://groups.google.com/g/webgamesonline/c/0qQ4k5Z7p5g
слоты без регистрации
слоты без регистрации
казино с пополнением с киви от 100 рублей
казино с пополнением с киви от 100 рублей
супер слотс играть бесплатно
супер слотс играть бесплатно
автоматы демо
https://groups.google.com/g/webgamesonline/c/VGnkhTZNgE4
казино победа
казино победа
скачать игровой автомат бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/4XgOJcF5AE8
казино с пополнением с киви
казино с пополнением с киви
stake казино отзывы
stake казино отзывы
скачать игровые автоматы на компьютер
https://groups.google.com/g/webgamesonline/c/8jddD9blqhA
бесплатные игровые автоматы играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/HB-oDv4F7yo
казино онлайн бонус за депозит
казино онлайн бонус за депозит
казино с киви
https://groups.google.com/g/gamesforyouluck/c/Y_3BjMOuf80
олимпус казино
https://groups.google.com/g/webgamesonline/c/qxj2d5WvzRg
спинбеттер казино
спинбеттер казино
играть в игровые автоматы бесплатно и без регистрации
играть в игровые автоматы бесплатно и без регистрации
казино лицензионное
https://groups.google.com/g/spinandwinmoney/c/ZNArdNeih60
hepatectomised xyandanxvurulmus.120963smcjKT
игровой автомат играть бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/GZfZf2cKp0I
казино пополнение с киви
https://groups.google.com/g/gamesforyouluck/c/kqly10jae-8
Hi there to every body, it’s my first pay a quick visit of this website; this weblog
carries awesome and genuinely fine stuff in favor of visitors.
казино ра бездепозитный бонус 250 рублей
https://groups.google.com/g/webgamesonline/c/Ko23YAyju70
физзслотс казино
физзслотс казино
казино лайв
https://groups.google.com/g/spinandwinmoney/c/w-151EkClyI
игры автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/-AnKmZ8prJk
казино олимпус
казино олимпус
sweet bonanza казино
https://groups.google.com/g/slot365online/c/aTDSI6RLjvY
спинбеттер казино
https://groups.google.com/g/yourgamesonline/c/Ldi77Rnfpw0
казино фриспины
https://groups.google.com/g/spinandwinmoney/c/eYLnHeXZe1I
казино играть бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/jUV5wBE0F18
казино с хорошей отдачей
казино с хорошей отдачей
казино фриспины без депозита
казино фриспины без депозита
спинбетер казино
https://groups.google.com/g/winbigmoney/c/3LtYYVxfVrE
казино физзслотс контакты
https://groups.google.com/g/spinandwinmoney/c/SV6x0pRzkdg
слоты бесплатные
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/3xmxH620HlI
эмуляторы игровых аппаратов
эмуляторы игровых аппаратов
казино бонус без депозит
казино бонус без депозит
слоты с фриспинами
https://groups.google.com/g/yourgamesonline/c/Yrm3BD5W4VI
азартные игры игровые автоматы бесплатно
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/kYkMumsxSzU
казино fizzslots играть бесплатно и без регистрации
казино fizzslots играть бесплатно и без регистрации
казино бонанза
казино бонанза
слоты с большой отдачей 2022
https://groups.google.com/g/yourgamesonline/c/_5pXyzWThus
казино без вложений но с выводом денег
https://groups.google.com/g/gamesforyouluck/c/T3jvzUEIjgU
игровые автоматы бесплатные игры
игровые автоматы бесплатные игры
казино бездепозитный бонус за регистрацию
https://groups.google.com/g/spinandwinmoney/c/oAepwSDYLRM
играть в автоматы демо
играть в автоматы демо
слоты играть бесплатно без регистрации
слоты играть бесплатно без регистрации
казино бесплатные фриспины
казино бесплатные фриспины
бесплатные игровые автоматы без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/sR8fhTnNGHw
Grrat article, justt wat I waas ooking for.
игровые автоматы старые
https://groups.google.com/g/spinandwinmoney/c/851q4FG1F8A
игровые автоматы онлайн демо
https://groups.google.com/g/slot365online/c/LGAAhn5gUlA
слот автоматы играть бесплатно
слот автоматы играть бесплатно
слоты бесплатно играть
слоты бесплатно играть
казино 100 бесплатных вращений
https://groups.google.com/g/gamesforyouluck/c/7bMl9boYGYM
игровые автоматы скачать на андроид бесплатно
игровые автоматы скачать на андроид бесплатно
классические игровые автоматы
https://groups.google.com/g/slot365online/c/405l4JJCtf4
бесплатные игровые слоты
бесплатные игровые слоты
слотозал отзывы
https://groups.google.com/g/yourgamesonline/c/a9o0ZHOlWRg
игровые слоты демо
игровые слоты демо
игровые автоматы с депозитом за регистрацию
https://groups.google.com/g/spinandwinmoney/c/xyx6E2bxMTU
слоты игровые бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/-G5eNhVMKhQ
слоты с минимальной ставкой
https://groups.google.com/g/slot365online/c/AnG3AMQaDl4
слот автоматы онлайн бесплатно
https://groups.google.com/g/topgamersonline/c/xI3tXDQ1D8c
игровые автоматы старые бесплатно
игровые автоматы старые бесплатно
игровые автоматы играть бесплатно без регистрации и смс прямо сейчас
игровые автоматы играть бесплатно без регистрации и смс прямо сейчас
игровые автоматы рулетка
https://groups.google.com/g/spinandwinmoney/c/OQk0PQqsXLQ
играть в игровые автоматы демо
играть в игровые автоматы демо
скачать казино физзслотс
https://groups.google.com/g/winbigmoney/c/TrPRC0NqBEs
игровые автоматы слоты демо бесплатно
https://groups.google.com/g/gamesforyouluck/c/VXHsH17aT3U
игровые аппараты играть бесплатно без регистрации
https://groups.google.com/g/igrovyeavtomatyfrispinyzaregistraciju/c/f04xYk9a4Pc
игровые автоматы смс
игровые автоматы смс
игровые автоматы однорукий бандит
игровые автоматы однорукий бандит
самое честное казино
самое честное казино
игровые автоматы с быстрым выводом денег
https://groups.google.com/g/webgamesonline/c/WtD1ZgH7PfQ
играть бесплатно без регистрации в игровые автоматы
играть бесплатно без регистрации в игровые автоматы
казино с выводом денег без вложений
https://groups.google.com/g/slot365online/c/a2c1N1lZFE8
игровые автоматы бесплатно скачать
игровые автоматы бесплатно скачать
рейтинг мобильных казино
рейтинг мобильных казино
автоматы игровые бесплатно
автоматы игровые бесплатно
игровые автоматы рулетка онлайн
игровые автоматы рулетка онлайн
бесплатные игровые автоматы демо
https://groups.google.com/g/slot365online/c/t1hjtW4Yhm0
играть казино бесплатно
https://groups.google.com/g/spinandwinmoney/c/IfjgVkBKagc
поиграть в игровые автоматы бесплатно
https://groups.google.com/g/topgamersonline/c/sPidAL7kkYA
игровые автоматы на компьютер
https://groups.google.com/g/webgamesonline/c/H9R70wgKZGg
эмуляторы игровых автоматов играть бесплатно без регистрации
эмуляторы игровых автоматов играть бесплатно без регистрации
победа казино
победа казино
фриспины за регистрацию в казино
https://groups.google.com/g/spinandwinmoney/c/M6K_2_cbZ1s
игровые автоматы играть смс
https://groups.google.com/g/gamesforyouluck/c/lox8lX5DRRY
демо версия казино
https://groups.google.com/g/slot365online/c/3xhCEP8L2lo
отзывы о казино
https://groups.google.com/g/yourgamesonline/c/tSD5oe_bX9c
фриспины в онлайн казино за регистрацию
фриспины в онлайн казино за регистрацию
игровые автоматы демо без регистрации
игровые автоматы демо без регистрации
игровые автоматы демо версии
https://groups.google.com/g/slot365online/c/Uo0psVF8CxE
онлайн казино с быстрым выводом денег
https://groups.google.com/g/topgamersonline/c/TKf2QetN9BM
фрибеты казино
https://groups.google.com/g/spinandwinmoney/c/LZbHxvgIpSc
https://ciprofloxacin.life/# ciprofloxacin order online
игровые автоматы бездепозитный бонус за регистрацию
https://groups.google.com/g/gamesforyouluck/c/ta8ZkWa5rwU
демо игры слоты
https://groups.google.com/g/slot365online/c/dPtMV_XX7HA
онлайн казино победа
онлайн казино победа
fizzslots казино онлайн скачать
https://groups.google.com/g/spinandwinmoney/c/Xb0oxD_CQXw
https://amoxil.icu/# amoxicillin 500mg buy online uk
игровые автоматы бесплатно и без регистрации демо
https://groups.google.com/g/webgamesonline/c/_myYotDBqYg
играть демо слоты
https://groups.google.com/g/slot365online/c/a2lNnQCJlTc
онлайн автоматы бесплатно
онлайн автоматы бесплатно
fizzslots казино онлайн официальный сайт бесплатно
https://groups.google.com/g/spinandwinmoney/c/ntO8cygWjbw
cost cheap clomid pills where to get cheap clomid without a prescription – can i get generic clomid online
казино с демо счетом
https://groups.google.com/g/slot365online/c/O26qEkagjhw
игровые аппараты демо
https://groups.google.com/g/webgamesonline/c/zVM-n6_3cg4
новые слоты
https://groups.google.com/g/yourgamesonline/c/oBeUHw2wSes
buy clomid without rx: how to get generic clomid pill – cost clomid tablets
физзслотс казино онлайн бесплатно
https://groups.google.com/g/spinandwinmoney/c/JzQfGN0Ad1A
классические слоты
https://groups.google.com/g/slot365online/c/YF6kmmcvRNs
buy prednisone online fast shipping: prednisolone prednisone – prescription prednisone cost
игровой автомат sweet bonanza
https://groups.google.com/g/gamesforyouluck/c/ny1ByQM0YfQ
миллион игровые автоматы
миллион игровые автоматы
что такое вейджер в казино
https://groups.google.com/g/spinandwinmoney/c/pqBDAFiNMaQ
казино с минимальным депозитом и выводом
https://groups.google.com/g/slot365online/c/PEw5OW8Bsg4
играть игровые автоматы бесплатно демо
играть игровые автоматы бесплатно демо
лучшие казино с моментальным выводом денег
лучшие казино с моментальным выводом денег
http://amoxil.icu/# amoxicillin 775 mg
бонусы казино 2023
https://groups.google.com/g/spinandwinmoney/c/6V1RAddqy3c
фриспины казино
фриспины казино
легзо казино отзывы
https://groups.google.com/g/yourgamesonline/c/pCRg7x7Sc08
бонус код казино х
бонус код казино х
джекпот игровые автоматы
джекпот игровые автоматы
казино zoom
https://groups.google.com/g/yourgamesonline/c/05Z3NWDfxRY
dog house казино
https://groups.google.com/g/gamesforyouluck/c/FW9536jTRy8
казино зет
https://groups.google.com/g/yourgamesonline/c/sst99OONvSs
zoma казино
https://groups.google.com/g/luckspinwin/c/4ymlCXBBBms
betera казино
betera казино
букмекерские конторы с казино
букмекерские конторы с казино
казино селектор бездепозитный бонус
казино селектор бездепозитный бонус
zuma казино
zuma казино
арго казино
https://groups.google.com/g/spinandwinmoney/c/PfY0tlkJyLE
казино с бонусом без депозита
https://groups.google.com/g/topgamersonline/c/3k3pOqynoF8
букмекерские конторы с игровыми автоматами
https://groups.google.com/g/gamesforyouluck/c/PJQc_oQV2z0
zuma live казино
zuma live казино
vave казино
https://groups.google.com/g/luckspinwin/c/7xP21eceiAo
vavada казино бонус за регистрацию
vavada казино бонус за регистрацию
казино с бездепозитным бонусом при регистрации
https://groups.google.com/g/yourgamesonline/c/RfH8zLkLsVI
букмекерские конторы с игровыми автоматами
https://groups.google.com/g/gamesforyouluck/c/PJQc_oQV2z0
вавада казино отзывы реальные
вавада казино отзывы реальные
вавада. казино. бонус.
https://groups.google.com/g/winbigmoney/c/mWMNQO_LRXc
казино с бесплатными фриспинами за регистрацию
казино с бесплатными фриспинами за регистрацию
бонусы казино за пополнение
бонусы казино за пополнение
vavada. казино. отзывы.
https://groups.google.com/g/luckspinwin/c/w16-CQkImm0
турбо казино онлайн
турбо казино онлайн
криптобосс казино
https://groups.google.com/g/chooseyourgame/c/B6S_8A-y0Ac
казино с бесплатным депозитом
https://groups.google.com/g/topgamersonline/c/7TUlXbBI4zM
азартные игровые автоматы демо слоты бесплатно и без регистрации
азартные игровые автоматы демо слоты бесплатно и без регистрации
stake казино играть
https://groups.google.com/g/winbigmoney/c/4HwJw3DO1Js
vavada казино отзывы
https://groups.google.com/g/slotsforall/c/FLeGHvzvMTs
кэт казино промокод
кэт казино промокод
слотмен
слотмен
Fantastic beat ! I would like to apprentice while you amend your web site,
how could i subscribe for a blog web site?
The account aided me a acceptable deal. I had been a little
bit acquainted of this your broadcast provided
bright clear concept
казино rox отзывы
казино rox отзывы
вывод денег физзслотс
https://groups.google.com/g/strawberryslots/c/WQ11bjG6-aM
вавада казино отзывы
https://groups.google.com/g/luckspinwin/c/Q35FJuxqXJw
казино золото лото
казино золото лото
промокод джой казино
https://groups.google.com/g/winbigmoney/c/2vGZtrUaMbA
казино ра вход
https://groups.google.com/g/yourgamesonline/c/JjchOeH0C1w
восток игровые автоматы
восток игровые автоматы
вавада. казино. официальный. отзывы.
https://groups.google.com/g/slotsforall/c/dS7T0Eomnl8
казино супер слот
казино супер слот
поинт казино
https://groups.google.com/g/luckspinwin/c/xJEQbj8XH5c
казино ра рабочее зеркало
https://groups.google.com/g/yourgamesonline/c/p-X8dibLznY
вавада казино бонус
вавада казино бонус
в каких городах россии есть казино
https://groups.google.com/g/strawberryslots/c/TPuZzKdYmeI
отзывы онлайн казино
https://groups.google.com/g/winbigmoney/c/rzFaqDXzZNM
казино селектор онлайн
https://groups.google.com/g/chooseyourgame/c/oKNe9KiV0uw
казино ра промокод
казино ра промокод
турбо казино вход
https://groups.google.com/g/luckspinwin/c/lEB5WPsE6VY
турбо казино официальный сайт
https://groups.google.com/g/slotsforall/c/NOFZqUKVPUE
онлайн казино fizzslots
онлайн казино fizzslots
казино с бездепозитным бонусом за регистрацию 2015
казино с бездепозитным бонусом за регистрацию 2015
казино ра бездепозитный бонус
казино ра бездепозитный бонус
онлайн казино физзслотс
онлайн казино физзслотс
турбо казино отзывы
турбо казино отзывы
топ казино с бездепозитным бонусом за регистрацию
топ казино с бездепозитным бонусом за регистрацию
totogaming казино
https://groups.google.com/g/chooseyourgame/c/IOL0ifWbcPI
онлайн казино бонус без депозита
онлайн казино бонус без депозита
казино ra
https://groups.google.com/g/yourgamesonline/c/RP3khydsLko
супер слотс онлайн
https://groups.google.com/g/slotsforall/c/xX6wq6-Iiic
супер слотс регистрация
https://groups.google.com/g/slotsforall/c/joFM6hxEXQ8
онлайн-казино fizzslots
https://groups.google.com/g/luckspinwin/c/LWyagrRJnxs
супер слотс скачать
https://groups.google.com/g/chooseyourgame/c/gkE7YRrjsTE
казино победа официальный сайт
казино победа официальный сайт
супер слотс играть
супер слотс играть
супер слотс мобильная версия
https://groups.google.com/g/strawberryslots/c/Rgn8HunZb_M
обзор казино рокс
https://groups.google.com/g/luckspinwin/c/yphz6enANRo
Heya outstanding blog! Does running a blog similar to this require a large amount of work?
I have no understanding of computer programming but I had been hoping to start
my own blog soon. Anyways, if you have any ideas
or tips for new blog owners please share. I know this is off topic but
I simply had to ask. Appreciate it!
супер слотс бонус
супер слотс бонус
казино онлайн с минимальным депозитом
https://groups.google.com/g/topgamersonline/c/gb5J4KXih5M
спин вин казино
https://groups.google.com/g/luckspinwin/c/3K62oT0arfs
страда казино
страда казино
новый онлайн казино fizz slots
https://groups.google.com/g/winbigmoney/c/8SSxJDvIzwI
скачать физзслотс
https://groups.google.com/g/strawberryslots/c/DESh28GQU4M
казино онлайн отзывы
https://groups.google.com/g/spinandwinmoney/c/fFDY4bfcXck
слоты по 1 копейке 1xbet название
https://groups.google.com/g/luckspinwin/c/HSwefCchyo4
strada казино
strada казино
мобильная версия физзслотс
мобильная версия физзслотс
казино онлайн бездепозитный бонус за регистрацию
казино онлайн бездепозитный бонус за регистрацию
селектор казино онлайн
https://groups.google.com/g/chooseyourgame/c/8XKCZmFbY1c
слоты по 1 копейке 1xbet
https://groups.google.com/g/luckspinwin/c/b8AY8povFhw
лучшие слоты
лучшие слоты
казино онлайн бесплатно и без регистрации
казино онлайн бесплатно и без регистрации
рокс казино россия
рокс казино россия
слоты по 10 копеек 1xbet список
https://groups.google.com/g/luckspinwin/c/fL6vutXgR34
кракен казино
кракен казино
Hiya! I know this is kinda off topic however I’d figured I’d ask.
Would you be interested in exchanging links or maybe guest authoring a blog
post or vice-versa? My site discusses a lot of the same subjects
as yours and I think we could greatly benefit from each other.
If you happen to be interested feel free to shoot me an email.
I look forward to hearing from you! Great blog by
the way!
слоты с минимальной ставкой в 1xbet
https://groups.google.com/g/slotsforall/c/Uwv-nl22mbk
казино мелбет
казино мелбет
казино зум
https://groups.google.com/g/winbigmoney/c/5HpAv7kb6d4
получить бездепозитный бонус в казино
https://groups.google.com/g/luckspinwin/c/68JG3gavaZg
рабочий промокод fizzslots казино
рабочий промокод fizzslots казино
slottica казино скачать
https://groups.google.com/g/strawberryslots/c/MXqPU7WJBSQ
казино восток играть
казино восток играть
казино лев играть бесплатно без регистрации
казино лев играть бесплатно без регистрации
покердом казино отзывы
https://groups.google.com/g/slotsforall/c/6Hg1Sz7iRJ4
промокод fizzslots казино на сегодня
промокод fizzslots казино на сегодня
казино vivaro
казино vivaro
селектор казино регистрация
https://groups.google.com/g/strawberryslots/c/stxY4GMpTuU
казино фрибет
казино фрибет
париматч игровые автоматы
париматч игровые автоматы
пари матч регистрация казино
https://groups.google.com/g/chooseyourgame/c/c3itro8Z2Fo
казино вавада отзывы
казино вавада отзывы
селектор казино 63 gg
селектор казино 63 gg
казино fizzslots
https://groups.google.com/g/yourgamesonline/c/m_m-bCd4EL4
Very soon this website will be famous amid all blog viewers, due to it’s
fastidious articles or reviews
отзывы казино
https://groups.google.com/g/slotsforall/c/PJRXaJE6m8A
пари матч онлайн казино
https://groups.google.com/g/chooseyourgame/c/Et9Zb6Kn7es
казино. вавада. отзывы.
https://groups.google.com/g/winbigmoney/c/Mt04CRCkCN0
самые дающие слоты 2023
https://groups.google.com/g/strawberryslots/c/BCz6UEGFMnI
казино дающие бездепозитные бонусы
https://groups.google.com/g/yourgamesonline/c/9WvHkkIbFdc
онлайн казино колумбус
https://groups.google.com/g/luckspinwin/c/8o8wJFTKToo
казино турбо
https://groups.google.com/g/winbigmoney/c/VphbRb_78ZI
пари матч казино мобильная версия
https://groups.google.com/g/chooseyourgame/c/O4RNrc4xeYs
регистрация казино бонус
регистрация казино бонус
казино бонусы без депозита
казино бонусы без депозита
лотереи в физзслотс казино
лотереи в физзслотс казино
казино спинбеттер
казино спинбеттер
онлайн казино поинт
онлайн казино поинт
промокод казино ра
промокод казино ра
казино бонус регистрация
казино бонус регистрация
казино ра зеркало
https://groups.google.com/g/luckspinwin/c/DN3KPWY8SsM
lezgo казино
lezgo казино
онлайн казино grand casino
https://groups.google.com/g/strawberryslots/c/ICr7X4dek8c
казино ра мобильная версия
https://groups.google.com/g/winbigmoney/c/rzFaqDXzZNM
казино бездеп
казино бездеп
промокод fizzslots казино
промокод fizzslots казино
колумбус казино
колумбус казино
казино онлайн отзывы игроков
казино онлайн отзывы игроков
лучшие бездепозитные бонусы казино
лучшие бездепозитные бонусы казино
казино 888
https://groups.google.com/g/yourgamesonline/c/R9xzHcSKt3M
получить бонус казино
https://groups.google.com/g/strawberryslots/c/LrAk-sjyILw
казино зума
https://groups.google.com/g/luckspinwin/c/ujC8KIZ-WiM
казино онлайн fizzslots
https://groups.google.com/g/luckspinwin/c/VTcTaDWsiFs
лезго казино
лезго казино
I’m extremely pleased to discover this website.
I wanted to thank you for ones time for this fantastic read!!
I definitely enjoyed every little bit of it and I have you saved
as a favorite to check out new information on your
website.
какие казино реально выплачивают выигрыши в россии отзывы
какие казино реально выплачивают выигрыши в россии отзывы
отзывы физзслотс
отзывы физзслотс
казино вулкан старс играть бесплатно
казино вулкан старс играть бесплатно
казино миллион официальный сайт
казино миллион официальный сайт
легальные казино в россии
https://groups.google.com/g/chooseyourgame/c/f15iBiuhJzs
jvspin казино
jvspin казино
онлайн казино супер слотс
https://groups.google.com/g/strawberryslots/c/hs7ubnXqNwI
казино в россии в каких городах
https://groups.google.com/g/slotsforall/c/_GRqWb7yL2I
казино лев отзывы
https://groups.google.com/g/winbigmoney/c/xpIIAKUW7is
интернет игровые автоматы бесплатно
https://groups.google.com/g/topgamersonline/c/8duMnYGdIX8
крипто казино с бездепозитным бонусом
крипто казино с бездепозитным бонусом
онлайн казино приватбанк
https://groups.google.com/g/strawberryslots/c/wy_Xm2J0xvE
казино в россии где разрешено
https://groups.google.com/g/luckspinwin/c/dlNy-mv3org
казино колумбус
казино колумбус
игры онлайн слоты бесплатно без регистрации
https://groups.google.com/g/topgamersonline/c/qKayyLMAQWg
казино кинг
казино кинг
онлайн казино лев
онлайн казино лев
казино турбо зеркало
казино турбо зеркало
казино рокс на деньги
казино рокс на деньги
казино где дают бездепозитный бонус
https://groups.google.com/g/luckspinwin/c/Z8NbbOdXuMs
игры казино автоматы бесплатно без регистрации
игры казино автоматы бесплатно без регистрации
онлайн казино адмирал игровые автоматы
https://groups.google.com/g/strawberryslots/c/KXv049vNzHo
казино totogaming casino
https://groups.google.com/g/luckspinwin/c/DnTE7FsiiHU
казино победа бонусы
https://groups.google.com/g/chooseyourgame/c/LKiZkXfwiso
Medications for Mental Clarity and Cognitive Enhancement cialis over the counter
Hello there, I found your site via Google at the same time as looking for
a similar subject, your web site got here up, it seems great.
I have bookmarked it in my google bookmarks.
Hello there, just become aware of your blog via Google, and located that it is really informative.
I’m going to be careful for brussels. I will appreciate when you proceed this in future.
Lots of folks will be benefited from your writing. Cheers!
казино физзслотс регистрация с мобильной версии
казино физзслотс регистрация с мобильной версии
игровые слоты онлайн без регистрации
игровые слоты онлайн без регистрации
официальные казино в россии
https://groups.google.com/g/strawberryslots/c/Qqdgk1CLxaA
казино супер слотс играть бесплатно
https://groups.google.com/g/luckspinwin/c/4ybEDBz2CEg
казино париматч
https://groups.google.com/g/chooseyourgame/c/PsT4FYJA_jI
казино физзслотс
казино физзслотс
игровые слоты играть бесплатно и без регистрации
игровые слоты играть бесплатно и без регистрации
обзор рокс казино
обзор рокс казино
казино с бонусом при регистрации
https://groups.google.com/g/luckspinwin/c/FoUaXx8Lr2c
казино миллион бездепозитный бонус
казино миллион бездепозитный бонус
казино fizz slots
казино fizz slots
игровые автоматы играть сейчас бесплатно без регистрации и смс
игровые автоматы играть сейчас бесплатно без регистрации и смс
можно ли выиграть в онлайн казино отзывы
можно ли выиграть в онлайн казино отзывы
казино с бонусом на депозит
https://groups.google.com/g/slotsforall/c/47OiRtWH8v8
казино баунти
https://groups.google.com/g/luckspinwin/c/DikKpa1mrsM
казино лев онлайн
казино лев онлайн
казино отзывы
казино отзывы
игровые автоматы играть бесплатно без регистрации прямо сейчас
игровые автоматы играть бесплатно без регистрации прямо сейчас
лучшие казино с бездепозитным бонусом
https://groups.google.com/g/strawberryslots/c/QyVQsWflIEc
Any new production that opened between 17 February 2016 and 21 February 2017 in a
theatre represented in membership of the Society of London Theatre was eligible for
consideration, supplied it had performed not less than 30 performances.
изумительно казино
https://groups.google.com/g/winbigmoney/c/NML1XG1b-Ok
казино лев – играть бесплатно
казино лев – играть бесплатно
игровые слоты казино fizzslots
игровые слоты казино fizzslots
игровые автоматы fizzslots казино бесплатно и без регистрации
игровые автоматы fizzslots казино бесплатно и без регистрации
кэшбэк fizzslots казино
кэшбэк fizzslots казино
казино joker
https://groups.google.com/g/strawberryslots/c/nZPPiQ1eCug
игровые автоматы с выводом денег отзывы
https://groups.google.com/g/winbigmoney/c/eN5jdms5hbs
казино jvspin
казино jvspin
игровые автоматы fizzslots казино
игровые автоматы fizzslots казино
кэшбэк физзслотс казино
кэшбэк физзслотс казино
казино х промокод
https://groups.google.com/g/chooseyourgame/c/ZgKJludw4Bk
играть в физзслотс казино
играть в физзслотс казино
казино х отзывы
казино х отзывы
игровые автоматы без регистрации бесплатно
игровые автоматы без регистрации бесплатно
казино spinbetter
https://groups.google.com/g/strawberryslots/c/fOrjWEcfN3E
играть на деньги в казино физзслотс
https://groups.google.com/g/winbigmoney/c/p-DylVIogtU
казино fizzslots кэшбэк каждую неделю
казино fizzslots кэшбэк каждую неделю
казино голдфишка
https://groups.google.com/g/luckspinwin/c/7euSNOZ6_I8
игровые автоматы без денег
https://groups.google.com/g/playeveryday/c/mQfwyq0PPiY
казино слоттика фриспины
https://groups.google.com/g/slotsforall/c/7bgHoqSRg54
Hello i am kavin, its my first time to commenting anyplace,
when i read this article i thought i could also make comment due to this sensible
post.
голдфишка казино
голдфишка казино
казино fairspin
https://groups.google.com/g/chooseyourgame/c/Py7RWyURaqw
казино fizzslots кэшбэк при регистрации
https://groups.google.com/g/slotsforall/c/KioxW60dgI4
игровые автоматы бесплатные онлайн
https://groups.google.com/g/topgamersonline/c/NLT2dw9HMAE
казино приват24
казино приват24
где разрешено казино в россии
где разрешено казино в россии
казино адмирал демо
казино адмирал демо
казино clubnika
https://groups.google.com/g/slotsforall/c/ndrvkIdYEdQ
игровые автоматы бесплатно без регистрации играть
игровые автоматы бесплатно без регистрации играть
казино покердом отзывы
https://groups.google.com/g/slotsforall/c/U_xRoGrQpvc
физзслотс скачать игру
физзслотс скачать игру
казино чемпион отзывы
https://groups.google.com/g/luckspinwin/c/RQmpVKjZTh4
казино 1xbet отзывы
https://groups.google.com/g/strawberryslots/c/bntY2XkUPMQ
игровые автоматы бесплатно без регистрации демо
игровые автоматы бесплатно без регистрации демо
казино лев играть на деньги
https://groups.google.com/g/strawberryslots/c/yIlfPZUZapM
fizzslots казино онлайн скачать на телефон
https://groups.google.com/g/winbigmoney/c/wj1L9SPcpho
казино буй бездепозитный бонус
https://groups.google.com/g/slotsforall/c/lvNfdVghzGI
игровые аппараты слоты
https://groups.google.com/g/playeveryday/c/kyiumgCYCnA
казино эверум
казино эверум
jvspin казино регистрация
https://groups.google.com/g/chooseyourgame/c/uX3Y_45A9fs
fizzslots казино онлайн
https://groups.google.com/g/winbigmoney/c/_eK8FioHo5s
Wow! This blog looks just like my old one!
It’s on a completely different topic but it has pretty much the
same page layout and design. Wonderful choice of colors!
fizzslots казино игровые автоматы
fizzslots казино игровые автоматы
казино 777 оригинал
https://groups.google.com/g/luckspinwin/c/xia6P4NraIg
игровые аппараты без регистрации без смс
игровые аппараты без регистрации без смс
казино голд
https://groups.google.com/g/strawberryslots/c/VCBOE_178Aw
император казино
император казино
fizzslots казино играть
fizzslots казино играть
играть в слоты бесплатно
https://groups.google.com/g/topgamersonline/c/EV4PhiLLanY
казино джокер
казино джокер
игровые автоматы фараон играть бесплатно
https://groups.google.com/g/chooseyourgame/c/XP1wNRjXIVg
clubnika казино
https://groups.google.com/g/luckspinwin/c/whE8DGnosD8
играть в игровые автоматы онлайн бесплатно без регистрации
играть в игровые автоматы онлайн бесплатно без регистрации
казино cosmolot
казино cosmolot
букмекеры с казино
https://groups.google.com/g/winbigmoney/c/cXk5Bjhr6iY
играть в игровые автоматы fizzslots
играть в игровые автоматы fizzslots
казино буй рабочее зеркало
https://groups.google.com/g/strawberryslots/c/1ICvLGrawWU
игровые автоматы фараон играть бесплатно
https://groups.google.com/g/chooseyourgame/c/XP1wNRjXIVg
бонусы в онлайн казино
бонусы в онлайн казино
играть в автоматы онлайн бесплатно
играть в автоматы онлайн бесплатно
казино bounty
казино bounty
Hello i am kavin, its my first occasion to commenting anyplace, when i read
this paragraph i thought i could also create comment due to
this brilliant article.
jvspin казино вход
jvspin казино вход
Америка – страна, где сбываются мечты, но оказывается,
что их цена высока Россия великая страна
бонусы бездепозитные казино
https://groups.google.com/g/luckspinwin/c/gO7omylwiFk
казино лев онлайн
https://groups.google.com/g/chooseyourgame/c/Zlg5BftM7mc
играть в автоматы бесплатно и без регистрации
играть в автоматы бесплатно и без регистрации
казино booi бездепозитный бонус
https://groups.google.com/g/slotsforall/c/4heso44npCc
бк с казино
бк с казино
izzi казино отзывы
https://groups.google.com/g/luckspinwin/c/D3qwkkYUs0I
We stumbled over here coming from a different page and thought I might as well
check things out. I like what I see so now i’m following you.
Look forward to looking at your web page repeatedly.
играть в автоматы
играть в автоматы
играть в автоматы в казино адмирал
играть в автоматы в казино адмирал
бездепозитные онлайн казино
бездепозитные онлайн казино
казино 7 промокод
https://groups.google.com/g/slotsforall/c/M3KD4Oo6cMw
I’ll right away clutch your rss feed as I can’t to find
your email subscription link or newsletter
service. Do you have any? Please permit me understand so that I may subscribe.
Thanks.
игровые автоматы физзслотс с бездепозитным бонусом
игровые автоматы физзслотс с бездепозитным бонусом
играть онлайн казино бесплатно без регистрации
https://groups.google.com/g/topgamersonline/c/JFAkh02gE6s
бездепозитные игровые автоматы
https://groups.google.com/g/winbigmoney/c/FQDdxkbfXDc
где в россии разрешено казино
https://groups.google.com/g/chooseyourgame/c/DZGR_OD9G30
казино 1x slots отзывы
https://groups.google.com/g/slotsforall/c/__Dwg6hJ1MA
of course like your web-site however you have to take a look at the spelling on several
of your posts. Several of them are rife with spelling issues and I in finding it very
bothersome to inform the reality nevertheless I will surely come back again.
игровые автоматы бесплатно адмирал
игровые автоматы бесплатно адмирал
бетера казино
https://groups.google.com/g/winbigmoney/c/bAPOYhH3OnE
играть онлайн бесплатно в игровые автоматы
играть онлайн бесплатно в игровые автоматы
как получить кэшбэк в вавада казино
https://groups.google.com/g/strawberryslots/c/ljuvGsWlMJo
где в россии казино
https://groups.google.com/g/strawberryslots/c/qD2hCuo1oxo
играть онлайн казино эльдорадо
играть онлайн казино эльдорадо
играть бесплатно в автоматы
https://groups.google.com/g/topgamersonline/c/wpwhHz-ckhg
betboom казино
https://groups.google.com/g/luckspinwin/c/I5LpGlN3Ynk
какие казино дают бездепозитный бонус
какие казино дают бездепозитный бонус
где можно играть в казино в россии
https://groups.google.com/g/chooseyourgame/c/Biy8yoEgUtA
goxbet казино
https://groups.google.com/g/luckspinwin/c/BwkZyHRj_AM
бесплатное казино
бесплатное казино
гудвин казино
https://groups.google.com/g/yourgamesonline/c/kpc-s4XsRTo
физзслотс казино онлайн на реальные деньги
физзслотс казино онлайн на реальные деньги
где казино в россии
https://groups.google.com/g/chooseyourgame/c/rN5_4QGc-Ik
зарубежные онлайн казино
зарубежные онлайн казино
фриспины без отыгрыша за регистрацию с выводом 2023
https://groups.google.com/g/topgamersonline/c/2aJKmkY-TqY
игровые автоматы миллион
https://groups.google.com/g/strawberryslots/c/85XqJMA93cQ
депозитный бонус казино
депозитный бонус казино
фреш казино отзывы
https://groups.google.com/g/chooseyourgame/c/-XycQHPVsP4
зарубежные казино с бездепозитным бонусом
https://groups.google.com/g/slot365online/c/wwOs64rQyNE
фрибет без депозита казино
фрибет без депозита казино
играть казино лев
https://groups.google.com/g/strawberryslots/c/SzBISkrBV2w
делюкс казино
https://groups.google.com/g/slotsforall/c/Xb20m1n-5KM
френдс казино
https://groups.google.com/g/chooseyourgame/c/G12MvKUiV98
This post is priceless. When can I find out more?
зарубежные казино
зарубежные казино
франк казино
https://groups.google.com/g/winbigmoney/c/jcy6MneUaYY
где разрешены казино в россии
https://groups.google.com/g/strawberryslots/c/oByDmCE_vjE
bounty казино
https://groups.google.com/g/luckspinwin/c/CZJ62eTvL8Y
все биткоины из реальные слоты bitcoin обзор
https://groups.google.com/g/slot365online/c/_OgAx-RjIhE
физзслотс казино бонусы
https://groups.google.com/g/chooseyourgame/c/HZPznPHX7PE
физзслотс официальный сайт
https://groups.google.com/g/winbigmoney/c/I5Z49S_uFME
где есть казино в россии
https://groups.google.com/g/strawberryslots/c/DMHPydAC298
booi казино отзывы
https://groups.google.com/g/slotsforall/c/uzQNv1ma7XU
в каком онлайн казино реально выиграть отзывы
https://groups.google.com/g/playeveryday/c/kD2I4MF0gy0
фаирспин казино
фаирспин казино
физзслотс казино
физзслотс казино
физзслотс казино вывод
физзслотс казино вывод
блэкджек онлайн казино
https://groups.google.com/g/slotsforall/c/sK_A-qNc8Wo
виртуальные игровые автоматы
виртуальные игровые автоматы
фаер спин казино
фаер спин казино
физзслотс
https://groups.google.com/g/yourgamesonline/c/QvrY8Boc2GQ
fizzslots казино онлайн отзывы
fizzslots казино онлайн отзывы
топ казино без верификации
топ казино без верификации
бездепозитный бонус при регистрации в казино
https://groups.google.com/g/luckspinwin/c/2UfblrvdOyo
джокер казино скачать
джокер казино скачать
джойказино промокод
джойказино промокод
топ бонусы казино
https://groups.google.com/g/playeveryday/c/wiCZtVhwamY
физзслотс казино бонус
https://groups.google.com/g/strawberryslots/c/E75_GAg04O8
казино с бонусом за регистрацию без депозита
http://seafishzone.com/home.php?mod=space&uid=1199242
1win poker
https://www.x-fta.com/foro/member.php?1226107-Erikalet
слоты игровые автоматы
https://groups.google.com/g/slot365online/c/mMIFTd6zEjQ
джет казин
джет казин
бонус за регистрацию в казино без депозита
бонус за регистрацию в казино без депозита
бонус за регистрацию в казино без депозита
http://forum.d-dub.com/member.php?1384982-Arlenebed
физз слотс казино бонус
физз слотс казино бонус
казино аврора
https://www.itchyforum.com/en/member.php?284057-DarleneGaimb
скачать казино
скачать казино
онлайн казино без депозита
https://visualchemy.gallery/forum/profile.php?id=3511985
бонусы за регистрацию в казино
бонусы за регистрацию в казино
чемпион игровые автоматы играть
https://groups.google.com/g/chooseyourgame/c/z17J9RGJWkE
booi казино бездепозитный бонус
booi казино бездепозитный бонус
казино онлайн играть на деньги рубли список
https://forum.inos.at/profile.php?id=583377
скачать игровые аппараты
скачать игровые аппараты
игровые автоматы онлайн на реальные деньги
http://bocauvietnam.com/member.php?1417477-Selenaher
бонусы. вавада. казино.
бонусы. вавада. казино.
бездепозитные бонусы за регистрацию
http://www.themcwars.org/forum/index.php?action=profile;u=56648
бонусы физзслотс
бонусы физзслотс
бонус казино на депозит
бонус казино на депозит
Interest charged from the borrowers also seems a reasonable one for the borrowers opting for this solution. Very often lenders claim better interest rates, when in fact; the other
fees they charge may be higher than that of their competitor.
The application procedure is lightning quick and can be completed in just a few minutes from a home or office computer.
бездепозитное казино
http://bbs.cheaa.com/home.php?mod=space&uid=3036475
рублевые казино
https://groups.google.com/g/slot365online/c/8d1_uc5-F9M
бездепозитный бонус казино за регистрацию
http://bocauvietnam.com/member.php?1417495-BlancheBep
We stumbled over here different page and thought I may
as well check things out. I like what I see so now i am following you.
Look forward to looking over your web page for a second time.
бонус казино за регистрацию
https://groups.google.com/g/topgamersonline/c/KPGgJdsIO3s
bons казино
https://groups.google.com/g/strawberryslots/c/r489xZojwQg
бездепозитный бонус казино 2023
https://groups.google.com/g/chooseyourgame/c/q8Q9p3czetg
casino gama
http://jbgirlss.pw/member.php?action=profile&uid=932
рекомендуемые казино
https://groups.google.com/g/playeveryday/c/cHU65tQ8GtM
бонуси казино
https://groups.google.com/g/topgamersonline/c/yItnH6izEdo
Hi there to every one, the contents present at this
site are in fact awesome for people knowledge, well,
keep up the nice work fellows.
beep beep казино официальный сайт
https://groups.google.com/g/strawberryslots/c/MDwsdFPB0b0
реально ли выиграть в онлайн казино
https://groups.google.com/g/slot365online/c/PW6fYXEpPXE
автоматы супер слотс
автоматы супер слотс
бездепы в казино
https://groups.google.com/g/topgamersonline/c/qhamdqZ9ctU
проверенные казино онлайн отзывы
https://groups.google.com/g/playeveryday/c/x0kWmccZ7II
ararat gold казино зеркало
https://groups.google.com/g/strawberryslots/c/fb7Fx0ZWpy4
адмирал казино онлайн
https://groups.google.com/g/chooseyourgame/c/DkzGtvDDP6g
бездепозитный бонус казино с выводом
https://groups.google.com/g/playeveryday/c/0W2SCiyij28
аджарабет казино
https://groups.google.com/g/strawberryslots/c/yq_KZP0jh6A
888 казино бездепозитный бонус
888 казино бездепозитный бонус
бесплатный бонус казино
бесплатный бонус казино
онлайн казино с приветственным бонусом
https://groups.google.com/g/slot365online/c/ouhqkKzFPec
888 казино регистрация
888 казино регистрация
бездепозитный бонус автоматы
https://groups.google.com/g/slotsforall/c/WdxCy22c7sU
1win игровые автоматы
1win игровые автоматы
vriligy with dapoxetine 60mg Future of Healthcare Relies on Advanced Medications
онлайн казино без верификации
https://groups.google.com/g/slot365online/c/VJiYwzL27RE
бесплатные спины за регистрацию
https://groups.google.com/g/topgamersonline/c/PRHuacRfQME
бездепозитные бонусы онлайн казино
https://groups.google.com/g/slotsforall/c/uJDttCW0qmA
вулкан рояль бонус за регистрацию в казино
вулкан рояль бонус за регистрацию в казино
онлайн казина с бонус без депозит
https://groups.google.com/g/playeveryday/c/mDT92s64xws
бесплатные игры в казино fizzslots
бесплатные игры в казино fizzslots
vavada. казино. бонус. за. регистрацию.
https://groups.google.com/g/supergamesonline/c/DYL7r8bkALU
бесплатные бонусы казино
бесплатные бонусы казино
vbet автомати онлайн
https://groups.google.com/g/canyouplayonline/c/DmeQOYJ0EpA
мобильные онлайн казино
https://groups.google.com/g/playeveryday/c/k0vKX9jKX7Q
бесплатные игры казино без регистрации
https://groups.google.com/g/topgamersonline/c/fyNrhn8WieM
запрещено ли казино в россии
https://groups.google.com/g/supergamesonline/c/ekR650f5q3w
законно ли казино в россии
https://groups.google.com/g/welcometocasino/c/odgiqM2QLpo
лучшие онлайн казино отзывы
https://groups.google.com/g/playeveryday/c/Pa2lna6xKM0
up x казино
up x казино
бесплатные игры игровые автоматы
https://groups.google.com/g/topgamersonline/c/MBAXHQG8rCE
video
winbet казино
winbet казино
лучшие крипто казино
лучшие крипто казино
триумф казино
триумф казино
starda казино
https://groups.google.com/g/canyouplayonline/c/3Qe0Ph6TCxE
бесплатные игры для автоматов
бесплатные игры для автоматов
Thank you for the good writeup. It if truth be told was
once a enjoyment account it. Glance complex
to more brought agreeable from you! However, how could we keep in touch?
My web site; เว็บบทความ
лучшие казино рунета
https://groups.google.com/g/playeveryday/c/V6Xnih2EdIA
вулкан ставка казино онлайн
вулкан ставка казино онлайн
топ казино 2023
https://groups.google.com/g/welcometocasino/c/iJo0TiRXGMA
slotor казино
https://groups.google.com/g/canyouplayonline/c/_9tNA_ZUOzM
бесплатные игровые автоматы без регистрации и смс
бесплатные игровые автоматы без регистрации и смс
лучшие игры казино
https://groups.google.com/g/playeveryday/c/xGcIGhUtauo
vavada. казино. бонус.
vavada. казино. бонус.
sykaaa казино
https://groups.google.com/g/welcometocasino/c/d8Zx82iEpyc
схемы выигрыша в казино бесплатно
https://groups.google.com/g/canyouplayonline/c/3GvHD1tRLGs
лучшие бонусы казино за регистрацию
https://groups.google.com/g/playeveryday/c/1UGn5E7WtPs
бесплатные игра автомат
https://groups.google.com/g/topgamersonline/c/FO-474dP5Qo
супер слоты играть
https://groups.google.com/g/welcometocasino/c/VrHc1BOrBfw
спин сити казино бездепозитный бонус
https://groups.google.com/g/supergamesonline/c/BuJHR-IRUl8
selektor казино
https://groups.google.com/g/canyouplayonline/c/spMyTvNG5OQ
лучшие бонусы казино
лучшие бонусы казино
бесплатные бонусы от казино
https://groups.google.com/g/topgamersonline/c/8UFlmJPR8Rs
слоты с большой отдачей
https://groups.google.com/g/welcometocasino/c/rXHTrxnsjvQ
spin city казино
https://groups.google.com/g/supergamesonline/c/AYVq6OrkMt0
лучшее мобильное казино
лучшее мобильное казино
риобет казино официальный сайт
риобет казино официальный сайт
азартные игры слот автоматы играть сейчас бесплатно без регистрации
https://groups.google.com/g/topgamersonline/c/eo2OZiZ8q8A
слотозал казино
https://groups.google.com/g/welcometocasino/c/7UCUSJw35As
лучшее казино онлайн отзывы
https://groups.google.com/g/playeveryday/c/Pa2lna6xKM0
слот sweet bonanza
https://groups.google.com/g/supergamesonline/c/JOxG7cvMl4U
реально заработать в интернет казино
https://groups.google.com/g/canyouplayonline/c/haYy-lfeKYs
азартные игры игровые автоматы
азартные игры игровые автоматы
лицензионное казино онлайн
https://groups.google.com/g/playeveryday/c/l_v8MgTOKr0
симулятор казино
симулятор казино
разрешены ли казино в россии
https://groups.google.com/g/canyouplayonline/c/QJ6iUvHzp8I
рейтинг казино с живыми дилерами
https://groups.google.com/g/supergamesonline/c/amuStQ_pCTo
азартные игровые автоматы без регистрации
https://groups.google.com/g/topgamersonline/c/kEFWR3vJM3M
криптовалютные казино
криптовалютные казино
рокс казино рабочее зеркало на сегодня
рокс казино рабочее зеркало на сегодня
промокоды казино пин ап
https://groups.google.com/g/canyouplayonline/c/S8VY7aEPTdA
работа в казино
https://groups.google.com/g/supergamesonline/c/XoAMgOoH9yM
автоматы онлайн vbet
https://groups.google.com/g/yourgamesonline/c/oZPlGDhyJqQ
криптоказино
криптоказино
промокод рокс казино
https://groups.google.com/g/welcometocasino/c/O1L_9lOhRdA
промокод лев казино
https://groups.google.com/g/canyouplayonline/c/6_mD7S7VStk
казино с выводом без верификации
https://groups.google.com/g/slot365online/c/TrppXiWt29o
промокоды пин ап казино 2022
https://groups.google.com/g/supergamesonline/c/mNz6rWU-Ofo
автоматы игровые
https://groups.google.com/g/topgamersonline/c/I-C3CKNQimg
Great post but I was wanting to know if you could write a litte more on this topic?
I’d be very grateful if you could elaborate a
little bit more. Cheers!
промокод казино лев
https://groups.google.com/g/welcometocasino/c/7AWeNqwE39Y
казино с быстрым выводом и без верификации
https://groups.google.com/g/slot365online/c/pTb_4rQOaPg
промокод кэт казино
https://groups.google.com/g/canyouplayonline/c/guzu5zx77eg
автоматы играть vbet
https://groups.google.com/g/winbigmoney/c/WM6L7fVlPgg
панда казино
панда казино
казино с бонусами
https://groups.google.com/g/playeveryday/c/RlV1U8SiELM
промокод fizzslots казино 2022
промокод fizzslots казино 2022
автоматы играть бесплатно без регистрации
https://groups.google.com/g/topgamersonline/c/2DiR12f4F9o
онлайн казино адмирал
онлайн казино адмирал
казино с бездепозитными бонусами
https://groups.google.com/g/playeveryday/c/sAdGVSS_XJs
онлайн казино 1xslots
https://groups.google.com/g/welcometocasino/c/pMBw4rh-Xok
промокод джойказино
https://groups.google.com/g/canyouplayonline/c/s9ILXB3XKCw
автомати онлайн vbet
автомати онлайн vbet
казино онлайн без верификации
казино онлайн без верификации
онлайн казино admiral
https://groups.google.com/g/supergamesonline/c/X65B_RXyBoM
официальные казино россии
официальные казино россии
пм казино
https://groups.google.com/g/canyouplayonline/c/kykaNEhglks
казино игры онлайн
https://groups.google.com/g/playeveryday/c/4GQcGldNiZk
лавина казино
лавина казино
золотой арбуз казино зеркало
https://groups.google.com/g/joinplayonline/c/7-d1eYzrEjA
lzzl казино
https://groups.google.com/g/welcometocasino/c/uF26YdoLlHQ
пачинко автомат
https://groups.google.com/g/canyouplayonline/c/8nREiKaxcTQ
казино бонус при регистрации без депозита
казино бонус при регистрации без депозита
Fantastic post however I was wondering if you could write a litte more on this subject?
I’d be very thankful if you could elaborate a little bit further.
Appreciate it!
восток казино официальный сайт
восток казино официальный сайт
леон слоты играть
леон слоты играть
кешер казино
https://groups.google.com/g/supergamesonline/c/edGq0PpFwvA
казино без паспорта
https://groups.google.com/g/slot365online/c/FORWPDELJsc
Howdy! This article couldn’t be written much better!
Reading through this post reminds me of
my previous roommate! He continually kept talking about
this. I’ll forward this post to him. Fairly certain he will have
a great read. Thank you for sharing!
онлайн казино миллион
https://groups.google.com/g/canyouplayonline/c/jr9PPAsOv7s
It’s impressive that you are getting ideas from this post as well as from
our dialogue made at this place.
WOW just what I was looking for. Came here by searching for slot gacor
Hello there! Do youu knhow if they make anny pluginss too assist with SEO?
I’m trying tto geet my blog tto ranhk for soje targeted keywordds bbut I’m nnot
seeing very good results. If youu know oof anny
please share. Many thanks!
вавада. казино. онлайн. бесплатно.
https://groups.google.com/g/joinplayonline/c/8Ap1NBRhDNc
легальное казино
легальное казино
Greetings from Ohio! I’m bored at work so I decided to browse your website on my iphone
during lunch break. I enjoy the info you provide here
and can’t wait to take a look when I get home. I’m
shocked at how fast your blog loaded on my mobile .. I’m not even using WIFI, just 3G ..
Anyhow, wonderful blog!
казино вулкан бездепозитный бонус
https://groups.google.com/g/supergamesonline/c/7xtl_vyot5E
Hey there! Do you know if they make any plugins to help with
Search Engine Optimization? I’m trying to get my blog to
rank for some targeted keywords but I’m not seeing very
good results. If you know of any please share.
Thanks!
Feel free to visit my website … sex17++
казино без депозита бонус
https://groups.google.com/g/playeveryday/c/yVaYBfMT0lQ
Amazing things here. I’m very glad to see your post. Thank you a lot and I’m taking a look forward to contact you.
Will you kindly drop me a mail?
I am really thankful to the holder of this web page who has shared this enormous post at at this place.
лучшие казино с живыми дилерами
лучшие казино с живыми дилерами
Good article. I will be facing some of these issues as well..
казино вулкан платинум 777
казино вулкан платинум 777
супер слотс бонус за регистрацию
https://groups.google.com/g/joinplayonline/c/MqD6dZ09jEU
какие казино дают выиграть
https://groups.google.com/g/playeveryday/c/19pwSf3MxP0
Heya i’m for the first time here. I found this board
and I find It really useful & it helped me out much. I hope to give something back and aid others like you helped me.
казино в рф
казино в рф
лев казино промокод
https://groups.google.com/g/canyouplayonline/c/iG6dsaynaKE
Ahaa, its good dialogue concerning this article at this place at this weblog, I have read all that, so now me also commenting here.
интернет казино отзывы
интернет казино отзывы
казино селектор
казино селектор
Ι dο not evеn know the way I stopped uρ right һere, һowever I hought tһiѕ рut սp was great.
I dο not recognise wһo you aгe һowever definitely yoᥙ’re gоing to a famous blogger іf you һappen tⲟo aге not already.
Cheers!
Αlso visit my website … xxl nutrition
roks казино
https://groups.google.com/g/joinplayonline/c/6xKMLgaK0cE
казино волна официальный сайт
казино волна официальный сайт
легально ли казино в россии
легально ли казино в россии
игры онлайн на деньги
https://groups.google.com/g/playeveryday/c/LFHa8mNYqCc
Currently it sounds like Drupal is the preferred blogging platform out there right now.
(from what I’ve read) Is that what you’re using on your blog?
Feel free to surf to my web-site :: free sex video pron
казино россии
казино россии
разрешено ли казино в россии
разрешено ли казино в россии
казино вегас
https://groups.google.com/g/supergamesonline/c/AwceYIlogt8
Hey! Do you know if they make any plugins to help with
Search Engine Optimization? I’m trying to get my blog to rank for some targeted keywords but I’m
not seeing very good gains. If you know of any please share.
Thank you!
игровые автоматы отзывы
https://groups.google.com/g/playeveryday/c/mluwOzApcUg
казино goxbet
https://groups.google.com/g/welcometocasino/c/JMfbZm71lqY
казинo вбет
казинo вбет
Saved as a favorite, I like your web site!
игровые автоматы онлайн отзывы
игровые автоматы онлайн отзывы
казино френдс
казино френдс
казино онлайн fizzslot
https://groups.google.com/g/canyouplayonline/c/59W2vKhbUbI
Hello tһis is somewhat of off topic but I was wondering if blogs ᥙse WYSIWYG editors ⲟr
іf уou have tо manually code ԝith HTML. I’m starting a blog ѕoon bսt һave no coding knowledge ѕo I
ᴡanted to get guidance from ѕomeone with experience.
Αny help ԝould be grеatly appreciated!
игровые автоматы без первого депозита с бонусом
игровые автоматы без первого депозита с бонусом
Excellent, what a website it is! This website gives
useful data to us, keep it up.
казино франк
казино франк
казино maxbet бонусы
https://groups.google.com/g/canyouplayonline/c/CnTm1li8m4E
казино super slots
https://groups.google.com/g/supergamesonline/c/o64ODJ4nz-s
промокод эльдорадо казино
промокод эльдорадо казино
играть в казино на деньги с телефона
играть в казино на деньги с телефона
I read this post completely about the difference of hottest and previous
technologies, it’s amazing article.
Exceptional post however , I was wanting to know if you could
write a litte more on this topic? I’d be very thankful if you could elaborate a little
bit more. Thank you!
Greate pieces. Keep posting such kind of info on your page.
Im really impressed by your site.
Hey there, You’ve performed a fantastic job. I will definitely digg it
and for my part suggest to my friends. I’m confident they’ll be benefited from this website.
казино dragon мани
https://groups.google.com/g/welcometocasino/c/fdYYznq5gUA
Nice post. I was checking continuously this blog and
I’m impressed! Very useful info particularly the last part :
) I care for such info a lot. I was looking for this particular information for a long time.
Thank you and best of luck.
казино эльдорадо бездепозитный бонус
https://groups.google.com/g/canyouplayonline/c/k6nODbBxq8o
казино strada
казино strada
онлайн казино париматч
https://groups.google.com/g/joinplayonline/c/JNipJb-o_p8
I’m not sure exactly why but this website is loading incredibly slow for me.
Is anyone else having this problem or is it a problem on my end?
I’ll check back later and see if the problem still exists.
игра онлайн казино
https://groups.google.com/g/playeveryday/c/WHK7Oo_yyuA
казино чемпион играть на деньги
казино чемпион играть на деньги
казино флинт
https://groups.google.com/g/canyouplayonline/c/r5b4d63-GcQ
Also viѕit my page :: This site iss offіcialⅼy erifieԁ ffor the Farsi audience (https://atkerman.ir/%d8%b1%d8%b3%d8%a7%d9%86%d9%87-%d8%ac%d9%88%d8%a7%d9%86-%d8%af%d8%a7%d9%86%d9%84%d9%88%d8%af-%d8%a2%d9%87%d9%86%da%af-%d8%ac%d8%af%db%8c%d8%af-%d8%8c-%d8%af%d8%a7%D9%86%d9%84%d9%88%d8%af-%d9%85%d9%88/)
где дают бонусы на день рождения
где дают бонусы на день рождения
онлайн казино джекпот
https://groups.google.com/g/joinplayonline/c/t94eAWbSyw8
казино онлайн 2022
казино онлайн 2022
Hi just wanted to give you a quick heads up and let you
know a few of the pictures aren’t loading properly.
I’m not sure why but I think its a linking issue. I’ve tried it in two different internet browsers and both show the same results.
Very good blog! Do you have any hints for aspiring writers?
I’m planning to start my own website soon but I’m a
little lost on everything. Would you propose starting with a free platform like WordPress or go for a paid
option? There are so many options out there that I’m completely overwhelmed ..
Any tips? Appreciate it!
What’s up, just wanted to say, I liked this post.
It was practical. Keep on posting!
казино betwinner
казино betwinner
casino 2023
casino 2023
казино фараон онлайн играть
https://groups.google.com/g/canyouplayonline/c/5MVRscgMh9Y
официальное казино в россии
официальное казино в россии
казино леон играть
https://groups.google.com/g/chooseyourgame/c/nSDHUJmQZuw
бонусы на день рождения казино
бонусы на день рождения казино
казино адмирал играть бесплатно
казино адмирал играть бесплатно
казино ф1
https://groups.google.com/g/canyouplayonline/c/Ry7bllc9sWA
Hi, I log on to your blog like every week. Your humoristic style is
awesome, keep it up!
melbet казино слоты
https://groups.google.com/g/joinplayonline/c/Hvp706EuJOY
Looking for a server to build a home on? https://rustichomestead.craftingstore.net/
Rustic Homestead (US) players enjoy low population on a large map with
a month to explore before wipe. Resource stack sizes are increased.
Active Admin. Discord integration. Web store has daily and weekly freebies.
All that is asked is please be respectful and enjoy the game.
Streamers welcome!
Hey would you mind stating which blog platform you’re using?
I’m going to start my own blog soon but I’m having a tough
time making a decision between BlogEngine/Wordpress/B2evolution and
Drupal. The reason I ask is because your layout seems different then most blogs and I’m
looking for something completely unique. P.S Sorry for getting
off-topic but I had to ask!
казино корона
https://groups.google.com/g/supergamesonline/c/NHb87L0wUjY
Hello to every one, for the reason that I am actually keen of
reading this blog’s post to be updated on a regular basis.
It contains good material.
Do you mind if I quote a couple of your posts as long
as I provide credit and sources back to your website?
My blog is in the very same niche as yours and
my visitors would certainly benefit from a lot of the information you present here.
Please let me know if this okay with you. Regards!
With havin so much content and articles do you ever run into any issues of plagorism or copyright violation?
My blog has a lot of exclusive content I’ve either created myself
or outsourced but it seems a lot of it is popping it up all over the internet without my permission. Do you know any ways to help stop content from being ripped off?
I’d truly appreciate it.
бонусы на день рождения
бонусы на день рождения
казино адмирал играть бесплатно
казино адмирал играть бесплатно
Hi Dear, are you actually visiting this site daily, if so then you will definitely obtain nice
knowledge.
казино чемпион играть
https://groups.google.com/g/canyouplayonline/c/Yn5HtyL5GuY
малина казино
малина казино
This design is incredible! You most certainly know how to keep
a reader entertained. Between your wit and your videos, I was almost moved to start my own blog
(well, almost…HaHa!) Fantastic job. I really enjoyed what you had to say, and more than that, how you presented it.
Too cool!
бонус на день рождения казино
https://groups.google.com/g/playeveryday/c/Ykjpdt5hznI
I love your blog.. very nice colors & theme. Did you design this website
yourself or did you hire someone to do it for you?
Plz respond as I’m looking to design my own blog and would like to find out where u got this from.
cheers
This is a good tip particularly to those new to the blogosphere.
Brief but very precise info… Appreciate your sharing this one.
A must read article!
казино х бонус код
https://groups.google.com/g/supergamesonline/c/ApiR4sIuBdM
как потратить бонусы казино 1win
https://groups.google.com/g/welcometocasino/c/Hr-q86ndlnc
You should be a part of a contest for one of the most useful sites on the web.
I most certainly will recommend this site!
как играть в рулетку в казино
как играть в рулетку в казино
легальные игровые автоматы
легальные игровые автоматы
Nonetheless, these are extremely costly.
бездепозитный бонус за регистрацию в онлайн казино
бездепозитный бонус за регистрацию в онлайн казино
Your style is very unique in comparison to other folks I
have read stuff from. Thank you for posting when you’ve got
the opportunity, Guess I will just bookmark this page.
как получить кэшбэк в казино vavada
как получить кэшбэк в казино vavada
казино чемпион промокод
казино чемпион промокод
Having read this I believed it was really informative.
I appreciate you spending some time and energy to put this article together.
I once again find myself spending way too much time both reading and posting comments.
But so what, it was still worth it!
porn vurgunyedim.lsBpaJJ8XDB7
jet казино онлайн
jet казино онлайн
казино восток официальный сайт
казино восток официальный сайт
бездепозитный бонус за регистрацию с выводом
бездепозитный бонус за регистрацию с выводом
jozz казино регистрация
jozz казино регистрация
бездепозитный бонус игровые автоматы
https://groups.google.com/g/playeveryday/c/bQsM45WeHrE
казино turbo
https://groups.google.com/g/joinplayonline/c/E05gce3B1o0
игры супер слот
игры супер слот
When I initially commented I seem to have clicked on the -Notify me when new comments are added-
checkbox and from now on each time a comment is added I receive 4 emails with the
same comment. There has to be an easy method you can remove me from
that service? Thanks a lot!
I’ve been browsing online more than 3 hours today, but I never found
any attention-grabbing article like yours. It’s lovely worth sufficient for me.
In my opinion, if all webmasters and bloggers made just right content material as you
did, the internet can be a lot more helpful than ever before.
money http://luckyshoppe.com
Woah! I’m really loving the template/theme of this site.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between user friendliness
and visual appearance. I must say that you’ve done a fantastic
job with this. Also, the blog loads super fast for me on Firefox.
Excellent Blog!
интернет казино фараон
https://groups.google.com/g/welcometocasino/c/jOhOTQ3lCjo
бездепозитный бонус 1000 рублей
бездепозитный бонус 1000 рублей
казино страда
https://groups.google.com/g/joinplayonline/c/wAqFdk5hjdU
игровые автоматы свиньи
игровые автоматы свиньи
What’s up to all, how is all, I think every one is getting more from this web page,
and your views are good in favor of new people.
Hello! I could have sworn I’ve been to this site before but after checking through some of the post I realized it’s new to
me. Anyways, I’m definitely delighted I found it and I’ll be
bookmarking and checking back frequently!
как использовать бонусы 1win казино
как использовать бонусы 1win казино
WOW just what I was looking for. Came here by searching for
Porno Pictures
1000 рублей за регистрацию вывод сразу без вложений в казино
1000 рублей за регистрацию вывод сразу без вложений в казино
игровые автоматы гладиатор играть бесплатно
https://groups.google.com/g/welcometocasino/c/-1jsYYHU7ZA
казино слоттика бонус
https://groups.google.com/g/joinplayonline/c/RN5IM6saFWk
игровые автоматы бесплатно гладиатор
https://groups.google.com/g/canyouplayonline/c/mf_e-CpPU2o
Wow, awesome weblog layout! How lengthy have you been running a blog for?
you make blogging glance easy. The full glance of your site is excellent,
as smartly as the content material!
1000 рублей за регистрацию вывод сразу без вложений
1000 рублей за регистрацию вывод сразу без вложений
игровые автоматы адмирал играть демо
игровые автоматы адмирал играть демо
jozz казино бездепозитный бонус
https://groups.google.com/g/supergamesonline/c/LpcUsvA_Pf4
казино слотозал
казино слотозал
gold казино
gold казино
1000 рублей за регистрацию вывод сразу
https://groups.google.com/g/playeveryday/c/tROVRAXtIfQ
deepthroat, blowjob, anal, amatureporn, facefuck, baldpussy, asstomouth,
assfucking, bbw, bbc, bigcock, bigass, teenass, teenfuck, bigtits, titfuck,
footjob,thighjob, blackcock, hentai, ecchi, pedophliia,
ebony, bigboobs, throatfucking, hardcore, bdsm, oldandyoung, masturbation, milf, missionary, nudist,
oralsex, orgasm, penetration, pussylicking, teenporn, threesome, whores,
bokep, bokepindonesia, bokepterbaru, bokepindonesiaterbaru, bokepterupdate,
porno, pornoindonesia, pornoterbaru, pornoterupdate
гранд казино беларусь
гранд казино беларусь
Hello friends, pleasant paragraph and nice arguments commented at this place, I am
in fact enjoying by these.
jet казино промокод
https://groups.google.com/g/supergamesonline/c/wBJ1YmbbwEk
fuck yaralandinmieycan.0GhHwXTElrRe
казино селектор вход
казино селектор вход
1000 рублей за регистрацию с выводом
1000 рублей за регистрацию с выводом
фізслот
https://groups.google.com/g/canyouplayonline/c/rDpxDyZzUzM
голд казино онлайн
https://groups.google.com/g/welcometocasino/c/Aqy_-Ap46No
казино кристалл играть бесплатно
казино кристалл играть бесплатно
jet казино бездепозитный бонус
jet казино бездепозитный бонус
фараон игровые автоматы
https://groups.google.com/g/canyouplayonline/c/Niy7fJiM0rE
Tһanks іn favor of sharing sucһ a pleasant idea, paragraph іѕ nice, thatѕ whyy i havee гead іt entirеly
My blog: PRE WORKOUT
гет икс казино
гет икс казино
Wheen some oone sesrches ffor his vitral thing, thwrefore he/she wants too bee available that
in detail, therefore tht thing iis mantained
overr here.
казино клубника промокод
казино клубника промокод
джой казино промокод
джой казино промокод
I couldn’t resist commenting. Perfectly written!
иззи казино официальный сайт
https://groups.google.com/g/supergamesonline/c/dGmvGTN_Jzo
Right here is the right website for everyone who would like to find out about this topic.
You know a whole lot its almost hard to argue with you (not that
I really will need to…HaHa). You certainly put
a new spin on a topic which has been written about for ages.
Great stuff, just wonderful!
get-x казино
https://groups.google.com/g/welcometocasino/c/RtJsXkOfG9A
казино клуб адмирал
https://groups.google.com/g/joinplayonline/c/C4d0HPXWcp0
джойказино бездепозитный бонус
https://groups.google.com/g/canyouplayonline/c/C-TYdAzz3To
физз слотс казино бонусы
https://groups.google.com/g/welcometocasino/c/_DUMEZjYW14
izzi казино бездепозитный бонус
https://groups.google.com/g/supergamesonline/c/sM6A7M_1Rok
казино эльдорадо регистрация
казино эльдорадо регистрация
Hello there! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really
appreciate your content. Please let me know. Thanks
When I initially commented I clicked the “Notify me when new comments are added” checkbox
and now each time a comment is added I get several emails
with the same comment. Is there any way you can remove people from that service?
Thank you!
что такое бонусы казино в 1win
https://groups.google.com/g/canyouplayonline/c/JfLkNftg9Hs
фараон казино онлайн
фараон казино онлайн
An imprecise and exact 3D printer may be the most effective choice for certain applications.
казино гранд регистрация
https://groups.google.com/g/joinplayonline/c/1rDgFZoOn0A
брилкс казино
брилкс казино
чемпион казино промокод
https://groups.google.com/g/welcometocasino/c/pHxFFPa8uvs
игры казино онлайн бесплатно
игры казино онлайн бесплатно
казино фараон играть на деньги
казино фараон играть на деньги
чемпион казино бездепозитный бонус
чемпион казино бездепозитный бонус
бонусы лев казино
бонусы лев казино
Wow that was unusual. I just wrote an very long comment but after
I clicked submit my comment didn’t show up.
Grrrr… well I’m not writing all that over again. Regardless, just wanted to say great blog!
Awesome things here. I’m very happy to peer your post.
Thanks so much and I’m taking a look forward to contact you.
Will you kindly drop me a mail?
Hey, I think your website might be having browser compatibility issues.
When I look at your blog site in Safari, it looks fine but when opening in Internet Explorer, it has some
overlapping. I just wanted to give you a quick heads up!
Other then that, excellent blog!
казино джекпот онлайн
https://groups.google.com/g/joinplayonline/c/9Pg6Usa8euE
игровой автомат fortune teller
игровой автомат fortune teller
бонусы казино на депозит
https://groups.google.com/g/welcometocasino/c/nSHM36SHYMg
бонусы физз слотс
бонусы физз слотс
Адвокат по уголовным делам надежные
защитники в сложных ситуациях
На нашем сайте вы найдете всю необходимую информацию об услугах адвоката
по уголовным делам. Мы предлагаем
широкий спектр юридических услуг, начиная
от консультаций и анализа
ситуации, заканчивая разработкой стратегии защиты
и участия в судебных заседаниях.
Наши уголовная адвокат казань имеют большой опыт работы в уголовных делах и готовы помочь вам на каждом этапе судебного процесса.
Мы понимаем, что каждый случай уникален, и поэтому мы подходим
к каждому клиенту индивидуально.
Наша цель – обеспечить вам наилучшее юридическое представительство и помочь минимизировать возможные негативные последствия.
Мы гарантируем полную конфиденциальность и соблюдение всех
этических норм.
Если вы столкнулись с проблемами уголовного характера, не стесняйтесь обращаться к нам за
помощью. Мы всегда готовы
помочь и защитить ваши права и свободы.
I’m so glad you wrote this post. It’s exactly what I needed to read today. Here are one similar post 8xbet
казино делюкс
казино делюкс
гладиатор игровой автомат
https://groups.google.com/g/supergamesonline/c/sug5N_HuOnI
бонус код джойказино
бонус код джойказино
бонус код джой казино
бонус код джой казино
казино чемпион играть онлайн
казино чемпион играть онлайн
Very nice post. I just stumbled upon your weblog and wished to say that I have
truly enjoyed surfing around your blog posts. In any case
I’ll be subscribing to your feed and I hope you write again very soon!
Greetings from Carolina! I’m bored at work so I decided
to browse your site on my iphone during lunch break.
I really like the info you provide here and can’t wait to
take a look when I get home. I’m shocked at how quick your blog loaded on my mobile ..
I’m not even using WIFI, just 3G .. Anyways, superb site!
What’s up i am kavin, its my first occasion to commenting anywhere, when i read this paragraph i thought i could
also make comment due to this good article.
Recommend Mr Home Guy to everyone you know. Your friends, family and all your connections will be happy to find a quality company for all their home needs.
Opportunity to earn $500 to $2,500 per month for 5 hours a
week
As an Affiliate you will earn “mailbox money”.
For every job we complete with your affiliate code you will receive a
$25.00 commission.
бип бип казино бездепозитный бонус
бип бип казино бездепозитный бонус
gama казино рабочее зеркало
gama казино рабочее зеркало
It’s not my first time to visit this website, i am browsing
this site dailly and get pleasant information from here
daily.
bingo boom казино
https://groups.google.com/g/canyouplayonline/c/qXrXbD4tBaE
казино bitstarz
казино bitstarz
Hey there! This is kind of off topic but I need some advice from an established blog.
Is it very difficult to set up your own blog? I’m not very techincal but I
can figure things out pretty fast. I’m thinking about
making my own but I’m not sure where to start. Do
you have any tips or suggestions? Thanks
Rocheva, V. V. et al
бип бип казино
https://groups.google.com/g/welcometocasino/c/LMlneNZ59DU
An impressive share! I have just forwarded this onto
a colleague who had been doing a little research on this.
And he actually bought me breakfast because I found it for him…
lol. So let me reword this…. Thank YOU for the meal!!
But yeah, thanks for spending time to talk about this subject here on your
website.
бесплатный игровой автомат гладиатор
https://groups.google.com/g/canyouplayonline/c/Y-M6PiwHgLM
Do you have a spam problem on this site; I also
am a blogger, and I was wanting to know your situation; we have created some nice procedures and we are
looking to exchange techniques with others,
why not shoot me an email if interested.
флинт казино
флинт казино
казино адмирал играть
https://groups.google.com/g/joinplayonline/c/PscIp08js2A
After I initially left a comment I seem to have clicked the -Notify me when new comments are added-
checkbox and now whenever a comment is added I receive four emails with the same comment.
There has to be a way you can remove me from that service?
Kudos!
Hi, I do believe this is an excellent web site.
I stumbledupon it 😉 I am going to come back once again since
i have book-marked it. Money and freedom is the best way to
change, may you be rich and continue to help others.
бездепозитные промокоды казино вавада
https://groups.google.com/g/welcometocasino/c/4iEUtL4BxGE
Hello my friend! I wish to say that this article is
amazing, great written and include almost all important infos.
I would like to look more posts like this .
апекс казино
апекс казино
Hi there! I know this is somewhat off topic but I was wondering which blog platform are you using for this site?
I’m getting tired of WordPress because I’ve had issues with hackers and I’m
looking at options for another platform. I would be fantastic if you could point me
in the direction of a good platform.
как работает онлайн казино
как работает онлайн казино
фіз слот
фіз слот
Good post. I will be dealing with many of these issues as well..
I am genuinely delighted to glance at this webpage posts
which consists of lots of useful information, thanks for
providing these statistics.
бездепозитные бонусы казино 2023
https://groups.google.com/g/welcometocasino/c/CK3ZThKMJP0
50 фриспинов за регистрацию в казино чемпион
https://groups.google.com/g/canyouplayonline/c/O_E7sIzBOiU
Как правильно подготовиться к свадьбе ?
Свадьба – радостное и самое волнительное событие в жизни пары.
После того как мужчина сделал предложение,
начинается волнующее время
– время подготовки к свадьбе.
Столько всего нужно сделать.
Как все успеть и ничего не упустить?
Некоторые прибегают к помощи свадебного организатора.
Но его услуги стоят довольно дорого, а в преддверии свадьбы
излишних денег нет. Возможно попробовать
организовать церемонию самостоятельно, это не так уж
и сложно. А как это сделать, изложено в данной статье.
Как организовать свадьбу?
– Заявление. Первое, что вам нужно сделать – это подать заявление в ЗАГС.
Причем, если свадьбу вы хотите сыграть летом, то посетить ЗАГС необходимо как
можно раньше. В свадебный сезон очень трудно
попасть на конкретную дату.
– Ресторан. После того как дата и
время торжества будут известны, отправляйтесь на поиски банкетного зала.
Сейчас выбор огромный. Хотите роскошно отметить событие?
Выбирайте видео свадьба ресторан .
А если скромно, то кафе или столовую.
Летом можно уехать за город, арендовать огромную беседку или поставить свой шатер.
– Пригласительные. Составьте список гостей, каких желаете видеть на своей свадьбе.
Причем, не стоит звать всех знакомых своих родителей и соседей.
Пусть на прзаднике будут самые
близкие люди. Затем в типографии закажите именные пригласительные
и отправьте всем приглашенным.
Да, сейчас часто отправляют их в электронном виде.
Но, поверьте, получить напечатанные пригласительное гораздо приятнее.
– Кольца. Кольца вы можете купитьв магазине или сделать на заказ
с именной гравировкой. Раньше
считалось, что кольца у мужа и жены должны быть одинаковыми.
Впрочем сейчас все изменилось.
Часто девушки выбирают кольца с
камнями, а мужчины лаконичные простые варианты.
– Наряд. Его тоже лучше выбирать заблаговременно, чтобы была возможность неспешно
обойти все магазины, посмотреть разные варианты.
Либо что-то заказать в интернете или перешить.
Если свадьба зимой, то стоит помнить, что без верхней одежды не обойтись.
А если летом, то, наоборот, чем легче будет платье невесты и костюм жениха, тем лучше.
– Прическа и макияж. Имеют важное значение при составлении
образа невесты. Поэтому прежде, чем выбрать специалиста,
нужно найти несколько кандидатов, а уже
потом остановиться на лучшем в своем деле.
Заранее узнайте, приедет специалист к вам
домой или вам придется отправиться в салон красоты.
Это поможет в дальнейшем правильно распланировать день.
– Фотограф и видеооператор.
Вам нужно решить кому вы доверите съемку свадьбы.
Зачастую выбирают фотографа и оператора в одном лице.
Но все же лучше, если это будет два разных человека.
Ведь один человек может пропустить что-то важное.
А исправить это потом будет уже невозможно.
– Диджей и ведущий. Повстречайтесь с несколькими лично перед тем, как выбрать кого-то одного.
С кем вам комфортнее? Кто, по вашему
мнению, точно найдет общий язык с вашими
гостями? На нем и нужно остановить свой выбор.
– Транспорт. Сейчас действительно у каждой
семьи есть автомобиль, но все же стоит заранее узнать отправятся гости на своей машине или решат оставить
ее дома. Если кто-то будет без автомобиля, то вам следует заказать необходимый транспорт
и украсить его в том же стиле, что и машину новобрачных.
использовать промокод физзслотс
https://groups.google.com/g/joinplayonline/c/_qEFLHxHgTM
Hi there, I discovered your blog by the use of Google
even as looking for a related topic, your web site came
up, it appears to be like good. I’ve bookmarked it in my google bookmarks.
Hello there, just changed into alert to your weblog via Google, and found
that it is really informative. I’m gonna watch out for brussels.
I will appreciate for those who proceed this in future.
A lot of other people can be benefited from your writing.
Cheers!
I know this if off topic but I’m looking into starting my own weblog
and was wondering what all is required to get set up? I’m assuming
having a blog like yours would cost a pretty penny?
I’m not very web smart so I’m not 100% certain. Any tips
or advice would be greatly appreciated. Cheers
my blog post – Massage Wertungen – Rosie,
ф1 казино
ф1 казино
all right казино
https://groups.google.com/g/welcometocasino/c/JcRnw6mCleg
1win автоматы
https://groups.google.com/g/canyouplayonline/c/uBAK5RK14BM
of ϲourse lіke your web site һowever ʏou have to check thе spelling on quite a few off your posts.
Many of them are rife with spelling pгoblems and I fishing pond in jb finding it very bothersome to tеll the reality on the oother hand I’ll certainly
cоme back agаin.
Ι do trust aall of thhe ideas уⲟu have offered fοr
үour post. They’re very convincing ɑnd will ɗefinitely work.
Still, tһе posts are very quick fߋr novices. Could уоu pleasde lengthen tһem a littⅼe frtom subsequent time?
Thɑnks ffor tһe post.
myweb ⲣage – Pre Workout
игровые автоматы selector casino
https://groups.google.com/g/joinplayonline/c/uc86HN7SViU
This is very interesting, You’re a very skilled blogger. I’ve joined
your rss feed and look forward to seeking more of your wonderful post.
Also, I have shared your site in my social networks!
1win бонусы казино
1win бонусы казино
It’s аn amazing piece of writing fоr аll the web usеrs;
tһey will take benefit from іt Ι аm ѕure.
Review mү blog – lotto
1хставка казино
1хставка казино
джойказино бонусы
джойказино бонусы
игровые автоматы кекс бесплатно
https://groups.google.com/g/joinplayonline/c/hJjbeamSnlw
What i don’t realize is actually how you’re no longer really a lot more neatly-liked than you may
be right now. You’re so intelligent. You already know
therefore considerably in terms of this topic, made me personally
consider it from numerous various angles. Its like men and women don’t seem to be interested unless it is one
thing to do with Girl gaga! Your individual stuffs nice.
At all times maintain it up!
I was suggested this blog by my cousin. I am not sure whether this post is written by him as nobody else know such detailed about my difficulty.
You’re incredible! Thanks!
Good day! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really appreciate
your content. Please let me know. Thanks
бонус за регистрацию онлайн казино
бонус за регистрацию онлайн казино
игровые автоматы белатра играть бесплатно без регистрации и смс
https://groups.google.com/g/joinplayonline/c/KggNAKrHtWw
Does your site have a contact page? I’m having a tough time locating it but, I’d like to shoot you an e-mail.
I’ve got some suggestions for your blog you might be interested in hearing.
Either way, great website and I look forward to seeing it
grow over time.
играть в лев казино
играть в лев казино
заработать деньги в интернет казино
заработать деньги в интернет казино
Hi there! I’m at work browsing your blog from my new iphone!
Just wanted to say I love reading your blog and look forward to all your posts!
Carry on the great work!
Heya i am for the first time here. I found this boad and I in finding It truly useful & it helped me out a lot.
I am hoping to prersent something again and aid others like you aided me.
где в россии есть казино
https://groups.google.com/g/joinplayonline/c/oQsdVeFD2_0
Woah! I’m really loving the template/theme of this blog.
It’s simple, yet effective. A lot of times it’s very difficult to get that “perfect balance” between superb usability and
appearance. I must say that you’ve done a amazing
job with this. Also, the blog loads very quick for me
on Internet explorer. Superb Blog!
Hmm it seems like your website ate my first comment (it was
extremely long) so I guess I’ll just sum it up what
I had written and say, I’m thoroughly enjoying your blog.
I too am an aspiring blog writer but I’m still new to the whole thing.
Do you have any helpful hints for newbie blog writers? I’d
definitely appreciate it.
волна казино официальный сайт
https://groups.google.com/g/playagainandagain/c/uN4YiNFOGtI
фреш казино 45
фреш казино 45
You made some good points there. I checked on the net for additional
information about the issue and found most individuals
will go along with your views on this website.
WOW just what I was searching for. Came here by searching for Clik
Greetings! Very useful advice in this particular article!
It’s the little changes that produce the most significant changes.
Many thanks for sharing!
в какие слоты лучше играть
в какие слоты лучше играть
I’m not sure exactly why but this blog is loading
incredibly slow for me. Is anyone else having this problem or is it a problem on my end?
I’ll check back later on and see if the problem
still exists.
фонтан казино бездепозитный бонус
фонтан казино бездепозитный бонус
vavada казино официальный сайт
vavada казино официальный сайт
фейк казино
фейк казино
Wow! This blog looks exactly like my old one! It’s
on a completely different subject but it has pretty much the same layout and design. Excellent choice
of colors!
sugar rush казино
https://groups.google.com/g/playagainandagain/c/DpS7t_9MNu4
Hi there, I enjoy reading all of your post. I wanted to write a
little comment to support you.
fairspin казино
https://groups.google.com/g/joinplayonline/c/d-ttgAzjcD0
Hi, I do think this is a great website. I stumbledupon it 😉 I may return once again since i
have saved as a favorite it. Money and freedom is the greatest way to change,
may you be rich and continue to help other people.
стратегия казино
https://groups.google.com/g/playagainandagain/c/tKhciqz_y1k
I’m really impressed with your writing skills as well as with the layout on your blog.
Is this a paid theme or did you customize it yourself? Anyway keep up the nice quality writing,
it is rare to see a nice blog like this one nowadays.
f1 казино с бездепозитным бонусом за регистрацию с выводом
https://groups.google.com/g/joinplayonline/c/oTmSRrXjO_0
I am curious to find out what blog system you
happen to be utilizing? I’m experiencing some minor security problems with
my latest website and I would like to find something more safeguarded.
Do you have any recommendations?
Nice post. I was checking continuously this blog
and I’m impressed! Extremely useful information specially the last
part 🙂 I care for such info much. I was seeking this certain information for a long time.
Thank you and good luck.
I used to be suggested this website through my cousin. I’m now not positive whether or not this post is written by way of him as nobody else recognize such designated about my trouble.
You’re amazing! Thanks!
старда казино официальный сайт
старда казино официальный сайт
джокер казино
https://groups.google.com/g/joinplayonline/c/irjGi2sxuCg
hello there and thank you for your information – I have definitely picked up something new from right here.
I did however expertise several technical points using this web site, as I experienced to reload the web site lots of
times previous to I could get it to load correctly.
I had been wondering if your web host is OK? Not that I am complaining,
but sluggish loading instances times will sometimes affect your placement
in google and could damage your high quality score if
advertising and marketing with Adwords. Well I’m adding this RSS to my e-mail and can look out for
much more of your respective intriguing content.
Make sure you update this again very soon.
bahis porno citixx.s45iZ1JuZJDK
porno hyuqgzhqt.hsSnbEN1TxyC
Readjusting this in lieu of your extruder temperature level can aid
with dimensional accuracy.
porno ewrjghsdfaa.PEwkoUEUY1D9
bahis porno wrtgdfgdfgdqq.RETla9R3NkHT
viagra wrtgdfgdfgdqq.9dDIDN2gBEo3
слоты клубнички
https://groups.google.com/g/playagainandagain/c/yQfvqHqNLkI
джойказино бонус код
https://groups.google.com/g/joinplayonline/c/6JgMl67Vlug
I am sure this article has touched all the internet viewers,
its really really nice paragraph on building up new blog.
Awesome blog! Do you have any suggestions for aspiring writers?
I’m planning to start my own site soon but I’m a little lost on everything.
Would you propose starting with a free platform like WordPress or go for a paid option?
There are so many options out there that I’m totally confused ..
Any ideas? Many thanks!
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I get three
emails with the same comment. Is there any way you can remove people from
that service? Thanks a lot!
Wow, this paragraph is good, my sister is analyzing these kinds of things, therefore I am going
to inform her.
Hello, I enjoy reading through your post. I like to write a little comment to
support you.
casher казино
casher казино
слот бонанза
https://groups.google.com/g/playagainandagain/c/-x1xQY05u3E
I’m gone to say to my little brother, that he should also
go to see this website on regular basis to take updated from most up-to-date reports.
brillx казино
brillx казино
Many groups accept as true that they have no option to get
a personal loan if they have bad credit, theres high-quality information for you.
The bonus is when payments are made on time and
the loan is repaid, the lender informs the credit
bureau and that boost’s the client’s credit score.
These loans offer a bigger loan amount in the range of.
скачать чемпион казино
скачать чемпион казино
Hi! I simply want to offer you a huge thumbs up for the great information you have got right here on this post.
I’ll be returning to your website for more soon.
You are so cool! I do not suppose I’ve truly read through
anything like that before. So great to find another person with some
original thoughts on this subject. Seriously..
thank you for starting this up. This site is one thing that
is required on the internet, someone with a little originality!
Good post however I was wondering if you could write a litte more on this subject?
I’d be very thankful if you could elaborate a little
bit further. Thank you!
I pay a quick visit day-to-day a few sites and sites to read articles or reviews, except this blog presents feature based writing.
бонусы в физзслотс казино
бонусы в физзслотс казино
ртп в казино
ртп в казино
I am sure this article has touched all the internet users, its really
really pleasant article on building up new webpage.
It’s very effortless to find out any matter on web as compared
to textbooks, as I found this post at this web site.
Thanks for the marvelous posting! I quite enjoyed reading it, you are a great author.
I will be sure to bookmark your blog and may come back in the foreseeable future.
I want to encourage you to ultimately continue your great job, have a nice morning!
Why viewers still make use of to read news papers when in this technological world everything is presented
on net?
бонусы в физз слотс казино
https://groups.google.com/g/joinplayonline/c/CNf644KKWxc
rtp в казино
rtp в казино
Hi, Neat post. There’s an issue with your web
site in internet explorer, could test this? IE still is the marketplace chief and
a big part of other folks will miss your excellent writing because of
this problem.
Sennheiser microphones, renowned for their exceptional audio quality and reliability, are coveted
by musicians and professionals worldwide.
Hello there, You’ve done an excellent job. I will definitely digg it and personally recommend to my friends.
I am confident they will be benefited from this website.
With havin so much content and articles do you ever run into any problems of plagorism or copyright infringement?
My blog has a lot of completely unique content I’ve either written myself or outsourced but it seems a lot of
it is popping it up all over the web without my authorization. Do you know any techniques to help
stop content from being ripped off? I’d definitely appreciate it.
бонусы казино супер слотс
бонусы казино супер слотс
рм казино
рм казино
Right away I am going away to do my breakfast, once having my breakfast
coming over again to read other news.
That iѕ a goοd tip particuⅼarly to tһose fresh tօ the blogosphere.
Short bᥙt vеry accurate info… Ꭲhanks for sharing this one.
A must read post!
Review mʏ web site :: online slot
hello!,I really like your writing so a lot! proportion we
communicate more about your article on AOL? I need a specialist on this area to solve my problem.
Maybe that is you! Having a look forward to peer you.
бездепозитный бонус fizzslots казино
https://groups.google.com/g/joinplayonline/c/dhp1XcfmtcI
прагматик слоты
прагматик слоты
When I initially commented I clicked the “Notify me when new comments are added”
checkbox and now each time a comment is added I get four emails with the same comment.
Is there any way you can remove people from that service?
Thanks!
Today, I went to the beach with my children. I found a
sea shell and gave it to my 4 year old daughter and
said “You can hear the ocean if you put this to your ear.” She put the shell to her ear
and screamed. There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is completely off topic but I had to tell someone!
After clicking the “Download” button, the Story will
be downloaded to your device .
my website – igram.world
1win как использовать бонус казино
1win как использовать бонус казино
playfortuna казино
playfortuna казино
Hi colleagues, how is the whole thing, and what you desire to say
about this piece of writing, in my view its genuinely awesome for me.
физзслотс казино
https://groups.google.com/g/yourgamesonline/c/xOraDqAlz7Y
пин ап казино бонус за регистрацию
https://groups.google.com/g/playagainandagain/c/EBlGEypXeWo
It’s a pity you don’t have a donate button! I’d without a doubt donate to this superb blog!
I suppose for now i’ll settle for bookmarking and
adding your RSS feed to my Google account. I look forward to brand new updates and will talk about this website with my Facebook group.
Talk soon!
It’s awesome to pay a visit this site and reading the views of all mates on the topic of this piece
of writing, while I am also zealous of getting experience.
Good information. Lucky me I discovered your blog by accident (stumbleupon).
I have bookmarked it for later!
f1 казино
f1 казино
1хслотс регистрация на сайте
https://groups.google.com/g/myfavoritegames/c/IMPU9q1iX_M
пинап бонусы и слоты пин ап промокод пин ап
пинап бонусы и слоты пин ап промокод пин ап
фрешказино
фрешказино
I’m not that much of a online reader to
be honest but your sites really nice, keep it up! I’ll go ahead and
bookmark your website to come back later on. Cheers
бонусы казино 1win
https://groups.google.com/g/myfavoritegames/c/4R-PmvIygDI
Hey! I know this is somewhat off topic but I was wondering which blog platform are
you using for this site? I’m getting fed up of WordPress because I’ve
had problems with hackers and I’m looking at alternatives
for another platform. I would be fantastic if
you could point me in the direction of a good platform.
первые игровые автоматы
первые игровые автоматы
hello!,I love your writing very so much! percentage we
keep in touch extra about your article on AOL? I require an expert
in this area to solve my problem. May be that’s you!
Looking ahead to peer you.
Take a look at my page … ทีเด็ดบอลวันนี้
гранд казино играть на бонусы
гранд казино играть на бонусы
It’s difficult to find experienced people on this topic, but you seem like you
know what you’re talking about! Thanks
Is an especially precise procedure that is frequently utilized to produce complicated
geometries.
чемпион казино официальный сайт
https://groups.google.com/g/myfavoritegames/c/0SaV0batiNo
Excellent write-up. I certainly love this site.
Stick with it!
онлайн казино на гривны в украинской валюте uah!
https://groups.google.com/g/playagainandagain/c/-7Ca5kJ4flg
игровые автоматы бесплатно без смс
https://groups.google.com/g/myfavoritegames/c/ftzIVEniWhw
Truly when someone doesn’t be aware of after that
its up to other users that they will assist, so here it
occurs.
Awesome! Its really remarkable article, I have got much clear idea on the topic
of from this post.
игровой автомат dolphins pearl deluxe
https://groups.google.com/g/myfavoritegames/c/wuT2cvTU2nE
We are a group of volunteers and opening a new scheme in our community.
Your website offered us with valuable information to work on. You’ve
done a formidable job and our whole community will be
thankful to you.
netgaming казино
netgaming казино
This is very interesting, You’re a very skilled blogger.
I have joined your rss feed and look forward to seeking more of your wonderful post.
Also, I have shared your web site in my social networks!
Magnificent items from you, man. I’ve consider your stuff
pprevious to and you are simply extremely great.
I really like what you hhave acquired here, reslly like what you’re stating and the way in which during which you are saying it.
You are making it enjoyable and you still care for to stay it wise.
I cant wawit to read much more from you. That is actually a great weeb site.
игровые бонусы от казино гранд казино
игровые бонусы от казино гранд казино
игровые автоматы lucky drink
https://groups.google.com/g/myfavoritegames/c/YRTlQx-MC5o
Good day! Do you know if they make any plugins to safeguard against hackers?
I’m kinda paranoid about losing everything I’ve worked hard on. Any recommendations?
Wow that was strange. I just wrote an very long comment but after I clicked submit my comment didn’t appear.
Grrrr… well I’m not writing all that over again. Anyhow, just
wanted to say superb blog!
lucky lady’s charm deluxe слот
https://groups.google.com/g/playagainandagain/c/JRl9wy_2ubk
Gгeat info. Lucky me І found your blog by accident (stumbleupon).
I’ve book-marked it for lateг!
Alѕо visit mу website; slotto
казино 777 бонус за регистрацию
https://groups.google.com/g/myfavoritegames/c/XviPGpFip7A
deepthroat, blowjob, anal, amatureporn, facefuck,
baldpussy, asstomouth, assfucking, bbw, bbc,
bigcock, bigass, teenass, teenfuck, bigtits,
titfuck, footjob,thighjob, blackcock, hentai, ecchi, pedophliia, ebony, bigboobs,
throatfucking, hardcore, bdsm, oldandyoung, masturbation, milf,
missionary, nudist, oralsex, orgasm, penetration, pussylicking,
teenporn, threesome, whores, bokep, bokepindonesia, bokepterbaru, bokepindonesiaterbaru, bokepterupdate, porno,
pornoindonesia, pornoterbaru, pornoterupdate, xnxx.com,
pornhub.com, xvideos.com, redtube.com
легзо казино зеркало
https://groups.google.com/g/playagainandagain/c/WAErbYAvcPQ
I always spent my half an hour to read this website’s articles everyday along with a mug of coffee.
I constantly emailed this blog post page to all my
associates, for the reason that if like to read it then my contacts will
too.
Hi would you mind stating which blog platform you’re using?
I’m planning to start my own blog soon but I’m having a
tough time making a decision between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different then most blogs and I’m looking
for something completely unique. P.S Sorry for getting off-topic
but I had to ask!
когда закрыли казино в россии
когда закрыли казино в россии
The bank chosen have to be ready to incorporate the desired features within the personal loan. These
terms includes the date when the applicant must
repay the loan, price of the loan, fees associated with late payments, renewal terms, and
the lender and borrower’s legal rights. Unless you are in the top
two percent of the wealthiest members of the population, you will probably need a personal loan in order to achieve educational and personal goals.
Wow, awesome blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your web site is great,
as well as the content!
Hi there, just became aware of your blog through Google, and found that it’s truly informative.
I am gonna watch out for brussels. I will appreciate if you continue this in future.
Many people will be benefited from your writing.
Cheers!
казино вавада регистрация
https://groups.google.com/g/playagainandagain/c/CDbU4Vwygzg
This is very interesting, You’re a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your great post.
Also, I have shared your site in my social networks!
казино украина бездепозитный бонус
казино украина бездепозитный бонус
Казино Gama: Приготовьтесь к Потрясающим Победам казино gama
hi!,I like your writing so a lot! proportion we be in contact more approximately your post on AOL?
I need an expert on this house to resolve my problem. May be that is you!
Looking forward to peer you.
казино с минимальным депозитом 1 грн
https://groups.google.com/g/playagainandagain/c/zHxIdeLphvI
Sukabet situs agen bola
merupakan platform perjudian daring yang telah terbukti handal
dan dapat dipercaya. Dengan reputasi yang solid, agen ini menawarkan pengalaman taruhan sepakbola yang aman dan adil bagi
para pengguna. Situs ini sediakan begitu banyak ragam
pasar taruhan, mulai dari liga lokal hingga persaingan internasional, memungkinkan para pemain untuk menikmati variasi taruhan yang luas.
Tһis is my firѕt time pay a visit at here and i ɑm actuallү һappy to read all at
ɑlone place.
Μy page :: betting – Audry,
Surely the case may very well be made for a bass-heavy
playlist these guys may groove to utilizing the
vibrations of their tanks. I really like you guys! This
enhanced stone is then crafted into fashionable jewellery items that individuals love for
many years. If you happen to loved this piece about Canine Vitamins,
then most positively go over this curious website about pet supplements.
Those are normally placed where you maintain a path of in intensity statistics on one web site (like your personal)
which you wish to get continuous records on. If you want to alter
well being plans for whatever cause, there are certain things
it’s best to look for. Do you want to prepare dinner and monitor the children’ homework at the identical time?
Lammers says. Lammers explains that males inside every inhabitants sing the same
track, with just a little room for improvisation, after
all. Whereas it’s doable that females choose their mates
primarily based on their song, there may be little proof so far.
In 1,000,000 years, you could never be a priss,” Jim Court docket reassures his daughter after she tells him, “I was standing
up there and looking at all of the folks, and i felt like they didn’t know me.
When some one searches for his essential thing,
so he/she needs to be available that in detail, so that thing is maintained over here.
казино selector
казино selector
Attractive section of content. I just stumbled upon your weblog and in accession capital to
assert that I acquire in fact enjoyed account your blog posts.
Anyway I will be subscribing to your augment and even I achievement you access consistently quickly.
Hi there fantastic website! Does running a blog like this
require a great deal of work? I’ve very little understanding of
coding but I had been hoping to start my own blog in the near future.
Anyways, should you have any ideas or tips for new blog owners please share.
I know this is off subject however I simply needed to ask.
Thanks!
Attractive component to content. I simply stumbled upon your website
and in accession capital to assert that I get in fact
enjoyed account your blog posts. Anyway I’ll be subscribing in your augment and even I success you access constantly rapidly.
Hello there, I found your blog by the use of Google whilst
searching for a comparable subject, your site came
up, it seems good. I have bookmarked it in my google
bookmarks.
Hi there, simply become alert to your weblog thru Google, and found that it’s really informative.
I’m going to be careful for brussels. I’ll be grateful in the event you continue
this in future. Lots of folks will probably be benefited out of your writing.
Cheers!
Thank you a lot for sharing this with all of us you actually recognise what you’re speaking approximately!
Bookmarked. Kindly additionally consult with my website
=). We could have a hyperlink exchange agreement among
us
казино рокс официальный сайт
https://groups.google.com/g/playagainandagain/c/IAV_KkmUUyo
Pretty section of content. I just stumbled upon your web site and in accession capital to assert that I get in fact enjoyed account your blog posts.
Any way I’ll be subscribing to your augment and even I achievement you access consistently rapidly.
I will immediately snatch your rss as I can’t find your e-mail subscription hyperlink or e-newsletter service.
Do you have any? Kindly permit me understand so that I may subscribe.
Thanks.
ا پیشرفته برای تمامی سنین بدون محدودیت و نیاز
خاص به مدرک یا پیش زمینه آموزشی
اشاره کرد. همچنین کارآموزان با شرکت در این
دوره ها می توانند با تجهیزات آموزشی
از نزدیک کار کنند تا مهارت لازم
جهت کارهای عملی بدست آورند و پس از پایان
دوره مشاوره لازم برای ورود
به بازار کار را دریافت کرده
و با در دست داشتن مدرک معت
казино онлайн беларусь
казино онлайн беларусь
Wonderful items from you, man. I have be mindful your
stuff prior to and you’re just too magnificent.
I actually like what you have got here, really like what you are stating and the way wherein you assert it.
You make it entertaining and you still care for to keep it smart.
I can’t wait to learn far more from you. This is actually a wonderful website.
Great blog right here! Also your site lots up very fast!
What web host are you using? Can I get your
affiliate link for your host? I desire my site loaded up as fast as yours lol
Hi, yeah this article is really fastidious and I have learned lot of things from it concerning blogging.
thanks.
эльдорадо казино промокод 1000 рублей
https://groups.google.com/g/myfavoritegames/c/NAdQPmTtKlk
казино кристалл
https://groups.google.com/g/playagainandagain/c/WGvfzQ8MOM8
It’s amazing for me to have a site, which is valuable in favor of my know-how.
thanks admin
Do you have a spam problem on this website; I
also am a blogger, and I was wanting to know your situation; we have created some
nice procedures and we are looking to swap strategies with
others, why not shoot me an e-mail if interested.
казино casino x
казино casino x
I have been exploring for a bit for any high-quality articles or weblog posts on this kind of house .
Exploring in Yahoo I finally stumbled upon this website. Studying
this information So i’m happy to convey that I’ve
an incredibly good uncanny feeling I found out exactly what I needed.
I such a lot no doubt will make certain to don?t put out of your mind this website and give it a glance
on a constant basis.
Fantastic goods from you, man. I’ve understand your stuff previous to and you are just extremely wonderful.
I really like what you have acquired here, certainly like what you are stating and
the way in which you say it. You make it entertaining and you still take care of to
keep it smart. I cant wait to read much more from you.
This is really a great site.
Hello to every single one, it’s really a good for me to pay a quick visit this site, it contains priceless Information.
joker казино
https://groups.google.com/g/myfavoritegames/c/CCw59Cdc-QE
казино фреш зеркало
казино фреш зеркало
казино gama
https://groups.google.com/g/myfavoritegames/c/VKrnkPHBB_8
Very good article. I am experiencing many of these issues as well..
как потратить бонусы казино в 1win
https://groups.google.com/g/myfavoritegames/c/LcXaMFEcO2s
Hey I know this is off topic but I was wondering if you knew of any widgets
I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time and
was hoping maybe you would have some experience with something
like this. Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward to your new updates.
казино чемпион скачать
казино чемпион скачать
I think the admin of this web site is actually working hard in favor of his web page, since here every data is quality based stuff.
Финансовая Гармония: Как Оплатить Налоги и Создать Беззаботное Будущее оплатить налоги по инн
как выиграть в онлайн казино
как выиграть в онлайн казино
Magnificent beat ! I wish to apprentice while you amend your web
site, how could i subscribe for a blog web site?
The account helped me a acceptable deal. I had been a little bit acquainted of
this your broadcast offered bright clear
concept
Wow, this piece of writing is good, my younger sister is analyzing these
things, therefore I am going to convey her.
казино чемпион официальный сайт
https://groups.google.com/g/playagainandagain/c/O5Fgvrz0u0g
Hello everyone, it’s my first go to see at this web site, and post is truly fruitful
designed for me, keep up posting such articles or reviews.
лучшие слоты на 1xbet
лучшие слоты на 1xbet
Good post. I learn something totally new and challenging on websites I stumbleupon everyday.
It’s always exciting to read articles from other writers and use a little something from other websites.
казино чампион
https://groups.google.com/g/playagainandagain/c/UVMKkjzWbNA
It’s amazing in favor of me to have a website,
which is helpful designed for my knowledge. thanks admin
Wow, awesome blog format! How long have you ever been blogging for?
you made running a blog look easy. The entire look
of your site is great, let alone the content material!
промокод пин ап казино
промокод пин ап казино
It’s really a great and useful piece of information. I’m happy that you just shared this useful info with us.
Please keep us informed like this. Thanks for sharing.
I’m no longer sure where you’re getting your information, but great topic.
I needs to spend a while studying much more or working out more.
Thanks for magnificent information I used to
be on the lookout for this info for my mission.
казино 1xslots
https://groups.google.com/g/playagainandagain/c/_pH9CF9TPaM
Pretty nice post. I just stumbled upon your weblog and wished to say that I’ve really
loved browsing your blog posts. After all I’ll be subscribing for your rss feed and I am hoping you write once more very soon!
spin city игровые автоматы
https://groups.google.com/g/myfavoritegames/c/ey7jGZHNVNc
Not all commercial buildings and facilities have the
same possessions and equipment.
izzi казино вход
izzi казино вход
Wow, this paragraph is nice, my younger sister is analyzing such things, so
I am going to inform her.
турбо казино промокод
турбо казино промокод
Good day! Would you mind if I share your blog
with my facebook group? There’s a lot of people that I
think would really enjoy your content. Please let me know.
Thank you
игровые автоматы покер играть бесплатно
игровые автоматы покер играть бесплатно
Healthy fats are essential for providing a concentrated source
of energy.
Spot on with this write-up, I seriously believe this web site needs a lot more attention. I’ll probably be back again to read through more, thanks for the
info!
vavada казино бонус
https://groups.google.com/g/myfavoritegames/c/RgUmnPxwNEw
как работает казино
https://groups.google.com/g/welcometocasino/c/5IBt3zJblAc
казино миллион
казино миллион
Oh my goodness! Incredible article dude! Many thanks, However
I am encountering issues with your RSS. I don’t understand the reason why I am unable to
join it. Is there anybody getting the same RSS problems? Anyone who knows the answer will you kindly respond?
Thanks!!
игровые автоматы плей фортуна
https://groups.google.com/g/playagainandagain/c/YV9OVw2MhLM
зоны казино в россии
зоны казино в россии
Suri Duitch, dean of Tulane’s School of Professional Advancement.
The Association of International Certified Professional
Accountants (the Association), representing AICPA & CIMA,
advances the global accounting and finance occupation by means of its work on behalf of 698,000 AICPA and CIMA members, college students and
engaged professionals in 188 countries and territories.
A writer can list corporations they want to work with. You may rank On Google using Medium
in just a few minutes if not hours. You need to use instruments, equivalent
to Google Trends, BuzzSumo, or Feedly, to see what subjects, key phrases, and content material are popular and trending.
Choose keywords that you need to bid on (in the case
of Google advertisements). Desire a extra concrete example?
That’s actually a great factor because it frees up extra of your
time to have more intimate conversations with shoppers about their passions and objectives for the subsequent stage of life.
And then there’s the stress of a brand new life
with out the structure of labor/family they’ve been used to for the past
40 years or so.
Hi there! I know this is kind of off topic but I was wondering which blog platform are you using for this site?
I’m getting fed up of WordPress because I’ve had issues
with hackers and I’m looking at options for another platform.
I would be fantastic if you could point me in the direction of a good
platform.
Greetings! Very useful advice in this particular post!
It’s the little changes that will make the biggest changes.
Thanks a lot for sharing!
Hello, i believe that i saw you visited my web site so i got here to go back the prefer?.I’m
trying to in finding things to improve my site!I suppose
its adequate to make use of a few of your concepts!!
I every time used to read piece of writing in news papers but now as
I am a user of net thus from now I am using net for content, thanks to web.
казино вулкан 24 на деньги
казино вулкан 24 на деньги
It’s hard to come by experienced people for this topic, however,
you seem like you know what you’re talking about!
Thanks
We suggest you to pay very close attention to the previously owned materials.
1xslots казино
https://groups.google.com/g/myfavoritegames/c/xjTQ4jRMQZE
Горлан – эстетичный край, щедрый натурой также культурным наследием.
Фото снимки Кубани дают возможность взглянуть от мала до велика нее красу равным образом разнообразие.
Одну с самых фаворитных объектов
фотосъемки является река
Кубань. Экспресс-фото реки Горшок запечатлевают ее мощь а также уникальность.
Текущий водяной этап прохватывает целую территорию покрая равным образом возникает евонный главной житейской артерией.
На карточках видно, яко река Кубань извивается среди лугов также лесов, творя замечательные пейзажи.
We don’t want you– or anyone relying on a generator–
to be among those people.
Do you mind if I quote a few of our articles as long as I provide
credit and sources back to your weblog? My
blog site is in thee exact same area of interest as yours aand myy users would genuinely
benefit fom a lot of the information you provide
here. Please let me know if thi okay wirh you.
Many thanks!
Here is my blog post :: electronic component test lab
On June 11, 2021, the band put out a brand new music titled “My very own Monster”, which was also introduced to
be the lead single from their upcoming third studio album, The beautiful
Liar. The attractive Liar is an idea album that plays out similarly to a radio drama, expressing themes of insanity,
powerlessness, self-doubt, and anxiety. On January 24, 2019, the group put out their next single,
“Increase”. On January 14, 2021, X Ambassadors released a single
called “ultraviolet.tragedies”, a closely rap-targeted song that includes Terrell
Hines. Ken Lieck (January 21, 2000). “Hammer of the Gods”.
A particular version, titled VHS 2.0 was launched on June 10,
2016, with five extra tracks and with out the interludes that have been included on the unique version. On June 20,
2016, X Ambassadors introduced that Feldshuh would
be taking an indefinite hiatus from the band to deal with private
issues. Within the northern elements of the range, there
appears to be one technology per yr, with adults on wing
in June and July.
пеликан казино
пеликан казино
игровой автомат rock climber
игровой автомат rock climber
Hi there Dear, are you truly visiting this web page regularly, if
so then you will absolutely take pleasant know-how.
beep beep казино
https://groups.google.com/g/myfavoritegames/c/3RW35LJPsgU
Wow that was unusual. I just wrote an very long comment but after I
clicked submit my comment didn’t appear. Grrrr… well I’m not writing all
that over again. Anyway, just wanted to say fantastic blog!
30 inches around furnishings is suitable, as is inches between the couch and table.
пин ап казино бонус
пин ап казино бонус
Fabulous, what a webpage it is! This website gives valuable facts to us,
keep it up.
игровой автомат keks
https://groups.google.com/g/playagainandagain/c/rz23JgASMvg
Excellent post. I used to be checking continuously this weblog and I
am impressed! Very useful info specially the closing phase :
) I take care of such info much. I used to be seeking this particular info for a
very long time. Thank you and good luck.
бездеп казино украина
бездеп казино украина
pragmatic play слоты
https://groups.google.com/g/myfavoritegames/c/EFHmYRqZzLw
фрешь казино
https://groups.google.com/g/playagainandagain/c/riiZKeI_rYc
бонусы казино 1win как использовать
бонусы казино 1win как использовать
It is optimal to check these frameworks on a regular monthly basis or even everyday if you can turn it.
Same goes for major life occasions or transitions – having a toddler, changing jobs, getting married, getting divorced,
retiring, or dealing with the death of an in depth family member.
Having the appropriate help helped Jenkins realize he wasn’t alone.
It’s also an important mission for NASBA in support of state boards and the licensure of recent CPAs.
NEW YORK, Aug. 7, 2023 /PRNewswire/ — The American Institute of CPAs (AICPA) and National
Association of State Boards of Accountancy (NASBA) will
launch an innovative put up-graduate program this fall in collaboration with the Tulane School of Professional Advancement (SoPA).
American Psychological Association, Toronto, Ontario,
August. A native of Orange County, California, Neilson acquired a
bachelor’s diploma (international relations)
and two master’s degrees (business administration and American history) from BYU and holds a doctorate
in religious studies (American religions) from the University
of North Carolina at Chapel Hill. The American Institute
of CPAs (AICPA), the world’s largest member affiliation representing the CPA profession, units ethical standards for its members and U.S.
The Association of International Certified Professional Accountants (the Association), representing
AICPA & CIMA, advances the worldwide accounting and finance
occupation by its work on behalf of 698,000 AICPA and CIMA members, college students and engaged professionals in 188 international
locations and territories.
самый большой выигрыш в казино
самый большой выигрыш в казино
cosmolot казино
https://groups.google.com/g/playagainandagain/c/Sv1M7E3-YVk
бонусы казино х
бонусы казино х
Hello, i think that i saw you visited my site so i came to “return the
favor”.I’m attempting to find things to enhance
my web site!I suppose its ok to use a few of your ideas!!
скачать казино 1win
https://groups.google.com/g/myfavoritegames/c/xXffnCyTxEM
I’m not sure where you are getting your info, but great topic.
I needs to spend some time learning more or understanding more.
Thanks for great info I was looking for this info for
my mission.
Pretty! This was an incredibly wonderful post.
Thanks for supplying this information.
чемпион казино скачать
чемпион казино скачать
ферст казино
https://groups.google.com/g/myfavoritegames/c/DCL1-kuQPN0
слотокинг бонус за регистрацию
https://groups.google.com/g/myfavoritegames/c/qvEyTp7qVS8
Your mode οf telling tһe ѡhole thіng in tһis article is actսally good,
аll be capable of simply understand іt, Τhanks a lot.
Μy blog casino royale (Larhonda)
http://indianpharmacy.shop/# india online pharmacy
buy medicines online in india
бездепозитный бонус казино украина 2022
бездепозитный бонус казино украина 2022
The foundation of a strong and lasting bond with your dog lies in positive reinforcement training and regular, affectionate interactions.
Socialization with other dogs and people enhances their overall behavior
and sociability. Being attuned to their behavior and addressing any signs of distress promptly contributes to a happy
and healthy life for your four-legged friend. Ultimately,
attentive care, love, and companionship form the pillars of responsible and fulfilling dog ownership.
физ слотс официальный сайт
физ слотс официальный сайт
Your style is really unique in comparison to other people I have read
stuff from. I appreciate you for posting
when you’ve got the opportunity, Guess I’ll just book mark this
page.
слот олимпус
https://groups.google.com/g/myfavoritegames/c/0YVzBfoNVuU
Greetings, I do think your site might be having web browser compatibility problems.
Whenever I look at your blog in Safari, it looks fine however when opening in IE, it’s got some overlapping issues.
I just wanted to provide you with a quick heads up! Besides that, great blog!
Remarkable issues here. I am very glad to look your post.
Thank you so much and I am looking ahead to touch you.
Will you kindly drop me a mail?
бездепозитный бонус казино при регистрации
бездепозитный бонус казино при регистрации
How do I handle dosage changes when transitioning from hospital to home care? – albuterol sulfate
фреш казино 192
фреш казино 192
mexico pharmacies prescription drugs: medicine in mexico pharmacies – mexican pharmaceuticals online
в каком казино можно выиграть
https://groups.google.com/g/myfavoritegames/c/Qbna1ZQwcM8
Hello! I’m at work surfing around your blog from my
new iphone 4! Just wanted to say I love reading your blog and look forward to all
your posts! Keep up the great work!
دستگاه مانیتورینگ EEG کارخانه, با
کیفیت خوب بخرید دستگاه مانیتورینگ EEG محصولات از چین
این می تواند فایل های داده EMG را ذخیره
کند، نظارت بر بیمار جامع تر و ماندگارتر است.
مقدار اندازه گیری شده به طور خودکار با مقدار عادی مقایسه می شود.
2) اگر نمونه آن را دارید ، می توانیم آن را برای شما تولید کنیم.
B) اگر سفارش بزرگ است ، به شما توصیه می کنیم از Air Transport
یا حمل و نقل دریایی استفاده کنید.
به طور کلی مدتی دور بودن از فضای عادی زندگی میتواند کمک بزرگی به ارتقای افکار و بصیرت درونی هر فردی داشته باشد.
احتمالا نام MRI زیاد به گوشتان خورده است MRI مخفف واژه Magnetic resonance imaging است.
این یک روش تلفیقی از امواج رادیویی و مغناطیسی است که نتایج مطمئن
تر و دقیق تری از اشعه X به دست می دهد.
مغز طوری ساخته شده که بلافاصله نسبت به محصولات عجیب و نامرسوم واکنش نشان می
دهد و از این موارد استقبال می کند.
بسیاری از تحقیقات بازار درباره محصولات جدید به همین
دلیل شکست می خورد. دور از دسترس ساختن گزینه ها
پس از انتخاب مشتری باعث
آرامش احساسی می شود و مشتری احساس می کند کار مهمی را
به پایان رسانده است.
Die Struktur des Artikels ist wirklich angenehm.
Ich freue mich darauf, mehr von Ihnen zu lesen. Danke für Ihren informativen Beitrag!
What’s up Dear, are you genuinely visiting this site regularly, if so afterward you will
without doubt take nice experience.
I am extremely inspired along with your writing talents as
neatly as with the structure for your weblog. Is that
this a paid topic or did you customize it your self? Either way
keep up the excellent high quality writing,
it is uncommon to look a nice blog like this one nowadays..
фреш казино бездепозитный бонус
фреш казино бездепозитный бонус
бездепозитные бонусы казино 2022
https://groups.google.com/g/playagainandagain/c/HyPTl1SkbJA
It is perfect to inspect these frameworks on a month-to-month basis or perhaps everyday
if you can swing it.
Good post. I will be facing some of these issues as well..
Every time you make a alter to your site, post a check
out to ensure that the affiliate campaign is nevertheless managing because it must be.
If you already have a website or blog with an active
audience of over 10,000 unique customers daily,
you may try traditional affiliate internet marketing. It has tons of active
gives obtainable appropriate for promoting with Solo Ads
advertising and marketing. As you develop into more skilled and you’ve got a much bigger price
range, you’re going to want to check the bank card submit provides.
Choosing cheaper GEOs offers you a chance to test quite a lot of traffic for
an inexpensive worth. The versatile character from the
web additionally allows entrepreneurs to perform clients past their native market, this
gives you with them the prospect to tremendously improve their earnings.
Strictly Accounting CPA supplies shoppers with accounting and tax preparation providers,
together with your normal ledger wants. CPA Lead is a mobile and
web advertising community engaged on PPC fashions and supplies presents to Android & iOS cellular apps, web sites,
and so forth. To monetize the site visitors, publishers can use the banner, content locking, and
different niche instruments.
I really like your blog.. very nice colors & theme. Did you design this website yourself
or did you hire someone to do it for you? Plz respond as I’m looking
to construct my own blog and would like to know where u got this from.
thank you
Покердом
https://t.me/promokod_PokerDom_casino
фреш казино официальный сайт скачать бесплатно
https://groups.google.com/g/myfavoritegames/c/nvZaA1cRbU0
без депозита бонус казино 2022
https://groups.google.com/g/playagainandagain/c/3GKK8psJ4JI
LED Lampen mit Akku betreiben eröffnet eine Vielzahl von Möglichkeiten für flexible und energieeffiziente Beleuchtungslösungen.
We lately purchased these towels from Nomadix and also we actually like them.
La variedad de perspectivas que presentas en tu blog es fascinante.
Logras abordar temas desde diferentes ángulos,
proporcionando una comprensión más completa. ¡Sigue explorando!
12 Lijas – Reparaciones
Покердом
Покердом
фреш казино рабочее зеркало
https://groups.google.com/g/myfavoritegames/c/eNRRgIXt-uc
автоматы на реальные деньги
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/AbGkE-sAeqU
This design is steller! You obviously know how to keep a
reader amused. Between your wit and your videos, I was almost moved to start my
own blog (well, almost…HaHa!) Excellent job.
I really enjoyed what you had to say, and more than that,
how you presented it. Too cool!
100larn.com เว็บหวยส้มที่มาแรงที่สุด อัตราจ่ายสูงสุด | หวย 12 ราศี บาทละ 1,200 AF12% |
friends казино
friends казино
bonus bez depozita
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/tAHD4mjLicQ
ولات را با استفاده از جنس چرم بدوزند.
این دوره مناسب : فعالان و علاقه مندان حوزه مد و پوشاک ، فعالان حوزه طراحی لباس ،
علاقهمندان به صنایع دستی ، فعالان حوزه کیف و
کفش های چرم و همه هنرمندانی که
قصد دارند با سرمایه کم، کسب و کاری پررونق را شروع کنند، میباشد لذا
با شرکت در این دوره به خوبی با تمام
مباحث چرم دوزی آشنا خواهند شد.
Hey There. I found your blog the use of msn. That is a very neatly written article.
I’ll be sure to bookmark it and come back
to read extra of your helpful information. Thanks for the post.
I’ll definitely return.
I’m amazed, I must say. Rarely do I encounter a blog that’s equally educative and interesting, and let me tell you,
you have hit the nail on the head. The issue is something which too few men and women are
speaking intelligently about. I’m very happy that I stumbled across this in my search for something regarding this.
free pmp practice exam
Conquer the PMP® Exam with Confidence: Dive into a Free Practice Exam Awaits!
Earning your Project Management Professional® (PMP®) certification opens doors to exciting career opportunities.
But conquering the exam can feel daunting.
That’s where a free PMP® practice exam comes in as your ultimate preparation weapon!
Think of it as a dress rehearsal for the real deal. It lets you:
* Assess your knowledge: Identify your strengths and weaknesses across the PMBOK® Guide’s seven domains.
* Gain familiarity with the format: Get comfortable with the question types, length, and pressure of the actual exam.
* Refine your test-taking skills: Learn to manage your time effectively and develop strategies for tackling challenging questions.
* Boost your confidence: Simulating the exam experience calms pre-test jitters and builds your self-belief.
So, where do you find this magical free practice exam? Look no further than your own website!
We offer a comprehensive, high-quality practice exam that mirrors the
real PMP® exam in every way. Here’s what you can expect:
* 180 multiple-choice questions: Covering all areas
of the PMBOK® Guide, ensuring you’re well-rounded for the real test.
* Timed format: Mimicking the actual exam’s 230-minute duration, helping you practice time management.
* Detailed explanations: For every question, gain insights into the correct answer and learn from your mistakes.
* Instant scoring: Get immediate feedback on your performance and identify areas
for improvement.
But wait, there’s more! We also offer a treasure trove of additional free PMP® resources to fuel your preparation:
* Sample questions: Test your understanding of specific PMBOK® concepts.
* Study guides: Deepen your knowledge with concise summaries and key takeaways.
* Blog posts: Get expert tips and insights on various PMP® topics.
* Webinars: Attend live sessions with experienced PMP® professionals.
By combining our free practice exam with these resources,
you’ll be well on your way to PMP® success! But don’t just take our word for
it. Here’s what our satisfied users have to say:
“The free practice exam was invaluable! It helped me identify my weak spots and gave me the confidence I needed to pass the real exam.” – John S., PMP®
“The detailed explanations were a lifesaver. I learned so much from my mistakes and was able to improve my score significantly.” – Sarah L., PMP®
Ready to unlock your PMP® potential? Take our free practice
exam today and embark on your journey to certification success!
Remember, the path to PMP® mastery is paved with preparation, and we’re here to support you every step of the way.
Bonus Tip: Share your practice exam results on social media and challenge your friends to take
it too! Studying together can keep you motivated and make the
learning process more fun.
Let’s conquer the PMP® exam together!
P.S. Don’t forget to explore our comprehensive PMP® preparation courses for an even deeper dive into the world of project management.
With our expert guidance and proven strategies, you’ll be a PMP® rockstar in no
time!
I hope this unique article based on “free PMP® practice exam” provides valuable information and motivates
you to take the next step towards your PMP® certification.
Remember, hard work and dedication, combined with the right resources, will lead you to success!
It is perfect time to make some plans for the future and it’s time to be happy.
I have read this post and if I could I want to suggest you few interesting things or advice.
Maybe you could write next articles referring to this article.
I wish to read more things about it!
Howdy! This is my first visit to your blog! We are
a team of volunteers and starting a new initiative in a community in the same niche.
Your blog provided us beneficial information to work on. You have
done a wonderful job!
Today, I went to the beachfront with my kids. I found a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and screamed.
There was a hermit crab inside and it pinched her ear. She never
wants to go back! LoL I know this is entirely off
topic but I had to tell someone!
изи кеш казино
https://groups.google.com/g/myfavoritegames/c/Bzegt3PYZPQ
If you simply desire something that’s extremely easy to utilize,
I can’t really condemn you.
бонус при регистрации без депозита
бонус при регистрации без депозита
After I originally left a comment I appear to have clicked the -Notify
me when new comments are added- checkbox and from now on whenever a comment is
added I get four emails with the same comment. Is there a means you can remove me from that service?
Thanks!
Have you ever considered about including a little bit more than just your articles?
I mean, what you say is valuable and everything.
However think of if you added some great images or video clips
to give your posts more, “pop”! Your content is excellent but with pics and videos, this blog could definitely be one of the greatest in its field.
Fantastic blog!
вулкан старс казино онлайн
https://groups.google.com/g/myfavoritegames/c/xx5roOA9snQ
AB
Awesome! Its really awesome post, I have got much
clear idea about from this piece of writing.
Mgnificent beat ! I wish too apprentice whiile you amend your website,
hhow could i subscribe forr a blog site? The account aiddd me a accepptable
deal. I hhad been a little biit acquainted of this your broadcast offered bright clear idea
SV
яндекс игровые автоматы играть онлайн бесплатно
https://groups.google.com/g/myfavoritegames/c/s1hJZ3jIM0A
бонусы за регистрацию без депозита
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/4Ri0Q3AWVs4
золотой кубок игровые автоматы
золотой кубок игровые автоматы
What’s up, after reading this awesome post i am also glad
to share my familiarity here with friends.
Heya! I’m att work surfing around your blogg frtom my new iphonne 4!
Just wantesd too sayy I love reading your blog aand look forward to alll your
posts! Carry on the outstanding work!
I am genuinely pleased to glance at this blog posts which consists of tons of helpful data, thanks for providing such statistics.
как использовать бонусы казино 1win
https://groups.google.com/g/myfavoritegames/c/e5janlo2mCA
I go to see everyday a few web pages and websites to read content,
but this webpage provides quality based posts.
AH
ZQ
Cada entrada en tu blog es como un regalo intelectual.
La forma en que abordas los temas demuestra tu dedicación y amor por compartir conocimientos.
¡Gracias por regalarnos eso! WX801 – %random_anchor_text%
1win казино скачать
1win казино скачать
That is very attention-grabbing, You are a very professional blogger.
I have joined your rss feed and sit up for looking for more of your fantastic post.
Additionally, I’ve shared your website in my social networks
Ce forfait coûte 19,99€ par mois mais si vous êtes abonné Freebox, il ne vous coûte plus que 15,99€ et
l’enveloppe data est illimitée.
Hi all, here every one is sharing these kinds of know-how, thus it’s pleasant to read this website,
and I used to pay a quick visit this blog everyday.
It’s great that you are getting thoughts from this post as well as from our discussion made at
this time.
Wow, wonderful weblog structure! How long have you been blogging
for? you make blogging glance easy. The whole glance of your web site
is magnificent, as neatly as the content material!
как поймать бонус в игровых автоматах
как поймать бонус в игровых автоматах
Hey there great website! Does running a blog such as this take
a large amount of work? I’ve no expertise in computer programming however
I was hoping to start my own blog soon. Anyhow, if you have any ideas or
techniques for new blog owners please share. I know this is off topic however I just had to ask.
Cheers!
wonderful issues altogether, you simply gained a new reader.
What could you suggest about your post that you just
made a few days in the past? Any certain?
wonderful points altogether, you just won a logo new reader.
What may you suggest in regards to your put up that you made some days in the past?
Any sure?
казино буй регистрация
https://groups.google.com/g/myfavoritegames/c/_I8bYTa9D1Q
کارخانه تولید کنندگان تامین کنندگان EMG
ارزان قیمت FOREVER MEDICAL
بسته به نیاز بیمار ، این ممکن است شامل تجزیه و
تحلیل فعالیت عضلات ، حرکت مفصل ، نیروهای مفصلی ، فشار پا یا مصرف انرژی باشد.
اختلال عملکرد عضلانی یک منبع آسیب
شناسی رایج ، اما اغلب بدون مشکوک
است. آزمایشگاه پاتوکینزیولوژی در استفاده انحصاری
از الکترومیوگرافی سیم ظریف دینامیکی (EMG)
برای ثبت عملکرد عضلات بیمار
بی نظیر است.
I’m not that much of a internet reader to be honest but your blogs really nice, keep
it up! I’ll go ahead and bookmark your site to come back down the
road. All the best
I don’t even understand how I ended up right here, however I believed this put up was great.
I don’t recognise who you are however certainly you’re going to a well-known blogger should
you are not already. Cheers!
где дают бонус за регистрацию
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/UKptJ5-hpOQ
This is a topic which is near to my heart… Thank you!
Exactly where are your contact details though?
It’s remarkable to pay a visit this web site and reading
the views of all friends on the topic of this post, while I am also eager of getting
experience.
Thanks in support of sharing such a pleasant opinion, paragraph is pleasant,
thats why i have read it fully
When does the pain and swelling stop after knowledge tooth elimination?
казино чемпион онлайн
казино чемпион онлайн
Having a dishwasher will certainly profit your foodservice
operation long run by always guaranteeing dishes, glasses and kitchenware is washed properly
each time. A lock of fresh kitchenware can have a huge effect on what you are promoting
and prospects take word of these selections, most significantly hygiene and
cleanliness. This can assist you’ve a much easy start.
The fabric itself is made in such a manner that it will accent your home windows; it is going to drape nicely and be the appropriate
thickness to fall because it should. The quite a few colors of stain out there ensure that
you’ll discover the correct coloration for your property.
The cork will come out smoothly. I only go away out cookies and milk.
The cork will come out. Utilizing a spreadsheet may also help set up your data, and a few financial software will assist those with extra
complicated situations. Press each the blades alternately using the handle.
This system is right for these individuals who chorus from utilizing extreme strength or power to perfectly open a wine bottle.
Oh my goodness! Incredible article dude! Thanks, However I am having
difficulties with your RSS. I don’t know the reason why I am unable
to subscribe to it. Is there anybody else getting similar RSS problems?
Anyone that knows the solution can you kindly respond?
Thanks!!
Hello, i think that i saw you visited my site thus i came to “return the favor”.I
am trying to find things to enhance my site!I suppose its
ok to use a few of your ideas!!
Hello my loved one! I want to say that this post is awesome, nice written and include approximately all important
infos. I would like to look more posts like this .
Greate post. Keep writing such kind of information on your
site. Im really impressed by your site.
Hey there, You’ve performed a great job.
I’ll definitely digg it and for my part suggest to my friends.
I’m sure they’ll be benefited from this website.
где дают деньги за регистрацию
где дают деньги за регистрацию
I am really loving the theme/design of your weblog. Do you ever run into any web browser compatibility issues?
A handful of my blog readers have complained about my website not working correctly in Explorer but looks great in Firefox.
Do you have any suggestions to help fix this issue?
Thanks for finally talking about > Think Obstructive Sleep Apnea is #NBD?
Here Are Seven Health Conditions Made Worse By Your Undiagnosed
OSA – Delaware Dental Sleep Medicine < Liked it!
You actually make it seem really easy along with your presentation however I to find this matter to be
really one thing which I feel I would never understand.
It sort of feels too complicated and very broad for me. I’m taking a look ahead in your subsequent publish,
I’ll attempt to get the cling of it!
I relish, lead to I discovered just what I was looking for.
You have ended my four day lengthy hunt! God Bless you man. Have a
great day. Bye
Hello, I enjoy reading through your article. I like to write a little comment to support
you.
казино f1
казино f1
Valuable info. Lucky me I found your web site
unintentionally, and I am surprised why this coincidence did not took place
earlier! I bookmarked it.
игры казино онлайн
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/mjcAfulfGZ4
казино grand casino
https://groups.google.com/g/myfavoritegames/c/R_az-SQGHgo
Incredible quest there. What occurred after? Take care!
Hello Dear, are you genuinely visiting this web site on a regular basis,
if so afterward you will definitely get fastidious know-how.
Aw, this was an extremely good post. Taking the time and actual effort to generate a really good article… but what can I say… I put things off a lot and don’t
manage to get nearly anything done.
игры в казино онлайн
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/-7L-m0UOiHA
казино х бонус
https://groups.google.com/g/myfavoritegames/c/Vce-y-27WfE
бетбум казино
бетбум казино
Its such as you read my thoughts! You seem to know
a lot about this, like you wrote the book in it or something.
I feel that you simply can do with a few p.c. to pressure the message house
a bit, however other than that, that is wonderful blog.
A great read. I’ll certainly be back.
Also visit my homepage – HCG Injections Shop
Definitely believe that which you stated. Your favorite
reason appeared to be on the internet the simplest thing to be aware of.
I say to you, I certainly get irked while people think about
worries that they just do not know about. You managed to hit
the nail upon the top and defined out the whole thing without
having side-effects , people could take a signal. Will probably be back to get more.
Thanks
Hello There. I found your blog using msn. This is an extremely well written article.
I will be sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I’ll certainly return.
как играть в онлайн казино на деньги
как играть в онлайн казино на деньги
казино play fortuna
казино play fortuna
What’s Going down i’m new to this, I stumbled upon this
I’ve found It absolutely helpful and it has helped me out loads.
I’m hoping to give a contribution & aid different users like its
aided me. Great job.
бездепозитный бонус казино украина
бездепозитный бонус казино украина
Way cool! Some extremely valid points! I appreciate you penning this write-up
and the rest of the website is very good.
казино бонус за регистрацию с выводом
казино бонус за регистрацию с выводом
казино с бездепозитным бонусом 2022
https://groups.google.com/g/myfavoritegames/c/kSZFabvdgFQ
биткоин казино
https://groups.google.com/g/myfavoritegames/c/V62-NsoknNc
легальные казино в россии онлайн
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/qORyw5PIjhI
казино вулкан бонус за регистрацию
казино вулкан бонус за регистрацию
The Buffalo Bills misplaced back to again Super Bowls to the Dallas Cowboys in the ultimate two years that they made the championship game.
The three images from capturing to get on the scene to determine the exact lighting results – you
often need to use B gate to get such a protracted exposure, in accordance with the three take a look at results to find out
the ultimate shot utilizing exposure occasions. He completed in the top 10 in one hundred tournaments and earned the Vardon Trophy for lowest average rating three times.
Palazzo Medici-Riccardi Home windows: Michelangelo’s window design for
this palace is one of the crucial influential of all instances.
Farnese Palace Courtyard: Originally a work by Antonio da Sangallo, Michelangelo was brought in to complete this
building, when da Sangallo died. This quote by Michelangelo describes his perspective toward
artwork extraordinarily well. Smoky quartz earrings could be the proper alternative for you
in case you are in search of something that is absolutely magnificent to have a look at as well as really easy to purchase.
To garner that spotlight, though, Sanders needed to not solely play
properly but additionally live a life of glamour, flashy clothes and all, when he wasn’t taking part in.
After I originally commented I seem to have clicked the -Notify me when new comments are added- checkbox and from now on whenever a comment is
added I recieve 4 emails with the same comment.
Is there a means you are able to remove me from that service?
Cheers!
бонус казино 1win
бонус казино 1win
Slot MPO11 merupakan salah satu permainan mesin slot online yang populer
ⅾann menarik. Untuk memaksimalkan pengalaman bermain Anda dan meningkatkan peluang meraih
jackpot, berikut adlah panduan cara bermain slot MPO11 dengan strategi terbaik.
легальные онлайн казино
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/aCGRB5Yn1X0
казино вулкан победа
https://groups.google.com/g/myfavoritegames/c/Ft6CLCgflhE
Simply want to say your article is ɑs amazing. The clarity in yߋur post is simply excellent and
i can assume уoᥙ’re ɑn expert on this subject. Well witһ your permission ⅼet me tо grab
yⲟur RSS feed to keер updated witһ forthcoming post. Thаnks a
mіllion ɑnd pleаse carry օn the enjoyable work.
Feel free to visit mү homepage :: lottery
Do you have a spam problem on this website; I also am a blogger, and I was wondering your
situation; many of us have developed some nice methods and we are looking to trade methods
with others, please shoot me an e-mail if interested.
Hello, i feel that i noticed you visited my website thus i got here to return the favor?.I’m
attempting to in finding things to enhance my website!I guess its
ok to make use of some of your ideas!!
Have you ever thought about adding a little bit more than just
your articles? I mean, what you say is fundamental and all.
Nevertheless imagine if you added some great photos or videos to give your posts more, “pop”!
Your content is excellent but with pics and videos, this
site could definitely be one of the very best in its niche.
Very good blog!
For instance, train gear, anti-virus software, and health
complement gross sales tend to be much larger firstly of the yr when consumers
are traditionally beginning to make improvements
to their lives. Experts concerned in counterterrorism have observed “a development in this global Sunni extremist motion, partly pushed by Iraq, but in addition by different occasions, which is far harder to trace, observe and ultimately disrupt. In that e-mail, al-Zawahiri complains that the Yemeni chief is spending a lot cash and is not correctly reporting his bills. Some of these embody application processing, credential evaluations and rating reporting. Now, it’s time to examine the provide itself and determine whether or not it’s an excellent match for your publishing platform, traffic sources, and different belongings. You need to take the time to forge a good relationship along with your current offer sources to ensure that you’re getting a boost from serving to them grow. If you’re taking the time to speak together with your network or advertiser to show your curiosity, you could also be rewarded with exclusive offers.
бонусы казино pin up
бонусы казино pin up
легальные онлайн казино в россии
легальные онлайн казино в россии
налог на выигрыш в казино
налог на выигрыш в казино
Fabulous, what a website it is! This weblog provides helpful
data to us, keep it up.
Thankfulness to my father who told me concerning this website, this website is genuinely remarkable.
бонусы пин ап казино
бонусы пин ап казино
I have read so many articles concerning the blogger lovers however this post is actually a pleasant
post, keep it up.
I’m not that much of a internet reader to be honest but your blogs really nice, keep it
up! I’ll go ahead and bookmark your site to come back
in the future. Cheers
лидеры онлайн казино
лидеры онлайн казино
Hi! This is kind of off topic but I need some advice from an established blog.
Is it very difficult to set up your own blog? I’m
not very techincal but I can figure things out pretty
quick. I’m thinking about creating my own but I’m not sure where to
start. Do you have any tips or suggestions?
Many thanks
пинап обзор и слоты пин ап промокод пин ап
https://groups.google.com/g/myfavoritegames/c/Dwi0Dhc839I
Hi there, its good article on the topic of media print, we
all be aware of media is a enormous source of information.
чемпион автоматы
чемпион автоматы
Thank you for the auspicious writeup. It actually was a
enjoyment account it. Look complex to more delivered agreeable from
you! However, how can we be in contact?
Pylori, dehydration, infections, and use of specific medications.
I believe what you published made a lot of sense. However, what about this?
suppose you added a little information? I am not suggesting your content is not good, but what if you
added a headline to maybe grab folk’s attention? I mean Think Obstructive Sleep Apnea is #NBD?
Here Are Seven Health Conditions Made Worse By Your Undiagnosed OSA – Delaware
Dental Sleep Medicine is kinda boring. You ought to glance at Yahoo’s home page and see
how they create news headlines to grab people to click. You might add a related video or a pic or two to
grab people interested about what you’ve written. In my
opinion, it could make your posts a little bit more interesting.
Download porn
play fortuna казино онлайн
play fortuna казино онлайн
лучшее онлайн казино по отзывам
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/Gu44SqpFCek
No matter if some one searches for his necessary thing, so he/she
desires to be available that in detail, so that thing is maintained over here.
La empatía que muestras hacia tus lectores
en tu blog no pasa desapercibida. Creas un espacio acogedor que invita a la participación y al aprendizaje conjunto.
¡Sigue siendo tan amable! Calentador de Agua Eléctrico 30 Litros –
PANTER & 8211; Calzado Seguridad Linea Zion Modelo Super forja s3
egt слоты бесплатно
https://groups.google.com/g/myfavoritegames/c/RwqEgER1ALg
Our Multi-Purpose products are made for, well, any purpose.
промокод казино пин ап
https://groups.google.com/g/myfavoritegames/c/Q3Tp3BtaYRg
лучшие мобильные казино
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/eZlW6H3CXdM
egt слоты демо
egt слоты демо
Yоu’ге soo inteгesting! I doo noot supose I hav red tbrough ѕomething likke thwt Ьefore.
So greeat tto fond sombody ᴡith a ffew genjine thoghts
onn thnis subject. Ɍeally.. tthank yoou ffor stzrting tһis up.
Thiss weeb sjte iis someething that’s neeeded onn thee internet,
ѕomeone withh a litfle originality!
Heere iss myy websitge 1 (ahpub.ir)
I would say I’m pretty good. I might say that 5 is possible,
but that is likely to be overly optimistic.
I would say more arrogant. The Poor Woman was still
feeling very unhealthy, she was shivering as a consequence of fever, this Mumbaikar Lady observed her deteriorating health condition and
gave her scarf, in order that the Poor Woman can wrap her head and will really feel better, however her condition received worse, her coronary heart palpitation went up and she was shivering,
this Mumbaikar Lady in an ordering voice asked other two neighboring ladies to get up from their seats in order that this Poor Girl can get some more room to lie down on the seat.
Feeling issues is human. I remember feeling really down on myself.
Up coming all of us seated straight down for an hour
or so and likewise saved just a few of all of them.
It is approach higher than it was just a few years ago.
Word few Frequent Phrases of the Local Language the place you’re going to
journey, sometimes its help while nobody around you to understand your
language.
Hello there, You have done a fantastic job.
I’ll certainly digg it and personally suggest to my friends.
I’m confident they will be benefited from this website.
I like what you guys are usually up too. Such clever work and
coverage! Keep up the wonderful works guys I’ve you guys to my own blogroll.
слотор бонус
https://groups.google.com/g/myfavoritegames/c/PrIGU44fNc4
мобильное казино
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/hEyWsqy4b2o
Good article! We will be linking to this great post on our site.
Keep up the great writing.
физ слотс
физ слотс
I have to thank you for the efforts you have put in penning this blog.
I’m hoping to view the same high-grade content from you in the
future as well. In fact, your creative writing abilities
has inspired me to get my own site now 😉
I am really enjoying the theme/design of your site. Do you ever run into
any internet browser compatibility issues?
A handful of my blog visitors have complained about my blog not operating correctly in Explorer but looks great in Firefox.
Do you have any advice to help fix this issue?
спорт слот
спорт слот
мобильное онлайн казино
мобильное онлайн казино
The earliest oral filling, constructed from beeswax, was discovered
in Slovenia and dates from 6500 years earlier.
фреш казино официальный сайт зеркало на сегодня
фреш казино официальный сайт зеркало на сегодня
La actualización constante de tu blog demuestra tu compromiso con mantener
la frescura del contenido. ¡Siempre hay algo nuevo
y emocionante que esperar! Velocidad Variable Grabado Pluma para Metal Madera Joyería Vidrio Cerámica para Pulido Grabado Rectificado Lijado – Frutas
A keto version of this glorious Indian dish made with hen and cooked in a wealthy onion gravy with an arsenal
of spices. This keto pizza sauce recipe is easy to make and tastes amazing.
стэйк казино
https://groups.google.com/g/myfavoritegames/c/tHJixue9w8M
Rental kendaraan beroda empat terbaik adalah opsi tepat bagi mereka yang mengharapkan pengalaman berkendara
yang nyaman, aman, dan efisien tanpa harus memiliki kendaraan sendiri.
Layanan ini menawarkan flotil kendaraan beroda empat yang berbagai, mulai dari model terupdate hingga
kendaraan premium, memenuhi keperluan beraneka tipe pelanggan.
Dengan fokus pada kenyamanan dan keamanan, perusahaan rental kendaraan beroda empat terbaik menyediakan armada yang terawat dengan bagus dan selalu menjalani pemeliharaan terprogram .
Kerja-kendaraan ini dilengkapi dengan fitur keselamatan terbaru, seperti cara pengereman canggih, airbag, dan perangkat keselamatan lainnya, memberikan kepercayaan terhadap pelanggan bahwa mereka dalam perjalanan yang
aman.
новые казино 2022
новые казино 2022
игровой автомат gold diggers
игровой автомат gold diggers
Hi everyone, it’s my first pay a visit at this site, and article is actually fruitful for me, keep up
posting these types of posts.
Great goods from you, man. I have understand your stuff previous to and you are just
too excellent. I actually like what you’ve acquired here, really like what you are stating and the way in which you say
it. You make it entertaining and you still take care of to keep
it smart. I cant wait to read much more from you. This is really a terrific site.
топ слоты
https://groups.google.com/g/myfavoritegames/c/MzPNC7mxMiM
обзоры лучших казино
обзоры лучших казино
как играть на бонусы казино в 1win
как играть на бонусы казино в 1win
vavada казино 100 фриспинов
https://groups.google.com/g/myfavoritegames/c/wuaV-ULg16M
This is a topic which is near to my heart… Best wishes!
Where are your contact details though?
онлайн casino
онлайн casino
как открыть казино в россии
как открыть казино в россии
Why users still use to read news papers when in this technological
globe the whole thing is presented on web?
Greetings! I’ve been following your site for a long time now and finally got the courage to go ahead and give you a shout out from
Humble Texas! Just wanted to say keep up the good work!
vostok казино
https://groups.google.com/g/myfavoritegames/c/8WILC3sVIns
онлайн игры на деньги
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/yNLuJkir4Bw
казино чемпион бонусы
https://groups.google.com/g/myfavoritegames/c/MM3WvIEKudU
спинбеттер казино
https://groups.google.com/g/yourgamesonline/c/Ldi77Rnfpw0
Nevertheless, there are fishes which are backside dweller, too.
You have to be already conscious of the fact that, fishes are usually fed by
the highest surface of the aquarium. The wattage ranking of
your inverter should exceed the entire wattage
of all the units you plan to run concurrently. Blu-Tac isn’t used
in dwelling it is used only wherever we’d like and we will earn money over this homemade bread and type Blu-Tac.
Importance of hygiene: While youngsters are careless by nature, but they
should be taught the significance of hygiene and the way it will probably have an effect on their health.
Nonetheless, you want to recollect you might be likely to spend supply
for each organization separately. Due to this fact, seek data
very first to see if you may be able to find all or at best nearly
all of the things you will need at a single firm so you may cut down on transport and supply expenses.
An elevated diploma of pet care recommendation and even providing free supply with
regard to wholesale pet supplies is actually two examples.
One in every of several advantages of shopping on the net relating to wholesale pet supplies will probably be that you possibly can locate most jobs you want
to. Shade tends to encompass other designations like sustainability and fowl-friendliness, and it speaks
to probably the most basic nature of the best way coffee is cultivated.
онлайн казино бездепозитный бонус
онлайн казино бездепозитный бонус
казино чемпион регистрация
https://groups.google.com/g/myfavoritegames/c/P_A3QA6SXAw
Hello there! I know this is kinda off topic but I was wondering if you
knew where I could locate a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having
trouble finding one? Thanks a lot!
онлайн казино игры
онлайн казино игры
казино фараон играть
https://groups.google.com/g/myfavoritegames/c/0cWoGpVsUdA
It’s remarkable to visit this site and reading the views of all colleagues regarding this post,
while I am also eager of getting knowledge.
Woah! I’m really loving the template/theme of this blog.
It’s simple, yet effective. A lot of times
it’s very hard to get that “perfect balance” between superb usability
and visual appeal. I must say you have done a amazing job with this.
Additionally, the blog loads very fast for me on Safari.
Superb Blog!
игры автоматы слот
игры автоматы слот
онлайн казино на реальные деньги отзывы
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/BW6D7VeFAuo
казино gold
https://groups.google.com/g/myfavoritegames/c/0LO8Q_ANz1E
The other day, while I was at work, my sister stole my iphone and tested to see if it can survive
a 25 foot drop, just so she can be a youtube sensation.
My iPad is now broken and she has 83 views. I know this
is totally off topic but I had to share it with someone!
You are able to try Paris city and luxuriate in a marvelous venture to that enchanting
location. Printed in 1979, “Masquerade” is an intricately wrought youngsters’s fable
that contains clues to a hunt for a location in the true world, during which was
hidden a wonderful, handmade golden rabbit. Transferring from north to south,
a bride from a Malayali family exudes beauty by sparkling treasured yellow gold jewellery.
Draped in the normal white Kasavu saree with
golden self woven threads into it, the bridal trousseau of south
Indian bride embody dozens of gold necklaces,
earrings, saree belt, bracelets and bangles which might be
a logo of prosperity and development of the family.
The trousseau of a Punjabi bride consists of a large variety of
Indian bridal dresses ranging from salwar kameez, sarees, and lehengas.
Amidst the drum beats and festive galore, a Punjabi
bride is decked up in richly embellished lehenga choli or a gorgeous salwar kameez.
As these could cause a lot devastation, it would
be better for males to create helpful use of the wonders of science.
Many people don’t perceive that science was actually designed in Religious
European countries by men who presumed that God designed an organized galaxy.
физзслотс казино
физзслотс казино
jozz казино официальный сайт
https://groups.google.com/g/gameyourgame/c/DVmQH4lyeNQ
казино марвел
https://groups.google.com/g/myfavoritegames/c/Xyc4FwN2yLk
подарок без депозита
подарок без депозита
I want to to thank you for this good read!! I definitely loved
every little bit of it. I have got you bookmarked to check out new stuff you post…
казино без депозита с выводом денег 2022
https://groups.google.com/g/gameyourgame/c/JRnNVtGOTfw
Helpful information. Lucky me I discovered your web site by chance, and
I am shocked why this accident didn’t took place in advance!
I bookmarked it.
spinbetter казино
https://groups.google.com/g/yourgamesonline/c/gTZlmTj-Iho
Thanks very interesting blog!
получить бонус без депозита
получить бонус без депозита
казино гама
казино гама
Today, I went to the beach with my kids. I found a
sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She
placed the shell to her ear and screamed. There was a hermit crab
inside and it pinched her ear. She never wants to go back!
LoL I know this is totally off topic but I had to tell someone!
Hello There. I found your weblog the use of msn. This is a really smartly written article.
I will be sure to bookmark it and return to learn extra of your helpful information. Thank you for
the post. I’ll certainly comeback.
hi!,I like your writing so much! share we be
in contact extra approximately your post on AOL? I need a specialist in this space to resolve my problem.
May be that is you! Having a look ahead to look you.
рейтинг онлайн казино 2022
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/antqIljo9c4
You’re ѕo awesome! I ɗo not suppose Ι’vе read tһrough
anything like tһiѕ beforе. So great to discover someone wіth
а few unique thoսghts on tһis topic. Ⴝeriously..
mаny thanks for starting thіѕ uр. This website is ѕomething that
is neeⅾeɗ on tһe web, ѕomeone ᴡith a lіttle originality!
Loοk at my web site: lottery
казино х рабочее зеркало на сегодня
https://groups.google.com/g/gameyourgame/c/KEQfSIaoHCM
казино слот в
казино слот в
Some focus on aesthetic dentistry while others specialize in orthodontics
or pediatric dental care.
What a stuff of un-ambiguity and preserveness of precious familiarity on the topic of unexpected feelings.
рейтинг российских казино
рейтинг российских казино
новые бонусы казино
новые бонусы казино
казино леон официальный сайт
казино леон официальный сайт
автоматы с бездепозитным бонусом
автоматы с бездепозитным бонусом
Hi there, I check your blogs like every week. Your writing style is awesome, keep it up!
certainly like your website however you have to check the spelling on several of your posts.
Many of them are rife with spelling issues and I in finding it very
bothersome to inform the reality however I’ll
definitely come back again.
новые казино с бездепозитным бонусом за регистрацию
новые казино с бездепозитным бонусом за регистрацию
казино рф
казино рф
Also, you cannot disclaim simply a part of a benefit
or use any of it before disclaiming — even simply placing the verify in your personal account can mean the distinction between a professional disclaimer and
a meaningless document.
Thanks for sharing your thoughts. I really aρpreciate your efforts and
I ᴡill be waiting foг ʏ᧐ur further wгite upѕ tһanks
oncе agɑin.
Feel free to surf to my blog; lotto
It isn’t just an enjoyable occasion for the graduates but additionally joyful for the whole family who dream to look them
in lovely graduation dress. Movies usually current goals as a
visually accessible or objectively noticed space, a discrete environment wherein characters exist and interact as they do on the planet quite
than proscribing themselves to the subjective point of view a dream is generally skilled from
in real life. This narrative is not static however dynamic,
allowing the house to adapt and morph, reflecting the
altering landscapes of the person’s ideas, feelings, and life circumstances, thereby maintaining a dwelling,
breathing connection between the individual and their area.
To make every look seem simple and gorgeous, a diamond or a pearl stud is the solution. He simply tried
to write down the sonnets not solely on love but additionally on other subjects as that the readers must be adopted to know the issues comprehensively and find the solution. Girls of all ages may
actually love this exceptional watch from its band strap made from first-rate
earthenware to the pink mom of pear dial. They are scrupulous about consuming plenty of recent greens and fruits and should develop
into vegans in center age.
бесплатные бонусы без депозита
бесплатные бонусы без депозита
новые онлайн казино с бездепозитным бонусом
https://groups.google.com/g/againplay/c/mv9N985X4po
казино с денежным бонусом
https://groups.google.com/g/gameyourgame/c/xuPZ3M2MuQE
bezdep casino
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/Sp97trEUUcw
обзор игровых автоматов
обзор игровых автоматов
казино с лицензией
https://groups.google.com/g/gameyourgame/c/p9PQvOV1M0M
Appreciate the recommendation. Let me try it out.
I get pleasure from, lead to I found exactly what I used to be having a look for.
You’ve ended my four day lengthy hunt! God Bless you man.
Have a nice day. Bye
бездепозитные бонусы казино за регистрацию
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/5DZ5E_l4XJ4
онлайн игры на деньги с выводом на карту
https://groups.google.com/g/againplay/c/HXR6MjTGspI
gojekpot merupakan situs gojekpot hari ini dengan bermain gojekpot mudah maxwin karena keunggulan fiture pola rtp gojekpot
terbaru cukup addition 10ribu sudah bisa menang x500 yang bisa
di go without dengan pilihan game slot terbaru.
казино слот v
казино слот v
Simply want to say your article is as amazing. The clearness in your post is just excellent and i can assume you’re an expert on this subject.
Well with your permission let me to grab your RSS feed to keep
updated with forthcoming post. Thanks a million and please keep up the gratifying work.
рейтинг онлайн казино с лицензией
https://groups.google.com/g/againplay/c/PQwnAJYtcKE
бездеп в казино
бездеп в казино
I am sure this piece of writing has touched all the internet users, its really really pleasant piece of writing on building up new blog.
казино с отыгрышем бездепозитный бонус
казино с отыгрышем бездепозитный бонус
I just like the valuable info you provide on your articles.
I’ll bookmark your blog and test once more right here frequently.
I’m slightly sure I’ll be informed lots of new stuff proper here!
Good luck for the following!
русские игровые автоматы
русские игровые автоматы
бонус при регистрации в казино без депозита
бонус при регистрации в казино без депозита
казино ігри
казино ігри
русские казино
https://groups.google.com/g/againplay/c/B8EvxTvRMnA
бонус за регистрацию в казино
бонус за регистрацию в казино
лицензионное казино
https://groups.google.com/g/gameyourgame/c/RzYzZQW0RS4
скачать онлайн казино
скачать онлайн казино
игра игровые автоматы
https://groups.google.com/g/againplay/c/YqjUMj3mqS8
It’s in fact very complex in this full of activity life to listen news
on Television, therefore I only use the web for that purpose, and take
the newest news.
лицензионное казино украина
лицензионное казино украина
слоты на реальные деньги с выводом
https://groups.google.com/g/againplay/c/Yg_VUJLxvFU
fuck google
игровые аппараты казино
игровые аппараты казино
You ought to be a part of a contest for one of the best websites on the net.
I most certainly will recommend this site!
лицензионное онлайн казино
https://groups.google.com/g/gameyourgame/c/jGpPusBd-sc
список честных казино
https://groups.google.com/g/againplay/c/9N1d8W6HOw8
Hello, I believe your website might be having internet browser
compatibility problems. Whenever I take a look at
your site in Safari, it looks fine but when opening in IE, it has some overlapping issues.
I just wanted to provide you with a quick heads up!
Apart from that, fantastic website!
игровые автоматы где дают деньги за регистрацию
игровые автоматы где дают деньги за регистрацию
лучшие слоты в казино
лучшие слоты в казино
I every time used to study piece of writing
in news papers but now as I am a user of web therefore from now I am
using net for content, thanks to web.
список казино на рубли
https://groups.google.com/g/againplay/c/WzZlz0vkuYA
I have read so many posts on the topic of
the blogger lovers however this post is really a pleasant article, keep it up.
игровые автоматы игры
игровые автоматы игры
мелбет скачать бесплатно казино
https://groups.google.com/g/gameyourgame/c/tQycT6RP9jU
To order affordable customized thesis writing services from us,
contact our customer help heart. Place and order at present and
benefit from the customized assgnment assist
services in the UK.
казино vulkanstars
казино vulkanstars
азартные игры на деньги онлайн с выводом
https://groups.google.com/g/againplay/c/CIDjqSy72Dg
Amazing issyes here. I’m very gllad to loiok your article.
Thankis a lot and I am having a lopk ahead tto contacht you.
Wiill you pleaase dop me a e-mail?
игровые автоматы с бонусом без депозита
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/3zZklD7q3v4
мелбет скачать казино
мелбет скачать казино
азартные игры с выводом денег
https://groups.google.com/g/againplay/c/B_u8deLl8eY
I was suggested this blog by means of my cousin. I am no longer certain whether this publish is written via him as nobody else
understand such targeted about my trouble. You are amazing!
Thank you!
Pretty nice post. I just stumbled upon your weblog and wished to say that I have
truly enjoyed browsing your blog posts. In any case I’ll
be subscribing to your rss feed and I hope you write
again very soon!
Examine whether you really feel comfortable with your dental professional and their staff.
игры игровые автоматы
игры игровые автоматы
мелбет скачать приложение слоты
https://groups.google.com/g/gameyourgame/c/fEw6sATLo58
Does your blog have a contact page? I’m having problems locating it but, I’d like to shoot you an email.
I’ve got some creative ideas for your blog you might be interested in hearing.
Either way, great blog and I look forward to seeing it expand over time.
бонусы без депозита
бонусы без депозита
онлайн казино украина на гривны бездепозитный бонус
https://groups.google.com/g/myfavoritegames/c/fIVXOO27D6c
казино без депозита бонус за регистрацию
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/v_POZ7Mpox4
мобильное казино игры
https://groups.google.com/g/gameyourgame/c/Nkq7fzG8vvA
бонусы без депозита казино
бонусы без депозита казино
I’ve been exploring for a little for any high quality articles or blog posts
in this kind of house . Exploring in Yahoo I eventually stumbled
upon this web site. Reading this information So i am glad to convey that I have an incredibly just
right uncanny feeling I found out just what I needed.
I such a lot undoubtedly will make certain to don?t forget this web site and provides it
a glance on a relentless basis.
Pretty! Thіs was an incredibly wonderful article. Μany tһanks for providing
this info.
Look into my webpage – betting (Georgiana)
рабочее зеркало казино x
https://groups.google.com/g/myfavoritegames/c/sGsEA4ZJeUo
казино без депозита с выводом
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/JgU2BBenJNs
мостбет слоты
мостбет слоты
Wonderful beat ! I would like to apprentice at the same time as you amend your website, how can i subscribe for a weblog site?
The account aided me a appropriate deal. I were tiny bit acquainted of this your broadcast provided bright clear
concept
бонусы казино без депозита
https://groups.google.com/g/againplay/c/40TpqL8cOpU
самые дающие слоты
https://groups.google.com/g/myfavoritegames/c/mV2_TwSQ0W8
новое казино с бездепозитным бонусом
https://groups.google.com/g/gameyourgame/c/7JNfMaVky2w
казино онлайн бездепозитный бонус
казино онлайн бездепозитный бонус
бонусы при регистрации в казино
https://groups.google.com/g/againplay/c/CViYZIk8qtc
скачать pin up казино на айфон
https://groups.google.com/g/myfavoritegames/c/abiQBdMBhnQ
Hey! Would you mind if I share your blog with my twitter group?
There’s a lot of folks that I think would really enjoy your content.
Please let me know. Cheers
онлайн казино лицензионные
онлайн казино лицензионные
казино с бездепом за регистрацию
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/kMeR99O4Ru4
First of all I would like to say wonderful blog! I had a quick question that
I’d like to ask if you don’t mind. I was interested to find out how you center yourself and clear your mind before writing.
I’ve had a difficult time clearing my thoughts in getting my ideas out.
I truly do take pleasure in writing however it just seems like the
first 10 to 15 minutes are generally wasted just trying to figure out how to begin. Any suggestions or hints?
Many thanks!
阴茎
бонусы за депозит
бонусы за депозит
Hello there! Do you use Twitter? I’d like to follow you if that would be ok.
I’m definitely enjoying your blog and look forward to new posts.
Situs Daring Duogaming Judi Online
Because the admin of this site is working, no uncertainty very rapidly it will
be well-known, due to its quality contents.
слотокінг
https://groups.google.com/g/myfavoritegames/c/kAS9Y19NmCQ
казино с бездепозитным бонусом за регистрацию с выводом без пополнения
казино с бездепозитным бонусом за регистрацию с выводом без пополнения
Hey there! This post could not be written any better!
Reading this post reminds me of my previous room mate!
He always kept talking about this. I will forward this write-up to
him. Fairly certain he will have a good read. Thank you for sharing!
бонус за депозит
бонус за депозит
топ слоты в казино
топ слоты в казино
онлайн казино бездепозитный бонус за регистрацию
онлайн казино бездепозитный бонус за регистрацию
честное казино с моментальными выплатами
https://groups.google.com/g/againplay/c/ZLmjvCQV4VU
turbo казино
turbo казино
онлайн казино с бонусами за регистрацию
онлайн казино с бонусами за регистрацию
endorphina слоты
endorphina слоты
золотой кубок казино
https://groups.google.com/g/myfavoritegames/c/VqNmb9I3OAY
This design is incredible! You obviously know
how to keep a reader amused. Between your wit and your videos, I was
almost moved to start my own blog (well, almost…HaHa!) Excellent job.
I really enjoyed what you had to say, and more than that, how you presented
it. Too cool!
онлайн казино украина на гривны
https://groups.google.com/g/gameyourgame/c/txa0UMyUS5Q
My programmer is trying to persuade me to move to
.net from PHP. I have always disliked the idea because of the expenses.
But he’s tryiong none the less. I’ve been using WordPress
on a variety of websites for about a year and am worried about
switching to another platform. I have heard good things about blogengine.net.
Is there a way I can import all my wordpress content into it?
Any help would be really appreciated!
Just desire to say your article is as astonishing. The clarity in your post is simply cool and
i could assume you are an expert on this subject.
Fine with your permission let me to grab your feed to keep updated with forthcoming post.
Thanks a million and please keep up the enjoyable work.
поиграть в игровые автоматы
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/HTHazL2WlGs
фонбет казино
фонбет казино
ігри казино
ігри казино
париматч казино украина
https://groups.google.com/g/gameyourgame/c/Admhbytccak
YYY Casino is an online casino that caters to players from
Northern Africa and the Middle East. It is licensed by
the Curacao Gaming Authority and uses SSL encryption to protect player data.
The casino offers a wide variety of games, including slots, table games, and
live dealer games. It also has a generous welcome bonus and a variety of other
promotions.
The design of YYY Casino is simple and easy to use.
The website is well-organized and the games are easy to find.
The casino also has a mobile app that you can use to play
on your smartphone or tablet.
брикс казино
https://groups.google.com/g/playagainandagain/c/IPCQW4dp0AQ
игровые автоматы бонус без депозита
игровые автоматы бонус без депозита
Neben jeder tollen Optik überzeugt der Live Bereich
des Online Internet casinos auch mit 1 soliden Auswahl a great Tisch- und Kartenspielen sowie Gameshows.
Here is my web site … vulkan Vegas (http://www.cookplay.cz)
Currеntly it looks lіke Expression Engine iѕ tһe preferred blogging platform out tһere riɡht noԝ.
(fгom what I’ve read) Is that what you are using
оn your blog?
Feel free tо visit mу web-site :: slot bet
игровые автоматы онлайн играть бесплатно
игровые автоматы онлайн играть бесплатно
Hello to all, the contents existing at this site are really amazing for people knowledge, well, keep up the nice work fellows.
игровые автоматы онлайн на деньги рубли
https://groups.google.com/g/againplay/c/4nf2ORn_fC8
поиграть в игровые автоматы
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/HTHazL2WlGs
игровые автоматы слоты играть бесплатно без регистрации
https://groups.google.com/g/againplay/c/0AXn5aWZeDE
Thank you for another informative website. Where else could I get that type of info written in such an ideal
means? I’ve a mission that I’m simply now working on, and I have been at the look out for such
information.
Amazing things here. I am very satisfied to look your
post. Thanks so much and I am having a look ahead to contact you.
Will you please drop me a mail?
If some one wants to be updated with newest technologies afterward he
must be pay a visit this site and be up to date everyday.
Hey There. I found your blog using msn. This is a really well written article.
I will make sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I will definitely comeback.
Having read this I thought it was very enlightening.
I appreciate you spending some time and energy to put this content together.
I once again find myself spending way too much time both reading and posting comments.
But so what, it was still worth it!
игровые автоматы с моментальным выводом
https://groups.google.com/g/againplay/c/JmT4USnVqQA
брикс казино
https://groups.google.com/g/playagainandagain/c/IPCQW4dp0AQ
I visited several web sites except the audio feature for audio songs current at this web page is truly superb.
игровые автоматы слоты онлайн
игровые автоматы слоты онлайн
Ahaa, its nice discussion concerning this piece of writing
at this place at this weblog, I have read all that, so at this time
me also commenting here.
This is my first time visit at here and i am genuinely pleassant to read everthing at one place.
игровые зоны россии
https://groups.google.com/g/againplay/c/-BOPSVRtFRE
поиграть в игровые автоматы
https://groups.google.com/g/—-novyekazinosbezdepozitnymbonusom/c/HTHazL2WlGs
казино играть бесплатно и без регистрации
https://groups.google.com/g/againplay/c/GfXztHzbWvw
Hello, i think that i saw you visited my website so i got here
to return the prefer?.I am trying to find issues to enhance my
web site!I guess its good enough to make use of some of your concepts!!
казино гусар
https://groups.google.com/g/againplay/c/LzZuDhXhCdc
казино игровых автоматов играть бесплатно без регистрации
казино игровых автоматов играть бесплатно без регистрации
hello!,I like your writing so much! proportion we keep in touch extra approximately your
article on AOL? I require an expert on this area to resolve my problem.
Maybe that is you! Having a look ahead to see you.
Good article! We are linking to this particularly great
post on our website. Keep up the good writing.
покердом казино скачать
покердом казино скачать
казино император
казино император
казино онлайн бесплатно без регистрации
казино онлайн бесплатно без регистрации
sexax pompadirha.wwB2Gbxg0T97
You’re so interesting! I don’t believe I’ve truly read through anything like this before.
So good to find another person with some genuine thoughts on this subject
matter. Really.. many thanks for starting this up.
This web site is one thing that is needed on the web,
someone with a little originality!
sexax asillartaklitler.C7fAtAznn6kP
рабочее зеркало казино х
рабочее зеркало казино х
Hi, I do think tһis is a great site. I stumbledupon іt 😉 I’m going to revisit once аgain since і have bookmarked
it. Money and freedom iѕ the beѕt way to сhange, mɑy ʏou be
rich and continue tο һelp otһеr people.
Ꮋere is my blog post lotto
I think that what you typed was very reasonable. But, what about this?
what if you were to create a awesome post title?
I am not suggesting your information is not solid., but what if you added something that grabbed folk’s attention? I mean Think
Obstructive Sleep Apnea is #NBD? Here Are Seven Health Conditions Made Worse By Your Undiagnosed OSA – Delaware
Dental Sleep Medicine is a little vanilla. You could look at Yahoo’s front page and note how they create article headlines to get people to click.
You might add a video or a related pic or two to grab readers excited about
everything’ve got to say. In my opinion, it could bring your
blog a little bit more interesting.
escort siteleri hephupx.0Gfsjqo1ryZL
I have been exploring for a bit for any high quality articles or weblog posts in this kind of area .
Exploring in Yahoo I ultimately stumbled upon this site.
Studying this information So i am satisfied to convey that I’ve a very excellent uncanny feeling I found out exactly what I needed.
I so much for sure will make sure to do not disregard this website and
give it a glance regularly.
Very great post. I simply stumbled upon your weblog and wanted to mention that I’ve truly enjoyed surfing around your
blog posts. After all I’ll be subscribing in your feed and I’m hoping you
write once more very soon!
Sweet blog! I found it while searching on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Thanks
Somebody necessarily help to make critically posts I might state.
That is the very first time I frequented your web page
and so far? I amazed with the research you made to create this actual submit incredible.
Excellent job!
excellent issues altogether, you simply won a new reader.
What would you suggest about your put up that you made some days ago?
Any certain?
Please let me know if you’re looking for a author for your site.
You have some really good posts and I believe I would be a good asset.
If you ever want to take some of the load off, I’d really like to write
some articles for your blog in exchange for a link back to mine.
Please send me an email if interested. Thank you!
I’d liҝe to thаnk you for the efforts үou’ve put in writing this site.
Ι’m hoping t᧐ view the ѕame hiɡh-grade content by you in tһe future as well.
In fact, your creative writing abilities һas encouraged mе tօ get mʏ νery
οwn blog noԝ 😉
Ꭺlso visit my blog post – games slot
What’s Going down i’m new to this, I stumbled upon this I’ve found It positively useful and it has helped me
out loads. I’m hoping to contribute & assist other users like
its helped me. Great job.
I’m curious to find out what blog platform you’re utilizing?
I’m experiencing some small security problems with my latest site
and I’d like to find something more secure.
Do you have any solutions?
Thanks very interesting blog!
I am extremely impressed together with your writing skills as smartly as with the format to your blog.
Is that this a paid topic or did you modify it your self?
Anyway keep up the nice quality writing, it’s uncommon to look
a great weblog like this one nowadays..
Greetings! Very helpful advice within this post!
It’s the little changes that produce the biggest changes. Many thanks for
sharing!
In brief, there is no need to trumpet new lovers online, or lash out with an instantaneous “Single”
standing change when that love dies in a huge ball of flames.
Now you’re quietly once more listed as single. Folks have occupied the realm now often called Enchanted Rock State Natural
Space for greater than 10,000 years. Founded by two medically trained Docs,
Ocean Cosmetics is a WA laser skin care clinic that uses evidence-based remedies to revive sagging
and drained skin, to boost your pure magnificence.
If infection ruptures the gland’s ducts, sweat can transfer into the
pores and skin around the glands, causing an itchy inflammation known as miliaria rubra, or “prickly heat.” If this situation advances,
the infected glands can swell with pus in a condition often known as miliaria pustulosa.
It might kind a boil that ruptures and oozes pus, or may develop into
a rash of tiny vesicles, blister-like bumps that itch and
ooze fluid when scratched. Sweat might build up in blocked eccrine
glands to kind miliaria crystalline, a rash of tiny, painless vesicles.
The base of a sweat gland is a coiled structure nestled in the
border between the pores and skin’s thick middle layer, or dermis, and the subcutaneous layer of
fat at the base of the pores and skin.
Псевдопсихология. Мышление ударение.
Точный тест на темперамент. Тест бесплатный. Какие факторы биологические или социальные влияют на развитие
человека и животного. Человеческий индивид это отдельный и типичный представитель человеческого рода.
Top project отзывы. Психическое и психологическое
здоровье.
Having read this I believed it was very informative.
I appreciate you taking the time and effort to put this article together.
I once again find myself personally spending way too
much time both reading and posting comments.
But so what, it was still worthwhile!
Và do đó, chúng tôi luôn tổ chức các chương
trình khuyến mãi 789win đặc biệt.
Chính sách bảo mật của 789win rất rõ ràng, không chia sẻ hay tiết lộ thông
tin cá nhân của người chơi cho bất kỳ tổ chức
hoặc cá nhân nào mà không có sự đồng ý rõ ràng từ phía
người chơi hoặc theo yêu cầu của pháp luật.
Theo nhiều dự báo, Cục Dự trữ Liên bang Mỹ (Fed) sẽ giữ nguyên lãi
suất vào cuộc họp chính sách sắp diễn ra vào ngày 31/10-1/11 nhưng tại cuộc họp này, Fed có thể cung cấp cho các nhà đầu tư cái nhìn sâu sắc về lộ trình lãi suất trước mắt.
Ngoài ra, 789Bet còn được biết đến với
việc cung cấp một loạt các sản phẩm cá cược đa dạng và phong
phú, từ các trò chơi casino trực tuyến đến các trận đấu thể thao hấp dẫn.
Кубань – прекрасный штаковина, щедрый природой равно культурным наследием.
Фото Кубани дают возможность понять всю нее красу и еще разнообразие.
Одним изо самых фаворитных тем фотосъемки является река Кубань.
Фото речки Кувшин запечатлевают ее силища и уникальность.
Этот воднистый этап пробирает целую территорию покрая также возникает евонный главнейшей жизненной артерией.
На фотографиях видно, яко яя Балакирь извивается среди лугов также
лесов, создавая великолепные
пейзажи.
Hey there, You have done an excellent job.
I’ll definitely digg it and personally recommend to my friends.
I am sure they will be benefited from this site.
sexx hepxhupx.OWGT7KgKeaU9
sektor benim zaten amin evladi juljulfbi.SZYxamMgwuVO
This design is wicked! You certainly know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Great job.
I really enjoyed what you had to say, and more than that, how
you presented it. Too cool!
fuck google
It’s perfect time to make some plans for the longer term and it’s time
to be happy. I’ve learn this submit and if I could I desire to counsel you few
attention-grabbing things or suggestions. Perhaps you could write subsequent
articles regarding this article. I want to read even more issues about it!
Hi there Dear, are you genuinely visiting this web page daily, if so then you
will absolutely take good know-how.
What’s up friends, its wonderful paragraph on the topic of tutoringand fully
defined, keep it up all the time.
Undeniably imagine that that you said. Your favourite reason seemed to be at the internet the
simplest thing to have in mind of. I say to you, I certainly get annoyed whilst folks consider issues that they just do not know about.
You managed to hit the nail upon the top as well as outlined out the whole thing without having side effect , other folks
could take a signal. Will likely be back to get more.
Thank you
Upload a data to see if it satisfies the demands for dimension, information and wall surface thickness.
I’m not that much of a online reader to be honest but your sites really nice,
keep it up! I’ll go ahead and bookmark your website to come back
down the road. All the best
Thanks for your marvelous posting! I really enjoyed reading
it, you might be a great author.I will be sure to bookmark your
blog and definitely will come back sometime soon. I want
to encourage that you continue your great posts, have a nice weekend!
Useful information. Lucky me I discovered your web site by accident,
and I’m surprised why this twist of fate did not happened
in advance! I bookmarked it.
I visited various web pages except the audio feature for audio
songs existing at this site is truly superb.
Yet how can you discover the experience of a dentistbefore you schedule an appointment?
I really like reading through an article tһat wilⅼ make people tһink.
Alѕo, many thɑnks for allowing foг me to comment!
Alsso visit mү ρage … semaglutide injection price
I have been browsing on-line more than three hours lately,
but I never found any interesting article like yours.
It is pretty value enough for me. In my view, if all webmasters and bloggers made
excellent content material as you probably did, the web will probably
be a lot more useful than ever before.
Казино Вавада не включено
в черные списки и не попало в рейтинги скриптовых казино, в которых не рекомендовано исполнять на копейка.
Тем не менее, нету достоверной информации о легальности деятельности и используемом софте, оттого
при игре на реальные денежные средства нужно быть смертельно осторожным.
Кроме этого, достаться на официальный сайт без зеркальной ссылки невозможно, а это указывает на блокировку игорного заведения.
Если забежать на официальный сайт вавада , плашка
лицензии внизу страницы будет кликабельной — нажав на неё, можно заприметить сертификат действующей лицензии.
Также на ресурсе нет информации об
использовании лицензионного игрового софта,
оттого уминать вероятность, что программное обеспечение скриптовое.
Портал Вавада предлагает много удобных способов внесения депозита и вывода денег отечественным игрокам.
Все транзакции проходят без комиссии.
Пополнение баланса осуществляется мгновенно, что позволяет клиенту сразу взяться наигрывать на копейка.
Вывод денег занимает минимум времени.
В этом поощрении предусмотрена денежная
доля и фриспины. За выполнение условий игрок получит 100 бесплатных вращений в игровом автомате The Great Pigsby
Megaways. Вейджер на денежную доля бонуса составляет х35, а выигрыш с
фриспинов прокручивают на ставках 20 раз.
На отыгрыш каждой части бонуса дается 14 дней.
Максимальный выигрыш с бонусных средств не может превышать размер
вознаграждения более чем в 10 один.
Казино Вавада не включено в черные списки и не попало в рейтинги скриптовых казино, в которых не рекомендовано
резаться на денежки. Тем не менее, нет достоверной информации о легальности деятельности и используемом софте, посему при
игре на реальные денежные средства нужно быть больно осторожным.
Кроме этого, достаться на официальный сайт без зеркальной ссылки невозможно, а
это указывает на блокировку игорного
заведения.
My brother suggested I might like this web site.
He was entirely right. This post truly made my day.
You cann’t imagine just how much time I had spent for this
info! Thanks!
Для основания вам нужно посетить официальный сайт
РаменБет казино и надавить на кнопку “Регистрация”.
Затем вам будет предложено заполнить
простую форму с основной информацией о себе, такую словно
имя, фамилия, дата рождения, электронная
почта и номер телефона.
После заполнения формы вам потребуется подтвердить свою электронную почту и номер телефона.
Да, у РаменБет казино уничтожать мобильная версия,
которая адаптирована для игры на смартфонах и планшетах.
Для доступа к мобильной версии
необходимо обнаружить официальный сайт казино на мобильном устройстве.
Мобильная версия предлагает все функции и игры, доступные на
десктопной версии сайта. Для любителей атмосферы настоящего казино предлагается возможность сражаться с лайв диллерами.
Они будут раздавать карты или ворочать рулетку
напрямик на ваших глазах. Это создаст ощущение
присутствия в настоящем казино
и добавит прибавочный степень
азарта. Как пройти процесс регистрации
в РаменБет казино? Для удобства игроков РаменБет казино
разработало мобильное приложение, которое позволяет употреблять всеми функциями казино на смартфонах и планшетах.
Приложение имеет немудрящий и интуитивно понятный интерфейс, а также адаптируется к разным
устройствам и операционным системам.
166 sono individuati ed autorizzati i limiti di impegno di spesa quindicennali per la progettazione e realizzazione
delle opere strategiche e di preminente interesse nazionale “individuate in apposito programma approvato”
dal CIPE, prevedendo, tra.
Good way of telling, and fastidious piece of writing to obtain data regarding my presentation subject, which i am going to deliver
in university.
of course like your web-site however you have to test the spelling
on several of your posts. Several of them are rife with spelling issues and I in finding it
very troublesome to inform the truth however I’ll certainly come again again.
naturally like your web-site but you have to check the spelling
on quite a few of your posts. A number of them are rife with spelling issues and I to find it very troublesome
to inform the reality on the other hand I’ll definitely come
again again.
It is the best time to make some plans for the future and it’s
time to be happy. I have read this post and if I could I want to suggest you few interesting things or tips.
Perhaps you could write next articles referring to this article.
I wish to read even more things about it!
Hi, everything is going nicely here and ofcourse every one is sharing facts, that’s genuinely fine, keep up
writing.
The banner stands have screw eyes that allow you to thread the rope with.
Hello There. I found your blog the use of msn. That is a really smartly written article.
I’ll make sure to bookmark it and come back to read extra of your useful info.
Thanks for the post. I will definitely comeback.
I’m pretty pleased to discover this site. I want to
to thank you for your time for this fantastic read!!
I definitely loved every part of it and I have you saved as a favorite to look at new stuff on your website.
Awesome! Its truly remarkable post, I have got much clear idea regarding from this
piece of writing.
Appreciating thе time and energy ʏou pᥙt into youг website ɑnd detailed іnformation ʏou offer.
Іt’ѕ nice tо come acrosѕ a blog eѵery once in a while tһat іsn’t tһe same outdated rehashed material.
Wonderful read! Ι’vе saved үour site and I’m including yоur RSS feeds t᧐ my Google account.
Feel free t᧐ visit my web-site lotto
I am regular visitor, how are you everybody? This article posted at
this site is truly fastidious.
What’s up, yup this article is really fastidious and I have learned lot of things from it concerning
blogging. thanks.
The exceptions to this are when there is a public policy that prevents it, or
when there is a whistleblower statute that protects employees who report
unsafe or unlawful activities by their employers.
Hmm iѕ anyone else hаving ρroblems ԝith the images on this blog loading?
I’m tгying to determine іf itѕ a proЬlem on my end or if it’s the blog.
Ꭺny responses wouⅼd be greatlү appreciated.
Ꮇу site: sport bet (Broderick)
I’m impressed, I must say. Seldom do I encounter a blog that’s equally educative and
amusing, and let me tell you, you have hit the nail on the head.
The issue is something too few men and women are speaking intelligently about.
I’m very happy I came across this in my hunt for something relating to this.
I would like to thank you for the efforts you have put in penning this website.
I am hoping to see the same high-grade blog posts by you in the future as well.
In fact, your creative writing abilities has encouraged
me to get my own website now 😉
Hi! Do you use Twitter? I’d like to follow you if that would be ok.
I’m definitely enjoying your blog annd look forward to new posts.
You could download the pin up number
Up Casino software or play typically the web version on the
official website.
Thanks a lot for sharing this with all people you actually recognise what you’re speaking approximately!
Bookmarked. Kindly also consult with my website =).
We may have a hyperlink exchange arrangement between us
Seguendo le istruzioni passo dopo passo, l’installazione non dovrebbe causare alcun problema.
Precision was specified from the superimposition in between the various scans made with the
very same intraoral scanner.
Do you have any video of that? I’d care to find out more details.
Hmm is anyone else having problems with the pictures on this blog loading?
I’m trying to find out if its a problem on my end
or if it’s the blog. Any feed-back would be greatly appreciated.
Hey There. I found your blog using msn. This is an extremely well written article.
I will be sure to bookmark it and return to read more of your useful info.
Thanks for the post. I will certainly return.
Hi there would you mind letting me know which web host you’re utilizing?
I’ve loaded your blog in 3 different web browsers
and I must say this blog loads a lot quicker then most. Can you recommend a good web hosting provider at
a reasonable price? Thanks a lot, I appreciate it!
fuck google bjluajszz.nTbjvddwosOr
sektor benim zaten amin evladi bxjluajsxzz.47cnU5tGIAig
bahis siteleri incest category 0qbxjluaxcxjsxzz.Cd5UkTkFUkMK
Greetings! Very helpful advice in this particular post!
It’s the little changes that produce the most important
changes. Thanks a lot for sharing!
Không những thế mà còn có rất nhiều các chương trình khuyến mãi hấp dẫn khác, quý khách
có thể xem thêm các chương trình khuyến mãi của 789WiN tại đây.
Ngoài điểm danh nhận thưởng, các bạn cũng có thể tham gia chương trình khuyến mãi song song với chương trình điểm danh hằng ngày nhận thưởng.
Số tiền này có thể sử dụng tham gia các trò chơi trong 789Bet,
khi thắng có thể rút ra như bình thường,
ngoài ra nếu may mắn bạn còn có cơ hội
nhận được những phần quà hấp dẫn của hệ thống nhà cái 789Bet như: đồng hồ, tiền, điện thoại, nước hoa,
… Bước 2: Cung Cấp Thông Tin Cá Nhân – Đảm Bảo Chính Xác Trang đăng ký yêu cầu bạn nhập thông tin cá nhân, bao gồm tên, địa chỉ email, số điện thoại
và các thông tin xác thực khác (nếu cần). Bước 2:
Cung Cấp Thông Tin Cá Nhân – Đảm Bảo Độ Chính Xác Tại trang đăng ký,
bạn sẽ cần nhập thông tin cá nhân của mình, bao gồm tên, địa chỉ email, số điện thoại và các thông
tin xác thực khác (nếu cần).
Thank you for the auspicious writeup. It in fact was
a amusement account it. Look advanced to far added agreeable
from you! However, how could we communicate?
Hello, I enjoy reading through your article post. I like
to write a little comment to support you.
Tham gia tuyển chọn, thực hiện các dự án, đề tài,
nhiệm vụ KHCN các cấp thuộc lĩnh vực
Xây dựng Công trình biển và dầu khí;
Xây dựng Công trình ven biển, ứng phó với biến đổi khí hậu;
Xây dựng cơ bản, … Nghiên cứu khoa học, phát triển công nghệ
và ứng dụng công nghệ mới thuộc lĩnh vực Xây dựng Công
trình biển và dầu khí; Xây dựng Công trình ven biển, ứng phó với biến đổi khí hậu.
Tham gia xây dựng các quy chuẩn, quy phạm, tiêu chuẩn Nhà
nước, tiêu chuẩn ngành thuộc lĩnh
vực chuyên môn có liên quan. Tư vấn, thiết kế,
thẩm định, quản lý chất lượng
các thiết bị, hệ thống công trình thuộc lĩnh vực chuyên môn có liên quan. Tổ chức các khóa New88 nghề, New88
ngắn hạn, các hội thảo, New88 chuyên đề nâng cao…
New88 đại học và sau đại học thuộc lĩnh vực chuyên môn.
I’m not sure where you’re getting your information, but great topic.
I must spend some time learning more or understanding more.
Thank you for magnificent information I used to be searching for this information for
my mission.
When someone writes an article he/she retains the plan of a user in his/her brain that how a user can understand it.
So that’s why this article is outstdanding.
Thanks!
This post is truly a good one it assists new web visitors, who are
wishing in favor of blogging.
Wow that was odd. I just wrote an incredibly long comment but after I clicked submit my comment didn’t
show up. Grrrr… well I’m not writing all that over again. Anyway,
just wanted to say great blog!
Are you looking for a trustworthy solution to enhance the life of your roof?
Shingle Magic Roof Sealer is the answer. Our unique product
delivers an unparalleled level of protection for your asphalt shingles, ensuring they remain durable.
With Shingle Magic Roof Sealer, you’re not just applying any ordinary product.
You’re investing in a top-quality roof rejuvenation solution formulated to
greatly increase the life of your roof by up to 30 years.
Choosing Shingle Magic is a savvy move for property owners aiming to protect their investment.
What makes Shingle Magic Roof Sealer? For starters, its proprietary formula seeps into the asphalt shingles, restoring their initial condition and look.
Furthermore, the sealer is incredibly simple to use, requiring little effort for maximum results.
In addition to Shingle Magic Roof Sealer extend the life of your roof, it also provides exceptional defense against environmental damage.
Whether it’s blistering sun, heavy rain, or freezing temperatures,
it remains well-protected.
Additionally, choosing Shingle Magic Roof Sealer signifies you’re selecting an green option. Its non-toxic makeup ensures minimal environmental
impact, making it a conscious choice for the planet.
In conclusion, Shingle Magic Roof Sealer is unparalleled as the best roof rejuvenation solution.
Not only does it extend the life of your roof and providing superior protection and an environmentally friendly option makes Shingle Magic as the ideal choice
for those aiming to care for their property’s future.
Furthermore, a significant advantage of Shingle Magic Roof Sealer
is its economic efficiency. In lieu of spending a significant amount on constant
repairs or a full roof replacement, choosing Shingle Magic saves you costs
in the long run. It’s a financially savvy choice that
offers premium results.
Furthermore, the user-friendly nature of Shingle
Magic Roof Sealer is noteworthy. You don’t need expert
skills to apply it. For those who like to handle
things themselves or choose for expert application, Shingle Magic guarantees a straightforward process with remarkable results.
Shingle Magic’s durability is yet another significant reason to choose it.
After application, it creates a shield that keeps the integrity of your
shingles for many years. It means less worry about environmental wear and tear and more
peace of mind about the health of your roof.
Regarding appearance, Shingle Magic Roof Sealer also
excels. Not only does it safeguard your roof but also boosts its aesthetic.
Shingles will seem newer, which adds to the attractiveness
and worth to your property.
Customer satisfaction with Shingle Magic Roof Sealer is another
testament to its efficacy. Numerous users have reported remarkable improvements in their roof’s state after using
the product. Reviews emphasize its user-friendliness, longevity, and excellent protection.
Finally, selecting Shingle Magic Roof Sealer is opting for a reliable solution for roof rejuvenation. Its combination of sturdiness, beauty, economic
efficiency, and simplicity positions it as the perfect choice for anyone seeking to enhance the life and look of their roof.
Don’t wait to give your roof the care it deserves
with Shingle Magic Roof Sealer.
Write more, thats all I have to say. Literally, it seems as though you
relied on the video to make your point. You clearly know what youre talking about, why
throw away your intelligence on just posting videos to your site when you could be giving us something informative to read?
Ꮤhy users ѕtill use tⲟ reɑd news papers when in thiѕ technological
globe еverything іs availaЬle on web?
Take a ⅼоok at my web-site – football bet
If you are publishing in an uncommon area,
such as on a pocket, we may advise a transfer.
What’s up, I log on to your new stuff daily. Your writing style is awesome, keep up the good work!
I’ve been browsing online more than three hours today, yet I never found any
interesting article like yours. It is pretty worth enough for me.
In my view, if all web owners and bloggers made good content as you did, the net will be much more useful than ever
before.
I absolutely love your blog.. Great colors &
theme. Did you develop this site yourself? Please reply back as I’m wanting to create my
own website and want to know where you got this from or what the theme is named.
Many thanks!
This is really interesting, You’re a very professional blogger.
I’ve joined your feed and look forward to looking for extra of your wonderful post.
Additionally, I have shared your website in my social
networks
Greetings from Colorado! I’m bored to death at work so I decided to check out your blog on my iphone during lunch
break. I really like the information you present here and can’t
wait to take a look when I get home. I’m surprised at how
quick your blog loaded on my cell phone .. I’m not
even using WIFI, just 3G .. Anyhow, great blog!
Amazing! This blog looks just like my old one!
It’s on a entirely different subject but it has pretty much the same page
layout and design. Outstanding choice of colors!
Pretty section of content. I just stumbled upon your web site and in accession capital to assert that I get in fact
enjoyed account your blog posts. Anyway I will be subscribing to your augment and even I achievement you
access consistently rapidly.
Incredible! This blog looks exactly like my old one! It’s on a entirely different topic but it has
pretty much the same layout and design. Great choice of colors!
First off I would like to say great blog! I had a quick question in which I’d like
to ask if you don’t mind. I was interested to know how you center yourself and clear your thoughts prior to writing.
I’ve had a tough time clearing my mind in getting my
ideas out there. I do take pleasure in writing
but it just seems like the first 10 to 15 minutes are
lost simply just trying to figure out how to begin. Any recommendations or hints?
Thanks!
You’re so cool! I don’t think I’ve truly read through anything like
that before. So nice to find somebody with a few genuine thoughts
on this subject. Really.. many thanks for starting this up.
This web site is one thing that is needed on the internet, someone
with a little originality!
Your means of describing all in this post is truly nice, every one
be capable of easily know it, Thanks a lot.
Very great post. I just stumbled upon your blog and wished to mention that I have truly
loved surfing around your blog posts. After all I’ll be subscribing
in your rss feed and I hope you write again very soon!
First, they recommend 100% plagiarism-free content material that will probably be written upon your request.
Need to request professional essay writer assist and get it proper
this moment?
Hi there, after reading this awesome piece of writing i am also happy to share my experience here with colleagues.
Hello! Do you use Twitter? I’d like to follow you if that would be okay.
I’m definitely enjoying your blog and look forward to new posts.
Nice post. I learn something totally new and challenging on websites I stumbleupon everyday.
It will always be helpful to read through articles from other
writers and practice something from their sites.
Hi, Neat post. There is an issue along with your
site in internet explorer, could test this? IE still is the market chief and a huge element of folks will omit
your wonderful writing due to this problem.
I’m extremely inspired with your writing skills
as smartly as with the layout in your blog. Is that this
a paid topic or did you modify it yourself? Either way keep up the nice
quality writing, it’s rare to peer a nice blog
like this one today..
I believe this is among the so much vital information for me.
And i’m happy reading your article. However should commentary on some normal issues, The web
site style is wonderful, the articles is in point of fact excellent
: D. Excellent process, cheers
The Modern Student’s Dilemma:
https://www.speedwaydigest.com/index.php/news/racing-news/83108-the-nascar-chronicles-evolution-of-the-stock-car-and-its-impact-on-racing-history
In today’s fast-paced instructional landscape, students run into
a plethora of challenges:
Time Constraints: Balancing coursework, part-time jobs, after-school activities, and individual life can leave
pupils with minimal time to commit to essay writing.
Complex Subjects: Some academic subjects need comprehensive expertise and expertise, which may be challenging for trainees to acquire
on their own.
High Expectations: Professors and trainers commonly have high
requirements for essays, anticipating well-researched,
flawlessly composed, and original material.
Stress and anxiety and Pressure: The pressure to perform well
academically can lead to tension and anxiety, affecting a student’s general health.
Just How Essay Services Help Students:
Essay writing services offer pupils with
a number of essential advantages that minimize these
obstacles:
Expert Writers: Essay services use experienced and educated authors that excel in various
scholastic areas. These specialists are fully equipped to
take on complicated topics and deliver top quality web content.
As the admin of this web page is working, no hesitation very shortly it will be well-known,
due to its quality contents.
I seriously love your site.. Great colors & theme.
Did you create this amazing site yourself? Please reply back
as I’m hoping to create my very own website and want to know where you got this from or just what the theme is called.
Appreciate it!
Remarkable! Its really remarkable post, I have got much clear idea concerning from this paragraph.
The snowball that she receives in return is far greater.
As consumers become increasingly indifferent to conventional
advertising and marketing systems, scent outlines alternatives
which might be much less aggressive.
fantastic issues altogether, you simply gained a brand new reader.
What could you suggest about your post that you just made
a few days in the past? Any positive?
my web site; A片
My family members always say that I am killing my time here at web,
however I know I am getting know-how all the time
by reading such nice articles.
Since the admin of this site is working, no hesitation very soon it will be well-known, due to its quality contents.
Valuable info. Fortunate me I found your website by chance, and I’m surprised why this accident
didn’t came about earlier! I bookmarked it.
It’s a pity you don’t have a donate button! I’d without
a doubt donate to this brilliant blog! I guess for now i’ll
settle for book-marking and adding your RSS feed to my Google
account. I look forward to brand new updates and will talk about this blog with my Facebook group.
Talk soon!
What’s up Dear, are you really visiting this web site daily,
if so afterward you will without doubt get fastidious know-how.
I was able to find good advice from your articles.
Prediksi Arta4d
Because the admin of this web site is working, no hesitation very
shortly it will be famous, due to its feature contents.
We are a gaggle of volunteers and opening a new scheme in our community.
Your web site offered us with valuable info
to work on. You’ve done an impressive activity and our whole group will
likely be grateful to you.
Have a look at my website; Llc New Mexico
That is a really good tip particularly to those new to the blogosphere.
Short but very accurate information… Many thanks for sharing this one.
A must read post!
Wow, marvelous blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your website is fantastic,
as well as the content!
Hello I am so grateful I found your blog, I really found you by error, while I was browsing on Yahoo for something else, Regardless I am here now and would just like to say
cheers for a tremendous post and a all round exciting blog (I also love
the theme/design), I don’t have time to look over it all at the minute but
I have saved it and also included your RSS feeds, so when I have time I will be back to read more, Please do
keep up the great work.
Hi to every single one, it’s in fact a pleasant for me to pay a visit
this web page, it consists of valuable Information.
Thanks for finally writing about > Think Obstructive Sleep
Apnea is #NBD? Here Are Seven Health Conditions Made Worse By
Your Undiagnosed OSA – Delaware Dental Sleep Medicine < Liked it!
It’s appropriate time to make some plans for the future and it’s
time to be happy. I have read this post and if I could I desire to suggest you
few interesting things or suggestions. Maybe you could write next articles referring to
this article. I desire to read even more things about it!
In the electronic age, where info is readily obtainable and
time is often scarce, the need for paper and essay writing solutions has actually skyrocketed.
These services assure convenience, quality, and prompt distribution, catering to the needs
of students, specialists, and services alike. Nonetheless, amidst the allure of
outsourcing academic or expert composing jobs, concerns regarding principles, credibility, and scholastic stability impend huge.
In this blog, we delve into the world of paper and essay writing
solutions, exploring the benefits and drawbacks, moral factors to
consider, and the impact they have on education and professional spheres.
https://www.linkedin.com/pulse/speedypaper-review-skillhubcom-pvhne
The Rise of Paper and Essay Writing Services
Paper and essay writing services have become a remedy to the obstacles faced by people and organizations in creating top quality composed
content. These services typically utilize a group of knowledgeable authors
who focus on numerous topics and disciplines.
Customers can put orders for customized essays, study papers, case studies, dissertations, and more, tailored to their specific
requirements and due dates. The benefit of contracting out creating tasks, combined with
the promise of well-researched and expertly composed material, has actually
fueled the spreading of these solutions across the web.
Pros and Cons
Pros:
Time-saving: One of the key benefits of paper and essay writing
services is the time conserved by outsourcing writing tasks.
This is particularly important for trainees and specialists juggling
several duties.
Quality Assurance: Reputable composing solutions typically ensure high-quality, plagiarism-free content,
backed by specialist writers and extensive quality
assurance measures.
Access to Expertise: Clients can access specialized knowledge and competence through expert writers, making sure that their papers are well-researched and informed by the
most current scholastic or sector insights.
Disadvantages:
Honest Concerns: There are honest implications associated with outsourcing scholastic projects, raising questions regarding scholastic
integrity and the credibility of the work submitted.
Dependence: Relying also heavily on writing services can prevent the advancement of critical reasoning, research study, and
creating skills crucial for scholastic and professional development.
Danger of Plagiarism: Despite assurances of originality, there is
a danger of plagiarism when using composing services,
specifically if correct citation and referencing methods are not followed.
Moral Considerations
The moral implications of making use of paper and essay writing services can not be overstated.
While these solutions may offer a fast fix to pushing due dates or academic obstacles,
they raise major concerns about honesty, honesty, and the worth of education and learning.
Pupils who consider outsourcing their jobs may jeopardize their own knowing experiences and academic integrity,
while professionals might deal with honest predicaments in offering work that is not
totally their very own.
This is very attention-grabbing, You are an overly skilled blogger.
I have joined your feed and look ahead to searching for more of your
fantastic post. Additionally, I’ve shared your web site in my social networks
I am truly grateful to the holder of this website who has
shared this wonderful post at at this time.
Nice post. I learn something totally new and challenging on websites I stumbleupon every day.
It will always be interesting to read through content from other authors and practice something from other sites.
Can I simply just say what a relief to discover somebody that
genuinely understands what they’re discussing over the internet.
You certainly understand how to bring a problem to light and make it important.
A lot more people really need to look at this and understand
this side of the story. I can’t believe you’re not
more popular because you surely possess the gift.
Also visit my site … USA Script Helpers
I have read so many articles about the blogger lovers except this
paragraph is really a good post, keep it up.
I visit each day a few websites and information sites to
read articles, but this weblog presents feature based writing.
I think the admin of this web page is truly working hard for his
web page, for the reason that here every information is quality based data.
Hi I am so happy I found your webpage, I really found you by accident, while I was browsing on Google for something else, Regardless I am here now and would just like to say thank you for a incredible post and
a all round interesting blog (I also love the theme/design), I don’t
have time to browse it all at the moment but
I have saved it and also included your RSS feeds, so when I have time
I will be back to read much more, Please do keep up the superb job.
It’s an amazing paragraph in favor of all the internet people; they will get benefit from it I am sure.
Very great post. I just stumbled upon your weblog and wished to
say that I’ve truly enjoyed surfing around your blog posts.
After all I’ll be subscribing for your rss feed and I’m hoping you write again soon!
I’m truly enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more enjoyable
for me to come here and visit more often. Did you hire out a developer to create your theme?
Fantastic work!
You can input a new promo code both during the accounts registration process or even when you’re placing a bet.
Look at my web-site :: 1xbet
Hi! I know this is kinda off topic however , I’d figured I’d ask.
Would you be interested in trading links or maybe guest authoring a blog post or vice-versa?
My website goes over a lot of the same subjects as yours and I feel we could greatly benefit
from each other. If you are interested feel free to shoot me an email.
I look forward to hearing from you! Superb blog by the way!
First, let’s talk about the difference between immigration and emigration. Since 1999, Ms.
Mayzel has been a host of Tv and Radio talk shows wherein she talks concerning the
information in immigration law and solutions questions on stay air.
I was able to find good information from your content.
Greetings from Idaho! I’m bored to death at work so I decided
to check out your site on my iphone during lunch break.
I enjoy the info you present here and can’t wait to take a
look when I get home. I’m amazed at how fast your blog loaded on my cell
phone .. I’m not even using WIFI, just 3G .. Anyhow, wonderful blog!
You really make it appear really easy with your presentation but I
to find this topic to be actually one thing that I think I might
by no means understand. It kind of feels too complicated and very broad for me.
I am taking a look ahead for your subsequent publish, I will try to get the hold of it!
What i do not realize is in fact how you’re no longer really a
lot more smartly-preferred than you may be now.
You are very intelligent. You realize therefore significantly on the subject of this subject, produced me individually believe it from
so many various angles. Its like women and men are not involved until it is something to do with
Girl gaga! Your own stuffs nice. All the time care for it up!
Hello! I just wanted to ask if you ever have any issues with hackers?
My last blog (wordpress) was hacked and I ended up losing many months of hard work due to
no back up. Do you have any solutions to protect against hackers?
It’s approximated that 40% of an indication store’s profits originate from personalized made
banners.
The electronic period has introduced a standard shift in the
means individuals and companies approach the creation of written material,
thanks to the spreading of paper and essay writing services.
While these solutions offer indisputable benefits, they additionally elevate important ethical issues.
This blog post aims to explore the honest measurements of paper and essay writing solutions, exploring both their sensible
advantages and honest factors to consider.
https://vocal.media/stories/chill-vibes-study-playlist-relaxing-music-for-focus
Comprehending Paper and Essay Writing Services
Paper and essay writing services have actually become go-to
options for those looking for help in generating written web content.
These services boast a swimming pool of competent writers with know-how throughout numerous topics and
self-controls. Customers can appoint custom-made essays,
research documents, theses, and more, tailored to their certain requirements and target
dates. The attraction of outsourcing writing tasks lies
in the guarantee of top notch, well-researched material supplied quickly.
Discovering the Advantages:
Time Efficiency: Outsourcing composing tasks saves valuable time for individuals with busy timetables or multiple commitments.
Quality Control: Reputable services ensure the production of high-grade,
initial web content crafted by seasoned authors.
Accessibility to Expertise: Clients gain from
access to specialized knowledge and insights, enhancing the deepness and accuracy of their composed job.
Inspecting the Ethical Concerns:
Academic Integrity: The usage of composing solutions questions concerning the authenticity of submitted work and concessions academic integrity.
Danger of Dependency: Overreliance on creating solutions may hinder the development of
important skills such as essential thinking and research study.
Plagiarism Risks: Despite assurances of originality, there is a prospective risk of unintended plagiarism if appropriate citation and referencing procedures are not followed.
Thanks in support of sharing such a good thinking, post is pleasant,
thats why i have read it fully
We’re a group of volunteers and opening a new scheme in our community.
Your website offered us with valuable info to work on.
You have done a formidable job and our whole community will
be thankful to you.
Hello there, You have done an incredible job.
I will definitely digg it and personally recommend to my friends.
I’m sure they’ll be benefited from this web site.
I am extremely impressed with your writing skills as well as
with the layout on your weblog. Is this a paid theme or did you customize it yourself?
Anyway keep up the excellent quality writing, it’s rare to see a great blog like this one these days.
It’s appropriate time to make a few plans for the longer term and it is time to be happy.
I have learn this publish and if I may I wish to counsel you
few fascinating things or suggestions. Perhaps
you can write next articles regarding this article.
I wish to read even more things about it!
Oh my goodness! Awesome article dude! Thank you, However I am experiencing
troubles with your RSS. I don’t understand the reason why
I am unable to subscribe to it. Is there anybody else getting the
same RSS issues? Anyone who knows the answer can you kindly respond?
Thanks!!
You would need to see an orthodontist for even more customized treatments, such as orthodontics.
I’m not that much of a internet reader to be honest but your sites really nice, keep it up!
I’ll go ahead and bookmark your site to come back down the road.
Many thanks
You have made some good points there. I checked on the internet for
more info about the issue and found most individuals will
go along with your views on this site.
These custom dissertation writers are geared up with the information, expertise, and expertise needed to get the jobs carried out.
It’s amazing designed for me to have a site, which is valuable in support of my
know-how. thanks admin
An interesting discussion is worth comment. I believe that you should publish more about this
topic, it may not be a taboo subject but usually folks
don’t talk about these topics. To the next! All the best!!
Very shortly this site will be famous amid all blog visitors, due to it’s good content
You do not desire anyone touching your smile that hasn’t had years
of experience doing it.
I’ll right away grasp your rss as I can not find your email subscription link or newsletter service.
Do you have any? Kindly allow me understand so that I may subscribe.
Thanks.
Seventy two gallons (274 liters). 40 gallons (151 liters).
The act states that an apology is not an admission of fault
for authorized functions, however merely an expression of sympathy.
my blog :: UK Immigration Lawyer (images.google.com.sg)
However, for many trendy people, the historic prescription holds true: Ambient music can calm the
internal storm, and perhaps present the
readability we need to make the following step in survival.
Other than the medical remedy, non-pharmacological therapy, including cognitive rehabilitation training, vocational
training, music therapy, and psychotherapy are also reported to be efficient.
Motorola Defy Contract may be obtained by way of on-line portals by several prominent
networks of UK together with Vodafone, O2, Orange and T-cell.
Brides especially need their large day to be as special as
attainable they usually invest considerably in each detail, including flower arrangements.
And since audiovisual is normally one among the highest three
costs for any event, the onus is on us as an event planner to extract as much worth from it as potential.
For this, we have taken some information from our long-term shoppers and
have heard from them what they worth most in the connection as part of
our annual training program. It additionally helps them understand the relationship between sounds and words.
This is really interesting, You are a very skilled blogger.
I have joined your rss feed and look forward to seeking more
of your wonderful post. Also, I’ve shared your website in my social networks!
Heya i’m for the primary time here. I came across this board and I find It truly useful & it helped me out much.
I am hoping to give one thing again and aid others like you
aided me.
Hello, I think your blog might be having browser compatibility issues.
When I look at your blog in Firefox, it looks fine but when opening in Internet
Explorer, it has some overlapping. I just wanted to give you a quick
heads up! Other then that, terrific blog!
I’m gone to convey my little brother, that he should also pay a quick visit this web site on regular basis to
obtain updated from hottest gossip.
Right away I am going away to do my breakfast, afterward
having my breakfast coming over again to read further news.
You really make it appear really easy together with your presentation but I in finding this topic to
be actually something which I believe I might by no means understand.
It kind of feels too complicated and extremely huge for me.
I’m having a look forward for your next post, I will attempt to get
the dangle of it!
Лучшее гей порно в сети порно с животными
I think this is among the most vital information for me.
And i am glad reading your article. But want to remark
on some general things, The web site style is wonderful, the articles is really excellent : D.
Good job, cheers
I every time emailed this blog post page to all my
contacts, as if like to read it afterward my contacts will too.
I enjoy what you guys tend to be up too. This kind of clever work and exposure!
Keep up the excellent works guys I’ve included you guys to our
blogroll.
Hi friends, how is everything, and what you wish for to
say on the topic of this paragraph, in my view
its really remarkable designed for me.
I seriously love your blog.. Very nice colors & theme. Did you develop this website yourself?
Please reply back as I’m trying to create my own blog and would love to know where you got this from or exactly what the theme
is called. Many thanks!
Great post. I was checking constantly this weblog and I’m inspired!
Extremely helpful information specifically the remaining part :
) I take care of such info much. I was looking for this certain info for a long time.
Thank you and good luck.
This is a topic that is close to my heart… Cheers!
Where are your contact details though?
Generally I do not learn post on blogs, but I would like to say that this write-up very
forced me to take a look at and do it! Your writing taste has
been surprised me. Thank you, very great post.
I do not know whether it’s just me or if everyone else
encountering issues with your website. It seems like some
of the written text on your posts are running off the screen. Can someone else
please comment and let me know if this is happening to them as well?
This may be a problem with my browser because I’ve had this happen previously.
Thank you
We’re a bunch of volunteers and opening a new scheme
in our community. Your web site provided us with useful information to
work on. You have performed an impressive process and our entire neighborhood might be grateful to you.
There is certainly a great deal to know about this issue.
I like all of the points you have made.
Woah! I’m really enjoying the template/theme of this site.
It’s simple, yet effective. A lot of times it’s tough to get that “perfect balance” between user friendliness
and visual appearance. I must say you have done a very good
job with this. Additionally, the blog loads very fast for me on Chrome.
Outstanding Blog!
I absolutely love your blog and find nearly all of your post’s to be just what
I’m looking for. Does one offer guest writers to write content for you personally?
I wouldn’t mind producing a post or elaborating on many of the subjects
you write with regards to here. Again, awesome blog!
Here is my web-site: เว็บบทความ
I think the admin of this website is actually working
hard in support of his site, as here every information is
quality based material.
Also visit my homepage – สาระน่ารู้
Hi! I understand this is kind of off-topic but
I needed to ask. Does running a well-established blog such as yours take a large amount of work?
I am brand new to operating a blog but I do write in my diary every day.
I’d like to start a blog so I can share my personal experience and views
online. Please let me know if you have any suggestions or tips for new aspiring blog owners.
Thankyou!
If you desire to grow your know-how only keep visiting this site and be updated with the most up-to-date information posted here.
I needed to thank you for this good read!! I definitely loved every bit of it.
I’ve got you bookmarked to check out new stuff you post…
When someone writes an paragraph he/she maintains the
image of a user in his/her brain that how a user can know it.
Thus that’s why this post is great. Thanks!
Nice answer back in return of this matter with solid arguments
and describing everything on the topic of that.
https://stanproperty.com
Thаnk you f᧐r sharing your thoughtѕ. I reɑlly
apρreciate y᧐ur efforts аnd Ӏ am waiting for your further
post thаnk you ߋnce aɡain.
My web site; lotto
Neat blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple tweeks
would really make my blog shine. Please let me
know where you got your theme. Appreciate it
Your style is so unique in comparison tto other folks I have read stuff from.
I appreciate you for posting when you have the opportunity, Guess I’ll just bookmark this page.
Great blog here! Also your website loads up very fast!
What web host are you using? Can I get your affiliate link to your host?
I wish my web site loaded up as quickly as yours lol
I think this is one of the most important information for me.
And i am glad reading your article. But want to remark on some general things, The site style is wonderful,
the articles is really nice : D. Good job, cheers
Heya! I understand this is somewhat off-topic
but I had to ask. Does operating a well-established website
such as yours take a massive amount work? I am brand new to
operating a blog however I do write in my diary every
day. I’d like to start a blog so I will be able to share my
experience and views online. Please let me know if you have any suggestions or tips for brand new aspiring blog owners.
Appreciate it!
Nice post. I learn something new and challenging on websites I stumbleupon everyday.
It will always be helpful to read articles from other authors and practice a little
something from their sites.
You ought to be a part of a contest for one of the finest blogs on the net.
I’m going to highly recommend this site!
I’m extremely impressed with your writing skills and also
with the layout on your weblog. Is this a paid theme or did you
modify it yourself? Either way keep up the excellent quality writing, it’s rare to see a great blog like this
one nowadays.
my web blog ทรรศนะบอล
May I just say what a comfort to discover someone that
genuinely knows what they’re discussing on the web.
You certainly know how to bring a problem to light and make it important.
situs and situs people need to check this out and understand
this side of the story. I can’t believe you’re not situs popular because you
definitely possess the gift.
It’s not my first time to visit this web page, i am visiting this web page dailly and get pleasant information from
here all the time.
I visited various blogs but the audio feature for audio songs
existing at this web page is in fact marvelous.
My partner and I stumbled over here by a different web
address and thought I might check things out.
I like what I see so i am just following you. Look forward to
exploring your web page yet again.
I was wondering if you ever considered changing the page layout of
your site? Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so
people could connect with it better. Youve got an awful lot of text for
only having one or two images. Maybe you could space it out better?
wonderful points altogether, you just gained a new reader.
What might you recommend about your publish that you simply made some days in the past?
Any positive?
An interesting discussion is definitely worth comment.
I believe that you need to write more on this subject, it might not be a taboo matter but usually people don’t speak about these topics.
To the next! Kind regards!!
© document.write(new Date().getFullYear()); Pokagon Band of Potawatomi Indians. Must be 21 years of age. Please play responsibly. Four Winds Casinos are Equal Opportunity Employers. Turn after turn of thrilling action makes Hollywood Casino at Kansas Speedway one of the most unique venues in the city. The KCK casino shares a site with racetrack Kansas Speedway, host of two high-speed NASCAR events each year. Dragon Link Free Slot Spin The Best in Entertainment is happening right now. The drive from Houston to Lake Charles is entirely on Interstate 10. Depending on when you leave, the drive (from downtown Houston) to these closest casinos takes from between 2 and 2 ½ hours. This award celebrates and honors hospitality businesses that have earned consistent and great traveler reviews on TripAdvisor over the past year, and continually delivered a quality customer experience.
https://l-patrick.ch/wynnbet-on-line-sportsbook-and-on-line-casino-home/
Orion Stars 777 is yet another well-liked casino game, so allow us to introduce it. Users in the United States are getting an interesting gambling experience from one of the most popular fish games, which can be found here. The popularity of these kinds of gaming platforms has grown over time, and they are particularly well-known in the nations of South Asia. Learn all there is to know about this application by reading the text all the way through if you want to be entertained for a significant amount of time. Reviews & guides to the best US sportsbooks & casinos. All the latest news on legal gambling in the regulated US states. Covering sportsbook apps, casino apps, poker apps, and all regulated US gambling apps. Before, you go for the Orion Stars Download link and get the Apk. You need to have some basic information regarding the app that you are about to download from this page.
Hey there! I simply would like to give you a huge thumbs up for the great info you
have got right here on this post. I’ll be returning to your website for more soon.
PG Slot
Hey would you mind stating which blog platform you’re working with?
I’m looking to start my own blog in the near future but I’m having a hard time selecting between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different
then most blogs and I’m looking for something unique.
P.S Apologies for getting off-topic but I had to ask!
This piece of writikng presents clear idea in favor of the new visitors
of blogging, that actually how to do blogging and site-building.
My web site – architekt praca Niemcy
Touche. Great arguments. Keep up the great work.
My relatives always say that I am killing my time here at web, but I know I am getting knowledge everyday by
reading thes good articles.
I’ve been surfing on-line more than 3 hours as of late, yet I never found any interesting
article like yours. It is pretty price enough for me. In my view,
if all webmasters and bloggers made just right content material as you probably did, the net can be a lot
more helpful than ever before.
http://stanproperty.com/bungalow
For latest news you have to pay a visit web and on the web I found this web site as a most excellent web
page for latest updates.
Piece of writing writing is also a fun, if you know afterward you can write otherwise
it is complicated to write.
Take a look at my site; PuffWow
Hello, constantly i used to check web site posts here early in the dawn, for the reason that
i like to learn more and more.
https://google.com/maps/place/Palmer+Media/@38.2628063,-85.7129946,15z/data=!4m2!3m1!1s0x8869731708871ad7:0xd6aba4e37a5fadd1/
Thank you for some other excellent article. The place else could anybody get that kind of info
in such an ideal method of writing? I’ve a presentation next week, and I’m on the look
for such information.
I all the time used to read piece of writing in news papers but now as I am a user
of web therefore from now I am using net for posts, thanks to web.
Do you mind if I quote a couple of your posts
as long as I provide credit and sources back to
your site? My blog site is in the exact same niche as yours and my users would truly benefit
from some of the information you provide here. Please let me
know if this okay with you. Many thanks!
You actually make it seem so easy with your presentation but I find this matter to be actually something which I think
I would never understand. It seems too complex and extremely broad for me.
I am looking forward for your next post, I’ll try to get the hang of it!
Enhance Your Workspace with Freedman’s Office Chairs in Fort Lauderdale
**Experience Unmatched Comfort with Freedman’s Ergonomic Office Chairs**
Freedman’s Office Furniture, situated at 515 E Las Olas Blvd Suite
120, Fort Lauderdale, FL 33301, brings you a premium selection of ergonomic office chairs designed to elevate your comfort and productivity.
Serving neighborhoods like Colee Hammock and Central Beach, Freedman’s is committed to providing
top-notch seating solutions for your workplace.
**Embracing Comfort and Style in Fort Lauderdale**
Founded in 1911, Fort Lauderdale boasts a rich history and a population of 181,
668 as of 2021. With 80,031 households, the city
thrives as a hub of business and leisure. Connected by the bustling I-75 highway, Fort Lauderdale is
a vibrant city known for its stunning beaches and diverse cultural scene.
**Seating Solutions Tailored to Fort Lauderdale’s Dynamic
Environment**
Just like Fort Lauderdale’s varied landscape, Freedman’s ergonomic
office chairs offer versatility and adaptability.
Whether you’re working in the bustling streets of Central Fort Lauderdale or the serene neighborhoods of Beverly Heights, our chairs provide
the perfect blend of support and style to complement your
workspace.
**Affordable Repairs and Climate-Adaptive Office Chairs**
Freedman’s understands the importance of a comfortable workspace.
That’s why we offer affordable repair services for our ergonomic office chairs in Fort Lauderdale.
Crafted to withstand the city’s varying temperatures, our
chairs ensure year-round comfort and support for all your professional endeavors.
**Exploring Fort Lauderdale’s Unique Points of Interest**
Discover the charm of Fort Lauderdale with these notable attractions:
– **Anglin’s Fishing Pier:** A historic landmark offering
scenic views and excellent fishing opportunities.
– **Bonnet House Museum & Gardens:** Immerse yourself in art, history,
and nature at this exquisite estate.
– **Dr. Von D. Mizell-Eula Johnson State Park:** Explore mangrove swamps, beaches,
and hiking trails in this coastal paradise.
– **El Prado Park:** A serene green space perfect for picnics and outdoor relaxation.
– **Esplanade Park:** Enjoy events and concerts in this lively park along the New River.
**Why Choose Freedman’s for Your Office Furniture Needs in Fort Lauderdale**
Opting for Freedman’s ergonomic office chairs means choosing unparalleled comfort, innovative design, and durability tailored to Fort Lauderdale’s dynamic environment.
Upgrade your workspace with Freedman’s, where each chair represents the perfect balance
of support, style, and functionality, ensuring a productive and comfortable
workday in Fort Lauderdale.
Hey theге! I’m at work browsing your blog
from my new iphone! Јust wanted to saу I love reading thгough уoսr blog and ⅼ᧐oҝ forward to all yoᥙr posts!
Keeρ up the fantastic ᴡork!
Feel free t᧐ visit mʏ website – casino
I got this web page from my friend who informed me regarding this website and
now this time I am browsing this web site and reading very informative articles
or reviews here.
You really make it seem so easy with your presentation but
I find this matter to be actually something which I think I
would never understand. It seems too complicated and very broad for me.
I am looking forward for your next post, I will
try to get the hang of it!
I have been surfing on-line greater than 3 hours lately,
but I by no means discovered any fascinating article like yours.
It’s lovely worth sufficient for me. In my view, if all
site owners and bloggers made good content material as you did, the
internet can be a lot more helpful than ever before.
It’s impressive that you are getting ideas from this piece of writing as well as
from our argument made here.
Heya! I just wanted to ask if you ever have any trouble with hackers?
My last blog (wordpress) was hacked and I ended up losing several weeks of hard work due to no backup.
Do you have any methods to protect against hackers?
Hello, all is going well here and ofcourse every one is sharing data,
that’s in fact good, keep up writing.
Have you ever considered publishing an e-book or guest authoring on other blogs?
I have a blog based on the same information you discuss and would love to
have you share some stories/information. I know my
viewers would enjoy your work. If you are even remotely interested, feel free to send me an e-mail.
situs judi slot online kasino oline togel online dan judi bola
Simply wish to say your article is as surprising.
The clarity in your post is simply spectacular and i could assume you are an expert on this
subject. Fine with your permission let me to grab your RSS feed to keep
updated with forthcoming post. Thanks a million and please
carry on the enjoyable work.
Hey there! Would you mind if I share your blog with my myspace group?
There’s a lot of people that I think would really enjoy your content.
Please let me know. Cheers
My family members all the time say that I am killing my time here at
net, except I know I am getting knowledge all the time by reading
thes good articles.
I like loοking thr᧐ugh an article that can maқe men ɑnd women thіnk.
Also, mаny thɑnks for allowing me to comment!
Нere is my webpage: gambling (Florida)
Have you ever thought about adding a little bit more than just your
articles? I mean, what you say is valuable and all.
However just imagine if you added some great graphics or video clips to give your
posts more, “pop”! Your content is excellent but with images and videos,
this blog could definitely be one of the best in its niche.
Awesome blog!
I am in fact pleased to glance at this webpage posts which consists of lots of valuable data, thanks for providing these kinds of statistics.
When it comes to plumbing repairs, Preferred Plumbers are a cut
above the rest for numerous reasons. Given our extensive experience and commitment to quality, we’re confident in stating that we’re the #1 choice
when you need a plumber. Here’s why:
Broad Service Spectrum
Our team is skilled in a broad range of plumbing services,
from detecting leaks and pipe repair to drain cleaning
and faucet installation. Whether you need assistance with your
sewer line or your water heater fixed, we have the skills to address all
your plumbing needs.
24/7 Availability
Emergencies don’t wait for business hours, and neither do we.
Preferred Plumbers is on call 24/7 to guarantee that plumbing emergencies are taken care of immediately, preventing further issues and bringing your peace of mind.
Focus on Customer Satisfaction
At our company, the customer is our foremost concern. We are committed to provide tailored solutions that satisfy
your specific needs, making sure that you’re completely satisfied with our work.
Exceptional Craftsmanship
Craftsmanship is at the heart of what we do at Preferred Plumbers.
We use only the best materials and cutting-edge techniques to
provide long-term fixes and installations. Our objective is to provide services that stand the test of
time.
No Hidden Fees
Knowing the cost of plumbing services upfront is crucial, which
is why we ensure transparent pricing. You’ll know the cost before any work begins,
with no unexpected charges to worry about.
Fully Licensed and Insured
For your protection, Preferred Plumbers is fully licensed and insured.
This means that all our services adheres to industry standards and
you’re protected in the rare case something goes
wrong.
Selecting Preferred Plumbers means selecting a company committed
to excellence. We’re not just another plumbing service; we’re partners in ensuring the well-being of your plumbing system.
Reach out to us today and experience why Preferred Plumbers are the #1 choice when you need a plumber.
My relatives all the time say that I am wasting my time here at net, except I know I am getting knowledge everyday by reading thes pleasant articles.
Thank you for the auspicious writeup. It in fact was a
amusement account it. Look advanced to far added agreeable from
you! However, how can we communicate?
Coping with Autoimmune Diseases – A Holistic Approach – albuterol nebulizer
Normally I do not learn article on blogs, however I would like to say that this write-up very compelled me to check
out and do it! Your writing style has been surprised me.
Thank you, very nice article.
You really make it seem so easy with your presentation but
I find this matter to be really something that I think I would never understand.
It seems too complex and extremely broad for me.
I’m looking forward for your next post, I’ll try to
get the hang of it!
Oh my goodness! Incredible article dude! Many thanks,
However I am having issues with your RSS. I don’t know the reason why I cannot join it.
Is there anyone else having similar RSS problems?
Anyone who knows the solution will you kindly respond? Thanx!!
My partner and I absolutely love your blog and find most of your post’s to be precisely what I’m
looking for. Do you offer guest writers to write content to suit your needs?
I wouldn’t mind producing a post or elaborating on a number of the subjects you write about here.
Again, awesome web site!
The rougher surface on the back will not produce a solid enough bond with
the vinyl’s adhesive.
This is the perfect webpage for everyone who hopes to understand this topic.
You understand so much its almost hard to argue with
you (not that I personally would want to…HaHa).
You certainly put a fresh spin on a subject that’s been written about for decades.
Great stuff, just great!
Υou actuaⅼly maқе іt seem ѕo easy with your presentation Ƅut Ӏ
find thiѕ topic to be ɑctually somеthing which I tһink I would never understand.
It seems toо complicated ɑnd extremely broad fоr me. I’m
looking forward fⲟr yoᥙr next post, I’ll tгy to gеt the hang of it!
Feel free t᧐ visit my site: gambling
Today, I went to the beachfront with my kids. I found
a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.”
She placed the shell to her ear and screamed.
There was a hermit crab inside and it pinched her ear. She never wants to go back!
LoL I know this is totally off topic but I had to tell someone!
It’s fantastic that you are getting ideas from this article as well as from our argument made at this place.
Hello there, You’ve done a great job. I will certainly digg it and
personally recommend to my friends. I’m confident they will be benefited from this site.
We’re a group of volunteers and starting a brand new scheme in our community.
Your website provided us with useful info to work on. You’ve performed an impressive task and our whole neighborhood shall be grateful to you.
If you wish for to take a great deal from this paragraph then you have to
apply these strategies to your won weblog.
Polypropylene, which is chemically inert, can be cleansed with nearly anything,
consisting of low and also high pH chemistries.
What’s up to every , since I am really eager of reading
this weblog’s post to be updated on a regular basis.
It contains nice information.
I always used to read paragraph in news papers but now as I am a user of net therefore from now I am using net for posts, thanks to
web.
I am extremely impressed with your writing skills as
well as with the layout on your weblog. Is this a paid theme or did you modify
it yourself? Anyway keep up the nice quality writing, it is rare to
see a great blog like this one nowadays.
It’s very effortless to find out any matter on net as compared to books, as I found this
post at this web page.
I know this site offers quality depending articles or
reviews and other stuff, is there any other web page which provides these
kinds of data in quality?
Greetingѕ! Ⅴery uѕeful advice ѡithin tһis post!
It іs tһe littlе ϲhanges tһat produce the biggest changeѕ.
Thanks for sharing!
Αlso visit my blog :: huay online
Hi Dear, are you truly visiting this web site daily, if so after
that you will definitely obtain nice know-how.
Discover the thrill of victory at our Mexican online casino. With adrenaline-pumping games and heart-stopping excitement, you’ll be on the edge of your seat with every bet. caliente casino en linea la riqueza esta a tus pies.
Thanks for your personal marvelous posting! I quite enjoyed reading it, you can be a great author.I will be sure to bookmark your blog and will come
back in the foreseeable future. I want to encourage continue your great writing, have a nice weekend!
Also visit my web site สาระน่ารู้
It’s remarkable in support of mе t᧐ һave
ɑ website, whicһ is valuable in support of my knowledge.
tһanks admin
Μy web-site – lotto – Dick –
Hey! Ɗo you uѕe Twitter? І’d like to follow you іf that would be okаy.
Ӏ’m definitely enjoying youг blog and look forward to new posts.
Looк at my site lotto bet
Wonderful blog! I found it while searching on Yahoo News.
Do you have any tips on how to get listed
in Yahoo News? I’ve been trying for a while but I never seem to get there!
Many thanks
The other day, while I was at work, my sister stole my
apple ipad and tested to see if it can survive a thirty foot drop, just so she can be a youtube sensation. My
apple ipad is now broken and she has 83 views.
I know this is completely off topic but I had to share it with someone!
You really make it appear so easy together with your presentation but I find this topic to be really one thing which I
feel I’d never understand. It sort of feels too complex and extremely broad for me.
I’m taking a look forward for your subsequent publish, I
will try to get the dangle of it!
Heya i am for the first time here. I came across this board and I find It really useful
& it helped me out a lot. I hope to give something back and help others
like you helped me.
Greetings from Colorado! I’m bored to tears
at work so I decided to browse your website on my iphone during lunch break.
I love the knowledge you provide here and can’t wait to take a look when I get home.
I’m shocked at how quick your blog loaded on my cell phone ..
I’m not even using WIFI, just 3G .. Anyhow, amazing site!
Your cart mirrors the order, quantity, and the rate that you need
to pay.
Hello mates, fastidious article and pleasant urging commented
at this place, I am actually enjoying by these.
Hey very niice blog!
Undeniably consider that which you said. Your favorite reason seemed to
be at the web the simplest thing to take note of.
I say to you, I certainly get irked even as people consider issues that they just don’t understand about.
You controlled to hit the nail upon the highest
and also defined out the whole thing with no need
side effect , folks can take a signal. Will likely be again to get more.
Thank you
Hi my friend! I wish to say that this article is amazing, great
written and come with approximately all vital infos.
I would like to peer more posts like this .
You can definitely see your expertise in the article you write.
The sector hopes for more passionate writers like you who
aren’t afraid to say how they believe. At all times go after your heart.
For most recent news you have to pay a quick visit web and on web I
found this web site as a most excellent web site for hottest updates.
Hi there, I discovered your site by the use of Google whilst searching for a related subject, your site came up,
it appears good. I have bookmarked it in my google bookmarks.
Hello there, simply turned into alert to your blog thru
Google, and located that it’s truly informative.
I am gonna watch out for brussels. I will be grateful for those who proceed this
in future. Numerous other folks will likely be benefited out of your writing.
Cheers!
Hi my family member! I want to say that this article is amazing, nice written and come with approximately all significant infos.
I would like to peer more posts like this .
We’re a group of volunteers and opening a new scheme in our community.
Your website offered us with valuable info to work
on. You’ve done an impressive job and our whole community will be thankful to you.
I have been exploring for a little for any high quality
articles or blog posts on this sort of space . Exploring in Yahoo I finally stumbled upon this site.
Studying this information So i am happy to express that I’ve a very just right uncanny feeling I came upon just what I needed.
I most indisputably will make sure to don?t disregard this web site and give it a look regularly.
An intriguing discussion is definitely worth comment. There’s no doubt that that
you ought to write more on this issue, it may not be a taboo matter but
usually people don’t speak about these subjects. To the next!
Best wishes!!
It is hard to discover a casino with the dedicated application, plus not all gambling dens have a good mobile Web Site variation.
We’re a group of volunteers and opening a new scheme in our community.
Your site offered us with valuable info to work on. You’ve
done a formidable job and our entire community
will be thankful to you.
Hey there! Someone in my Myspace group shared this website with us so I came to give it a look.
I’m definitely loving the information. I’m bookmarking and will be tweeting this to my followers!
Excellent blog and terrific design and style.
WOW just what I was searching for. Came here by searching for pocket
option
Здесь выигрыши будут не так часто, но высокие котировки
позволяют комфортно себя чувствовать при использовании грамотной системы.
Pretty component of content. I just stumbled upon your website and in accession capital to claim that I acquire in fact loved account your
weblog posts. Anyway I’ll be subscribing to your feeds or even I success you access constantly rapidly.
bookmarked!!, I love your website!
Thank you for the auspicious writeup. It in truth was
a amusement account it. Look complex to far added agreeable from you!
By the way, how could we keep up a correspondence?
Thank you for every other wonderful post. Where else may just anybody get that kind of information in such
a perfect method of writing? I’ve a presentation next week, and I’m at the search for such info.
Play like a pro at our Mexican online casino. With expert tips and strategies, you’ll maximize your chances of hitting the big time. caliente casino en lГnea la clave para una buena vida.
deepthroat, blowjob, anal, amatureporn, facefuck, baldpussy,
asstomouth, assfucking, bbw, bbc, bigcock, bigass,
teenass, teenfuck, bigtits, titfuck, footjob,thighjob, blackcock, hentai, ecchi, pedophliia, ebony, bigboobs,
throatfucking, hardcore, bdsm, oldandyoung, masturbation, milf, missionary, nudist, oralsex, orgasm, penetration, pussylicking, teenporn, threesome, whores, bokep, bokepindonesia, bokepterbaru, bokepindonesiaterbaru, bokepterupdate, porno, pornoindonesia, pornoterbaru, pornoterupdate, xnxx.com, pornhub.com,
xvideos.com, redtube.com
Hello there! This is my first comment here so I just
wanted to give a quick shout out and tell you I genuinely enjoy
reading your articles. Can you suggest any other
blogs/websites/forums that deal with the same topics?
Thank you so much!
Hey! I could һave sworn I’ve been to this website
befօre but afteг checking throսgh some ⲟf the post І realized it’s neԝ to mе.
Anyᴡays, Ӏ’m definitely glad І foᥙnd it and I’ll be book-marking аnd checking baϲk
often!
Taкe a look at my blog :: lotto (Savannah)
Hello, i think that i saw you visited my blog so i came to “return the favor”.I
am attempting to find things to enhance my web site!I suppose
its ok to use a few of your ideas!!
Howdy! I’m at work surfing around your blog from my new iphone 3gs!
Just wanted to say I love reading your blog and look forward to all your posts!
Carry on the outstanding work!
My coder is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the expenses.
But he’s tryiong none the less. I’ve been using WordPress on numerous websites for about a year and am concerned about switching to another platform.
I have heard fantastic things about blogengine.net. Is there a way
I can import all my wordpress posts into it? Any help would be
really appreciated!
I just like the valuable information you provide for your articles.
I will bookmark your blog and take a look at again right here regularly.
I’m rather certain I’ll be informed lots of new stuff right right here!
Best of luck for the following!
Today, I went to the beachfront with my kids.
I found a sea shell and gave it to my 4 year old daughter
and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and screamed.
There was a hermit crab inside and it pinched her
ear. She never wants to go back! LoL I know this is totally off topic but I had to tell someone!
What’s Going down i am new to this, I stumbled upon this I’ve found It absolutely helpful and it has
helped me out loads. I am hoping to give a contribution & aid other users like its aided
me. Good job.
Thank you a lot fօr sharing this with all people үou aⅽtually recognise
ԝhat ʏou’rе talking ɑbout! Bookmarked. Kindly ɑlso visit my web site =).
Ꮤe may haѵe a hyperlink alternate arrangement аmong
uѕ
My һomepage: lottery; Karissa,
FO
With havin so much written content do you ever run into any issues of
plagorism or copyright violation? My blog has
a lot of completely unique content I’ve either written myself
or outsourced but it appears a lot of it is popping it
up all over the web without my permission. Do you know
any methods to help protect against content from being ripped off?
I’d genuinely appreciate it.
Pretty! This has been an incredibly wonderful article. Thank you for supplying this information.
When I initially left a comment I seem to have clicked the -Notify me when new comments are added-
checkbox and now each time a comment is added I recieve four emails with the exact
same comment. Perhaps there is an easy method you are able to
remove me from that service? Many thanks!
Hi there, just became alert to your blog through Google, and found that it is really informative.
I’m going to watch out for brussels. I will appreciate if you continue this in future.
Many people will be benefited from your writing.
Cheers!
Nice blog right here! Additionally your web site so much up fast!
What host are you the usage of? Can I am getting your associate
link on your host? I wish my web site loaded up
as fast as yours lol
Situs Togel
Hello terrific website! Does running a blog similar
to this require a large amount of work? I have very little understanding of computer programming however I had been hoping to start
my own blog soon. Anyways, if you have any recommendations
or techniques for new blog owners please share. I know this is
off subject however I just needed to ask. Thanks!
Stability Healthcare San Pedro
222 Ꮤ 6th St Suite 330,
San Pedro, CA 90731, United Stɑtes
18557424767
Bookmarks (http://www.protopage.com)
Very nice post. I just stumbled upon your weblog and wished to say
that I have truly enjoyed surfing around your blog posts. After
all I’ll be subscribing to your feed and I hope you write again soon!
Hello I am so grateful I found your blog page, I really found you by
mistake, while I was researching on Yahoo for something else, Regardless
I am here now and would just like to say many thanks for a marvelous post and
a all round entertaining blog (I also love the theme/design),
I don’t have time to look over it all at the minute but I
have bookmarked it and also added in your RSS feeds, so when I have time I will be back to read
a lot more, Please do keep up the excellent work.
Greate post. Keep posting such kind of info on your page. Im really impressed by your blog.
Hey there, You’ve performed a fantastic job. I will definitely digg it
and individually suggest to my friends. I am confident they will be benefited from this web site.
Definitely believe that that you stated. Your favorite justification appeared to
be on the internet the easiest factor to take into account of.
I say to you, I definitely get irked whilst folks think about
worries that they just do not recognize about. You controlled to hit
the nail upon the highest as neatly as defined out the entire thing with
no need side effect , people could take a signal.
Will probably be back to get more. Thank you
Thanks , I’ve just been searching for info approximately this topic for ages and yours is
the greatest I’ve came upon till now. However, what concerning the bottom line?
Are you sure about the source?
What’s up friends, how is all, and what you desire to say on the topic of this
post, in my view its really remarkable designed for me.
The Walt Disney World resort, which started in 1971 with the opening of the Magic
Kingdom, dwarfs Disneyland in California and gives all of the room
the corporate wants for enlargement. Tokyo Disneyland on April 16, 1983, making
it the first worldwide Disney park. Based mostly on shares outstanding,
the company is valued around $one hundred fifty billion in 2017, making it one of the world’s most useful brands.
The corporate opened Disney’s California Journey next to Disneyland in 2001.
That very same yr, the company expanded Tokyo Disneyland
with the opening of Tokyo DisneySea. The Disney Brothers
Cartoon Studio formed on October 16, 1923 — the identical day that Roy and Walt Disney inked a deal
to make a collection of short films recognized because the “Alice Comedies.” The movies
centered on the adventures of a stay-motion younger woman named Alice, along
with cartoon buddies. Disney made its first enterprise into full-size
dwell-motion motion pictures in 1950 with “Treasure Island.” Of course,
that didn’t imply the corporate was carried out with animation — just a little movie known as “Cinderella” came out
that very same year. When Disney misplaced the rights to Oswald,
thanks to a studio dispute, he moved on to just a little creation that we all know today as Mickey Mouse.
Spot on with this write-up, I really believe this amazing site needs a
great deal more attention. I’ll probably be back again to read more, thanks for the advice!
Good post. I’m dealing with some of these issues as well..
Why viewers still make use of to read news papers when in this
technological world all is existing on net?
I think this is one of the most vital info for me. And i’m glad reading
your article. But wanna remark on few general things,
The website style is perfect, the articles is really great : D.
Good job, cheers
I visited several sites however the audio quality for audio songs
existing at this web page is truly excellent.
I am in fact grateful to the holder of this web site who
has shared this great article at at this place.
It’s very straightforward to find out any matter on web as
compared to textbooks, as I found this piece of writing
at this website.
I’m not that much of a online reader to be honest but
your blogs really nice, keep it up! I’ll go ahead
and bookmark your site to come back down the road.
Many thanks
I like the helpful information you provide in your articles.
I will bookmark your weblog and check again here frequently.
I am quite certain I’ll learn lots of new stuff
right here! Best of luck for the next!
Thankfulness to my father who shared with me concerning this blog, this weblog is truly awesome.
My brother recommended I might like this blog. He was entirely right.
This submit truly made my day. You can not consider simply how
so much time I had spent for this info! Thank you!
I love it when people get together and share ideas.
Great site, keep it up!
There’s a more recent idea of verifiability: nontrivial statements in Wikipedia articles should be cited to
some supply where the reader may confirm them.
I’vе learn somе excellent stuff hеre. Certainlу price bookmarking fοr revisiting.
I surprise how so much attempt you sеt to
ⅽreate thіs қind of fantastic informative web site.
mү webpage sa casino
I am no longer positive the place you’re getting your
information, however great topic. I needs to spend some time studying
much more or figuring out more. Thank you for magnificent info I was in search
of this information for my mission.
Hi there, I do believe your site could possibly be having internet browser compatibility issues.
Whenever I take a look at your web site in Safari, it looks fine however when opening in Internet Explorer, it’s got some overlapping issues.
I just wanted to provide you with a quick heads up!
Aside from that, great website!
Hello! This is kind of off topic but I need some help from an established
blog. Is it difficult to set up your own blog?
I’m not very techincal but I can figure things out pretty quick.
I’m thinking about creating my own but I’m not sure where to begin. Do you have any points or suggestions?
Many thanks
Hey, I think your website might be having browser compatibility issues.
When I look at your blog in Firefox, it looks fine but when opening in Internet Explorer,
it has some overlapping. I just wanted to give you a quick heads up!
Other then that, excellent blog!
I loved as much aѕ үoᥙ’ll receive carried οut right here.
The sketch іs attractive, your authored
material stylish. nonetһeless, yoᥙ command get bought аn impatience over tһat you
wish be delivering tһe follⲟwing. unwell unquestionably ϲome more formerⅼy aɡain sіnce exɑctly the same nearlʏ a lot often inside case
you shield this increase.
Also visit my web-site: lottery
I relish, cause I found exactly what I was having a look
for. You’ve ended my 4 day lengthy hunt! God Bless you man. Have a great day.
Bye
Wonderful blog! I found it while surfing around on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Cheers
Win big and win often at our Mexican online casino. With generous payouts and thrilling tournaments, the sky’s the limit when you play with us. betmexico iniciar sesion te da mas.
obviously like your web-site but you have to take a look at the spelling on several of your posts.
Several of them are rife with spelling problems and I in finding it very troublesome to tell the reality however I will
surely come back again.
My relatives evеry timе saу that I am killing my timе һere at web,
but I know I am getting know-how everyday by reading sᥙch nice articles οr reviews.
Look intо my web site: lotto
Hmm is anyone else encountering problems with the images on this blog loading?
I’m trying to find out if its a problem on my end or if it’s the blog.
Any suggestions would be greatly appreciated.
I like the valuable info you provide in your articles.
I will bookmark your weblog and check again here regularly.
I am quite sure I’ll learn many new stuff right here!
Good luck for the next!
Ꮩery nice post. I jᥙst stumbled up᧐n yߋur
blog and wished t᧐ say that I һave reɑlly enjoyed surfing aroᥙnd yߋur blog posts.
Ιn any ⅽase I will be subscribing to үour feed and I hope үou ԝrite ɑgain soon!
Feel free to visit mʏ blog post :: huay online – Zane –
Nice post. I was checking continuously this blog and I’m impressed!
Very helpful info specifically the last part 🙂 I care for such
info a lot. I was seeking this certain information for a long time.
Thank you and good luck.
I for all time emailed this blog post page to all my associates, as if like to read it
then my contacts will too.
This is my first time pay a visit at here and i am genuinely impressed to read
everthing at single place.
Thanks very nice blog!
Thanks for finally talking about > Think Obstructive Sleep Apnea is #NBD?
Here Are Seven Health Conditions Made Worse By Your Undiagnosed OSA – Delaware Dental Sleep Medicine < Loved it!
Quality posts is the crucial to interest the people to visit the website,
that’s what this web site is providing.
What’s up colleagues, fastidious piece of writing and good
urging commented at this place, I am really enjoying by these.
Hey! Would you mind if I share your blog with my twitter
group? There’s a lot of people that I think would really appreciate
your content. Please let me know. Many thanks
This is my first time visit at here and i am really pleassant to read all at one
place.
This site was… how do I say it? Relevant!! Finally I’ve found something that helped me.
Kudos!
I am truly pleased to read this website posts which includes tons of useful information, thanks for
providing these statistics.
Həmçinin, Esports həvəskarları virtual fənlər üzrə çempionatların nəticələrinə uzunmüddətli mərc
edə bilərlər.
my blog – mostbet azerbaycan (cerradurainteligente.org)
Way cool! Some very valid points! I appreciate you
writing this write-up plus the rest of the website is also very good.
It’s really very complicated in this busy life to listen news on TV, thus I just use world wide web for that
reason, and take the most recent information.
I was suggested this blog by my cousin. I am not sure whether
or not this post is written through him as no one else
recognize such unique about my difficulty. You are incredible!
Thank you!
Keep on working, great job!
I like the helpful info you provide in your articles. I will
bookmark your weblog and check again here frequently.
I’m quite sure I will learn lots of new stuff right here!
Best of luck for the next!
Hello! I’m at work surfing around your blog from my new apple iphone!
Just wanted to say I love reading through your blog and look forward to all your posts!
Carry on the outstanding work!
Hi there just wanted to give you a quick heads up.
The text in your content seem to be running off the
screen in Safari. I’m not sure if this is a formatting issue or something to do with browser compatibility but I
figured I’d post to let you know. The layout look
great though! Hope you get the issue fixed soon. Many thanks
You actually make it seem really easy along with your presentation however I find this
matter to be really something which I think I’d by no means understand.
It sort of feels too complicated and extremely huge for me.
I am looking ahead in your next post, I will try to get
the hold of it!
I really like reading an article that can make men and women think.
Also, many thanks for allowing for me to comment!
Hey there! This post coᥙld not be written any better!
Reading tһiѕ post reminds me of my good old rօom mate!
He ɑlways қept chatting ɑbout this. Ι wilⅼ forward tһis write-սр
to him. Pretty ѕure һe ԝill havе a gooԀ reаⅾ.
Thanks for sharing!
Check οut my blog post :: lotto
There’s certainly a great deal to know about this issue.
I love all of the points you’ve made.
Hi there, just became aware of your blog through Google, and found that it’s
truly informative. I’m gonna watch out for brussels. I’ll appreciate if you continue this in future.
Numerous people will be benefited from your writing. Cheers!
Dalam beberapa waktu terakhir, game slot online telah menjadi
sangat populer. Ini disebabkan oleh kemajuan teknologi yang memungkinkan para pemain untuk mengakses informasi dan berbagai hiburan secara online, termasuk permainan slot.
Bermain slot online bukan lagi sekadar mengisi waktu
luang, tetapi juga menjadi salah satu cara untuk menghasilkan keuntungan. Tidak mengherankan bahwa
banyak orang tertarik dengan game ini.
Hello! I know this is kind of off topic but I was wondering if you knew where I could locate a captcha
plugin for my comment form? I’m using the same blog platform as yours
and I’m having difficulty finding one? Thanks a lot!
Hello, every time i used to check weblog posts here in the early hours
in the break of day, since i like to learn more and more.
Hurrah, that’s what I was searching for, what a stuff!
existing here at this weblog, thanks admin of this site.
I was suggested this blog by my cousin. I’m not sure whether this post is written by
him as no one else know such detailed about my problem.
You are wonderful! Thanks!
Start with these movies to ease your means into
turning into a better author. In different words, you’ll be able to
get up in the morning, brew your self a espresso, sit down at your own desk,
and begin working on your projects.
Aw, this was an exceptionally good post. Taking a few minutes and actual effort to generate a top notch article… but what can I say… I hesitate a lot and never
manage to get anything done.
I’ve been surfing online more than three hours today,
yet I never found any interesting article like yours.
It is pretty worth enough for me. Personally, if all webmasters and bloggers made good content as you did,
the net will be a lot more useful than ever before.
I like the helpful information you provide in your articles.
I’ll bookmark your weblog and check again here frequently. I’m quite certain I’ll learn a lot of new stuff right
here! Best of luck for the next!
Hi there everybody, here eѵery person is sharing ѕuch know-how,
ѕo it’s fastidious tо read this web site, and I սsed to pay ɑ visit tһis webpage alⅼ the timе.
Feel free tо surf to my site: lotto bet
It’s very easy to find out any matter on net as compared to textbooks, as
I found this paragraph at this website.
whoah this blog is wonderful i love reading your articles.
Keep up the great work! You know, a lot of persons are hunting round for this info, you could help them greatly.
I would like to thank you for the efforts you’ve put in writing this site.
I am hoping to see the same high-grade conttent from you in the future as
well.In truth, your creative writing abilities has motivated me to get mmy very ownn ite now 😉
Howdy are using WordPress for your site platform? I’m new to the blog world but
I’m trying to get started and set up my own. Do you
require any coding expertise to make your own blog?
Any help would be greatly appreciated!
You shoulⅾ take paгt in a contest for one of the finest
sites ⲟn the web. I most certaіnly wіll recommend this blog!
Feel free tߋ visit my web site … huay online (Darwin)
Fantastic items from you, man. I’ve consider your stuff previous to and you’re
simply extremely excellent. I really like what you’ve
bought here, certainly like what you’re stating and the best way through which you say it.
You make it enjoyable and you still care for to stay it sensible.
I cant wait to read much more from you. That
is actually a tremendous site.
Are you in need of a trustworthy solution to enhance the life of
your roof? Shingle Magic Roof Sealer is what you need.
This innovative product provides a unique standard of
maintenance for your asphalt shingles, making sure they
remain durable.
With Shingle Magic Roof Sealer, you’re not just applying
any ordinary product. You’re opting for a top-quality roof rejuvenation solution formulated to significantly extend the life of your roof for many years to come.
It’s a smart choice for property owners looking to preserve their investment.
Why choose Shingle Magic Roof Sealer? For starters, its exclusive formula gets into the asphalt shingles, restoring their initial strength and look.
Moreover, the sealer is remarkably simple to use,
requiring no work for top results.
Not only does Shingle Magic Roof Sealer prolong
the life of your roof, but it provides exceptional resistance
to environmental damage. Whether it’s intense UV rays, heavy rain,
or freezing temperatures, it is well-protected.
Additionally, opting for Shingle Magic Roof Sealer means you’re opting for an eco-friendly option. Its safe composition ensures little environmental impact,
making it a thoughtful choice for eco-conscious homeowners.
To sum up, Shingle Magic Roof Sealer excels as the best roof rejuvenation solution. Not
only does it prolong the life of your roof while offering superior protection and an environmentally
friendly option makes it as the wise choice for those looking to care for their property’s future.
Additionally, a significant advantage of Shingle Magic Roof Sealer is its
affordability. In lieu of investing a significant amount on regular repairs or a full roof replacement, using
Shingle Magic saves you money in the long run.
It’s an economical solution that still delivers top-notch results.
Furthermore, the simplicity of its application of Shingle
Magic Roof Sealer is a major plus. You don’t need specialized knowledge to apply it.
For those who like to handle things themselves or opt for expert application, Shingle Magic ensures a smooth process with outstanding
results.
Shingle Magic’s lasting power also serves as a significant reason to
choose it. After application, it creates a protective barrier that preserves the integrity of your shingles for many years.
It means less worry about weather damage and more peace
of mind about the state of your roof.
Regarding visual appeal, Shingle Magic Roof Sealer also stands out.
It not only protects your roof but also
enhances its appearance. Shingles will seem refreshed, thus adding curb appeal and market value to your property.
Customer satisfaction with Shingle Magic Roof Sealer is
further evidence to its quality. Countless customers have seen significant improvements
in their roof’s health after using the product. Feedback underscore
its user-friendliness, longevity, and excellent defensive capabilities.
Finally, selecting Shingle Magic Roof Sealer is selecting a trusted solution for
roof rejuvenation. With its blend of longevity, aesthetic
enhancement, economic efficiency, and ease of application renders
it the perfect choice for homeowners seeking to enhance the life and look of their roof.
Don’t hesitate to transform your roof with Shingle Magic Roof Sealer.
Hello there! Do yoou use Twitter? I’d like to follow you if that would be okay.
I’m undoubtedly enjoying your blog and look
forward to new updates.
My page: Sex Forum
This article offers clear idea in favor of the new users of blogging,
that really how to do running a blog.
Hello, Neat post. There is an issue along with your web site in web explorer,
could check this? IE still is the marketplace chief and a good component
to other folks will omit your magnificent writing due to this problem.
Wonderful, what a web site it is! This weblog presents helpful facts too us, keep
it up.
Hi to every , for the reason that I am truly keen of reading this weblog’s post to be updated daily.
It carries pleasant stuff.
Spot on with this write-up, I truly believe this web site needs a great deal more attention. I’ll probably be returning to read through more, thanks for the info!
This is my first time go to see at here and i am really happy to read all at single place.
Hey there! I could have sworn I’ve been to this site before but after checking through some
of the post I realized it’s new to me. Anyways, I’m definitely glad
I found it and I’ll be book-marking and checking back frequently!
Everyone loves it whenever people get together and share thoughts.
Great website, stick with it!
viagra pokkerx.cHu8vwRgbpvU
I was suggested this blog via my cousin. I’m not positive whether or not this post is written by way of
him as no one else realize such specific about my difficulty.
You’re amazing! Thanks!
craft porn footballxx.wsLcs3JaRB6f
porn mobileidn.KhXYQmP5PggL
It’s a pity you don’t have a donate button! I’d
certainly donate to this excellent blog! I guess for now i’ll settle for bookmarking and
adding your RSS feed to my Google account. I look forward to fresh updates
and will share this website with my Facebook group. Talk soon!
bahis siteleri sikis bingoxx.maYrodcqqbXK
escort siteleri 250tldenemebonusuxx.BsoPDEKeeIxZ
Fantastic post!
Check out: Sex Chat
You could certainly see your skills in the work you write.
The world hopes for more passionate writers such as you who
aren’t afraid to say how they believe. At all times follow your
heart.
Yesterday, while I was at work, my sister stole my iPad and tested to see if
it can survive a 40 foot drop, just so she can be a youtube sensation. My iPad is now broken and she has 83 views.
I know this is completely off topic but I had to share it with someone!
Awesome! Check out:
Online Sex
porno siteleri eyeconartxx.DxfAzzBj3TbL
I am not sure where you’re getting your information, but good topic.
I needs to spend some time learning more or understanding more.
Thanks for wonderful information I was looking
for this info for my mission.
You could definitely see your expertise in the work you write.
The arena hopes for more passionate writers such as you who are not afraid to mention how they believe.
All the time follow your heart.
Thank you for sharing your info. I truly appreciate your efforts
and I will be waiting for your further write ups thank you once again.
mostbet bd – panorama-cdds.com, Bangladesh is
frequently regarded as to be one of the finest poker store in the particular industry.
Excellent goods from you, man. I have keep
in mind your stuff prior to and you’re simply extremely great.
I actually like what you have received right here,
certainly like what you’re saying and the way in which in which you are saying it.
You’re making it entertaining and you still take care of to stay it smart.
I cant wait to learn far more from you. That is really a great website.
Even as you simply click any sports routines, all events
appear at the show display.
Also visit my website: 1xbet
Thanks for sharing your thoughts. I truly appreciate your efforts and I will be waiting
for your further post thank you once again.
Magnificent goods from you, man. I’ve understand your
stuff previous to and you’re just too great. I really like what you’ve acquired here, really like what you’re stating and the way in which you say it.
You make it enjoyable and you still care for to keep it sensible.
I can not wait to read far more from you. This is really a tremendous
website.
Hi there just wanted to give you a quick heads up. The text in your content seem to be running
off the screen in Chrome. I’m not sure if this is a format issue or something to do with web browser compatibility but I figured I’d post to
let you know. The design and style look great though!
Hope you get the issue fixed soon. Cheers
Great blog! Do you have any helpful hints for aspiring writers?
I’m hoping to start my own site soon but I’m a little lost on everything.
Would you recommend starting with a free platform like WordPress or go for a paid option? There
are so many options out there that I’m totally confused ..
Any suggestions? Bless you!
It’s really very complicated in this busy life
to listen news on Television, therefore I just use the web
for that purpose, and take the newest information.
I’ve recently started a site, the info you offer on this
website has helped me greatly. Thanks for all of your
time & work.
Wow, that’s what I was searching for, what a information! present
here at this weblog, thanks admin of this web page.
What’s Happening i am new to this, I stumbled upon this
I’ve discovered It positively helpful and it has aided
me out loads. I’m hoping to give a contribution & aid other customers like its helped me.
Great job.
I’m really impressed together with your writing skills as well as with the layout to your blog.
Is this a paid theme or did you modify it your self? Anyway keep up the nice
high quality writing, it is uncommon to see a great weblog
like this one today..
Hello there! Would you mind if I share your blog with my facebook group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Thanks
Great blog right here! Also your site quite a bit up very fast!
What host are you the use of? Can I get your associate
hyperlink on your host? I wish my site loaded up as quickly
as yours lol
Asking questions are genuinely fastidious thing if you are not understanding anything completely, however this article presents nice understanding even.
Hi there! Do you know if they make any plugins
to safeguard against hackers? I’m kinda paranoid about losing everything I’ve
worked hard on. Any suggestions?
What’s Happening i’m new to this, I stumbled upon this I’ve
found It absolutely helpful and it has helped me out loads.
I am hoping to give a contribution & help different customers like its aided me.
Good job.
my web-site :: http://top.wroclawski.wroclaw.pl
Good site you’ve got here.. It’s hard to find quality
writing like yours these days. I honestly appreciate people like
you! Take care!!
Enhance Your Workspace with Freedman’s Office Chairs in Fort Lauderdale
**Experience Unmatched Comfort with Freedman’s Ergonomic Office Chairs**
Freedman’s Office Furniture, situated at 515 E Las Olas Blvd Suite 120, Fort Lauderdale, FL 33301, brings you a premium selection of
ergonomic office chairs designed to elevate your comfort and productivity.
Serving neighborhoods like Colee Hammock and Central
Beach, Freedman’s is committed to providing top-notch seating solutions for your workplace.
**Embracing Comfort and Style in Fort Lauderdale**
Founded in 1911, Fort Lauderdale boasts a rich history and a population of 181,668 as
of 2021. With 80,031 households, the city thrives as a hub of business and leisure.
Connected by the bustling I-75 highway, Fort Lauderdale is a vibrant city known for
its stunning beaches and diverse cultural scene.
**Seating Solutions Tailored to Fort Lauderdale’s Dynamic Environment**
Just like Fort Lauderdale’s varied landscape, Freedman’s
ergonomic office chairs offer versatility and adaptability.
Whether you’re working in the bustling streets of Central Fort Lauderdale or the serene neighborhoods of
Beverly Heights, our chairs provide the perfect blend of support
and style to complement your workspace.
**Affordable Repairs and Climate-Adaptive Office Chairs**
Freedman’s understands the importance of a comfortable
workspace. That’s why we offer affordable repair services for our ergonomic office
chairs in Fort Lauderdale. Crafted to withstand the
city’s varying temperatures, our chairs ensure year-round comfort and
support for all your professional endeavors.
**Exploring Fort Lauderdale’s Unique Points of Interest**
Discover the charm of Fort Lauderdale with these notable attractions:
– **Anglin’s Fishing Pier:** A historic landmark offering scenic views and excellent fishing opportunities.
– **Bonnet House Museum & Gardens:** Immerse yourself in art, history,
and nature at this exquisite estate.
– **Dr. Von D. Mizell-Eula Johnson State Park:** Explore mangrove swamps, beaches, and hiking
trails in this coastal paradise.
– **El Prado Park:** A serene green space perfect for
picnics and outdoor relaxation.
– **Esplanade Park:** Enjoy events and concerts in this lively park
along the New River.
**Why Choose Freedman’s for Your Office Furniture Needs in Fort Lauderdale**
Opting for Freedman’s ergonomic office chairs means choosing unparalleled comfort, innovative design,
and durability tailored to Fort Lauderdale’s dynamic environment.
Upgrade your workspace with Freedman’s, where each chair represents the perfect balance
of support, style, and functionality, ensuring a productive and
comfortable workday in Fort Lauderdale.
Howdy this is kinda of off topic but I was wanting to know if blogs use
WYSIWYG editors or if you have to manually code with HTML.
I’m starting a blog soon but have no coding skills so I wanted
to get guidance from someone with experience.
Any help would be enormously appreciated!
I really love your site.. Very nice colors & theme.
Did you create this website yourself? Please reply back as I’m
planning to create my own website and want to find out where you got this from or exactly what the
theme is named. Many thanks!
No matter if some one searches for his necessary thing,
therefore he/she wishes to be available that in detail, therefore that thing is
maintained over here.
HF
After going over a number of the blog posts on your web page, I really like
your technique of writing a blog. I saved as a favorite
it to my bookmark website list and will be checking back soon. Please visit my website as well and let me know your opinion.
I got this web site from my buddy who shared with me concerning this site and
at the moment this time I am visiting this site and reading very informative
articles or reviews at this time.
Die Struktur des Artikels ist wirklich angenehm. Ich freue mich darauf, mehr von Ihnen zu lesen. Danke für Ihren informativen Beitrag!
You really make it seem so easy with your presentation but I find this topic to
be really something that I think I would never understand.
It seems too complicated and extremely broad for me.
I am looking forward for your next post, I’ll try to get
the hang of it!
It’s enormous that you are getting thoughts from this paragraph as well as
from our discussion made here.
Wonderful post however , I was wanting to know if you could
write a litte more on this subject? I’d be very thankful if
you could elaborate a little bit more. Bless you!
my homepage … http://new.elblaski.elblag.pl
When I initially commented Ι appear to have clicked tһе -Notify mе when new
comments are ɑdded- checkbox аnd noᴡ eаch
time a comment is adɗed I gеt 4 emails with thе exact ѕame comment.
Iѕ tһere a way you arе able to remove me from that service?
Ƭhanks!
Herе is my web site … lotto24
This is my first time pay a visit at here and i
am really happy to read all at single place.
Hey! Do you use Twitter? I’d like to follow you if that would be
okay. I’m undoubtedly enjoying your blog and look forward to new
posts.
Unquestionably consider that which you said. Your favourite justification appeared to be on the internet the simplest thing to keep in mind
of. I say to you, I certainly get annoyed even as other
folks consider worries that they just do not recognize about.
You controlled to hit the nail upon the highest and also outlined
out the whole thing with no need side-effects , other
folks can take a signal. Will probably be back to get more.
Thanks
What Makes a Great Essay Writing Service?
linkedin.com
Before diving into our exploration of EssayPro, it’s vital to
comprehend the standards that make an essay composing service attract attention from the remainder:
High quality of Work: A first-class essay writing service must consistently deliver
premium, well-researched, and error-free material.
Prompt Delivery: Meeting target dates is necessary for trainees, so a trusted service needs
to ensure that projects are delivered without delay.
Expert Writers: The business must employ skilled and certified authors capable of taking
care of a variety of topics and topics.
Plagiarism-Free Guarantee: Originality is critical.
A respectable service needs to supply plagiarism-free documents, backed by plagiarism
checks.
Budget Friendly Pricing: Services should provide fair and transparent rates, making their
help easily accessible to students.
Customer Support: Responsive and handy customer assistance is important
to deal with any kind of questions or issues immediately.
I love reading through a post that can make men and women think.
Also, thanks for allowing me to comment!
porno izle vvsetohimalxxvc.yE06mcNXxpx8
Hello Dear, are you truly visiting this web page regularly, if so afterward you will without
doubt take pleasant knowledge.
I’m not that much of a internet reader to be honest but your blogs really nice, keep it up!
I’ll go ahead and bookmark your site to come back in the future.
Cheers
Nach unseren Vulkan Vegas Erfahrungen wird perish Auszahlungsquote immer angegeben.
gгeat ρut uр, ᴠery informative. Ӏ ԝonder wһy the
opposite experts οf this sector Ԁon’t understand this.
Ⲩou must proceed your writing. Ι’m sure, you’ve a
great readers’ base alreaⅾy!
Here is mу web-site :: lotto bet (Willard)
Write more, thats all I have to say. Literally, it seems
as though you relied on the video to make your point.
You definitely know what youre talking about, why waste your intelligence on just posting
videos to your site when you could be giving us something enlightening to read?
I think the admin of this web site is genuinely working hard in support of his web site,
since here every stuff is quality based data.
This is my first time pay a visit at here and i am in fact impressed to read all at one place.
На сайте представлены лучшие игровые автоматы,
разработанные как отечественными, эдак и зарубежными производителями
софта для интернет-казино.
Все представленные игры являются сертифицированными, что гарантирует их беспорочность и надежность.
Для входа на зеркало официального сайта игрока не требуется учреждать дополнительное программное
обеспечение или использовать ВПН, так
что зеркала и официальный сайт имеют общую базу данных.
Использование зеркала позволяет
залпом получить доступ к аккаунту, а игрок может использовать свой обычный логин и пароль.
Компания-оператор казино добавляет слоты, игры и
бонусы, что может ввергнуть к перегрузке
сервера. Основной сайт интернет-казино может быть недоступным по
нескольким причинам. Первая причина –
блокировка провайдера по требованию контролирующих государственных органов.
Вторая – проведение технических работ на сайте.
Для обхода блокировок используются актуальные адреса зеркал официального сайта.
Создание зеркал позволяет любителям азартных развлечений авторизоваться на сайте онлайн-казино и получить бесперебойный доступ к азартным развлечениям в любой момент времени.
пароль для входа в интимный кабинет; Если
игрок ищет животрепещущий адрес зеркала официального сайта онлайн-казино, рекомендуется адресоваться к администрации казино для получения этой информации.
Это связано с тем, что в сети могут возникать мошеннические ресурсы с вредоносными ссылками.
I’ll immediately snatch your rss as I can not find your e-mail subscription hyperlink or newsletter service.
Do you’ve any? Kindly let me recognise in order that I may just subscribe.
Thanks.
Great info. Lucky me I recently found your blog by accident (stumbleupon).
I’ve book-marked it for later!
website with wordpress
Appreciate the recommendation. Will try it out.
Hello! This is my 1st comment here so I just wanted to give a quick shout out and
say I genuinely enjoy reading your articles. Can you recommend any other
blogs/websites/forums that cover the same subjects?
Thanks a ton!
You are so awesome! I do not think I’ve read something like this
before. So wonderful to discover another person with genuine thoughts on this subject
matter. Seriously.. thanks for starting this up. This site is
one thing that is required on the internet, someone with a little originality!
Do you mind if I quote a few of your posts as long as I
provide credit and sources back to your website?
My website is in the exact same niche as yours and my visitors would
truly benefit from some of the information you present here.
Please let me know if this ok with you. Regards!
This is a topic that is near to my heart… Thank you!
Where are your contact details though?
Ιf ʏօu wisһ for to gеt а ցood deal frоm thіs post then yoս һave
to apply sᥙch strategies tο your ԝon web site.
Herе is my blog … sport bet
Fantastic goods from you, man. I’ve understand your stuff previous to and you
are just too great. I really like what you’ve acquired here, certainly like
what you’re stating and the way in which you say it. You make it
entertaining and you still take care of to keep it smart.
I can’t wait to read much more from you. This is actually a tremendous web site.
Компания Садко интернет магазин по продаже сантехники, оборудования и аксессуаров для обустройства ванной комнаты и кухни.
Компания Садко предлагает широкий ассортимент товаров
от ведущих производителей, включая
и многое другое.
Одним из преимуществ сайта является то,
что пользователи могут получить квалифицированную консультацию от
специалистов по выбору сантехники, а также помощь в оформлении заказа и доставки до подъезда.
Компания Садко предлагает различные варианты оплаты
и доставки в партнерстве с надежными транспортными компаниями.
Yes! Finally someone writes about Bocoran Jitu.
you’re tгuly a excellent webmaster. Ꭲhe site loading pace is
incredible. It kind οf feels tһat yօu ɑre ⅾoing ɑny unique trick.
Aⅼso, Ƭhе сontents are masterwork. yⲟu’ѵe done a excellent task іn tһis subject!
Ꮇy site :: gambling (Rachel)
We are a group of volunteers and starting a new scheme in our community.
Your site offered us with valuable information to work on. You’ve done an impressive job and our whole community will
be grateful to you.
If you wish for to improve your experience only keep visiting
this web site and be updated with the most up-to-date news update posted here.
Компания Садко интернет магазин по продаже сантехники,
оборудования и аксессуаров для ванной комнаты и кухни.
Здесь клиенты могут найти широкий ассортимент продукции от ведущих производителей, таких как и многое другое.
Одним из преимуществ сайта является возможность получить квалифицированную
консультацию от специалистов по подбору сантехники, а также помощь в оформлении
заказа и доставки до квартиры.
Компания Садко предлагает различные варианты оплаты и
доставки в партнерстве с надежными транспортными компаниями.
What’s up colleagues, how is the whole thing, and what you would like to say regarding
this post, in my view its really amazing designed
for me.
agentie De Creatie Brasov
Whats up very nice website!! Guy .. Excellent ..
Wonderful .. I’ll bookmark your web site and take the feeds also?
I am happy to search out a lot of helpful info here within the put up, we want work out extra strategies in this regard, thanks for sharing.
. . . . .
Check out my homepage … http://top.radomski.radom.pl
I was recommended this website by means of my cousin. I’m not
positive whether this publish is written by him as nobody else recognise such detailed
about my problem. You’re amazing! Thank you!
My webpage :: http://new.warszawski.waw.pl
I love your blog.. very nice colors & theme. Did you design this website yourself or
did you hire someone to do it for you? Plz reply as I’m looking to construct my own blog
and would like to know where u got this from.
thanks
New cryptocurrencies. Add them to your wallet and contact me: michel710@tutanota.com to receive part of
them for free. Thank you
I have to thank you for the efforts you’ve
put in writing this site. I’m hoping to see the same high-grade content by you later on as well.
In fact, your creative writing abilities has encouraged me to get my own, personal site now 😉
am siteleri tthighereduhryyy.2qMXnW86PLo
Keep this going please, great job!
branding
When someone writes an post he/she maintains the idea of a user in his/her brain that how a
user can know it. So that’s why this post is outstdanding.
Thanks!
Hey just wanted to give you a quick heads up and let you know a few of the images aren’t loading
correctly. I’m not sure why but I think its a linking issue.
I’ve tried it in two different internet browsers and both show the same outcome.
I am now not positive the place you are getting your
info, however great topic. I needs to spend some time studying more or
working out more. Thank you for fantastic information I used
to be looking for this info for my mission.
Great goods from you, man. I’ve understand your stuff previous to and you are
just extremely fantastic. I actually like what
you have acquired here, certainly like what you are saying and the way in which you say
it. You make it entertaining and you still care for to
keep it smart. I cant wait to read much more from you. This is really a terrific website.
Hi there! Do you know if they make any plugins to safeguard against hackers?
I’m kinda paranoid about losing everything I’ve worked hard on. Any recommendations?
Thankfulness to my father who told me about this web site,
this blog is actually awesome.
My blog post :: พิมเสนน้ำ สรรพคุณ
Sweet blog! І fοund it wһile surfing ɑround օn Yahoo News.
Ⅾo yoս һave any tips on how to ɡеt listed іn Yahoo News?
I’ѵe bеen trying foг a whіⅼe bսt I never sеem to get
therе! Τhanks
Feel free tо visit my site :: football betting
Slot
Hiya! I know this is kinda off topic however I’d figured I’d ask.
Would you be interested in trading links or maybe guest writing a blog post or vice-versa?
My blog addresses a lot of the same subjects
as yours and I believe we could greatly benefit from each other.
If you might be interested feel free to shoot me an e-mail.
I look forward to hearing from you! Superb blog by the way!
I want to to thank you for this excellent read!! I certainly enjoyed every bit
of it. I have you book-marked to look at new things you post…
Do you have a spam issue on this site; I also am a blogger, and I was
wondering your situation; we have developed some nice
methods and we are looking to trade solutions with others, please shoot me an email if interested.
Unquestionably consider that that you stated.
Your favorite justification seemed to be at the net the easiest
factor to understand of. I say to you, I definitely get
annoyed at the same time as other people think about issues that they
plainly do not realize about. You managed to hit the nail upon the
highest and also defined out the whole thing without having side effect
, people can take a signal. Will probably be again to get more.
Thank you
Spot on with this write-up, I absolutely feel this site needs far more attention.
I’ll probably be back again to read through more, thanks for the information!
Fantastic! Check out:
livejasmin Cam Sex
Today, I went to the beach with my kids. I found a sea shell and gave it to my 4 year
old daughter and said “You can hear the ocean if you put this to your ear.”
She put the shell to her ear and screamed. There was a hermit
crab inside and it pinched her ear. She never wants to go back!
LoL I know this is entirely off topic but I had to tell someone!
You can use white vinegar to eliminate water residue, and
dirt gathered due to years of weathering.
Wow! After all I got a website from where I know how to actually get
useful facts concerning my study and knowledge.
my web blog: 手機A片
Definitely believe that which you said. Your favorite reason seemed to be at the internet the
simplest thing to consider of. I say to you, I
definitely get irked even as other folks think about issues that they
just don’t realize about. You managed to hit the nail upon the highest and also outlined out
the whole thing with no need side effect , folks could take a signal.
Will likely be again to get more. Thank you
After I initially commented I seem to have clicked on the -Notify me when new comments
are added- checkbox and from now on whenever
a comment is added I receive 4 emails with the exact same comment.
There has to be a means you can remove me from that service?
Many thanks!
Feel free to surf to my blog http://top.stargardzki.stargard.pl
Wonderful blog! I found it while browsing on Yahoo News. Do you
have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Appreciate it
Do you mind if I quote a couple of your posts as long as I provide credit and
sources back to your website? My blog is in the exact same niche as yours and my users would certainly benefit from some of the information you provide here.
Please let me know if this ok with you. Appreciate it!
When someone writes an piece of writing he/she keeps the
thought of a user in his/her brain that how a user can understand it.
Thus that’s why this post is perfect. Thanks!
I could not resist commenting. Exceptionally well written!
Hello there! I know this is somewhat off topic but I was wondering if you knew where I could locate a captcha plugin for
my comment form? I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
Hmm is anyone else having problems with the images on this
blog loading? I’m trying to figure out if its a problem on my
end or if it’s the blog. Any responses would be greatly appreciated.
https://www.basset.net/members/forexpeppers.70277/
What’s up everyone, it’s my first go to see
at this website, and piece of writing is actually fruitful designed for me, keep up posting such
posts.
I really like your blog.. very nice colors & theme. Did you design this website yourself or did you hire someone to do it for you?
Plz reply as I’m looking to design my own blog and would like to know where u got this from.
appreciate it
Thanks for finally writing about > Think Obstructive Sleep Apnea is #NBD?
Here Are Seven Health Conditions Made Worse By Your
Undiagnosed OSA – Delaware Dental Sleep Medicine < Liked it!
Everyone loves it whenever people come together and share thoughts.
Great site, keep it up!
obviously like your website however you have to take a
look at the spelling on several of your posts. Many of
them are rife with spelling problems and I find it very troublesome to inform
the truth on the other hand I’ll definitely come back again.
I think that everything typed was actually very logical.
However, what about this? what if you were to write a awesome headline?
I ain’t suggesting your content isn’t good., however suppose you added a title to maybe grab folk’s attention? I mean Think Obstructive Sleep Apnea is #NBD?
Here Are Seven Health Conditions Made Worse By Your Undiagnosed
OSA – Delaware Dental Sleep Medicine is kinda vanilla. You ought to look at
Yahoo’s home page and note how they create article titles to get people interested.
You might add a related video or a pic or two
to get people excited about everything’ve got to say. Just my opinion, it might make your blog a little bit more interesting.
I was wondering if you ever thought of changing the structure of your website?
Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so people could connect
with it better. Youve got an awful lot of text for only having
1 or 2 images. Maybe you could space it out better?
Excellent weblog here! Also your website quite a bit up very fast!
What host are you the use of? Can I am getting your affiliate hyperlink for your host?
I desire my web site loaded up as quickly as yours lol
Heya i am for the primary time here. I found this board and I to find
It truly helpful & it helped me out a lot. I am hoping
to present one thing back and help others like you aided me.
When someone writes an paragraph he/she maintains the image
of a user in his/her mind that how a user can know it. Therefore that’s
why this paragraph is amazing. Thanks!
Every weekend i used to pay a quick visit this web page, for the
reason that i want enjoyment, as this this website conations actually good
funny data too.
Heya i’m for the first time here. I found this board and
I find It truly useful & it helped me out much.
I hope to give something back and aid others like you helped me.
I always used to read post in news papers but now as I am a user of net therefore from now I am
using net for articles or reviews, thanks to web.
It’s awesome to pay a visit this website
and reading the views of all colleagues regarding this
piece of writing, while I am also keen of getting experience.
I used to be recommended this web site by means of my cousin. I’m not positive whether this publish is written through him as nobody else recognise such
designated about my trouble. You’re amazing! Thanks!
Togel
Togel online telah menjadi permainan yang sangat diminati oleh masyarakat Indonesia
dari generasi ke generasi Situs Togel Selain menyajikan keseruan dan ketegangan dalam bermain, togel juga memberikan peluang besar untuk
mendapatkan keuntungan finansial tanpa harus mengeluarkan modal besar.
Oleh karena itu, tidak mengherankan jika semakin banyak pemain togel yang beralih ke platform online untuk
mengejar keberuntungan mereka.
Hello There. I found your blog using msn. This is a very well
written article. I will make sure to bookmark it and come back
to read more of your useful information. Thanks for the post.
I’ll certainly comeback.
Does your site have a contact page? I’m having a tough
time locating it but, I’d like to shoot you an e-mail. I’ve got some recommendations for your blog you might be interested in hearing.
Either way, great website and I look forward to seeing it grow over time.
porn
Hello! I know this is kind of off topic but I was wondering if you
knew where I could find a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
Greetings from Florida! I’m bored to tears at work so I decided to browse your site on my iphone
during lunch break. I really like the information you present here and can’t wait to take
a look when I get home. I’m surprised at how quick your blog loaded on my mobile ..
I’m not even using WIFI, just 3G .. Anyways, good blog!
There’s certainly a lot to know about this topic.
I love all of the points you made.
You actually make it seem so easy with your presentation but I
find this topic to be actually something which I think I would never understand.
It seems too complex and very broad for me. I’m looking forward for your next post, I’ll try to get the hang of it!
I am really impressed along with your writing skills as neatly as with the structure to your
weblog. Is that this a paid subject or did you customize it yourself?
Anyway keep up the excellent high quality writing, it is rare to see a nice blog
like this one today..
2. Melihat Tabel Pembayaran
I would like to thank you for the efforts you’ve put
in writing this blog. I really hope to see the same high-grade content from you later on as well.
In truth, your creative writing abilities has encouraged me to get my own, personal
blog now 😉
Nice answer back in return of this matter with firm arguments and describing the whole thing regarding that.
Highly energetic blog, I loved that a lot. Will there be a part 2?
Completing a analysis paper requires vital time, particularly for college students juggling multiple assignments or half-time jobs.
Hi! I know this is kinda off topic however I’d figured I’d ask.
Would you be interested in exchanging links or maybe guest authoring a blog article or vice-versa?
My blog goes over a lot of the same topics as yours and I believe we
could greatly benefit from each other. If you might be interested feel free
to send me an e-mail. I look forward to hearing from you!
Fantastic blog by the way!
Thank you for any other informative web site. The place else may just I get that kind of information written in such an ideal approach?
I’ve a project that I’m just now running on, and I have been at the look out for such info.
My family all the time say that I am killing my time here at web, except I
know I am getting experience everyday by reading such
good articles.
What’s up every one, here every one is sharing these knowledge, therefore it’s nice to read this web
site, and I used to pay a quick visit this blog all the time.
always i used to read smaller content which as well clear their motive, and that is also happening
with this piece of writing which I am reading now.
Have you ever thought about publishing an ebook or guest authoring on other blogs?
I have a blog centered on the same subjects you discuss and
would love to have you share some stories/information. I know my audience would enjoy your work.
If you are even remotely interested, feel free to send me an e mail.
my web-site Buy Tapentadol
Hi there, all is going sound here and ofcourse every one is sharing facts,
that’s genuinely fine, keep up writing.
Have you ever thought about including a little bit more than just your articles?
I mean, what you say is fundamental and all.
However just imagine if you added some great visuals or
video clips to give your posts more, “pop”! Your content is excellent but with pics and clips, this
site could definitely be one of the greatest in its niche.
Very good blog!
I have to thank you foor the efforts you’veput in writing this website.
I really hope to see the same high-grade blog posts by you later
on as well. In fact, your creative writing abilities has motivatfed me
to get myy own, personal blog now 😉
Wow that was unusual. I just wrote an extremely long comment but after I clicked submit my comment didn’t appear.
Grrrr… well I’m not writing all that over again. Anyhow, just wanted to say great blog!
Look at my webpage http://new.radomski.radom.pl
WOW just what I was looking for. Came here by searching for slot rajacuan
Banners must constantly be saved rolled up, with the lettering and graphics to the outside.
Wonderful beat ! I would like to apprentice while you amend your website,
how could i subscribe for a blog website? The account aided me a acceptable deal.
I had been tiny bit acquainted of this your broadcast offered bright clear concept
I love it when folks get together and share views.
Great blog, keep it up!
Howdy! Do you know if they make any plugins to help with Search Engine Optimization? I’m trying
to get my blog to rank for some targeted keywords but I’m not seeing very good
success. If you know of any please share. Many thanks!
Alles in allem sind in unserem Online vulkan vegas casino knapp 180
Tischspiele verfügbar.
I’m extremely impressed with your writing skills as well as with the layout on your blog.
Is this a paid theme or did you customize it yourself? Either way
keep up the excellent quality writing, it is rare to see a nice blog like this one today.
This post offers clear idea in favor of the new users of blogging,
that actually how to do running a blog.
Here is my webpage; Fake Ids For roblox
This piece of writing presents clear idea in support of the new viewers of
blogging, that in fact how to do blogging.
Hello! I know this is somewhat off topic but I was wondering if you
knew where I could locate a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having trouble finding one?
Thanks a lot!
Ahaa, its fastidious discussion regarding this
piece of writing here at this webpage, I have read all that, so now me also
commenting at this place.
You could definitely see your skills within the work you write.
The sector hopes for even more passionate writers like you who are not
afraid to say how they believe. Always follow your heart.
Thank you a bunch for sharing this with all folks you really understand what you’re talking approximately!
Bookmarked. Please additionally consult with my site =).
We may have a link alternate arrangement between us
My site … http://top.szczecinski.szczecin.pl
Michael Dwamena is the creator of 3D Printerly, a platform dedicated
to streamlining 3D printing for enthusiasts and experts alike.
Hello There. I found your blog using msn. This is a very
well written article. I’ll make sure to bookmark it and return to read more
of your useful information. Thanks for the post. I will definitely comeback.
Wow! At last I got a webpage from where I be able to actually take valuable facts regarding my study and
knowledge.
Hi there! I could have sworn I’ve been to this website before
but after reading through some of the post I realized it’s new to me.
Anyhow, I’m definitely delighted I found it and I’ll be book-marking
and checking back frequently!
Sweet blog! I found it while surfing around on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Many thanks
I just like the valuable information you supply
on your articles. I’ll bookmark your blog and take a look at once more right here frequently.
I am rather sure I will learn many new stuff
proper here! Good luck for the next!
Great post.
Hey there, You have done an excellent job. I will certainly digg it and personally suggest to my friends.
I’m confident they’ll be benefited from this site.
mostbet bd – allianceguarding.com, Bangladesh
accepts grownup (over 18+) bettors and betters.
Hello, just wanted to tell you, I loved this post. It was inspiring.
Keep on posting!
Good post. I learn something new and challenging on sites I stumbleupon everyday.
It will always be useful to read content from other writers
and practice a little something from their web sites.
Hi there, i read your blog from time to time and i own a similar one and
i was just curious if you get a lot of spam feedback?
If so how do you stop it, any plugin or anything you can recommend?
I get so much lately it’s driving me crazy so any support is very much appreciated.
Hello friends, pleasant article and good urging commented at this place,
I am in fact enjoying by these.
Hi there! This post couldn’t be written any better! Reading through this post reminds me of my previous room
mate! He always kept talking about this. I will forward this post to him.
Fairly certain he will have a good read. Many thanks for sharing!
Keep on working, great job!
My page electronic component test labs
First of all I would like to say awesome blog! I had a quick question in which
I’d like to ask if you don’t mind. I was interested
to find out how you center yourself and clear your head prior to writing.
I’ve had difficulty clearing my mind in getting my ideas out.
I do take pleasure in writing but it just seems like the first 10 to 15 minutes are generally lost simply just trying to figure out how
to begin. Any recommendations or tips? Many thanks!
Hi there everyone, it’s my first visit at this
web page, and post is genuinely fruitful designed for me, keep up posting
these posts.
Bạn là một game thủ đam mê?
Bạn muốn khám phá những tựa game mới
nhất, hot nhất?
Bạn muốn nâng cao kỹ năng và trở thành game thủ chuyên nghiệp?
Cổng thông tin Game chính là nơi dành cho bạn!
Tại đây, bạn có thể:
Tìm kiếm thông tin về tất cả các dòng game: Từ game
online đình đám như Liên Minh Huyền Thoại, Liên Quân Mobile, Genshin Impact đến game offline kinh điển như Half Life, chúng tôi đều có đầy đủ.
Đọc những bài review game chi tiết, khách quan và đầy đủ:
Đội ngũ reviewer của chúng tôi sẽ giúp bạn đánh giá
ưu nhược điểm của từng game, từ đó đưa ra lựa chọn phù hợp nhất.
Tham gia cộng đồng game thủ sôi nổi: Chia sẻ niềm đam mê, học
hỏi kinh nghiệm và kết bạn với những người chơi khác.
Cập nhật những tin tức game mới nhất:
Luôn cập nhật những thông tin mới nhất về các
giải đấu eSports, sự kiện game và những
tựa game sắp ra mắt.
Xem những video gameplay hấp dẫn: Xem những màn chơi đỉnh cao của các game thủ
chuyên nghiệp.
Tải về các phần mềm hỗ trợ chơi game:
Cung cấp các phần mềm cần thiết để tối ưu hóa trải nghiệm chơi game của bạn.
Cổng thông tin Game – Nơi bạn có thể:
Khám phá thế giới game đầy thú vị.
Trải nghiệm những giây phút giải trí tuyệt vời.
Nâng cao kỹ năng và trở thành game thủ
chuyên nghiệp.
Kết nối với cộng đồng game thủ đam mê.
Hãy truy cập trang web của chúng tôi ngay hôm nay
để bắt đầu hành trình chinh phục mọi tựa game!
Cổng thông tin Game – Đồng hành cùng mọi game thủ trên hành trình
chinh phục những đỉnh cao mới!
Ngoài ra, chúng tôi còn cung cấp:
Bí kíp và mẹo chơi game hữu ích:
Giúp bạn nâng cao kỹ năng và chiến thắng
trong mọi trận đấu.
Hướng dẫn cách kiếm tiền từ game:
Chia sẻ những cách thức kiếm tiền online
uy tín dành cho game thủ.
Cơ hội tham gia các giải đấu eSports: Thử sức và khẳng định
bản thân trên đấu trường chuyên nghiệp.
Cổng thông tin Game – Nơi đam mê được kết nối, kỹ năng được
nâng tầm!
Hãy tham gia cùng chúng tôi để khám phá thế giới game đầy sôi động và cùng
nhau chinh phục mọi thử thách!
I am regular reader, how are you everybody? This paragraph posted
at this web site is truly fastidious.
Hi there, I read your new stuff regularly. Your story-telling style is awesome,
keep doing what you’re doing!
If some one wants expert view regarding running a blog afterward i recommend
him/her to pay a quick visit this webpage, Keep up the good work.
It’s amazing in support of me to have a site, which is useful designed for my
know-how. thanks admin
That is really fascinating, You’re an overly skilled blogger.
I’ve joined your rss feed and stay up for in quest of extra of
your magnificent post. Also, I have shared your website in my social networks
DL
Chào mừng bạn đến với Cổng thông tin Game – Thiên đường giải trí cho
mọi game thủ!
Bạn đang tìm kiếm:
Đánh giá chi tiết về các tựa game online và
offline hot nhất?
Hướng dẫn chơi game, mẹo và thủ thuật hữu ích giúp bạn nâng cao
kỹ năng?
Cộng đồng game thủ sôi nổi để chia sẻ niềm đam mê và học hỏi
kinh nghiệm?
Cổng thông tin Game chính là điểm đến lý tưởng dành cho bạn!
Tại đây, bạn có thể:
Tìm kiếm thông tin về tất cả các dòng game: Từ game online đình đám như Liên Minh Huyền Thoại, Liên Quân Mobile, Genshin Impact đến game offline kinh
điển như Half Life, chúng tôi đều có đầy đủ.
Đọc những bài review game chi tiết, khách quan và đầy đủ: Đội ngũ reviewer
của chúng tôi sẽ giúp bạn đánh giá ưu nhược điểm
của từng game, từ đó đưa ra lựa chọn phù hợp nhất.
Tham gia cộng đồng game thủ sôi nổi: Chia sẻ niềm đam mê, học hỏi
kinh nghiệm và kết bạn với những người chơi khác.
Cập nhật những tin tức game mới nhất: Luôn cập nhật những thông tin mới nhất về các giải đấu eSports, sự kiện game và những tựa game sắp ra mắt.
Cổng thông tin Game – Nơi đam mê được kết nối!
Hãy truy cập trang web của chúng tôi ngay hôm nay để khám phá thế giới game đầy thú vị và
trải nghiệm những giây phút giải trí tuyệt vời!
Ngoài ra, chúng tôi còn cung cấp:
Video gameplay hấp dẫn: Xem những màn chơi đỉnh cao của các game
thủ chuyên nghiệp.
Hướng dẫn cài đặt và chơi game: Hỗ trợ
bạn cài đặt và chơi game một cách dễ dàng.
Phần mềm hỗ trợ chơi game: Cung cấp các phần mềm cần thiết
để tối ưu hóa trải nghiệm chơi game của bạn.
Cổng thông tin Game – Đồng hành cùng mọi game thủ
trên hành trình chinh phục những tựa game đỉnh cao!
DUBAI77 merupakan salah satu situs casino dan judi slot online terpopuler bagi para pemain casino dan slot gacor
karena menawarkan berbagai macam permainan judi
casino dan slot online yang lebih mudah dimainkan dan tersedia dalam
banyak jenis.
No matter if some one searches for his required
thing, so he/she desires to be available that in detail, thus that thing is maintained over here.
Very nice post. I just stumbled upon your blog and wished to say that I’ve really enjoyed surfing around your blog posts.
In any case I will be subscribing to your feed and I hope you write again soon!
This piece of writing offers clear idea in support of the new users of blogging, that genuinely how to do running a
blog.
Rather, the material will be cut to the exact size of your sign without completed
side.
I’m impressed, I must say. Seldom do I encounter a blog that’s equally educative and
amusing, and without a doubt, you have hit the nail on the head.
The issue is something that not enough men and women are speaking intelligently
about. Now i’m very happy I stumbled across this during my search for something relating to this.
Hi, after reading this amazing post i am ttoo hppy to share my famkiliarity here with
mates.
My web blog Elektromonter (medium.com)
Hey there! I’m at work browsing your blog from my new apple
iphone! Just wanted to say I love reading through your blog and look forward to all your posts!
Carry on the great work!
It is truly a great and helpful piece of information. I’m satisfied that
you just shared this helpful info with us. Please stay
us up to date like this. Thanks for sharing.
We’re a group of volunteers and starting
a new scheme in our community. Your web site provided us with
valuable info to work on. You have done an impressive job and
our entire community will be grateful to you.
What’s up to every one, it’s in fact a pleasant for me to
go to see this site, it consists of priceless Information.
Prediksi Jeeptoto
I simply could not leave your site prior to suggesting that I actually loved the usual info a person supply
in your guests? Is going to be back steadily to
inspect new posts
Hello there! I could have sworn I’ve been to this site before but after looking at many of the posts I realized it’s new to me.
Anyhow, I’m certainly happy I discovered it and I’ll be book-marking it and checking back often!
We’re a group of volunteers and opening a new scheme in our
community. Your website provided us with valuable information to work on. You have done an impressive job and our entire community will
be thankful to you.
I just couldn’t leave your site prior to suggesting that I actually enjoyed the standard info
an individual supply in your guests? Is gonna be back steadily
in order to investigate cross-check new posts
Keep on working, great job!
Excellent items from you, man. I have take into account your stuff previous to and
you are just extremely wonderful. I actually like
what you have obtained right here, really like what you are stating and the best way during which you say
it. You make it enjoyable and you still take care of to keep it wise.
I cant wait to learn far more from you. This is really a wonderful site.
Howdy, i read your blog from time to time and i own a similar one and i was just curious if you get
a lot of spam feedback? If so how do you reduce it, any plugin or anything you can recommend?
I get so much lately it’s driving me insane so any assistance is very much appreciated.
Thank you for another excellent post. The place
else may anybody get that kind of information in such a perfect
means of writing? I’ve a presentation subsequent week,
and I am on the look for such info.
I couldn’t refrain from commenting. Well written!
This website certainly has all of the information I wanted concerning this subject
and didn’t know who to ask.
Wow! This blog looks just like my old one! It’s on a entirely
different subject but it has pretty much the same layout and
design. Superb choice of colors!
Prediksi Jeeptoto
When some one searches for his necessary thing, therefore he/she needs to be available that in detail, so that thing is maintained over here.
Hi there, I do believe your website may be having
internet browser compatibility problems. Whenever I look at your website in Safari, it looks fine however when opening in IE,
it has some overlapping issues. I merely wanted to give
you a quick heads up! Besides that, wonderful site!
my blog: radiation Checker
Simply want to say your article is as astounding. The clearness
in your post is simply nice and i can assume you are an expert on this subject.
Well with your permission allow me to grab your
feed to keep up to date with forthcoming post.
Thanks a million and please carry on the enjoyable
work.
Whats up are using WordPress for your site platform?
I’m new to the blog world but I’m trying to get started and
create my own. Do you need any coding knowledge to make your own blog?
Any help would be greatly appreciated!
Aw, this was an incredibly good post. Spending some time and
actual effort to produce a very good article… but what can I say… I hesitate a whole
lot and never manage to get anything done.
Neben Live-Chat existiert ebenso der zusätzliche FAQ-Bereich, der vorab different Schwierigkeiten lösen soll, überzeugt die Zocker.
my web blog Vulkan Vegas
My programmer is trying to persuade me to move to
.net from PHP. I have always disliked the idea because of the costs.
But he’s tryiong none the less. I’ve been using WordPress on a number of
websites for about a year and am concerned about switching
to another platform. I have heard very good things
about blogengine.net. Is there a way I can transfer
all my wordpress posts into it? Any help would be really appreciated!
Why viewers still make use of to read news papers when in this technological
globe everything is presented on web?
With havin so much content do you ever run into any issues
of plagorism or copyright infringement? My site has a lot of completely unique content I’ve eother written myself oor
outsourcedd but it loos like a lot of it is popping it up alll
over the web without my permission. Do you know any methods to help reduc content from being ripped
off? I’d certainly appreciate it.
cuándo se puede aplicar el 10 de iva en reformas
Hi it’s me, I am also visiting this website daily, this web page is in fact fastidious
and the visitors are really sharing good thoughts.
Thanks for ones marvelous posting! I quite enjoyed reading
it, you will be a great author. I will make certain to bookmark your blog
and will come back later in life. I want to encourage you continue your great job, have a nice day!
Join the excitement at our Mexican casino platform. With action-packed games and electrifying bonuses, you’ll never want to play anywhere else. caliente mx casino te da mucho.
Everything is very open with a really clear description of the issues.
It was really informative. Your website is very helpful. Many thanks for sharing!
I like the valuable info you provide in your articles.
I will bookmark your blog and check again here frequently.
I’m quite sure I will learn many new stuff right here! Best of luck for the next!
You could certainly see your skills within the article you write.
The world hopes for even more passionate writers like
you who aren’t afraid to mention how they believe.
All the time go after your heart.
Also visit my webpage; trifieldmeter
Hi there would you mind letting me know which webhost you’re using?
I’ve loaded your blog in 3 different web browsers and I must say this blog loads a lot faster then most.
Can you suggest a good hosting provider at a honest
price? Kudos, I appreciate it!
always i used to read smaller articles or reviews that as well clear their motive, and
that is also happening with this post which I am reading at this place.
Good day I am so grateful I found your blog page, I really found you by accident, while
I was looking on Yahoo for something else, Nonetheless I am
here now and would just like to say kudos for a marvelous post and a all round thrilling
blog (I also love the theme/design), I don’t have time
to browse it all at the minute but I have saved it and
also added in your RSS feeds, so when I have time I will be back to read a lot more, Please do keep up the superb jo.
Hey there would you mind stating which blog platform you’re using?
I’m going to start my own blog in the near future but I’m having
a tough time deciding between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your design seems different then most blogs and I’m looking for something completely unique.
P.S Apologies for being off-topic but I had to
ask!
Everything is very open with a clear description of the issues.
It was definitely informative. Your website is useful.
Thank you for sharing!
Pretty section of content. I just stumbled upon your web site and in accession capital to assert that I acquire actually enjoyed account your blog
posts. Any way I will be subscribing to your augment
and even I achievement you access consistently quickly.
Please let me know if you’relooking for a article writer for your blog.
You have some really great articles annd I believe I would be a good
asset. If you ever want to tzke some off thhe load off, I’d really likee
to write some articles for your blog in exchange for
a link bacxk to mine. Please blast me an e-mail if interested.
Regards!
cuando entra en vigor la reforma del subsidio por desempleo
I know this web page presents quality dependent articles and
other information, is there any other website which gives such data in quality?
Greetings! Very helpful advice in this particular article!
It’s the little changes that will make the largest changes.
Thanks for sharing!
It is not my first time to pay a quick visit this website, i am browsing this web page dailly and
get good facts from here all the time.
Play with confidence at our Mexican online casino. With fair play guaranteed and transparent policies, you can trust that every game is as thrilling as the last. mi casino este es tu futuro.
I’m not sure why but this web site is loading very slow for me.
Is anyone else having this problem or is it a issue on my end?
I’ll check back later and see if the problem still exists.
There’s definately a great deal to learn about this subject.
I really like all of the points you’ve made.
I’m extremely inspired along with your writing abilities and
also with the structure for your weblog. Is this a paid theme or did you customize it your self?
Anyway stay up the excellent quality writing, it’s uncommon to
look a great blog like this one these days..
It’s actually a cool and helpful piece of information. I’m glad
that you simply shared this helpful information with us. Please keep us up to date like this.
Thanks for sharing.
I love reading through an article that can make men and women think.
Also, many thanks for permitting me to comment!
It’s a shame you don’t have a donate button! I’d certainly donate to this superb blog!
I suppose for now i’ll settle for bookmarking and adding your RSS
feed to my Google account. I look forward to brand new updates and will share
this site with my Facebook group. Chat soon!
Saya akhir-akhir ini mengeksplorasi berbagai slot online
di Corla188 dan harus saya akui, pengalamannya benar-benar melebihi ekspektasi!
Dengan beragamnya pilihan permainan dan antarmuka yang user-friendly, tidak heran jika Corla188 diklaim sebagai sebuah
situs slot online terbaik. Apa yang paling saya hargai adalah keamanan dan keandalan platform
ini, memberikan rasa aman saat bermain. Plus, bonus dan promosinya sangat menarik, memberikan lebih banyak kesempatan untuk menang.
Bagi siapa saja yang mencari pengalaman bermain slot online yang berkualitas tinggi, saya sangat menyarankan Corla188!
https://www.google.com/maps?cid=7633946833729155395
It’s an remarkable paragraph in support of all the online viewers; they
will obtain advantage from it I am sure.
Incredible points. Great arguments. Keep up the good work.
I was able to find good advice from yohr content.
It’s impressive that you are getting ideas from this piece of writing as well as from our argument made at this time.
Pretty! This has been an extremely wonderful post. Thanks for supplying this info.
Everything posted was very reasonable. However, what about this?
suppose you were to create a awesome post title? I am not suggesting your content isn’t good., however what if you added a title that makes people want more?
I mean Think Obstructive Sleep Apnea is #NBD? Here Are Seven Health Conditions Made
Worse By Your Undiagnosed OSA – Delaware
Dental Sleep Medicine is a little boring. You might peek at Yahoo’s home page and note how they create news headlines to
get viewers to open the links. You might try adding a video or
a related pic or two to get readers excited about what you’ve got
to say. In my opinion, it could make your blog a little livelier.
The Twiggs insulator is unlike the typical dome-shaped insulator
due to its distinctive style.
my website :: https://my.desktopnexus.com/brainresult1
Hi there to all, how is everything, I think every one is getting more
from this web site, and your views are nice in favor of new users.
Peculiar article, totally what I wanted to find.
Its such as you learn my mind! You seem to grasp so much approximately this, such as you wrote the ebook in it or something.
I believe that you can do with some p.c. to power
the message home a bit, but other than that,
this is excellent blog. A fantastic read. I’ll definitely be back.
Of course, before publishing in them, try to know
extra about their rules and regulation with regard to submitting articles slightly
than getting disillusioned in the first stage of publication.
Hi there, I check your blogs daily. Your story-telling style is awesome, keep it up!
Appreciating the dedication you put into your site and detailed information you provide.
It’s great to come across a blog every once in a while
that isn’t the same old rehashed information. Fantastic read!
I’ve saved your site and I’m including your RSS feeds to my Google account.
I think that is one of the such a lot important info for me.
And i am glad studying your article. But want to remark on few
normal things, The web site style is ideal, the
articles is truly excellent : D. Just right task, cheers
I couldn’t refrain from commenting. Very well written!
Hello to every one, the contents present at this site are truly amazing for
people knowledge, well, keep up the nice work fellows.
Depending on the objectives of Bangladeshi newcomers, mostbet az offers
diverse promotions.
Hi I am so glad I found your site, I really found
you by error, while I was looking on Yahoo for something else, Anyhow I am here now and
would just like to say thanks for a incredible post and a all round thrilling blog (I also love the theme/design), I don’t have time to read through it all at the moment but I have bookmarked it and
also added in your RSS feeds, so when I have time I will
be back to read more, Please do keep up the awesome work.
My developer is trying to persuade me to move to .net from PHP.
I have always disliked the idea because of the costs. But he’s tryiong none the less.
I’ve been using WordPress on a number of websites for about a year and
am worried about switching to another platform. I have heard fantastic things about
blogengine.net. Is there a way I can import
all my wordpress posts into it? Any help would be greatly appreciated!
Very nice blog post. I definitely appreciate this website.
Continue the good work!
I really like your blog.. very nice colors & theme.
Did you create this website yourself or did you hire someone to
do it for you? Plz answer back as I’m looking to construct my own blog
and would like to find out where u got this from.
thanks
Для тех, кто не ищет тривиальных решений для интерьера и желает внести свежесть в дизайн помещения, есть отличное решение: печать на обоях.
Фотообои помогут удачно дополнить любое интерьерное решение.
Фотообои уже давно стали массовым продуктом, поэтому в них трудно найти
что-то действительно уникальное, поэтому многие
используют их в качестве альтернативы обычным обоям.
В специализированных мастерских
можно заказать широкоформатная печать казань
печать фотообоев любых дизайнов, расцветок и форматов.
Это позволяет вместо обычных обоев
получить уникальное украшение интерьера.
Поскольку фотообои широко востребованы как в жилых, так и
в офисных помещениях, специализированные компании предлагают услуги
по печати фотообоев как корпоративным, так
и частным лицам.
Hey there this is somewhat of off topic but I was wondering if
blogs use WYSIWYG editors or if you have to manually code with HTML.
I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with experience.
Any help would be enormously appreciated!
Photo Offered The author utilizes this Hemingray glass insulator as a paperweight.
Feel free to visit my web blog – https://www.mapleprimes.com/users/bluesweets07
Bei der Registrierung müssen Sie mögliche Fehler berücksichtigen und” “perish Allgemeinen Geschäftsbedingungen sorgfältig lesen.
my web-site :: vulkan vegas (https://www.sme.rmutt.ac.th/vulkan-vegas-casino-bonus-ohne-einzahlung-25-euro-489)
Good answer back in return of this issue
with genuine arguments and describing the whole thing about that.
Do you have a spam problem on this blog; I also am
a blogger, and I was curious about your situation; we have
developed some nice procedures and we are looking to swap methods with others, why
not shoot me an email if interested.
Hello there! I know this is kinda off topic but I was wondering which blog platform are you
using for this website? I’m getting tired of WordPress because I’ve had issues with hackers and I’m looking at alternatives for another platform.
I would be great if you could point me in the direction of a good platform.
Very shortly this site will be famous amid all
blogging and site-building users, due to it’s nice posts
If you want to increase your familiarity only keep visiting
this web page and be updated with the hottest news
posted here.
Everything is very open with a very clear explanation of the issues.
It was really informative. Your site is very useful.
Thanks for sharing!
Hey superb blog! Does running a blog similar to this require a lot of work?
I’ve no knowledge of programming however I was hoping to start
my own blog soon. Anyhow, should you have any suggestions or tips for new blog owners please share.
I understand this is off topic nevertheless I just had to ask.
Many thanks!
Pretty section of content. I just stumbled upon your site and in accession capital to assert
that I get actually enjoyed account your blog
posts. Any way I will be subscribing to your feeds and even I achievement you access consistently
quickly.
I wanted to thank you for this good read!! I definitely enjoyed every bit of
it. I have got you book-marked to look at new things you post…
Great goods from you, man. I have understand your stuff previous to and you’re just extremely wonderful.
I actually like what you’ve acquired here, really like what you’re saying and
the way in which you say it. You make it enjoyable and you
still take care of to keep it wise. I can not wait to read far more from
you. This is really a wonderful web site.
Thank you for the auspicious writeup. It in reality used to be
a entertainment account it. Glance complicated to more
added agreeable from you! By the way, how could we communicate?
Keep on writing, great job!
Hello there! This blog post couldn’t be written any better!
Going through this post reminds me of my previous roommate!
He constantly kept talking about this. I’ll send this article to him.
Pretty sure he’ll have a very good read. Thanks for sharing!
I know this if off topic but I’m looking into starting my own weblog and was
wondering what all is needed to get set up? I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% sure. Any suggestions or advice would be greatly appreciated.
Cheers
Hello There. I found your weblog using msn. This is a really smartly written article.
I’ll make sure to bookmark it and come back to learn more
of your useful info. Thanks for the post. I will certainly comeback.
Your style is really unique compared to other
people I have read stuff from. Thanks for posting when you have the opportunity, Guess I will just
book mark this web site.
I am regular visitor, how are you everybody? This article posted
at this website is genuinely pleasant.
Hello, I desire to subscribe for this blog to
take newest updates, thus where can i do it please assist.
DUBAI77 merupakan salah satu situs casino dan judi slot online terpopuler bagi para pemain casino dan slot gacor karena menawarkan berbagai macam
permainan judi casino dan slot online yang lebih
mudah dimainkan dan tersedia dalam banyak jenis.
Terrific post however , I was wondering if you could write a
litte more on this topic? I’d be very thankful if you could elaborate a little bit further.
Thanks!
Heya i am for the first time here. I found this board and I
find It really useful & it helped me out a lot.
I hope to give something back and aid others like you helped me.
I am actually pleased to read this webpage posts which consists of tons of
useful data, thanks for providing such information.
It’s in reality a great and useful piece of information. I
am happy that you shared this helpful information with us.
Please stay us up to date like this. Thanks for sharing.
It’s nearly impossible to find knowledgeable people about this
topic, however, you seem like you know what you’re talking about!
Thanks
Appreciation to my father who told me concerning this web site, this weblog
is in fact awesome.
Discover the ultimate companion for intense, unforgettable passionate nights with viagra without a doctor prescription . Revitalize your intimate life and explore new realms.
Hello to every single one, it’s really a fastidious for me to go to see this
site, it contains precious Information.
We’re a gaggle of volunteers and opening a new scheme in our community.
Your website provided us with helpful info to work
on. You have performed a formidable process and our entire community might be thankful to you.
I have read so many articles or reviews regarding the blogger
lovers except this paragraph is in fact a nice article, keep it up.
thor368
My brother suggested I might like this website.
He was entirely right. This post actually made my day. You can not
imagine simply how much time I had spent for this info! Thanks!
Amazing! This blog looks just like my old one! It’s on a entirely different topic but it has
pretty much the same page layout and design. Wonderful choice of colors!
I was recommended this web site by my cousin. I am not sure whether this post is written by him as nobody else
know such detailed about my problem. You’re amazing!
Thanks!
I read this piece of writing completely regarding the difference of latest and
previous technologies, it’s remarkable article.
Your way of describing all in this paragraph is actually fastidious,
every one be able to effortlessly understand it, Thanks a lot.
Hey there! This is kind of off topic but I
need some advice from an established blog. Is it very difficult to set up
your own blog? I’m not very techincal but I can figure things
out pretty quick. I’m thinking about creating my own but I’m not sure where
to begin. Do you have any ideas or suggestions?
Appreciate it
This web site definitely has all the information and facts
I needed about this subject and didn’t know who to ask.
Why users still use to read news papers when in this
technological globe everything is presented on net?
Woah! I’m really digging the template/theme
of this site. It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between superb usability and visual
appeal. I must say you have done a amazing job with this.
Additionally, the blog loads extremely quick for me on Opera.
Outstanding Blog!
There’s definately a great deal to find out about this issue.
I love all of the points you made.
Your means of telling the whole thing in this piece of writing is in fact pleasant, every one be able to
simply be aware of it, Thanks a lot.
Everything is very open with a clear explanation of the
issues. It was truly informative. Your site is useful.
Many thanks for sharing!
Incredible points. Great arguments. Keep up the good effort.
Great blog here! Also your website loads up very
fast! What web host are you using? Can I get your affiliate link to your host?
I wish my web site loaded up as quickly as yours lol
Hello this is kknd of of off topic but I was wondering if blogs use WYSIWYG editors or if yyou have to manually cokde with HTML.
I’m starting a blog soon but have no coding experience so I wanted too get advice
from someone with experience. Any help woulkd be greatly
appreciated!
Visit my website … Ochroniarz
It’s awesome to pay a visit this website and reading the views of all mates
about this article, while I am also eager of getting know-how.
Appreciation to my father who informed me about this weblog,
this website is really remarkable.
With havin so much content do you ever run into any problems of plagorism or copyright infringement?
My site has a lot of unique content I’ve either authored myself
or outsourced but it appears a lot of it is popping
it up all over the web without my agreement.
Do you know any solutions to help protect against content from being stolen? I’d definitely appreciate it.
The Hemingray 45 glass insulator is valued as low as $1 and as higher as $700.
My site https://crawfordowen2.bloggersdelight.dk/2023/11/27/purple-glass-insulators-for-sale/
If you would like to increase your experience only keep visiting this website and be
updated with the most up-to-date information posted here.
Hi, Neat post. There’s an issue with your website in web explorer, would test this?
IE still is the marketplace leader and a huge part of people will pass over
your magnificent writing due to this problem.
Bukmeyker kontoru şəxsi idman növlərini də nəzərdən qaçırmayıb.
My web blog; mostbet az
I think the admin of this web page is really working hard in support of his web site, as here
every data is quality based information.
I am regular visitor, how are you everybody? This piece of
writing posted at this site is truly pleasant.
Hey there! I know this is kinda off topic nevertheless I’d figured I’d ask.
Would you be interested in trading links or maybe guest writing a blog article
or vice-versa? My blog covers a lot of the same subjects as yours
and I believe we could greatly benefit from each
other. If you happen to be interested feel free to
send me an email. I look forward to hearing from you!
Fantastic blog by the way!
Thanks , I’ve just been searching for info approximately this topic for a
while and yours is the greatest I’ve found out so far.
However, what concerning the conclusion? Are you sure about
the source?
I like the valuable information you supply to your articles.
I’ll bookmark your blog and test once more here regularly.
I am relatively sure I’ll be informed lots of new stuff right here!
Best of luck for the following!
Every weekend i used to pay a quick visit this site, for the reason that i wish
for enjoyment, for the reason that this this site conations truly fastidious funny
material too.
Hello my friend! I want to say that this article is amazing, nice written and
include approximately all important infos.
I’d like to see more posts like this .
Hello, this weekend is nice designed for me, for the reason that this
occasion i am reading this fantastic informative post here at my home.
крипто биржи в россии
Hi, Neat post. There is an issue together with your site in web explorer, might check this?
IE nonetheless is the market chief and a good portion of people will
omit your magnificent writing due to this problem.
I’m very pleased to uncover this site. I want to to thank you for your time just for this wonderful read!!
I definitely liked every little bit of it and I
have you bookmarked to see new stuff in your website.
I like the valuable information you provide in your articles.
I’ll bookmark your weblog and check again here frequently.
I am quite sure I’ll learn a lot of new stuff right here!
Best of luck for the next!
Hi there, just became alert to your blog through Google, and found that it’s really informative.
I am going to watch out for brussels. I will be grateful if
you continue this in future. Many people will be benefited from your writing.
Cheers!
This information is priceless. When can I find out more?
Howdy! Do you use Twitter? I’d like to follow you if that
would be okay. I’m definitely enjoying your blog and
look forward to new posts.
Hello, i feel that i saw you visited my website so i came to return the want?.I’m trying to to find issues to enhance my web
site!I guess its good enough to use some of your ideas!!
Greetings! Very useful advice within this article! It is the little changes that produce the largest changes.
Many thanks for sharing!
Hello there, just became aware of your blog through
Google, and found that it is truly informative.
I am gonna watch out for brussels. I will appreciate if you continue this
in future. Many people will be benefited from your writing.
Cheers!
When someone writes an paragraph he/she keeps the
image of a user in his/her mind that how a user can know it.
Thus that’s why this article is outstdanding. Thanks!
I am in fact thankful to the holder of this site who has shared this great paragraph at at this place.
New cryptocurrencies. Add them to your wallet and contact me:
michel710@tutanota.com to receive part of them for free.
Thank you
When I originally commented I appear to have clicked
the -Notify me when new comments are added- checkbox and from now on every time a comment is added I
get 4 emails with the exact same comment. Is there a means you are able to remove me from that
service? Thank you!
Hi there, You have done a great job. I
will certainly digg it and personally recommend to my friends.
I am sure they’ll be benefited from this site.
Very rapidly this web page will be famous among all blog people, due
to it’s fastidious articles or reviews
What’s up to all, since I am in fact keen of reading this weblog’s post to
be updated on a regular basis. It consists of good information.
Its like you read my mind! You seem to know a lot approximately this, like you wrote the e-book
in it or something. I believe that you simply
can do with a few percent to force the message home a bit, but instead of
that, this is great blog. A fantastic read.
I will definitely be back.
Today, while I was at work, my cousin stole my iPad and tested to see if
it can survive a 40 foot drop, just so she
can be a youtube sensation. My iPad is now destroyed and she has
83 views. I know this is totally off topic but I had to share it with someone!
Enhance Your Workspace with Freedman’s Office Chairs in Fort Lauderdale
**Experience Unmatched Comfort with Freedman’s Ergonomic Office
Chairs**
Freedman’s Office Furniture, situated at 515 E Las Olas
Blvd Suite 120, Fort Lauderdale, FL 33301, brings you a premium selection of ergonomic office chairs designed to elevate
your comfort and productivity. Serving neighborhoods like Colee Hammock and Central Beach, Freedman’s is committed to
providing top-notch seating solutions for your workplace.
**Embracing Comfort and Style in Fort Lauderdale**
Founded in 1911, Fort Lauderdale boasts a rich history and a population of 181,
668 as of 2021. With 80,031 households, the city thrives as a
hub of business and leisure. Connected by the bustling I-75 highway, Fort Lauderdale
is a vibrant city known for its stunning beaches and diverse cultural scene.
**Seating Solutions Tailored to Fort Lauderdale’s Dynamic
Environment**
Just like Fort Lauderdale’s varied landscape, Freedman’s ergonomic office
chairs offer versatility and adaptability. Whether you’re working
in the bustling streets of Central Fort Lauderdale or the serene neighborhoods of Beverly
Heights, our chairs provide the perfect blend of support and style to
complement your workspace.
**Affordable Repairs and Climate-Adaptive Office Chairs**
Freedman’s understands the importance of a comfortable workspace.
That’s why we offer affordable repair services for our
ergonomic office chairs in Fort Lauderdale. Crafted to withstand the city’s varying temperatures,
our chairs ensure year-round comfort and support for all your professional
endeavors.
**Exploring Fort Lauderdale’s Unique Points of Interest**
Discover the charm of Fort Lauderdale with these notable attractions:
– **Anglin’s Fishing Pier:** A historic landmark offering scenic views and excellent fishing opportunities.
– **Bonnet House Museum & Gardens:** Immerse yourself
in art, history, and nature at this exquisite estate.
– **Dr. Von D. Mizell-Eula Johnson State Park:**
Explore mangrove swamps, beaches, and hiking trails in this coastal paradise.
– **El Prado Park:** A serene green space perfect
for picnics and outdoor relaxation.
– **Esplanade Park:** Enjoy events and concerts in this lively park along the New River.
**Why Choose Freedman’s for Your Office Furniture Needs in Fort Lauderdale**
Opting for Freedman’s ergonomic office chairs means choosing unparalleled
comfort, innovative design, and durability tailored to Fort Lauderdale’s
dynamic environment. Upgrade your workspace with
Freedman’s, where each chair represents the perfect balance
of support, style, and functionality, ensuring a productive and comfortable workday in Fort Lauderdale.
Useful info. Fortunate me I discovered your website by accident, and I’m stunned
why this accident did not came about earlier! I bookmarked it.
Everything is very open with a clear explanation of the
challenges. It was truly informative. Your website is very useful.
Thank you for sharing!
Just want to say your article is as surprising. The clearness on your post is just spectacular and that
i could think you are a professional in this subject. Fine together with your permission allow me to take hold of your feed to keep updated with coming near near post.
Thank you one million and please carry on the enjoyable work.
What i don’t understood is actually how
you are now not actually a lot more well-favored
than you may be right now. You are very intelligent. You already know thus
considerably in relation to this topic, made me in my opinion consider
it from so many various angles. Its like women and men aren’t fascinated until it
is something to accomplish with Girl gaga! Your individual
stuffs great. At all times care for it up!
Thank you for another great post. Where else could anybody get that type of info in such a perfect method
of writing? I have a presentation next week, and I am at the search for such information.
Great post but I was wanting to know if you could write a litte more on this subject?
I’d be very thankful if you could elaborate a little bit more.
Cheers!
excellent publish, very informative. I ponder why the other specialists of
this sector don’t understand this. You should proceed your writing.
I’m sure, you have a great readers’ base already!
Hmm is anyone else experiencing problems with the pictures on this blog loading?
I’m trying to find out if its a problem on my end or if
it’s the blog. Any responses would be greatly appreciated.
I’ve been browsing online more than 3 hours these days, but I never discovered any attention-grabbing article
like yours. It’s beautiful worth sufficient for me.
Personally, if all site owners and bloggers made excellent content material as
you did, the internet shall be a lot more helpful than ever before.
Кроме того, казино работает круглосуточно, без выходных и праздничных дней, что делает его доступным в любое момент.
Администрация Kent Casino также постаралась построить максимально комфортные ситуация для своих клиентов.
Процедура верификации личности
пользователя является обязательной для всех пользователей.
Проверка личности пользователя осуществляется после регистрации.
Для подтверждения предоставленной личной информации от игрока потребуется послать на
адрес электронной почты администрации интернет-портала сканкопии или фото
соответствующих документов.
Дополнительно игрокам, которые планируют использовать банковскую карту выслать фото своей карты с
двух сторон. Для входа на зеркало
официального сайта игрока не требуется учреждать дополнительное программное
обеспечение или использовать ВПН, этак что зеркала и официальный
сайт имеют общую базу данных.
Использование зеркала позволяет залпом получить
доступ к аккаунту, а игрок может использовать собственный обычный логин
и пароль. Компания-оператор казино добавляет слоты, игры и бонусы, что может ввергнуть
к перегрузке сервера. Прогматик
Плей и многих других провайдеров.
Дополнительно от любителя
азартных развлечений требуется выбрать одну из доступных валют для проведения всех финансовых расчетов.
Nice blog here! Also your website loads up fast!
What web host are you using? Can I get your affiliate link
to your host? I wish my site loaded up as fast as yours lol
I know this if off topic but I’m looking into starting my own weblog and was wondering
what all is required to get setup? I’m assuming having a
blog like yours would cost a pretty penny? I’m not very internet smart
so I’m not 100% certain. Any suggestions or advice would be greatly appreciated.
Cheers
There’s definately a lot to know about this topic.
I love all the points you have made.
Hi, all is going sound here and ofcourse every one is sharing facts, that’s in fact
fine, keep up writing.
I’m really enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more enjoyable for me to come here and visit more often. Did you hire out a designer to create
your theme? Fantastic work!
Your style is unique in comparison too otheг people Ӏ hɑve rwad
stuff frߋm. I appгeciate you for posting when you haѵe the opportunity, Guess I’ll јust bookmark this site.
My blog post: مو
Good day! Do you know if they make any plugins to protect against
hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any tips?
Wonderful beat ! I would like to apprentice while you amend your website, how could i subscribe for a blog web
site? The account helped me a acceptable
deal. I had been a little bit acquainted of this your broadcast offered bright
clear concept
If some one desires expert view regarding blogging after that i recommend him/her to go to see
this blog, Keep up the good work.
I know this site presents quality depending articles or reviews
and other data, is there any other website which provides such data in quality?
In the realm of plumbing services, Preferred Plumbers are a cut above the rest for several key reasons.
Given our extensive experience and dedication to excellence, we’re confident
in stating that we’re the #1 choice when you need a plumber.
Here’s why:
Expertise in a Wide Range of Services
Our team is proficient in numerous plumbing services,
from leak detection and repairing pipes to drain cleaning and faucet installation. Whether you need sewer
line repair or water heater repair, we have the knowledge to address all your plumbing needs.
24/7 Availability
Plumbing emergencies don’t wait for business hours,
and neither do we. Preferred Plumbers is ready to help around the clock to make sure that plumbing emergencies are taken care of immediately,
preventing further issues and getting your peace of mind.
Customer-Centric Approach
At our company, the customer is our foremost concern. We strive
to provide tailored solutions that address your specific needs, ensuring that you’re fully satisfied with our work.
Superior Quality
Quality is never compromised at Preferred Plumbers.
We use top-quality materials and advanced methods to
ensure durable repairs and installations.
Our goal is to deliver services that stand the test of time.
Transparent Pricing
Being aware of the cost of plumbing services upfront is
important, which is why Preferred Plumbers provide straightforward quotes.
You’ll know the cost before we start, with no hidden fees to worry
about.
Fully Licensed and Insured
To protect you, Preferred Plumbers is fully licensed and insured.
This indicates that our work meets the highest industry standards and you’re protected in the event event
of an accident.
Choosing Preferred Plumbers means opting for a team that is dedicated
to excellence. We do more than just repair leaks; we’re your partners in ensuring the integrity of your plumbing system.
Get in touch today and experience why Preferred Plumbers
are the #1 choice when you need a plumber.
I have read so many posts about the blogger lovers but this paragraph is actually
a fastidious post, keep it up.
Terrific work! This is the type of information that should be shared around the
net. Disgrace on the search engines for now
not positioning this post upper! Come on over and talk over
with my website . Thank you =)
Hey! Do you know if they make any plugins to assist with
SEO? I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good success.
If you know of any please share. Cheers!
Outstanding story there. What happened after? Good luck!
Please let me know if you’re looking for a author for your weblog.
You have some really great articles and I think I would be a
good asset. If you ever want to take some of the load off, I’d really
like to write some articles for your blog in exchange for
a link back to mine. Please send me an email if interested.
Many thanks!
Its not my first time to pay a quick visit this web
site, i am browsing this web page dailly and obtain pleasant data from
here everyday.
Thanks for ones marvelous posting! I certainly enjoyed reading it, you will be a great author.I will always bookmark
your blog and will eventually come back very soon. I want to encourage
you continue your great writing, have a nice day!
Togel
It’s wonderful that you are getting thoughts from this paragraph as well as from our argument made at this
time.
http://www.free hd porn video.com gghkyogg.GI8HdYqeHT5
Fantastic goods from you, man. I’ve understand your stuff previous to and you are just too fantastic.
I really like what you’ve acquired here, certainly like what you are saying and the way in which you say it.
You make it enjoyable and you still take care of to keep it wise.
I can’t wait to read much more from you. This is actually a tremendous site.
Hi! This post couldn’t be written any better! Reading through
this post reminds me of my old room mate! He always kept talking about this.
I will forward this post to him. Fairly certain he
will have a good read. Many thanks for sharing!
Hmm is anyone else encountering problems with the pictures on this blog loading?
I’m trying to determine if its a problem on my end or if it’s the
blog. Any feed-back would be greatly appreciated.
Hey there! Quick question that’s totally off topic.
Do you know how to make your site mobile friendly?
My blog looks weird when viewing from my iphone 4.
I’m trying to find a theme or plugin that might be able to
correct this problem. If you have any suggestions, please
share. Cheers!
best hd sex videos ggjennifegg.qZkOcEEh828
Great blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple tweeks would really make my blog stand out.
Please let me know where you got your design. Bless you
I couldn’t resist commenting. Exceptionally well written!
hd sex video download 4k ggjinnysflogg.6PmPwjEECxH
Hi! I know this is kinda off topic but I’d figured I’d ask.
Would you be interested in trading links or maybe guest writing
a blog post or vice-versa? My site goes over a lot of the same subjects as yours and I feel we could greatly benefit from each other.
If you are interested feel free to shoot me
an e-mail. I look forward to hearing from you!
Terrific blog by the way!
Howdy! This article couldn’t be written much better!
Going through this article reminds me of my previous
roommate! He constantly kept preaching about this. I will forward this information to him.
Fairly certain he will have a very good read. Thanks for sharing!
I read this article completely on the topic oof the comparison of hottest and previous technologies, it’s remarkable article.
Also visit my homepage; Massage Forum
Hello I am so happy I found your web site, I really
found you by mistake, while I was searching on Aol for something else, Regardless I am
here now and would just like to say kudos for a incredible post and a all round exciting
blog (I also love the theme/design), I don’t have time to read through it all
at the minute but I have book-marked it and also
included your RSS feeds, so when I have time
I will be back to read more, Please do keep up the excellent job.
Kupulan Nama-Nama Daftar Sitgus Judii Slot Onoine Tepercaya dan Provider Slot88 Slot Gacr
Terupdate dii 2021
Masxih menxari kumpula daftar sius judi sloot online teerpercaya yang fqir play?
Sekkian banyak bandar slot onnline ywng bertebarn di internet pasti membuat anda kebingungan, mana web juci soot onlinee bobafit dan mana yang takk bonaft bsgi
parra pemain. Permainan slot online amat populer dan disukai oleh kalangan masyarakat
Indonesia secara kbusus ddi kota-kota besar. Apalagi ketika menghadapi psndemi yang ttak kunjung habbis ini, orang
– oraqng berbondong-bondong mencari situys jufi sllt online terpercaya 2022 untuuk mengisi waktu luangnya.
Kumpulan dari nama-nama daftar sslot onlinee bertebazran melewati duia online.
Untuik meregistrasikan diri, anda bjsa melaksanakan pencarian melewati google,
acuzn sahabat maupun dari sociazl media berupa Facebook, Instagram daan Twitter.
Tipe game slot ssah dan original daat anda temui meelewati
mahkotaslot sedbagai wwebsite jui lot online terupdate 2021.
Lman slot online uang autentik lazimnya menawatkan game jujdi onliine lainnya
yanng tidak keok menarik, variasi-macam gme judi online lainnya akan kami bahas pada sesi berikutnya.
Sebaggai sorang pennggemar game sloot online gacfor yamg adaa ddi Indonesia, mungkiin anda udah taak asng tentang permainan slot erta provider sslot online yang kami sediakan. Bahkan, anda mungkin sudah mendafarkan dir
ddi website lai melainkann merasa kurang nyaman baik dafi
seegi pelayanan ataupun dari seti kemmenangan yang didapat.
Ada beberapa website judi skot onlpine tdnar daan populer ddan kami di sin adir memberikan rekomendasi permaqinan web udi soot online gacor slot88 ternama dentan deretan keuntumgan dalam hhal blnus jackpot slolt yang mudsah menang.
Kemudahan yang diperokleh karena perkembangan twknologi iazlah anda bisa memainkannya dirumah, kantor, aataupun daerah nongkrong bermodalkan tlepon selkuler serta dunia oline saja.
my page; slot deposit dana
Asking questions are in fact good thing if you are not understanding something
fully, however this article offers nice understanding even.
magnificent submit, very informative. I ponder why the opposite specialists of this sector do not notice
this. You should proceed your writing. I am sure, you’ve a
great readers’ base already!
I just could not depart your website before suggesting that
I actually loved the standard information an individual
supply on your guests? Is gonna be again regularly to check out new posts
Wow! This blog looks just like my old one!
It’s on a entirely different topic but it has pretty much the same page layout and design. Excellent choice of colors!
slot online
Slot
Asking questions are genuinely good thing if you are not understanding anything completely, but this paragraph
offers good understanding yet.
Wow that was odd. I just wrote an very long comment but after I clicked
submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Anyway, just wanted to
say wonderful blog!
I used to be able to find good advice from your blog posts.
Ahaa, its nice dialogue on the topic of this post here at this website, I have read all that, so now me
also commenting at this place.
I could not refrain from commenting. Very well written!
It’s an amazing paragraph for all the online viewers; they will get advantage from it I am sure.
If you desire to take a good deal from this post then you have to
apply such techniques to your won web site.
I know this site provides quality depending content and extra data, is there any other website which
offers these information in quality?
Thank you a bunch for sharing this with all people you
actually know what you are speaking approximately! Bookmarked.
Kindly additionally discuss with my site =).
We will have a hyperlink alternate arrangement among us
We absolutely love your blog and find nearly all
of your post’s to be what precisely I’m looking for.
Would you offer guest writers to write content for yourself?
I wouldn’t mind publishing a post or elaborating on most of the subjects you write regarding here.
Again, awesome weblog!
Someone necessarily help to make significantly articles I might state.
This is the first time I frequented your website page and so
far? I amazed with the research you made to create this
particular put up incredible. Excellent process!
An impressive share! I have just forwarded this onto a co-worker who had been conducting a little homework on this.
And he actually ordered me dinner because I stumbled upon it for him…
lol. So let me reword this…. Thank YOU for the meal!!
But yeah, thanks for spending some time to discuss this subject here on your blog.
I am really delighted to read this website posts which consists of tons of valuable
information, thanks for providing such data.
Computers and gadgets as of late have turn into too relevant that with out this, it
can be onerous to accomplish things and function or carry out your
work. The gadgets and gadgets getting used nowadays are portable already.
Hi there, I enjoy reading through your post.
I like to write a little comment to support you.
Everything is very open with a clear explanation of the issues.
It was definitely informative. Your website is very helpful.
Thanks for sharing!
Howdy! This is my first visit to your blog! We are a team of volunteers and
starting a new project in a community in the same niche.
Your blog provided us useful information to work on.
You have done a marvellous job!
Hi there, I believe your blog might be having internet browser compatibility issues.
When I take a look at your web site in Safari, it looks fine however when opening in I.E.,
it has some overlapping issues. I just wanted to give you a quick heads
up! Besides that, great website!
Howdy would you mind sharing which blog platform you’re working with?
I’m planning to start my own blog soon but I’m having a tough time selecting between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different
then most blogs and I’m looking for something completely unique.
P.S My apologies for getting off-topic but I had to ask!
Amazing blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple adjustements would really make my blog shine.
Please let me know where you got your theme.
Bless you
Howdy! I could have sworn I’ve been to this website before but
after checking through some of the post I realized it’s new
to me. Nonetheless, I’m definitely happy I found it and I’ll be book-marking and checking back often!
I was extremely pleased to uncover this site.
I want to to thank you for your time just for this fantastic read!!
I definitely enjoyed every part of it and I have
you book-marked to see new things on your site.
Howdy! I simply wish to offer you a huge thumbs up for the great info you’ve got right here on this post.
I will be coming back to your blog for more soon.
What’s Happening i am new to this, I stumbled upon this
I’ve found It absolutely useful and it has helped me
out loads. I hope to contribute & help other users like its helped me.
Great job.
I’m not sure where you’re getting your information, but good
topic. I needs to spend some time learning much more or understanding more.
Thanks for great information I was looking for this info for my mission.
Hey there I am so happy I found your blog page, I really found you by error, while I was researching on Askjeeve for
something else, Regardless I am here now and would just like to say thank you for a remarkable post and a all round entertaining blog (I also love the
theme/design), I don’t have time to look over it all at the moment but I have book-marked it and also included your RSS feeds, so when I have
time I will be back to read much more, Please do keep up the fantastic job.
If you would like to get a great deal from this post then you have to apply
such methods to your won website.
This website definitely has all of the information I needed concerning this
subject and didn’t know who to ask.
Aw, this was an extremely good post. Taking the time and actual effort to
generate a very good article… but what can I say… I hesitate a whole lot and don’t seem to get nearly anything done.
I’m curious to find out what blog system you have been using?
I’m having some small security issues with my latest website and
I’d like to find something more risk-free. Do you have any suggestions?
Do you have a spam problem on this website; I also am a blogger, and I was curious about your situation; many of us have developed some nice methods
and we are looking to trade techniques with other folks, why not shoot
me an email if interested.
What’s up, yup this piece of writing is actually nice and I have learned lot of things
from it on the topic of blogging. thanks.
Hi there fantastic blog! Does running a blog like
this require a great deal of work? I have absolutely no knowledge of computer programming but I was hoping
to start my own blog in the near future.
Anyway, should you have any recommendations or techniques for new blog owners please share.
I know this is off topic however I simply had to ask. Kudos!
Woah! I’m really loving the template/theme of this site.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between superb usability and
appearance. I must say you have done a awesome job with
this. Additionally, the blog loads very quick for me on Opera.
Excellent Blog!
This is my first time pay a quick visit at here and i am truly happy to read everthing at alone place.
Hey! Quick question that’s totally off topic.
Do you know how to make your site mobile friendly?
My web site looks weird when viewing from my iphone.
I’m trying to find a theme or plugin that might be able
to resolve this problem. If you have any suggestions,
please share. Thank you!
I just couldn’t depart your site prior to suggesting that I
actually loved the usual info a person provide on your visitors?
Is gonna be back continuously to inspect new posts
I have read so many articles or reviews concerning the blogger lovers except this post is really
a good paragraph, keep it up.
We stumbled over here from a different website and
thought I may as well check things out. I like what
I see so now i am following you. Look forward to looking over your web page for
a second time.
Hi, I do believe this is a great web site. I stumbledupon it 😉 I may return once again since I bookmarked it.
Money and freedom is the greatest way to change, may you be rich
and continue to guide others.
My web page: vulkan vegas; solafide.cz,
Excellent post. I was checking constantly this blog and
I’m inspired! Extremely useful information specifically the closing part 🙂 I deal with such
info much. I was seeking this particular information for
a very long time. Thank you and best of luck.
Thanks for your personal marvelous posting!
I quite enjoyed reading it, you might be a great author.
I will make sure to bookmark your blog and will eventually come back sometime soon. I want to
encourage you to ultimately continue your great posts, have a nice evening!
archive Porn
Definitely believe that that you stated. Your favourite justification seemed to be on the web the easiest factor
to keep in mind of. I say to you, I certainly get annoyed while other folks consider worries that they just do not recognize
about. You controlled to hit the nail upon the
top as neatly as defined out the whole thing with no
need side-effects , folks can take a signal. Will likely be back to get more.
Thanks
Thanks to my father who stated to me about this blog, this
web site is truly amazing.
I think the admin of this web page is truly working hard in support of his web
page, because here every data is quality based
data.
Write more, thats all I have to say. Literally, it seems as though you relied
on the video to make your point. You definitely know what
youre talking about, why throw away your intelligence on just posting videos to your blog when you could be giving us something informative to read?
I am really loving the theme/design of your website. Do you
ever run into any internet browser compatibility issues?
A number of my blog visitors have complained about my website not working correctly in Explorer but looks great in Opera.
Do you have any tips to help fix this issue?
Hi, i read your blog occasionally and i own a similar one and
i was just curious if you get a lot of spam feedback?
If so how do you protect against it, any plugin or anything you can recommend?
I get so much lately it’s driving me insane so any support
is very much appreciated.
Thanks for some other wonderful article. Where else may just anyone get that type
of information in such an ideal means of writing? I have a presentation next week,
and I am on the look for such information.
deepthroat, blowjob, anal, amatureporn, facefuck, baldpussy, asstomouth, assfucking,
bbw, bbc, bigcock, bigass, teenass, teenfuck, bigtits,
titfuck, footjob,thighjob, blackcock, hentai, ecchi, pedophliia, ebony, bigboobs, throatfucking,
hardcore, bdsm, oldandyoung, masturbation, milf, missionary,
nudist, oralsex, orgasm, penetration, pussylicking, teenporn, threesome, whores, bokep, bokepindonesia, bokepterbaru, bokepindonesiaterbaru, bokepterupdate, porno, pornoindonesia,
pornoterbaru, pornoterupdate, xnxx.com, pornhub.com, xvideos.com, redtube.com
Your mode of explaining all in this article is really pleasant, every one
be capable of simply know it, Thanks a lot.
Thanks to my father who stated to me on the topic of this blog, this webpage is genuinely awesome.
DUBAI77 merupakan salah satu situs casino dan judi slot online terpopuler bagi para pemain casino dan slot gacor karena menawarkan berbagai macam permainan judi casino dan slot online yang lebih mudah dimainkan dan tersedia dalam banyak
jenis.
It’s difficult to find knowledgeable people about this subject, however, you sound
like you know what you’re talking about! Thanks
Hello, I wish for to subscribe for this webpage to obtain hottest updates, therefore where can i do it please help.
Then-highschool scholar Stacey recalls that he first learned
of the dying toll when he turned on the radio and heard nationally syndicated columnist Walter Winchell speaking about Donora.
Begin off with the most basic tasks first. Within the laundry room,
begin out with folding, and then transfer to ironing and loading the machine.
After Anthony Davis requested a commerce out of latest Orleans, the Pelicans may’ve gone
in a distinct course at head coach. Le’Veon Bell
determined to take a seat out the 2018 season after the Steelers placed the franchise tag on him for the second 12
months in a row. How a lot does she spend on groceries every year?
Too much publicity might be dangerous to your loved ones, and
may cause problems to the respiratory system. Employees
were paid a full day’s wage for only a few hours of
labor, as a result of too much exposure to
the zinc may make them in poor health.
Hey there! I realize this is kind of off-topic but I had to ask.
Does building a well-established website like yours require
a massive amount work? I’m completely new
to blogging but I do write in my diary everyday. I’d like to
start a blog so I can easily share my own experience
and thoughts online. Please let me know if you have any kind of suggestions or tips for new aspiring bloggers.
Thankyou!
Here is my webpage – https://pornhd.mobi
Great web site you have got here.. It’s difficult to find quality writing like
yours these days. I honestly appreciate individuals like you!
Take care!!
I think this is one of the most significant info for
me. And i’m glad reading your article. But wanna remark on some general
things, The website style is perfect, the articles is really excellent : D.
Good job, cheers
The pharmacodynamics of buy hydroxychloroquine 400 mg reveal hydroxychloroquine’s ability to accumulate in tissues, offering insights into its long-lasting effects in conditions like rheumatoid arthritis and lupus.
I got this web page from my friend who told me on the topic of this site and now
this time I am visiting this website and reading very informative content at
this time.
The other day, while I was at work, my cousin stole my
iPad and tested to see if it can survive a twenty
five foot drop, just so she can be a youtube sensation. My
apple ipad is now destroyed and she has 83 views. I know this is completely off topic but I had to share it with someone!
This is very interesting, You’re a very skilled blogger.
I have joined your feed and look forward to seeking more of
your great post. Also, I’ve shared your site in my social networks!
Thankfulness to my father who informed me гegarding thіѕ webpage, tһis wblog іs in fact amazing.
my blog post … Porn Movies
Hey there! This is my first visit to your blog! We are a collection of volunteers and starting
a new initiative in a community in the same niche.
Your blog provided us valuable information to work on. You have done a extraordinary job!
Nice answers in return of this difficulty with real arguments and explaining all on the topic of that.
I believe this is among the most significant info for me.
And i’m glad reading your article. However wanna statement on few normal
issues, The site taste is ideal, the articles is truly excellent : D.
Excellent job, cheers
I got this web site from my friend who informed me about this site
and now this time I am browsing this site and reading very
informative articles at this time.
Helpful info. Fortunate me I found your web site unintentionally, and I am shocked why this twist of fate didn’t happened in advance!
I bookmarked it.
DUBAI77 merupakan salah satu situs casino dan judi slot online terpopuler bagi
para pemain casino dan slot gacor karena menawarkan berbagai macam permainan judi casino dan slot online
yang lebih mudah dimainkan dan tersedia dalam banyak jenis.
Nice blog here! Also your site loads up fast! What host are you using?
Can I get your affiliate link to your host? I wish my site loaded
up as quickly as yours lol
It’s very simple to find out any topic on net as compared to books, as I found this post at this website. зарубежные сериалы в хорошем HD качестве
Hi there, just became alert to your blog through Google, and found that it’s really informative.
I’m going to watch out for brussels. I will be grateful if you continue this in future.
Many people will be benefited from your writing.
Cheers!
It is appropriate time to make some plans for the future and it’s time to be happy.
I’ve read this post and if I could I wish to suggest you few interesting things or advice.
Perhaps you can write next articles referring to
this article. I desire to read more things about it!
I have to thank you for the efforts you have put in penning this website.
I’m hoping to check out the same high-grade content by you in the future as
well. In fact, your creative writing abilities has encouraged me to get my own, personal site now 😉
BA
I am truly grateful to the owner of this web page who has shared this enormous paragraph at at this
time.
Hello There. I found your blog using msn. This is a very well written article.
I will be sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I’ll certainly return.
Greetings! I’ve been following your weblog for a while now and finally got the bravery to go ahead and
give you a shout out from Lubbock Texas! Just wanted to say keep up the great job!
Way cool! Some extremely valid points! I appreciate you penning
this write-up and also the rest of the website is extremely good.
My brother suggested I might like this web site.
He was entirely right. This post actually made my day.
You can not imagine simply how much time I had spent for this info!
Thanks!
Hi there! Do you know if they make any plugins to protect against hackers?
I’m kinda paranoid about losing everything I’ve
worked hard on. Any suggestions?
It’s an amazing piece of writing in favor of all the online visitors; they will
take advantage from it I am sure.
It’s very straightforward to find out any topic on net as compared to textbooks,
as I found this article at this site.
Why viewers still make use of to read news papers when in this
technological globe the whole thing is available on web?
Today, I went to the beach front with my children. I found a sea shell and gave it to my 4 year old daughter
and said “You can hear the ocean if you put this to your ear.” She placed the shell
to her ear and screamed. There was a hermit crab
inside and it pinched her ear. She never wants to go back!
LoL I know this is entirely off topic but I had to tell someone!
Good post. I am going through a few of these issues as well..
Because the admin of this site is working, no question very soon it will be
well-known, due to its feature contents.
Hello There. I discovered your blog the use of msn. That is a very smartly written article.
I will be sure to bookmark it and return to read more of your useful info.
Thanks for the post. I will definitely return.
Hurrah! Finally I got a website from where I be capable of really obtain useful information concerning my study and knowledge.
Appreciate the recommendation. Let me try it out.
Normally I do not read post on blogs, however I wish to say that this write-up very compelled me to try and
do so! Your writing taste has been surprised me.
Thank you, quite great article.
Thanks for sharing your thoughts about máy nén khí piston. Regards
Excellent article. Keep posting such kind of information on your site.
Im really impressed by your site.
Hi there, You’ve done a fantastic job. I’ll definitely
digg it and in my opinion suggest to my friends. I’m sure they’ll be benefited from this web site.
My developer is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the expenses.
But he’s tryiong none the less. I’ve been using WordPress
on several websites for about a year and am nervous about switching to another platform.
I have heard great things about blogengine.net.
Is there a way I can transfer all my wordpress posts into it?
Any help would be really appreciated!
Welcome on the Secure and trustworthy 24 hour pragmatic play Gacor demo slot web-site.
Simple to Earn On-line Taking part in on the web betting is the most enjoyable action you are able to do in 2023 now.
By selecting to Participate in on the internet betting on quite possibly the most
dependable GACOR SLOT website, you’ll get a number of hundred varieties of intriguing
and worthwhile games. All games manufactured right here come
from the best Formal suppliers. So gamers will
find a number of the finest recreation gives that normally present large and a number of
wins. Your slot device gambling functions are going to be a lot more rigorous, In particular if you
decide to Perform gacor slot equipment game titles.
Some individuals opt to Engage in effortless slot machines so sign up on our
Web site, we can pay all their winnings quickly. The get charge is extremely high
since it has an extremely large RTP price.
Hər gün təzə 1win azerbaycan mallar təzə endirimlərlə sizi sevindirəcəyik.
Hello There. I found your blog using msn. This is a
really well written article. I will make sure to bookmark it and return to read more of your useful information. Thanks for the post.
I’ll definitely comeback.
Keep this going please, great job!
Excellent post. Keep posting such kind of information on your blog.
Im really impressed by your blog.
Hey there, You’ve performed a great job. I’ll definitely digg it and in my view suggest to my friends.
I am confident they will be benefited from this site.
I think the admin of this site is in fact working hard in support of his web site, as here every stuff is
quality based material.
Hey! I know this is somewhat off topic but I was wondering if you knew where
I could get a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
Сталь Маркет – это ваш надежный партнер
в сфере металлопроката. Мы предлагаем широкий выбор металлопродукции от ведущих производителей.
Наша компания гарантирует высококачественные товары, которые
соответствуют всем стандартам и требованиям.
Мы предлагаем следующие виды продажа металлопроката арматуру, двутавровую балку, круглую сталь, квадратную сталь,
стальную полосу, стальной равнополочный уголок,
стальной неравнополочный уголок, горячекатаный
швеллер, стальные горячекатаные листы и стальную проволоку.
Преимущества выбора нашей компании, Сталь Маркет: мы предлагаем
широкий ассортимент металлопроката,
продукция высокого качества, доступные цены, удобную систему оплаты, быструю доставку по всей России и
индивидуальный подход к каждому клиенту.
Wow because this is great job! Congrats and keep it up.
https://www.telewizjaolsztyn.pl
A person essentially lend a hand to make seriously articles
I might state. This is the very first time
I frequented your web page and to this point?
I surprised with the analysis you made to create this actual
publish incredible. Excellent process!
LX
Hmm is anyone else experiencing problems with
the pictures on this blog loading? I’m trying to
figure out if its a problem on my end or if it’s the blog.
Any feedback would be greatly appreciated.
I’m gone to say to my little brother, that he should also pay
a visit this blog on regular basis to obtain updated from
most up-to-date news update.
I am not positive the place you are getting your information, but great topic.
I needs to spend a while learning more or working out more.
Thank you for great info I was looking for this info for my mission.
Do you have a spam issue on this blog; I also am a blogger, and I was
wondering your situation; we have created some nice practices and we are looking to exchange
strategies with other folks, be sure to shoot me an email if interested.
Greetings! I know this is kind of off topic but I was wondering if you knew where I could locate a captcha plugin for
my comment form? I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
You have made some good points there. I checked on the web to find out more about
the issue and found most people will go along with your views on this
site.
I’ve been exploring for a bit for any high-quality articles or blog posts in this kind of house .
Exploring in Yahoo I at last stumbled upon this site.
Reading this info So i’m glad to express that I have a very just right uncanny feeling I came upon exactly what I needed.
I most indubitably will make sure to don?t overlook this website
and give it a look on a relentless basis.
Great post.
Hi, just wanted to mention, I enjoyed this post.
It was inspiring. Keep on posting!
In fact when someone doesn’t be aware of afterward its up to other people that they will help, so here it occurs.
fashionflag full hd porn site fashionflag.K3CdBwcnZSB
Hi! I realize this is sort of off-topic however I had to ask.
Does operating a well-established blog such as yours require a massive amount work?
I’m completely new to writing a blog however I do write in my journal
everyday. I’d like to start a blog so I can easily share my own experience and views online.
Please let me know if you have any kind of ideas
or tips for new aspiring blog owners. Thankyou!
I know this website presents quality depending content and
extra material, is there any other web page which presents these things in quality?
Aw, this was a very nice post. Taking the time and actual effort to generate a very good article… but what
can I say… I put things off a whole lot and don’t manage to get nearly anything done.
Great article! This is the kind of info that should be shared around the web.
Shame on Google for now not positioning this put up
upper! Come on over and talk over with my website . Thanks =)
I am truly grateful to the owner of this site who has shared this fantastic post at here.
This info is priceless. How can I find out more?
Really when someone doesn’t be aware of then its up to other visitors that they will assist, so here it occurs.
goodhere Blowjob porn vurucutewet.UiCN2VmlQz1
If you wish for to obtain a good deal from this piece of writing then you have to apply such strategies to your
won website.
ladyandtherose Granny porn backlinkseox.ELLxA7686Ue
I am truly grateful to the owner of this
web site who has shared this fantastic piece of writing
at here.
jenniferroy クンニリングス ポルノの japanesexxporns.luExTAY7LKs
Hey would you mind letting me know which web host you’re using?
I’ve loaded your blog in 3 completely different internet browsers and I must say this blog loads a lot quicker then most.
Can you suggest a good web hosting provider at a honest price?
Kudos, I appreciate it!
I’m really loving the theme/design of your site. Do you ever run into
any browser compatibility problems? A handful of my blog readers have complained about my website not working
correctly in Explorer but looks great in Chrome. Do you have any ideas to help
fix this problem?
Hmm is anyone else experiencing problems with the images on this blog loading?
I’m trying to determine if its a problem on my end or if it’s the blog.
Any responses would be greatly appreciated.
บทความที่น่าตื่นเต้นมากมาย!
ฉันชอบแนวทางที่คุณได้ย้ำถึงความสำคัญของการเลือก
“เว็บแท้ pg” เพื่อประสบการณ์การเล่นเกมที่เหมาะสมที่สุด มันเป็นเรื่องสำคัญที่นักเล่นเกมทุกคนควรจะรู้ เนื่องจากว่าการเล่นในเว็บไซต์ที่มีคุณภาพไม่เพียงแค่ให้โอกาสสำหรับเพื่อการชนะที่ดีขึ้น
แม้กระนั้นยังรวมถึงการเข้าถึงเล่นเกมสล็อตออนไลน์ที่มากมาย,
โบนัสสล็อตที่น่าดึงดูด, แล้วก็โอกาสสำหรับการได้รับฟรีสปินสล็อตด้วย
ข้อคิดเห็นของคุณเกี่ยวกับ “สล็อตฝากถอนไม่มีขั้นต่ำ เว็บตรง” และการหลีกเลี่ยงเว็บผ่านเอเย่นต์ก็เป็นจุดที่ดีมาก ซึ่งเป็นสิ่งที่หลายคนบางทีอาจไม่นึกถึง แม้กระนั้นมันสำคัญมากในการรักษาความโปร่งใสแล้วก็ความมั่นใจในการเล่นเกม
ฉันอยากเพิ่มจากประสบการณ์ส่วนตัวว่าการหา “เว็บตรงไม่ผ่านเอเย่นต์ 2024” และก็ “เกมสล็อตออนไลน์ ได้เงินจริง เครดิตฟรีไหนดี” ไม่เพียงแต่ช่วยให้คุณสามารถเล่นเกมที่คุณชอบได้ แต่ยังช่วยทำให้คุณเจอกับชุมชนของผู้เล่นที่เห็นใจและก็พร้อมแบ่งปันวิธีการเล่นสล็อต รีวิวเกมส์
slot และแม้กระทั่งสูตรชนะสล็อต ซึ่งสามารถเป็นทรัพยากรที่มีค่าเพื่อช่วยให้คุณปรับแก้เกมของคุณ
ขอบคุณอีกครั้งสำหรับบทความที่สุดยอดนี้!
ฉันรอที่จะอ่านเพิ่มจากคุณรวมทั้งตรวจเกมสล็อตใหม่ๆที่คุณชี้แนะ
It’s really very complex in this active life to listen news on TV, so I simply use the web for that
reason, and take the latest information.
landuse Handjob porn lancdcuse.TqHVkaPtFBz
buy ivermectin online, featuring ivermectin, has been explored for its potential use in the treatment of parasitic infections in agricultural crops. Its broad spectrum of activity and safety profile make it a valuable tool for managing plant parasites, supporting crop health and agricultural productivity in farming systems worldwide.
falbobrospizzamadison Celebrity porn jkkıjxxx.azFh5ymeB3X
казино brillx официальный сайт играть
https://brillx-kazino.com
Brillx Казино — это место, где сливаются воедино элегантность и бесконечные возможности. Необычная комбинация азартных игр и роскошной атмосферы позволит вам окунуться в мир бриллиантового веселья. Наше бриллиантовое казино уверенно входит в число лидеров азартной индустрии, и в этом году мы готовы порадовать вас еще большим разнообразием игр и выигрышей.Так что не упустите свой шанс вступить в мир Brillx Казино! Играйте онлайн бесплатно и на деньги в 2023 году, окунувшись в море невероятных эмоций и неожиданных поворотов. Brillx – это не просто игровые аппараты, это источник вдохновения и увлечения. Поднимите ставки и дайте себе шанс на большую победу вместе с нами!
बृहत् मुर्गा अश्लील qqyyooppxx.LbefPqt5ecN
What’s up to every body, it’s my first visit of this
weblog; this weblog contains remarkable and truly fine stuff
in support of readers.
брилкс казино
brillx casino
В 2023 году Brillx предлагает совершенно новые уровни азарта. Мы гордимся тем, что привносим инновации в каждый аспект игрового процесса. Наши разработчики работают над уникальными и захватывающими играми, которые вы не найдете больше нигде. От момента входа на сайт до момента, когда вы выигрываете крупную сумму на наших аппаратах, вы будете окружены неповторимой атмосферой удовольствия и удачи.Играть онлайн бесплатно в игровые аппараты стало еще проще с нашим интуитивно понятным интерфейсом. Просто выберите свой любимый слот и погрузитесь в мир ярких красок и захватывающих приключений. Наши разнообразные бонусы и акции добавят нотку удивительности к вашей игре. К тому же, для тех, кто желает ощутить настоящий азарт, у нас есть возможность играть на деньги. Это шанс попытать удачу и ощутить адреналин, который ищет настоящий игрок.
Cashify helps you Sell phone online at the best prices.
brillx казино
брилкс казино
В 2023 году Brillx Казино стало настоящим оазисом для азартных путешественников. Подарите себе незабываемые моменты радости и азарта. Не упустите свой шанс сорвать куш и стать частью легендарной истории на страницах брилкс казино.Brillx Казино — это место, где сливаются воедино элегантность и бесконечные возможности. Необычная комбинация азартных игр и роскошной атмосферы позволит вам окунуться в мир бриллиантового веселья. Наше бриллиантовое казино уверенно входит в число лидеров азартной индустрии, и в этом году мы готовы порадовать вас еще большим разнообразием игр и выигрышей.
अंतरजातीय अश्लीलता के बारे में बतावल गइल बा hjkvbasdfzxzz.BWINw8kxtuU
Наша компания выдает проф услуги числом бурению скважин сверху воду в С-петербурге и Питерской области. Наша сестра обладаем состоятельным опытом на этой области и еще гарантируем лучшее создавание круглых работ.
Бурение скважин – это надежный и энергоэффективный фотоспособ достатка хозяйственного хозяйства, фирм равным образом организаций невинной а также лучшей водой. Наша команда искусников осуществляет эмпайр скважин многообразной глубины и диаметра, с точки зрения отличительные черты донных вод в течение конкретном регионе – https://burenie-na-vodu-spb.online/luzhsky/nizovo/.
Мы утилизируем прогрессивное ясс равным образом технологические процессы, яко разрешает нам проделывать труда я мухой (а) также безопасно. Наша швырок – снабдить покупателей безопасным и еще устойчивым водоснабжением, которое будет прислуживать долгие годы.
Сверх бурения скважин, автор этих строк также предлагаем хостинг-услуги числом устройству скважинной доктрины: энергоустановка насосов, фильтров, резервуаров (а) также противоположного оборудования для предоставления комфортного использования водой.
We stumbled over here by a different web address
and thought I may as well check things out. I like what I see so i am just following you.
Look forward to looking over your web page yet again.
Benar, game slot online telah menjadi sangat populer dalam beberapa tahun terakhir.
Ini karena kemudahan akses melalui internet dan kemajuan teknologi yang memungkinkan pengembangan permainan yang lebih menarik dan interaktif.
I’m really inspired along with your writing talents and also with
the format for your weblog. Is this a paid theme
or did you customize it yourself? Either way stay up the nice high quality writing,
it’s rare to look a nice weblog like this one nowadays..
My programmer is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the
costs. But he’s tryiong none the less. I’ve been using Movable-type on several websites for
about a year and am anxious about switching to another platform.
I have heard excellent things about blogengine.net.
Is there a way I can import all my wordpress posts into it?
Any kind of help would be greatly appreciated!
Hi there, just became alert to your blog through Google,
and found that it is truly informative. I’m gonna watch out
for brussels. I’ll appreciate if you continue this in future.
Numerous people will be benefited from your writing.
Cheers!
excellent issues altogether, you smply won a logo new reader.
What may you recommend in regards to your submit that you msde a few days in the past?
Any positive?
Also visit mmy web page … 카지노사이트
Every weekend i used to pay a quick visit this web page,
as i wish for enjoyment, since this this web page conations truly pleasant
funny data too.
If some one needs to be updated with most up-to-date technologies therefore he must
be go to see this web page and be up to date everyday.
Every weekend i used to pay a quick visit this site, for the reason that i want enjoyment, for the reason that this this web page conations
in fact good funny stuff too.
Hey I know this is off topic but I was wondering if you knew of any
widgets I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time and was hoping maybe you would have some experience
with something like this. Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward
to your new updates.
I do not even know how I stopped up right here, but
I thought this post was good. I do not understand who you might be but definitely you
are going to a famous blogger when you are
not already. Cheers!
पीओवी पोर्न txechdyzxca.IQN2bA85uhN
I like the valuable information you provide in your articles.
I will bookmark your blog and check again here frequently.
I am quite sure I will learn a lot of new stuff right here!
Best of luck for the next!
Also visit my homepage: situs slot togel
онлайн казино brillx сайт
https://brillx-kazino.com
Добро пожаловать в увлекательный мир азарта и развлечений на официальном сайте Brillx Казино! Если вы ищете захватывающий опыт игры в игровые аппараты, то ваш поиск завершен. Brillx Казино – это не просто блистательный выбор игр, это настоящее путешествие в мир азарта и возможностей.Brillx Казино — это место, где сливаются воедино элегантность и бесконечные возможности. Необычная комбинация азартных игр и роскошной атмосферы позволит вам окунуться в мир бриллиантового веселья. Наше бриллиантовое казино уверенно входит в число лидеров азартной индустрии, и в этом году мы готовы порадовать вас еще большим разнообразием игр и выигрышей.
Excellent, what a website it is! This website provides
valuable data to us, keep it up.
First of all I want to say great blog! I had a quick question which I’d like to ask if
you don’t mind. I was curious to know how you center yourself and clear your thoughts
prior to writing. I’ve had difficulty clearing my mind in getting my thoughts out.
I do take pleasure in writing but it just seems like the first 10 to 15 minutes are lost just trying to figure out how to
begin. Any recommendations or tips? Kudos!
скачать казино brillx
brillx официальный сайт
Вас ждет огромный выбор игровых аппаратов, способных удовлетворить даже самых изысканных игроков. Брилкс Казино знает, как удивить вас каждым спином. Насладитесь блеском и сиянием наших игр, ведь каждый слот — это как бриллиант, который только ждет своего обладателя. Неважно, играете ли вы ради веселья или стремитесь поймать удачу за хвост и выиграть крупный куш, Brillx сделает все возможное, чтобы удовлетворить ваши азартные желания.Ощутите адреналин и азарт настоящей игры вместе с нами. Будьте готовы к захватывающим приключениям и невероятным сюрпризам. Brillx Казино приглашает вас испытать удачу и погрузиться в мир бесконечных возможностей. Не упустите шанс стать частью нашей игровой семьи и почувствовать всю прелесть игры в игровые аппараты в 2023 году!
brillx casino официальный мобильная версия
брилкс казино
Но если вы ищете большее, чем просто весело провести время, Brillx Казино дает вам возможность играть на деньги. Наши игровые аппараты – это не только средство развлечения, но и потенциальный источник невероятных доходов. Бриллкс Казино сотрясает стереотипы и вносит свежий ветер в мир азартных игр.Играя на Brillx Казино, вы можете быть уверены в честности и безопасности своих данных. Мы используем передовые технологии для защиты информации наших игроков, так что вы можете сосредоточиться исключительно на игре и наслаждаться процессом без каких-либо сомнений или опасений.
गर्भवती अश्लीलता hkyonet.8KuoKOHA9aa
İstifadəçi promosyon kodları sayəsində ümumən başqa
bonusları əldə edə biləcək.
Feel free to visit my website – mostbet az
Престижные Дипломы: Купить и Открыть Двери Карьеры http://russdiplomiki.com/kupit-diplom-v-mezhdurechenske.html
My partner and I stumbled over here coming from a different website and thought I might check
things out. I like what I see so now i am following you. Look forward
to looking over your web page yet again.
My brother recommended I might like this web site.
He was totally right. This post truly made my day.
You can not imagine simply how much time I had spent for
this information! Thanks!
I’m extremely impressed with your writing skills and also with the layout on your weblog.
Is this a paid theme or did you customize it yourself?
Anyway keep up the nice quality writing, it is rare to see a great blog like this one nowadays.
Slot Online
Wonderful beat ! I would like to apprentice at the same time as you amend your web site, how can i
subscribe for a blog site? The account aided me a acceptable deal.
I had been tiny bit acquainted of this your broadcast offered vivid clear concept
Hello there! This post could not be written any better!
Reading through this post reminds me of my previous room mate!
He always kept talking about this. I will forward this write-up to him.
Fairly certain he will have a good read. Many thanks for sharing!
Откройте Двери Фортуны:
Гама Казино в Лучшем Свете https://svadbodelov.ru
Hmm is anyone else having problems with the images on this
blog loading? I’m trying to find out if its a problem on my end or if it’s the blog.
Any feed-back would be greatly appreciated.
Hi, I wish for to subscribe for this web site to take newest updates,
therefore where can i do it please help.
Wow, wonderful weblog layout! How lengthy have you ever been running a
blog for? you make blogging glance easy. The overall look of your website is fantastic,
as smartly as the content material!
ਅਸੀਂ ਅਸ਼ਲੀਲ ਹਾਂ madisonivysex.8xlv9K9RuiO
Its like you read my mind! You seem to know a lot about this, like
you wrote the book in it or something. I think that
you can do with some pics to drive the message home a bit, but instead of that, this is fantastic blog.
A fantastic read. I will definitely be back.
It’s very easy to find out any matter on web as compared to books, as I found this paragraph
at this web page.
ladesbet ਹਾਰਡਕੋਰ ਪੋਰਨੋਗ੍ਰਾਫੀ ladesinemi.yI2dG2uUgEY
ladesbet 偽タクシーポルノ ladestinemi.dbRULcGjHk5
Hi to all, it’s actually a pleasant for me to pay a visit this site, it contains
important Information.
obviously like your web site however you need to take a
look at the spelling on several of your posts.
Several of them are rife with spelling problems and I find it very bothersome to tell the truth on the
other hand I’ll surely come back again.
thor368
It’s going to be ending of mine day, except before ending I am reading this impressive article to improve my knowledge.
Hey! I know this is somewhat off topic but I was wondering if you
knew where I could get a captcha plugin for
my comment form? I’m using the same blog platform as yours and I’m having problems finding one?
Thanks a lot!
Marvelous, what a weblog it is! This website provides useful information to us, keep it up.
Hello, I want to subscribe for this blog to take latest updates,
so where can i do it please help out.
Hey there! This is my 1st comment here so I just wanted to give a quick
shout out and tell you I genuinely enjoy reading your articles.
Can you suggest any other blogs/websites/forums that
deal with the same topics? Appreciate it!
Excellent blog! Do you have any helpful hints for
aspiring writers? I’m hoping to start my own site soon but I’m a little lost on everything.
Would you recommend starting with a free platform like WordPress or go for a paid option? There
are so many choices out there that I’m completely overwhelmed ..
Any recommendations? Many thanks!
No mawtter if some one searches for his requieed thing,
thus he/she wishes to be available that in detail, therefore that thing is maintained over here.
Visit my blog post … Arta4d
Hey! Someone in my Myspace group shared this site with us so I
came to give it a look. I’m definitely loving the information.
I’m book-marking and will be tweeting this to my followers!
Wonderful blog and excellent design.
Pretty great post. I simply stumbled upon your weblog and wanted to mention that I have truly loved browsing your blog posts.
In any case I’ll be subscribing in your rss feed and I hope you write again soon!
Hi! I’ve been following your weblog for some time now and finally got the courage to go ahead and give you a shout out from Houston Tx!
Just wanted to say keep up the good job!
What’s up, I check your blogs like every week. Your humoristic
style is awesome, keep it up!
What i don’t understood is if truth be told how you are now not really a lot more
well-appreciated than you might be now. You’re so intelligent.
You already know therefore significantly relating to this
matter, produced me individually believe it from numerous various angles.
Its like men and women are not interested unless it is something to accomplish with Woman gaga!
Your individual stuffs outstanding. Always handle it up!
It is appropriate time to make some plans for the future and it’s time to be happy.
I’ve read this post and if I could I wish to suggest you
some interesting things or tips. Perhaps you can write next articles referring
to this article. I desire to read even more things about it!
Wow! After all I got a weblog from where I know how to in fact get useful facts
regarding my study and knowledge.
This is really interesting, You’re a very skilled blogger.
I’ve joined your feed and look forwarrd tto seesking more of your magnificent post.
Also, I have shared your site in my social networks!
My webpage; wa slot togel
SELAMAT DATANG DI DUBAI77 WEBSITE TERPERCAYA SUDAH BERDIRI SEJAK
2022 di ASIA. Dan saat ini management membangun akses
untuk pencinta BETTING ONLINE di INDONESIA kami demi pelayanan yang jauh lebih baik
dari sebelum nya
I don’t even know how I ended up here, but I thought this post was great.
I don’t know who you are but certainly you’re going to a famous blogger if you
are not already 😉 Cheers!
I am regular visitor, how are you everybody? This article posted
at this site is truly fastidious.
Thanks very nice blog!
Hi there i am kavin, its my first occasion to commenting anywhere, when i read this paragraph i thought i could
also create comment due to this brilliant post.
whoah this blog is great i really like studying your articles.
Keep up the great work! You understand, lots of persons are looking
around for this info, you could help them greatly.
When I initialy commented I clicked the “Notify me when new comments are added” checkbox and
now each time a comment is added I get three e-mails with the
same comment. Is there anyy way you can remlve me from that service?
Bless you!
Feell free to surf to my blog :: praca za granicą dojenie krów
Hey There. I found your blog using msn. This is a really smartly written article.
I will be sure to bookmark it and come back to learn more of your
helpful information. Thank you for the post.
I will definitely return.
This excellent website truly has all the information and facts I needed concerning this subject
and didn’t know who to ask.
Spot on with this write-up, I really believe that this website needs a lot more attention. I’ll probably be
returning to read through more, thanks for the info!
Howdy! I could have sworn I’ve been to your blog
before but after going through a few of the articles I realized it’s new to me.
Nonetheless, I’m definitely pleased I stumbled upon it and I’ll be book-marking it and checking back frequently!
Heya i am for the first time here. I came across this board and I to find
It truly useful & it helped me out a lot. I am hoping to provide one thing back and aid others like you helped me.
I’d like to find out more? I’d care to find out some additional information.
Nice blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple tweeks would
really make my blog stand out. Please let me
know where you got your theme. With thanks
I am sure this paragraph has touched all the internet visitors, its really really
fastidious article on building up new blog.
Hi, i read your blog from time to time and i own a similar one and i was just curious if you get a lot
of spam remarks? If so how do you stop it, any plugin or anything you can recommend?
I get so much lately it’s driving me mad so any
help is very much appreciated.
I’ve read a few good stuff here. Certainly value bookmarking for
revisiting. I wonder how a lot effort you put to make any such fantastic informative web site.
“Onlayn qumar bazarında birincilik onlayn kazinolar və bukmekerlər tərəfindən bölüşdürülür.
Also visit my blog; 1win
If some one wants expert view on the topic of running a blog afterward i propose him/her to
pay a visit this website, Keep up the pleasant job.
Наша команда поддержки готова пособить вам 24
часа в сутки, 7 дней в неделю. Мы предлагаем тонкий степень сервиса, основанный на профессионализме и дружелюбии.
Вход в онлайн казино Kent не лишь открывает
для вас доступ к захватывающим играм
и высокому RTP, да и дает вероятность обратиться к нашей службе поддержки в
любое период. Новым игрокам мы предлагаем приветственный бонус, какой придаст вашему игровому процессу
добавочный весомый стимул.
Зеркало казино Kent обеспечивает надежное подключение к нашему сайту, а
обход блокировки поможет вам выступать
даже в тех регионах, где доступ к онлайн казино ограничен.
Мы ценим каждого нового игрока и предлагаем особенный бонус, чтобы вы смогли
пережить все преимущества игры
в Kent Casino. Получите бонус при первом депозите и начните свое поездка по нашим захватывающим играм с
дополнительными бесплатными средствами!
Kent Online Casino предлагает широкий выбор
игр от ведущих разработчиков, быстрые выплаты выигрышей,
щедрые бонусы и акции для игроков, а
также профессиональную поддержку пользователей.
У нас в Kent Casino мы предлагаем игры с высоким процентом
возврата (RTP). Это означает, что
у вас поглощать больше шансов выиграть и получить свои денежки
назад. Мы тщательно выбираем игры с наилучшими параметрами для наших игроков, дабы любой мог
упиваться азартом и приумножить собственный банкролл.
Hi i am kavin, its my first occasion to commenting anyplace, when i read this piece of
writing i thought i could also create comment due to this sensible piece of writing.
I have read so many content about the blogger lovers however this piece of writing is truly a fastidious piece of writing, keep it
up.
I every time used to read post in news papers but now as I am a user of
web therefore from now I am using net for posts, thanks to web.
Great information. Lucky me I came across your website
by chance (stumbleupon). I have book marked it for later!
This is a really good tip particularly to those fresh to
the blogosphere. Simple but very accurate information… Many thanks for sharing this one.
A must read article!
Woah! I’m really loving the template/theme
of this site. It’s simple, yet effective. A lot of times it’s difficult to get
that “perfect balance” between user friendliness and visual appeal.
I must say that you’ve done a very good job with this.
In addition, the blog loads very quick for me on Safari.
Outstanding Blog!
I don’t know if it’s just me or if everyone else experiencing problems
with your site. It appears as though some of the written text within your posts are running
off the screen. Can somebody else please comment and let me
know if this is happening to them as well? This might be a problem with my internet browser because I’ve had this happen previously.
Thank you
hello!,I like your writing so much! proportion we be in contact extra approximately your post on AOL?
I require a specialist in this area to unravel my problem.
May be that’s you! Taking a look forward to look you.
Greetings! Quick question that’s entirely ooff topic.
Do you know how to make your site mobile friendly? My weblog
looks weird when viewing from my iphone4.I’m trying to find a template
or plugin that might be able to correct tthis issue. If you have any suggestions, please share.
Many thanks!
Feel free to surf to my website 카지노사이트
Good post. I learn something new and challenging on websites I stumbleupon on a daily basis.
It’s always helpful to read through content from other writers and use a little something from other sites.
https://zelpgo.ru
https://mfc-sosnovskoe.ru
Казино с выводом на Киви
Howdy, i read your blog occasionally and i own a similar one and i was
just curious if you get a lot of spam responses?
If so how do you stop it, any plugin or
anything you can advise? I get so much lately it’s driving me crazy
so any support is very much appreciated.
Woah! I’m really digging the template/theme of this blog.
It’s simple, yet effective. A lot of times it’s tough
to get that “perfect balance” between user friendliness and appearance.
I must say that you’ve done a awesome job with this.
Also, the blog loads super fast for me on Safari. Excellent
Blog!
Hi there! I know this is somewhat off topic but I was wondering which blog platform are
you using for this website? I’m getting fed up of WordPress
because I’ve had issues with hackers and I’m looking at alternatives for another platform.
I would be awesome if you could point me in the direction of a good platform.
Hi there Dear, are you actually visiting this web
page on a regular basis, if so then you will absolutely get nice experience.
I am curious to find out what blog platform you happen to be working
with? I’m having some small security issues with my latest site and I would like to find something more safeguarded.
Do you have any recommendations?
Hi there! Would you mind if I share your blog with my
myspace group? There’s a lot of people that I think would really appreciate your content.
Please let me know. Thank you
NJ
Hello, for all time i used to check website posts here in the early hours in the daylight, for the reason that i love to find
out more and more.
Appreciating the commitment you put into your website and
in depth information you present. It’s great to come across a blog every once in a while that isn’t the same old rehashed information. Fantastic
read! I’ve bookmarked your site and I’m including your RSS feeds to my
Google account.
Why viewers still make use of to read news papers when in this technological globe the whole thing is accessible on web?
Hello There. I found your weblog the use of msn. That is an extremely neatly written article.
I’ll be sure to bookmark it and come back to learn extra of your helpful info.
Thanks for the post. I’ll definitely comeback.
Touche. Great arguments. Keep up the amazing work.
These are truly great ideas in on the topic of blogging.
You have touched some nice factors here. Any way keep up wrinting.
PBN sites
We’ll generate a web of private blog network sites!
Merits of our private blog network:
We execute everything so Google DOES NOT realize THAT THIS IS A private blog network!!!
1- We acquire web domains from separate registrars
2- The main site is hosted on a VPS server (Virtual Private Server is fast hosting)
3- The remaining sites are on different hostings
4- We assign a unique Google profile to each site with confirmation in Search Console.
5- We make websites on WordPress, we don’t utilise plugins with assisted by which Trojans penetrate and through which pages on your websites are generated.
6- We never reiterate templates and employ only unique text and pictures
We never work with website design; the client, if desired, can then edit the websites to suit his wishes
This info is invaluable. How can I find out more?
fildena 150
My family all the time say that I am wasting my time here at
net, except I know I am getting familiarity daily by reading such fastidious articles.
I love your blog.. very nice colors & theme. Did you design this website yourself
or did you hire someone to do it for you? Plz respond as I’m looking to create my own blog and would like to find out where u got this
from. cheers
I’m extremely impressed along with your writing talents and also with the format on your
weblog. Is this a paid theme or did you customize it your self?
Anyway keep up the nice quality writing, it is uncommon to see a nice blog like this one
nowadays..
I know this web page presents quality depending posts and additional information, is
there any other web site which offers such information in quality?
Excellent blog here! Also your website loads up fast! What
host are you using? Can I get your affiliate link to your host?
I wish my website loaded up as fast as yours lol
I have been browsing online more than 2 hours today, yet I never found any interesting article like yours.
It’s pretty worth enough for me. Personally, if all web owners and bloggers made good content
as you did, the web will be much more useful than ever
before.
Very good post. I will be going through many of these issues as well..
whoah this weblog is great i really like studying your posts.
Keep up the great work! You recognize, a lot of persons are searching around
for this information, you can aid them greatly.
Hello every one, here every one is sharing such experience, so it’s
fastidious to read this blog, and I used to pay a visit this blog
everyday.
My page … king james translation
Wow, that’s what I was exploring for, what a stuff! existing here at this web site, thanks admin of this web page.
If some one needs expert view on the topic of running a blog after that i advise him/her to
pay a quick visit this webpage, Keep up the fastidious job.
What’s up to every , as I am genuinely eager of reading this weblog’s post to be updated regularly.
It consists of nice stuff.
Do you mind if I quote a couple of your articles as long as I
provide credit and sources back to your blog?
My blog site is in the very same area of interest as yours and my users would genuinely benefit from a
lot of the information you provide here. Please let me know if this okay with you.
Regards!
Undeniably believe that which you said. Your favorite justification appeared
to be on the net the easiest thing to be aware of. I say to you, I
certainly get annoyed while people think about worries that they plainly do not know about.
You managed to hit the nail upon the top as well as defined out
the whole thing without having side effect , people can take a signal.
Will probably be back to get more. Thanks
Hi! This is my first visit to your blog! We are a group of volunteers and starting a new initiative in a community in the same niche.
Your blog provided us useful information to work on. You have
done a wonderful job!
top 10 pharmacies in india http://indiaph24.store/# india online pharmacy
top 10 online pharmacy in india
Right here is the perfect blog for anyone who really wants to find out about this topic.
You realize a whole lot its almost hard to argue with you (not
that I actually would want to…HaHa). You definitely put a new spin on a topic that has been discussed for a long
time. Great stuff, just excellent!
Hi everybody, here every one is sharing such familiarity, therefore it’s pleasant to read
this webpage, and I used to pay a quick visit this
website everyday.
What OTC medications are available for gastroenteritis relief clomid for fertile woman?
obviously like your web site but you have to check the spelling on quite a few of your
posts. Many of them are rife with spelling issues and I
in finding it very bothersome to inform the
reality then again I will certainly come back again.
Brands that manufacture chronometer watches
Understanding COSC Certification and Its Importance in Watchmaking
COSC Accreditation and its Stringent Standards
Controle Officiel Suisse des Chronometres, or the Official Swiss Chronometer Testing Agency, is the authorized Switzerland testing agency that certifies the accuracy and accuracy of wristwatches. COSC accreditation is a mark of excellent craftsmanship and reliability in chronometry. Not all timepiece brands follow COSC accreditation, such as Hublot, which instead adheres to its own demanding standards with mechanisms like the UNICO, reaching equivalent accuracy.
The Art of Exact Timekeeping
The central system of a mechanical timepiece involves the mainspring, which delivers power as it loosens. This system, however, can be prone to external factors that may affect its accuracy. COSC-accredited mechanisms undergo strict testing—over fifteen days in various conditions (five positions, 3 temperatures)—to ensure their resilience and dependability. The tests assess:
Mean daily rate accuracy between -4 and +6 seconds.
Mean variation, highest variation rates, and effects of temperature variations.
Why COSC Certification Matters
For watch enthusiasts and connoisseurs, a COSC-accredited timepiece isn’t just a piece of technology but a testament to lasting quality and precision. It symbolizes a watch that:
Offers exceptional dependability and precision.
Ensures assurance of superiority across the complete design of the timepiece.
Is apt to hold its worth better, making it a sound investment.
Well-known Chronometer Brands
Several well-known manufacturers prioritize COSC validation for their watches, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, offers collections like the Record and Soul, which highlight COSC-accredited movements equipped with advanced substances like silicone balance suspensions to enhance durability and performance.
Historic Background and the Development of Timepieces
The idea of the chronometer originates back to the need for accurate chronometry for navigation at sea, emphasized by John Harrison’s work in the 18th century. Since the formal establishment of COSC in 1973, the certification has become a standard for evaluating the accuracy of luxury watches, maintaining a legacy of excellence in horology.
Conclusion
Owning a COSC-accredited watch is more than an visual selection; it’s a commitment to excellence and precision. For those valuing accuracy above all, the COSC certification offers peace of thoughts, ensuring that each validated timepiece will operate reliably under various conditions. Whether for personal satisfaction or as an investment, COSC-certified watches stand out in the world of horology, maintaining on a legacy of precise timekeeping.
My partner and I absolutely love your blog and find a lot of
your post’s to be exactly what I’m looking for. can you offer guest writers
to write content for yourself? I wouldn’t mind publishing a post or elaborating on most of the subjects you write with
regards to here. Again, awesome website!
線上賭場
It’s amazing for me to have a web page, which is useful in support of my knowledge.
thanks admin
Hello! This post could not be written any better! Reading through this post
reminds me of my good old room mate! He always kept talking about this.
I will forward this page to him. Pretty sure he will have a
good read. Thank you for sharing!
En Son Dönemsel En Beğenilen Bahis Platformu: Casibom
Kumarhane oyunlarını sevenlerin artık duymuş olduğu Casibom, en son dönemde adından genellikle söz ettiren bir bahis ve casino sitesi haline geldi. Ülkemizin en iyi bahis platformlardan biri olarak tanınan Casibom’un haftalık göre değişen erişim adresi, alanında oldukça yeni olmasına rağmen güvenilir ve kazandıran bir platform olarak tanınıyor.
Casibom, yakın rekabeti olanları geride bırakarak köklü casino sitelerinin önüne geçmeyi başarıyor. Bu pazarda uzun soluklu olmak önemli olsa da, katılımcılarla etkileşimde olmak ve onlara ulaşmak da benzer derecede önemlidir. Bu noktada, Casibom’un her saat servis veren canlı destek ekibi ile rahatlıkla iletişime geçilebilir olması önemli bir artı sağlıyor.
Hızla büyüyen oyuncu kitlesi ile dikkat çeken Casibom’un gerisindeki başarı faktörleri arasında, sadece ve yalnızca bahis ve canlı casino oyunlarına sınırlı olmayan kapsamlı bir hizmetler yelpazesi bulunuyor. Spor bahislerinde sunduğu geniş seçenekler ve yüksek oranlar, oyuncuları ilgisini çekmeyi başarıyor.
Ayrıca, hem atletizm bahisleri hem de bahis oyunları katılımcılara yönlendirilen sunulan yüksek yüzdeli avantajlı bonuslar da dikkat çekiyor. Bu nedenle, Casibom hızla sektörde iyi bir reklam başarısı elde ediyor ve büyük bir oyuncuların kitlesi kazanıyor.
Casibom’un kar getiren ödülleri ve tanınırlığı ile birlikte, web sitesine üyelik ne şekilde sağlanır sorusuna da değinmek gerekir. Casibom’a mobil cihazlarınızdan, bilgisayarlarınızdan veya tabletlerinizden internet tarayıcı üzerinden kolayca ulaşılabilir. Ayrıca, web sitesinin mobil uyumlu olması da büyük bir avantaj sunuyor, çünkü artık pratikte herkesin bir akıllı telefonu var ve bu telefonlar üzerinden kolayca ulaşım sağlanabiliyor.
Mobil cep telefonlarınızla bile yolda gerçek zamanlı bahisler alabilir ve maçları canlı olarak izleyebilirsiniz. Ayrıca, Casibom’un mobil cihazlarla uyumlu olması, memleketimizde casino ve oyun gibi yerlerin meşru olarak kapatılmasıyla birlikte bu tür platformlara erişimin büyük bir yolunu oluşturuyor.
Casibom’un emin bir kumarhane platformu olması da gereklidir bir artı getiriyor. Lisanslı bir platform olan Casibom, sürekli bir şekilde eğlence ve kazanç elde etme imkanı sunar.
Casibom’a abone olmak da son derece kolaydır. Herhangi bir belge şartı olmadan ve ücret ödemeden platforma kolaylıkla üye olabilirsiniz. Ayrıca, site üzerinde para yatırma ve çekme işlemleri için de birçok farklı yöntem vardır ve herhangi bir kesim ücreti talep edilmemektedir.
Ancak, Casibom’un güncel giriş adresini takip etmek de elzemdir. Çünkü gerçek zamanlı iddia ve kumarhane siteleri popüler olduğu için sahte siteler ve dolandırıcılar da belirmektedir. Bu nedenle, Casibom’un sosyal medya hesaplarını ve güncel giriş adresini düzenli olarak kontrol etmek önemlidir.
Sonuç, Casibom hem itimat edilir hem de kar getiren bir bahis sitesi olarak dikkat çekiyor. yüksek ödülleri, geniş oyun seçenekleri ve kullanıcı dostu mobil uygulaması ile Casibom, oyun tutkunları için ideal bir platform sağlar.
Amazing things here. I’m very satisfied to peer your article.
Thank you a lot and I’m looking ahead to touch you.
Will you please drop me a e-mail?
We are thrilled to introduce Leadee – a practical extension for accumulating messages through Contact Form 7, Ninja Forms, and WPForms.
How does it work?
If you collect applications on the site, the add-on automatically saves
them and assigns a multitude of valuable data:
1) from which source the client visited the
first time
2) what device was used
3) from which page the submission was made and much more.
As a result, you receive a table with structured
data and can export to .csv or Excel.
Where to download it?
On the leadee.io site or in the WordPress repository at .
How much does it is it?
The extension is at no cost, but you can help it grow into a cool service
with a subscription.
Generally I don’t read post on blogs, but I wish to say that this write-up very pressured me to try and do it!
Your writing style has been amazed me. Thank you, quite great article.
레버리지스탁
로드스탁과 레버리지 스탁: 투자 전략의 참신한 분야
로드스탁을 통해 공급하는 레버리지 스탁은 주식 투자법의 한 방법으로, 높은 수익률을 목표로 하는 투자자들에게 매혹적인 옵션입니다. 레버리지 사용을 사용하는 이 방법은 투자자들이 자신의 투자금을 넘어서는 자금을 투입할 수 있도록 함으로써, 주식 장에서 훨씬 큰 힘을 가질 수 있는 기회를 공급합니다.
레버리지 스탁의 원리
레버리지 스탁은 기본적으로 자금을 빌려 운용하는 방법입니다. 사례를 들어, 100만 원의 투자금으로 1,000만 원 상당의 주식을 사들일 수 있는데, 이는 투자자가 일반적인 투자 금액보다 훨씬 더 많은 주식을 구매하여, 주식 가격이 상승할 경우 관련된 더 큰 수익을 얻을 수 있게 해줍니다. 그러나, 증권 가격이 내려갈 경우에는 그 피해 또한 커질 수 있으므로, 레버리지 사용을 이용할 때는 신중하게 생각해야 합니다.
투자 전략과 레버리지
레버리지 사용은 특히 성장 잠재력이 높은 기업에 적용할 때 유용합니다. 이러한 사업체에 큰 비중으로 적용하면, 잘 될 경우 막대한 이익을 가져올 수 있지만, 그 반대의 경우 큰 리스크도 감수하게 됩니다. 그러므로, 투자자들은 자신의 리스크 관리 능력을 가진 상장 분석을 통해, 어느 기업에 얼마만큼의 자본을 투입할지 결정해야 합니다.
레버리지의 장점과 위험 요소
레버리지 스탁은 큰 수익을 제공하지만, 그만큼 큰 위험도 동반합니다. 증권 장의 변동성은 추정이 곤란하기 때문에, 레버리지를 사용할 때는 언제나 장터 경향을 면밀히 관찰하고, 손해를 최소화하기 위해 수 있는 계획을 세워야 합니다.
최종적으로: 신중한 고르기가 필요
로드스탁에서 제공된 레버리지 스탁은 막강한 투자 도구이며, 잘 활용하면 많은 수익을 벌어들일 수 있습니다. 하지만 높은 리스크도 고려해야 하며, 투자 결정은 충분히 많은 사실과 세심한 판단 후에 이루어져야 합니다. 투자하는 사람의 재정 상황, 위험을 감수하는 능력, 그리고 장터 상황을 생각한 균형 잡힌 투자 방법이 중요합니다.
https://zelpgo.ru
https://zelpgo.ru
Backlinks seo
Potent Backlinks in Weblogs and Remarks: Enhance Your SEO
Backlinks are crucial for improving search engine rankings and enhancing site visibility. By including backlinks into weblogs and remarks wisely, they can significantly increase visitors and SEO overall performance.
Adhering to Search Engine Algorithms
Today’s backlink placement methods are finely adjusted to align with search engine algorithms, which now prioritize link high quality and relevance. This guarantees that backlinks are not just numerous but meaningful, directing users to useful and pertinent content. Website owners should emphasis on incorporating backlinks that are situationally suitable and enhance the overall content material quality.
Rewards of Making use of Clean Contributor Bases
Using up-to-date donor bases for links, like those maintained by Alex, delivers substantial rewards. These bases are frequently refreshed and consist of unmoderated websites that don’t pull in complaints, guaranteeing the links put are both powerful and certified. This method assists in sustaining the efficacy of hyperlinks without the risks associated with moderated or troublesome sources.
Only Sanctioned Sources
All donor sites used are authorized, steering clear of legal pitfalls and sticking to digital marketing requirements. This determination to using only sanctioned resources assures that each backlink is legitimate and trustworthy, thereby developing reliability and trustworthiness in your digital existence.
SEO Impact
Skillfully positioned backlinks in blogs and comments provide more than just SEO benefits—they enhance user encounter by linking to appropriate and high-quality content. This strategy not only meets search engine criteria but also engages consumers, leading to better targeted traffic and enhanced online proposal.
In substance, the right backlink strategy, particularly one that utilizes refreshing and reliable donor bases like Alex’s, can alter your SEO efforts. By focusing on quality over quantity and sticking to the newest standards, you can make sure your backlinks are both potent and productive.
Осмотр Тетер в чистоту: Каким образом обезопасить свои цифровые активы
Все больше пользователей обращают внимание в секурити личных цифровых активов. Каждый день обманщики придумывают новые подходы кражи цифровых средств, и также держатели цифровой валюты являются страдающими своих афер. Один подходов охраны становится проверка кошельков на наличие нелегальных финансов.
С каким намерением это потребуется?
Прежде всего, для того чтобы обезопасить собственные активы против мошенников а также украденных денег. Многие инвесторы сталкиваются с риском утраты личных активов по причине хищных схем или краж. Тестирование кошельков способствует определить подозрительные транзакции или предотвратить потенциальные убытки.
Что мы предлагаем?
Мы предлагаем подход анализа электронных кошельков и также транзакций для выявления начала фондов. Наша система анализирует данные для выявления противозаконных операций и оценки опасности для вашего портфеля. Благодаря данной проверке, вы сможете избегать проблем с регуляторами и также защитить себя от участия в незаконных переводах.
Каким образом это работает?
Мы работаем с передовыми аудиторскими агентствами, вроде Kudelsky Security, для того чтобы гарантировать прецизионность наших проверок. Мы применяем передовые технологии для выявления опасных операций. Ваши данные обрабатываются и сохраняются согласно с высокими стандартами безопасности и приватности.
Как проверить свои Tether на нетронутость?
Если хотите убедиться, что ваша USDT-бумажники чисты, наш сервис обеспечивает бесплатную проверку первых пяти кошельков. Просто введите положение вашего кошелька на на нашем веб-сайте, или наш сервис предоставим вам полную информацию доклад о его положении.
Защитите свои средства сегодня же!
Избегайте риска стать жертвой шарлатанов или попасть в неприятную ситуацию по причине незаконных транзакций. Свяжитесь с нашей команде, для того чтобы сохранить свои криптовалютные финансовые ресурсы и предотвратить затруднений. Сделайте первый шаг к сохранности вашего криптовалютного портфеля уже сейчас!
How can I check if my medication is available through a pharmacy assistance program kamagra priligy?
Осмотр USDT в нетронутость: Каковым способом обезопасить свои цифровые состояния
Все больше людей обращают внимание к безопасность своих цифровых средств. День ото дня шарлатаны придумывают новые способы разграбления цифровых средств, и также собственники криптовалюты оказываются пострадавшими их интриг. Один способов охраны становится проверка бумажников в наличие нелегальных денег.
Для чего это важно?
Прежде всего, для того чтобы защитить свои финансы против мошенников а также похищенных денег. Многие вкладчики встречаются с потенциальной угрозой убытков их финансов из-за мошеннических механизмов или краж. Анализ бумажников помогает определить подозрительные транзакции и предотвратить возможные убытки.
Что мы предлагаем?
Мы предоставляем сервис анализа электронных кошельков и также операций для выявления источника средств. Наша система исследует данные для выявления незаконных операций или оценки опасности для вашего портфеля. За счет этой проверке, вы сможете избегать проблем с регуляторами или защитить себя от участия в незаконных операциях.
Каким образом это работает?
Мы сотрудничаем с передовыми аудиторскими агентствами, например Kudelsky Security, с целью предоставить точность наших проверок. Мы применяем современные технологии для обнаружения рискованных операций. Ваши данные обрабатываются и хранятся в соответствии с высокими стандартами безопасности и приватности.
Каким образом проверить личные Tether в прозрачность?
Если вам нужно убедиться, что ваши USDT-бумажники нетронуты, наш подход обеспечивает бесплатное тестирование первых пяти бумажников. Просто вбейте место личного кошелька на на нашем веб-сайте, и также наша команда предоставим вам детальный доклад об его положении.
Гарантируйте безопасность для свои активы уже сегодня!
Не подвергайте опасности подвергнуться мошенников или попасть в неблагоприятную обстановку по причине нелегальных операций. Обратитесь к нашему агентству, с тем чтобы предохранить ваши криптовалютные активы и предотвратить сложностей. Предпримите первый шаг к безопасности криптовалютного портфеля сегодня!
Как убедиться в чистоте USDT
Анализ кошельков на выявление наличия подозрительных средств: Охрана своего электронного портфельчика
В мире цифровых валют становится все значимее необходимее соблюдать безопасность личных финансов. Ежедневно жулики и хакеры выработывают свежие методы мошенничества и воровства виртуальных денег. Одним из важных инструментов обеспечения является проверка кошельков на наличие подозрительных денег.
Почему же именно поэтому важно, чтобы осмотреть личные электронные кошельки для хранения криптовалюты?
Прежде всего, вот это нужно для того, чтобы защиты своих финансовых средств. Многие пользователи сталкиваются с риском утраты своих финансов по причине непорядочных планов или воровства. Анализ бумажников способствует предотвращению выявить вовремя подозрительные действия и предупредить.
Что предлагает вашему вниманию организация?
Мы предлагаем послугу проверки данных цифровых кошельков для хранения криптовалюты и транзакций средств с задачей выявления места происхождения средств передвижения и предоставления подробного доклада. Компания предлагает платформа анализирует данные для обнаружения потенциально нелегальных манипуляций и оценить риск для того чтобы личного портфеля активов. Благодаря нашей проверке, вы будете способны предотвратить возможные с органами контроля и защитить себя от случайной вовлеченности в финансировании незаконных деятельностей.
Как проводится процесс?
Компания наша организация имеет дело с авторитетными аудиторскими организациями структурами, как например Halborn, для того чтобы гарантировать и правильность наших проверок данных. Мы применяем передовые и техники анализа данных для выявления опасных операций средств. Персональные данные наших клиентов обрабатываются и сохраняются согласно высокими требованиями.
Важный запрос: “проверить свои USDT на чистоту”
В случае если вы хотите убедиться чистоте личных кошельков USDT, наши профессионалы оказывает возможность исследовать бесплатной проверки первых пяти кошельков. Просто введите адрес своего кошелька в соответствующее поле на нашем сайте проверки, и мы вышлем вам детальный отчет о его статусе.
Обезопасьте свои деньги уже сегодня!
Не подвергайте себя риску становиться пострадать криминальных элементов или попасть неприятном положении неправомерных действий с ваших деньгами. Доверьте свои финансы специалистам, которые помогут, вам и вашим деньгам защититься криптовалютные активы и предотвратить возможные проблемы. Предпримите первый шаг безопасности вашего цифрового портфеля в данный момент!
Тетер – является устойчивая цифровая валюта, связанная к национальной валюте, например USD. Это делает ее в частности популярной среди инвесторов, так как данная криптовалюта предлагает стабильность цены в условиях волатильности рынка криптовалют. Однако, также как и любая другая разновидность криптовалюты, USDT подвержена опасности использования в целях скрытия происхождения средств и субсидирования неправомерных операций.
Промывка средств через цифровые валюты превращается все больше и больше распространенным способом с тем чтобы обеспечения анонимности. Используя различные приемы, дельцы могут попытаться легализовывать незаконно добытые средства путем сервисы обмена криптовалют или миксеры, чтобы осуществить происхождение менее очевидным.
Именно в связи с этим, проверка USDT на чистоту оказывается значимой практикой защиты для пользовательской аудитории цифровых валют. Доступны специализированные услуги, какие осуществляют проверку операций и кошельков, чтобы идентифицировать сомнительные транзакции и противоправные финансирование. Эти платформы способствуют участникам устранить непреднамеренной участи в преступных действий и предотвратить блокировку аккаунтов со со стороны надзорных органов.
Анализ USDT на чистоту также как предотвращает защитить себя от финансовых потерь. Владельцы могут быть уверены в том, что их финансовые ресурсы не связаны с нелегальными транзакциями, что соответственно снижает риск блокировки аккаунта или лишения капитала.
Таким образом, в условиях повышающейся сложности среды криптовалют необходимо принимать меры для обеспечения безопасности своих активов. Проверка USDT на чистоту с использованием специализированных услуг представляет собой одним из вариантов предотвращения незаконной деятельности, обеспечивая пользователям цифровых валют дополнительный уровень и защиты.
Проверка USDT на чистоту
Тестирование USDT на чистоту: Каковым способом защитить свои цифровые активы
Все больше индивидуумов обращают внимание к безопасность собственных криптовалютных активов. Ежедневно обманщики предлагают новые способы кражи цифровых средств, а также собственники электронной валюты оказываются жертвами их интриг. Один из подходов охраны становится проверка бумажников на наличие противозаконных финансов.
Для чего это важно?
Преимущественно, для того чтобы защитить свои средства от дельцов и также похищенных денег. Многие участники сталкиваются с потенциальной угрозой потери своих фондов в результате мошеннических планов или грабежей. Анализ кошельков помогает обнаружить непрозрачные операции и предотвратить возможные потери.
Что наша команда предлагаем?
Мы предлагаем услугу проверки цифровых кошельков или операций для выявления источника средств. Наша технология проверяет данные для определения нелегальных действий или оценки угрозы для вашего портфеля. За счет такой проверке, вы сможете избежать проблем с регулированием а также предохранить себя от участия в противозаконных операциях.
Как это работает?
Наша фирма сотрудничаем с лучшими аудиторскими компаниями, например Halborn, с целью предоставить точность наших тестирований. Мы внедряем передовые технологии для определения опасных сделок. Ваши данные обрабатываются и хранятся согласно с высокими стандартами безопасности и конфиденциальности.
Как выявить свои Tether в чистоту?
При наличии желания подтвердить, что ваши USDT-кошельки чисты, наш сервис предлагает бесплатное тестирование первых пяти кошельков. Легко передайте место собственного кошелька на на нашем веб-сайте, и также мы предоставим вам подробный отчет об его положении.
Охраняйте свои средства сегодня же!
Не подвергайте опасности попасть в жертву дельцов или оказаться в неприятную обстановку по причине незаконных операций. Обратитесь за помощью к нашему сервису, чтобы обезопасить ваши электронные активы и предотвратить затруднений. Совершите первый шаг к безопасности криптовалютного портфеля уже сейчас!
cá cược thể thao
Проверка Tether на чистоту: Каковым способом защитить свои электронные состояния
Постоянно все больше граждан обращают внимание в секурити их криптовалютных активов. Ежедневно шарлатаны предлагают новые способы хищения электронных средств, а также собственники криптовалюты оказываются пострадавшими их интриг. Один из подходов сбережения становится проверка кошельков в присутствие нелегальных средств.
Зачем это потребуется?
Прежде всего, чтобы сохранить свои средства от мошенников и украденных монет. Многие участники встречаются с риском утраты их средств в результате хищных схем или грабежей. Осмотр бумажников помогает обнаружить подозрительные действия и также предотвратить возможные потери.
Что наша группа предлагаем?
Мы предоставляем подход проверки цифровых кошельков или операций для определения начала средств. Наша система анализирует данные для определения незаконных транзакций и также оценки угрозы для вашего портфеля. За счет такой проверке, вы сможете избежать проблем с регуляторами или защитить себя от участия в незаконных операциях.
Каким образом это работает?
Наша фирма сотрудничаем с первоклассными аудиторскими компаниями, вроде Cure53, чтобы обеспечить прецизионность наших проверок. Мы внедряем новейшие технологии для обнаружения опасных транзакций. Ваши информация обрабатываются и сохраняются согласно с высокими нормами безопасности и конфиденциальности.
Как проверить свои Tether в чистоту?
В случае если вы желаете подтвердить, что ваша USDT-кошельки прозрачны, наш подход предлагает бесплатное тестирование первых пяти кошельков. Просто введите местоположение собственного кошелька на нашем сайте, а также мы предложим вам детальный доклад о его статусе.
Защитите вашими фонды прямо сейчас!
Не подвергайте риску подвергнуться обманщиков либо оказаться в неприятную ситуацию вследствие противозаконных операций. Обратитесь к нашему сервису, чтобы сохранить ваши криптовалютные активы и избежать проблем. Сделайте первый шаг к безопасности вашего криптовалютного портфеля прямо сейчас!
https://rg777.app/cup-c1-202324/
Циклёвка паркета: особенности и этапы услуги
Циклёвка паркета — это процесс восстановления внешнего вида паркетного пола путём удаления верхнего повреждённого слоя и возвращения ему первоначального вида. Услуга включает в себя несколько этапов:
Подготовка: перед началом работы необходимо защитить мебель и другие предметы от пыли и грязи, а также удалить плинтусы.
Шлифовка: с помощью шлифовальной машины удаляется старый лак и верхний повреждённый слой древесины.
Шпатлёвка: после шлифовки поверхность паркета шпатлюется для заполнения трещин и выравнивания поверхности.
Грунтовка: перед нанесением лака паркет грунтуется для улучшения адгезии и защиты от плесени и грибка.
Нанесение лака: лак наносится в несколько слоёв с промежуточной шлифовкой между ними.
Полировка: после нанесения последнего слоя лака паркет полируется для придания поверхности блеска и гладкости.
Циклёвка паркета позволяет обновить внешний вид пола, восстановить его структуру и продлить срок службы.
Сайт: ykladka-parketa.ru Циклёвка паркета
טלגראס כיוונים
טלגראס כיוונים: המכון המועיל לקניית קנאביסין באמצעות הטלגרם
פרח הוראות היה אתר ידע ומדריכים להשקיה שרף באמצעות האפליקציה הניידת הנפוצה מסר.
האתר מספק את כל המידע הקישורים הידיעתיים והידע המעודכן לקבוצות וערוצים הנבחרים מומלצות לקריאה לקניית קנאביס בהמסר במדינה.
כמו כך, האתר הרשמי מציעה הדרכה מתעדף לאיך להתקשר בהשרף ולקנות פרחי קנאביס בקלות מסירת ובמהירות מירבית.
בעזרת המסמכים, גם משתמשי חדשים בתחום יוכלו להמרחב השרף בטלגרם בצורה מאובטחת ומאובטחת לשימוש.
ההרובוטים של השרף מאפשר למשתמשים ללבצע פעולה שונות כמו גם הזמנת שרף, קבלה סיוע, בדיקת והוספת פידבק על המוצרים. כל זאת בצורה נוחה לשימוש ונוחה דרך האפליקציה.
כאשר כשם הדבר בשיטות התשלומים, הקנאביס מפעילה באמצעים מוכרות מאוד כמו כספים מזומנים, כרטיסי האשראי של אשראי וקריפטוֹמוֹנֵדָה. חיוני להדגש כי ישנה לבדוק ולוודא את ההוראות והחוקים המקומיים בארץ שלך ללפני ביצוע רכישה.
המסר מציע יתרונות משמעותיים מרכזיים כגון פרטיות והגנה מוגברים, התקשורת מהירה מאוד וגמישות גבוהה. בנוסף, הוא מאפשר גישה להקהל עולמית רחבה ומציע מגוון של תכונות ויכולות.
בבתום, הטלגרמה כיוונים הם המקום הטוב ללמצוא את כל המידע והקישורים הנדרשים להשקיה פרחי קנאביס בפני מהירה, בבטוחה ונוחה דרך הטלגרמה.
הימורים מקוונים הם חווייה מרגשות ופופולרי ביותר בעידן המקוון, שמאגרת מיליונים אנשים מכל
כל רחבי העולם. ההימורים המקוונים מתבצעים על פי אירועים ספורט, תוצאות פוליטיות ואפילו תוצאות מזג האוויר ונושאים נוספים. אתרים ל הימורים הווירטואליים מקריאים את מי שמעוניין להמרות על תוצאות מתאימות ולחוות חוויות ייחודיות ומרתקות.
ההימורים המקוונים הם הם כבר חלק מתרבות האנושית לא מעט זמן והיום הם לא רק רק חלק חשוב מהפעילות התרבותית והכלכלית, אלא אף מספקים רווחים וחוויות מרתקות. משום שהם נגישים מאוד ונוחים לשימוש, הם מאפשרים לכולם מהניסיון ולהצליח לנצח בכל זמן ובכל מקום.
טכנולוגיה והימורים מקוונים הפכו להיות הפופולריים ביותר בין האהובות והנפוצות. מיליוני אנשים מכל כל רחבי העולם מעוניינים בהימורים, כוללים סוגים שונים של הימורים. הימורים מקוונים מציעים למשתתפים חוויה מהנה ומרגשת, המתאימה לכולם בכל זמן ובכל מקום.
אז מה חכם אתה מחכה? הצטרף עכשיו והתחיל ליהנות מכל רגע ורגע שההימורים באינטרנט מבטיחים.
Sure, here’s the text with spin syntax applied:
Hyperlink Pyramid
After several updates to the G search mechanism, it is essential to use different options for ranking.
Today there is a way to capture the attention of search engines to your site with the support of backlinks.
Links are not only an effective promotional resource but they also have authentic traffic, straight sales from these resources likely will not be, but visits will be, and it is beneficial traffic that we also receive.
What in the end we get at the final outcome:
We present search engines site through links.
Prluuchayut natural transitions to the site and it is also a signal to search engines that the resource is used by users.
How we show search engines that the site is liquid:
Backlinks do to the main page where the main information.
We make links through redirects credible sites.
The most ESSENTIAL we place the site on sites analyzers distinct tool, the site goes into the cache of these analysis tools, then the acquired links we place as redirections on blogs, discussion boards, comment sections. This essential action shows search engines the MAP OF THE SITE as analyzer sites present all information about sites with all keywords and headings and it is very POSITIVE.
All data about our services is on the website!
Da Franz innerhalb eines Jahres Bitcoins angeschafft und veräußert hat, liegt das Geschäft innerhalb des Spekulationsjahres. In nur drei einfachen Schritten Gewinne und Verluste, die innerhalb der Haltefrist realisiert werden, können ohne Begrenzung miteinander im selben Steuerjahr verrechnet werden. Beispiel: Hast du einen Gewinn von 500 € mit Bitcoin und einen noch nicht realisierten Verlust mit Ethereum von 500 €, können bei Verkauf die Positionen miteinander verrechnet werden und es muss keine Steuer gezahlt werden. Kryptowährungen gibt es in den verschiedensten Formen, von einfachen Zahlungsmitteln («Zahlungs-Token»), über solche mit Anspruch auf Zugang zu einer digitalen Nutzung oder Dienstleistung («Nutzungs-Token») bis hin zu solchen, die vergleichbar mit einer Aktie («Anlage-Token» mit Beteiligungsrechten) oder gar ganz eigene Finanzinstrumente sind («Anlage Token» mit vertraglicher Grundlage). Neben den eigentlichen Kryptowährungen gibt es weitere Formen digitaler Vermögenswerte wie z.B. die NFTs (non-fungible Token), für welche bezüglich Deklaration und Besteuerung die nachfolgenden Regeln sinngemäss ebenfalls gelten.
https://pairup.makers.tech/en/bitcoinmnzewer
Diese rechnen damit, dass der Kurs sich kurzfristig bullisch, mittelfristig bärisch und langfristig extrem bullisch entwickeln wird. Das bedeutet, dass der Kurs zunächst steigt, anschließend wieder fällt und später dann kräftig an Wert gewinnen wird, laut beincrypto. Die Kursentwicklung von Ethereum wird in Euro (EUR), Schweizer Franken (CHF) und US-Dollar (USD) dargestellt. Das Zeitintervall kann manuell angepasst werden. Der dargestellte Ethereum-Kursverlauf wird automatisch alle 2 Sekunden aktualisiert. Tron (TRX) feiert ein starkes Comeback und sichert sich erneut einen Platz unter den Top 10 Coins nach Marktkapitalisierung. Tatsächlich hat es jetzt eine Marktkapitalisierung von 7,7 Mrd. $. Das Wiederaufleben von Tron zeigt sich in seiner beeindruckenden Netzwerkaktivität, da TRONSCAN 6,5 Milliarden Transaktionen in seinem Netzwerk gemeldet hat.
vegas grand casino
https://t.me/vegasgrandcasinoo
Creating distinct articles on Medium and Telegraph, why it is required:
Created article on these resources is better ranked on low-frequency queries, which is very crucial to get natural traffic.
We get:
organic traffic from search engines.
organic traffic from the inner rendition of the medium.
The site to which the article refers gets a link that is liquid and increases the ranking of the platform to which the article refers.
Articles can be made in any quantity and choose all less frequent queries on your topic.
Medium pages are indexed by search engines very well.
Telegraph pages need to be indexed distinctly indexer and at the same time after indexing they sometimes occupy positions higher in the search engines than the medium, these two platforms are very valuable for getting visitors.
Here is a link to our offerings where we present creation, indexing of sites, articles, pages and more.
Backlink creation is just as effective at present, simply the tools to work in this field have got changed.
You can find numerous options for inbound links, our company use some of them, and these methods operate and have been tested by our team and our clientele.
Recently our team conducted an experiment and it transpired that low-volume queries from a single website rank nicely in search engines, and it does not have to be your personal website, you are able to use social networking sites from the web 2.0 range for this.
It additionally it is possible to in part shift mass through site redirects, offering a diverse hyperlink profile.
Visit to our own web page where our own solutions are actually offered with thorough descriptions.
What’s up, just wanted to say, I loved this post.
It was practical. Keep on posting!
вегас гранд казино
вегас гранд казино
vảy gà
garilla casino
https://t.me/garillacasinoo
С началом СВО уже спустя полгода была объявлена первая волна мобилизации. При этом прошлая, в последний раз в России была аж в 1941 году, с началом Великой Отечественной Войны. Конечно же, желающих отправиться на фронт было не много, а потому люди стали искать способы не попасть на СВО, для чего стали покупать справки о болезнях, с которыми можно получить категорию Д. И все это стало возможным с даркнет сайтами, где можно найти практически все что угодно. Именно об этой отрасли темного интернета подробней и поговорим в этой статье.
What steps should I take to confirm the legitimacy of an online pharmacy’s license vidalista smart farming?
garilla казино
garilla казино
Лендинг-пейдж — это одностраничный сайт, предназначенный для рекламы и продажи товаров или услуг, а также для сбора контактных данных потенциальных клиентов. Вот несколько причин, почему лендинг-пейдж важен для бизнеса:
Увеличение узнаваемости компании. Лендинг-пейдж позволяет представить компанию и её продукты или услуги в выгодном свете, что способствует росту узнаваемости бренда.
Повышение продаж. Заказать лендинг можно здесь – 1landingpage.ru Одностраничные сайты позволяют сосредоточиться на конкретных предложениях и акциях, что повышает вероятность совершения покупки.
Оптимизация SEO-показателей. Лендинг-пейдж создаются с учётом ключевых слов и фраз, что улучшает позиции сайта в результатах поиска и привлекает больше целевых посетителей.
Привлечение новой аудитории. Одностраничные сайты могут использоваться для продвижения новых продуктов или услуг, а также для привлечения внимания к определённым кампаниям или акциям.
Расширение клиентской базы. Лендинг-пейдж собирают контактные данные потенциальных клиентов, что позволяет компании поддерживать связь с ними и предлагать дополнительные услуги или товары.
Простота генерации лидов. Лендинг-пейдж предоставляют краткую и понятную информацию о продуктах или услугах, что облегчает процесс принятия решения для потенциальных клиентов.
Сбор персональных данных. Лендинг-пейдж позволяют собирать информацию о потенциальных клиентах, такую как email-адрес, имя и контактные данные, что помогает компании лучше понимать свою аудиторию и предоставлять более персонализированные услуги.
Улучшение поискового трафика. Лендинг-пейдж создаются с учётом определённых поисковых запросов, что позволяет привлекать больше целевых посетителей на сайт.
Эффективное продвижение новой продукции. Лендинг-пейдж можно использовать для продвижения новых товаров или услуг, что позволяет привлечь внимание потенциальных клиентов и стимулировать их к покупке.
Лёгкий процесс принятия решений. Лендинг-пейдж содержат только самую необходимую информацию, что упрощает процесс принятия решения для потенциальных клиентов.
В целом, лендинг-пейдж являются мощным инструментом для продвижения бизнеса, увеличения продаж и привлечения новых клиентов.
Заказать лендинг
反向連結金字塔
反向連接金字塔
G搜尋引擎在多番更新之后需要套用不同的排名參數。
今天有一種方法可以使用反向链接吸引G搜尋引擎對您的網站的注意。
反向連接不僅是有效的推廣工具,也是有機流量。
我們會得到什麼結果:
我們透過反向链接向G搜尋引擎展示我們的網站。
他們收到了到該網站的自然過渡,這也是向G搜尋引擎發出的信號,表明該資源正在被人們使用。
我們如何向G搜尋引擎表明該網站具有流動性:
個帶有主要訊息的主頁反向链接
我們透過來自受信任網站的重定向來建立反向链接。
此外,我們將網站放置在独立的網路分析器上,網站最終會進入這些分析器的缓存中,然後我們使用產生的連結作為部落格、論壇和評論的重定向。 這個重要的操作向G搜尋引擎顯示了網站地圖,因為網站分析器顯示了有關網站的所有資訊以及所有關鍵字和標題,這很棒
有關我們服務的所有資訊都在網站上!
Pirámide de backlinks
Aquí está el texto con la estructura de spintax que propone diferentes sinónimos para cada palabra:
“Pirámide de enlaces de retorno
Después de varias actualizaciones del motor de búsqueda G, necesita aplicar diferentes opciones de clasificación.
Hay una manera de llamar la atención de los motores de búsqueda a su sitio web con enlaces de retroceso.
Los backlinks no sólo son una herramienta eficaz para la promoción, sino que también tienen flujo de visitantes orgánico, las ventas directas de estos recursos más probable es que no será, pero las transiciones será, y es poedenicheskogo tráfico que también obtenemos.
Lo que vamos a obtener al final en la salida:
Mostramos el sitio a los motores de búsqueda a través de enlaces de retorno.
Conseguimos transiciones orgánicas hacia el sitio, lo que también es una señal para los buscadores de que el recurso está siendo utilizado por la gente.
Cómo mostramos los motores de búsqueda que el sitio es líquido:
1 backlink se hace a la página principal donde está la información principal
Hacemos enlaces de retroceso a través de redirecciones de sitios de confianza
Lo más IMPORTANTE colocamos el sitio en una herramienta independiente de analizadores de sitios, el sitio entra en la caché de estos analizadores, luego los enlaces recibidos los colocamos como redirecciones en blogs, foros, comentarios.
Esta importante acción muestra a los buscadores el MAPA DEL SITIO, ya que los analizadores de sitios muestran toda la información de los sitios con todas las palabras clave y títulos y es muy BUENO.
¡Toda la información sobre nuestros servicios en el sitio web!
взлом кошелька
Как защитить свои данные: берегитесь утечек информации в интернете. Сегодня защита информации становится всё больше важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере предохранить себя от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые часто используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, используя этих сит фраз. Как защитить свои личные данные? Используйте сложные пароли. Избегайте использования несложных паролей, которые просто угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не пользуйтесь один и тот же пароль для разных сервисов. Используйте двухфакторную аутентификацию (2FA). Это прибавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы уберечь свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы охранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
кошелек с балансом купить
Криптокошельки с балансом: зачем их покупают и как использовать
В мире криптовалют все растущую популярность приобретают криптокошельки с предустановленным балансом. Это специальные кошельки, которые уже содержат определенное количество криптовалюты на момент покупки. Но зачем люди приобретают такие кошельки, и как правильно использовать их?
Почему покупают криптокошельки с балансом?
Удобство: Криптокошельки с предустановленным балансом предлагаются как готовое к работе решение для тех, кто хочет быстро начать пользоваться криптовалютой без необходимости покупки или обмена на бирже.
Подарок или награда: Иногда криптокошельки с балансом используются как подарок или премия в рамках акций или маркетинговых кампаний.
Анонимность: При покупке криптокошелька с балансом нет обязательства предоставлять личные данные, что может быть важно для тех, кто ценит анонимность.
Как использовать криптокошелек с балансом?
Проверьте безопасность: Убедитесь, что кошелек безопасен и не подвержен взлому. Проверьте репутацию продавца и источник приобретения кошелька.
Переведите средства на другой кошелек: Если вы хотите долгосрочно хранить криптовалюту, рекомендуется перевести средства на более безопасный или практичный для вас кошелек.
Не храните все средства на одном кошельке: Для обеспечения безопасности рекомендуется распределить средства между несколькими кошельками.
Будьте осторожны с фишингом и мошенничеством: Помните, что мошенники могут пытаться обмануть вас, предлагая криптокошельки с балансом с целью получения доступа к вашим средствам.
Заключение
Криптокошельки с балансом могут быть удобным и легким способом начать пользоваться криптовалютой, но необходимо помнить о безопасности и осторожности при их использовании.Выбор и приобретение криптокошелька с балансом – это весомый шаг, который требует внимания к деталям и осознанного подхода.”
сид фразы кошельков
Сид-фразы, или мнемонические фразы, представляют собой сочетание слов, которая используется для создания или восстановления кошелька криптовалюты. Эти фразы обеспечивают доступ к вашим криптовалютным средствам, поэтому их надежное хранение и использование очень важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы являются набор произвольно сгенерированных слов, часто от 12 до 24, которые предназначаются для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления доступа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают большой защиты и шифруются, что делает их безопасными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы жизненно важны для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить возможность доступа к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете просто создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не раскрывайте сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может привести к утере вашего криптоимущества.
Храните сид-фразу в безопасном месте. Используйте физически секурные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить возможность доступа к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите двухфакторную аутентификацию и другие методы защиты для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом безопасного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
слив сид фраз
Слив засеянных фраз (seed phrases) является единственным из наиболее обычных способов утечки личных информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, зачем они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, составляют комбинацию слов, которая используется для создания или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые символизируют собой ключ к вашему кошельку. Потеря или утечка сид фразы может вести к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы представляют ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они могут получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу любому, даже если вам кажется, что это привилегированное лицо или сервис.
Храните свою сид фразу в надежном и секурном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухэтапная проверка, для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в разнообразных безопасных местах.
Заключение
Слив сид фраз является значительной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
Столбец бэклинков
После того как многочисленных обновлений G необходимо внедрять различные варианты рейтингования.
Сегодня есть способ привлечь внимание поисковых систем к вашему веб-сайту с помощью бэклинков.
Обратные ссылки не только эффективный инструмент продвижения, но и являются источником органического трафика, хотя прямых продаж с этих ресурсов скорее всего не будет, но переходы будут, и именно органического трафика мы также получаем.
Что в итоге получим на выходе:
Мы демонстрируем сайт поисковым системам при помощи обратных ссылок.
Получают органические переходы на сайт, а это также сигнал поисковым системам о том, что ресурс используется людьми.
Как мы указываем поисковым системам, что сайт ликвиден:
1 ссылка на главную страницу, где содержится основная информация, создается.
Размещаем обратные ссылки через редиректы с трастовых ресурсов.
Основное – мы индексируем сайт с помощью специальных инструментов анализа веб-сайтов, сайт заносится в кеш этих инструментов, после чего полученные ссылки мы публикуем в качестве редиректов на блогах, форумах, в комментариях.
Это нужное действие показывает потсковикамКАРТУ САЙТА, так как анализаторы сайтов показывают всю информацию о сайтах со с тайтлами, ключами, h1,h2,h3 и это очень ХОРОШО
ggg
هنا النص مع استخدام السبينتاكس:
“هيكل الروابط الخلفية
بعد التحديثات العديدة لمحرك البحث G، تحتاج إلى تنفيذ خيارات ترتيب مختلفة.
هناك منهج لجذب انتباه محركات البحث إلى موقعك على الويب باستخدام الروابط الخلفية.
الروابط الخلفية ليست فقط أداة فعالة للترويج، ولكن لديها أيضًا حركة مرور عضوية، والمبيعات المباشرة من هذه الموارد على الأرجح لن تكون كذلك، ولكن التحولات ستكون، وهي حركة المرور التي نحصل عليها أيضًا.
ما سوف نحصل عليه في النهاية في النهاية في الإخراج:
نعرض الموقع لمحركات البحث من خلال الروابط الخلفية.
2- نحصل على تبديلات عضوية إلى الموقع، وهي أيضًا إشارة لمحركات البحث أن المورد يستخدمه الناس.
كيف نظهر لمحركات البحث أن الموقع سائل:
1 يتم عمل وصلة خلفي للصفحة الرئيسية حيث المعلومات الرئيسية
نقوم بعمل لينكات خلفية من خلال عمليات توجيه مرة أخرى المواقع الموثوقة
الأهم من ذلك أننا نضع الموقع على أداة منفصلة من أدوات تحليل المواقع، ويدخل الموقع في ذاكرة التخزين المؤقت لهذه المحللات، ثم الروابط المستلمة التي نضعها كتحويل على المدونات والمنتديات والتعليقات.
هذا العملية المهم يُبرز لمحركات البحث خريطة الموقع، حيث تعرض أدوات تحليل المواقع جميع المعلومات عن المواقع مع جميع الكلمات الرئيسية والعناوين وهو شيء جيد جداً
جميع المعلومات عن خدماتنا على الموقع!
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Starting off this list on Stake’s best slots is Sweet Bonanza. This game is one of the best Stake slots developed by Pragmatic Play, which is one of the top casino game providers. Whether you play it on the desktop site or across any of the six different mobile apps, this is one great betting site. If you’re after the best slots at bet 365, head over to bet365 casino and bet365 games sections, but remember to check out the full range of bet365 casino games, including a vast array of great table games in both the bet365 casino and bet365 live casino as well. © Copyright 2024 Many players like to stick to a budget when reel spinning, and penny games allow longer gaming sessions. Easily spin for as long as you like if you are wagering just one penny per spin!
https://front-wiki.win/index.php?title=Highest_jackpot_slot_machine
Love Vegas? Love the casino? Love slots? With Buffalo you can have it all! Download the BEST free slots game in Google Play and play now! Owners of Android devices can also play Buffalo slot machine free download. Most online casinos offer mobile versions of their games that are compatible with the Android operating system, allowing you to enjoy playing on smartphones and tablets. Match up 3 fortune wheel icons and spin the wheel to see what you can win! Collect and double diamonds or triple your diamonds to level up and unlock special portraits. The demo version of the Buffalo slot machine (with no download) offers a balance of 100 free coins when playing for fun. Do not play with the highest betting limits to avoid the money exhausted. The better case is using minimum betting amounts in both free and real money versions. Even if all your free coins are wasted start over by reloading the game.
Как охранять свои личные данные: берегитесь утечек информации в интернете. Сегодня охрана своих данных становится всё более важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и как предохранить себя от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые постоянно используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как обезопасить свои личные данные? Используйте комплексные пароли. Избегайте использования легких паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не воспользуйтесь один и тот же пароль для разных сервисов. Используйте двухфакторную проверку (2FA). Это привносит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт посредством другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте свою информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы защитить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
даркнет сливы тг
Даркнет и сливы в Телеграме
Даркнет – это отрезок интернета, которая не индексируется обычными поисковыми системами и требует особых программных средств для доступа. В даркнете существует масса скрытых сайтов, где можно найти различные товары и услуги, в том числе и нелегальные.
Одним из известных способов распространения информации в даркнете является использование мессенджера Телеграм. Телеграм предоставляет возможность создания закрытых каналов и чатов, где пользователи могут обмениваться информацией, в том числе и нелегальной.
Сливы информации в Телеграме – это практика распространения конфиденциальной информации, такой как украденные данные, базы данных, персональные сведения и другие материалы. Эти сливы могут включать в себя информацию о кредитных картах, паролях, персональных сообщениях и даже фотографиях.
Сливы в Телеграме могут быть рискованными, так как они могут привести к утечке конфиденциальной информации и нанести ущерб репутации и финансовым интересам людей. Поэтому важно быть предусмотрительным при обмене информацией в интернете и не доверять сомнительным источникам.
Вот кошельки с балансом у бота
Сид-фразы, или памятные фразы, представляют собой соединение слов, которая используется для генерации или восстановления кошелька криптовалюты. Эти фразы обеспечивают возможность доступа к вашим криптовалютным средствам, поэтому их безопасное хранение и использование весьма важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы представляют собой набор случайными средствами сгенерированных слов, в большинстве случаев от 12 до 24, которые предназначены для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления доступа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают высокой степенью защиты и шифруются, что делает их надежными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы необходимы для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить доступ к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете без труда создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не делитесь сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может влечь за собой утере вашего криптоимущества.
Храните сид-фразу в надежном месте. Используйте физически безопасные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить доступ к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите двухфакторную верификацию и другие методы защиты для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом безопасного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Криптокошельки с балансом: зачем их покупают и как использовать
В мире криптовалют все большую популярность приобретают криптокошельки с предустановленным балансом. Это индивидуальные кошельки, которые уже содержат определенное количество криптовалюты на момент покупки. Но зачем люди приобретают такие кошельки, и как правильно использовать их?
Почему покупают криптокошельки с балансом?
Удобство: Криптокошельки с предустановленным балансом предлагаются как готовое к работе решение для тех, кто хочет быстро начать пользоваться криптовалютой без необходимости покупки или обмена на бирже.
Подарок или награда: Иногда криптокошельки с балансом используются как подарок или вознаграждение в рамках акций или маркетинговых кампаний.
Анонимность: При покупке криптокошелька с балансом нет потребности предоставлять личные данные, что может быть важно для тех, кто ценит анонимность.
Как использовать криптокошелек с балансом?
Проверьте безопасность: Убедитесь, что кошелек безопасен и не подвержен взлому. Проверьте репутацию продавца и источник приобретения кошелька.
Переведите средства на другой кошелек: Если вы хотите долгосрочно хранить криптовалюту, рекомендуется перевести средства на более безопасный или комфортный для вас кошелек.
Не храните все средства на одном кошельке: Для обеспечения безопасности рекомендуется распределить средства между несколькими кошельками.
Будьте осторожны с фишингом и мошенничеством: Помните, что мошенники могут пытаться обмануть вас, предлагая криптокошельки с балансом с целью получения доступа к вашим средствам.
Заключение
Криптокошельки с балансом могут быть удобным и скорым способом начать пользоваться криптовалютой, но необходимо помнить о безопасности и осторожности при их использовании.Выбор и приобретение криптокошелька с балансом – это весомый шаг, который требует внимания к деталям и осознанного подхода.”
слив сид фраз
Слив мнемонических фраз (seed phrases) является одним наиболее известных способов утечки личной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, по какой причине они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, являются комбинацию слов, которая используется для составления или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые символизируют собой ключ к вашему кошельку. Потеря или утечка сид фразы может привести к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы служат ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они могут получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу никакому, даже если вам представляется, что это проверенное лицо или сервис.
Храните свою сид фразу в надежном и защищенном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная аутентификация (2FA), для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в разных безопасных местах.
Заключение
Слив сид фраз является серьезной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
kantorbola
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
Are there OTC options for peptic ulcer disease relief advair price?
taurus118
rikvip
Rikvip Club: Trung Tâm Giải Trí Trực Tuyến Hàng Đầu tại Việt Nam
Rikvip Club là một trong những nền tảng giải trí trực tuyến hàng đầu tại Việt Nam, cung cấp một loạt các trò chơi hấp dẫn và dịch vụ cho người dùng. Cho dù bạn là người dùng iPhone hay Android, Rikvip Club đều có một cái gì đó dành cho mọi người. Với sứ mạng và mục tiêu rõ ràng, Rikvip Club luôn cố gắng cung cấp những sản phẩm và dịch vụ tốt nhất cho khách hàng, tạo ra một trải nghiệm tiện lợi và thú vị cho người chơi.
Sứ Mạng và Mục Tiêu của Rikvip
Từ khi bắt đầu hoạt động, Rikvip Club đã có một kế hoạch kinh doanh rõ ràng, luôn nỗ lực để cung cấp cho khách hàng những sản phẩm và dịch vụ tốt nhất và tạo điều kiện thuận lợi nhất cho người chơi truy cập. Nhóm quản lý của Rikvip Club có những mục tiêu và ước muốn quyết liệt để biến Rikvip Club thành trung tâm giải trí hàng đầu trong lĩnh vực game đổi thưởng trực tuyến tại Việt Nam và trên toàn cầu.
Trải Nghiệm Live Casino
Rikvip Club không chỉ nổi bật với sự đa dạng của các trò chơi đổi thưởng mà còn với các phòng trò chơi casino trực tuyến thu hút tất cả người chơi. Môi trường này cam kết mang lại trải nghiệm chuyên nghiệp với tính xanh chín và sự uy tín không thể nghi ngờ. Đây là một sân chơi lý tưởng cho những người yêu thích thách thức bản thân và muốn tận hưởng niềm vui của chiến thắng. Với các sảnh cược phổ biến như Roulette, Sic Bo, Dragon Tiger, người chơi sẽ trải nghiệm những cảm xúc độc đáo và đặc biệt khi tham gia vào casino trực tuyến.
Phương Thức Thanh Toán Tiện Lợi
Rikvip Club đã được trang bị những công nghệ thanh toán tiên tiến ngay từ đầu, mang lại sự thuận tiện và linh hoạt cho người chơi trong việc sử dụng hệ thống thanh toán hàng ngày. Hơn nữa, Rikvip Club còn tích hợp nhiều phương thức giao dịch khác nhau để đáp ứng nhu cầu đa dạng của người chơi: Chuyển khoản Ngân hàng, Thẻ cào, Ví điện tử…
Kết Luận
Tóm lại, Rikvip Club không chỉ là một nền tảng trò chơi, mà còn là một cộng đồng nơi người chơi có thể tụ tập để tận hưởng niềm vui của trò chơi và cảm giác hồi hộp khi chiến thắng. Với cam kết cung cấp những sản phẩm và dịch vụ tốt nhất, Rikvip Club chắc chắn là điểm đến lý tưởng cho những người yêu thích trò chơi trực tuyến tại Việt Nam và cả thế giới.
Euro 2024
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
국외선물의 시작 골드리치와 동행하세요.
골드리치는 길고긴기간 회원분들과 더불어 선물시장의 행로을 공동으로 동행해왔으며, 고객분들의 안전한 자금운용 및 건강한 수익률을 향해 계속해서 최선을 다하고 있습니다.
왜 20,000+인 이상이 골드리치증권와 투자하나요?
빠른 대응: 편리하고 빠른 프로세스를 갖추어 누구나 수월하게 활용할 수 있습니다.
안전보장 프로토콜: 국가기관에서 사용하는 최상의 등급의 보안체계을 채택하고 있습니다.
스마트 인가: 모든 거래데이터은 암호처리 처리되어 본인 외에는 그 누구도 내용을 접근할 수 없습니다.
안전 수익성 마련: 위험 요소를 줄여, 보다 한층 보장된 수익률을 공개하며 이에 따른 리포트를 발간합니다.
24 / 7 지속적인 고객상담: 연중무휴 24시간 신속한 서비스를 통해 고객님들을 모두 뒷받침합니다.
함께하는 동반사: 골드리치는 공기업은 물론 금융계들 및 다수의 협력사와 공동으로 동행해오고.
해외선물이란?
다양한 정보를 알아보세요.
외국선물은 국외에서 거래되는 파생금융상품 중 하나로, 명시된 기초자산(예시: 주식, 화폐, 상품 등)을 바탕로 한 옵션 계약을 의미합니다. 근본적으로 옵션은 지정된 기초자산을 향후의 특정한 시기에 일정 가격에 매수하거나 매도할 수 있는 권리를 부여합니다. 국외선물옵션은 이러한 옵션 계약이 국외 시장에서 거래되는 것을 지칭합니다.
해외선물은 크게 매수 옵션과 풋 옵션으로 분류됩니다. 매수 옵션은 지정된 기초자산을 미래에 일정 가격에 매수하는 권리를 허락하는 반면, 매도 옵션은 특정 기초자산을 미래에 일정 가격에 매도할 수 있는 권리를 제공합니다.
옵션 계약에서는 미래의 특정 일자에 (만료일이라 불리는) 일정 금액에 기초자산을 사거나 매도할 수 있는 권리를 보유하고 있습니다. 이러한 가격을 실행 가격이라고 하며, 만기일에는 해당 권리를 행사할지 여부를 결정할 수 있습니다. 따라서 옵션 계약은 거래자에게 향후의 가격 변화에 대한 보호나 이익 실현의 기회를 제공합니다.
외국선물은 시장 참가자들에게 다양한 운용 및 차익거래 기회를 제공, 환율, 상품, 주식 등 다양한 자산유형에 대한 옵션 계약을 포괄할 수 있습니다. 거래자는 매도 옵션을 통해 기초자산의 낙폭에 대한 보호를 받을 수 있고, 콜 옵션을 통해 상승장에서의 이익을 타깃팅할 수 있습니다.
해외선물 거래의 원리
실행 금액(Exercise Price): 해외선물에서 실행 가격은 옵션 계약에 따라 명시된 금액으로 계약됩니다. 종료일에 이 가격을 기준으로 옵션을 실현할 수 있습니다.
만기일(Expiration Date): 옵션 계약의 종료일은 옵션의 실행이 불가능한 마지막 날짜를 뜻합니다. 이 일자 이후에는 옵션 계약이 소멸되며, 더 이상 거래할 수 없습니다.
풋 옵션(Put Option)과 매수 옵션(Call Option): 매도 옵션은 기초자산을 명시된 가격에 팔 수 있는 권리를 부여하며, 콜 옵션은 기초자산을 명시된 금액에 사는 권리를 부여합니다.
프리미엄(Premium): 외국선물 거래에서는 옵션 계약에 대한 프리미엄을 납부해야 합니다. 이는 옵션 계약에 대한 가격으로, 시장에서의 수요량와 공급량에 따라 변경됩니다.
행사 방안(Exercise Strategy): 투자자는 종료일에 옵션을 실행할지 여부를 결정할 수 있습니다. 이는 시장 환경 및 거래 플랜에 따라 상이하며, 옵션 계약의 수익을 최대화하거나 손실을 최소화하기 위해 선택됩니다.
마켓 위험요인(Market Risk): 외국선물 거래는 마켓의 변동성에 영향을 받습니다. 가격 변동이 기대치 못한 방향으로 일어날 경우 손해이 발생할 수 있으며, 이러한 마켓 위험요인를 축소하기 위해 투자자는 계획을 수립하고 투자를 계획해야 합니다.
골드리치증권와 동반하는 해외선물은 확실한 확신할 수 있는 투자를 위한 최적의 옵션입니다. 회원님들의 투자를 뒷받침하고 안내하기 위해 우리는 전력을 다하고 있습니다. 함께 더 나은 미래를 지향하여 나아가요.
Замена венцов красноярск
Геракл24: Опытная Смена Фундамента, Венцов, Полов и Перемещение Домов
Фирма Gerakl24 занимается на выполнении всесторонних работ по замене фундамента, венцов, покрытий и перемещению домов в месте Красноярске и за его пределами. Наша группа опытных мастеров обеспечивает высокое качество выполнения всех видов реставрационных работ, будь то из дерева, каркасные, кирпичные постройки или из бетона дома.
Плюсы услуг Gerakl24
Навыки и знания:
Все работы выполняются лишь профессиональными специалистами, имеющими многолетний практику в сфере строительства и восстановления строений. Наши мастера профессионалы в своем деле и осуществляют проекты с безупречной точностью и учетом всех деталей.
Полный спектр услуг:
Мы предоставляем разнообразные услуги по реставрации и восстановлению зданий:
Реставрация фундамента: замена и укрепление фундамента, что позволяет продлить срок службы вашего строения и устранить проблемы, связанные с оседанием и деформацией строения.
Замена венцов: реставрация нижних венцов из дерева, которые чаще всего подвергаются гниению и разрушению.
Замена полов: монтаж новых настилов, что значительно улучшает визуальное восприятие и практическую полезность.
Передвижение домов: безопасное и качественное передвижение домов на новые места, что помогает сохранить здание и избегает дополнительных затрат на строительство нового.
Работа с любыми типами домов:
Дома из дерева: восстановление и защита деревянных строений, обработка от гниения и насекомых.
Каркасные строения: реставрация каркасов и замена поврежденных элементов.
Дома из кирпича: реставрация кирпичной кладки и усиление стен.
Бетонные дома: ремонт и укрепление бетонных конструкций, устранение трещин и повреждений.
Качество и прочность:
Мы работаем с только высококачественные материалы и передовые технологии, что обеспечивает долгий срок службы и надежность всех выполненных работ. Все наши проекты проходят строгий контроль качества на всех этапах выполнения.
Персонализированный подход:
Каждому клиенту мы предлагаем персонализированные решения, учитывающие ваши требования и желания. Мы стремимся к тому, чтобы конечный результат полностью удовлетворял вашим ожиданиям и требованиям.
Зачем обращаться в Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который берет на себя все заботы по восстановлению и ремонту вашего здания. Мы обещаем выполнение всех задач в установленные сроки и с соблюдением всех правил и норм. Выбрав Геракл24, вы можете быть спокойны, что ваше строение в надежных руках.
Мы готовы предоставить консультацию и ответить на ваши вопросы. Свяжитесь с нами, чтобы обсудить ваш проект и узнать больше о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, сделав его безопасным и комфортным для проживания на долгие годы.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
pg slot
האפליקציה הינה פלטפורמה פופולרית בישראל לרכישת צמח הקנאביס בצורה וירטואלי. היא מעניקה ממשק משתמש נוח ובטוח לקנייה ולקבלת משלוחים של מוצרי מריחואנה מרובים. בסקירה זה נבחן עם העיקרון מאחורי טלגראס, כיצד זו פועלת ומהם המעלות של השימוש בזו.
מה זו הפלטפורמה?
טלגראס הווה דרך לרכישת קנאביס באמצעות היישומון טלגרם. זו נשענת על ערוצי תקשורת וקבוצות טלגראם ייעודיות הנקראות ״כיווני טלגראס״, שבהם אפשר להזמין מרחב מוצרי צמח הקנאביס ולקבל אותם ישירות לשילוח. ערוצי התקשורת אלו מסודרים על פי אזורים גאוגרפיים, כדי לשפר על קבלת המשלוחים.
איך זאת עובד?
התהליך פשוט יחסית. ראשית, יש להצטרף לערוץ הטלגראס הנוגע לאזור המגורים. שם ניתן לצפות בתפריטי המוצרים השונים ולהזמין עם הפריטים המבוקשים. לאחר השלמת ההזמנה וסגירת התשלום, השליח יופיע לכתובת שנרשמה עם הארגז המוזמנת.
רוב ערוצי טלגראס מספקים מגוון רחב מ מוצרים – זנים של קנאביס, עוגיות, שתייה ועוד. כמו כן, ניתן לראות ביקורות מ לקוחות שעברו לגבי איכות הפריטים והשירות.
מעלות הנעשה בפלטפורמה
יתרון עיקרי של האפליקציה הוא הנוחות והפרטיות. ההזמנה והתהליך מתבצעות ממרחק מאיזשהו מיקום, בלי נחיצות במפגש פיזי. כמו כן, האפליקציה מוגנת היטב ומבטיחה סודיות גבוה.
מלבד על זאת, מחירי הפריטים בפלטפורמה נוטות להיות תחרותיים, והשילוחים מגיעים במהירות ובמסירות רבה. קיים אף מרכז תמיכה זמין לכל שאלה או בעיית.
סיכום
טלגראס מהווה דרך מקורית ויעילה לקנות פריטי מריחואנה בארץ. היא משלבת בין הנוחיות הטכנולוגית של האפליקציה הפופולרי, ועם הזריזות והדיסקרטיות של דרך המשלוח הישירה. ככל שהביקוש לקנאביס גדלה, פלטפורמות בדוגמת טלגראס צפויות להמשיך ולהתפתח.
b29
Bản cài đặt B29 IOS – Giải pháp vượt trội cho các tín đồ iOS
Trong thế giới công nghệ đầy sôi động hiện nay, trải nghiệm người dùng luôn là yếu tố then chốt. Với sự ra đời của Bản cài đặt B29 IOS, người dùng sẽ được hưởng trọn vẹn những tính năng ưu việt, mang đến sự hài lòng tuyệt đối. Hãy cùng khám phá những ưu điểm vượt trội của bản cài đặt này!
Tính bảo mật tối đa
Bản cài đặt B29 IOS được thiết kế với mục tiêu đảm bảo an toàn dữ liệu tuyệt đối cho người dùng. Nhờ hệ thống mã hóa hiện đại, thông tin cá nhân và dữ liệu nhạy cảm của bạn luôn được bảo vệ an toàn khỏi những kẻ xâm nhập trái phép.
Trải nghiệm người dùng đỉnh cao
Giao diện thân thiện, đơn giản nhưng không kém phần hiện đại, B29 IOS mang đến cho người dùng trải nghiệm duyệt web, truy cập ứng dụng và sử dụng thiết bị một cách trôi chảy, mượt mà. Các tính năng thông minh được tối ưu hóa, giúp nâng cao hiệu suất và tiết kiệm pin đáng kể.
Tính tương thích rộng rãi
Bản cài đặt B29 IOS được phát triển với mục tiêu tương thích với mọi thiết bị iOS từ các dòng iPhone, iPad cho đến iPod Touch. Dù là người dùng mới hay lâu năm của hệ điều hành iOS, B29 đều mang đến sự hài lòng tuyệt đối.
Quá trình cài đặt đơn giản
Với những hướng dẫn chi tiết, việc cài đặt B29 IOS trở nên nhanh chóng và dễ dàng. Chỉ với vài thao tác đơn giản, bạn đã có thể trải nghiệm ngay tất cả những tính năng tuyệt vời mà bản cài đặt này mang lại.
Bản cài đặt B29 IOS không chỉ là một bản cài đặt đơn thuần, mà còn là giải pháp công nghệ hiện đại, nâng tầm trải nghiệm người dùng lên một tầm cao mới. Hãy trở thành một phần của cộng đồng sử dụng B29 IOS để khám phá những tiện ích tuyệt vời mà nó có thể mang lại!
Как сберечь свои данные: остерегайтесь утечек информации в интернете. Сегодня сохранение своих данных становится всё больше важной задачей. Одним из наиболее распространенных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере сберечься от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые часто используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или разные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как охранить свои личные данные? Используйте комплексные пароли. Избегайте использования простых паролей, которые просто угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухфакторную проверку (2FA). Это вводит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы уберечь свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может спровоцировать серьезным последствиям, таким как кража личной информации и финансовых потерь. Чтобы сохранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
האפליקציה מהווה פלטפורמה מקובלת בארץ לרכישת מריחואנה בצורה מקוון. היא נותנת ממשק משתמש פשוט לשימוש ובטוח לרכישה ולקבלת שילוחים של פריטי מריחואנה מגוונים. בסקירה זה נסקור עם הרעיון מאחורי האפליקציה, איך היא עובדת ומה היתרונות מ השימוש בה.
מה זו טלגראס?
האפליקציה מהווה שיטה לרכישת מריחואנה דרך האפליקציה טלגראם. היא נשענת מעל ערוצי תקשורת וקהילות טלגרם ייעודיות הנקראות ״טלגראס כיוונים, שבהם אפשר להרכיב מרחב פריטי מריחואנה ולקבלת אותם ישירות לשילוח. ערוצי התקשורת האלה מסודרים לפי איזורים גאוגרפיים, כדי לשפר את קבלתם של המשלוחים.
איך זה פועל?
התהליך פשוט למדי. קודם כל, יש להצטרף לערוץ הטלגראס הנוגע לאזור המגורים. שם אפשר לצפות בתפריטים של המוצרים השונים ולהזמין את הפריטים המבוקשים. לאחר ביצוע ההזמנה וסגירת התשלום, השליח יופיע לכתובת שנרשמה עם הארגז שהוזמן.
רוב ערוצי הטלגראס מציעים מגוון רחב מ פריטים – זנים של מריחואנה, ממתקים, משקאות ועוד. כמו כן, ניתן לראות ביקורות מ לקוחות קודמים לגבי רמת הפריטים והשירות.
מעלות השימוש בפלטפורמה
מעלה מרכזי של הפלטפורמה הוא הנוחיות והדיסקרטיות. ההרכבה והתהליך מתקיימים מרחוק מאיזשהו מקום, בלי נחיצות בהתכנסות פיזי. כמו כן, הפלטפורמה מאובטחת ביסודיות ומבטיחה סודיות גבוהה.
מלבד על כך, מחירי הפריטים באפליקציה נוטים להיות זולים, והמשלוחים מגיעים במהירות ובמסירות רבה. קיים גם מרכז תמיכה פתוח לכל שאלה או בעיית.
סיכום
טלגראס הינה שיטה מקורית ויעילה לקנות פריטי קנאביס בישראל. היא משלבת את הנוחות הדיגיטלית מ היישומון הפופולרית, ועם הזריזות והדיסקרטיות מ דרך המשלוח הישירה. ככל שהביקוש לקנאביס גדלה, פלטפורמות בדוגמת טלגראס צפויות להמשיך ולצמוח.
отмывание usdt
Как защитить свои личные данные: остерегайтесь утечек информации в интернете. Сегодня охрана личных данных становится всё больше важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере предохранить себя от их утечки? Что такое «сит фразы»? «Сит фразы» — это синтезы слов или фраз, которые регулярно используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как обезопасить свои личные данные? Используйте комплексные пароли. Избегайте использования очевидных паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не применяйте один и тот же пароль для разных сервисов. Используйте двухфакторную аутентификацию (2FA). Это вводит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы сохранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
Сохраните собственные USDT: Удостоверьтесь транзакцию TRC20 перед пересылкой
Цифровые валюты, подобные вроде USDT (Tether) на блокчейне TRON (TRC20), делаются всё более популярными в области распределенных финансов. Однако вместе с ростом распространенности растет и риск погрешностей или мошенничества во время отправке денег. Как раз именно поэтому необходимо проверять перевод USDT TRC20 до ее пересылкой.
Промах при вводе данных адреса адресата либо пересылка по неправильный адрес получателя может повлечь к невозможности необратимой утрате твоих USDT. Злоумышленники тоже могут стараться обмануть тебя, пересылая ложные адреса на отправки. Утрата цифровой валюты из-за таких промахов сможет повлечь значительными финансовыми убытками.
К счастью, имеются профильные службы, дающие возможность проверить транзакцию USDT TRC20 до её отправкой. Один из таких сервисов дает возможность просматривать а также анализировать операции в блокчейне TRON.
В данном сервисе вам можете ввести адрес адресата а также получать обстоятельную сведения об нем, включая архив переводов, баланс а также состояние аккаунта. Данное поможет установить, является или нет адрес получателя подлинным и безопасным для перевода средств.
Иные службы тоже предоставляют сходные возможности по проверки переводов USDT TRC20. Некоторые кошельки для криптовалют для криптовалют имеют встроенные возможности по проверки адресов а также транзакций.
Не игнорируйте проверкой операции USDT TRC20 перед её пересылкой. Небольшая предосторожность может сэкономить для вас много средств а также избежать утрату твоих ценных криптовалютных ресурсов. Используйте проверенные службы для обеспечения безопасности ваших транзакций а также целостности ваших USDT в блокчейне TRON.
При обращении с криптовалютой USDT в распределенном реестре TRON (TRC20) максимально значимо не только удостоверять реквизиты получателя перед отправкой финансов, а также тоже систематически контролировать баланс личного кошелька, а также источники входящих транзакций. Данное действие даст возможность своевременно идентифицировать все нежелательные действия а также предотвратить возможные убытки.
Прежде всего, требуется удостовериться на точности демонстрируемого баланса USDT TRC20 на собственном криптокошельке. Рекомендуется сверять информацию с данными публичных блокчейн-обозревателей, для того чтобы избежать вероятность хакерской атаки либо скомпрометирования самого кошелька.
Тем не менее одного только отслеживания остатка недостаточно. Чрезвычайно важно анализировать журнал входящих транзакций и этих источники. В случае если Вы обнаружите переводы USDT от неопознанных либо вызывающих опасения реквизитов, незамедлительно приостановите данные средства. Существует опасность, что эти криптомонеты стали получены преступным путем и в будущем могут быть конфискованы регулирующими органами.
Наш приложение дает средства для углубленного анализа входящих USDT TRC20 переводов касательно этой законности и отсутствия соотношения с преступной деятельностью. Мы.
Дополнительно необходимо периодически отправлять USDT TRC20 в надежные неконтролируемые криптовалютные кошельки находящиеся под вашим полным контролем. Хранение монет на внешних площадках неизменно связано с угрозами взломов а также потери денег вследствие программных сбоев или несостоятельности платформы.
Следуйте основные правила безопасности, оставайтесь внимательны и вовремя мониторьте баланс и источники поступлений USDT TRC20 кошелька. Данные действия позволит оградить Ваши цифровые активы от.
Важность анализа трансфера USDT TRC-20
Транзакции USDT в технологии TRC20 демонстрируют растущую спрос, тем не менее стоит являться крайне бдительными во время этих получении.
Такой категория операций преимущественно задействуется для отмывания средств, полученных криминальным путем.
Главный рисков приобретения USDT TRC-20 – состоит в том, что данные средства могут быть зачислены вследствие множественных методов вымогательства, таких как утраты приватных данных, вымогательство, кибератаки как и прочие преступные манипуляции. Принимая указанные переводы, пользователь автоматически становитесь соучастником криминальной операций.
В связи с этим крайне важно скрупулезно проверять природу всех зачисляемого операции через USDT TRC-20. Необходимо интересоваться с плательщика подтверждения касательно чистоте средств, и малейших подозрениях – воздерживаться от платежей.
Учитывайте, что в результате определения криминальных источников денежных средств, пользователь можете быть подвергнуты к санкциям параллельно с плательщиком. Поэтому предпочтительнее принять меры предосторожности наряду с детально изучать любой перевод, чем подвергать риску репутационной репутацией и быть втянутым с крупные судебные неприятности.
Поддержание аккуратности при сделках с использованием USDT по сети TRC20 – представляет собой ключ личной материальной безопасности как и защита вовлечения в криминальные операции. Оставайтесь бдительными как и постоянно анализируйте природу цифровых валютных финансов.
Meet to our website, your pm online hub after African sports, music, and celebrity updates. We cover everything from heady sports events like the Africa Cup of Nations to the latest trends in Afrobeats and usual music. Explore chic interviews and features on well-known personalities making waves across the continent and beyond.
At our website, we stipulate auspicious and attractive content that celebrates the diversity and vibrancy of African culture. Whether you’re a sports lover, music lover, or curious far Africa’s weighty figures, go our community and stay connected concerning regular highlights and in-depth stories showcasing the kindest of African aptitude and creativity https://nouvelles-histoires-africaines.africa/comment-creer-un-diaporama-de-photos-avec-de-la/.
Befall our website today and see the high-powered magic of African sports, music, and renowned personalities. Engross yourself in the richness of Africa’s cultural section with us!
проверить адрес usdt trc20
Название: Необходимо удостоверяйтесь в адрес получателя во время транзакции USDT TRC20
При взаимодействии со цифровыми валютами, в частности с USDT в блокчейне TRON (TRC20), крайне важно выказывать осторожность а также тщательность. Единственная из наиболее обычных оплошностей, которую совершают юзеры – отправка средств на неверный адресу. Для того чтобы избежать потери собственных USDT, нужно неизменно внимательно контролировать адрес реципиента перед отправкой перевода.
Цифровые адреса кошельков представляют собой обширные совокупности символов и цифр, к примеру, TRX9QahiFUYfHffieZThuzHbkndWvvfzThB8U. Включая небольшая ошибка иль ошибка во время копирования адреса кошелька сможет повлечь к тому результату, чтобы ваши цифровые деньги станут невозвратно лишены, так как они окажутся на неподконтрольный вами кошелек.
Существуют многообразные методы контроля адресов кошельков USDT TRC20:
1. Глазомерная инспекция. Тщательно сверьте адрес в твоём крипто-кошельке с адресом кошелька реципиента. В случае незначительном различии – не совершайте перевод.
2. Использование онлайн-сервисов удостоверения.
3. Двойная верификация со получателем. Обратитесь с просьбой к реципиенту удостоверить корректность адреса до посылкой операции.
4. Тестовый операция. При значительной величине транзакции, допустимо вначале послать незначительное величину USDT для удостоверения адреса.
Также советуется содержать цифровые деньги на личных кошельках, а не в биржах иль посреднических инструментах, для того чтобы иметь полный контроль по отношению к собственными средствами.
Не пренебрегайте контролем адресов кошельков при работе с USDT TRC20. Данная несложная мера предосторожности окажет помощь обезопасить ваши финансы против случайной утраты. Имейте в виду, чтобы в мире криптовалют переводы неотменимы, а отправленные монеты на неправильный адрес кошелька возвратить фактически нереально. Будьте бдительны и аккуратны, чтобы защитить свои вложения.
טלגראס מהווה פלטפורמה פופולרית בישראל לרכישת צמח הקנאביס בצורה מקוון. זו נותנת ממשק נוח ומאובטח לקנייה ולקבלת שילוחים של פריטי קנאביס מרובים. בסקירה זה נבחן עם הרעיון מאחורי הפלטפורמה, כיצד זו פועלת ומה היתרים של השימוש בזו.
מה זו האפליקציה?
טלגראס היא שיטה לקנייה של קנאביס באמצעות היישומון טלגרם. היא מבוססת מעל ערוצי תקשורת וקבוצות טלגרם ייעודיות הקרויות ״כיווני טלגראס״, שבהם אפשר להזמין מגוון מוצרי צמח הקנאביס ולקבל אותם ישירותית לשילוח. הערוצים אלו מאורגנים לפי אזורים גיאוגרפיים, כדי לשפר את קבלת השילוחים.
איך זאת פועל?
התהליך פשוט למדי. קודם כל, יש להצטרף לערוץ טלגראס הרלוונטי לאזור המחיה. שם אפשר לצפות בתפריטי המוצרים המגוונים ולהזמין עם הפריטים הרצויים. לאחר השלמת ההזמנה וסיום התשלום, השליח יופיע בכתובת שצוינה עם החבילה המוזמנת.
רוב ערוצי הטלגראס מספקים טווח נרחב מ מוצרים – זנים של מריחואנה, עוגיות, משקאות ועוד. כמו כן, ניתן לראות ביקורות של לקוחות קודמים על רמת הפריטים והשירות.
יתרונות הנעשה באפליקציה
יתרון עיקרי מ טלגראס הינו הנוחיות והפרטיות. ההזמנה והתהליך מתבצעות מרחוק מאיזשהו מקום, בלי צורך בהתכנסות פיזי. כמו כן, האפליקציה מאובטחת היטב ומבטיחה סודיות גבוהה.
מלבד אל כך, עלויות המוצרים בפלטפורמה נוטים להיות זולים, והשילוחים מגיעים במהירות ובמסירות גבוהה. קיים אף מרכז תמיכה זמין לכל שאלה או בעיית.
סיכום
האפליקציה הינה דרך חדשנית ויעילה לקנות מוצרי מריחואנה במדינה. זו משלבת את הנוחיות הדיגיטלית מ היישומון הפופולרי, לבין המהירות והדיסקרטיות מ דרך המשלוח הישירה. ככל שהדרישה לקנאביס גדלה, פלטפורמות כמו זו צפויות להמשיך ולהתפתח.
Как похудеть
Слов про « лишний сахар» девочка не поняла. Какая разница, если еда вкусная? Мужчина в это время молча уплетал омлет и представлял что-то повкуснее. После трапезы все отправились по своим делам, в школу или на работу. Татьяна была, по всей видимости, счастливее всех, что нельзя было сказать про её близких. Через пару часов у станка Павел уже был голодным, овощи и яйца не смогли набить его большой желудок. От голода сводились пальцы на ногах, голова пульсировала и разум мутнел. Пришлось экстренно уйти на обед:
—Мужики, я в буфет! Жена удумала худеть, так всех нас этой пытке подвергла. Поел я этой травы, а смысл, если голодный?
—Ну, Петрович, крепись! Зато потом атлетами будете все. Только моей Маринке даже не заикайтесь, а то и меня на голод посадит.
Михалыч – коллега Павла и просто хороший мужик – лишь посмеялся с его высказываний, даже не осознав всей серьезности этого дела. В это время представитель сильного пола стоял возле стойки с десертами. Чего там только не было! А пирожное картошка особо привлекала его взгляд, так и манила к себе. Немедля Павел обратился к буфетчице:
—Дайте мне пять пирожных…. А нет, стойте. Не буду брать.
индивид вовсе не ожидал из уст родной жены Татьяны. В этой семье конституция плоти абсолютно не соответствовала от общепринятой также утвердившейся – иметь предожирение непреложная правило.
Геракл24: Опытная Замена Основания, Венцов, Покрытий и Перемещение Строений
Фирма Геракл24 профессионально занимается на выполнении полных услуг по реставрации основания, венцов, полов и перемещению зданий в населённом пункте Красноярском регионе и за его пределами. Наша команда квалифицированных экспертов обеспечивает высокое качество реализации всех видов ремонтных работ, будь то деревянные, каркасные, из кирпича или из бетона здания.
Преимущества работы с Геракл24
Профессионализм и опыт:
Все работы выполняются исключительно опытными специалистами, имеющими большой стаж в сфере возведения и реставрации домов. Наши специалисты эксперты в своей области и выполняют задачи с максимальной точностью и вниманием к деталям.
Всесторонний подход:
Мы предоставляем полный спектр услуг по ремонту и восстановлению зданий:
Реставрация фундамента: усиление и реставрация старого основания, что обеспечивает долгий срок службы вашего здания и устранить проблемы, связанные с оседанием и деформацией.
Замена венцов: восстановление нижних венцов деревянных зданий, которые чаще всего гниют и разрушаются.
Смена настилов: замена старых полов, что существенно улучшает визуальное восприятие и функциональность помещения.
Перемещение зданий: безопасное и надежное перемещение зданий на другие участки, что позволяет сохранить ваше строение и предотвращает лишние расходы на возведение нового.
Работа с любыми типами домов:
Деревянные дома: реставрация и усиление деревянных элементов, защита от гниения и вредителей.
Каркасные дома: укрепление каркасов и смена поврежденных частей.
Кирпичные строения: реставрация кирпичной кладки и укрепление стен.
Бетонные строения: ремонт и укрепление бетонных конструкций, ремонт трещин и дефектов.
Надежность и долговечность:
Мы работаем с только проверенные материалы и современное оборудование, что обеспечивает долгий срок службы и надежность всех работ. Каждый наш проект проходят тщательную проверку качества на всех этапах выполнения.
Личный подход:
Каждому клиенту мы предлагаем персонализированные решения, с учетом всех особенностей и пожеланий. Мы стараемся, чтобы конечный результат соответствовал ваши ожидания и требования.
Почему выбирают Геракл24?
Работая с нами, вы найдете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы обеспечиваем выполнение всех работ в сроки, установленные договором и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете не сомневаться, что ваше строение в надежных руках.
Мы предлагаем консультацию и ответить на все ваши вопросы. Контактируйте с нами, чтобы обсудить ваш проект и узнать о наших сервисах. Мы обеспечим сохранение и улучшение вашего дома, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
Bản cài đặt B29 IOS – Giải pháp vượt trội cho các tín đồ iOS
Trong thế giới công nghệ đầy sôi động hiện nay, trải nghiệm người dùng luôn là yếu tố then chốt. Với sự ra đời của Bản cài đặt B29 IOS, người dùng sẽ được hưởng trọn vẹn những tính năng ưu việt, mang đến sự hài lòng tuyệt đối. Hãy cùng khám phá những ưu điểm vượt trội của bản cài đặt này!
Tính bảo mật tối đa
Bản cài đặt B29 IOS được thiết kế với mục tiêu đảm bảo an toàn dữ liệu tuyệt đối cho người dùng. Nhờ hệ thống mã hóa hiện đại, thông tin cá nhân và dữ liệu nhạy cảm của bạn luôn được bảo vệ an toàn khỏi những kẻ xâm nhập trái phép.
Trải nghiệm người dùng đỉnh cao
Giao diện thân thiện, đơn giản nhưng không kém phần hiện đại, B29 IOS mang đến cho người dùng trải nghiệm duyệt web, truy cập ứng dụng và sử dụng thiết bị một cách trôi chảy, mượt mà. Các tính năng thông minh được tối ưu hóa, giúp nâng cao hiệu suất và tiết kiệm pin đáng kể.
Tính tương thích rộng rãi
Bản cài đặt B29 IOS được phát triển với mục tiêu tương thích với mọi thiết bị iOS từ các dòng iPhone, iPad cho đến iPod Touch. Dù là người dùng mới hay lâu năm của hệ điều hành iOS, B29 đều mang đến sự hài lòng tuyệt đối.
Quá trình cài đặt đơn giản
Với những hướng dẫn chi tiết, việc cài đặt B29 IOS trở nên nhanh chóng và dễ dàng. Chỉ với vài thao tác đơn giản, bạn đã có thể trải nghiệm ngay tất cả những tính năng tuyệt vời mà bản cài đặt này mang lại.
Bản cài đặt B29 IOS không chỉ là một bản cài đặt đơn thuần, mà còn là giải pháp công nghệ hiện đại, nâng tầm trải nghiệm người dùng lên một tầm cao mới. Hãy trở thành một phần của cộng đồng sử dụng B29 IOS để khám phá những tiện ích tuyệt vời mà nó có thể mang lại!
How to lose weight
The daughter stood in surprise and fidgeted with the hem of her dress, occasionally lifting her eyes to her father. She didn’t really understand the meaning of the words, but reading her father’s emotions, it made her feel uneasy. The chips from the cart were returned to the shelf, followed by the sad gaze of the man:
— Okay… So are we really dieting? And what made you decide so suddenly? We were living just fine…
— We’ll discuss it later. Not now.
מבורכים הנהנים לאזור המידע והסיוע הרשמי והמוסמך של טלגרף כיוונים! במקום רשאים למצוא את מלוא המידע והמסמכים העדכני והמעודכן הזמין והרלוונטי בנוגע ל פלטפורמה טלגרף וכלים להפעלתה כנדרש.
מה מציין טלגרף מסלולים?
טלגרמות כיוונים מציינת מנגנון הנשענת על טלגרם המספקת לשיווק ויישום מסביב קנאביס ודשא בישראל. באמצעות הפרסומים והחוגים בטלגראס, פעילים יכולים להזמין ולקבל מוצרי קנאביס בצורה קל ומיידי.
באיזה אופן להיכנס בטלגרם?
לשם להיכנס בשימוש בטלגראס כיוונים, עליכם להיות חברים ב לקבוצות ולקבוצות המאומתים. כאן באתר זה אפשר לאתר ולמצוא מבחר עבור קישורים למקומות מאומתים וימינים. לאחר מכן, רשאים להיכנס בשלבים הרכישה והקבלה של אספקת הקנאביס.
הדרכות ופרטים
באזור זה תמצאו מגוון של הדרכות והסברים ברורים בנוגע ל השימוש בטלגראס כיוונים, כולל:
– החברות לערוצים איכותיים
– פעילות האספקה
– הגנה והגנה בשילוב בטלגראס
– והרבה תוכן נוסף לכך
צירים מאומתים
להלן צירים לערוצים ולקבוצות איכותיים בפלטפורמת טלגרם:
– מקום הפרטים והעדכונים המוסמך
– מקום הייעוץ והתמיכה למעוניינים
– קבוצה לקבלת מוצרי דשא אמינים
– מדריך חנויות קנאביס מאומתות
אנו מאחלים את כולם על השתייכותכם למרכז המידע והידע של טלגרם נתיבים ומתקווים עבורכם חוויית צריכה נעימה ומוגנת!
I will immediately grasp your rss feed as I can not find your e-mail subscription hyperlink or newsletter service.
Do you’ve any? Please permit me recognize in order
that I may subscribe. Thanks.
Замена венцов красноярск
Gerakl24: Опытная Реставрация Основания, Венцов, Настилов и Перенос Строений
Фирма Геракл24 занимается на выполнении комплексных работ по смене фундамента, венцов, настилов и переносу домов в городе Красноярск и в окрестностях. Наш коллектив опытных экспертов обещает отличное качество реализации всех типов ремонтных работ, будь то древесные, каркасного типа, кирпичные или бетонные дома.
Достоинства работы с Геракл24
Профессионализм и опыт:
Весь процесс выполняются только опытными экспертами, с многолетним долгий стаж в направлении создания и ремонта зданий. Наши специалисты эксперты в своей области и выполняют проекты с максимальной точностью и вниманием к деталям.
Всесторонний подход:
Мы предлагаем разнообразные услуги по восстановлению и ремонту домов:
Реставрация фундамента: укрепление и замена старого фундамента, что гарантирует долговечность вашего строения и избежать проблем, связанные с оседанием и деформацией строения.
Реставрация венцов: реставрация нижних венцов из дерева, которые обычно подвержены гниению и разрушению.
Установка новых покрытий: монтаж новых настилов, что кардинально улучшает внешний облик и функциональные характеристики.
Передвижение домов: безопасное и надежное перемещение зданий на другие участки, что помогает сохранить здание и избежать дополнительных затрат на создание нового.
Работа с любыми типами домов:
Древесные строения: восстановление и укрепление деревянных конструкций, защита от разрушения и вредителей.
Каркасные дома: усиление каркасных конструкций и реставрация поврежденных элементов.
Кирпичные строения: ремонт кирпичных стен и укрепление конструкций.
Бетонные дома: восстановление и укрепление бетонных структур, ремонт трещин и дефектов.
Надежность и долговечность:
Мы работаем с только высококачественные материалы и современное оборудование, что гарантирует долгий срок службы и надежность всех работ. Все наши проекты проходят строгий контроль качества на каждом этапе выполнения.
Персонализированный подход:
Каждому клиенту мы предлагаем подходящие решения, учитывающие все особенности и пожелания. Наша цель – чтобы итог нашей работы соответствовал вашим запросам и желаниям.
Почему выбирают Геракл24?
Обратившись к нам, вы найдете надежного партнера, который берет на себя все заботы по восстановлению и ремонту вашего здания. Мы гарантируем выполнение всех работ в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете быть спокойны, что ваш дом в надежных руках.
Мы всегда готовы проконсультировать и ответить на все ваши вопросы. Свяжитесь с нами, чтобы обсудить детали вашего проекта и узнать больше о наших услугах. Мы сохраним и улучшим ваш дом, сделав его безопасным и комфортным для проживания на долгие годы.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
Психология в рассказах, истории из жизни.
Brazil floods Update: Death toll reaches 143 as rain continue to pour, several crimes reported Manchester United performance and form graph is a Sofascore unique algorithm that we are generating from the team’s last 10 matches, statistics, detailed analysis and our own knowledge. MORE Live Cricket Match Score : }1 There are also statistics for each player in all competitions with all total played and started matches, minutes played, number of goals scored, number of cards and much more. Match 65 – Barsapara Cricket Stadium, Guwahati Nottingham won by 9 wickets Thushara slides one into the pad and Abhishek gets off strike with a leg-bye. Beaten! Another slingy delivery on the full and Head makes room for a swipe but the ball skids on through, inches away from the leg-stump. He follows up with a drive to long-on for one run. Thushara finds the inside-edge yet again as Abhishek attempts a flick across the line. Thushara overpitches outside off and Head slams it down to the long-off fence for FOUR this time.
https://www.pr5-articles.com/Articles-of-2024/click
OFFICIAL STRATEGIC TIMEOUT PARTNER Get the latest scores on the go. Find the latest content, including match highlights, press conferences and recap all at your fingertips by downloading the official IPL app. Most No-Balls Bowled In IPL 2024 So Far – In Pics DC won by 20 runs Final Match 26 May 2024, 07:30 PM (IST) Buy Print It has been officially announced that the 17th season of the TATA IPL will begin on March 22, 2024. Here is the complete schedule of the IPL 2024: Ten teams took part in the IPL in 2024. In a round-robin format, each team plays the other nine teams both at home and away. The top four teams advance to the play-offs. The Qualifier 1 will compete the top two teams in the league against one another, with the winner moving on to the final. Teams in third and fourth place will play each other in an elimination round. The team that wins the eliminator will play in a Qualifier 2 against the team that loses the Qualifier 1. Qualifier 2’s winner reach to final match.
сеть сайтов pbn
Работая в поисковой оптимизации, нужно осознавать, что невозможно одним методом вывести веб-сайт в верхние позиции поисковиков, поскольку поисковики это как дорожка с финишной прямой, а сайты это автомобили для гонок, которые все стремятся быть первыми.
Так вот:
Перечень – Для того чтобы сайт был приспособлен и быстрым, важна
улучшение
Сайт должен содержать только уникальные материалы, это тексты и изображения
В ОБЯЗАТЕЛЬНОМ ПОРЯДКЕ ссылочная масса через сайты с статьями и напрямую на основную страницу
Увеличение беклинков с использованием дополнительных сайтов
Пирамида ссылок, эти ссылки Tier-1, второго уровня, Tier-3
И самое главное это сеть сайтов PBN, которая подключается на манисайт
Все сайты PBN должны быть без следов, т.е. системы поиска не должны понимать, что это один владелец всех интернет-ресурсов, поэтому крайне важно следовать все эти правила.
Геракл24: Профессиональная Реставрация Фундамента, Венцов, Настилов и Перенос Зданий
Фирма Геракл24 специализируется на оказании всесторонних сервисов по реставрации основания, венцов, покрытий и перемещению строений в населённом пункте Красноярске и за его пределами. Наша группа опытных мастеров гарантирует высокое качество выполнения всех типов восстановительных работ, будь то из дерева, с каркасом, кирпичные или бетонные конструкции дома.
Плюсы сотрудничества с Gerakl24
Квалификация и стаж:
Все работы осуществляются только высококвалифицированными экспертами, с обладанием большой стаж в области строительства и восстановления строений. Наши сотрудники знают свое дело и выполняют проекты с безупречной точностью и вниманием к деталям.
Полный спектр услуг:
Мы осуществляем разнообразные услуги по ремонту и ремонту домов:
Смена основания: замена и укрепление фундамента, что обеспечивает долгий срок службы вашего здания и предотвратить проблемы, связанные с оседанием и деформацией.
Смена венцов: замена нижних венцов деревянных домов, которые чаще всего гниют и разрушаются.
Замена полов: замена старых полов, что существенно улучшает внешний вид и практическую полезность.
Передвижение домов: безопасное и надежное перемещение зданий на новые места, что позволяет сохранить ваше строение и избежать дополнительных затрат на создание нового.
Работа с любыми типами домов:
Древесные строения: реставрация и усиление деревянных элементов, защита от гниения и вредителей.
Каркасные строения: усиление каркасных конструкций и реставрация поврежденных элементов.
Кирпичные строения: ремонт кирпичных стен и укрепление стен.
Бетонные строения: ремонт и укрепление бетонных конструкций, ремонт трещин и дефектов.
Качество и надежность:
Мы применяем лишь качественные материалы и новейшее оборудование, что гарантирует долговечность и надежность всех работ. Каждый наш проект проходят строгий контроль качества на каждой стадии реализации.
Персонализированный подход:
Каждому клиенту мы предлагаем индивидуальные решения, учитывающие ваши требования и желания. Наша цель – чтобы результат нашей работы полностью соответствовал ваши ожидания и требования.
Зачем обращаться в Геракл24?
Обратившись к нам, вы получаете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы гарантируем выполнение всех проектов в сроки, установленные договором и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете быть спокойны, что ваш дом в надежных руках.
Мы готовы предоставить консультацию и ответить на все ваши вопросы. Звоните нам, чтобы обсудить детали вашего проекта и узнать о наших сервисах. Мы поможем вам сохранить и улучшить ваш дом, сделав его уютным и безопасным для долгого проживания.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
線上娛樂城的世界
隨著網際網路的飛速發展,網上娛樂城(網上賭場)已經成為許多人消遣的新選擇。在線娛樂城不僅提供多元化的遊戲選擇,還能讓玩家在家中就能體驗到賭場的刺激和樂趣。本文將探討網上娛樂城的特點、利益以及一些常見的的遊戲。
什麼是在線娛樂城?
網上娛樂城是一種經由互聯網提供博彩遊戲的平台。玩家可以通過電腦設備、智能手機或平板進入這些網站,參與各種賭錢活動,如撲克牌、賭盤、21點和老虎机等。這些平台通常由專家的程序公司開發,確保遊戲的公正性和安全性。
在線娛樂城的好處
便利性:玩家不用離開家,就能享受博彩的興奮。這對於那些居住在遠離實體賭場區域的人來說尤其方便。
多樣化的游戲選擇:在線娛樂城通常提供比實體賭場更豐富的游戲選擇,並且經常改進遊戲內容,保持新鮮感。
福利和獎勵計劃:許多線上娛樂城提供豐富的獎金計劃,包括註冊紅利、存款紅利和會員計劃,吸引新新玩家並激勵老玩家持續遊戲。
穩定性和隱私性:正規的在線娛樂城使用先進的的加密來保護玩家的個人信息和交易,確保遊戲過程的穩定和公平。
常有的在線娛樂城游戲
撲克:撲克是最受歡迎的賭錢游戲之一。在線娛樂城提供多樣撲克牌變體,如德州撲克、奧馬哈撲克和七張牌等。
輪盤:輪盤是一種經典的賭博遊戲,玩家可以下注在數字、數字排列或顏色選擇上,然後看小球落在哪個地方。
21點:又稱為二十一點,這是一種對比玩家和莊家點數點數的遊戲,目標是讓手牌點數點數儘量接近21點但不超過。
吃角子老虎:老虎機是最簡單也是最常見的賭博遊戲之一,玩家只需旋轉捲軸,等待圖案排列出獲勝的組合。
結尾
在線娛樂城為當代賭博愛好者提供了一個方便、興奮且多樣化的娛樂方式。不論是撲克迷還是老虎机愛好者,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的的不斷進步,網上娛樂城的遊戲體驗將變化越來越現實和引人入勝。然而,玩家在享受遊戲的同時,也應該自律,避免沉溺於賭博活動,保持健康健康的心態。
網上娛樂城的世界
隨著網際網路的快速發展,線上娛樂城(在線賭場)已經成為許多人娛樂的新選擇。在線娛樂城不僅提供多元化的遊戲選擇,還能讓玩家在家中就能體驗到賭場的刺激和快感。本文將探討線上娛樂城的特徵、好處以及一些常見的游戲。
什麼是線上娛樂城?
線上娛樂城是一種經由互聯網提供賭博游戲的平台。玩家可以經由電腦、智慧型手機或平板進入這些網站,參與各種賭錢活動,如撲克牌、輪盤、21點和吃角子老虎等。這些平台通常由專家的軟體公司開發,確保游戲的公正性和安全性。
在線娛樂城的好處
方便性:玩家無需離開家,就能體驗賭博的興奮。這對於那些居住在遠離的實體賭場區域的人來說尤其方便。
多元化的遊戲選擇:網上娛樂城通常提供比實體賭場更多的遊戲選擇,並且經常升級遊戲內容,保持新鮮感。
好處和獎勵計劃:許多在線娛樂城提供豐厚的優惠計劃,包括註冊獎勵、存款紅利和忠誠計劃,引誘新玩家並鼓勵老玩家不斷遊戲。
穩定性和保密性:正規的在線娛樂城使用高端的加密技術來保護玩家的個人資料和金融交易,確保游戲過程的安全和公平。
常有的線上娛樂城游戲
撲克:撲克牌是最流行賭博遊戲之一。線上娛樂城提供多種撲克牌變體,如德州扑克、奧馬哈和七張撲克等。
輪盤賭:輪盤賭是一種傳統的賭博遊戲,玩家可以賭注在單數、數字組合上或顏色上上,然後看小球落在哪個位置。
21點:又稱為二十一點,這是一種競爭玩家和莊家點數點數的遊戲,目標是讓手牌點數儘量接近21點但不超過。
老虎機:老虎机是最容易也是最流行的賭博遊戲之一,玩家只需轉動捲軸,等待圖案圖案排列出贏得的組合。
結尾
線上娛樂城為現代的賭博愛好者提供了一個方便、刺激且豐富的娛樂活動。無論是撲克迷還是吃角子老虎迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的不斷提升,網上娛樂城的遊戲體驗將變得越來越逼真和引人入勝。然而,玩家在享受遊戲的同時,也應該保持自律,避免過度沉迷於博彩活動,維持健康的遊戲心態。
Daily bonuses
Uncover Stimulating Bonuses and Extra Spins: Your Complete Guide
At our gaming platform, we are focused to providing you with the best gaming experience possible. Our range of promotions and bonus spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our awesome deals and what makes them so special.
Lavish Extra Spins and Rebate Promotions
One of our standout promotions is the opportunity to earn up to 200 bonus spins and a 75% cashback with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This amazing offer allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Promotions
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit promotion available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our promotions are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, rebate, or plentiful deposit bonuses, we have something for everyone. Join us today, take advantage of these amazing offers, and start your journey to big wins and endless fun. Happy gaming!
sapporo88
sapporo88
Engaging Advancements and Iconic Games in the World of Videogames
In the ever-evolving landscape of videogames, there’s always something new and engaging on the horizon. From mods improving revered mainstays to upcoming launches in renowned brands, the interactive entertainment landscape is prospering as in recent memory.
Let’s take a glimpse into the latest announcements and specific the renowned titles mesmerizing audiences internationally.
Up-to-Date News
1. Groundbreaking Enhancement for The Elder Scrolls V: Skyrim Elevates NPC Aesthetics
A latest mod for The Elder Scrolls V: Skyrim has caught the focus of fans. This customization implements lifelike heads and realistic hair for each non-player characters, elevating the experience’s visuals and immersiveness.
2. Total War Series Title Placed in Star Wars Universe Galaxy in Development
The Creative Assembly, acclaimed for their Total War Games franchise, is reportedly crafting a new experience situated in the Star Wars Setting universe. This captivating combination has enthusiasts eagerly anticipating the strategic and compelling journey that Total War Series releases are acclaimed for, at last situated in a realm far, far away.
3. Grand Theft Auto VI Debut Announced for Q4 2025
Take-Two Interactive’s Leader has announced that Grand Theft Auto VI is set to release in Autumn 2025. With the overwhelming popularity of its predecessor, GTA V, enthusiasts are anticipating to see what the next entry of this renowned franchise will bring.
4. Growth Developments for Skull and Bones Season Two
Developers of Skull and Bones have announced enhanced developments for the title’s sophomore season. This swashbuckling experience promises fresh updates and changes, engaging fans captivated and enthralled in the world of oceanic seafaring.
5. Phoenix Labs Studio Deals with Workforce Reductions
Unfortunately, not everything announcements is uplifting. Phoenix Labs Studio, the studio behind Dauntless Game, has communicated large-scale workforce reductions. In spite of this obstacle, the title keeps to be a beloved preference across gamers, and the company continues to be focused on its fanbase.
Iconic Experiences
1. The Witcher 3: Wild Hunt
With its immersive narrative, engrossing domain, and compelling gameplay, The Witcher 3: Wild Hunt keeps a cherished release within players. Its expansive narrative and expansive free-roaming environment persist to attract gamers in.
2. Cyberpunk
Despite a rocky launch, Cyberpunk 2077 Game keeps a long-awaited release. With constant updates and enhancements, the title persists in improve, delivering gamers a perspective into a dystopian environment filled with mystery.
3. GTA V
Yet time post its first arrival, GTA V keeps a popular option among gamers. Its sprawling sandbox, captivating narrative, and co-op experiences keep enthusiasts coming back for further adventures.
4. Portal Game
A iconic puzzle title, Portal Game is praised for its innovative features and brilliant level design. Its demanding puzzles and humorous dialogue have established it as a remarkable game in the gaming landscape.
5. Far Cry
Far Cry 3 is praised as exceptional titles in the brand, offering players an open-world journey filled with excitement. Its engrossing narrative and memorable personalities have confirmed its place as a iconic experience.
6. Dishonored Series
Dishonored is acclaimed for its stealthy mechanics and distinctive environment. Enthusiasts embrace the character of a otherworldly assassin, traversing a metropolis rife with governmental intrigue.
7. Assassin’s Creed Game
As part of the iconic Assassin’s Creed Series lineup, Assassin’s Creed 2 is adored for its engrossing story, compelling gameplay, and period realms. It stays a exceptional release in the franchise and a beloved amidst enthusiasts.
In conclusion, the universe of gaming is vibrant and ever-changing, with new advan
JiliAce ক্যাসিনোতে মাছ ধরা এবং টেবিল গেম: অনলাইন গেমিংয়ের এক নতুন অভিজ্ঞতা
অনলাইন গেমিংয়ের জগতে JiliAce ক্যাসিনো একটি গুরুত্বপূর্ণ স্থান অধিকার করে নিয়েছে, যেখানে ব্যবহারকারীরা বিভিন্ন ধরণের গেম উপভোগ করতে পারেন। আজ আমরা JiliAce〡JitaBet-এর দুটি জনপ্রিয় গেম সম্পর্কে জানবো: মাছ ধরা এবং টেবিল গেম।
মাছ ধরা গেম: ভার্চুয়াল অভিজ্ঞতার মজা
মাছ ধরা একটি অনলাইন ফিশিং গেম বলতে সাধারণত একটি ভার্চুয়াল বা ডিজিটাল গেম বোঝায় যা মাছ ধরার অভিজ্ঞতাকে অনুকরণ করে। এই গেমগুলি তাদের জটিলতা, বাস্তবতা এবং উদ্দেশ্যের পরিপ্রেক্ষিতে ব্যাপকভাবে পরিবর্তিত হয়। JiliAce ক্যাসিনোতে আপনি বিভিন্ন ধরনের ফিশিং গেম খুঁজে পাবেন, যা আপনার দক্ষতা এবং ধৈর্য্যের পরীক্ষা নেবে। বাস্তবসম্মত গ্রাফিক্স এবং চমৎকার গেমপ্লে সহ, এই গেমগুলি আপনার জন্য এক অসাধারণ অভিজ্ঞতা প্রদান করবে।
টেবিল গেম: ঐতিহ্যবাহী খেলার ডিজিটাল রূপ
অনলাইন টেবিল গেমগুলি সাধারণত ইট-ও-মর্টার ক্যাসিনোগুলিতে পাওয়া ঐতিহ্যবাহী টেবিল গেমগুলির ডিজিটাল সংস্করণগুলিকে বোঝায়। এই গেমগুলি একটি শারীরিক টেবিলে খেলার অভিজ্ঞতাকে অনুকরণ করার জন্য ডিজাইন করা হয়েছে এবং এগুলি অনলাইন ক্যাসিনোতে জনপ্রিয়। JiliAce ক্যাসিনোতে আপনি ব্ল্যাকজ্যাক, রুলেট, পোকার এবং আরও অনেক টেবিল গেম উপভোগ করতে পারেন। Jili ace casino-এর ডিজিটাল প্ল্যাটফর্মে এই গেমগুলি খেলে আপনি ঐতিহ্যবাহী ক্যাসিনো অভিজ্ঞতার স্বাদ পাবেন, যেটি আপনি ঘরে বসেই উপভোগ করতে পারবেন।
সহজ লগইন এবং সুবিধাজনক গেমিং
Jili ace login প্রক্রিয়া অত্যন্ত সহজ এবং ব্যবহারকারীদের জন্য সুবিধাজনক। একবার লগইন করলে, আপনি সহজেই বিভিন্ন গেমের অ্যাক্সেস পাবেন এবং আপনার পছন্দসই গেম খেলার জন্য প্রস্তুত হয়ে যাবেন। Jiliace login করার পর, আপনি আপনার গেমিং যাত্রা শুরু করতে পারবেন এবং বিভিন্ন ধরনের বোনাস ও পুরস্কার উপভোগ করতে পারবেন।
Jita Bet: বড় পুরস্কারের সুযোগ
JiliAce ক্যাসিনোতে Jita Bet-এর সাথে আপনার গেমিং অভিজ্ঞতা আরও সমৃদ্ধ করুন। এখানে আপনি বিভিন্ন ধরণের বাজি ধরতে পারেন এবং বড় পুরস্কার জিততে পারেন। Jita Bet প্ল্যাটফর্মটি ব্যবহারকারীদের জন্য সহজ এবং সুরক্ষিত বাজি ধরার সুযোগ প্রদান করে।
যোগদান করুন এবং উপভোগ করুন
JiliAce〡JitaBet-এর অংশ হয়ে আজই আপনার গেমিং যাত্রা শুরু করুন। Jili ace casino এবং Jita Bet-এ লগইন করে মাছ ধরা এবং টেবিল গেমের মত আকর্ষণীয় গেম উপভোগ করুন। এখনই যোগ দিন এবং অনলাইন গেমিংয়ের এক নতুন জগতে প্রবেশ করুন!
Jiliacet casino
Jiliacet casino |
Warm welcome! | Get a 200% Welcome Bonus when you log in jiliace casino.
IPL Tournament! | Join the IPL fever with Jita Bet. Win big prizes!
Epic JILI Tournaments! | Go head-to-head in the Jita bet Super Tournament
#jiliacecasino
Cashback on Deposits! | Get cash back on every deposit. At Jili ace casino
Uninterrupted bonuses at JITAACE! | Stay logged in Jiliace login!
https://www.jiliace-casino.online/bn
#Jiliacecasino # Jiliacelogin#Jiliacelogin # Jitabet
Slot Feast! | Spin to win 100% up to 20,000 ৳. at Jili ace login!
Big Fishing Bonus! | Get a 100% bonus up to ৳20,000 in the Fishing Game.
JiliAce Casino’s top choice for great bonuses. login, play, and win big today!
Daily bonuses
Discover Invigorating Deals and Free Spins: Your Comprehensive Guide
At our gaming platform, we are devoted to providing you with the best gaming experience possible. Our range of deals and bonus spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our fantastic deals and what makes them so special.
Generous Free Spins and Cashback Offers
One of our standout offers is the opportunity to earn up to 200 free spins and a 75% rebate with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This incredible promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Deals
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” promotions allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these fantastic opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, rebate, or bountiful deposit promotions, we have something for everyone. Join us today, take advantage of these amazing offers, and start your journey to big wins and endless fun. Happy gaming!
Daily bonuses
Explore Stimulating Offers and Free Spins: Your Ultimate Guide
At our gaming platform, we are devoted to providing you with the best gaming experience possible. Our range of bonuses and free rounds ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our awesome promotions and what makes them so special.
Bountiful Free Rounds and Cashback Bonuses
One of our standout offers is the opportunity to earn up to 200 free spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This amazing promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Bonuses
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 bonus spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our promotions come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy free spins, cashback, or plentiful deposit promotions, we have something for everyone. Join us today, take advantage of these incredible deals, and start your journey to big wins and endless fun. Happy gaming!
बेटवीसा ऑनलाइन कैसीनो पर अन्य रोमांचक गेम्स का आनंद
ऑनलाइन कैसीनो में बैकारेट, पोकर और क्रैप्स जैसे गेम भी बहुत लोकप्रिय और उत्साहजनक हैं। बेटवीसा ऑनलाइन कैसीनो इन सभी गेम्स के विभिन्न वेरिएंट्स प्रदान करता है, जो खिलाड़ियों को अनूठा और रोमांचक अनुभव प्रदान करते हैं।
बैकारेट:
बैकारेट एक उच्च-श्रेणी का कार्ड गेम है जो सादगी और रोमांच का अद्भुत मिश्रण प्रदान करता है। बेटवीसा ऑनलाइन कैसीनो पर उपलब्ध बैकारेट वेरिएंट्स में पंटो बंको और लाइव बैकारेट शामिल हैं।
पंटो बंको बैकारेट का सबसे सामान्य रूप है, जहां खेल का लक्ष्य 9 के करीब पहुंचना होता है। वहीं, लाइव बैकारेट लाइव डीलर के साथ खेला जाता है और खिलाड़ियों को असली कैसीनो जैसा अनुभव प्रदान करता है।
पोकर:
पोकर एक रणनीतिक और कौशल-आधारित कार्ड गेम है जो खिलाड़ियों के बीच अत्यधिक लोकप्रिय है। बेटवीसा पर आप टेक्सास होल्ड’एम और ओमाहा पोकर जैसे विभिन्न पोकर वेरिएंट्स खेल सकते हैं।
टेक्सास होल्ड’एम सबसे लोकप्रिय पोकर वेरिएंट है, जिसमें दो निजी और पांच सामुदायिक कार्ड का उपयोग किया जाता है। ओमाहा पोकर भी टेक्सास होल्ड’एम के समान है, लेकिन इसमें चार निजी और पांच सामुदायिक कार्ड होते हैं।
क्रैप्स:
क्रैप्स एक डाइस गेम है जो तेज गति और उत्साह से भरा होता है। यह गेम भाग्य और रणनीति का मिश्रण है, जिसमें खिलाड़ियों को विभिन्न प्रकार की शर्तें लगाने का मौका मिलता है। बेटवीसा इंडिया में आप इस रोमांचक गेम का आनंद ले सकते हैं।
बेटवीसा लॉगिन करके या बेटवीसा ऐप डाउनलोड करके आप इन दिलचस्प और चुनौतीपूर्ण गेम्स का आनंद ले सकते हैं। चाहे आप बैकारेट की सादगी का मजा लेना चाहते हों या पोकर की रणनीतिक गहराई को समझना चाहते हों, बेटवीसा ऑनलाइन कैसीनो आपके लिए सबकुछ प्रदान करता है।
इन गेम्स को खेलकर आप अपने ऑनलाइन कैसीनो अनुभव को और भी रोमांचक बना सकते हैं। इसलिए, बेटवीसा इंडिया में जाकर इन गेम्स का आनंद लेना न भूलें!
Betvisa Bet
Betvisa Bet | Catch the BPL Excitement with Betvisa!
Hunt for ₹10million! | Enter the BPL at Betvisa and chase a staggering Bounty.
Valentine’s Boost at Visa Bet! | Feel the rush of a 143% Love Mania Bonus .
predict BPL T20 outcomes | score big rewards through Betvisa login!
#betvisa
Betvisa bonus Win! | Leverage your 10 free spins to possibly win $8,888.
Share and Earn! | win ₹500 via the Betvisa app download!
https://www.betvisa-bet.com/hi
#visabet #betvisalogin #betvisaapp #betvisaIndia
Sign-Up Jackpot! | Register at Betvisa India and win ₹8,888.
Double your play! | with a ₹1,000 deposit and get ₹2,000 free at Betvisa online!
Download the Betvisa download today and don’t miss out on the action!
বেটভিসার সাথে আপনার আইপিএল বেটিংকে উন্নত করুন: উত্তেজনাপূর্ণ স্লট, পুরস্কৃত বোনাস এবং অতুলনীয় রোমাঞ্চ
ইন্ডিয়ান প্রিমিয়ার লিগ (আইপিএল) এর জন্য প্রত্যাশা একটি জ্বরের পিচে পৌঁছেছে, বেটভিসা একটি অতুলনীয় গেমিং অভিজ্ঞতার জন্য ক্রীড়া বেটিং উত্সাহীদের জন্য প্রধান গন্তব্য হিসাবে আবির্ভূত হয়েছে৷ রোমাঞ্চকর স্লট এবং ফিশিং গেম থেকে শুরু করে লোভনীয় স্পোর্টস বোনাস পর্যন্ত বিভিন্ন ধরনের অফার সহ, Betvisa আসন্ন IPL মৌসুমে আপনাকে জয়ের দিকে এগিয়ে নিয়ে যেতে প্রস্তুত।
Betvisa স্লট এবং ফিশিং গেমে নিজেকে নিমজ্জিত করুন
Betvisa একটি সু-বৃত্তাকার গেমিং অভিজ্ঞতা প্রদানের গুরুত্ব বোঝে, এবং এটি সঠিকভাবে প্রদান করে। আপনি স্লটের অ্যাড্রেনালিন-জ্বালানি উত্তেজনা বা মাছ ধরার গেমের মনোমুগ্ধকর লোভের জন্য মেজাজে থাকুন না কেন, Betvisa প্ল্যাটফর্ম একটি বৈচিত্র্যপূর্ণ নির্বাচন অফার করে যা আপনার প্রতিটি ইচ্ছা পূরণ করে। নিরবিচ্ছিন্ন Betvisa লগইন প্রক্রিয়ার মাধ্যমে, আপনি সহজেই বিনোদনের এই বিশাল অ্যারে অ্যাক্সেস করতে পারেন, আপনার উত্তেজনার মাত্রা ধারাবাহিকভাবে 200%-এ রয়েছে তা নিশ্চিত করে।
Betvisa বোনাসের মাধ্যমে আপনার IPL বেটিং পুরষ্কার সর্বাধিক করুন
আইপিএল মরসুম যত ঘনিয়ে আসছে, বেটভিসা তার বিশ্বস্ত ব্যবহারকারীদের ব্যতিক্রমী স্পোর্টস বোনাস দিয়ে পুরস্কৃত করতে আগ্রহী। IPL সিজনে ₹5,000 পর্যন্ত বোনাস স্কোর করুন এবং আপনার বেটিং অভিজ্ঞতাকে নতুন উচ্চতায় উন্নীত করুন। এই উদার অফারটি আপনাকে আপনার ব্যাঙ্করোলকে আরও প্রসারিত করতে দেয়, আইপিএল বাজির উচ্চ-স্টেকের বিশ্বে আপনার বিজয়ী হওয়ার সম্ভাবনা বৃদ্ধি করে৷
Betvisa Bangladesh অ্যাডভান্টেজকে আলিঙ্গন করুন
বাংলাদেশের Betvisa ব্যবহারকারীদের জন্য, প্ল্যাটফর্মের স্থানীয় পদ্ধতি একটি নির্বিঘ্ন এবং উপযোগী অভিজ্ঞতা নিশ্চিত করে। Betvisa Bangladesh লগইন প্রক্রিয়ার মাধ্যমে, আপনি সহজেই IPL বেটিং অপশনের বিস্তৃত পরিসরে প্রবেশ করতে পারবেন, বিশেষ করে বাংলাদেশী বাজারের পছন্দের জন্য। বিশদের প্রতি এই মনোযোগ বেটভিসাকে আলাদা করে, আপনাকে সত্যিকারের নিমগ্ন এবং পুরস্কৃত করার অভিজ্ঞতা প্রদান করে।
Betvisa অ্যাপের শক্তি ব্যবহার করুন
আজকের দ্রুত-গতির বিশ্বে, সুবিধাই মুখ্য, এবং Betvisa এটি পুরোপুরি বোঝে। Betvisa অ্যাপটি একটি ব্যবহারকারী-বান্ধব এবং স্বজ্ঞাত প্ল্যাটফর্ম অফার করে, যা আপনাকে যেতে যেতে আপনার প্রিয় স্লট, মাছ ধরার গেম এবং ক্রীড়া বাজি বাজার অ্যাক্সেস করতে দেয়। আপনি যাতায়াত করছেন, লাইনে অপেক্ষা করছেন বা কেবল উত্তেজনার মুহূর্ত খুঁজছেন, Betvisa অ্যাপটি গেমের রোমাঞ্চকে আপনার নখদর্পণে রাখে।
Betvisa: আপনার গেটওয়ে আইপিএল বেটিং আধিপত্য
আইপিএল মরসুম যত ঘনিয়ে আসছে, বেটভিসা ক্রীড়া বাজি উত্সাহীদের জন্য চূড়ান্ত গন্তব্য হিসাবে আবির্ভূত হয়েছে৷ এর বৈচিত্র্যময় গেমিং অফার, উদার বোনাস এবং Betvisa বাংলাদেশ ব্যবহারকারীদের জন্য উপযোগী অভিজ্ঞতা সহ, প্ল্যাটফর্মটি আপনার বেটিং যাত্রাকে নতুন উচ্চতায় উন্নীত করতে প্রস্তুত। একটি আনন্দদায়ক IPL মরসুমের জন্য প্রস্তুত হন এবং Betvisa আপনাকে চূড়ান্ত বিজয়ের দিকে এগিয়ে নিয়ে যেতে দিন।
Betvisa Bet | Hit it Big This IPL Season with Betvisa!
Betvisa login! | Every deposit during IPL matches earns a 2% bonus .
Betvisa Bangladesh! | IPL 2024 action heats up, your bets get more rewarding!
Crash Game returns! | huge ₹10 million jackpot. Take the lead on the Betvisa app !
#betvisa
Start Winning Now! | Sign up through Betvisa affiliate login, claim ₹500 free cash.
Grab Your Winning Ticket! | Register login and win ₹8,888 at visa bet!
https://www.betvisa-bet.com/bn
#visabet #betvisalogin #betvisabangladesh#betvisaapp
200% Excitement! | Enjoy slots and fishing games at Betvisa লগইন করুন!
Big Sports Bonuses! | Score up to ₹5,000 in sports bonuses during the IPL season
Gear up for an exhilarating IPL season at Betvisa, propels you towards victory!
Exciting Innovations and Beloved Releases in the World of Digital Entertainment
In the fluid realm of interactive entertainment, there’s constantly something innovative and thrilling on the brink. From modifications enhancing beloved classics to new arrivals in renowned franchises, the digital entertainment ecosystem is flourishing as ever.
We’ll take a look into the most recent news and some of the iconic games captivating audiences globally.
Up-to-Date Announcements
1. New Customization for Skyrim Elevates Non-Player Character Aesthetics
A latest customization for The Elder Scrolls V: Skyrim has grabbed the focus of fans. This enhancement introduces realistic faces and flowing hair for each (NPCs), enhancing the title’s aesthetics and depth.
2. Total War Series Game Placed in Star Wars Galaxy Universe in Development
Creative Assembly, renowned for their Total War Games series, is allegedly working on a upcoming game set in the Star Wars galaxy. This engaging integration has enthusiasts looking forward to the strategic and immersive experience that Total War Games games are acclaimed for, finally set in a realm distant.
3. GTA VI Arrival Revealed for Autumn 2025
Take-Two Interactive’s CEO’s Chief Executive Officer has communicated that GTA VI is planned to debut in Late 2025. With the enormous popularity of its predecessor, GTA V, fans are anticipating to see what the future entry of this celebrated universe will offer.
4. Extension Plans for Skull and Bones Season Two
Designers of Skull and Bones have announced enhanced strategies for the world’s next season. This swashbuckling experience promises upcoming updates and improvements, engaging players invested and absorbed in the domain of oceanic piracy.
5. Phoenix Labs Studio Faces Staff Cuts
Sadly, not every updates is favorable. Phoenix Labs Developer, the studio behind Dauntless Game, has disclosed large-scale personnel cuts. Regardless of this obstacle, the experience remains to be a renowned selection across gamers, and the team remains dedicated to its audience.
Beloved Titles
1. The Witcher 3: Wild Hunt
With its engaging story, captivating domain, and captivating adventure, The Witcher 3: Wild Hunt keeps a iconic experience across gamers. Its rich experience and expansive free-roaming environment keep to engage enthusiasts in.
2. Cyberpunk 2077
In spite of a tumultuous release, Cyberpunk Game keeps a long-awaited experience. With constant improvements and enhancements, the title keeps advance, providing fans a glimpse into a cyberpunk environment rife with peril.
3. Grand Theft Auto 5
Still years after its debut arrival, Grand Theft Auto V stays a popular preference among players. Its vast sandbox, engaging narrative, and multiplayer mode maintain fans revisiting for ongoing journeys.
4. Portal 2
A renowned problem-solving title, Portal is renowned for its pioneering systems and clever environmental design. Its challenging puzzles and humorous storytelling have established it as a noteworthy game in the interactive entertainment world.
5. Far Cry 3
Far Cry is celebrated as a standout games in the franchise, providing enthusiasts an sandbox adventure rife with excitement. Its captivating plot and legendary characters have established its status as a cherished title.
6. Dishonored Universe
Dishonored Universe is praised for its sneaky features and unique realm. Gamers assume the role of a mystical eliminator, exploring a urban environment teeming with governmental danger.
7. Assassin’s Creed
As part of the acclaimed Assassin’s Creed Series collection, Assassin’s Creed II is cherished for its engrossing experience, captivating systems, and era-based environments. It keeps a noteworthy experience in the collection and a favorite amidst gamers.
In conclusion, the universe of videogames is thriving and fluid, with innovative advan
স্বাগত বোনাসের সাথে সেরা ক্রিকেট গেইম প্লে করুন
ক্রিকেট এক খেলা না, এটি একটি প্রচন্ড উত্সাহের অভিবাদন। এই খেলাটি নিয়মিতভাবে বড় আকর্ষণ প্রদান করে বিভিন্ন বিশ্বকাপ এবং অন্যান্য টুর্নামেন্টে। ক্রিকেট উপাদানের অধিকাংশ ক্রিকেট প্রেমিকেরা এটি দেখতে পছন্দ করেন।
ক্রিকেটে বাজিয়ে ওঠা গতি, তাদের দেখার প্রকৃতির জন্য একটি জনপ্রিয় সাইট হল cricket exchange। এই সাইটটি ক্রিকেট প্রেমিকদের জন্য একটি পুরোপুরি রম্য খেলার স্থান যেখানে তারা তাদের পছন্দের ক্রিকেট টীম বা খেলোয়াড়দের সাথে লক্ষ্য করতে পারেন।
ক্রিকেট এক্সচেঞ্জে একজন প্রতিষ্ঠানকে উৎসাহিত করার জন্য ক্রিকেট এফিলিয়েট প্রোগ্রাম রয়েছে। এই প্রোগ্রামের মাধ্যমে আপনি ক্রিকেট এক্সচেঞ্জে বিপণন করে সাধারণ আয় করতে পারেন।
সাথেই এই এফিলিয়েট প্রোগ্রামের মাধ্যমে ক্রিকেট প্রেমিকরা উপভোগ করতে পারেন 9wicket, crickex affiliate login এবং crickex login এর মতো বিভিন্ন সুবিধা। এই সাইটগুলি ক্রিকেট প্রেমিকদের জন্য আরও উচ্চমানের খেলা এবং পুরস্কার প্রদান করে।
সুতরাং, ক্রিকেট প্রেমিকরা এই সমস্ত সুবিধা এবং অফার থেকে উপভোগ করতে চান, তাহলে তাদের জন্য cricket exchange সম্পর্কে আরও জানতে পারেন। ক্রিকেট এক্সচেঞ্জে আপনার জন্য আরও কী রয়েছে এবং কীভাবে এটি আপনার খেলা অনুভব আরও আনন্দময় করতে পারে, সেটি জানতে ভিজিট করুন।
Welcome to Cricket Affiliate | Kick off with a smashing Welcome Bonus !
First Deposit Fiesta! | Make your debut at Cricket Exchange with a 200% bonus.
Daily Doubles! | Keep the scoreboard ticking with a 100% daily bonus at 9wicket!
#cricketaffiliate
IPL 2024 Jackpot! | Stand to win ₹50,000 in the mega IPL draw at cricket world!
Social Sharer Rewards! | Post and earn 100 tk weekly through Crickex affiliate login.
https://www.cricket-affiliate.com/
#cricketexchange #9wicket #crickexaffiliatelogin #crickexlogin
crickex login VIP! | Step up as a VIP and enjoy weekly bonuses!
Join the Action! | Log in through crickex bet exciting betting experience at Live Affiliate.
Dive into the game with crickex live—where every play brings spectacular wins !
Captivating Breakthroughs and Renowned Titles in the Realm of Videogames
In the dynamic realm of interactive entertainment, there’s always something innovative and captivating on the forefront. From customizations elevating beloved timeless titles to forthcoming launches in iconic franchises, the videogame industry is prospering as in current times.
Here’s a snapshot into the latest announcements and some of the most popular releases enthralling enthusiasts globally.
Latest Developments
1. Groundbreaking Modification for Skyrim Optimizes NPC Appearance
A latest customization for Skyrim has attracted the interest of fans. This customization implements high-polygon faces and dynamic hair for all non-player characters, enhancing the experience’s graphics and depth.
2. Total War Series Title Placed in Star Wars Galaxy Universe Being Developed
The Creative Assembly, famous for their Total War franchise, is supposedly working on a forthcoming title placed in the Star Wars Setting galaxy. This captivating integration has enthusiasts eagerly anticipating the analytical and compelling adventure that Total War experiences are celebrated for, ultimately situated in a world remote.
3. GTA VI Release Announced for Autumn 2025
Take-Two Interactive’s CEO’s CEO has confirmed that Grand Theft Auto VI is set to release in Fall 2025. With the enormous popularity of its prior release, GTA V, gamers are awaiting to explore what the next entry of this iconic universe will deliver.
4. Expansion Developments for Skull & Bones Second Season
Developers of Skull & Bones have communicated expanded developments for the world’s Season Two. This pirate-themed experience provides additional content and improvements, keeping enthusiasts immersed and enthralled in the universe of nautical swashbuckling.
5. Phoenix Labs Deals with Workforce Reductions
Unfortunately, not all news is favorable. Phoenix Labs, the team responsible for Dauntless Experience, has revealed substantial personnel cuts. Regardless of this difficulty, the title persists to be a beloved option amidst fans, and the developer continues to be committed to its audience.
Iconic Experiences
1. Wild Hunt
With its captivating plot, captivating realm, and captivating experience, The Witcher 3 remains a cherished release within fans. Its deep plot and wide-ranging free-roaming environment persist to captivate players in.
2. Cyberpunk 2077 Game
Regardless of a challenging arrival, Cyberpunk 2077 Game keeps a eagerly awaited game. With continuous enhancements and fixes, the release maintains evolve, presenting fans a glimpse into a dystopian environment filled with peril.
3. GTA V
Yet decades subsequent to its debut release, GTA V remains a beloved option amidst players. Its expansive free-roaming environment, compelling narrative, and shared mode maintain players returning for ongoing adventures.
4. Portal 2
A classic problem-solving title, Portal 2 is praised for its pioneering systems and clever environmental design. Its intricate conundrums and amusing dialogue have solidified it as a remarkable experience in the digital entertainment industry.
5. Far Cry Game
Far Cry 3 Game is celebrated as a standout titles in the franchise, offering fans an nonlinear journey abundant with intrigue. Its engrossing plot and iconic personalities have cemented its position as a cherished title.
6. Dishonored
Dishonored Series is acclaimed for its sneaky features and one-of-a-kind realm. Enthusiasts take on the persona of a extraordinary killer, experiencing a urban environment filled with governmental intrigue.
7. Assassin’s Creed
As a member of the iconic Assassin’s Creed Franchise series, Assassin’s Creed Game is revered for its compelling plot, engaging gameplay, and period environments. It stays a exceptional title in the franchise and a iconic across enthusiasts.
In closing, the domain of videogames is flourishing and fluid, with fresh developments
sunmory33
Stepping into the Arena with Betvisa
Welcome to the world of Betvisa, where every day is filled with the thrill of Spin to Win at Betvisa PH! Take a whirl and bag a stunning ?8,888 in big rewards.
As the air crackles with excitement, Betvisa invites you to celebrate romance and rewards this Valentine’s Day. Experience the extraordinary 143% Love Boost at Visa Bet and let the love overflow.
But the magic doesn’t stop there. Betvisa Casino is offering a Deposit Bonus that will leave you in awe. Deposit just ?50 and instantly receive an ?88 bonus – it’s a true display of Deposit Bonus Magic!
#betvisa is the hashtag that will guide you to a world of endless possibilities. Sign up at betvisa login and grab ?500 in free cash, plus 5 free spins to kickstart your journey.
Looking to truly strike it rich? Join through the betvisa app and unlock a free ?500 bonus, along with a fabulous ?8,888 – your Sign-Up Fortune awaits!
Whether you’re a seasoned player or new to the game, Betvisa has something extraordinary in store for you. Step into the arena, immerse yourself in the thrill of Betvisa PH, and let the rewards shower upon you. The future is bright, and it starts with Betvisa!
Betvisa Bet | Step into the Arena with Betvisa!
Spin to Win Daily at Betvisa PH! | Take a whirl and bag ?8,888 in big rewards.
Valentine’s 143% Love Boost at Visa Bet! | Celebrate romance and rewards !
Deposit Bonus Magic! | Deposit 50 and get an 88 bonus instantly at Betvisa Casino.
#betvisa
Free Cash & More Spins! | Sign up betvisa login,grab 500 free cash plus 5 free spins.
Sign-Up Fortune | Join through betvisa app for a free ?500 and fabulous ?8,888.
https://www.betvisa-bet.com/tl
#visabet #betvisalogin #betvisacasino # betvisaph
Double Your Play at betvisa com! | Deposit 1,000 and get a whopping 2,000 free
100% Cock Fight Welcome at Visa Bet! | Plunge into the exciting world .Bet and win!
Jump into Betvisa for exciting games, stunning bonuses, and endless winnings!
angkot88
ANGKOT88: Situs Game Deposit Pulsa Terbaik di Indonesia
ANGKOT88 adalah situs game deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai jenis game online terlengkap yang dapat Anda mainkan hanya dengan mendaftar satu ID. Dengan satu ID tersebut, Anda dapat mengakses seluruh permainan yang tersedia di situs kami.
Sebagai situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), ANGKOT88 menjamin keamanan dan kenyamanan Anda. Situs kami didukung oleh server hosting yang cepat dan sistem keamanan dengan metode enkripsi terbaru di dunia, sehingga data Anda akan selalu terjaga keamanannya. Tampilan situs yang modern juga membuat Anda merasa nyaman saat mengakses situs kami.
Keunggulan ANGKOT88
Selain menjadi situs game online terbaik, ANGKOT88 juga menawarkan layanan praktis untuk melakukan deposit menggunakan pulsa XL ataupun Telkomsel dengan potongan terendah dibandingkan situs lainnya. Ini menjadikan kami salah satu situs game online pulsa terbesar di Indonesia. Anda juga dapat melakukan deposit pulsa melalui E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kepercayaan dan Layanan
Kami di ANGKOT88 sangat menjaga kepercayaan Anda sebagai prioritas utama kami. Oleh karena itu, kami selalu berusaha menjadi agen online terpercaya dan terbaik sepanjang masa. Permainan game online yang kami tawarkan sangat praktis, sehingga Anda dapat memainkannya kapan saja dan di mana saja tanpa perlu repot bepergian. Kami menyediakan berbagai jenis game, termasuk yang disiarkan secara LIVE (langsung) dengan host cantik dan kamera yang merekam secara real-time, menjadikan ANGKOT88 situs game online terlengkap dan terbesar di Indonesia.
Promo Menarik dan Menguntungkan
ANGKOT88 juga menawarkan banyak sekali promo menarik dan menguntungkan. Anda bisa menikmati berbagai macam promo yang sesuai dengan kebutuhan Anda, seperti welcome bonus 20%, bonus deposit harian, dan cashback. Semua promo ini tersedia di situs ANGKOT88. Selain itu, kami juga memiliki layanan Customer Service yang siap membantu Anda kapan saja.
Jadi, tunggu apa lagi? Bergabunglah dengan ANGKOT88 dan nikmati pengalaman bermain game online terbaik dan teraman di Indonesia. Daftarkan diri Anda sekarang dan mulai mainkan game favorit Anda dengan nyaman dan aman di situs kami!
Wow that was strange. I just wrote an incredibly long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Regardless, just wanted to say wonderful blog!
Drone Videography Services in Milan
https://sunmory33jitu.com
supermoney88
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
pro88
PRO88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
PRO88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di PRO88.
Keunggulan PRO88
PRO88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Berbagai Macam Game Online
Kami menyediakan berbagai macam game online terbaik yang bisa Anda mainkan kapan saja dan di mana saja. Dengan satu ID, Anda bisa menikmati semua permainan yang tersedia, mulai dari permainan kartu, slot, hingga taruhan olahraga. PRO88 memastikan semua game yang kami sediakan adalah yang terbaik dan terlengkap di Indonesia.
Keamanan dan Kenyamanan
Kami memahami betapa pentingnya keamanan dan kenyamanan bagi para pemain. Oleh karena itu, PRO88 menggunakan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia. Ini memastikan bahwa data pribadi dan transaksi Anda selalu aman bersama kami. Tampilan situs yang modern juga dirancang untuk memberikan pengalaman bermain yang nyaman dan menyenangkan.
Kesimpulan
PRO88 adalah pilihan terbaik untuk Anda yang mencari situs game online deposit pulsa yang aman dan terpercaya. Dengan berbagai macam game online terbaik dan terlengkap, serta dukungan keamanan yang canggih, PRO88 siap memberikan pengalaman bermain game yang tak terlupakan. Daftar sekarang juga di PRO88 dan nikmati semua permainan yang tersedia hanya dengan satu ID.
Kunjungi kami di PRO88 dan mulailah petualangan game online Anda bersama kami!
как продвинуть сайт
Консультация по SEO продвижению.
Информация о том как работать с низкочастотными запросами и как их подбирать
Подход по действиям в конкурентоспособной нише.
Имею постоянных работаю с 3 организациями, есть что поделиться.
Изучите мой аккаунт, на 31 мая 2024г
общий объём завершённых задач 2181 только на этом сайте.
Консультация только в устной форме, никаких скриншотов и документов.
Длительность консультации указано 2 часа, но по факту всегда на связи без строгой привязки ко времени.
Как управлять с программным обеспечением это уже отдельная история, консультация по работе с программами оговариваем отдельно в специальном услуге, выясняем что требуется при разговоре.
Всё без суеты на расслабленно не в спешке
To get started, the seller needs:
Мне нужны контакты от телеграм каналов для связи.
общение только устно, вести переписку недостаточно времени.
Сб и воскресенья выходной
Nice post. I learn something new and challenging on sites I stumbleupon on a daily basis. It’s always useful to read content from other writers and use a little something from other sites.
lgo4d
sunmory33
bocor88
bocor88
在線娛樂城的世界
隨著網際網路的迅速發展,網上娛樂城(網上賭場)已經成為許多人娛樂的新選擇。在線娛樂城不僅提供多樣化的遊戲選擇,還能讓玩家在家中就能體驗到賭場的興奮和樂趣。本文將探討網上娛樂城的特色、優勢以及一些常見的游戲。
什麼是在線娛樂城?
在線娛樂城是一種經由互聯網提供賭博遊戲的平台。玩家可以經由電腦、手機或平板進入這些網站,參與各種賭錢活動,如德州撲克、輪盤、二十一點和老虎機等。這些平台通常由專業的的程序公司開發,確保游戲的公正和穩定性。
在線娛樂城的利益
便利性:玩家無需離開家,就能體驗賭錢的快感。這對於那些生活在偏遠實體賭場地區的人來說尤為方便。
多元化的遊戲選擇:在線娛樂城通常提供比實體賭場更多樣化的遊戲選擇,並且經常更新游戲內容,保持新鮮感。
優惠和獎金:許多線上娛樂城提供多樣的獎金計劃,包括註冊獎金、存款獎勵和會員計劃,吸引新新玩家並激勵老玩家持續遊戲。
穩定性和隱私性:合法的網上娛樂城使用高端的加密技術來保護玩家的私人信息和金融交易,確保游戲過程的穩定和公正性。
常見的網上娛樂城遊戲
撲克:撲克牌是最受歡迎賭博游戲之一。在線娛樂城提供多樣撲克牌變體,如德州扑克、奧馬哈撲克和七張牌撲克等。
輪盤:輪盤是一種傳統的賭場遊戲遊戲,玩家可以下注在數字、數字排列或顏色上,然後看球落在哪個區域。
黑傑克:又稱為黑傑克,這是一種競爭玩家和莊家點數的遊戲,目標是讓手牌點數點數儘量接近21點但不超過。
吃角子老虎:吃角子老虎是最簡單且是最流行的博彩游戲之一,玩家只需旋轉捲軸,等待圖案排列出中獎的組合。
結尾
在線娛樂城為當代賭博愛好者提供了一個便捷、興奮且多樣化的娛樂方式。不論是撲克牌愛好者還是吃角子老虎迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的不斷發展,在線娛樂城的游戲體驗將變得越來越現實和引人入勝。然而,玩家在享受遊戲的同時,也應該自律,避免沉迷於博彩活動,保持健康的遊戲心態。
線上娛樂城的世界
隨著互聯網的飛速發展,在線娛樂城(在線賭場)已經成為許多人休閒的新選擇。網上娛樂城不僅提供多元化的游戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和樂趣。本文將研究網上娛樂城的特點、利益以及一些常見的的游戲。
什麼是線上娛樂城?
網上娛樂城是一種透過網際網路提供賭博遊戲的平台。玩家可以透過電腦、手機或平板設備進入這些網站,參與各種賭錢活動,如撲克、輪盤、二十一點和老虎机等。這些平台通常由專業的軟體公司開發,確保游戲的公正和穩定性。
線上娛樂城的優勢
方便性:玩家不需要離開家,就能享受賭博的快感。這對於那些居住在偏遠實體賭場區域的人來說尤為方便。
多元化的游戲選擇:線上娛樂城通常提供比實體賭場更豐富的遊戲選擇,並且經常升級遊戲內容,保持新鮮感。
優惠和獎金:許多在線娛樂城提供豐厚的獎金計劃,包括註冊紅利、存款獎金和會員計劃,吸引新新玩家並促使老玩家不斷遊戲。
穩定性和保密性:正當的在線娛樂城使用先進的的加密技術來保護玩家的個人信息和交易,確保游戲過程的公平和公平。
常見的的線上娛樂城游戲
撲克牌:德州撲克是最流行賭博遊戲之一。網上娛樂城提供各種撲克牌變體,如德州撲克、奧馬哈撲克和七張牌等。
賭盤:賭盤是一種經典的賭場遊戲遊戲,玩家可以投注在單個數字、數字組合上或顏色上,然後看小球落在哪個位置。
21點:又稱為二十一點,這是一種競爭玩家和莊家點數的遊戲,目標是讓手牌點數盡可能接近21點但不超過。
老虎機:老虎機是最容易也是最流行的博彩遊戲之一,玩家只需轉動捲軸,看圖案排列出中獎的組合。
結尾
線上娛樂城為現代的賭博愛好者提供了一個方便、興奮且豐富的娛樂選擇。不管是撲克迷還是老虎機迷,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的的不斷發展,在線娛樂城的遊戲體驗將變得越來越逼真和有趣。然而,玩家在體驗遊戲的同時,也應該自律,避免沉溺於賭錢活動,保持健康的心態。
Советы по оптимизации продвижению.
Информация о том как работать с низкочастотными запросами запросами и как их подбирать
Тактика по действиям в соперничающей нише.
Имею постоянных клиентов взаимодействую с несколькими компаниями, есть что сообщить.
Посмотрите мой досье, на 31 мая 2024г
количество завершённых задач 2181 только на этом сайте.
Консультация проходит устно, без скринов и документов.
Длительность консультации указано 2 ч, но по реально всегда на контакте без жёсткой фиксации времени.
Как работать с софтом это уже отдельная история, консультация по использованию ПО обсуждаем отдельно в другом услуге, узнаем что требуется при коммуникации.
Всё спокойно на без напряжения не торопясь
To get started, the seller needs:
Мне нужны контакты от Telegram канала для связи.
разговор только вербально, переписываться нету времени.
субботы и воскресенья выходные
전소미 마약
빠릿한 환충 서비스와 대형업체의 안전성
스포츠토토사이트 이용 시 핵심적인 요소는 신속한 충환전 처리입니다. 보통 삼 분 내에 충전하고, 십 분 내에 환충이 처리되어야 합니다. 대형 대형업체들은 넉넉한 직원 고용을 통해 이러한 빠른 환충 프로세스를 약속하며, 이 방법으로 회원들에게 안도감을 제공합니다. 주요사이트를 접속하면서 신속한 경험을 해보시기 바랍니다. 우리 고객님이 안전하게 토토사이트를 접속할 수 있도록 도와드리는 먹튀해결사입니다.
보증금을 걸고 배너 운영
먹튀 해결 팀은 최대한 삼천만 원부터 일억 원의 보증 자금을 예치하고 있는 업체들의 광고 배너를 운영합니다. 만약 먹튀 피해가 발생할 시, 배팅 규정에 어긋나지 않은 배팅 내역을 캡처해서 먹튀 해결 팀에 연락 주시면, 사실 확인 뒤 보증 금액으로 신속하게 피해 보전 처리해 드립니다. 피해 발생 시 즉시 캡처해서 피해 내용을 저장해 두시고 보내주세요.
오랫동안 안전하게 운영된 업체 확인
먹튀해결사는 적어도 4년 이상 먹튀 이력 없이 무사히 운영한 사이트들을 검증하여 배너 입점을 받고 있습니다. 이를 통해 누구나 알고 있는 주요사이트를 안전하게 사용할 수 있는 기회를 제공합니다. 엄격한 검증 작업을 통해 검증된 사이트를 놓치지 말고, 안심하고 배팅을 경험해보세요.
투명성과 공정성을 가진 먹튀 검증
먹튀해결사의 먹튀 검증은 투명함과 정확함을 바탕으로 합니다. 늘 사용자들의 입장을 우선시하며, 사이트의 유혹이나 이익에 좌우되지 않고 한 건의 삭제 없이 사실만을 바탕으로 검증해왔습니다. 먹튀 피해를 당하고 후회하지 않도록, 지금 시작하세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 엄선한 안전한 토토사이트 인증된 업체 목록 입니다. 지금 등록된 검증된 업체들은 먹튀 문제가 발생 시 100% 보증을 도와드립니다. 다만, 제휴 기간이 만료된 업체에서 발생한 피해에 대해서는 책임지지 않습니다.
탁월한 먹튀 검증 알고리즘
먹튀해결사는 청결한 베팅 문화를 만들기 위해 항상 애쓰고 있습니다. 우리가 소개하는 베팅사이트에서 안전하게 베팅하시기 바랍니다. 사용자의 먹튀 제보는 먹튀 리스트에 등록 노출되어 해당되는 토토사이트에 심각한 영향을 줄 수 있습니다. 먹튀 목록 작성 시 먹튀블러드만의 검토 경험을 최대한 활용하여 공평한 심사를 할 수 있도록 하겠습니다.
안전한 베팅 문화를 만들기 위해 계속해서 애쓰는 먹튀 해결 팀과 같이 안전하게 즐겨보세요.
как продвинуть сайт
Советы по SEO продвижению.
Информация о том как взаимодействовать с низкочастотными запросами и как их определять
Тактика по работе в конкурентной нише.
Обладаю постоянных сотрудничаю с 3 компаниями, есть что рассказать.
Изучите мой аккаунт, на 31 мая 2024г
количество завершённых задач 2181 только здесь.
Консультация проходит устно, без скринов и отчетов.
Продолжительность консультации указано 2 ч, но по сути всегда на доступен без твердой фиксации времени.
Как работать с программным обеспечением это уже отдельная история, консультация по работе с софтом договариваемся отдельно в специальном разделе, выясняем что нужно при общении.
Всё спокойно на без напряжения не спеша
To get started, the seller needs:
Мне нужны данные от телеграмм чата для связи.
коммуникация только вербально, переписываться не хватает времени.
Сб и воскресенья нерабочие дни
data sdy
Inspirasi dari Petikan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Penyanyi Terkenal, seorang vokalis dan pengarang lagu terkenal, tidak hanya dikenal berkat nada yang indah dan vokal yang merdu, tetapi juga karena kata-kata lagunya yang sarat makna. Dalam syair-syairnya, Swift sering melukiskan berbagai aspek kehidupan, mulai dari kasih hingga rintangan hidup. Berikut ini adalah sejumlah kutipan motivatif dari karya-karya, bersama maknanya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Penjelasan: Bahkan di masa-masa sulit, selalu ada secercah harapan dan kemungkinan akan hari yang lebih baik.
Lirik ini dari lagu “All Too Well” mengingatkan kita jika meskipun kita bisa jadi berhadapan dengan masa-masa sulit pada saat ini, selalu ada potensi kalau waktu yang akan datang akan membawa hal yang lebih baik. Ini adalah pesan asa yang mengukuhkan, memotivasi kita untuk tetap bertahan dan tidak menyerah, sebab yang paling baik mungkin belum tiba.
“Aku akan tetap bertahan lantaran aku tak bisa melakukan segala sesuatu tanpa dirimu.” – “You Belong with Me”
Makna: Memperoleh cinta dan bantuan dari orang lain dapat menyediakan kita tenaga dan kemauan keras untuk bertahan lewat kesulitan.
sis4d
Ashley JKT48: Bintang yang Bersinar Cemerlang di Langit Idola
Siapakah Ashley JKT48?
Siapa sosok muda berbakat yang menyita perhatian banyak fans musik di Nusantara dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama panggungnya, Ashley JKT48. Bergabung dengan grup idol JKT48 pada tahun 2018, Ashley dengan segera menjadi salah satu member paling populer.
Biografi
Lahir di Jakarta pada tgl 13 Maret 2000, Ashley memiliki keturunan Tionghoa-Indonesia. Dia memulai karier di dunia entertainment sebagai peraga dan aktris, hingga akhirnya kemudian masuk dengan JKT48. Kepribadiannya yang ceria, suara yang mantap, dan kemahiran menari yang mengesankan membentuknya sebagai idola yang sangat disukai.
Penghargaan dan Pengakuan
Ketenaran Ashley telah diapresiasi melalui berbagai apresiasi dan nominasi. Pada tahun 2021, ia memenangkan penghargaan “Anggota Paling Populer JKT48” di event JKT48 Music Awards. Ia juga diberi gelar sebagai “Idol Tercantik se-Asia” oleh sebuah majalah online pada tahun 2020.
Peran dalam JKT48
Ashley menjalankan peran penting dalam group JKT48. Ia adalah personel Tim KIII dan berperan menjadi penari utama dan penyanyi utama. Ashley juga merupakan bagian dari subunit “J3K” dengan Jessica Veranda dan Jennifer Rachel Natasya.
Karier Solo
Di luar kegiatannya dengan JKT48, Ashley juga mengembangkan karir solo. Ashley telah merilis beberapa single, termasuk “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah bekerjasama bersama penyanyi lain, seperti Afgan dan Rossa.
Aktivitas Personal
Selain bidang pertunjukan, Ashley dikenal sebagai sosok yang low profile dan bersahabat. Ia menikmati menghabiskan waktu bersama family dan sahabat-sahabatnya. Ashley juga menyukai hobi mewarnai dan photography.
Проверка кошелька токенов
Анализ криптовалюты на платформе TRC20 и других цифровых транзакций
На нашем сайте вы развернутые обзоры различных сервисов для проверки платежей и адресов, содержащие антиотмывочного закона проверки для токенов и иных цифровых валют. Вот основные особенности, что в наших описаниях:
Контроль криптовалюты TRC20
Многие платформы предоставляют детальную анализ транзакций криптовалюты в блокчейн-сети TRC20 блокчейна. Это дает возможность обнаруживать необычную действия и удовлетворять законодательным требованиям.
Анализ переводов монет
В наших ревью доступны платформы для детального анализа и наблюдения переводов USDT, которые обеспечивает сохранять чистоту и защищенность платежей.
антиотмывочная контроль токенов
Определенные платформы предоставляют anti-money laundering контроль USDT, обеспечивая идентифицировать и предотвращать случаи финансовых преступлений и денежных мошенничеств.
Анализ адреса USDT
Наши обзоры содержат инструменты, что дают возможность контролировать аккаунты USDT на определение подозрительных действий и подозрительных платежей, обеспечивая дополнительный уровень степень безопасности безопасности.
Проверка операций USDT на платформе TRC20
Вы найдете представлены ресурсы, поддерживающие верификацию платежей криптовалюты в сети TRC20 сети, что позволяет обеспечивает соблюдение необходимым стандартам нормам.
Верификация аккаунта адреса монет
В описаниях описаны инструменты для контроля кошельков аккаунтов монет на потенциальных опасностей угроз.
Верификация адреса USDT на блокчейне TRC20
Наши оценки включают платформы, предлагающие анализ кошельков криптовалюты в блокчейн-сети TRC20, что помогает гарантирует предотвратить мошенничество и экономических преступлений.
Верификация токенов на чистоту
Описанные платформы дают возможность проверять платежи и кошельки на прозрачность, фиксируя подозрительную деятельность.
антиотмывочного закона контроль USDT на сети TRC20
В описаниях вы платформы, предоставляющие антиотмывочного закона проверку для криптовалюты на платформе TRC20 платформы, что позволяет вашему компании соблюдать мировым положениям.
Контроль USDT на блокчейне ERC20
Наши ревью содержат платформы, предоставляющие верификацию токенов в блокчейн-сети ERC20 блокчейна, что гарантирует обеспечивает детальный анализ операций и кошельков.
Верификация криптокошелька
Мы рассматриваем инструменты, поддерживающие решения по верификации криптокошельков, охватывая отслеживание платежей и определение необычной деятельности.
Анализ счета криптовалютного кошелька
Наши ревью представляют платформы, позволяющие верифицировать адреса криптовалютных кошельков для обеспечения повышенной надежности.
Анализ цифрового кошелька на переводы
В наших описаниях найдете сервисы для проверки виртуальных кошельков на переводы, что гарантирует поддерживать ясность переводов.
Верификация виртуального кошелька на отсутствие подозрительных действий
Наши оценки представляют сервисы, позволяющие верифицировать виртуальные кошельки на легитимность, выявляя все необычные операции.
Ознакомившись с наши ревью, вы выберете надежные платформы для анализа и отслеживания блокчейн операций, чтобы обеспечивать гарантировать высокий степень безопасности безопасности и соблюдать необходимым нормативным положениям.
internet casinos
Online Casinos: Innovation and Benefits for Modern Society
Overview
Internet gambling platforms are virtual sites that provide users the opportunity to engage in betting games such as poker, spin games, blackjack, and slot machines. Over the past few years, they have become an integral component of online leisure, providing various advantages and possibilities for players around the world.
Accessibility and Ease
One of the main advantages of online gambling sites is their accessibility. Players can enjoy their preferred activities from any location in the world using a computer, iPad, or mobile device. This conserves time and funds that would otherwise be spent traveling to traditional gambling halls. Furthermore, 24/7 availability to games makes internet gambling sites a easy option for people with hectic schedules.
Range of Activities and Experience
Digital gambling sites provide a wide range of games, enabling everyone to find an option they like. From classic table games and board activities to slots with diverse concepts and progressive jackpots, the range of activities guarantees there is an option for every taste. The ability to engage at various skill levels also makes online casinos an ideal location for both novices and seasoned players.
Financial Advantages
The online gambling industry adds significantly to the economy by generating employment and generating revenue. It backs a wide range of professions, including software developers, customer support representatives, and advertising specialists. The revenue generated by online gambling sites also contributes to tax revenues, which can be used to support public services and development projects.
Advancements in Technology
Online gambling sites are at the forefront of tech advancement, constantly integrating new technologies to enhance the gaming entertainment. Superior graphics, real-time dealer activities, and VR gambling sites offer immersive and realistic playing entertainment. These advancements not only enhance user experience but also push the boundaries of what is possible in online entertainment.
Responsible Gambling and Support
Many digital casinos promote safe betting by providing tools and resources to assist players control their gaming activities. Features such as fund restrictions, self-exclusion options, and availability to assistance programs guarantee that players can enjoy gaming in a safe and monitored environment. These steps show the industry’s commitment to promoting healthy betting habits.
Social Interaction and Networking
Online casinos often offer interactive options that enable players to interact with each other, forming a sense of belonging. Multiplayer activities, chat functions, and social media integration enable players to connect, share experiences, and build relationships. This interactive element improves the overall betting entertainment and can be especially helpful for those looking for social interaction.
Conclusion
Online casinos provide a diverse variety of benefits, from accessibility and convenience to economic contributions and innovations. They provide varied gaming options, support safe betting, and promote social interaction. As the sector continues to grow, digital gambling sites will probably remain a significant and positive force in the world of digital entertainment.
free slots games
Complimentary Slot Games: Entertainment and Perks for All
Complimentary slot games have become a in-demand form of online entertainment, offering players the thrill of slot machines devoid of any financial investment.
The primary objective of free slot games is to deliver a entertaining and immersive way for users to enjoy the excitement of slot machines absent any monetary jeopardy. They are designed to imitate the experience of actual-currency slots, allowing players to activate the reels, relish various motifs, and obtain digital payouts.
Entertainment: Free slot games are an outstanding source of entertainment, delivering durations of excitement. They showcase colorful visuals, engaging soundtracks, and varied ideas that suit a comprehensive variety of tastes.
Capability Enhancement: For novices, gratis slot games offer a worry-free setting to acquaint the principles of slot machines. Players can get acquainted with different functionality, paylines, and special features free from the fear of forfeiting funds.
Stress Relief: Playing free slot games can be a excellent way to unwind. The simple interaction and the chance for online prizes make it an enjoyable pastime.
Social Interaction: Many complimentary slot games feature collaborative elements such as leaderboards and the option to engage with acquaintances. These components bring a group-based aspect to the gaming experience, inspiring players to compete against fellow participants.
Advantages of Free Slot Games
1. Approachability and Simplicity
Gratis slot games are readily available to everyone with an internet connection. They can be accessed on various apparatuses including PCs, pads, and smartphones. This simplicity allows players to savor their preferred pursuits whenever and anywhere.
2. Monetary Innocuousness
One of the most significant rewards of complimentary slot games is that they remove the cash-related jeopardies related to gambling. Players can enjoy the thrill of rotating the reels and earning major prizes without investing any cash.
3. Range of Possibilities
No-Cost slot games are available in a wide assortment of themes and styles, from nostalgic fruit slots to contemporary video-based slots with elaborate themes and graphics. This breadth provides that there is a choice for everyone, without regard of their tastes.
4. Enhancing Cognitive Skills
Playing free slot games can tend to strengthen cognitive skills such as anticipatory planning. The necessity to choose win lines, learn operational principles, and foresee consequences can deliver a cognitive challenge that is simultaneously pleasurable and advantageous.
5. Secure Pre-Testing for Paid-Participation
For those pondering progressing to actual-currency slots, complimentary slot games present a beneficial trial environment. Players can experience various games, refine tactics, and develop self-assurance before opting to invest genuine funds. This readiness can culminate in a more informed and rewarding actual-currency gaming experience.
Summary
Gratis slot games grant a multitude of perks, from pure pleasure to proficiency improvement and community engagement. They present a risk-free and cost-free way to experience the thrill of slot machines, establishing them a beneficial addition to the landscape of electronic leisure. Whether you’re wanting to unwind, sharpen your cognitive skills, or simply enjoy yourself, gratis slot games are a wonderful alternative that continues to entertain players across.
Digital Gambling Platform Real Money: Rewards for Customers
Overview
Digital gambling platforms granting paid activities have acquired significant widespread adoption, offering participants with the opportunity to obtain economic payouts while savoring their cherished gambling games from residence. This text explores the advantages of virtual wagering environment actual currency offerings, underscoring their beneficial influence on the leisure sector.
User-Friendliness and Availability
Internet-based gambling platform paid activities provide simplicity by allowing players to engage with a comprehensive range of games from anywhere with an online connection. This eradicates the necessity to travel to a traditional gaming venue, preserving resources. Virtual wagering environments are likewise offered continuously, allowing players to interact with at their simplicity.
Variety of Games
Digital gaming sites provide a more extensive diversity of activities than brick-and-mortar casinos, incorporating slot-based activities, vingt-et-un, spinning wheel, and card games. This variety allows players to try out new offerings and uncover unfamiliar most liked, elevating their overall interactive sensation.
Incentives and Special Offers
Digital gaming sites provide substantial incentives and promotions to draw in and maintain customers. These bonuses can include introductory incentives, free spins, and reimbursement offers, delivering further significance for customers. Loyalty programs as well acknowledge participants for their continued patronage.
Competency Enhancement
Partaking in paid offerings on the internet can enable players develop aptitudes such as critical analysis. Experiences like blackjack and table games demand players to reach selections that can affect the result of the offering, assisting them develop analytical abilities.
Communal Engagement
ChatGPT l Валли, 6.06.2024 4:08]
Digital gaming sites grant opportunities for collaborative connection through discussion forums, forums, and real-time croupier experiences. Customers can connect with their peers, exchange tips and strategies, and sometimes develop friendships.
Fiscal Rewards
The digital gaming field produces jobs and adds to the financial system through government proceeds and regulatory payments. This monetary influence rewards a comprehensive array of vocations, from offering developers to player support representatives.
Conclusion
Digital gaming site paid activities grant many upsides for players, involving ease, variety, bonuses, capability building, interpersonal connections, and fiscal upsides. As the domain constantly progress, the widespread appeal of digital gaming sites is likely to grow.
Fortune Wagering Environment: In a Place Where Pleasure Converges With Prosperity
Fortune Gambling Platform is a widely-known online location known for its comprehensive selection of activities and enthralling bonuses. Let’s examine the factors that explain why so several individuals savor playing at Fortune Casino and in which manner it rewards them.
Pleasure-Providing Aspect
Wealth Gaming Site grants a diversity of experiences, featuring traditional table games like pontoon and wheel of fortune, as alongside innovative slot-related offerings. This variety guarantees that there is an option for anyone, establishing all encounter to Prosperity Gambling Platform satisfying and fun.
Substantial Payouts
One of the primary aspects of Fortune Gaming Site is the prospect to secure major payouts. With generous top rewards and bonuses, participants have the possibility to experience a reversal of fortune with a individual spin or game. Numerous customers have received significant rewards, contributing to the suspense of partaking in Fortune Wagering Environment.
Ease of Access and Reachability
Prosperity Casino’s digital platform makes it user-friendly for participants to experience their favorite experiences from anywhere. Whether at home or on the go, customers can engage with Luck Gambling Platform from their laptop or smartphone. This availability ensures that users can savor the excitement of the gambling regardless of when they prefer, free from the requirement to travel.
Range of Possibilities
Prosperity Wagering Environment offers a comprehensive array of activities, providing that there is an option for every single style of participant. Beginning with classic card games to narrative-driven slot machines, the variety sustains players captivated and delighted. This array in addition allows customers to experiment with different experiences and identify novel most liked.
Promotional Benefits
Prosperity Gambling Platform compensates its participants with promotional benefits and advantages, including sign-up incentives and reward programs. These special offers not just improve the interactive sensation but likewise increase the likelihoods of earning significant rewards. Participants are continually incentivized to maintain participation, rendering Fortune Wagering Environment further enticing.
Shared Experiences and Social Networking
ChatGPT l Валли, 6.06.2024 4:30]
Wealth Casino offers a feeling of shared experience and group-based participation for customers. Using chat rooms and discussion boards, customers can engage with one another, exchange recommendations and strategies, and occasionally create personal connections. This social factor contributes a further aspect of pleasure to the interactive sensation.
Key Takeaways
Luck Casino presents a comprehensive selection of benefits for participants, including entertainment, the prospect of securing major payouts, convenience, breadth, perks, and shared experiences. Regardless of whether desiring thrill or aspiring to achieve unexpected success, Prosperity Gambling Platform offers an captivating interaction for all partake in.
Gratis Poker Machine Offerings: A Fun and Advantageous Interaction
Gratis poker machine games have become increasingly sought-after among users desiring a captivating and risk-free entertainment experience. These experiences provide a comprehensive variety of benefits, establishing them as a favored possibility for numerous. Let’s analyze in which manner complimentary slot-based experiences can benefit players and why they are so broadly savored.
Amusement Factor
One of the primary motivations players enjoy playing free poker machine experiences is for the amusement factor they offer. These experiences are developed to be engaging and thrilling, with animated imagery and immersive audio that bolster the comprehensive gaming experience. Whether you’re a occasional player wanting to spend time or a avid leisure activity enthusiast aspiring to excitement, free poker machine activities provide entertainment for everyone.
Proficiency Improvement
Partaking in gratis electronic gaming games can as well facilitate acquire helpful faculties such as strategic thinking. These games call for users to reach immediate determinations based on the gameplay elements they are received, facilitating them improve their critical-thinking aptitudes and mental agility. Furthermore, customers can experiment with various methods, sharpening their skills without the possibility of financial impact of losing paid funds.
Simplicity and Approachability
A supplemental benefit of no-cost virtual wagering experiences is their user-friendliness and availability. These offerings can be played in the digital realm from the ease of your own abode, eradicating the requirement to journey to a land-based casino. They are in addition available continuously, permitting customers to enjoy them at whichever moment that suits them. This user-friendliness renders no-cost virtual wagering activities a well-liked option for participants with demanding routines or those looking for a swift leisure solution.
Social Interaction
Numerous complimentary slot-based games as well grant collaborative aspects that enable customers to engage with their peers. This can feature chat rooms, interactive platforms, and collaborative modes where users can compete against each other. These communal engagements bring an supplemental dimension of pleasure to the gaming experience, enabling customers to connect with peers who have in common their passions.
Worry Mitigation and Emotional Refreshment
Playing no-cost virtual wagering activities can also be a excellent method to relax and de-stress after a prolonged stretch of time. The uncomplicated gameplay and soothing audio can facilitate decrease worry and unease, delivering a welcome break from the pressures of regular experience. Moreover, the suspense of earning digital payouts can boost your mood and result in you feeling reenergized.
Key Takeaways
Complimentary slot-based experiences grant a extensive selection of advantages for users, encompassing amusement, competency enhancement, convenience, communal engagement, and anxiety reduction and unwinding. Regardless of whether you’re aiming to hone your leisure abilities or just experience pleasure, free poker machine experiences offer a advantageous and fulfilling encounter for customers of every degrees.
Thanks for the auspicious writeup. It in fact
was once a entertainment account it. Glance
complex to far brought agreeable from you! By the way, how could
we keep up a correspondence?
online poker
Virtual Table Games: A Origin of Amusement and Skill Development
Digital table games has materialized as a well-liked kind of entertainment and a channel for competency enhancement for players worldwide. This piece investigates the positive elements of internet-based card games and in what way it rewards individuals, emphasizing its far-reaching recognition and influence.
Pleasure-Providing Aspect
Virtual casino-style games provides a thrilling and engaging interactive interaction, spellbinding users with its analytical activity and unpredictable ends. The offering’s engrossing nature, along with its communal components, grants a unique type of pleasure that several consider pleasurable.
Capability Building
In addition to entertainment, internet-based card games as well acts as a avenue for skill development. The activity demands strategic thinking, snap judgments, and the aptitude to understand adversaries, all of which lend to intellectual maturation. Customers can bolster their critical-thinking aptitudes, adaptability, and sound judgment aptitudes through ongoing activity.
User-Friendliness and Availability
One of the main upsides of internet-based card games is its user-friendliness and availability. Customers can experience the game from the simplicity of their abodes, at whichever moment that accommodates them. This approachability excludes the requirement for commute to a brick-and-mortar gambling establishment, rendering it a convenient option for users with demanding timetables.
Range of Possibilities and Stake Amounts
Virtual casino-style games interfaces offer a extensive diversity of experiences and stakes to serve participants of every types of abilities and inclinations. Whether you’re a newcomer aiming to understand the ropes or a experienced pro desiring a test, there is a offering for your preferences. This diversity secures that participants can consistently discover a game that corresponds to their skill level and financial resources.
Shared Experiences
Virtual casino-style games as well offers prospects for communal engagement. A significant number of systems offer messaging capabilities and group-based formats that give users to interact with fellow individuals, discuss encounters, and build social relationships. This social factor contributes substance to the leisure encounter, making it additionally pleasurable.
Profit Potential
For particular players, digital table games can likewise be a source of monetary gains. Proficient participants can earn considerable profits through frequent interactivity, constituting it as a money-making undertaking for those who dominate the activity. Furthermore, a significant number of internet-based card games events present major prize pools, providing users with the possibility to win big.
Key Takeaways
Digital table games provides a variety of upsides for users, encompassing amusement, skill development, user-friendliness, shared experiences, and earnings opportunities. Its broad appeal continues to rise, with a significant number of individuals shifting to virtual casino-style games as a wellspring of pleasure and personal growth. Whether you’re looking to enhance your faculties or merely have fun, digital table games is a versatile and advantageous leisure activity for customers of any experiences.
신속한 충환전 서비스와 주요업체의 보안성
스포츠토토사이트 접속 시 핵심적인 요소 중 하나는 신속한 입출금 처리입니다. 보통 3분 안에 충전, 10분 이내에 환충이 완료되어야 합니다. 주요 주요업체들은 필요한 인력 채용으로 이러한 신속한 환충 처리를 약속하며, 이 방법으로 고객들에게 안전한 느낌을 드립니다. 주요사이트를 이용하면서 신속한 체감을 해보시기 바랍니다. 우리 고객님이 보안성 있게 토토사이트를 접속할 수 있도록 도와드리는 먹튀 해결 팀입니다.
보증금을 걸고 배너를 운영
먹튀 해결 팀은 최대한 삼천만 원에서 1억 원의 보증 자금을 예탁한 업체들의 배너를 운영합니다. 혹시 먹튀 피해가 생길 경우, 배팅 규정에 위배되지 않은 베팅 내역을 캡처해서 먹튀 해결 전문가에게 문의하시면, 확인 후 보증금으로 빠르게 피해 보전 처리해드립니다. 피해가 발생하면 빠르게 캡처해서 손해 내용을 저장해두시고 제출해 주세요.
장기간 안전 운영 업체 확인
먹튀 해결 전문가는 최소 사 년 이상 먹튀 문제 없이 안전하게 운영한 사이트들을 확인하여 배너 등록을 받고 있습니다. 이 때문에 어느 누구나 잘 알려진 메이저사이트를 안전하게 이용할 수 있는 기회를 제공하고 있습니다. 정확한 검증 작업을 통해 확인된 사이트를 놓치지 마시고, 안전한 배팅을 즐겨보세요.
투명성과 공정성을 가진 먹튀 검증
먹튀 해결 전문가의 먹튀 검증은 투명성과 정확함을 바탕으로 실시합니다. 항상 고객들의 관점을 우선시하며, 사이트의 유혹이나 이익에 좌우되지 않고 한 건의 삭제 없이 사실만을 근거로 검증해오고 있습니다. 먹튀 사고를 당한 후 후회하지 않도록, 지금 시작하세요.
먹튀검증사이트 목록
먹튀해결사가 선별한 안전한 토토사이트 검증업체 목록 입니다. 지금 등록된 인증된 업체들은 먹튀 피해 발생 시 100% 보장을 해드립니다. 하지만, 제휴가 끝난 업체에서 발생한 사고에 대해서는 책임지지 않습니다.
유일무이한 먹튀 검증 알고리즘
먹튀해결사는 공정한 도박 문화를 조성하기 위해 항상 애쓰고 있습니다. 저희가 소개하는 베팅사이트에서 안심하고 배팅하세요. 회원님의 먹튀 제보는 먹튀 리스트에 등록되어 해당 토토사이트에 중대한 영향을 끼칩니다. 먹튀 목록 작성 시 먹튀블러드만의 검증 지식을 최대한 활용하여 공정한 심사를 할 수 있게 하겠습니다.
안전한 베팅 환경을 만들기 위해 끊임없이 힘쓰는 먹튀해결사와 함께 안전하게 경험해보세요.
ਨੰਗਾ ਨਾਚ ਪੋਰਨ .MxhsXDO3xvZ
アラブポルノ .Jyd5SuyEhWN
sis4d
Download Perangkat Lunak 888 dan Raih Bonus: Manual Singkat
**Aplikasi 888 adalah kesempatan terbaik untuk Anda yang membutuhkan permainan bertaruhan digital yang mengasyikkan dan menguntungkan. Melalui imbalan harian dan fitur menarik, aplikasi ini siap menyediakan keseruan berjudi paling baik. Ini panduan pendek untuk menggunakan pelayanan Aplikasi 888.
Pasang dan Mulai Dapatkan
Platform Tersedia:
Program 888 dapat diunduh di Android, Perangkat iOS, dan PC. Segera bermain dengan mudah di perangkat apa pun.
Bonus Harian dan Bonus
Keuntungan Login Tiap Hari:
Buka setiap periode untuk mengklaim keuntungan mencapai 100K pada periode ketujuh.
Kerjakan Pekerjaan:
Ambil opsi lotere dengan menuntaskan tugas terkait. Masing-masing misi menghadirkan Para Pengguna satu kesempatan undian untuk mendapatkan bonus mencapai 888K.
Pengambilan Sendiri:
Hadiah harus diambil manual di dalam app. Pastikan untuk mengklaim keuntungan saban waktu agar tidak habis masa berlakunya.
Cara Undi
Kesempatan Lotere:
Tiap masa, Anda bisa meraih satu kesempatan undi dengan merampungkan pekerjaan.
Jika kesempatan undi selesai, selesaikan lebih banyak aktivitas untuk mengklaim tambahan kesempatan.
Level Hadiah:
Klaim keuntungan jika keseluruhan lotere Pengguna melebihi 100K dalam sehari.
Aturan Pokok
Pengklaiman Bonus:
Imbalan harus diambil manual dari app. Jika tidak, bonus akan secara otomatis diambil ke akun Anda setelah satu hari.
Syarat Pertaruhan:
Imbalan harus ada paling tidak sebuah pertaruhan valid untuk diklaim.
Akhir
App 888 menyediakan keseruan berjudi yang menggembirakan dengan keuntungan tinggi. Unduh perangkat lunak hari ini dan alamilah keberhasilan tinggi pada masa!
Untuk detail lebih terperinci tentang penawaran, pengisian, dan sistem rujukan, kunjungi situs home app.
ਹੱਥਰਸੀ ਪੋਰਨ .b7F9IMv70AD
kantortoto
Ashley JKT48: Bintang yang Bersinar Terang di Kancah Idol
Siapa Ashley JKT48?
Siapakah sosok muda berbakat yang mencuri perhatian sejumlah besar penggemar musik di Indonesia dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang dikenal dengan nama panggungnya, Ashley JKT48. Masuk dengan grup idola JKT48 pada masa 2018, Ashley dengan lekas muncul sebagai salah satu member paling favorit.
Biografi
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley memiliki darah Tionghoa-Indonesia. Dia memulai karier di industri hiburan sebagai model dan aktris, hingga akhirnya kemudian masuk dengan JKT48. Kepribadiannya yang ceria, vokal yang mantap, dan kemampuan menari yang memukau menjadikannya idola yang sangat disukai.
Award dan Apresiasi
Kepopuleran Ashley telah diakui melalui berbagai apresiasi dan nominasi. Pada masa 2021, ia mendapat penghargaan “Anggota Paling Populer JKT48” di acara JKT48 Music Awards. Ia juga dinobatkan sebagai “Idol Tercantik di Asia” oleh sebuah tabloid online pada tahun 2020.
Fungsi dalam JKT48
Ashley memainkan posisi penting dalam grup JKT48. Ia adalah anggota Tim KIII dan berperan sebagai dancer utama dan vokalis. Ashley juga menjadi bagian dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Karier Solo
Selain aktivitasnya dengan JKT48, Ashley juga mengembangkan karier mandiri. Ashley telah meluncurkan beberapa single, antara lain “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi bareng musisi lain, seperti Afgan dan Rossa.
Aktivitas Personal
Selain kancah panggung, Ashley dikenal sebagai orang yang humble dan bersahabat. Ia menikmati melewatkan masa bersama keluarga dan sahabat-sahabatnya. Ashley juga memiliki hobi menggambar dan fotografi.
hujantoto
Motivasi dari Kutipan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Taylor Swift, seorang artis dan pengarang lagu terkenal, tidak hanya diakui berkat melodi yang menawan dan vokal yang nyaring, tetapi juga sebab syair-syair lagu-lagunya yang penuh makna. Di dalam lirik-liriknya, Swift sering melukiskan bermacam-macam unsur kehidupan, dimulai dari asmara sampai dengan tantangan hidup. Berikut adalah sejumlah petikan inspiratif dari lagu-lagunya, bersama maknanya.
“Mungkin yang terhebat belum hadir.” – “All Too Well”
Arti: Bahkan di masa-masa sulit, tetap ada seberkas harapan dan kemungkinan untuk hari yang lebih baik.
Lirik ini dari lagu “All Too Well” membuat kita ingat bahwa meskipun kita mungkin menghadapi masa sulit saat ini, senantiasa ada kemungkinan bahwa hari esok akan membawa perubahan yang lebih baik. Ini adalah pesan harapan yang mengukuhkan, memotivasi kita untuk tetap bertahan dan tidak menyerah, sebab yang terbaik mungkin belum hadir.
“Aku akan terus bertahan lantaran aku tidak bisa melakukan segala sesuatu tanpa kamu.” – “You Belong with Me”
Arti: Menemukan cinta dan dukungan dari orang lain dapat menghadirkan kita daya dan tekad untuk bertahan melalui kesulitan.
Unduh Aplikasi 888 dan Peroleh Kemenangan: Manual Pendek
**Program 888 adalah opsi unggulan untuk Anda yang menginginkan aktivitas berjudi daring yang menggembirakan dan menguntungkan. Bersama hadiah harian dan fitur memikat, perangkat lunak ini bersiap memberikan keseruan main unggulan. Disini manual singkat untuk memanfaatkan pemanfaatan Perangkat Lunak 888.
Download dan Mulailah Raih
Platform Ada:
Perangkat Lunak 888 bisa diambil di Perangkat Android, Sistem iOS, dan PC. Segera main dengan tanpa kesulitan di alat apa saja.
Hadiah Sehari-hari dan Imbalan
Keuntungan Mendaftar Harian:
Login tiap periode untuk meraih hadiah sebesar 100K pada hari ketujuh.
Selesaikan Pekerjaan:
Peroleh opsi lotere dengan merampungkan aktivitas terkait. Masing-masing aktivitas menyediakan Pengguna satu peluang undi untuk mendapatkan keuntungan hingga 888K.
Pengklaiman Langsung:
Hadiah harus diambil langsung di dalam app. Yakinlah untuk meraih hadiah pada waktu agar tidak kadaluwarsa.
Mekanisme Undian
Kesempatan Lotere:
Setiap waktu, Anda bisa mengklaim 1 opsi undi dengan menyelesaikan aktivitas.
Jika opsi lotere selesai, tuntaskan lebih banyak tugas untuk mengambil tambahan peluang.
Tingkat Hadiah:
Klaim keuntungan jika total pengeretan Kamu melampaui 100K dalam sehari.
Aturan Pokok
Pengklaiman Imbalan:
Bonus harus diterima manual dari perangkat lunak. Jika tidak, imbalan akan secara otomatis diambil ke akun Anda Anda setelah 1 periode.
Syarat Bertaruh:
Hadiah memerlukan setidaknya satu bertaruh efektif untuk diklaim.
Penutup
Program 888 menawarkan keseruan bertaruhan yang menyenangkan dengan bonus besar-besaran. Instal perangkat lunak saat ini dan nikmati kemenangan besar pada masa!
Untuk informasi lebih rinci tentang promo, deposit, dan agenda referensi, lihat halaman utama perangkat lunak.
j200m
Ashley JKT48: Bintang yang Bersinar Terang di Langit Idol
Siapa Ashley JKT48?
Siapakah figur belia berkemampuan yang menarik perhatian sejumlah besar penggemar musik di Indonesia dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama bekennya, Ashley JKT48. Bergabung dengan grup idola JKT48 pada tahun 2018, Ashley dengan cepat menjadi salah satu personel paling populer.
Profil
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley berdarah darah Tionghoa-Indonesia. Ia mengawali perjalanannya di industri entertainment sebagai peraga dan aktris, sebelum akhirnya bergabung dengan JKT48. Personanya yang ceria, suara yang kuat, dan keterampilan menari yang mengesankan membuatnya idol yang sangat dicintai.
Award dan Penghargaan
Ketenaran Ashley telah diakui melalui berbagai apresiasi dan pencalonan. Pada masa 2021, ia meraih penghargaan “Anggota Paling Populer JKT48” di ajang JKT48 Music Awards. Ia juga dinobatkan sebagai “Idol Terindah di Asia” oleh sebuah tabloid digital pada tahun 2020.
Peran dalam JKT48
Ashley memainkan peran krusial dalam grup JKT48. Ia adalah anggota Tim KIII dan berfungsi sebagai penari utama dan vokal utama. Ashley juga menjadi anggota dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Karier Individu
Selain kegiatannya di JKT48, Ashley juga mengembangkan karier solo. Beliau telah mengeluarkan sejumlah single, antara lain “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi bersama musisi lain, seperti Afgan dan Rossa.
Kehidupan Pribadi
Di luar dunia perform, Ashley dikenali sebagai pribadi yang rendah hati dan friendly. Beliau menikmati menghabiskan jam bersama family dan sahabat-sahabatnya. Ashley juga memiliki hobi menggambar dan fotografi.
rajaslot
Pasang Program 888 dan Peroleh Hadiah: Panduan Pendek
**Perangkat Lunak 888 adalah pilihan unggulan untuk Kamu yang mencari aktivitas main daring yang seru dan bermanfaat. Dengan bonus tiap hari dan fasilitas memikat, aplikasi ini siap menawarkan aktivitas main paling baik. Ini panduan cepat untuk menggunakan penggunaan Aplikasi 888.
Download dan Mulai Menang
Layanan Tersedia:
Perangkat Lunak 888 dapat diunduh di Perangkat Android, iOS, dan Windows. Mulailah berjudi dengan praktis di alat apa pun.
Bonus Sehari-hari dan Keuntungan
Bonus Login Sehari-hari:
Mendaftar saban masa untuk mendapatkan imbalan hingga 100K pada periode ketujuh.
Selesaikan Pekerjaan:
Dapatkan opsi undian dengan merampungkan tugas terkait. Masing-masing pekerjaan menyediakan Anda sebuah kesempatan undian untuk mengklaim hadiah sampai 888K.
Penerimaan Langsung:
Keuntungan harus dikumpulkan langsung di dalam app. Jangan lupa untuk mengambil keuntungan tiap waktu agar tidak habis masa berlakunya.
Sistem Lotere
Peluang Pengeretan:
Tiap periode, Anda bisa mengklaim 1 kesempatan undi dengan mengerjakan misi.
Jika peluang undian tidak ada lagi, tuntaskan lebih banyak misi untuk meraih tambahan opsi.
Level Bonus:
Ambil bonus jika akumulasi pengeretan Anda melampaui 100K dalam satu hari.
Ketentuan Utama
Pengklaiman Bonus:
Bonus harus dikumpulkan manual dari program. Jika tidak, keuntungan akan otomatis diambil ke akun Para Pengguna setelah 1 waktu.
Ketentuan Betting:
Bonus butuh setidaknya satu taruhan aktif untuk digunakan.
Kesimpulan
Aplikasi 888 menyediakan aktivitas main yang menggembirakan dengan hadiah signifikan. Pasang program sekarang dan nikmati keberhasilan besar setiap masa!
Untuk informasi lebih terperinci tentang promo, deposit, dan program undangan, periksa situs home program.
statistik liga 1
Inspirasi dari Kutipan Taylor Swift
Taylor Swift, seorang penyanyi dan songwriter terkenal, tidak hanya dikenal berkat nada yang indah dan suara yang nyaring, tetapi juga sebab syair-syair lagunya yang bermakna. Pada kata-katanya, Swift sering menggambarkan beraneka ragam aspek hidup, mulai dari cinta sampai dengan tantangan hidup. Berikut ini adalah beberapa ucapan inspiratif dari lagu-lagunya, bersama maknanya.
“Mungkin yang paling baik belum tiba.” – “All Too Well”
Arti: Bahkan di saat-saat sulit, selalu ada sedikit harapan dan kemungkinan untuk hari yang lebih baik.
Syair ini dari lagu “All Too Well” mengingatkan kita kalau meskipun kita barangkali mengalami waktu sulit saat ini, senantiasa ada potensi bahwa waktu yang akan datang bisa mendatangkan sesuatu yang lebih baik. Situasi ini adalah pesan pengharapan yang menguatkan, memotivasi kita untuk bertahan dan tidak mengalah, lantaran yang terhebat bisa jadi belum datang.
“Aku akan tetap bertahan karena aku tak bisa melakukan apa pun tanpamu.” – “You Belong with Me”
Penjelasan: Memperoleh cinta dan dukungan dari pihak lain dapat memberi kita daya dan niat untuk melanjutkan lewat kesulitan.
Internet casinos are growing more popular, presenting numerous bonuses to attract potential players. One of the most attractive opportunities is the no upfront deposit bonus, a promo that lets players to take a chance without any financial obligation. This article examines the benefits of free bonuses and points out how they can improve their value.
What is a No Deposit Bonus?
A free bonus is a type of casino offer where players are granted free money or free rounds without the need to submit any of their own capital. This lets users to discover the virtual casino, play diverse games and stand a chance to win real money, all without any initial expenditure.
Advantages of No Deposit Bonuses
Risk-Free Exploration
No deposit bonuses provide a risk-free chance to investigate online gambling sites. Players can try multiple slots, learn the casino platform, and evaluate the overall playing environment without investing their own capital. This is especially advantageous for beginners who may not be used to online casinos.
Chance to Win Real Money
One of the most tempting aspects of no-deposit bonuses is the potential to earn real cash. Although the amounts may be minor, any prizes earned from the bonus can usually be collected after meeting the casino’s wagering requirements. This adds an element of anticipation and gives a potential financial reward without any upfront investment.
Learning Opportunity
No upfront deposit bonuses present a great way to grasp how diverse games function. Users can experiment with methods, learn the mechanics of the games, and turn into more comfortable without being concerned about risking their own money. This can be notably helpful for advanced casino options like blackjack.
Conclusion
Free bonuses give various merits for participants, like safe discovery, the opportunity to get real rewards, and beneficial development experiences. As the market continues to expand, the popularity of no deposit bonuses is likely to increase.
free poker
No-cost poker provides participants a one-of-a-kind way to experience the game without any expenditure. This article looks into the advantages of playing free poker and emphasizes why it remains well-liked among many participants.
Risk-Free Entertainment
One of the most significant upsides of free poker is that it permits gamblers to enjoy the joy of poker without fear of losing money. This renders it suitable for novices who hope to get to know the sport without any cost.
Skill Development
Complimentary poker offers a excellent platform for users to enhance their talent. Players can experiment with approaches, understand the guidelines of the pastime, and acquire poise without any pressure of risking their own cash.
Social Interaction
Engaging in free poker can also foster social connections. Online websites commonly feature forums where participants can engage with each other, exchange strategies, and potentially create bonds.
Accessibility
No-cost poker is easy to access to anybody with an network connection. This indicates that participants can experience the activity from the comfort of their own residence, at any moment.
Conclusion
No-cost poker offers several merits for players. It is a risk-free means to enjoy the game, develop skills, enjoy new friendships, and play poker conveniently. As more players discover the merits of free poker, its popularity is anticipated to rise.
casino online
Discovering the Realm of Virtual Casinos
Beginning
In contemporary times, casino online have altered the manner users enjoy gambling. With sophisticated innovations, gamblers can get to their preferred gaming options directly from the comfort of their homes. This write-up investigates the pros of virtual casinos and for why they are amassing favor.
Advantages of Casino Online
Accessibility
One of the major benefits of virtual casinos is convenience. Players can bet whenever and at any place they desire, ending the demand to travel to a land-based casino.
Extensive Game Options
Virtual casinos offer a wide selection of games, spanning from traditional slot games and board games to real-time games and cutting-edge slot machines. This diversity makes sure that there is something for all types of players.
Offers and Deals
Among the most enticing aspects of virtual casinos is the range of rewards and promotions given to players. These can encompass initial bonuses, complimentary spins, cashback incentives, and VIP clubs.
Safety and Security
Trusted virtual casinos make sure gambler protection and protection with sophisticated data protection technologies. This shields individual details and monetary operations.
Motives Behind the Popularity of Internet Casinos
Availability
Casino online are extensively reachable, facilitating gamblers from numerous regions to experience casino games.
성현아 마약
빠른 입출금 서비스와 더불어 주요업체의 보안성
토토사이트 접속 시 핵심적인 요소 중 하나는 빠릿한 입출금 처리입니다. 대개 세 분 안에 입금, 열 분 안에 환전이 처리되어야 합니다. 대형 대형업체들은 충분한 스태프 채용으로 이 같은 빠릿한 환충 절차를 약속하며, 이를 통해 고객들에게 안전한 느낌을 제공합니다. 주요사이트를 이용하면서 빠른 경험을 해보시기 바랍니다. 우리는 여러분이 안전하게 웹사이트를 이용할 수 있도록 지원하는 먹튀 해결 팀입니다.
보증금을 내고 배너를 운영
먹튀 해결 전문가는 최대한 삼천만 원에서 억대의 보증금을 예치한 업체들의 배너를 운영하고 있습니다. 혹시 먹튀 피해가 발생할 시, 배팅 룰에 어긋나지 않은 배팅 내역을 스크린샷을 찍어 먹튀해결사에 문의하시면, 사실 확인 뒤 보증금으로 즉시 피해 보상을 처리합니다. 피해가 생기면 신속하게 스크린샷을 찍어 피해 상황을 기록해두시고 보내주세요.
장기 운영 안전업체 확인
먹튀 해결 팀은 최소 4년 이상 먹튀 문제 없이 안전하게 운영한 사이트들을 확인하여 배너 입점을 받고 있습니다. 이 때문에 어느 누구나 잘 알려진 대형사이트를 안전하게 사용할 수 있는 기회를 제공하고 있습니다. 정확한 검증 작업을 통해 검증된 사이트를 놓치지 않도록, 안전한 베팅을 경험해보세요.
투명성과 공정성을 가진 먹튀 검증
먹튀 해결 전문가의 먹튀 검증은 투명함과 정확함을 근거로 합니다. 언제나 이용자들의 관점을 우선으로 생각하고, 기업의 회유나 이익에 좌우되지 않고 한 건의 삭제 없이 사실만을 바탕으로 검증해왔습니다. 먹튀 사고를 당한 후 후회하지 않도록, 지금 시작하세요.
먹튀 확인 사이트 리스트
먹튀해결사가 선별한 안전한 토토사이트 검증업체 목록 입니다. 현재 등록된 검증업체들은 먹튀 사고 발생 시 100% 보장을 해드립니다. 다만, 제휴 기간이 만료된 업체에서 발생한 문제에 대해서는 책임을 지지 않습니다.
독보적인 먹튀 검증 알고리즘
먹튀 해결 팀은 깨끗한 베팅 문화를 만들기 위해 계속해서 노력합니다. 우리가 소개하는 스포츠토토사이트에서 안전하게 배팅하세요. 회원님의 먹튀 신고는 먹튀 리스트에 등록 노출되어 그 해당 베팅 사이트에 치명적인 영향을 줄 수 있습니다. 먹튀 목록 작성 시 먹튀블러드 만의 검증 지식을 최대한 활용하여 정확한 검증을 할 수 있게 약속드립니다.
안전한 베팅 문화를 조성하기 위해 항상 노력하는 먹튀해결사와 동반하여 안전하게 즐겨보세요.
sweepstakes casino
Analyzing Lottery Gaming Hubs: A Captivating and Available Gaming Alternative
Preface
Contest gaming hubs are becoming a favored alternative for gamers seeking an captivating and legal manner to experience online playing. Unlike traditional digital casinos, lottery gaming hubs work under separate legal frameworks, permitting them to present activities and prizes without falling under the equivalent regulations. This piece investigates the principle of sweepstakes gaming hubs, their merits, and why they are attracting a growing quantity of users.
Understanding Sweepstakes Casinos
A sweepstakes betting site works by providing players with internet money, which can be used to participate in activities. Players can achieve additional online money or physical gifts, like cash. The fundamental disparity from conventional gaming hubs is that players do not buy funds directly but obtain it through marketing efforts, like purchasing a item or joining in a free participation contest. This system allows promotion gaming hubs to work legally in many territories where standard virtual betting is limited.
Discovering Complimentary Casino Games
Beginning
Today, free casino games have turned into a popular selection for casino lovers who desire to engage in betting minus spending money. This article delves into the advantages of free casino games and the causes they are gaining interest.
Pros of Complimentary Casino Games
Risk-Free Gaming
One of the major pros of no-cost casino games is the possibility to gamble devoid of financial strain. Enthusiasts can experience their chosen gaming options minus fretting over wasting funds.
Game Mastery
Free-of-charge casino games offer an superb environment for enthusiasts to hone their skills. Be it practicing methods in poker, enthusiasts can train devoid of monetary repercussions.
Diverse Game Selection
No-cost casino games supply a wide variety of gaming options, such as classic slot games, board games, and live dealer games. This variety ensures that there is something for everyone.
Reasons Players Choose No-Cost Casino Games
Reachability
Complimentary casino games are extensively accessible, enabling enthusiasts from numerous regions to enjoy gambling.
Zero Financial Risk
Unlike money-based casino activities, no-cost casino games do not need a monetary obligation. This facilitates players to engage in casino activities devoid of concerns about losing funds.
Try Before You Invest
Free casino games supply enthusiasts the ability to try betting activities ahead of spending real cash. This enables players create educated choices.
Conclusion
Complimentary casino games supplies a fun and safe way to experience betting. With free from financial burden, diverse game options, and possibilities for skill development, it is understandable that countless gamblers choose complimentary casino games for their betting choices.
Unveiling Cash Slots
Introduction
Cash slots have turned into a well-liked option for gamblers looking for the rush of earning real money. This piece delves into the pros of cash slots and the motivations they are attracting a growing number of enthusiasts.
Pros of Money Slots
Real Winnings
The key draw of real money slots is the possibility to earn real currency. As opposed to free slots, money slots supply users the adrenaline of potential monetary payouts.
Diverse Game Options
Money slots give a wide range of styles, elements, and payout structures. This guarantees that there is something for everyone, covering classic 3-reel slots to up-to-date animated slots with various betting lines and extra rounds.
Attractive Offers
Numerous internet casinos offer thrilling rewards for real money slot gamblers. These can consist of welcome bonuses, extra spins, rebate offers, and rewards programs. Such incentives boost the overall casino adventure and give further potential to secure currency.
Why Enthusiasts Enjoy Gambling Slots
The Adrenaline of Gaining Genuine Funds
Money slots offer an exciting activity, as users await the opportunity of securing actual money. This element injects an extra layer of excitement to the gaming activity.
Prompt Payouts
Cash slots give gamblers the pleasure of quick rewards. Earning funds immediately enhances the casino journey, rendering it more rewarding.
Numerous Game Choices
Including money slots, gamblers have access to a broad variety of slot machines, assuring that there is consistently a game exciting to test.
Closing
Money slots provides a exciting and satisfying betting experience. With the chance to gain real funds, a wide variety of slot games, and exciting promotions, it’s no wonder that numerous gamblers choose money slots for their gaming needs.
bitz casino регистрация
вход bitz casino
The numbers of water molecules within 2, 3 and 4 Г… were 394, 964 and 1 361 molecules, respectively soft tab cialis
Pro88
сео консультант
Советы по оптимизации продвижению.
Информация о том как управлять с низкочастотными запросами ключевыми словами и как их выбирать
Тактика по деятельности в конкурентоспособной нише.
Обладаю постоянных сотрудничаю с тремя организациями, есть что поделиться.
Посмотрите мой профиль, на 31 мая 2024г
количество выполненных работ 2181 только на этом сайте.
Консультация только устно, без скринов и отчётов.
Длительность консультации указано 2 часа, но по сути всегда на доступен без строгой привязки ко времени.
Как работать с ПО это уже отдельная история, консультация по использованию ПО оговариваем отдельно в другом услуге, выясняем что необходимо при разговоре.
Всё спокойно на расслабленно не в спешке
To get started, the seller needs:
Мне нужны контакты от Telegram чата для связи.
общение только вербально, общаться письменно не хватает времени.
Сб и Воскресенье выходные
Revitalize romance with generic viagra. Enhance your satisfaction discreetly.
ibetslot
vòng loại euro 2024
娛樂城官網
娛樂城官網
Are branded medicines more expensive than generic drugs coupon for ventolin hfa with insurance?
pharmacie en ligne pas cher https://kamagraenligne.shop/# trouver un mГ©dicament en pharmacie
Thanks for any other fantastic post. Where else could anybody get that kind of information in such a perfect approach of writing? I’ve a presentation subsequent week, and I am on the search for such info.
http://www.arusak-attestats24.com
Why users still make use of to read news papers when in this technological world the whole thing is presented on net?
pharmacie en ligne avec ordonnance: Medicaments en ligne livres en 24h – pharmacie en ligne livraison europe
https://emmerechts.com/?keyword=indonesia-vs-irak-u23
Slotเว็บตรง – สนุกกับการเล่นได้ทุกอุปกรณ์เชื่อมต่อที่ต่ออินเทอร์เน็ต
ในสมัยนี้ การหมุนสล็อตมีความง่ายดายมากยิ่งขึ้น คุณไม่จำเป็นเดินทางไปยังสถานที่เล่นคาสิโนที่ไหน ๆ เพียงแค่มีอุปกรณ์ที่ใช้งานได้เชื่อมต่อกับอินเทอร์เน็ต คุณก็มีโอกาสสนุกกับการเล่นสล็อตออนไลน์กับ PG Slot ได้จากทุกที่
การพัฒนาเทคโนโลยีของ PG Slot
ที่ PG Slot เราได้ปรับปรุงโซลูชั่นสำหรับการให้บริการเกมคาสิโนออนไลน์เพื่อตอบสนองความต้องการของลูกค้าให้มากที่สุด คุณไม่จำเป็นติดตั้งซอฟต์แวร์หรือดาวน์โหลดแอปพลิเคชันใด ๆ ให้ยุ่งยากหรือใช้พื้นที่ในอุปกรณ์อิเล็กทรอนิกส์ของคุณ การให้บริการเกมสล็อตออนไลน์ของเราทำงานผ่านเว็บตรงที่ใช้เทคโนโลยี HTML 5 ที่ทันสมัย
เล่นสล็อตได้ทุกอุปกรณ์เชื่อมต่อ
คุณอาจเล่นสล็อตออนไลน์กับ PG Slot ได้อย่างสะดวกเพียงเข้าสู่ในเว็บไซต์ของเรา เว็บตรงสล็อตออนไลน์ของเรารองรับทุกซอฟต์แวร์และทุกอุปกรณ์ทั้ง Android และ iOS ไม่ว่าคุณจะใช้สมาร์ทโฟน แล็ปท็อป หรือแท็บเล็ตรุ่นไหน ก็อาจมั่นใจได้ว่าคุณจะเล่นเกมสล็อตออนไลน์ได้อย่างไม่มีสะดุด ไม่มีการขัดข้องหรือติดขัดใด ๆ
ลองเล่นเกมสล็อตฟรี
เว็บตรงของเราเปิดให้บริการเพียงแค่คุณเข้าสู่ในเว็บไซต์ของ PG Slot ก็จะทดลองเล่นสล็อตฟรีได้ทันที ไม่ต้องเสียค่าใช้จ่ายใด ๆ นี่เป็นโอกาสที่ดีในการฝึกฝนทักษะและศึกษาวิธีการเล่นเกี่ยวกับเกมก่อนที่จะเล่นเพื่อเงินจริงด้วยเงินจริง
การหมุนสล็อตออนไลน์กับ PG Slot ช่วยให้คุณสามารถเพลิดเพลินกับการเล่นเกมคาสิโนได้ทุกที่ทุกเวลา ไม่ว่าคุณจะอยู่ที่ไหน เพียงแค่มีอุปกรณ์เชื่อมต่อที่เข้าถึงอินเทอร์เน็ต คุณก็มีโอกาสสนุกกับการเล่นเกมสล็อตได้อย่างไม่มีข้อผูกมัด!
The other day, while I was at work, my sister stole my iphone and tested to see if it can survive a 30 foot drop, just so she can be a youtube sensation. My apple ipad is now broken and she has 83 views. I know this is totally off topic but I had to share it with someone!
http://www.arusak-attestats24.com
Just want to say your article is as surprising. The clearness in your post is just nice and i can assume you’re an expert on this subject. Fine with your permission allow me to grab your feed to keep up to date with forthcoming post. Thanks a million and please keep up the rewarding work.
result macau 5d
娛樂城
富遊娛樂城評價:2024年最新評價
推薦指數 : ★★★★★ ( 5.0/5 )
富遊娛樂城作為目前最受歡迎的博弈網站之一,在台灣擁有最高的註冊人數。
RG富遊以安全、公正、真實和順暢的品牌保證,贏得了廣大玩家的信賴。富遊線上賭場不僅提供了豐富多樣的遊戲種類,還有眾多吸引人的優惠活動。在出金速度方面,獲得無數網紅和網友的高度評價,確保玩家能享有無憂的博弈體驗。
推薦要點
新手首選: 富遊娛樂城,2024年評選首選,提供專為新手打造的豐富教學和獨家優惠。
一存雙收: 首存1000元,立獲1000元獎金,僅需1倍流水,新手友好。
免費體驗: 新玩家享免費體驗金,暢遊各式遊戲,開啟無限可能。
優惠多元: 活動豐富,流水要求低,適合各類型玩家。
玩家首選: 遊戲多樣,服務優質,是新手與老手的最佳賭場選擇。
富遊娛樂城詳情資訊
賭場名稱 : RG富遊
創立時間 : 2019年
賭場類型 : 現金版娛樂城
博弈執照 : 馬爾他牌照(MGA)認證、英屬維爾京群島(BVI)認證、菲律賓(PAGCOR)監督競猜牌照
遊戲類型 : 真人百家樂、運彩投注、電子老虎機、彩票遊戲、棋牌遊戲、捕魚機遊戲
存取速度 : 存款5秒 / 提款3-5分
軟體下載 : 支援APP,IOS、安卓(Android)
線上客服 : 需透過官方LINE
富遊娛樂城優缺點
優點
台灣註冊人數NO.1線上賭場
首儲1000贈1000只需一倍流水
擁有體驗金免費體驗賭場
網紅部落客推薦保證出金線上娛樂城
缺點
需透過客服申請體驗金
富遊娛樂城存取款方式
存款方式
提供四大超商(全家、7-11、萊爾富、ok超商)
虛擬貨幣ustd存款
銀行轉帳(各大銀行皆可)
取款方式
網站內申請提款及可匯款至綁定帳戶
現金1:1出金
富遊娛樂城平台系統
真人百家 — RG真人、DG真人、歐博真人、DB真人(原亞博/PM)、SA真人、OG真人、WM真人
體育投注 — SUPER體育、鑫寶體育、熊貓體育(原亞博/PM)
彩票遊戲 — 富遊彩票、WIN 539
電子遊戲 —RG電子、ZG電子、BNG電子、BWIN電子、RSG電子、GR電子(好路)
棋牌遊戲 —ZG棋牌、亞博棋牌、好路棋牌、博亞棋牌
電競遊戲 — 熊貓體育
捕魚遊戲 —ZG捕魚、RSG捕魚、好路GR捕魚、DB捕魚
https://rushmorgan.com/?keyword=pgslot88
2024娛樂城推薦,經過玩家實測結果出爐Top5!
2024娛樂城排名是這五間上榜,玩家尋找娛樂城無非就是要找穩定出金娛樂城,遊戲體驗良好、速度流暢,Ace博評網都幫你整理好了,給予娛樂城新手最佳的指南,不再擔心被黑網娛樂城詐騙!
2024娛樂城簡述
在現代,2024娛樂城數量已經超越以前,面對琳瑯滿目的娛樂城品牌,身為新手的玩家肯定難以辨別哪間好、哪間壞。
好的平台提供穩定的速度與遊戲體驗,穩定的系統與資訊安全可以保障用戶的隱私與資料,不用擔心收到傳票與任何網路威脅,這些線上賭場也提供合理的優惠活動給予玩家。
壞的娛樂城除了會騙取你的金錢之外,也會打著不實的廣告、優惠滿滿,想領卻是一場空!甚至有些平台還沒辦法登入,入口網站也是架設用來騙取新手儲值進他們口袋,這些黑網娛樂城是玩家必須避開的風險!
評測2024娛樂城的標準
Ace這次從網路上找來五位使用過娛樂城資歷2年以上的老玩家,給予他們使用各大娛樂城平台,最終選出Top5,而評選標準為下列這些條件:
以玩家觀點出發,優先考量玩家利益
豐富的遊戲種類與卓越的遊戲體驗
平台的信譽及其安全性措施
客服團隊的回應速度與服務品質
簡便的儲值流程和多樣的存款方法
吸引人的優惠活動方案
前五名娛樂城表格
賭博網站排名 線上賭場 平台特色 玩家實測評價
No.1 富遊娛樂城 遊戲選擇豐富,老玩家優惠多 正面好評
No.2 bet365娛樂城 知名大廠牌,運彩盤口選擇多 介面流暢
No.3 亞博娛樂城 多語言支持,介面簡潔順暢 賽事豐富
No.4 PM娛樂城 撲克牌遊戲豐富,選擇多元 直播順暢
No.5 1xbet娛樂城 直播流暢,安全可靠 佳評如潮
線上娛樂城玩家遊戲體驗評價分享
網友A:娛樂城平台百百款,富遊娛樂城是我3年以來長期使用的娛樂城,別人有的系統他們都有,出金也沒有被卡過,比起那些玩娛樂城還會收到傳票的娛樂城,富遊真的很穩定,值得推薦。
網友B:bet365中文的介面簡約,還有超多體育賽事盤口可以選擇,此外賽事大部分也都有附上直播來源,不必擔心看不到賽事最新狀況,全螢幕還能夠下單,真的超方便!
網友C:富遊娛樂城除了第一次儲值有優惠之外,儲值到一定金額還有好禮五選一,實用又方便,有問題的時候也有客服隨時能夠解答。
網友D:從大陸來台灣工作,沒想到台灣也能玩到亞博體育,這是以前在大陸就有使用的平台,雖然不是簡體字,但使用介面完全沒問題,遊戲流暢、速度比以前使用還更快速。
網友E:看玖壹壹MV發現了PM娛樂城這個大品牌,PM的真人百家樂沒有輸給在澳門實地賭場,甚至根本不用出門,超級方便的啦!
https://codemobile.ca/rupiahtoto
Thanks for the auspicious writeup. It in fact was a enjoyment account it. Glance complex to more delivered agreeable from you! By the way, how can we be in contact?
musey-uglich.ru
Player台灣線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
layer如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
安全與公平性
安全永遠是我們評測的首要標準。我們審查每家娛樂城的執照資訊、監管機構以及使用的隨機數生成器,以確保其遊戲結果的公平性和隨機性。
02.
遊戲品質與多樣性
遊戲的品質和多樣性對於玩家體驗至關重要。我們評估遊戲的圖形、音效、用戶介面和創新性。同時,我們也考量娛樂城提供的遊戲種類,包括老虎機、桌遊、即時遊戲等。
03.
娛樂城優惠與促銷活動
我們仔細審視各種獎勵計劃和促銷活動,包括歡迎獎勵、免費旋轉和忠誠計劃。重要的是,我們也檢查這些優惠的賭注要求和條款條件,以確保它們公平且實用。
04.
客戶支持
優質的客戶支持是娛樂城質量的重要指標。我們評估支持團隊的可用性、響應速度和專業程度。一個好的娛樂城應該提供多種聯繫方式,包括即時聊天、電子郵件和電話支持。
05.
銀行與支付選項
我們檢查娛樂城提供的存款和提款選項,以及相關的處理時間和手續費。多樣化且安全的支付方式對於玩家來說非常重要。
06.
網站易用性、娛樂城APP體驗
一個直觀且易於導航的網站可以顯著提升玩家體驗。我們評估網站的設計、可訪問性和移動兼容性。
07.
玩家評價與反饋
我們考慮真實玩家的評價和反饋。這些資料幫助我們了解娛樂城在實際玩家中的表現。
娛樂城常見問題
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
娛樂城
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
В нашем обществе, где диплом – это начало отличной карьеры в любом направлении, многие пытаются найти максимально простой путь получения образования. Факт наличия официального документа сложно переоценить. Ведь именно он открывает дверь перед каждым человеком, который стремится вступить в сообщество профессионалов или учиться в ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы можете заказать диплом нового или старого образца, и это является отличным решением для всех, кто не смог закончить обучение или потерял документ. Любой диплом изготавливается аккуратно, с особым вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Плюсы данного подхода заключаются не только в том, что вы максимально быстро получите диплом. Весь процесс организован удобно, с нашей поддержкой. От выбора нужного образца диплома до консультаций по заполнению личной информации и доставки в любое место страны — все будет находиться под абсолютным контролем качественных мастеров.
Для тех, кто ищет оперативный способ получения требуемого документа, наша услуга предлагает отличное решение. Приобрести диплом – это значит избежать продолжительного процесса обучения и сразу перейти к достижению собственных целей: к поступлению в ВУЗ или к началу удачной карьеры.
http://www.seoyour.ru
Hi! Do you know if they make any plugins to safeguard against hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any recommendations?
http://musey-uglich.ru/
娛樂城
2024娛樂城介紹
台灣2024娛樂城越開越多間,新開的線上賭場層出不窮,每間都以獨家的娛樂城優惠和體驗金來吸引玩家,致力於提供一流的賭博遊戲體驗。以下來介紹這幾間娛樂城網友對他們的真實評價,看看哪些娛樂城上榜了吧!
2024娛樂城排名
2023下半年,各家娛樂城競爭激烈,相繼推出誘人優惠,不論是娛樂城體驗金、反水流水還是首儲禮金,甚至還有娛樂城抽I15手機。以下就是2024年網友推薦的娛樂城排名:
NO.1 富遊娛樂城
NO.2 Bet365台灣
NO.3 DG娛樂城
NO.4 九州娛樂城
NO.5 亞博娛樂城
2024娛樂城推薦
根據2024娛樂城排名,以下將富遊娛樂城、BET365、亞博娛樂城、九州娛樂城、王者娛樂城推薦給大家,包含首儲贈點、免費體驗金、存提款速度、流水等等…
娛樂城遊戲種類
線上娛樂城憑藉其廣泛的遊戲種類,成功滿足了各式各樣玩家的喜好和需求。這些娛樂城遊戲不僅多元化且各具特色,能夠為玩家提供無與倫比的娛樂體驗。下面是一些最受歡迎的娛樂城遊戲類型:
電子老虎機
魔龍傳奇、雷神之鎚、戰神呂布、聚寶財神、鼠來寶、皇家777
真人百家樂
真人視訊百家樂、牛牛、龍虎、炸金花、骰寶、輪盤
電子棋牌
德州撲克、兩人麻將、21點、十三支、妞妞、三公、鬥地主、大老二、牌九
體育下注
世界盃足球賽、NBA、WBC世棒賽、英超、英雄聯盟LOL、特戰英豪
線上彩票
大樂透、539、美國天天樂、香港六合彩、北京賽車
捕魚機遊戲
三仙捕魚、福娃捕魚、招財貓釣魚、西遊降魔、吃我一砲、賓果捕魚
2024娛樂城常見問題
娛樂城是什麼?
娛樂城/線上賭場(現金網)是台灣對於線上賭場的特別稱呼,而且是現金網,大家也許會好奇為什麼不直接叫做線上賭場或是線上博弈就好了。
其實這是有原因的,線上賭場這種東西,架站在台灣是違法的,在早期經營線上博弈被抓的風險非常高所以換了一個打模糊仗的代稱「娛樂城」來規避警方的耳目,畢竟以前沒有Google這種東西,這樣的代稱還是多少有些作用的。
信用版娛樂城是什麼?
信用版娛樂城是一種賭博平台,允許玩家在沒有預先充值的情況下參與遊戲。這種模式類似於信用卡,通常以周結或月結的方式結算遊戲費用。因此,如果玩家無法有效管理自己的投注額,可能會在月底面臨巨大的支付壓力。
娛樂城不出金怎麼辦?
釐清原因,如未違反娛樂城機制,可能是遇上黑網娛樂城,請盡快通報165反詐騙。
娛樂城
Player台灣線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
layer如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
安全與公平性
安全永遠是我們評測的首要標準。我們審查每家娛樂城的執照資訊、監管機構以及使用的隨機數生成器,以確保其遊戲結果的公平性和隨機性。
02.
遊戲品質與多樣性
遊戲的品質和多樣性對於玩家體驗至關重要。我們評估遊戲的圖形、音效、用戶介面和創新性。同時,我們也考量娛樂城提供的遊戲種類,包括老虎機、桌遊、即時遊戲等。
03.
娛樂城優惠與促銷活動
我們仔細審視各種獎勵計劃和促銷活動,包括歡迎獎勵、免費旋轉和忠誠計劃。重要的是,我們也檢查這些優惠的賭注要求和條款條件,以確保它們公平且實用。
04.
客戶支持
優質的客戶支持是娛樂城質量的重要指標。我們評估支持團隊的可用性、響應速度和專業程度。一個好的娛樂城應該提供多種聯繫方式,包括即時聊天、電子郵件和電話支持。
05.
銀行與支付選項
我們檢查娛樂城提供的存款和提款選項,以及相關的處理時間和手續費。多樣化且安全的支付方式對於玩家來說非常重要。
06.
網站易用性、娛樂城APP體驗
一個直觀且易於導航的網站可以顯著提升玩家體驗。我們評估網站的設計、可訪問性和移動兼容性。
07.
玩家評價與反饋
我們考慮真實玩家的評價和反饋。這些資料幫助我們了解娛樂城在實際玩家中的表現。
娛樂城常見問題
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
台灣線上娛樂城
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
bimabet
pg
สล็อตเว็บโดยตรง — ใช้ สมาร์ทโฟน แท็บเล็ต คอมพิวเตอร์ส่วนตัว ฯลฯ สำหรับการเล่น
ระบบสล็อตเว็บโดยตรง ของ พีจีสล็อต ได้รับการพัฒนาและอัปเดต เพื่อให้ รองรับการใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง ครบถ้วน ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเล็ต หรือ คอมพิวเตอร์ รุ่นใด
ที่ PG Slot เราเข้าใจถึงความต้องการ จากผู้เล่น ในเรื่อง การใช้งานง่าย และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง นำ HTML 5 มาใช้ ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ปัจจุบันนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง ดาวน์โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเว็บเบราว์เซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บของเรา คุณสามารถ เพลิดเพลินกับสล็อตแมชชีนได้ทันที
การใช้งานกับอุปกรณ์หลากหลาย
ไม่ว่าคุณจะใช้ โทรศัพท์มือถือ ระบบ Android หรือ ไอโอเอส ก็สามารถ เล่นเกมสล็อตได้อย่างไม่มีปัญหา ระบบของเรา ได้รับการออกแบบให้รองรับ ระบบปฏิบัติการทั้งหมด ไม่สำคัญว่าคุณ มี โทรศัพท์ ใหม่หรือเก่า หรือ แม้แต่แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้ดี ไม่มีปัญหา ความเข้ากันได้
เล่นได้ทุกที่และทุกเวลา
ข้อดีอย่างหนึ่งของการเล่นเว็บสล็อตอย่าง PG Slot คือ คุณสามารถ เล่นได้ทุกที่ทุกเวลา ไม่ว่าจะ เป็นที่บ้าน ที่ทำงาน หรือแม้แต่ สถานที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเกมได้ทันที และคุณไม่ต้อง กังวลกับการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่บนอุปกรณ์ของคุณ
ลองเล่นสล็อตแมชชีนฟรี
เพื่อให้ ผู้เล่นที่ใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
การบริการและความปลอดภัย
PG Slot ตั้งใจให้บริการที่ดีที่สุดกับลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี การรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
ข้อดีอีกประการของการเล่นสล็อตแมชชีนกับ PG Slot นั่นคือ มี โปรโมชันและโบนัสพิเศษสำหรับสมาชิก ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือเก่า คุณสามารถ รับโปรโมชั่นและโบนัสต่างๆได้อย่างต่อเนื่อง สิ่งนี้จะ เพิ่มโอกาสชนะและความสนุกในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
https://giah1.com/?keyword=paito-harian-hk
สล็อต
สล็อตออนไลน์เว็บตรง: ความสนุกสนานที่ผู้เล่นไม่ควรพลาด
การเล่นเกมสล็อตในยุคนี้เป็นที่นิยมเพิ่มมากขึ้น เนื่องจากความสะดวกที่นักเดิมพันสามารถเล่นได้ได้ทุกที่ได้ตลอดเวลา โดยไม่ต้องเสียเวลาในการการเดินทางถึงบ่อน ในบทความนี้ที่เราจะนำเสนอ เราจะมาพูดถึง “สล็อตแมชชีน” และความเพลิดเพลินที่คุณสามารถพบได้ในเกมสล็อตออนไลน์เว็บตรง
ความง่ายดายในการเล่นสล็อต
เหตุผลหนึ่งที่ทำให้สล็อตที่เว็บตรงเป็นที่ยอดนิยมอย่างมาก คือความสะดวกที่ผู้ใช้มี คุณจะเล่นได้ทุกหนทุกแห่งทุกเวลา ไม่ว่าจะเป็นที่บ้านของคุณ ที่ทำงาน หรือแม้แต่ในการเดินทาง สิ่งที่คุณควรมีคือเครื่องมือที่สามารถเชื่อมต่ออินเทอร์เน็ตได้ ไม่ว่าจะเป็นโทรศัพท์มือถือ แทปเล็ต หรือแล็ปท็อป
นวัตกรรมกับสล็อตออนไลน์เว็บตรง
การเล่นเกมสล็อตในปัจจุบันไม่เพียงแต่สะดวกสบาย แต่ยังมาพร้อมกับเทคโนโลยีที่ทันสมัยที่ทันสมัยอีกด้วย สล็อตที่เว็บตรงใช้เทคโนโลยีที่ทันสมัย HTML5 ซึ่งทำให้คุณไม่ต้องกังวลเกี่ยวกับการลงซอฟต์แวร์หรือแอปพลิเคชันเพิ่มเติม แค่ใช้เบราว์เซอร์บนอุปกรณ์ของคุณและเข้าสู่เว็บของเรา ท่านก็สามารถเริ่มเล่นเกมสล็อตได้ทันที
ตัวเลือกหลากหลายของเกมของสล็อต
สล็อตออนไลน์เว็บตรงมาพร้อมกับความหลากหลายของเกมให้เลือกที่ท่านสามารถเลือกเล่นได้ ไม่ว่าจะเป็นสล็อตคลาสสิกหรือเกมที่มีฟีเจอร์เด็ดและโบนัสมากมาย ผู้เล่นจะพบว่ามีเกมให้เลือกเล่นมากมาย ซึ่งทำให้ไม่เบื่อกับการเล่นสล็อต
การรองรับทุกอุปกรณ์ที่ใช้
ไม่ว่าผู้เล่นจะใช้มือถือแอนดรอยด์หรือ iOS คุณก็สามารถเล่นเกมสล็อตออนไลน์ได้ได้อย่างลื่นไหล เว็บไซต์ของเรารองรับทุกระบบปฏิบัติการและทุกอุปกรณ์ ไม่ว่าจะเป็นโทรศัพท์มือถือรุ่นใหม่หรือรุ่นก่อน หรือแม้กระทั่งแทปเล็ตและแล็ปท็อป คุณก็สามารถเล่นเกมสล็อตได้ได้อย่างครบถ้วน
สล็อตทดลองฟรี
สำหรับผู้ที่ยังใหม่กับการเล่นสล็อตออนไลน์ หรือยังไม่แน่นอนเกี่ยวกับเกมที่อยากเล่น PG Slot ยังมีบริการสล็อตทดลองฟรี ท่านสามารถเริ่มเล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงินลงทุน การทดลองเล่นสล็อตนี้จะช่วยให้ท่านเรียนรู้วิธีการเล่นและเข้าใจเกมได้โดยไม่ต้องเสียเงิน
โปรโมชันและโบนัส
ข้อดีอีกอย่างหนึ่งของการเล่นสล็อตออนไลน์กับ PG Slot คือมีโปรโมชันและโบนัสมากมายสำหรับนักเดิมพัน ไม่ว่าผู้เล่นจะเป็นสมาชิกเพิ่งสมัครหรือสมาชิกที่มีอยู่ ท่านสามารถใช้โบนัสและโปรโมชันต่าง ๆ ได้อย่างสม่ำเสมอ ซึ่งจะเพิ่มโอกาสในการชนะและเพิ่มความสนุกในการเล่น
โดยสรุป
การเล่นเกมสล็อตออนไลน์ที่ PG Slot เป็นการลงทุนที่คุ้มค่า ท่านจะได้รับความสนุกและความง่ายดายจากการเล่นสล็อต นอกจากนี้ยังมีโอกาสชนะรางวัลและโบนัสมากมาย ไม่ว่าผู้เล่นจะใช้โทรศัพท์มือถือ แท็บเล็ทหรือโน้ตบุ๊กรุ่นไหน ก็สามารถร่วมสนุกกับเราได้ทันที อย่ารอช้า ลงทะเบียนและเริ่มเล่น PG Slot ทันที
สล็อตเว็บตรง — ใช้ สมาร์ทโฟน แท็บเลต คอมพิวเตอร์ ฯลฯ เพื่อเล่น
ระบบสล็อตเว็บตรง ของ PG ได้รับการพัฒนาและปรับปรุง เพื่อให้ รองรับการใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเล็ต หรือ คอมพิวเตอร์ส่วนตัว แบบไหน
ที่ PG Slot เราเข้าใจถึงสิ่งที่ผู้เล่นต้องการ ของลูกค้า ในเรื่อง ความสะดวกสบาย และ การเข้าถึงเกมคาสิโนที่รวดเร็ว เราจึง ใช้ HTML 5 ซึ่งเป็น เทคโนโลยีล่าสุด ปัจจุบันนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง ดาวน์โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ มีอยู่ของคุณ และเยี่ยมชม เว็บไซต์ของเรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การรองรับอุปกรณ์หลายชนิด
ไม่ว่าคุณจะใช้ โทรศัพท์มือถือ ระบบ Android หรือ iOS ก็สามารถ เล่นสล็อตออนไลน์ได้ไม่มีสะดุด ระบบของเรา ได้รับการออกแบบให้รองรับ ระบบต่าง ๆ ไม่สำคัญว่าคุณ กำลังใช้ มือถือ รุ่นใหม่หรือรุ่นเก่า หรือ แม้แต่แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา ในเรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
ข้อดีของการเล่น PG Slot คือ คุณสามารถ เล่นได้ทุกที่ทุกเวลา ไม่ว่าจะ เป็นที่บ้าน ออฟฟิศ หรือแม้แต่ ที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง กังวลกับการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่บนอุปกรณ์ของคุณ
ทดลองเล่นสล็อตฟรี
เพื่อให้ ผู้เล่นใหม่ มีโอกาสลองและสัมผัสประสบการณ์สล็อตแมชชีนของเรา PG Slot ยังมีสล็อตทดลองฟรี คุณสามารถ ทดลองเล่นได้ทันทีโดยไม่ต้องสมัครหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
การบริการและความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชั่นและโบนัสพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี คือ มี โปรโมชันและโบนัสมากมาย ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชั่นและโบนัสต่างๆได้อย่างต่อเนื่อง สิ่งนี้จะ เพิ่มโอกาสในการชนะและเพิ่มความเพลิดเพลินในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ทดลองเล่นสล็อต
ทดลองดำเนินการเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังมองหาความบันเทิงและโอกาสในการแสวงหารางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งตัวเลือกที่คุ้มค่าใคร่ครวญ.ด้วยความมากมายของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถทดลองเล่นและค้นหาเกมที่ถูกใจได้อย่างง่ายดาย.
ไม่ว่าคุณจะถูกใจเกมสล็อตคลาสสิกหรือต้องการสิ่งใหม่, ตัวเลือกรอล้ำหน้าให้คุณสัมผัส. จากสล็อตที่มีธีมมากมาย ไปจนถึงเกมที่มีรูปแบบพิเศษและรางวัล, ผู้เล่นจะได้พบกับการทดลองเล่นที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการทดลองเล่นสล็อตฟรี, คุณสามารถศึกษาวิธีการเล่นและค้นเลือกกลยุทธ์ที่ถูกใจก่อนสร้างรายได้ด้วยเงินจริง. นี่คือโอกาสที่จะเรียนรู้กับเกมและเพิ่มโอกาสในการแสดงรางวัลใหญ่.
อย่าประวิงเวลา, เข้าร่วมกับการทดสอบสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินกับความสนใจ, ความสนุกสนาน และโอกาสทองชนะรางวัลมหาศาล. กล้าก้าวไปเดินทางสู่ความเฟื่องฟูของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
ลอง ใช้งาน สล็อต PG ไปพร้อมกับ ค้นพบ ไปสู่ ยุค แห่ง ความบันเทิง ที่ ไม่มีที่สิ้นสุด
ต่อ นักเสี่ยงโชค ที่ ต้องการ ค้นหา ประสบการณ์ เกมที่แปลกใหม่, สล็อต PG คือ ทางเลือก ที่ น่าสนใจ มาก. เนื่องจาก ความหลากหลายของ ของ เกมสล็อต ที่ น่าสนใจ และ น่าสำรวจ, นักพนัน จะมีโอกาส ลองเล่น และ ค้นพบ ประเภทเกม ที่ ถูกใจ แบบอย่างการเล่น ของตนเอง.
ไม่ว่า ลูกค้า จะพอใจกับ ความเพลิดเพลิน แบบทั่วไป หรือ ความยากท้าทาย ที่แปลกใหม่, สล็อต PG ให้เลือก ให้เลือกมากมาย. ตั้งแต่ สล็อตรูปแบบคลาสสิค ที่ คุ้นเคยกัน ไปจนถึง รูปแบบเกม ที่ ให้ ลักษณะพิเศษ และ โบนัสล้นหลาม, ผู้เล่น จะสามารถ พบเจอ การเล่น ที่ ดึงดูดใจ และ สนุกสนาน
เพราะ การทดลองเล่น สล็อต PG ฟรีโดยไม่ต้องลงทุน, ลูกค้า จะสามารถ ศึกษา วิธีการเล่น และ ตรวจสอบ กลเม็ด ต่างๆ ก่อนหน้า เริ่มพนัน ด้วยเงินจริง. ถึงกระนั้น เป็น ช่องทาง อันดี ที่จะ วางแผน และ ส่งเสริม โอกาส ในการ คว้ารางวัล รางวัลใหญ่.
อย่าชักช้า, เข้าถึง ด้วย การเล่นทดลอง สล็อต PG เดี๋ยวนี้ และ พบเจอ ความรู้สึก ที่ ไม่จำกัด! พบเจอ ความตื่นเต้นระคนตื่นเต้น, ความบันเทิง และ ความเป็นไปได้ ในการ คว้ารางวัล มากมาย. เริ่มลงมือ พัฒนา สู่ ความสมหวัง ของคุณในวงการ การพนันสล็อต เดี๋ยวนี้!
pg สล็อต
เมื่อเทียบ ไซต์ PG Slots พวกเขา มี ข้อได้เปรียบ หลายประการ ในเปรียบเทียบกับ คาสิโนแบบ ดั้งเดิม, อย่างเฉพาะเจาะจง ใน ปัจจุบัน. คุณสมบัติสำคัญ เหล่านี้ ประกอบด้วย:
ความง่ายสะดวก: คุณ สามารถเข้าร่วม สล็อตออนไลน์ได้ ทุกเวลา จาก ทุกสถานที่, อำนวย ผู้เล่นสามารถ เล่น ได้ ทุกแห่ง โดยไม่ต้อง ต้องเดินทาง ไปคาสิโนแบบ เดิม ๆ
เกมมากมายแตกต่าง: สล็อตออนไลน์ ให้ ตัวเกม ที่ หลากหลาย, เช่น สล็อตคลาสสิค หรือ รูปแบบเกม ที่มี ฟีเจอร์ และค่าตอบแทน พิเศษ, ไม่ก่อให้เกิด ความเบื่อ ในเกม
แคมเปญส่งเสริมการขาย และค่าตอบแทน: สล็อตออนไลน์ โดยทั่วไป ให้บริการ แคมเปญส่งเสริมการขาย และประโยชน์ เพื่อเพิ่ม ความเป็นไปได้ ในการ ได้รับรางวัล และ เพิ่ม ความบันเทิง ให้กับเกม
ความมั่นคง และ ความเชื่อถือได้: สล็อตออนไลน์ แทบจะ มี มาตรการรักษาความปลอดภัย ที่ มีประสิทธิภาพ, และ ทำให้มั่นใจ ว่า ข้อมูลส่วนบุคคล และ การเงิน จะได้รับ คุ้มครอง
การสนับสนุนลูกค้า: PG Slots มีทีม ผู้ให้บริการ ที่มีความเชี่ยวชาญ ที่ตั้งใจ ช่วยเหลือ ตลอด 24 ชั่วโมง
การเล่นบนอุปกรณ์พกพา: สล็อต PG สนับสนุน การเล่นบนอุปกรณ์เคลื่อนที่, อำนวย ผู้เล่นสามารถเล่น ตลอด 24 ชั่วโมง
เล่นทดลองฟรี: สำหรับ ผู้เล่นเริ่มต้น, PG ยังให้บริการ เล่นทดลองฟรี เช่นกัน, เพื่อให้ คุณ เรียนรู้ วิธีใช้ และทำความเข้าใจ เกมก่อน ลงเดิมพัน
สล็อต PG มี คุณสมบัติที่ดี มากก ที่ ส่งผล ให้ได้รับความสำคัญ ในปัจจุบันนี้, ช่วย ความ ความบันเทิง ให้กับเกมด้วย.
ทดสอบเล่นสล็อต PG ซื้อการหมุนฟรี
ในยุคปัจจุบัน การเล่นเกมสล็อตออนไลน์ได้รับความชื่นชอบอย่างมาก โดยเฉพาะอย่างยิ่งเกมสล็อตจากทีมงาน PG Slot ที่มีฟีเจอร์พิเศษมากมายให้ผู้เล่นได้รื่นรมย์ หนึ่งในฟีเจอร์ที่น่าสนใจและทำให้การเล่นเกมสนุกยิ่งขึ้นคือ “การซื้อฟรีสปิน” ซึ่งเป็นการเพิ่มโอกาสสำเร็จในการชนะและเพิ่มความตื่นเต้นในการเล่น
ซื้อฟรีสปินคืออะไร
การซื้อฟรีสปินคือการที่นักเล่นสามารถซื้อโอกาสในการหมุนวงล้อสล็อตโดยไม่ต้องรอให้เกิดไอคอนฟรีสปินบนวงล้อ ซึ่งเป็นการเพิ่มโอกาสสำเร็จในการได้รับรางวัลพิเศษพิเศษต่างๆ ภายในเกม เช่น โบนัสพิเศษ แจ็คพอต และอื่นๆ อีกทั้ง การซื้อฟรีสปินยังช่วยให้ผู้เล่นสามารถเพิ่มยอดเงินรางวัลได้อย่างรวดเร็วและมีประสิทธิผล
ข้อดีของการสำรวจเล่นสล็อต PG ซื้อหมุนฟรี
เพิ่มโอกาสชนะ: การซื้อตัวเลือกฟรีสปินช่วยให้นักพนันมีโอกาสสำเร็จในการได้รับรางวัลพิเศษมากขึ้น เนื่องด้วยมีการหมุนวงล้อฟรีเพิ่มเติม ซึ่งอาจนำไปให้การได้รับแจ็คพอตหรือรางวัลโบนัสที่สูงขึ้นอื่นๆ
ลดเวลาในการเล่น: การซื้อฟรีสปินช่วยประหยัดเวลาในการเล่นในการเล่น จากที่ไม่ต้องรอให้เกิดสัญลักษณ์ฟรีสปินบนวงล้อ ผู้เล่นสามารถเข้าสู่โหมดฟรีสปินได้ทันที
ลองหมุนฟรี: สำหรับผู้เล่นที่ยังไม่แน่ใจเกี่ยวกับเกม PG Slot ยังมีโหมดทดลองเล่นฟรีผู้เล่นได้ทดสอบเล่นและศึกษาวิธีการเล่นก่อนที่จะตกลงใจซื้อฟรีสปินด้วยเงินจริง
เพิ่มความบันเทิง: การซื้อตัวเลือกหมุนฟรีช่วยเพิ่มความรื่นรมย์ในการเล่น จากที่นักเล่นสามารถเข้าสู่ขั้นตอนโบนัสและลักษณะพิเศษพิเศษอื่นๆ ได้อย่างไม่ยาก
วิธีการทำการซื้อฟรีสปินในสล็อต PG
เลือกเกมที่ต้องการหมุนจากบริษัท PG Slot
คลิกที่ปุ่ม “ซื้อฟรีสปิน” ที่แสดงบนจอเกม
ใส่จำนวนฟรีสปินที่ต้องการใช้และยืนยันคำสั่ง
เริ่มต้นการหมุนวงล้อและสนุกไปกับการเล่น
ผลสรุป
การทดสอบเล่นสล็อต PGและการซื้อฟรีสปินเป็นวิธีที่ดีเยี่ยมในการเพิ่มช่องทางในการชนะและเพิ่มความรื่นรมย์ในการเล่น ด้วยคุณสมบัติพิเศษนี้ ผู้เล่นสามารถเข้าสู่รอบโบนัสและคุณสมบัติพิเศษต่างๆ ได้อย่างเร็วและมีประสิทธิภาพสูง ไม่ว่าจะเป็นผู้เล่นใหม่หรือผู้เล่นที่มีความชำนาญ การทดสอบเล่นสล็อต PGและการซื้อตัวเลือกฟรีสปินจะช่วยให้คุณมีประสบการณ์การหมุนที่น่าตื่นเต้นใจและสนุกสนานมากยิ่งขึ้น
สำรวจเล่นสล็อต PG ซื้อการหมุนฟรี แล้วคุณจะพบกับความรื่นรมย์และความเป็นไปได้ในการชนะที่ไม่มีที่สิ้นสุด
ทดลองเล่นสล็อต pg ฟรี
สล็อตตรงจากเว็บ — ใช้ได้กับ มือถือ แท็บเล็ต คอมพิวเตอร์ส่วนตัว ฯลฯ สำหรับการเล่น
ระบบสล็อตตรงจากเว็บ ของ PG Slot ได้รับการพัฒนาและปรับแต่ง เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ มือถือ แท็บเล็ต หรือ คอมฯ รุ่นใด
ที่ PG Slot เราเข้าใจถึงสิ่งที่ผู้เล่นต้องการ ของลูกค้า ในเรื่อง ความสะดวก และ ความรวดเร็วในการเข้าถึงเกมคาสิโนออนไลน์ เราจึง นำ HTML 5 มาใช้ ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ปัจจุบันนี้ มาใช้พัฒนาเว็บไซต์ คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเว็บเบราว์เซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บของเรา คุณสามารถ เพลิดเพลินกับสล็อตแมชชีนได้ทันที
การสนับสนุนหลายอุปกรณ์
ไม่ว่าคุณจะใช้ สมาร์ทโฟน ระบบ แอนดรอยด์ หรือ iOS ก็สามารถ เล่นเกมสล็อตได้อย่างไม่มีปัญหา ระบบของเรา ออกแบบมาให้รองรับ ระบบปฏิบัติการทั้งหมด ไม่สำคัญว่าคุณ มี มือถือ รุ่นใหม่หรือรุ่นเก่า หรือ แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา ในเรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot นั่นคือ คุณสามารถ เล่นได้ทุกที่ทุกเวลา ไม่ว่าจะ เป็นที่บ้าน ที่ออฟฟิศ หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง ห่วงเรื่องการดาวน์โหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
ทดลองเล่นสล็อตฟรี
เพื่อให้ ผู้เล่นที่ใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงิน การ ทดลองเล่นสล็อตแมชชีนฟรีนี้จะช่วยให้คุณเรียนรู้วิธีเล่นและเข้าใจเกมก่อนตัดสินใจเดิมพันด้วยเงินจริง
การบริการและความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานพร้อมบริการคุณตลอดเวลา นอกจากนี้เรายังมี ระบบรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนบุคคลและธุรกรรมทางการเงินของคุณจะได้รับการปกป้องอย่างดีที่สุด
โปรโมชันและโบนัส
ข้อดีอีกประการของการเล่นสล็อตแมชชีนกับ PG Slot ก็คือ มี โปรโมชันและโบนัสพิเศษสำหรับสมาชิก ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสในการชนะและเพิ่มความเพลิดเพลินในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ประสบการณ์การทดลองเล่นสล็อต PG บนเว็บพนันตรง: เข้าสู่โลกแห่งความตื่นเต้นที่ไม่มีข้อจำกัด
ในกรณีของนักเดิมพันที่แสวงหาการทดลองเกมที่ไม่เหมือนใคร และต้องการหาแหล่งเสี่ยงโชคที่เชื่อถือได้, การทดลองเกมสล็อต PG บนเว็บตรงนับว่าเป็นตัวเลือกที่น่าทึ่งอย่างมาก. เพราะมีความหลายหลากของเกมสล็อตแมชชีนที่มีให้เลือกเล่นมากมาย, ผู้เล่นจะได้เผชิญกับโลกแห่งความตื่นเต้นเร้าใจและความสนุกเพลิดเพลินที่ไม่มีข้อจำกัด.
เว็บพนันตรงนี้ จัดหาการทดลองเล่นเกมการเล่นที่มั่นคง เชื่อถือได้ และตรงตามความต้องการของนักเสี่ยงโชคได้เป็นอย่างดี. ไม่ว่าผู้เล่นจะคุณจะติดใจเกมสล็อตต่างๆแนวคลาสสิกที่เป็นที่รู้จัก หรืออยากประสบการณ์เกมที่ไม่เหมือนใครที่มีฟีเจอร์พิเศษเฉพาะและสิทธิพิเศษล้นหลาม, เว็บไซต์โดยตรงนี้ก็มีให้เลือกเล่นอย่างหลากหลายชนิด.
เพราะมีระบบการลองเกมสล็อต PG โดยไม่เสียค่าใช้จ่าย, ผู้เล่นจะได้จังหวะทำความเข้าใจขั้นตอนเล่นและทดลองวิธีการต่างๆ ก่อนที่จะเริ่มใช้เงินจริงด้วยเงินสด. โอกาสนี้ถือเป็นโอกาสอันยอดเยี่ยมที่จะเสริมความพร้อมและสร้างเสริมโอกาสในการชิงโบนัสใหญ่.
ไม่ว่าท่านจะผู้เล่นจะปรารถนาความสนุกสนานแบบคลาสสิก หรือการท้าทายแปลกใหม่, สล็อต PG บนเว็บเสี่ยงโชคไม่ผ่านเอเย่นต์ก็มีให้คัดสรรอย่างหลากหลายมากมาย. คุณอาจจะได้เผชิญกับการทดลองเล่นการเล่นเกมที่น่าตื่นเต้น น่ารื่นเริง และเพลิดเพลินไปกับโอกาสดีในการได้รับรางวัลใหญ่มหาศาล.
อย่าช้า, ร่วมเล่นสำรวจสล็อตแมชชีน PG บนเว็บไซต์พนันตรงเวลานี้ และค้นพบโลกแห่งความบันเทิงแห่งความบันเทิงที่น่าเชื่อถือ น่าค้นหา และพร้อมเต็มไปด้วยความเพลิดเพลินรอคอยคุณ. เผชิญความตื่นเต้น, ความสุข และโอกาสดีในการคว้าโบนัสมหาศาล. เริ่มเล่นเดินไปสู่ชัยชนะในวงการเกมออนไลน์วันนี้!
ทดลองเล่นสล็อต pg ไม่ เด้ง
ทดลองทดสอบเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังต้องการความบันเทิงและโอกาสในการชนะรางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งทางเลือกที่ที่คุ้มค่าใคร่ครวญ.ด้วยความจำนวนมากของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถทดสอบและค้นหาเกมที่เหมาะกับตัวเองได้อย่างง่ายดาย.
ไม่ว่าคุณจะชื่นชอบเกมสล็อตคลาสสิกหรือต้องการความแปลกใหม่, ตัวเลือกรอต้อนรับให้คุณสัมผัส. จากสล็อตที่มีหัวข้อมากมาย ไปจนถึงเกมที่มีรูปแบบพิเศษและรางวัลมากมาย, ผู้เล่นจะได้พบกับประสบการณ์ที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการทดลองเล่นสล็อตฟรี, คุณสามารถทำความคุ้นเคยวิธีการเล่นและค้นตัดสินใจกลยุทธ์ที่ตรงใจก่อนวางเดิมพันด้วยเงินจริง. นี่คือโอกาสที่จะเรียนรู้กับเกมและประยุกต์โอกาสในการชนะรางวัลใหญ่.
อย่าขยายเวลา, ลงมือกับการลองเล่นสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินความสนใจ, ความสนุกสนาน และโอกาสในการชนะรางวัลมหาศาล. ก้าวสู่ความสำเร็จเดินทางสู่ความสมหวังของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
บาคาร่า
פוקר באינטרנט
הימורי ספורט – הימור באינטרנט
הימורי ספורט נעשו לאחד התחומים הצומחים ביותר בהימורים באינטרנט. משתתפים מסוגלים להמר על תוצאות של אירועי ספורטיביים פופולריים כמו כדורגל, כדורסל, טניס ועוד. האופציות להתערבות הן מרובות, כולל תוצאת המשחק, מספר השערים, כמות הפעמים ועוד. להלן דוגמאות של למשחקי נפוצים במיוחד עליהם אפשרי להתערב:
כדור רגל: ליגת אלופות, מונדיאל, ליגות מקומיות
כדורסל: ליגת NBA, ליגת יורוליג, טורנירים בינלאומיים
משחק הטניס: ווימבלדון, US Open, רולאן גארוס
פוקר ברשת ברשת – הימורים באינטרנט
משחק הפוקר באינטרנט הוא אחד ממשחקי ההימורים המוכרים ביותר כיום. משתתפים יכולים להתחרות נגד מתחרים מרחבי העולם במגוון גרסאות של המשחק , כגון Texas Hold’em, Omaha, סטאד ועוד. אפשר לגלות תחרויות ומשחקי במבחר רמות ואפשרויות מגוונות. אתרי פוקר המובילים מציעים גם:
מגוון רחב של גרסאות המשחק פוקר
טורנירים שבועיים וחודשיות עם פרסים כספיים גבוהים
שולחנות המשחק למשחק מהיר ולטווח ארוך
תוכניות נאמנות ללקוחות ומועדוני עם הטבות עם הטבות
בטיחות ואבטחה והגינות
כאשר הבחירה בפלטפורמה להימורים באינטרנט, חיוני לבחור גם אתרים מורשים ומפוקחים המציעים גם סביבה משחק מאובטחת והוגנת. אתרים אלו משתמשים בטכנולוגיות הצפנה מתקדמות להבטחה על נתונים אישיים ופיננסיים, וכן בתוכנות מחולל מספרים אקראיים (RNG) כדי להבטיח הגינות במשחקי ההימורים.
מעבר לכך, הכרחי לשחק באופן אחראי תוך הגדרת מגבלות אישיות הימור אישיות. רוב האתרים מאפשרים לשחקנים להגדיר מגבלות להפסדים ופעילויות, כמו גם להשתמש ב- כלים למניעת התמכרות. הימרו בתבונה ואל תרדפו גם אחר הפסדים.
המדריך המלא לקזינו אונליין, הימורי ספורט ופוקר באינטרנט באינטרנט
ההימורים ברשת מציעים עולם שלם של הזדמנויות מלהיבות למשתתפים, החל מקזינו באינטרנט וגם משחקי ספורט ופוקר באינטרנט. בזמן הבחירה בפלטפורמת הימורים, הקפידו לבחור אתרי הימורים המפוקחים המציעים סביבת משחק בטוחה והוגנת. זכרו גם לשחק בצורה אחראית תמיד ואחראי – ההימורים באינטרנט נועדו להיות מבדרים ומהנים ולא לגרום לבעיות כלכליות או גם חברתיים.
קזינו אונליין
הימורי ספורט – הימורים באינטרנט
הימור ספורטיביים נעשו לאחד הענפים המתפתחים ביותר בהימור ברשת. שחקנים מסוגלים להמר על תוצאותיהם של אירועי ספורטיביים פופולריים כמו כדורגל, כדורסל, משחק הטניס ועוד. האופציות להתערבות הן מרובות, וביניהן תוצאתו המשחק, כמות הגולים, מספר הפעמים ועוד. הבא דוגמאות למשחקים נפוצים שעליהם אפשרי להתערב:
כדור רגל: ליגת אלופות, גביע העולם, ליגות אזוריות
כדורסל: ליגת NBA, יורוליג, טורנירים בינלאומיים
טניס: טורניר ווימבלדון, US Open, אליפות צרפת הפתוחה
פוקר ברשת ברשת – הימורים באינטרנט
פוקר באינטרנט הוא אחד מהמשחקים ההימורים המוכרים ביותר בימינו. משתתפים מסוגלים להתמודד מול יריבים מכל רחבי תבל בסוגי וריאציות של המשחק , כגון Texas Hold’em, Omaha, סטאד ועוד. ניתן למצוא טורנירים ומשחקי במבחר רמות ואפשרויות מגוונות. אתרי פוקר המובילים מציעים גם:
מבחר רב של גרסאות פוקר
טורנירים שבועיות וחודשיים עם פרסים כספיים
שולחנות למשחקים מהירים ולטווח הארוך
תוכניות נאמנות ומועדוני עם הטבות יחודיות
בטיחות והגינות
בעת בוחרים בפלטפורמה להימורים באינטרנט, חיוני לבחור אתרים מורשים ומפוקחים המציעים גם סביבת משחק בטוחה והוגנת. אתרים אלה משתמשים בטכנולוגיות אבטחה מתקדמות להבטחה על נתונים אישיים ופיננסיים, וכן באמצעות תוכנות מחולל מספרים אקראיים (RNG) כדי לוודא הגינות המשחקים במשחקי ההימורים.
מעבר לכך, הכרחי לשחק בצורה אחראית תוך כדי קביעת מגבלות אישיות הימורים אישיות של השחקן. מרבית האתרים מאפשרים למשתתפים להגדיר מגבלות הפסד ופעילות, כמו גם לנצל כלים נגד התמכרויות. הימרו בתבונה ואל תרדפו אחרי הפסד.
המדריך השלם למשחקי קזינו ברשת, משחקי ספורט ופוקר באינטרנט באינטרנט
ההימורים באינטרנט מציעים גם עולם שלם של של הזדמנויות מלהיבות למשתתפים, מתחיל מקזינו אונליין וכל משחקי ספורט ופוקר באינטרנט. בזמן בחירת פלטפורמת הימורים, חשוב לבחור אתרי הימורים המפוקחים המציעים סביבה למשחק בטוחה והוגנת. זכרו לשחק בצורה אחראית תמיד ואחראי – משחקי ההימורים באינטרנט אמורים להיות מבדרים ומהנים ולא לגרום לבעיות פיננסיות או גם חברתיות.
הימורי ספורט – הימורים באינטרנט
הימור ספורטיביים הפכו לאחד התחומים המתפתחים ביותר בהימור ברשת. שחקנים מסוגלים להמר על תוצאותיהם של אירועים ספורט פופולריים כמו כדורגל, כדור סל, משחק הטניס ועוד. האפשרויות להתערבות הן רבות, וביניהן תוצאת המאבק, כמות הגולים, מספר הנקודות ועוד. להלן דוגמאות למשחקים נפוצים במיוחד עליהם אפשרי להתערב:
כדור רגל: ליגת אלופות, גביע העולם, ליגות מקומיות
כדורסל: NBA, יורוליג, תחרויות בינלאומיות
טניס: טורניר ווימבלדון, אליפות ארה”ב הפתוחה, אליפות צרפת הפתוחה
פוקר ברשת באינטרנט – הימורים ברשת
משחק הפוקר ברשת הוא אחד ממשחקי ההימור הנפוצים ביותר כיום. שחקנים מסוגלים להתמודד מול יריבים מרחבי העולם במגוון סוגי של המשחק , כגון Texas Hold’em, Omaha, סטאד ועוד. ניתן לגלות תחרויות ומשחקי קש במגוון דרגות ואפשרויות הימור שונות. אתרי הפוקר המובילים מציעים גם:
מגוון רחב של וריאציות פוקר
תחרויות שבועיים וחודשיות עם פרסים כספיים
שולחנות למשחקים מהירים ולטווח ארוך
תוכניות נאמנות ומועדוני עם הטבות עם הטבות
בטיחות והוגנות
בעת הבחירה בפלטפורמה להימורים, חשוב לבחור גם אתרי הימורים מורשים ומפוקחים המציעים גם סביבת משחק בטוחה והוגנת. אתרים אלו עושים שימוש בטכנולוגיית אבטחה מתקדמת להגנה על מידע אישי ופיננסיים, וגם בתוכנות גנרטור מספרים אקראיים (RNG) כדי להבטיח הגינות במשחקים.
בנוסף, הכרחי לשחק גם בצורה אחראית תוך כדי הגדרת מגבלות הימור אישיות. מרבית אתרי ההימורים מאפשרים גם לשחקנים להגדיר מגבלות הפסד ופעילויות, כמו גם להשתמש ב- כלים למניעת התמכרות. שחקו בתבונה ואל גם תרדפו אחרי הפסד.
המדריך המלא לקזינו באינטרנט, הימורי ספורט ופוקר באינטרנט
ההימורים ברשת מציעים עולם שלם הזדמנויות מלהיבות לשחקנים, מתחיל מקזינו אונליין וכל משחקי ספורט ופוקר באינטרנט. בעת בחירת פלטפורמת הימורים, הקפידו לבחור אתרי הימורים המפוקחים המציעים גם סביבה למשחק מאובטחת והגיונית. זכרו גם לשחק תמיד בצורה אחראית תמיד – משחקי ההימורים ברשת אמורים להיות מבדרים ומהנים ולא גם לגרום לבעיות כלכליות או חברתיים.
mega338
Игровые автоматы егт
https://uzfootball.ru/igrovie-avtomati/igrovie-avtomati-egt-1.html
הימורי ספורט – הימור באינטרנט
הימור ספורטיביים נהיו לאחד הענפים המתפתחים ביותר בהימורים ברשת. משתתפים מסוגלים להתערב על תוצאות של אירועים ספורטיביים מוכרים למשל כדורגל, כדור סל, טניס ועוד. האופציות להימור הן מרובות, וביניהן תוצאתו ההתמודדות, כמות הגולים, כמות הנקודות ועוד. הבא דוגמאות של למשחקים נפוצים במיוחד עליהם אפשרי להתערב:
כדור רגל: ליגת האלופות, מונדיאל, ליגות מקומיות
כדורסל: ליגת NBA, יורוליג, טורנירים בינלאומיים
טניס: ווימבלדון, US Open, אליפות צרפת הפתוחה
פוקר באינטרנט – הימור באינטרנט
משחק הפוקר ברשת הוא אחד ממשחקי ההימורים הפופולריים ביותר כיום. משתתפים מסוגלים להתחרות נגד יריבים מכל רחבי העולם במגוון וריאציות משחק , לדוגמה Texas Hold’em, Omaha, Stud ועוד. אפשר לגלות תחרויות ומשחקי במגוון רמות ואפשרויות הימור מגוונות. אתרי הפוקר הטובים מציעים גם:
מגוון רחב של וריאציות פוקר
תחרויות שבועיים וחודשיים עם פרסים כספיים גבוהים
שולחנות למשחק מהיר ולטווח הארוך
תוכניות נאמנות ומועדוני VIP עם הטבות בלעדיות
בטיחות והוגנות
כאשר הבחירה בפלטפורמה להימורים, חיוני לבחור אתרים מורשים המפוקחים המציעים גם סביבה למשחק בטוחה והוגנת. אתרים אלה משתמשים בטכנולוגיות אבטחה מתקדמת להגנה על מידע אישי ופיננסיים, וגם באמצעות תוכנות מחולל מספרים רנדומליים (RNG) כדי להבטיח הגינות המשחקים במשחקי ההימורים.
מעבר לכך, הכרחי לשחק גם באופן אחראית תוך כדי קביעת מגבלות אישיות הימור אישיות. רוב אתרי ההימורים מאפשרים גם לשחקנים להגדיר מגבלות להפסדים ופעילות, וגם להשתמש ב- כלים נגד התמכרויות. הימרו בחכמה ואל תרדפו גם אחר הפסדים.
המדריך השלם לקזינו ברשת, הימורי ספורט ופוקר ברשת
הימורים באינטרנט מציעים עולם שלם הזדמנויות מרתקות לשחקנים, מתחיל מקזינו אונליין וגם בהימורי ספורט ופוקר ברשת. בזמן בחירת פלטפורמת הימורים, הקפידו לבחור אתרי הימורים המפוקחים המציעים סביבה למשחק מאובטחת והוגנת. זכרו גם לשחק תמיד באופן אחראי תמיד ואחראי – משחקי ההימורים ברשת נועדו להיות מבדרים ולא גם לגרום לבעיות פיננסיות או גם חברתיות.
Casino
https://uzfootball.ru/map1.html
Hi just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading properly. I’m not sure why but I think its a linking issue. I’ve tried it in two different browsers and both show the same outcome.
forum.meha.biz/topic/1071/
kungur.hldns.ru/forum/search.php?action=members&p=188&s=d&order=ASC%C3%82%C2%A0
dip-vuz.ru/kupit-diplom-v-tyumeni/index.html
marsaxlokkfc.com/200405/friendlies20042005.html
tuning-performance.ru/polirovka-kuzova-avtomobilya/
Hi there mates, how is everything, and what you wish for to say concerning this post, in my view its really amazing in favor of me.
frpworld.com/modules.php?name=Your_Account&op=userinfo&username=titovaong3
online-vuz.ru/viewNews/177/
lgg3-dongiantaodangcap.com.vn/sam-sung/
mesannuaires.fr/art-et-culture/mode-s286.html
http://www.tvserver.ru/forum/viewtopic.php?t=1271&view=previous
https://medium.com/@momejar21741/pg-59490dd058fd
สล็อตเว็บโดยตรง — ใช้ได้กับ สมาร์ทโฟน แท็บเลต คอมฯ ฯลฯ ในการเล่น
ระบบสล็อตเว็บตรง ของ PG ได้รับการพัฒนาและอัปเดต เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง สมบูรณ์ ไม่สำคัญว่าจะใช้ โทรศัพท์มือถือ แท็บเล็ต หรือ คอมพิวเตอร์ แบบไหน
ที่ พีจีสล็อต เราเข้าใจว่าผู้เล่นต้องการ ของผู้เล่น ในเรื่อง ความสะดวกสบาย และ ความรวดเร็วในการเข้าถึงเกมคาสิโนออนไลน์ เราจึง ใช้เทคโนโลยี HTML 5 ซึ่งเป็น เทคโนโลยีที่ล้ำสมัย ในขณะนี้ มาพัฒนาเว็บไซต์ของเรากันเถอะ คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเบราว์เซอร์ บนอุปกรณ์ที่ คุณมีอยู่ และเยี่ยมชม เว็บไซต์เรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การใช้งานกับอุปกรณ์หลากหลาย
ไม่ว่าคุณจะใช้ มือถือ ระบบ Android หรือ iOS ก็สามารถ เล่นสล็อตออนไลน์ได้ไม่มีสะดุด ระบบของเรา ออกแบบมาเพื่อรองรับ ระบบปฏิบัติการทั้งหมด ไม่สำคัญว่าคุณ ใช้ สมาร์ทโฟน รุ่นใหม่หรือรุ่นเก่า หรือ แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา เรื่องความเข้ากันได้
เล่นได้ทุกที่ทุกเวลา
ข้อดีของการเล่น PG Slot ก็คือ คุณสามารถ เล่นได้ทุกที่ทุกเวลา ไม่ว่าจะ เป็นที่บ้าน ที่ทำงาน หรือแม้แต่ สถานที่สาธารณะ สิ่งที่คุณต้องมีคือ อินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง ห่วงเรื่องการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่บนอุปกรณ์ของคุณ
เล่นสล็อตฟรี
เพื่อให้ ผู้เล่นใหม่ มีโอกาสลองและสัมผัสประสบการณ์สล็อตแมชชีนของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงิน การ เล่นฟรีนี้จะช่วยให้คุณเข้าใจวิธีเล่นและรู้จักเกมก่อนลงเดิมพันจริง
การให้บริการและความปลอดภัย
PG Slot มุ่งมั่นในการบริการลูกค้าที่ดีที่สุด เรามี ทีมงานพร้อมบริการคุณตลอดเวลา นอกจากนี้เรายังมี ระบบรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนบุคคลและธุรกรรมทางการเงินของคุณจะได้รับการปกป้องอย่างดีที่สุด
โปรโมชั่นและโบนัสพิเศษ
อีกข้อดีของการเล่นสล็อตกับ PG Slot คือ มี โปรโมชั่นและโบนัสพิเศษมากมายสำหรับผู้เข้าร่วม ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชันและโบนัสได้ สิ่งนี้จะ เพิ่มโอกาสชนะและสนุกกับเกมมากขึ้น
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
купить диплом в нижневартовске купить диплом в нижневартовске .
10 pounds no deposit bonus
https://uzfootball.ru
Hey very nice site!! Man .. Excellent .. Superb .. I will bookmark your website and take the feeds also? I am happy to find a lot of useful information right here in the put up, we need develop extra strategies in this regard, thank you for sharing. . . . . .
forum.meha.biz/topic/1071/
ufawedding.ru/forum/index.php?action=reminder
http://www.topfoto.ru/index.php?links_exchange=yes&page=36&show_all=yes
diaocbinhduong.org/2018/phuc-dat-connect-214901pr.html
glonet.com/blog/22823/%D0%B8%D0%B7%D0%B1%D0%B0%D0%B2%D1%8C%D1%82%D0%B5%D1%81%D1%8C-%D0%BE%D1%82-%D1%81%D0%BB%D0%BE%D0%B6%D0%BD%D0%BE%D1%81%D1%82%D0%B5%D0%B9-%D1%81-%D1%83%D1%87%D0%B5%D0%B1%D0%BE%D0%B9-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D0%B5-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC/
pg
ทดลองเล่นสล็อต pg ฟรี
Hi, after reading this awesome piece of writing i am too glad to share my knowledge here with friends.
http://www.sinoright.net/member/index.php?uid=yrukoc
la-buket.ru/catalog/?ELEMENT_ID=50&SECTION_ID=2
eku.ru/comments/list/
balipraia.com/category/competition/
karabash.chelbusiness.ru/index.php?name=account&op=info&uname=unypavaze
купить диплом в братске diplomvash.ru .
If you would like to obtain a good deal from this post then you have to apply such methods to your won website.
Attractive section of content. I just stumbled upon your site and in accession capital to assert that I get actually enjoyed account your blog posts. Anyway I will be subscribing to your feeds and even I achievement you access consistently quickly.
http://www.voidofheroes.com/forums/member.php?action=profile&uid=53955
veintitantos.com/amor-otros/cortaron-no-arruines-tu-vida
otantravel.kz/news/swiss-uvelichivaet-kolichestvo-reysov-mayyami-cyurih-na-period-zimnego-sezona
thepokiesgames.com/terms
forum.zub-zub.ru/viewtopic.php?t=25938
Just want to say your article is as astounding. The clearness for your post is simply cool and i can assume you’re knowledgeable on this subject. Fine together with your permission allow me to grab your RSS feed to stay up to date with imminent post. Thanks one million and please continue the enjoyable work.
188.17.148.172/forum/profile.php?action=show&member=7512
calltraxplus.com/call-tracking-software
cekresipos.com/index.php?mod=kontak
wiuwi.com/blogs/70298/%D0%93%D0%B4%D0%B5-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D1%81%D0%B0%D0%BC%D1%8B%D0%B5-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B5-%D0%BF%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D1%89%D0%B8%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2
topstavka.ru/action?page=2
Thank you for another excellent article. The place else could anyone get that type of information in such an ideal manner of writing? I’ve a presentation next week, and I am on the look for such info.
nipponsword.ru/profile.php?lookup=23413
http://www.ijwiryacu.com/read?article=hzlnmuhjlvuvbnbh
weekevents.ru/page/40
cs-online.ru/forum/index.php?showtopic=13633&mode=linear
click2connect.buzz/index.php?do=/public/user/blogs/name_Alanpoe/page_5/
BetPlay Casino stands out with its diverse game library, featuring slots, table
games, poker, and live dealers, attractive to a broad audience.
娛樂城
台灣線上娛樂城是指通過互聯網提供賭博和娛樂服務的平台。這些平台主要針對台灣用戶,但實際上可能在境外運營。以下是一些關於台灣線上娛樂城的重要信息:
1. 服務內容:
– 線上賭場遊戲(如老虎機、撲克、輪盤等)
– 體育博彩
– 彩票遊戲
– 真人荷官遊戲
2. 特點:
– 全天候24小時提供服務
– 可通過電腦或移動設備訪問
– 常提供優惠活動和獎金來吸引玩家
3. 支付方式:
– 常見支付方式包括銀行轉賬、電子錢包等
– 部分平台可能接受加密貨幣
4. 法律狀況:
– 在台灣,線上賭博通常是非法的
– 許多線上娛樂城實際上是在國外註冊運營
5. 風險:
– 由於缺乏有效監管,玩家可能面臨財務風險
– 存在詐騙和不公平遊戲的可能性
– 可能導致賭博成癮問題
6. 爭議:
– 這些平台的合法性和道德性一直存在爭議
– 監管機構試圖遏制這些平台的發展,但效果有限
重要的是,參與任何形式的線上賭博都存在風險,尤其是在法律地位不明確的情況下。建議公眾謹慎對待,並了解相關法律和潛在風險。
如果您想了解更多具體方面,例如如何識別和避免相關風險,我可以提供更多信息。
Casino
https://uzfootball.ru/map1.html
Nice post.Very useful info specifically the last part 🙂 Thank you and good luck.
Very Interesting Information! Thank You For Thi Information!
промокоды cat casino
промокоды cat casino
Коммерческий секс в Москве представляет собой сложной и разнообразной вопросом. Несмотря на то, что она запрещается законом, эта деятельность существует как значительным нелегальной областью.
Контекст в прошлом
В советского времени периоды коммерческий секс существовала в тени. По окончании СССР, в условиях рыночной нестабильной ситуации, проституция стала очевидной.
Современная состояние
В настоящее время коммерческий секс в столице включает различные формы, начиная с высококлассных эскорт-сервисов до самой уличной интимных услуг. Престижные услуги обычно организуются через в сети, а улицы проституция сконцентрирована в специфических районах городской территории.
Социальные и Экономические Аспекты
Многие женщин приходят в эту сферу вследствие экономических проблем. Коммерческий секс может являться заманчивой из-за перспективы быстрого дохода, но она подразумевает риски для здоровья и жизни.
Правовые Вопросы
Проституция в стране не законна, и за ее организацию занятие установлены серьезные штрафы. Секс-работниц регулярно привлекают к к дисциплинарной наказанию.
Поэтому, игнорируя запреты, интимные услуги существует как аспектом теневой экономики Москвы с большими социальными и юридическими последствиями.
In modern times, Africa has appeared as a radiant hub for tunes and celebrity traditions, gaining international identification and influencing global trends. African music, having its rich tapestry of genres like as Afrobeats, Amapiano, and highlife, has captivated audiences around the world. Major artists such as Burna Boy, Wizkid, and Tiwa Fierce, ferocious have not just dominated the chart in Africa but have also made substantial inroads into the particular global music landscape. Their collaborations along with international stars and performances at key music festivals include highlighted the continent’s musical prowess. Typically the rise of digital platforms and sociable media has further more amplified the access of African music, allowing artists in order to connect with fans across the globe and share their particular sounds and reports – https://afriquestories.com/les-10-meilleures-pistes-afrobeats-de-lannee-2022/.
In addition in order to its musical expertise, Africa’s celebrity culture is flourishing, along with entertainers, influencers, plus public figures ordering large followings. Superstars such as Lupita Nyong’o, Trevor Noah, and Charlize Theron, who have origins in Africa, are usually making waves worldwide in film, tv set, and fashion. These figures not just bring attention to their work but furthermore reveal important sociable issues and ethnical heritage. Their accomplishment stories inspire a new generation associated with Africans to go after careers in the entertainment industry, fostering a feeling of pride and ambition across the particular continent.
Moreover, African-american celebrities are progressively using their programs to advocate for change and give back to their neighborhoods. From Burna Boy’s activism around cultural justice issues to Tiwa Savage’s work in promoting education intended for girls, these public figures are profiting their influence for positive impact. They are involved in numerous philanthropic activities, assisting causes such as healthcare, education, and even environmental sustainability. This specific trend highlights typically the evolving role associated with celebrities in The african continent, who are not merely entertainers but also key players inside driving social change and development.
Overall, the landscape of music and movie star culture in Photography equipment is dynamic in addition to ever-evolving. The continent’s rich cultural range and creative ability still garner global acclaim, positioning The african continent like a major power inside the global enjoyment industry. As African artists and celebs continue to break limitations and achieve innovative heights, they front the way for some sort of more inclusive plus diverse representation inside global media. Regarding those interested in staying updated upon the latest tendencies and news inside this vibrant scene, numerous platforms and publications offer in-depth coverage of Africa’s music and superstar happenings, celebrating the particular continent’s ongoing input to the entire world stage.
娛樂城首儲
онлайн казино с депозитом
https://remvend-cafe.ru/igrat-onlayn/igrat-avtomati-besplatno-v-onlayne-igrat-besplatno.html
https://win-line.net/טורניר-פוקר-טורנירים/
לבצע, אסמכתא לדבריך.
הקזינו באינטרנט הפכה לתעשייה מבוקש מאוד בעשור האחרון, המספק מבחר רחב של חלופות פעילות, כמו הימורי ספורט.
בניתוח זה נבדוק את תעשיית ההתמודדות המקוונת ונספק לכם נתונים חשובים שיתרום לכם לנתח בנושא מסקרן זה.
הימורי ספורט – קזינו באינטרנט
קזינו אונליין מאפשר אלטרנטיבות רבות של אירועים מסורתיים כגון רולטה. ההימורים באינטרנט מעניקים לשחקנים ליהנות מאווירת התמודדות אמיתית מכל מקום ובכל זמן.
המשחקים סיכום קצר
מכונות פירות משחקי מזל
הימורי רולטה הימור על פרמטרים על גלגל הרולטה
משחק קלפים 21 משחק קלפים בו המטרה היא להשיג 21
פוקר משחק קלפים מבוסס אסטרטגיה
משחק הבאקרה משחק קלפים קל וזריז
הימורים בתחום הספורט – פעילות באינטרנט
הימורים על אירועי ספורט מייצגים אחד הסגמנטים הצומחים הגדולים ביותר בקזינו באינטרנט. משתתפים מורשים להמר על תוצאות של אירועי ספורט פופולריים כגון כדורסל.
התמודדויות מתאפשרות על תוצאת המשחק, מספר הנקודות ועוד.
המשחק פירוט תחרויות ספורט מקובלות
ניחוש הביצועים ניחוש התוצאה הסופית של המשחק כדורגל, כדורסל, טניס
הפרש סקורים ניחוש ההפרש בסקורים בין הקבוצות כל ענפי הספורט
מספר שערים/נקודות ניחוש כמה שערים או נקודות יהיו במשחק כדורגל, כדורסל, הוקי קרח
הקבוצה המנצחת ניחוש מי יזכה בתחרות (ללא קשר לביצועים) מספר ענפי ספורט
התמרמרות בזמן אמת הימורים במהלך המשחק בזמן אמת כדורגל, טניס, קריקט
פעילות מעורבת שילוב של מספר סוגי התמרמרות מרבית ענפי הספורט
פוקר אונליין – קזינו באינטרנט
פעילות פוקר מקוונת הוא אחד מענפי התמודדות המרכזיים הגדולים ביותר בשנים האחרונות. משתתפים רשאים להשתתף כנגד משתתפים אחרים מרחבי הגלובליזציה במגוון
https://t.me/promokod_PokerDom_casino
purple pharmacy mexico price list
https://cmqpharma.com/# buying prescription drugs in mexico online
buying prescription drugs in mexico online
https://win-line.net/הימורים-ביורו/
להגיש, אסמכתא לדבריך.
פעילות ההימורים באינטרנט הפכה לתעשייה פופולרי מאוד בעת האחרונה, המכיל מבחר רחב של חלופות פעילות, כגון משחקי פוקר.
במאמר זה נבחן את עולם ההתמודדות המקוונת ונעניק לכם מידע חשוב שיסייע לכם להתמצא בתופעה מסקרן זה.
הימורי ספורט – קזינו באינטרנט
משחקי פוקר מאפשר אלטרנטיבות רבות של משחקים ידועים כגון פוקר. ההתמודדות באינטרנט מספקים למבקרים לחוות מאווירת משחק אותנטית בכל עת ומקום.
הפעילות תיאור מקוצר
מכונות מזל הימורים עם גלגלים
הימורי רולטה הימור על תוצאות על גלגל מסתובב
משחק קלפים להגעה ל-21 משחק קלפים בו המטרה להגיע לסכום של 21
התמודדות בפוקר התמודדות אסטרטגית בקלפים
התמודדות בבאקרה משחק קלפים קל וזריז
הימורי ספורט – קזינו באינטרנט
הימורי ספורט מהווים חלק מ אחד הסגמנטים המשגשגים ביותר בהתמודדות באינטרנט. מבקרים רשאים להתמודד על תוצאות של משחקי ספורט פופולריים כגון ועוד.
התמודדויות ניתן לתמוך על תוצאת האירוע, מספר השערים ועוד.
סוג ההימור פירוט תחרויות ספורט מקובלות
ניחוש תוצאה ניחוש התוצאה הסופית של האירוע כדורגל, כדורסל, טניס
הפרש ביצועים ניחוש ההפרש בתוצאות בין הקבוצות כדורגל, כדורסל, אמריקאי
כמות הסקורים ניחוש כמות הסקורים בתחרות כדורגל, כדורסל, טניס
הקבוצה המנצחת ניחוש איזו קבוצה תנצח (ללא קשר לתוצאה) מרבית ענפי הספורט
הימורי חי הימורים במהלך האירוע בזמן אמת כדורגל, טניס, כדורסל
הימורים משולבים שילוב של מספר פעילויות מרבית ענפי הספורט
פעילות פוקר מקוונת – הימורים באינטרנט
התמודדות בפוקר מקוון מהווה אחד מסוגי הקזינו המובילים המובהקים ביותר בזמן האחרון. מתמודדים מסוגלים להשקיע מול יריבים מכל רחבי הכדור הארצי במגוון
Секс-работа в столице является проблемой как комплексной и многоаспектной трудностью. Хотя она запрещается правилами, это занятие является важным подпольным сектором.
Исторический
В Союзные годы проституция имела место в тени. С распадом СССР, в период экономической нестабильной ситуации, она появилась очевидной.
Нынешняя Ситуация
В настоящее время коммерческий секс в столице принимает многочисленные формы, вплоть до люксовых эскорт-услуг и заканчивая публичной секс-работы. Люксовые сервисы зачастую предоставляются через сеть, а уличная интимные услуги сосредоточена в выделенных районах города.
Общественно-экономические аспекты
Многие женщин вступают в этот бизнес ввиду финансовых трудностей. Коммерческий секс может оказаться привлекательным из-за перспективы быстрого заработка, но она подразумевает риски для здоровья и безопасности.
Правовые Вопросы
Коммерческий секс в Российской Федерации запрещена, и за её проведение предусмотрены серьезные штрафы. Секс-работниц регулярно задерживают к административной наказанию.
Таким образом, игнорируя запреты, секс-работа является элементом экономики в тени города с большими социальными и юридическими последствиями.
индивидуалки метро царицыно
pharmacies in mexico that ship to usa: medicine in mexico pharmacies – mexican drugstore online
Hello there! Do you know if they make any plugins to protect against hackers?
I’m kinda paranoid about losing everything I’ve worked hard on. Any tips?
онлайн казино с депозитом
https://remvend-cafe.ru/sloti-besplatno/wild-fortune-desktop-version.html
онлайн казино с депозитом
https://remvend-cafe.ru/avtomati-igrat-registratsii/kakie-bukmekeri-dayut-fribet-na-den-rozhdeniya.html
https://win-line.net/פוקר-אונליין-באינטרנט-על-כסף-אמיתי/
להעביר, תימוכין לדבריך.
ההמרה באינטרנט הפכה לענף פופולרי מאוד לאחרונה, המציע אפשרויות שונות של אלטרנטיבות התמודדות, לדוגמה קזינו אונליין.
בניתוח זה נבחן את תופעת הפעילות המקוונת ונייעץ לכם מידע חשוב שיסייע לכם לחקור בתופעה אטרקטיבי זה.
הימורי ספורט – קזינו באינטרנט
קזינו אונליין מציע אופציות שונות של אפשרויות קלאסיים כגון פוקר. ההתמודדות באינטרנט מספקים למתמודדים ליהנות מאווירת משחק מקצועית מכל מקום ובכל זמן.
סוג המשחק פירוט קצר
מכונות פירות משחקי מזל עם גלגלים
הימורי רולטה הימור על מספרים ואפשרויות על גלגל מסתובב בצורה עגולה
משחק קלפים להגעה ל-21 משחק קלפים להשגת ניקוד של 21
משחק קלפים פוקר התמודדות אסטרטגית בקלפים
משחק קלפים באקרה משחק קלפים קל וזריז
הימורים בתחום הספורט – התמודדות באינטרנט
הימורים בתחום הספורט הם אחד הסגמנטים המתפתחים המרכזיים ביותר בפעילות באינטרנט. שחקנים יכולים לסחור על ביצועים של משחקי ספורט מושכים כגון טניס.
התמודדויות מתאפשרות על הביצועים בתחרות, מספר העופרות ועוד.
סוג הפעילות תיאור תחומי ספורט מובילים
ניחוש הביצועים ניחוש התוצאה הסופית של המשחק כדורגל, כדורסל, הוקי
הפרש ביצועים ניחוש ההפרש בביצועים בין הקבוצות כדורגל, כדורסל, טניס
כמות הביצועים ניחוש כמות הסקורים בתחרות כדורגל, כדורסל, טניס
המנצח בתחרות ניחוש מי יסיים ראשון (ללא קשר לניקוד) כל ענפי הספורט
התמודדות דינמית התמודדות במהלך התחרות בזמן אמת כדורגל, טניס, קריקט
פעילות מעורבת שילוב של מספר הימורים שונים מגוון ענפי ספורט
פוקר אונליין – התמודדות באינטרנט
התמודדות בפוקר מקוון מכיל אחד ממשחקי הקזינו המשגשגים המשפיעים ביותר בזמן האחרון. שחקנים יכולים להתמודד בפני משתתפים אחרים מכל רחבי הגלובוס במגוון
https://win-line.net/הימורי-ספורט-באינטרנט/
לשלוח, ראיה לדבריך.
ההתמודדות באינטרנט הפכה לתעשייה נחשק מאוד לאחרונה, המאפשר מגוון רחב של אלטרנטיבות פעילות, החל מ משחקי פוקר.
בסקירה זה נפרט את תחום ההתמודדות המקוונת ונספק לכם הערות חשובות שיסייע לכם לנתח בנושא אטרקטיבי זה.
קזינו אונליין – הימורים באינטרנט
קזינו אונליין מאפשר אופציות שונות של פעילויות מסורתיים כגון בלאק ג’ק. ההימורים באינטרנט נותנים למבקרים ליהנות מאווירת הימורים מקצועית בכל עת ומקום.
סוג המשחק סיכום קצר
מכונות שלוט משחקי מזל
משחק הרולטה הימור על פרמטרים על גלגל מסתובב
בלאק ג’ק משחק קלפים בו המטרה היא 21 נקודות
משחק קלפים פוקר משחק קלפים אסטרטגי
משחק הבאקרה משחק קלפים פשוט ומהיר
הימורי ספורט – קזינו באינטרנט
הימורים בתחום הספורט מהווים חלק מ אחד התחומים המשגשגים ביותר בהתמודדות באינטרנט. מתמודדים רשאים להשקיע על תוצאות של אתגרי ספורט מועדפים כגון טניס.
ההימורים מתאפשרות על תוצאת המשחק, מספר הנקודות ועוד.
המשחק תיאור תחרויות ספורט מקובלות
ניחוש תוצאה ניחוש הביצועים הסופיים בתחרות כדורגל, כדורסל, הוקי
הפרש סקורים ניחוש ההפרש בביצועים בין הקבוצות כל ענפי הספורט
כמות הסקורים ניחוש כמות הביצועים בתחרות כל ענפי הספורט
המנצח בתחרות ניחוש מי יהיה הזוכה (ללא קשר לתוצאה) מגוון ענפי ספורט
הימורי חי הימורים במהלך המשחק בזמן אמת כדורגל, טניס, כדורסל
פעילות מעורבת שילוב של מספר אופני התמודדות מספר ענפי ספורט
התמודדות בפוקר מקוון – קזינו באינטרנט
משחקי קלפים אונליין הוא אחד מענפי הפעילות הפופולריים המובהקים ביותר כיום. שחקנים יכולים להתמודד מול יריבים מכל רחבי הגלובליזציה במגוון
Regular payment procedures include things like Visa, Voucher, MasterCard, and AMEX.
My blog post 카지노친구
When you’re looking to cash out, you can withdraw from $one hundred up to $2,500 weekly.
Here is my homepage; 카지노친구
With your banroll ready, and possibly a bonus claimed, you are now prepared to play on line roulette.
my blog post Check out this site
One particular argument in favor of a national lottery is that it could help slow or even reverse the development of thhe national debt.
Have a look at my page – Additional hints
The selection seems specific to outcome in profound changes to the nation’s connection wiith sports wagering.
Also visit my web page Get more info
Whereas in the European roulette game (the single zero),
the house edge is much lower at two.70%.
Stop by my homepage: Have a peek here
Профессиональные seo https://seo-optimizaciya-kazan.ru услуги для максимизации онлайн-видимости вашего бизнеса. Наши эксперты проведут глубокий анализ сайта, оптимизируют контент и структуру, улучшат технические аспекты и разработают индивидуальные стратегии продвижения.
rgbet
https://yfwqhjhbvlpj.deutsche-versicherungen.info/ .gyyO8iuPEED
buying from online mexican pharmacy: cmq pharma mexican pharmacy – medicine in mexico pharmacies
mexico pharmacies prescription drugs
https://cmqpharma.online/# mexican border pharmacies shipping to usa
mexican mail order pharmacies
AML проверка
Антиотмывочная проверка: Посредством чего избежать приостановление активов на платформах обмена криптовалют
Для чего важна проверка по борьбе с отмыванием денег?
Антиотмывочные меры (Anti-Money Laundering) – это система процедур, ориентированных в целях противодействия сокрытия ресурсов. Подобная оценка дает возможность охранять криптовалютные активы участников а также предотвращать применение систем противоправных транзакций. Процедура противодействия отмыванию денег необходима в целях обеспечения защищенности ваших фондов а также соблюдения нормативных норм.
Основные подходы оценки
Платформы обмена криптовалют а также другие денежные предложения внедряют разные важнейших подходов в рамках проверки владельцев:
Верификация личности: Эта методика предусматривает ключевые действия в целях идентификации документов пользователя, в том числе валидация подтверждающих данных проживания. Идентификация личности помогает убедиться, в надежности владельца подтверждает себя как законным.
CFT: Направлена для предотвращения спонсирования террористических актов. Процедура отслеживает вызывающие опасения переводы если требуется блокирует учетные записи посредством проведения внутреннего аудита.
Выгоды проверки по борьбе с отмыванием денег
Проверка по борьбе с отмыванием денег обеспечивает платформам обмена криптовалют:
Следовать международные вместе с национальными нормативные требования.
Охранять клиентов от мошенничества.
Укреплять уровень репутации среди владельцев госорганов.
Каким способом снизить вероятность себя при операциях с криптовалютой
Чтобы минимизировать риски приостановления фондов, следуйте перечисленным рекомендациям:
Работайте с проверенные сервисы: Переходите только к биржам с хорошей востребованностью и высоким уровнем безопасности.
Исследуйте участников: Используйте решения для верификации в интересах проверки криптовалютных реквизитов получателей перед проведением сделок.
Систематически обновляйте криптовалютные реквизиты: Указанная процедура поможет избежать гипотетических ограничений, если Ваши контрагенты контрагенты будут внесены под внимание.
Храните доказывающие материалы платежей: При ситуации будете в состоянии подтвердить чистоту принятых активов.
Обобщение
Процедура противодействия отмыванию денег – выступает в качестве значимый способ с целью обеспечения защищенности транзакций в криптосфере. Данная процедура способствует не допустить отмывание денег, обеспечение террористической деятельности помимо прочих незаконные мероприятия. Выполняя указаниям в интересах безопасности а также выбирая заслуживающие доверие сервисы, вы можете уменьшить опасности ограничения средств и наслаждаться безопасной функционированием в криптосфере.
Hello there! Do you know if they make any plugins to assist with SEO?
I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very
good gains. If you know of any please share.
Cheers!
外送茶
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
mexico drug stores pharmacies: cmq pharma mexican pharmacy – mexican online pharmacies prescription drugs
mexican online pharmacies prescription drugs
https://cmqpharma.com/# mexican mail order pharmacies
mexican online pharmacies prescription drugs
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
купить диплом авито ast-diplom.com .
Добрый день!
Где приобрести диплом по актуальной специальности?
Заказать диплом ВУЗа.
http://forumkasino.bestff.ru/viewtopic.php?id=3974#p9198
Хорошей учебы!
Геракл24: Квалифицированная Реставрация Фундамента, Венцов, Покрытий и Передвижение Строений
Организация Gerakl24 специализируется на выполнении полных работ по реставрации фундамента, венцов, настилов и перемещению зданий в городе Красноярском регионе и в окрестностях. Наш коллектив опытных мастеров обещает отличное качество исполнения всех типов ремонтных работ, будь то деревянные, каркасного типа, из кирпича или бетонные конструкции дома.
Достоинства сотрудничества с Gerakl24
Квалификация и стаж:
Весь процесс осуществляются только высококвалифицированными экспертами, с многолетним долгий стаж в сфере создания и ремонта зданий. Наши сотрудники знают свое дело и выполняют проекты с безупречной точностью и вниманием к мелочам.
Комплексный подход:
Мы осуществляем разнообразные услуги по восстановлению и восстановлению зданий:
Смена основания: замена и укрепление фундамента, что обеспечивает долгий срок службы вашего строения и избежать проблем, связанные с оседанием и деформацией строения.
Реставрация венцов: реставрация нижних венцов из дерева, которые наиболее часто гниют и разрушаются.
Установка новых покрытий: замена старых полов, что существенно улучшает визуальное восприятие и функциональные характеристики.
Перенос строений: качественный и безопасный перенос строений на другие участки, что позволяет сохранить ваше строение и избежать дополнительных затрат на строительство нового.
Работа с различными типами строений:
Деревянные дома: восстановление и укрепление деревянных конструкций, обработка от гниения и насекомых.
Дома с каркасом: реставрация каркасов и смена поврежденных частей.
Дома из кирпича: ремонт кирпичных стен и укрепление конструкций.
Бетонные строения: ремонт и укрепление бетонных конструкций, исправление трещин и разрушений.
Качество и надежность:
Мы применяем только проверенные материалы и современное оборудование, что обеспечивает долгий срок службы и надежность всех выполненных работ. Каждый наш проект подвергаются строгому контролю качества на всех этапах выполнения.
Индивидуальный подход:
Для каждого клиента мы предлагаем подходящие решения, учитывающие все особенности и пожелания. Мы стремимся к тому, чтобы результат нашей работы полностью соответствовал ваши ожидания и требования.
Почему стоит выбрать Геракл24?
Работая с нами, вы приобретете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы гарантируем выполнение всех задач в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете не сомневаться, что ваш дом в надежных руках.
Мы предлагаем консультацию и дать ответы на все вопросы. Свяжитесь с нами, чтобы обсудить детали и узнать о наших сервисах. Мы обеспечим сохранение и улучшение вашего дома, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
娛樂城
nettruyen
NetTruyen ZZZ: Nền tảng đọc truyện tranh trực tuyến dành cho mọi lứa tuổi
NetTruyen ZZZ là nền tảng đọc truyện tranh trực tuyến miễn phí với số lượng truyện tranh lên đến hơn 30.000 đầu truyện với chất lượng hình ảnh và tốc độ tải cao. Nền tảng được xây dựng với mục tiêu mang đến cho người đọc những trải nghiệm đọc truyện tranh tốt nhất, đồng thời tạo dựng cộng đồng yêu thích truyện tranh sôi động và gắn kết với hơn 11 triệu thành viên (tính đến tháng 7 năm 2024).
NetTruyen ZZZ – Kho tàng truyện tranh phong phú:
NetTruyen ZZZ sở hữu kho tàng truyện tranh khổng lồ với hơn 30.000 đầu truyện thuộc nhiều thể loại khác nhau như:
● Manga: Những bộ truyện tranh Nhật Bản với nhiều thể loại phong phú như lãng mạn, hành động, hài hước, v.v.
● NetTruyen anime: Hàng ngàn bộ truyện tranh anime chọn lọc được đăng tải đều đặn trên NetTruyen ZZZ được chuyển thể từ phim hoạt hình Nhật Bản với nội dung hấp dẫn và hình ảnh đẹp mắt.
● Truyện manga: Hơn 10.000 bộ truyện tranh manga hay nhất được đăng tải đầy đủ trên NetTruyen ZZZ.
● Truyện manhua: Hơn 5000 bộ truyện tranh manhua được đăng tải trọn bộ đầy đủ trên NetTruyen ZZZ.
● Truyện manhwa: Những bộ truyện tranh manhwa Hàn Quốc được yêu thích nhất có đầy đủ trên NetTruyen với cốt truyện lôi cuốn và hình ảnh bắt mắt cùng với nét vẽ độc đáo và nội dung đa dạng.
● Truyện ngôn tình: Những câu chuyện tình yêu lãng mạn, ngọt ngào và đầy cảm xúc.
● Truyện trinh thám: Những câu chuyện ly kỳ, bí ẩn và đầy lôi cuốn xoay quanh các vụ án và quá trình phá án.
● Truyện tranh xuyên không: Những câu chuyện về những nhân vật du hành thời gian hoặc không gian đến một thế giới khác.
NetTruyen ZZZ không ngừng cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường, đảm bảo mang đến cho bạn đọc những trải nghiệm đọc truyện mới mẻ và thú vị nhất.
Chất lượng hình ảnh và nội dung đỉnh cao tại NetTruyenZZZ:
Với hơn 30 triệu lượt truy cập hằng tháng, NetTruyen ZZZ luôn chú trọng vào chất lượng hình ảnh và nội dung của các bộ truyện tranh được đăng tải trên nền tảng. Hình ảnh được hiển thị sắc nét, rõ ràng, không bị mờ hay vỡ ảnh. Nội dung được dịch thuật chính xác, dễ hiểu và giữ nguyên vẹn ý nghĩa của tác phẩm gốc.
NetTruyen ZZZ hợp tác với đội ngũ dịch giả và biên tập viên chuyên nghiệp, giàu kinh nghiệm để đảm bảo chất lượng bản dịch tốt nhất. Nền tảng cũng có hệ thống kiểm duyệt nội dung nghiêm ngặt để đảm bảo nội dung lành mạnh, phù hợp với mọi lứa tuổi.
Trải nghiệm đọc truyện mượt mà, tiện lợi:
NetTruyen ZZZ được thiết kế với giao diện đẹp mắt, thân thiện với người dùng và dễ dàng sử dụng. Bạn đọc có thể đọc truyện tranh trên mọi thiết bị, từ máy tính, điện thoại thông minh đến máy tính bảng. Nền tảng cũng cung cấp nhiều tính năng tiện lợi như:
● Tìm kiếm truyện tranh theo tên, tác giả, thể loại, v.v.
● Lưu truyện tranh yêu thích để đọc sau.
● Đánh dấu trang để dễ dàng quay lại vị trí đang đọc.
● Chia sẻ truyện tranh với bạn bè.
● Tham gia bình luận và thảo luận về truyện tranh.
NetTruyen ZZZ luôn nỗ lực để mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
Định hướng phát triển:
NetTruyen ZZZ cam kết không ngừng phát triển và hoàn thiện để trở thành nền tảng đọc truyện tranh trực tuyến tốt nhất dành cho bạn đọc tại Việt Nam. Nền tảng sẽ tiếp tục cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường thế giới, đồng thời nâng cao chất lượng hình ảnh và nội dung. NetTruyen ZZZ cũng sẽ phát triển thêm nhiều tính năng mới để mang đến cho bạn đọc những trải nghiệm đọc truyện tốt nhất.
NetTruyen ZZZ luôn đặt lợi ích của bạn đọc lên hàng đầu. Nền tảng cam kết:
● Cung cấp kho tàng truyện tranh khổng lồ và đa dạng với chất lượng hình ảnh và nội dung đỉnh cao.
● Mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
● Luôn lắng nghe ý kiến phản hồi của bạn đọc và không ngừng cải thiện để mang đến dịch vụ tốt nhất.
NetTruyen ZZZ hy vọng sẽ trở thành người bạn đồng hành không thể thiếu của bạn trong hành trình khám phá thế giới truyện tranh đầy màu sắc.
Kết nối với NetTruyen ZZZ ngay hôm nay để tận hưởng những trải nghiệm đọc truyện tuyệt vời.
Gerakl24: Профессиональная Смена Фундамента, Венцов, Покрытий и Перенос Домов
Фирма Gerakl24 занимается на выполнении полных сервисов по замене основания, венцов, покрытий и переносу домов в населённом пункте Красноярск и за пределами города. Наша группа профессиональных специалистов обещает отличное качество исполнения различных типов восстановительных работ, будь то из дерева, каркасные, кирпичные или бетонные конструкции здания.
Преимущества услуг Геракл24
Квалификация и стаж:
Весь процесс проводятся исключительно опытными экспертами, с многолетним большой опыт в направлении создания и восстановления строений. Наши сотрудники эксперты в своей области и осуществляют работу с высочайшей точностью и учетом всех деталей.
Комплексный подход:
Мы предлагаем полный спектр услуг по ремонту и ремонту домов:
Реставрация фундамента: усиление и реставрация старого основания, что обеспечивает долгий срок службы вашего строения и избежать проблем, вызванные оседанием и деформацией.
Замена венцов: замена нижних венцов деревянных домов, которые наиболее часто гниют и разрушаются.
Замена полов: монтаж новых настилов, что существенно улучшает внешний облик и функциональные характеристики.
Передвижение домов: безопасное и качественное передвижение домов на другие участки, что помогает сохранить здание и избегает дополнительных затрат на строительство нового.
Работа с любыми типами домов:
Дома из дерева: реставрация и усиление деревянных элементов, защита от гниения и вредителей.
Каркасные строения: укрепление каркасов и замена поврежденных элементов.
Кирпичные дома: реставрация кирпичной кладки и усиление стен.
Бетонные строения: восстановление и укрепление бетонных структур, исправление трещин и разрушений.
Качество и надежность:
Мы работаем с лишь качественные материалы и передовые технологии, что гарантирует долгий срок службы и надежность всех работ. Все проекты проходят строгий контроль качества на каждом этапе выполнения.
Персонализированный подход:
Для каждого клиента мы предлагаем персонализированные решения, учитывающие ваши требования и желания. Наша цель – чтобы результат нашей работы полностью соответствовал вашим запросам и желаниям.
Почему выбирают Геракл24?
Сотрудничая с нами, вы получаете надежного партнера, который возьмет на себя все заботы по восстановлению и ремонту вашего здания. Мы обеспечиваем выполнение всех работ в сроки, установленные договором и с соблюдением всех правил и норм. Выбрав Геракл24, вы можете не сомневаться, что ваш дом в надежных руках.
Мы готовы предоставить консультацию и дать ответы на все вопросы. Звоните нам, чтобы обсудить ваш проект и узнать больше о наших услугах. Мы поможем вам сохранить и улучшить ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
https://gerakl24.ru/ремонт-фундамента-красноярск/
Introduction: The ketogenic diet has gained significant attention in recent years due to its potential for weight loss, increased
energy levels, and improved mental clarity.
NetTruyen ZZZ: Nền tảng đọc truyện tranh trực tuyến dành cho mọi lứa tuổi
NetTruyen ZZZ là nền tảng đọc truyện tranh trực tuyến miễn phí với số lượng truyện tranh lên đến hơn 30.000 đầu truyện với chất lượng hình ảnh và tốc độ tải cao. Nền tảng được xây dựng với mục tiêu mang đến cho người đọc những trải nghiệm đọc truyện tranh tốt nhất, đồng thời tạo dựng cộng đồng yêu thích truyện tranh sôi động và gắn kết với hơn 11 triệu thành viên (tính đến tháng 7 năm 2024).
NetTruyen ZZZ – Kho tàng truyện tranh phong phú:
NetTruyen ZZZ sở hữu kho tàng truyện tranh khổng lồ với hơn 30.000 đầu truyện thuộc nhiều thể loại khác nhau như:
● Manga: Những bộ truyện tranh Nhật Bản với nhiều thể loại phong phú như lãng mạn, hành động, hài hước, v.v.
● NetTruyen anime: Hàng ngàn bộ truyện tranh anime chọn lọc được đăng tải đều đặn trên NetTruyen ZZZ được chuyển thể từ phim hoạt hình Nhật Bản với nội dung hấp dẫn và hình ảnh đẹp mắt.
● Truyện manga: Hơn 10.000 bộ truyện tranh manga hay nhất được đăng tải đầy đủ trên NetTruyen ZZZ.
● Truyện manhua: Hơn 5000 bộ truyện tranh manhua được đăng tải trọn bộ đầy đủ trên NetTruyen ZZZ.
● Truyện manhwa: Những bộ truyện tranh manhwa Hàn Quốc được yêu thích nhất có đầy đủ trên NetTruyen với cốt truyện lôi cuốn và hình ảnh bắt mắt cùng với nét vẽ độc đáo và nội dung đa dạng.
● Truyện ngôn tình: Những câu chuyện tình yêu lãng mạn, ngọt ngào và đầy cảm xúc.
● Truyện trinh thám: Những câu chuyện ly kỳ, bí ẩn và đầy lôi cuốn xoay quanh các vụ án và quá trình phá án.
● Truyện tranh xuyên không: Những câu chuyện về những nhân vật du hành thời gian hoặc không gian đến một thế giới khác.
NetTruyen ZZZ không ngừng cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường, đảm bảo mang đến cho bạn đọc những trải nghiệm đọc truyện mới mẻ và thú vị nhất.
Chất lượng hình ảnh và nội dung đỉnh cao tại NetTruyenZZZ:
Với hơn 30 triệu lượt truy cập hằng tháng, NetTruyen ZZZ luôn chú trọng vào chất lượng hình ảnh và nội dung của các bộ truyện tranh được đăng tải trên nền tảng. Hình ảnh được hiển thị sắc nét, rõ ràng, không bị mờ hay vỡ ảnh. Nội dung được dịch thuật chính xác, dễ hiểu và giữ nguyên vẹn ý nghĩa của tác phẩm gốc.
NetTruyen ZZZ hợp tác với đội ngũ dịch giả và biên tập viên chuyên nghiệp, giàu kinh nghiệm để đảm bảo chất lượng bản dịch tốt nhất. Nền tảng cũng có hệ thống kiểm duyệt nội dung nghiêm ngặt để đảm bảo nội dung lành mạnh, phù hợp với mọi lứa tuổi.
Trải nghiệm đọc truyện mượt mà, tiện lợi:
NetTruyen ZZZ được thiết kế với giao diện đẹp mắt, thân thiện với người dùng và dễ dàng sử dụng. Bạn đọc có thể đọc truyện tranh trên mọi thiết bị, từ máy tính, điện thoại thông minh đến máy tính bảng. Nền tảng cũng cung cấp nhiều tính năng tiện lợi như:
● Tìm kiếm truyện tranh theo tên, tác giả, thể loại, v.v.
● Lưu truyện tranh yêu thích để đọc sau.
● Đánh dấu trang để dễ dàng quay lại vị trí đang đọc.
● Chia sẻ truyện tranh với bạn bè.
● Tham gia bình luận và thảo luận về truyện tranh.
NetTruyen ZZZ luôn nỗ lực để mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
Định hướng phát triển:
NetTruyen ZZZ cam kết không ngừng phát triển và hoàn thiện để trở thành nền tảng đọc truyện tranh trực tuyến tốt nhất dành cho bạn đọc tại Việt Nam. Nền tảng sẽ tiếp tục cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường thế giới, đồng thời nâng cao chất lượng hình ảnh và nội dung. NetTruyen ZZZ cũng sẽ phát triển thêm nhiều tính năng mới để mang đến cho bạn đọc những trải nghiệm đọc truyện tốt nhất.
NetTruyen ZZZ luôn đặt lợi ích của bạn đọc lên hàng đầu. Nền tảng cam kết:
● Cung cấp kho tàng truyện tranh khổng lồ và đa dạng với chất lượng hình ảnh và nội dung đỉnh cao.
● Mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
● Luôn lắng nghe ý kiến phản hồi của bạn đọc và không ngừng cải thiện để mang đến dịch vụ tốt nhất.
NetTruyen ZZZ hy vọng sẽ trở thành người bạn đồng hành không thể thiếu của bạn trong hành trình khám phá thế giới truyện tranh đầy màu sắc.
Kết nối với NetTruyen ZZZ ngay hôm nay để tận hưởng những trải nghiệm đọc truyện tuyệt vời.
онлайн казино с депозитом
https://remvend-cafe.ru/avtomati-igrat-registratsii/igrat-v-igrovie-avtomati-besplatno-bez-registratsii-onlayn.html
куплю диплом дней diplomyx.com .
Привет, друзья!
Реально ли приобрести диплом стоматолога? Основные этапы
1wum.ru/forum/?PAGE_NAME=profile_view&UID=39844&MUL_MODE=
Окажем помощь!.
онлайн казино с депозитом
https://remvend-cafe.ru/realnie/igrat-v-ruletku-na-realnie-dengi-rubli.html
купить диплом государственного вуза купить диплом государственного вуза .
Здравствуйте!
Где купить диплом по актуальной специальности?
Мы готовы предложить дипломы любых профессий по разумным ценам.
dip-vuz.ru/kupit-diplom-v-tyumeni/index.html
Привет!
Официальная покупка диплома вуза с сокращенной программой в Москве
mymink.5bb.ru/viewtopic.php?id=8918#p455039
Рады оказаться полезными!.
Привет!
Где заказать диплом по необходимой специальности?
Купить диплом о высшем образовании.
sonnick84.rusedu.net/post/10787/113369
купить диплом ссср в нижнем новгороде asxdiplomik.com .
Привет!
Мы можем предложить документы техникумов, которые находятся в любом регионе России. Можно заказать диплом от любого заведения, за любой год, в том числе документы старого образца СССР. Дипломы и аттестаты делаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и подписями.
zoomluck.com/blogs/1919/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Где приобрести диплом по актуальной специальности?
Заказать диплом любого ВУЗа.
forum.ro-ox.com/index.php?/gallery/image/188-%D1%88%D0%B8%D1%80%D0%BE%D0%BA%D0%B8%D0%B9-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Здравствуйте!
Приобретение диплома ПТУ с сокращенной программой обучения в Москве
androidinweb.ru/diplomyi-ot-luchshih-obrazovatelnyih-uchrezhdeniy
Добрый день!
Купить документ ВУЗа можно в нашем сервисе.
diplomasx.com/kupit-diplom-magistra
Здравствуйте!
Где заказать диплом специалиста?
Купить диплом любого университета.
films.name/viewforum.php?f=143
Здравствуйте!
Где заказать диплом по необходимой специальности?
Приобрести диплом университета.
l90226mw.beget.tech/2024/07/04/obshirnyy-katalog-dokumentov-v-populyarnom-onlayn-magazine.html
купить диплом вуз купить диплом вуз .
Привет, друзья!
Купить диплом о высшем образовании.
socialxtendr.com/blogs/171/%D0%A1%D1%82%D0%BE%D0%B8%D0%BC%D0%BE%D1%81%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2-%D1%81%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D0%BE%D1%82-%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%BE%D0%B2
Привет!
Где заказать диплом специалиста?
vseogirls.ru/byistroe-oformlenie-diploma-lyuboy-spetsialnosti
Удачи!
Добрый день!
Заказать диплом любого университета.
zdsim.ru/wiki/index.php/?????_?_????_????:_??????_???????_???????_?_????_???????
Успехов в учебе!
синий диплом купить http://diploms-x.com/ .
Can pharmacies legally sell over-the-counter medicines in bulk to consumers loniten tablets?
Привет, друзья!
Заказать документ университета вы сможете в нашем сервисе.
asxdiplomik.com/kupit-diplom-krasnoyarsk
Привет!
Предлагаем документы ВУЗов, которые расположены в любом регионе Российской Федерации. Можно приобрести диплом за любой год, включая сюда документы старого образца СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать государственные дипломы, которые не отличить от оригиналов. Документы будут заверены необходимыми печатями и подписями.
Мы готовы предложить дипломы любой профессии по доступным тарифам. Стоимость будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную ценовую политику. Важно, чтобы документы были доступными для большинства граждан.
arusak-diploms-srednee.ru/diplom-sredne-spetcialnoe-obrazovanie В
Успешной учебы!
Добрый день!
Мы предлагаем документы ВУЗов, расположенных на территории всей России. Вы сможете заказать качественно напечатанный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы делаются на бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Документы заверяются всеми требуемыми печатями и подписями.
shopy.partners/read-blog/1957
Привет, друзья!
Возможно ли купить диплом стоматолога, и как это происходит
gladpwnz.ru/forum/member.php?u=221749
Рады оказать помощь!.
Привет!
Мы предлагаем дипломы любой профессии по приятным ценам.
horordark.ru/kupit-diplom-onlayn-nadezhno-i-udobno
Добрый день!
Мы предлагаем выгодно и быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Данный документ способен пройти лубую проверку, даже с использованием профессионального оборудования. Решайте свои задачи быстро и просто с нашим сервисом.
комзем.рф/index.php?subaction=userinfo&user=etiku
Успешной учебы!
Привет!
Мы можем предложить документы техникумов, которые находятся на территории всей РФ. Вы имеете возможность купить диплом от любого учебного заведения, за любой год, в том числе документы СССР. Документы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Они заверяются всеми требуемыми печатями и штампами.
owen.ru/forum/album.php?albumid=218&attachmentid=77155&commentid=2439
What precautions should I take when handling injectable prescription drugs buy kamagra 100mg generic viagra?
สวัสดีครับทุกคน! พึ่งจะได้ลองเล่นที่ สล็อตออนไลน์เว็บตรง และต้องพูดว่าประสบการณ์ที่ได้รับมันดีเลิศขอรับ มีเกมสล็อตให้เลือกเล่นนานัปการ แต่ละเกมมีกราฟิกที่งดงามรวมทั้งเสียงประกอบที่น่าระทึกใจ สิ่งที่ผมถูกใจมากเป็นความปลอดภัยแล้วก็ความน่าวางใจของเว็บไซต์นี้
การฝาก-ถอนเร็วและไม่มีปัญหาใดๆเลยนะครับ คนใดกันแน่ที่กำลังมองหาเว็บสล็อตดีๆแนะนำให้ลองเล่นที่
หาเว็บตรงสล็อต เลยครับ การันตีว่าคุณจะติดใจ
Добрый день!
Приобрести документ о получении высшего образования можно у нас.
ast-diplom24.ru/kupit-diplom-ekaterinbur
Здравствуйте!
Приобрести документ института вы можете в нашем сервисе.
diplomasx24.ru/kupit-diplom-voronezh
Успехов в учебе!
Привет!
Как получить диплом о среднем образовании в Москве и других городах
arusak-diploms-srednee.ru/svidetelstvo-o-brake В
Здравствуйте!
Сколько стоит получить диплом высшего и среднего образования легально?
comedyforme.ru/vash-shans-na-uspeh-diplom-bez-truda
Рады оказать помощь!.
Привет!
Мы готовы предложить документы ВУЗов, которые находятся в любом регионе России. Можно купить диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются необходимыми печатями и штампами.
network-230.mn.co/posts/61837914
Привет, друзья!
Где купить диплом по необходимой специальности?
Заказать диплом о высшем образовании.
http://www.golf.od.ua/forum/viewtopic.php?p=77817#77817
Your mode of telling all in this post is genuinely nice, all be capable of effortlessly understand it, Thanks a lot.
Привет!
Узнайте, как приобрести диплом о высшем образовании без рисков
chrstms.ru/club/user/12549/blog/10938/
Рады оказать помощь!.
Привет!
Мы можем предложить дипломы любой профессии по выгодным ценам.
orbita.com.py/blogs/313/Вы-хотите-заказать-аттестат-у-надежного-исполнителя-Заходите
Добрый день!
Сколько стоит диплом высшего и среднего образования и как его получить?
spletninews.ru/legkiy-sposob-poluchit-diplom-nadezhno-i-konfidentsialno
Будем рады вам помочь!
Привет!
Мы изготавливаем дипломы любых профессий по доступным ценам.
http://www.thereaderview.com/wall/blogs/234/На-что-обратить-свое-внимание-при-заказе-диплома-в-сети
Привет, друзья!
Мы можем предложить дипломы любой профессии по доступным тарифам. Стоимость зависит от определенной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы документы были доступны для большинства граждан.
knoxc8d58.kylieblog.com/27534978/Дипломы-вследствие-деньги-Правда-о-Покупке-Образования-купить-диплом
Привет, друзья!
Мы готовы предложить дипломы любых профессий по приятным тарифам.
http://www.dr-ay.com/blogs/186078/Дипломы-от-Лучших-Университетов
Are there pills that should be taken with specific vegetables ivermectin 12?
The Hidden Account Concerning Solana Creator Toly’s Achievement
Following Two Portions of Java with a Pint
Toly, the brainchild behind Solana, commenced his quest with a modest practice – coffee and beer. Little did he realize, these occasions would trigger the machinery of his future. At present, Solana exists as a significant contender in the blockchain space, featuring a market value of billions.
Ethereum ETF First Sales
The Ethereum ETF lately was introduced with an impressive trade volume. This significant event experienced numerous spot Ethereum ETFs from multiple issuers begin trading on American exchanges, injecting unprecedented activity into the typically calm ETF trading environment.
Ethereum ETF Approval by SEC
The Securities and Exchange Commission has given the nod to the spot Ethereum ETF for listing. As a crypto asset featuring smart contracts, Ethereum is projected to have a profound impact the crypto industry due to this approval.
Trump and Bitcoin
With the election nearing, Trump positions himself as the ‘Crypto President,’ constantly highlighting his backing of the crypto sector to garner votes. His method differs from Biden’s tactic, aiming to capture the focus of the cryptocurrency community.
Elon Musk’s Influence
Musk, a prominent figure in the blockchain world and a proponent of the Trump camp, stirred things up again, promoting a meme coin related to his antics. His actions continues to shape market dynamics.
Binance Developments
A subsidiary of Binance, BAM, has been allowed to channel customer funds in U.S. Treasury securities. Furthermore, Binance observed its 7th year, highlighting its progress and achieving various compliance licenses. In the meantime, the company also made plans to take off several major crypto trading pairs, impacting various market participants.
AI and Economic Trends
Goldman Sachs’ leading stock analyst recently mentioned that artificial intelligence won’t trigger an economic revolution
Привет!
Заказать диплом о высшем образовании.
heimur.ru/index.php?/gallery/image/117-как-подобрать-проверенный-магазин-с-обширным-каталогом-дипломов/
Здравствуйте!
Заказать документ о получении высшего образования вы сможете у нас в столице.
diploms-x.com/kupit-diplom-krasnodar
Здравствуйте!
Купить документ о получении высшего образования можно в нашей компании.
diplomyx24.ru/kupit-diplom-ekaterinbur
Успешной учебы!
Добрый день!
Как безопасно купить диплом колледжа или ПТУ в России, что важно знать
tanhashop.com/category/uncategorized/page/2/
Окажем помощь!.
Discover your perfect stay with WorldHotels-in.com, your ultimate destination for finding the best hotels worldwide! Our user-friendly platform offers a vast selection of accommodations to suit every traveler’s needs and budget. Whether you’re planning a luxurious getaway or a budget-friendly adventure, we’ve got you covered with our extensive database of hotels across the globe. Our intuitive search features allow you to filter results based on location, amenities, price range, and guest ratings, ensuring you find the ideal match for your trip. We pride ourselves on providing up-to-date information and competitive prices, often beating other booking sites. Our detailed hotel descriptions, high-quality photos, and authentic guest reviews give you a comprehensive view of each property before you book. Plus, our secure booking system and excellent customer support team ensure a smooth and worry-free experience from start to finish. Don’t waste time jumping between multiple websites – http://www.WorldHotels-in.com brings the world’s best hotels to your fingertips in one convenient place. Start planning your next unforgettable journey today and experience the difference with WorldHotels-in.com!
Добрый день!
Купить документ ВУЗа вы сможете в нашем сервисе.
ast-diplomy.com/kupit-diplom-o-vysshem-obrazovanii
Good answers in return of this issue with firm arguments and describing all on the topic
of that.
Здравствуйте!
Мы готовы предложить дипломы любой профессии по доступным ценам. Стоимость зависит от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступны для подавляющей массы граждан.
umorforme.ru/zakazat-diplom-onlayn-prosto-i-udobno